Synergy of Regenerative Periodontal Surgery and Orthodontics Improves Quality of Life of Patients with Stage IV Periodontitis: 24-Month Outcomes of a Multicenter RCT
Abstract
1. Introduction
2. Materials & Methods
2.1. Study Design and Patients
2.2. Minimally Invasive Regenerative Periodontal Surgery
2.3. Orthodontic Therapy
2.4. Supportive Care
2.5. Periodontal Parameters
- (1)
- Clinical attachment level (CAL),
- (2)
- Probing pocket depth (PPD),
- (3)
- Bleeding on probing (BOP),
- (4)
- Full-mouth bleeding scores (FMBS),
- (5)
- Full-mouth plaque scores (FMPS).
2.6. Patient-Reported Outcomes
2.7. Data Analysis
3. Results
3.1. Periodontal Outcomes
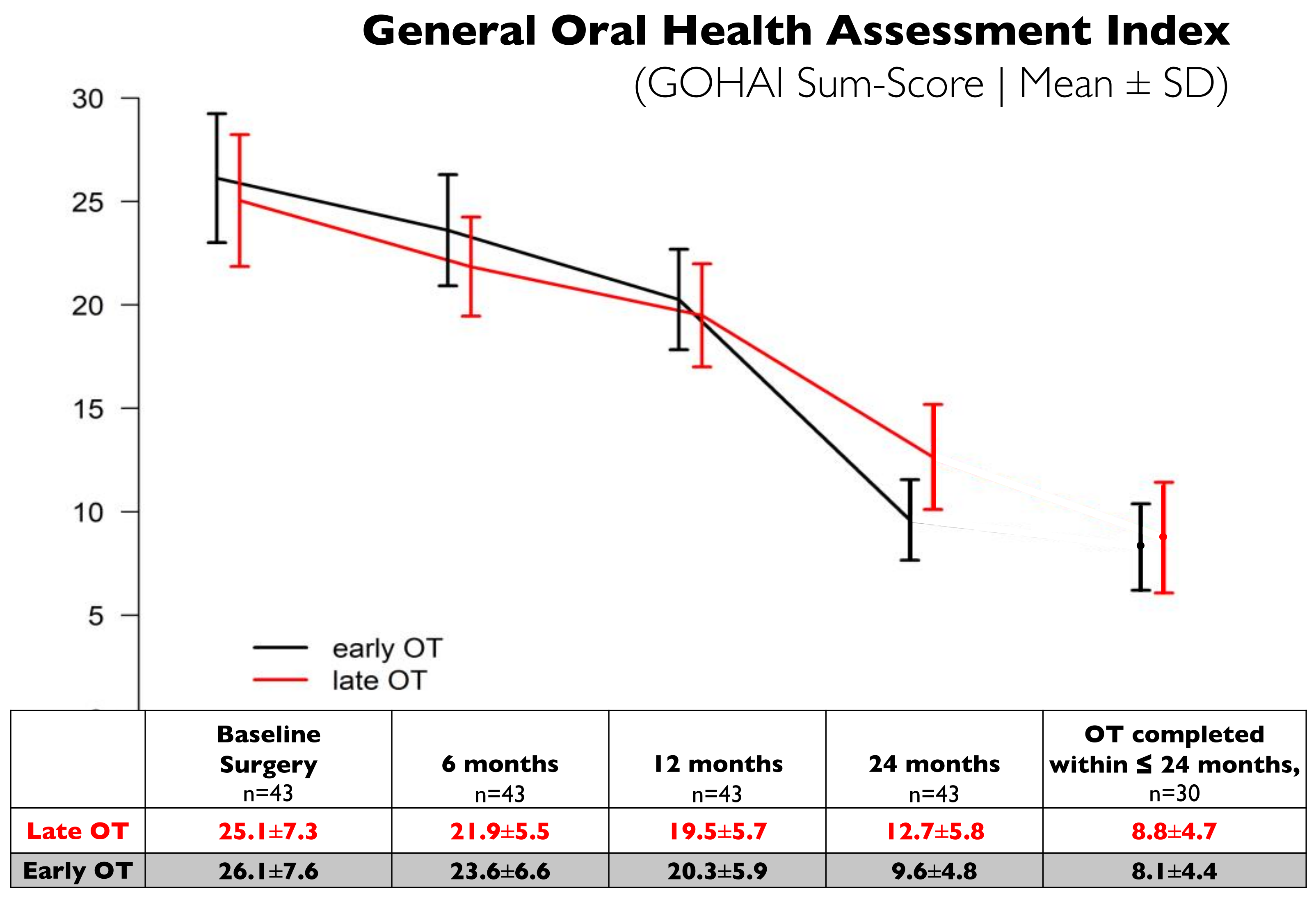
3.2. Oral Health-Related Quality of Life (OHrQoL)
4. Discussion
5. Conclusions
- (1)
- significantly improved periodontal conditions,
- (2)
- significantly higher CAL-gain for early initiation of OT,
- (3)
- an overall significantly improved OHrQoL.
