Oral Manifestations of Inflammatory Bowel Disease and the Role of Non-Invasive Surrogate Markers of Disease Activity
Abstract
1. Introduction
2. Oral Lesions in Patients with IBD
3. Specific Oral Lesions
3.1. Clinical Characteristics
3.2. Diagnosis
4. Non-Specific Oral Lesions
5. Malignant Oral Manifestations
6. Diagnosis of IBD in Patients with Oral Manifestation
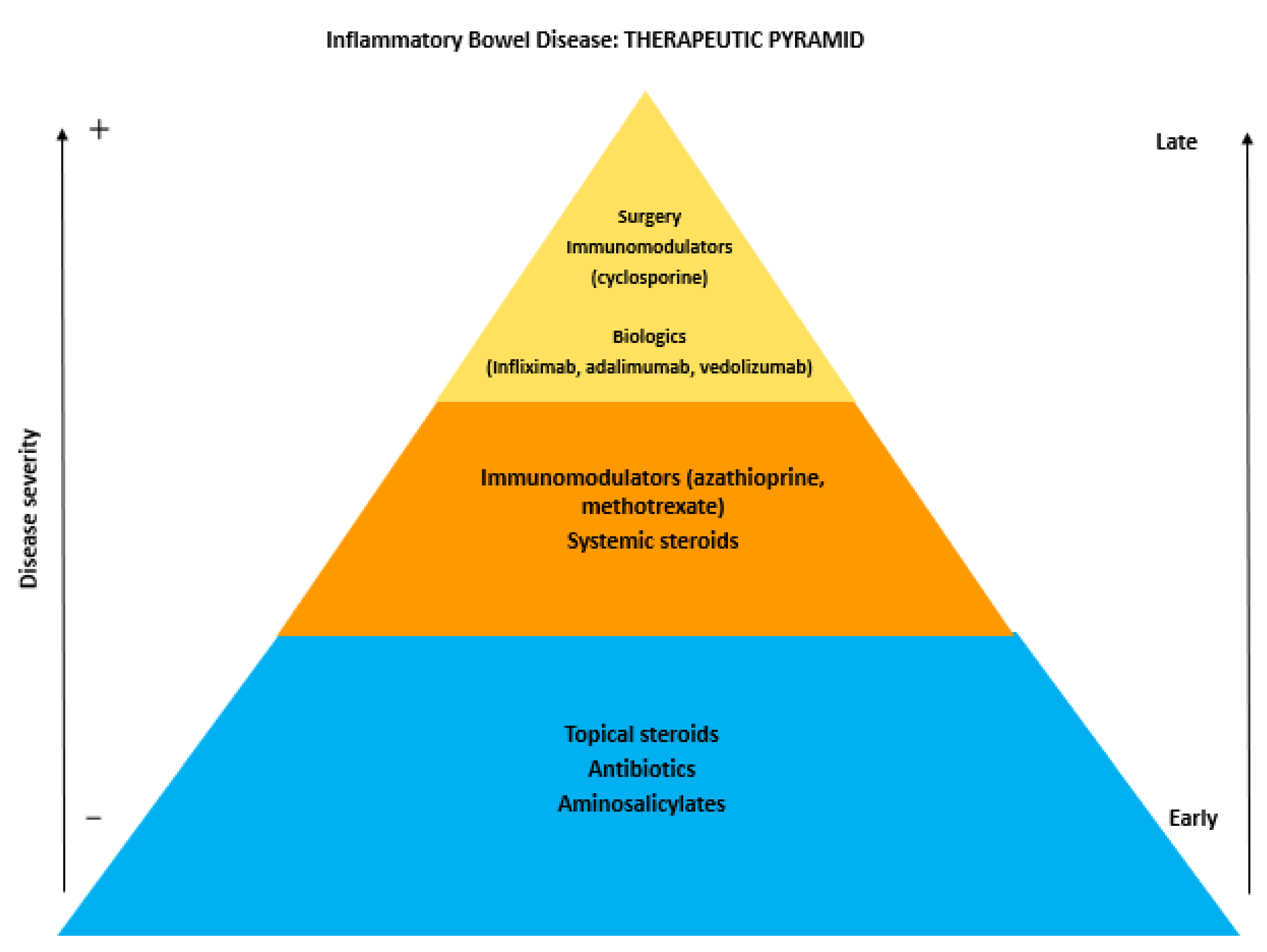
7. Treatment of Oral Manifestations in Patients with IBD
8. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Abraham, C.; Cho, J.H. Inflammatory bowel disease. N. Engl. J. Med. 2009, 361, 2066–2078. [Google Scholar] [CrossRef]
- Sands, B.E. From symptom to diagnosis: Clinical distinctions among various forms of intestinal inflammation. Gastroenterology 2004, 126, 1518–1532. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, C.N.; Blanchard, J.F.; Rawsthorne, P.; Yu, N. The Prevalence of Extraintestinal Diseases in Inflammatory Bowel Disease: A Population-Based Study. Am. J. Gastroenterol. 2001, 96, 1116–1122. [Google Scholar] [CrossRef] [PubMed]
- Ribaldone, D.G.; Pellicano, R.; Actis, G.C. The gut and the Inflammatory Bowel Diseases inside-out: The extra-intestinal manifestations. Minerva Gastroenterol. Dietol. 2019. [Google Scholar] [CrossRef]
- Su, C.G.; Judge, T.A.; Lichtenstein, G.R. Extraintestinal manifestations of inflammatory bowel disease. Gastroenterol. Clin. North Am. 2002, 31, 307–327. [Google Scholar] [CrossRef]
- Adriani, A.; Pantaleoni, S.; Luchino, M.; Ribaldone, D.G.; Reggiani, S.; Sapone, N.; Sguazzini, C.; Isaia, G.; Pellicano, R.; Astegiano, M. Osteopenia and osteoporosis in patients with new diagnosis of inflammatory bowel disease. Panminerva Med. 2014, 56, 145–149. [Google Scholar] [PubMed]
- Colìa, R.; D’Onofrio, F.; Cantatore, F.P. Ulcerative colitis and systemic lupus erythematosus. Minerva Med. 2013, 104, 579–581. [Google Scholar]
- Hugot, J.-P.; Chamaillard, M.; Zouali, H.; Lesage, S.; Cézard, J.-P.; Belaiche, J.; Almer, S.; Tysk, C.; O’Morain, C.A.; Gassull, M.; et al. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn’s disease. Nature 2001, 411, 599–603. [Google Scholar] [CrossRef]
- Silverberg, M.S.; Mirea, L.; Bull, S.B.; Murphy, J.E.; Steinhart, A.H.; Greenberg, G.R.; McLeod, R.S.; Cohen, Z.; Wade, J.A.; Siminovitch, K.A. A population- and family-based study of Canadian families reveals association of HLA DRB1*0103 with colonic involvement in inflammatory bowel disease. Inflamm. Bowel Dis. 2003, 9, 1–9. [Google Scholar] [CrossRef]
