The Clinical Frailty Scale: Do Staff Agree?
Abstract
1. Introduction
2. Methodology
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- WHO Clinical Consortium on Healthy Ageing: Topic Focus: Frailty and Intrinsic Capacity: Report of Consortium Meeting, 2016 in Geneva, Switzerland. Available online: https://www.who.int/ageing/health-systems/first-CCHA-meeting-report.pdf?ua=1 (accessed on 24 June 2020).
- Romero-Ortuno, R.; O’Shea, D. Fitness and frailty: opposite ends of a challenging continuum! Will the end of age discrimination make frailty assessments an imperative? Age Ageing 2013, 42, 279–280. [Google Scholar] [CrossRef] [PubMed]
- British Geriatrics Society, Fit for frailty guideline. Available online: https://www.bgs.org.uk/sites/default/files/content/resources/files/2018-05-23/fff_full.pdf (accessed on 24 June 2020).
- Wou, F.; Gladman, J.; Bradshaw, L.; Franklin, M.; Edmans, J.; Conroy, S. The predictive properties of frailty-rating scales in the acute medical unit. Eur. Geriatr. Med. 2013, 4, S74. [Google Scholar] [CrossRef]
- Rockwood, K.; Song, X.; Macknight, C.; Bergman, H.; Hogan, D.B.; McDowell, I.; Mitnitski, A. A global clinical measure of fitness and frailty in elderly people. Can. Med Assoc. J. 2005, 173, 489–495. [Google Scholar] [CrossRef] [PubMed]
- Specialised Clinical Frailty Network, the Clinical Frailty Scale. Available online: https://www.scfn.org.uk/clinical-frailty-scale (accessed on 24 June 2020).
- Darvall, J.N.; Bellomo, R.; Paul, E.; Subramaniam, A.; Santamaria, J.D.; Bagshaw, S.M.; Rai, S.; E Hubbard, R.; Pilcher, D. Frailty in very old critically ill patients in Australia and New Zealand: a population-based cohort study. Med J. Aust. 2019, 211, 318–323. [Google Scholar] [CrossRef] [PubMed]
- O’Caoimh, R.; Costello, M.; Small, C.; Spooner, L.; Flannery, A.; O’Reilly, L.; Heffernan, L.; Mannion, E.; Maughan, A.; Joyce, A.; et al. Comparison of Frailty Screening Instruments in the Emergency Department. Int. J. Environ. Res. Public Heal. 2019, 16, 3626. [Google Scholar] [CrossRef] [PubMed]