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Martin, C.; Celis, B.; Ambrosio, N.; Bollain, J.; Antonoglou, G.N.; Figuero, E. Effect of orthodontic therapy in periodontitis and non-periodontitis patients: A systematic review with meta-analysis. J. Clin. Periodontol. 2022, 49 (Suppl. S24), 72–101. [Google Scholar] [CrossRef] [PubMed]
- Papageorgiou, S.N.; Antonoglou, G.N.; Michelogiannakis, D.; Kakali, L.; Eliades, T.; Madianos, P. Effect of periodontal-orthodontic treatment of teeth with pathological tooth flaring, drifting, and elongation in patients with severe periodontitis: A systematic review with meta-analysis. J. Clin. Periodontol. 2022, 49 (Suppl. S24), 102–120. [Google Scholar] [CrossRef] [PubMed]
- Kloukos, D.; Roccuzzo, A.; Stähli, A.; Sculean, A.; Katsaros, C.; Salvi, G. Effect of combined periodontal and orthodontic treatment of tilted molars, and of teeth with intrabony and furcation defects in stage IV periodontitis patients. A systematic review. J. Clin. Periodontol. 2022, 49 (Suppl. S24), 121–148. [Google Scholar] [CrossRef] [PubMed]
- Herrera, D.; Sanz, M.; Kebschull, M.; Jepsen, S.; Sculean, A.; Berglundh, T.; Papapanou, P.N.; Chapple, I.; Tonetti, M.S.; Participants, E.F.P.W.; et al. Treatment of stage IV periodontitis: The EFP S3 level clinical practice guideline. J. Clin. Periodontol. 2022, 49 (Suppl. S24), 4–71. [Google Scholar] [CrossRef] [PubMed]
- Cortellini, P.; Tonetti, M.S. Clinical concepts for regenerative therapy in intrabony defects. Periodontol. 2000 2015, 68, 282–307. [Google Scholar] [CrossRef] [PubMed]
- Broseler, F.; Tietmann, C.; Hinz, A.K.; Jepsen, S. Long-term results of periodontal regenerative therapy: A retrospective practice-based cohort study. J. Clin. Periodontol. 2017, 44, 520–529. [Google Scholar] [CrossRef]
- Nibali, L.; Koidou, V.P.; Nieri, M.; Barbato, L.; Pagliaro, U.; Cairo, F. Regenerative surgery versus access flap for the treatment of intra-bony periodontal defects: A systematic review and meta-analysis. J. Clin. Periodontol. 2020, 47 (Suppl. S22), 320–351. [Google Scholar] [CrossRef]
- Nibali, L.; Sultan, D.; Arena, C.; Pelekos, G.; Lin, G.H.; Tonetti, M. Periodontal infrabony defects: Systematic review of healing by defect morphology following regenerative surgery. J. Clin. Periodontol. 2021, 48, 100–113. [Google Scholar] [CrossRef]
- Sanz, M.; Herrera, D.; Kebschull, M.; Chapple, I.; Jepsen, S.; Berglundh, T.; Sculean, A.; Tonetti, M.S.; Participants, E.F.P.W.; Methodological, C. Treatment of stage I-III periodontitis-The EFP S3 level clinical practice guideline. J. Clin. Periodontol. 2020, 47, 4–60. [Google Scholar] [CrossRef]
- Jepsen, K.; Tietmann, C.; Kutschera, E.; Wullenweber, P.; Jager, A.; Cardaropoli, D.; Gaveglio, L.; Sanz Sanchez, I.; Martin, C.; Fimmers, R.; et al. The effect of timing of orthodontic therapy on the outcomes of regenerative periodontal surgery in patients with stage IV periodontitis: A multicenter randomized trial. J. Clin. Periodontol. 2021, 48, 1282–1292. [Google Scholar] [CrossRef]
- Roccuzzo, M.; Marchese, S.; Dalmasso, P.; Roccuzzo, A. Periodontal Regeneration and Orthodontic Treatment of Severely Periodontally Compromised Teeth: 10-Year Results of a Prospective Study. Int. J. Periodontics Restor. Dent. 2018, 38, 801–809. [Google Scholar] [CrossRef] [PubMed]