- Langmann, T.; Moehle, C.; Mauerer, R.; Scharl, M.; Liebisch, G.; Zahn, A.; Stremmel, W.; Schmitz, G. Loss of detoxification in inflammatory bowel disease: Dysregulation of pregnane X receptor target genes. Gastroenterology 2004, 127, 26–40. [Google Scholar] [CrossRef]
- Caviglia, G.P.; Rosso, C.; Stalla, F.; Rizzo, M.; Massano, A.; Abate, M.L.; Olivero, A.; Armandi, A.; Vanni, E.; Younes, R.; et al. On-Treatment Decrease of Serum Interleukin-6 as a Predictor of Clinical Response to Biologic Therapy in Patients with Inflammatory Bowel Diseases. J. Clin. Med. 2020, 9, 800. [Google Scholar] [CrossRef] [PubMed]
- Mari, A.; Abu Baker, F.; Mahamid, M.; Sbeit, W.; Khoury, T. The Evolving Role of Gut Microbiota in the Management of Irritable Bowel Syndrome: An Overview of the Current Knowledge. J. Clin. Med. 2020, 9, 685. [Google Scholar] [CrossRef] [PubMed]
- Ardizzone, S.; Puttini, P.S.; Cassinotti, A.; Porro, G.B. Extraintestinal manifestations of inflammatory bowel disease. Dig. Liver Dis. 2008, 40, S253–S259. [Google Scholar] [CrossRef]
- Dudeney, T.P. Crohn’s disease of the mouth. Proc. R. Soc. Med. 1969, 62, 1237. [Google Scholar] [CrossRef] [PubMed]
- Katsanos, K.H.; Torres, J.; Roda, G.; Brygo, A.; Delaporte, E.; Colombel, J.F. Review article: Non-malignant oral manifestations in inflammatory bowel diseases. Aliment. Pharmacol. Ther. 2015, 42, 40–60. [Google Scholar] [CrossRef]
- Pittock, S.; Drumm, B.; Fleming, P.; McDermott, M.; Imrie, C.; Flint, S.; Bourke, B. The oral cavity in Crohn’s disease. J. Pediatr. 2001, 138, 767–771. [Google Scholar] [CrossRef]
- Lenaerts, C.; Roy, C.C.; Vaillancourt, M.; Weber, A.M.; Morin, C.L.; Seidman, E. High incidence of upper gastrointestinal tract involvement in children with Crohn disease. Pediatrics 1989. [Google Scholar] [CrossRef]
- Dupuy, A.; Cosnes, J.; Revuz, J.; Delchier, J.C.; Gendre, J.P.; Cosnes, A. Oral Crohn disease: Clinical characteristics and long-term follow-up of 9 cases. Arch. Dermatol. 1999. [Google Scholar] [CrossRef]
- Lauritano, D.; Boccalari, E.; Di Stasio, D.; Della Vella, F.; Carinci, F.; Lucchese, A.; Petruzzi, M. Prevalence of oral lesions and correlation with intestinal symptoms of inflammatory bowel disease: A systematic review. Diagnostics 2019, 9, 77. [Google Scholar] [CrossRef]
- Harty, S.; Fleming, P.; Rowland, M.; Crushell, E.; McDermott, M.; Drumm, B.; Bourke, B. A prospective study of the oral manifestations of Crohn’s disease. Clin. Gastroenterol. Hepatol. 2005. [Google Scholar] [CrossRef]