- Kahlon, S.; Pederson, J.; Majumdar, S.R.; Belga, S.; Lau, D.; Fradette, M.; Boyko, D.; Bakal, J.A.; Johnston, C.; Padwal, R.; et al. Association between frailty and 30-day outcomes after discharge from hospital. Can. Med Assoc. J. 2015, 187, 799–804. [Google Scholar] [CrossRef] [PubMed]
- Patel, K.V.; Brennan, K.L.; Brennan, M.L.; Jupiter, D.C.; Shar, A.; Davis, M.L. Association of a Modified Frailty Index With Mortality After Femoral Neck Fracture in Patients Aged 60 Years and Older. Clin. Orthop. Relat. Res. 2013, 472, 1010–1017. [Google Scholar] [CrossRef] [PubMed]
- Gregorevic, K.J.; E Hubbard, R.; Lim, W.K.; Katz, B. The clinical frailty scale predicts functional decline and mortality when used by junior medical staff: a prospective cohort study. BMC Geriatr. 2016, 16, 117. [Google Scholar] [CrossRef] [PubMed]
- Davies, J.; Whitlock, J.; Gutmanis, I.; Kane, S.-L. Inter-Rater Reliability of the Retrospectively Assigned Clinical Frailty Scale Score in a Geriatric Outreach Population. Can. Geriatr. J. 2018, 21, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Pugh, R.; Ellison, A.; Pye, K.; Subbe, C.P.; Thorpe, C.M.; Lone, N.; Clegg, A. Feasibility and reliability of frailty assessment in the critically ill: a systematic review. Crit. Care 2018, 22, 49. [Google Scholar] [CrossRef] [PubMed]
- Rolfson, D.B.; Majumdar, S.R.; Tsuyuki, R.T.; Tahir, A.; Rockwood, K. Validity and reliability of the Edmonton frailty score. Age and Ageing 2006, 35, 526–529. [Google Scholar] [CrossRef] [PubMed]

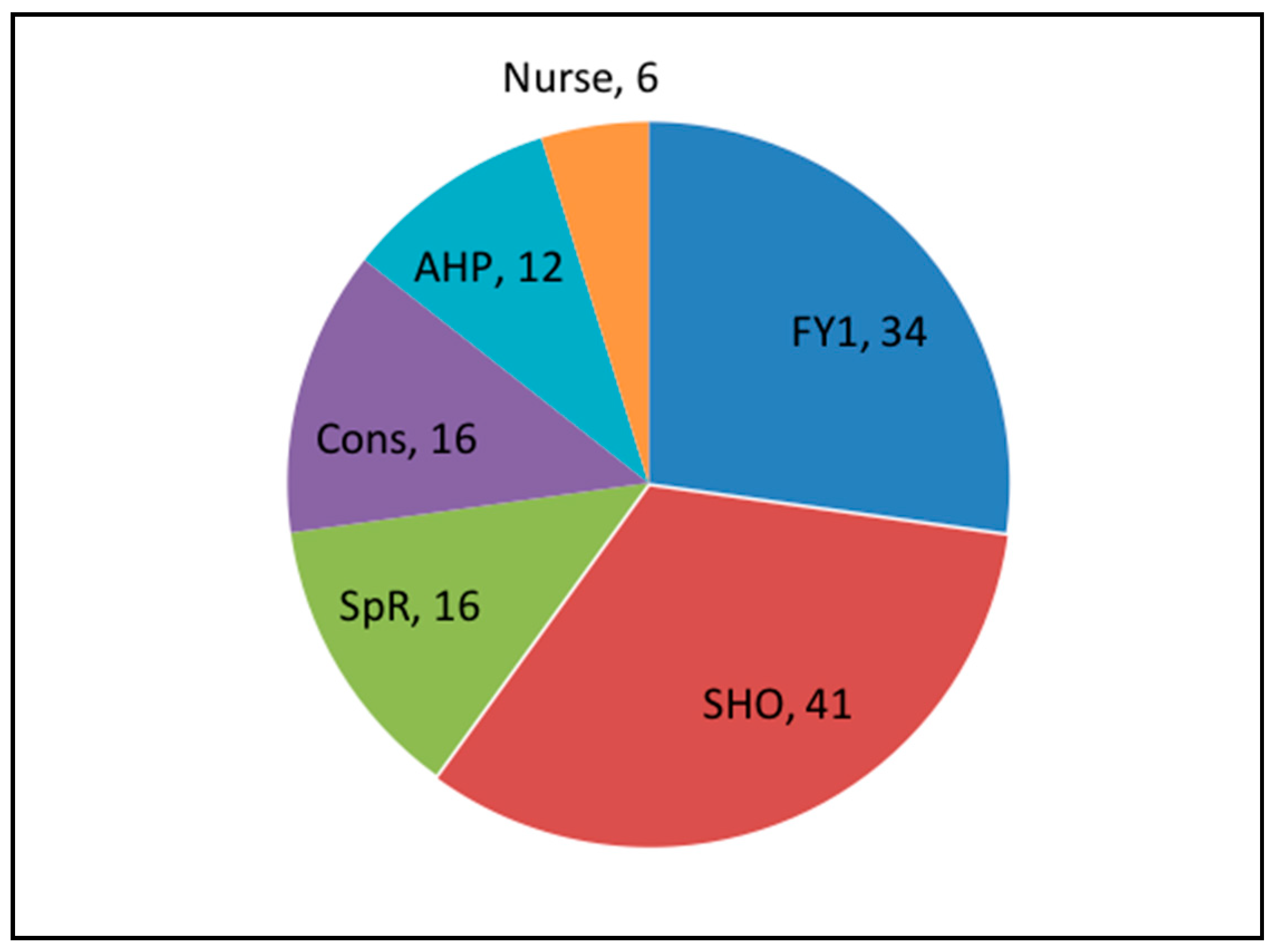
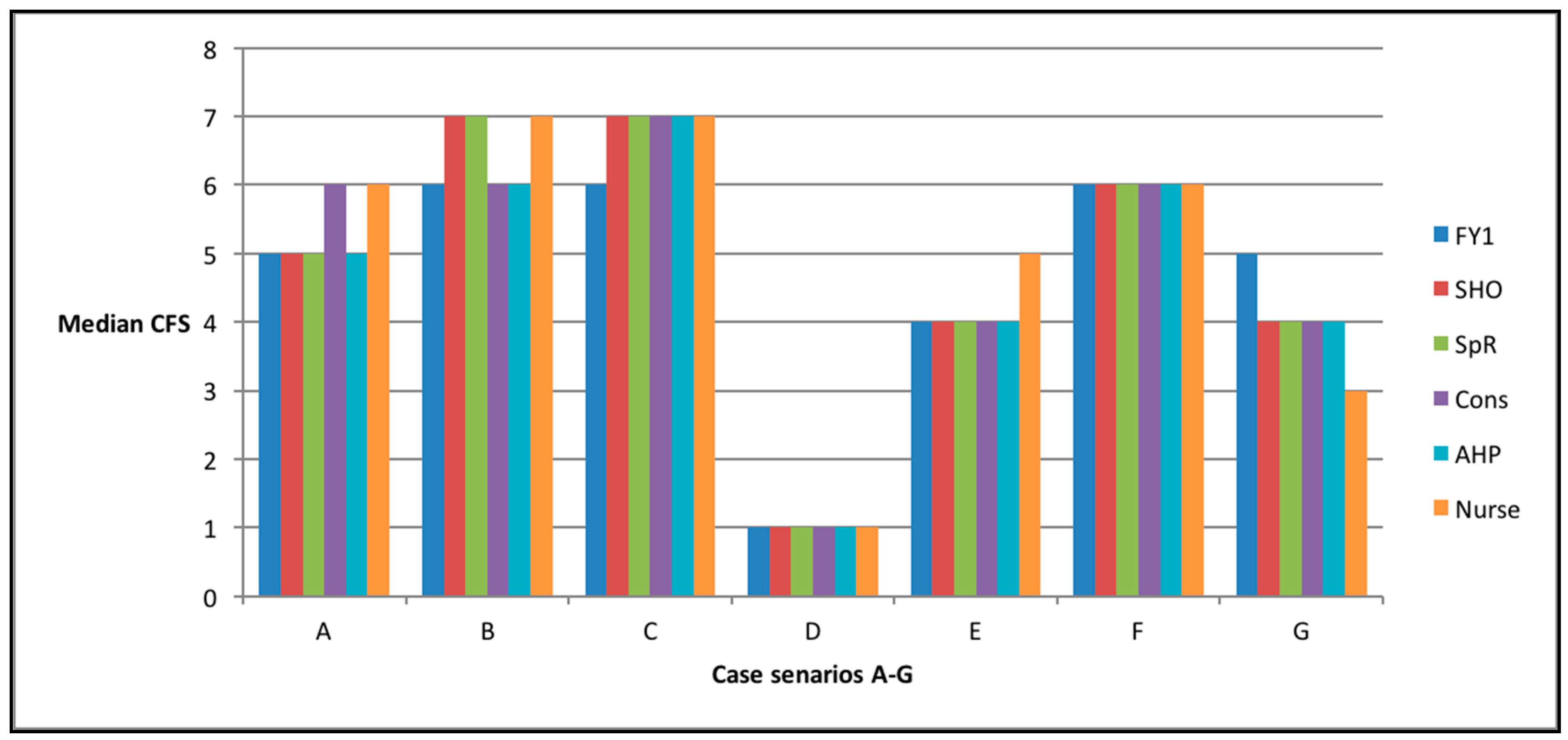
| Staff Grade | Years Qualified | Experience with CFS |
|---|---|---|
| FY1 | Immediately post qualification | None |
| SHO | Second year post training (may be longer depending on the individual) | None |
| Registrar | Min 4 years after undergraduate training | A few may have used the CFS |
| Consultant | At least nine years post graduate training | Depending on Specialty. Geriatricians would have experience other specialties not |
| Nursing/ AHP | Mixed 1–20 | No exposure to CFS |
| Case History | |
|---|---|