- Aimetti, M.; Garbo, D.; Ercoli, E.; Grigorie, M.M.; Citterio, F.; Romano, F. Long-Term Prognosis of Severely Compromised Teeth Following Combined Periodontal and Orthodontic Treatment: A Retrospective Study. Int. J. Periodontics Restor. Dent. 2020, 40, 95–102. [Google Scholar] [CrossRef] [PubMed]
- Tietmann, C.; Broseler, F.; Axelrad, T.; Jepsen, K.; Jepsen, S. Regenerative periodontal surgery and orthodontic tooth movement in stage IV periodontitis: A retrospective practice-based cohort study. J. Clin. Periodontol. 2021, 48, 668–678. [Google Scholar] [CrossRef] [PubMed]
- Garbo, D.; Aimetti, M.; Bongiovanni, L.; Vidotto, C.; Mariani, G.M.; Baima, G.; Romano, F. Periodontal and Orthodontic Synergy in the Management of Stage IV Periodontitis: Challenges, Indications and Limits. Life 2022, 12, 2131. [Google Scholar] [CrossRef]
- Tietmann, C.; Jepsen, S.; Heibrok, H.; Wenzel, S.; Jepsen, K. Long-term stability of regenerative periodontal surgery and orthodontic tooth movement in stage IV periodontitis: 10-year data of a retrospective study. J. Periodontol. 2023. [Google Scholar] [CrossRef]
- Pini Prato, G.P.; Chambrone, L. Orthodontic treatment in periodontal patients: The use of periodontal gold standards to overcome the “grey zone”. J. Periodontol. 2020, 91, 437–441. [Google Scholar] [CrossRef]
- Nemcovsky, C.E.; Sasson, M.; Beny, L.; Weinreb, M.; Vardimon, A.D. Periodontal healing following orthodontic movement of rat molars with intact versus damaged periodontia towards a bony defect. Eur. J. Orthod. 2007, 29, 338–344. [Google Scholar] [CrossRef]
- Vardimon, A.D.; Nemcovsky, C.E.; Dre, E. Orthodontic tooth movement enhances bone healing of surgical bony defects in rats. J. Periodontol. 2001, 72, 858–864. [Google Scholar] [CrossRef]
- Diedrich, P.; Fritz, U.; Kinzinger, G.; Angelakis, J. Movement of periodontally affected teeth after guided tissue regeneration (GTR)-an experimental pilot study in animals. J. Orofac. Orthop. 2003, 64, 214–227. [Google Scholar] [CrossRef]
- Cardaropoli, D.; Re, S.; Manuzzi, W.; Gaveglio, L.; Cardaropoli, G. Bio-oss collagen and orthodontic movement for the treatment of infrabony defects in the esthetic zone. Int. J. Periodont. Rest. 2006, 26, 553–559. [Google Scholar]
- Ogihara, S.; Wang, H.L. Periodontal regeneration with or without limited orthodontics for the treatment of 2- or 3-wall infrabony defects. J. Periodontol. 2010, 81, 1734–1742. [Google Scholar] [CrossRef] [PubMed]
- Attia, M.S.; Hazzaa, H.H.; Al-Aziz, F.A.; Elewa, G.M. Evaluation of Adjunctive Use of Low-Level Diode Laser Biostimulation with Combined Orthodontic Regenerative Therapy. J. Int. Acad. Periodontol. 2019, 21, 63–73. [Google Scholar] [PubMed]
- Attia, M.S.; Shoreibah, E.A.; Ibrahim, S.A.; Nassar, H.A. Regenerative Therapy of Osseous Defects Combined with Orthodontic Tooth Movement. J. Int. Acad. Periodontol. 2012, 14, 17–25. [Google Scholar] [PubMed]
- Ghezzi, C.; Viganò, V.M.; Francinetti, P.; Zanotti, G.; Masiero, S. Orthodontic Treatment After Induced Periodontal Regeneration in Deep Infrabony Defects. Clin. Adv. Periodontics 2013, 3, 24–31. [Google Scholar] [CrossRef]
- Locker, D.; Matear, D.; Stephens, M.; Lawrence, H.; Payne, B. Comparison of the GOHAI and OHIP-14 as measures of the oral health-related quality of life of the elderly. Community Dent. Oral Epidemiol. 2008, 29, 373–381. [Google Scholar] [CrossRef]
- FDI General Assembly. Oral Health and Quality of Life. Available online: https://www.fdiworlddental.org/oral-health-and-quality-life (accessed on 22 April 2023).