- Vasovic, M.; Gajovic, N.; Brajkovic, D.; Jovanovic, M.; Zdravkovaic, N.; Kanjevac, T. The relationship between the immune system and oral manifestations of inflammatory bowel disease: A review. Cent. Eur. J. Immunol. 2016, 41, 302–310. [Google Scholar] [CrossRef] [PubMed]
- Rehberger, A.; Püspök, A.; Stallmeister, T.; Jurecka, W.; Wolff, K. Crohn’s disease masquerading as aphthous ulcers. Eur. J. Dermatol. 1998, 8, 274–276. [Google Scholar] [PubMed]
- Laranjeira, N.; Fonseca, J.; Meira, T.; Freitas, J.; Valido, S.; Leitão, J. Oral mucosa lesions and oral symptoms in inflammatory bowel disease patients. Arq. Gastroenterol. 2015, 52, 105–110. [Google Scholar] [CrossRef] [PubMed]
- Lourenco, S.V.; Hussein, T.P.; Bologna, S.B.; Sipahi, A.M.; Nico, M.M. Oral manifestations of inflammatory bowel disease: A review based on the observation of six cases. J. Eur. Acad. Dermatol. Venereol. 2010, 24, 204–207. [Google Scholar] [CrossRef]
- Said, H.S.; Suda, W.; Nakagome, S.; Chinen, H.; Oshima, K.; Kim, S.; Kimura, R.; Iraha, A.; Ishida, H.; Fujita, J.; et al. Dysbiosis of salivary microbiota in inflammatory bowel disease and its association with oral immunological biomarkers. DNA Res. 2014, 21, 15–25. [Google Scholar] [CrossRef]
- Muhvić-Urek, M.; Tomac-Stojmenović, M.; Mijandrušić-Sinčić, B. Oral pathology in inflammatory bowel disease. World J. Gastroenterol. 2016, 22, 5655–5667. [Google Scholar] [CrossRef]
- Gale, G.; Sigurdsson, G.V.; Östman, S.; Malmborg, P.; Högkil, K.; Hasséus, B.; Jontell, M.; Saalman, R. Does Crohn’s Disease with Concomitant Orofacial Granulomatosis Represent a Distinctive Disease Subtype? Inflamm. Bowel Dis. 2016, 22, 1071–1077. [Google Scholar] [CrossRef]
- Halme, L.; Meurman, J.H.; Laine, P.; von Smitten, K.; Syrjänen, S.; Lindqvist, C.; Strand-Pettinen, I. Oral findings in patients with active or inactive Crohn’s disease. Oral Surg. Oral Med. Oral Pathol. 1993. [Google Scholar] [CrossRef]
- Fatahzadeh, M.; Schwartz, R.A.; Kapila, R.; Rochford, C. Orofacial Crohn’s disease: An oral enigma. Acta Dermatovenerol. Croat. 2009, 17, 289–300. [Google Scholar]
- Gibson, J.; Wray, D.; Bagg, J. Oral staphylococcal mucositis: A new clinical entity in or ofacial granulomatosisand Crohn’s disease. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2000. [Google Scholar] [CrossRef]
- Nagpal, S.; Acharya, A.B.; Thakur, S.L. Periodontal disease and anemias associated with Crohn’s disease. A case report. N. Y. State Dent. J. 2012, 78, 47–50. [Google Scholar]