| A. | 84-year-old male. Admitted with a fall. Lives alone. Independent washing and dressing. Uses a walking stick in the house, housebound. Problems with urinary incontinence and wears pads. Has a BD care package when son away. |
| B. | 81-year-old female. Walks with a Zimmer frame. Single level living. Undertakes a strip wash. Needs help with dressing, cooking, cleaning, shopping. Housebound. Carers 4 times a day. Unable to manage finances. |
| C. | 91-year-old male. Independent with transfers from bed to chair but help otherwise to transfer chair to commode. Walks with a Zimmer frame but needs assistance. Help with personal activities of daily living (ADLs) (washing, dressing, shaving). Continence is an issue. Short term memory problems. Housebound. Unable to manage finances. |
| D. | 74-year-old female. Working in an office, independent and self-caring. Drives a car. No care issues. |
| E. | 89-year-old female. Walks with a stick and uses a 4-wheel shopper. Beginning to struggle with transfers (out of chair, off toilet) and lower half dressing. No package of care. |
| F. | 84-year-old female. Recurrent falls and troubles with medication. Housebound, carers three times a day. Continent. Help with cooking, shopping and dressing. Requires help with medication. Cannot manage finances. |
| G. | 82-year-old female. Falls, dementia. Independently mobile. Out shopping. Walks with a stick. Independent with personal and extended ADLS. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Young, R.L.; Smithard, D.G. The Clinical Frailty Scale: Do Staff Agree? Geriatrics 2020, 5, 40. https://doi.org/10.3390/geriatrics5020040
Young RL, Smithard DG. The Clinical Frailty Scale: Do Staff Agree? Geriatrics. 2020; 5(2):40. https://doi.org/10.3390/geriatrics5020040
Chicago/Turabian StyleYoung, Rebekah L., and David G. Smithard. 2020. "The Clinical Frailty Scale: Do Staff Agree?" Geriatrics 5, no. 2: 40. https://doi.org/10.3390/geriatrics5020040
APA StyleYoung, R. L., & Smithard, D. G. (2020). The Clinical Frailty Scale: Do Staff Agree? Geriatrics, 5(2), 40. https://doi.org/10.3390/geriatrics5020040