- Graziani, F.; Tsakos, G. Patient-based outcomes and quality of life. Periodontol. 2000 2020, 83, 277–294. [Google Scholar] [CrossRef]
- Ohrn, K.; Jonsson, B. A comparison of two questionnaires measuring oral health-related quality of life before and after dental hygiene treatment in patients with periodontal disease. Int. J. Dent. Hyg. 2012, 10, 9–14. [Google Scholar] [CrossRef]
- Needleman, I.; McGrath, C.; Floyd, P.; Biddle, A. Impact of oral health on the life quality of periodontal patients. J. Clin. Periodontol. 2004, 31, 454–457. [Google Scholar] [CrossRef]
- Yang, C.; Crystal, Y.O.; Ruff, R.R.; Veitz-Keenan, A.; McGowan, R.C.; Niederman, R. Quality Appraisal of Child Oral Health-Related Quality of Life Measures: A Scoping Review. JDR Clin. Trans. Res. 2020, 5, 109–117. [Google Scholar] [CrossRef]
- Schierz, O.; Baba, K.; Fueki, K. Functional oral health-related quality of life impact: A systematic review in populations with tooth loss. J. Oral Rehabil. 2021, 48, 256–270. [Google Scholar] [CrossRef]
- Larsson, P. Methodological studies of orofacial aesthetics, orofacial function and oral health-related quality of life. Swed. Dent. J. Suppl. 2010, 204, 11–98. [Google Scholar]
- McGrath, C.; Bedi, R. An evaluation of a new measure of oral health related quality of life—OHQoL-UK(W). Community Dent. Health 2001, 18, 138–143. [Google Scholar]
- Aslund, M.; Pjetursson, B.E.; Lang, N.P. Measuring oral health-related quality-of-life using OHQoL-GE in periodontal patients presenting at the University of Berne, Switzerland. Oral Health Prev. Dent. 2008, 6, 191–197. [Google Scholar]
- Ferreira, M.C.; Dias-Pereira, A.C.; Branco-de-Almeida, L.S.; Martins, C.C.; Paiva, S.M. Impact of periodontal disease on quality of life: A systematic review. J. Periodontal Res. 2017, 52, 651–665. [Google Scholar] [CrossRef]
- Buset, S.L.; Walter, C.; Friedmann, A.; Weiger, R.; Borgnakke, W.S.; Zitzmann, N.U. Are periodontal diseases really silent? A systematic review of their effect on quality of life. J. Clin. Periodontol. 2016, 43, 333–344. [Google Scholar] [CrossRef]
- Franke, M.; Broseler, F.; Tietmann, C. Patient-related evaluation after systematic periodontal therapy—A clinical study on periodontal health-related quality of life (PHQoL). Oral Health Prev. Dent. 2015, 13, 163–168. [Google Scholar] [CrossRef]
- Petersen, P.E. The World Oral Health Report 2003: Continuous improvement of oral health in the 21st century—The approach of the WHO Global Oral Health Programme. Community Dent. Oral Epidemiol. 2003, 31 (Suppl. S1), 3–23. [Google Scholar] [CrossRef]
- Petersen, P.E. Global policy for improvement of oral health in the 21st century-implications to oral health research of World Health Assembly 2007, World Health Organization. Community Dent. Oral Epidemiol. 2009, 37, 1–8. [Google Scholar] [CrossRef]
- Ajwa, N.; AlHammad, A.; AlAmmar, L.; AlMarjan, M.; AlShugair, T.; AlManie, L.; Bangalore, D. The Influence of Orthodontic Treatment Need on Oral Health-Related Quality of Life among 12–18-Year-Old Adolescents in Riyadh. Healthcare 2022, 10, 2153. [Google Scholar] [CrossRef]
- Bekes, K.; Kuhr, K.; Ohm, C.; Frenzel Baudisch, N.; Jordan, A.R. Does orthodontic treatment need have an impact on oral health-related quality of life? J. Orofac. Orthop. 2023, 84, 19–25. [Google Scholar] [CrossRef]
- Atchison, K.A.; Dolan, T.A. Development of the Geriatric Oral Health Assessment Index. J. Dent. Educ. 1990, 54, 680–687. [Google Scholar] [CrossRef] [PubMed]
- Hassel, A.J.; Rolko, C.; Koke, U.; Leisen, J.; Rammelsberg, P. A German version of the GOHAI. Community Dent. Oral Epidemiol. 2008, 36, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Aguirre-Bustamante, J.; Baron-Lopez, F.J.; Carmona-Gonzalez, F.J.; Perez-Farinos, N.; Warnberg, J. Validation of a modified version of the Spanish Geriatric Oral Health Assessment Index (GOHAI-SP) for adults and elder people. BMC Oral Health 2020, 20, 61. [Google Scholar] [CrossRef] [PubMed]
- Bianco, A.; Mazzea, S.; Fortunato, L.; Giudice, A.; Papadopoli, R.; Nobile, C.G.A.; Pavia, M. Oral Health Status and the Impact on Oral Health-Related Quality of Life among the Institutionalized Elderly Population: A Cross-Sectional Study in an Area of Southern Italy. Int. J. Environ. Res. Public Health 2021, 18, 2175. [Google Scholar] [CrossRef]
- Wiegand, C.; White, R. Microdeformation in wound healing. Wound Repair Regen. 2013, 21, 793–799. [Google Scholar] [CrossRef] [PubMed]
- Krishnan, V.; Davidovitch, Z. On a path to unfolding the biological mechanisms of orthodontic tooth movement. J. Dent. Res. 2009, 88, 597–608. [Google Scholar] [CrossRef]
- Lu, F.; Ogawa, R.; Nguyen, D.T.; Chen, B.; Guo, D.; Helm, D.L.; Zhan, Q.; Murphy, G.F.; Orgill, D.P. Microdeformation of three-dimensional cultured fibroblasts induces gene expression and morphological changes. Ann. Plast. Surg. 2011, 66, 296–300. [Google Scholar] [CrossRef]
- Suzuki, R.; Nemoto, E.; Shimauchi, H. Cyclic tensile force up-regulates BMP-2 expression through MAP kinase and COX-2/PGE2 signaling pathways in human periodontal ligament cells. Exp. Cell Res. 2014, 323, 232–241. [Google Scholar] [CrossRef]
- Tantilertanant, Y.; Niyompanich, J.; Everts, V.; Supaphol, P.; Pavasant, P.; Sanchavanakit, N. Cyclic tensile force stimulates BMP9 synthesis and in vitro mineralization by human periodontal ligament cells. J. Cell Physiol. 2019, 234, 4528–4539. [Google Scholar] [CrossRef]
- Fletcher, D.A.; Mullins, R.D. Cell mechanics and the cytoskeleton. Nature 2010, 463, 485–492. [Google Scholar] [CrossRef]
- Maurer, M.; Lammerding, J. The Driving Force: Nuclear Mechanotransduction in Cellular Function, Fate, and Disease. Annu. Rev. Biomed. Eng. 2019, 21, 443–468. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Zhan, Q.; Bao, M.; Yi, J.; Li, Y. Biomechanical and biological responses of periodontium in orthodontic tooth movement: Up-date in a new decade. Int. J. Oral Sci. 2021, 13, 20. [Google Scholar] [CrossRef] [PubMed]
- Zainal Ariffin, S.H.; Yamamoto, Z.; Zainol Abidin, I.Z.; Megat Abdul Wahab, R.; Zainal Ariffin, Z. Cellular and molecular changes in orthodontic tooth movement. Sci. World J. 2011, 11, 1788–1803. [Google Scholar] [CrossRef]
- Vining, K.H.; Mooney, D.J. Mechanical forces direct stem cell behaviour in development and regeneration. Nat. Rev. Mol. Cell Biol. 2017, 18, 728–742. [Google Scholar] [CrossRef]
- Alghamdi, B.; Jeon, H.H.; Ni, J.; Qiu, D.; Liu, A.; Hong, J.J.; Ali, M.; Wang, A.; Troka, M.; Graves, D.T. Osteoimmunology in Periodontitis and Orthodontic Tooth Movement. Curr. Osteoporos. Rep. 2023, 21, 128–146. [Google Scholar] [CrossRef]
- Wong, R.M.; Ng, S.K.; Corbet, E.F.; Keung Leung, W. Non-surgical periodontal therapy improves oral health-related quality of life. J. Clin. Periodontol. 2012, 39, 53–61. [Google Scholar] [CrossRef]
- Shanbhag, S.; Dahiya, M.; Croucher, R. The impact of periodontal therapy on oral health-related quality of life in adults: A systematic review. J. Clin. Periodontol. 2012, 39, 725–735. [Google Scholar] [CrossRef]
- Brauchle, F.; Noack, M.; Reich, E. Impact of periodontal disease and periodontal therapy on oral health-related quality of life. Int. Dent. J. 2013, 63, 306–311. [Google Scholar] [CrossRef]
- Botelho, J.; Machado, V.; Proenca, L.; Bellini, D.H.; Chambrone, L.; Alcoforado, G.; Mendes, J.J. The impact of nonsurgical periodontal treatment on oral health-related quality of life: A systematic review and meta-analysis. Clin. Oral Investig. 2020, 24, 585–596. [Google Scholar] [CrossRef]
- Santuchi, C.C.; Cortelli, J.R.; Cortelli, S.C.; Cota, L.O.; Fonseca, D.C.; Alencar, C.O.; Costa, F.O. Scaling and Root Planing per Quadrant Versus One-Stage Full-Mouth Disinfection: Assessment of the Impact of Chronic Periodontitis Treatment on Quality of Life—A Clinical Randomized, Controlled Trial. J. Periodontol. 2016, 87, 114–123. [Google Scholar] [CrossRef]
- Ozcelik, O.; Haytac, M.C.; Seydaoglu, G. Immediate post-operative effects of different periodontal treatment modalities on oral health-related quality of life: A randomized clinical trial. J. Clin. Periodontol. 2007, 34, 788–796. [Google Scholar] [CrossRef]
- Saito, A.; Hosaka, Y.; Kikuchi, M.; Akamatsu, M.; Fukaya, C.; Matsumoto, S.; Ueshima, F.; Hayakawa, H.; Fujinami, K.; Nakagawa, T. Effect of initial periodontal therapy on oral health-related quality of life in patients with periodontitis in Japan. J. Periodontol. 2010, 81, 1001–1009. [Google Scholar] [CrossRef]
- Saito, A.; Ota, K.; Hosaka, Y.; Akamatsu, M.; Hayakawa, H.; Fukaya, C.; Ida, A.; Fujinami, K.; Sugito, H.; Nakagawa, T. Potential impact of surgical periodontal therapy on oral health-related quality of life in patients with periodontitis: A pilot study. J. Clin. Periodontol. 2011, 38, 1115–1121. [Google Scholar] [CrossRef]
- Theodoridis, C.; Violesti, A.; Nikiforidou, M.; Menexes, G.C.; Vouros, I.D. Short-Term Impact of Non-Surgical and Surgical Periodontal Therapy on Oral Health-Related Quality of Life in a Greek Population-A Prospective Cohort Study. Dent. J. 2020, 8, 54. [Google Scholar] [CrossRef]
- Makino-Oi, A.; Ishii, Y.; Hoshino, T.; Okubo, N.; Sugito, H.; Hosaka, Y.; Fukaya, C.; Nakagawa, T.; Saito, A. Effect of periodontal surgery on oral health-related quality of life in patients who have completed initial periodontal therapy. J. Periodontal Res. 2016, 51, 212–220. [Google Scholar] [CrossRef]
- Ribeiro, L.G.; Antunes, L.S.; Kuchler, E.C.; Baratto-Filho, F.; Kirschneck, C.; Guimaraes, L.S.; Antunes, L.A.A. Impact of malocclusion treatments on Oral Health-Related Quality of Life: An overview of systematic reviews. Clin. Oral Investig. 2023, 27, 907–932. [Google Scholar] [CrossRef]
- Kara-Boulad, J.M.; Burhan, A.S.; Hajeer, M.Y.; Khattab, T.Z.; Nawaya, F.R. Evaluation of the Oral Health-Related Quality of Life (OHRQoL) in Patients Undergoing Lingual Versus Labial Fixed Orthodontic Appliances: A Randomized Controlled Clinical Trial. Cureus 2022, 14, e23379. [Google Scholar] [CrossRef]
- Jonsson, B.; Ohrn, K. Evaluation of the effect of non-surgical periodontal treatment on oral health-related quality of life: Estimation of minimal important differences 1 year after treatment. J. Clin. Periodontol. 2014, 41, 275–282. [Google Scholar] [CrossRef]
- Tsakos, G.; Allen, P.F.; Steele, J.G.; Locker, D. Interpreting oral health-related quality of life data. Community Dent. Oral Epidemiol. 2012, 40, 193–200. [Google Scholar] [CrossRef]
- Gennai, S.; Izzetti, R.; Pioli, M.C.; Music, L.; Graziani, F. Impact of rehabilitation versus edentulism on systemic health and quality of life in patients affected by periodontitis: A systematic review and meta-analysis. J. Clin. Periodontol. 2022, 49 (Suppl. S24), 328–358. [Google Scholar] [CrossRef]
- Hirschfeld, J.; Reichardt, E.; Sharma, P.; Hilber, A.; Meyer-Marcotty, P.; Stellzig-Eisenhauer, A.; Schlagenhauf, U.; Sickel, F.E. Interest in orthodontic tooth alignment in adult patients affected by periodontitis: A questionnaire-based cross-sectional pilot study. J. Periodontol. 2019, 90, 957–965. [Google Scholar] [CrossRef]

| Early OT n = 23 | Late OT n = 20 | Early vs. Late OT | |||||
|---|---|---|---|---|---|---|---|
| BL-12 mo | BL-24 mo | BL-12 mo | BL-24 mo | ∆Change BL-24 mo | |||
| ∆CAL (mean ± SD) | mm | 5.39 ± 2.2 | 5.96 ± 2.10 | 4.45 ± 1.7 | 4.65 ± 1.76 | 1.31 | p = 0.034 |
| Estimate | 95% CI | [6.3, 4.4] | [6.81, 5.10] | [5.3, 3.6] | [5.42, 3.88] | [2.5, 0.1] | |
| ∆PPD (mean ± SD) | mm | 4.21 ± 1.9 | 4.43 ± 1.62 | 3.90 ± 1.5 | 3.90 ± 1.33 | 0.53 | p = 0.248 |
| Estimate | 95% CI | [5.0, 3.4] | [5.1, 3.7] | [4.6, 3.2] | [4.5, 3.3] | [1.46, 0.39] | |
| Variable | Early OT (n = 23) | Late OT (n = 20) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Baseline | 12 mo | 24 mo | BL vs. 24 mo | Baseline | 12 mo | 24 mo | BL vs. 24 mo | ||
| CAL (mean ± SD) | mm | 9.8 ± 2.5 | 4.4 ± 1.7 | 3.9 ±1.9 | p <0.0001 | 9.2 ± 2.5 | 4.7 ± 2.4 | 4.50 ± 2.19 | p < 0.0001 |
| Estimate | 95% CI | [8.8, 10.9] | [3.7, 5.2] | [3.1, 4.7] | [5.0, 6.7] | [8.0, 10.4] | [3.6, 5.8] | [3.5, 5.5] | [3.9, 5.5] |
| PPD (mean ± SD) | mm | 7.3 ± 1.6 | 3.1 ± 0.9 | 2.9 ± 0.9 | p < 0.0001 | 7.1 ± 1.7 | 3.2 ± 1.1 | 3.2 ± 0.9 | p < 0.0001 |
| Estimate | 95% CI | [6.6, 8.0] | [2.7, 3.5] | [2.5, 3.3] | [3.7, 5.1] | [6.3, 7.9] | [2.7, 3.7] | [2.7, 3.6] | [3.1, 5.4] |
| PI | n (%) | 4 (17%) | 3 (13%) | 2 (8%) | 1 (5%) | 2 (10%) | 2 (10%) | ||
| BOP | n (%) | 13 (53%) | 7 (30%) | 4 (17%) | 9 (45%) | 3 (15%) | 0 (0%) | ||
| PUS | n (%) | 1 | 0 | 0 | 2 | 0 | 0 | ||
| Pocket closure (PPD ≤ 4 mm) | n (%) | n/a | 21 (91%) | 21 (91%) | n/a | 17 (85%) | 18 (90%) | ||
| Pocket closure (PPD ≤ 4 mm, no BOP) | n (%) | n/a | 16 (69%) | 18 (78%) | n/a | 15 (75%) | 15 (75%) | ||
| Variables | Early OT (n = 23) | Late OT (n = 20) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Baseline | 6 Months | 12 Months | 24 Months | Baseline | 6 Months | 12 Months | 24 Months | ||
| Orthodontic therapy | Number of patients | ||||||||
| active | n | 23 | 12 | 20 | 17 | 2 | |||
| retention | n | 9 | 5 | 3 | 6 | ||||
| finished | n | 2 | 18 | 0 | 12 | ||||
| Full-mouth plaque scores & bleeding scores | |||||||||
| FMPS * (mean ± SD) | (%) | 12.9 ± 4.9 | 15.0 ± 6 | 16.9 ± 10.1 | 13.2 ± 7.3 | 15.2 ± 6.2 | 15.0 ± 7.0 | 17.1 ± 8.6 | 13.4 ± 6.7 |
| 95% CI | [11, 15] | [12, 18] | [13, 21] | [10, 16] | [12, 18] | [12, 18] | [13, 21] | [10, 16] | |
| FMBS ** (mean ± SD) | (%) | 10.5 ± 4.8 | 10.6 ± 4.9 | 14.7 ± 13.1 | 9.2 ± 8.2 | 12.7 ± 6.8 | 7.7 ± 4.9 | 11.0 ± 9.0 | 7.2 ± 4.1 |
| 95% CI | [8, 13] | [9, 13] | [9, 21] | [5, 13] | [10, 16] | [6, 10] | [7, 15] | [5, 9] | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jepsen, K.; Tietmann, C.; Martin, C.; Kutschera, E.; Jäger, A.; Wüllenweber, P.; Gaveglio, L.; Cardaropoli, D.; Sanz-Sánchez, I.; Fimmers, R.; et al. Synergy of Regenerative Periodontal Surgery and Orthodontics Improves Quality of Life of Patients with Stage IV Periodontitis: 24-Month Outcomes of a Multicenter RCT. Bioengineering 2023, 10, 695. https://doi.org/10.3390/bioengineering10060695
Jepsen K, Tietmann C, Martin C, Kutschera E, Jäger A, Wüllenweber P, Gaveglio L, Cardaropoli D, Sanz-Sánchez I, Fimmers R, et al. Synergy of Regenerative Periodontal Surgery and Orthodontics Improves Quality of Life of Patients with Stage IV Periodontitis: 24-Month Outcomes of a Multicenter RCT. Bioengineering. 2023; 10(6):695. https://doi.org/10.3390/bioengineering10060695
Chicago/Turabian StyleJepsen, Karin, Christina Tietmann, Conchita Martin, Eric Kutschera, Andreas Jäger, Peter Wüllenweber, Lorena Gaveglio, Daniele Cardaropoli, Ignacio Sanz-Sánchez, Rolf Fimmers, and et al. 2023. "Synergy of Regenerative Periodontal Surgery and Orthodontics Improves Quality of Life of Patients with Stage IV Periodontitis: 24-Month Outcomes of a Multicenter RCT" Bioengineering 10, no. 6: 695. https://doi.org/10.3390/bioengineering10060695
APA StyleJepsen, K., Tietmann, C., Martin, C., Kutschera, E., Jäger, A., Wüllenweber, P., Gaveglio, L., Cardaropoli, D., Sanz-Sánchez, I., Fimmers, R., & Jepsen, S. (2023). Synergy of Regenerative Periodontal Surgery and Orthodontics Improves Quality of Life of Patients with Stage IV Periodontitis: 24-Month Outcomes of a Multicenter RCT. Bioengineering, 10(6), 695. https://doi.org/10.3390/bioengineering10060695