- Turchi, R.M.; Soriano, H.; Rodgers, G.L. Tb or not Tb: Crohn’s disease presenting with tonsillar granulomas. Otolaryngol. Head Neck Surg. 2006, 134, 528–530. [Google Scholar] [CrossRef] [PubMed]
- Katz, J.; Shenkman, A.; Stavropoulos, F.; Melzer, E. Oral signs and symptoms in relation to disease activity and site of involvement in patients with inflammatory bowel disease. Oral Dis. 2003. [Google Scholar] [CrossRef] [PubMed]
- Trikudanathan, G.; Venkatesh, P.G.K.; Navaneethan, U. Diagnosis and therapeutic management of extra-intestinal manifestations of inflammatory bowel disease. Drugs 2012, 72, 2333–2349. [Google Scholar] [CrossRef] [PubMed]
- Rogers, R.S.; Bekic, M. Diseases of the lips. Semin. Cutan. Med. Surg. 1997, 16, 328–336. [Google Scholar] [CrossRef]
- Mijandrusic-Sincic, B.; Licul, V.; Gorup, L.; Brnčić, N.; Glažar, I.; Lučin, K. Pyostomatitis vegetans associated with inflammatory bowel disease—Report of two cases. Coll. Antropol. 2010, 34, 279–282. [Google Scholar]
- Atarbashi-Moghadam, S.; Lotfi, A.; Atarbashi-Moghadam, F. Pyostomatitis Vegetans: A Clue for Diagnosis of Silent Crohn’s Disease. J. Clin. Diagn. Res. 2016, 10, ZD12–ZD13. [Google Scholar] [CrossRef]
- Correll, R.W.; Wescott, W.B.; Jensen, J.L. Recurring, painful oral ulcers. J. Am. Dent. Assoc. 1981. [Google Scholar] [CrossRef]
- Femiano, F.; Lanza, A.; Buonaiuto, C.; Perillo, L.; Dell’Ermo, A.; Cirillo, N. Pyostomatitis vegetans: A review of the literature. Med. Oral Patol. Oral Cir. Bucal 2009, 14, E114–E117. [Google Scholar]
- Markopoulos, A.K.; Antoniades, D.Z.; Gaga, E. Pyostomatitis Vegetans as an Oral Manifestation of Ulcerative Colitis: Report of Two Cases. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endodontology 2005. [Google Scholar] [CrossRef]
- Papageorgiou, S.N.; Hagner, M.; Nogueira, A.V.B.; Franke, A.; Jäger, A.; Deschner, J. Inflammatory bowel disease and oral health: Systematic review and a meta-analysis. J. Clin. Periodontol. 2017, 44, 382–393. [Google Scholar] [CrossRef] [PubMed]
- Habashneh, R.A.; Khader, Y.S.; Alhumouz, M.K.; Jadallah, K.; Ajlouni, Y. The association between inflammatory bowel disease and periodontitis among Jordanians: A case-control study. J. Periodont. Res. 2012, 47, 293–298. [Google Scholar] [CrossRef] [PubMed]
- Figueredo, C.M.; Brito, F.; Barros, F.C.; Menegat, J.S.B.; Pedreira, R.R.; Fischer, R.G.; Gustafsson, A. Expression of cytokines in the gingival crevicular fluid and serum from patients with inflammatory bowel disease and untreated chronic periodontitis. J. Periodont. Res. 2011, 46, 141–146. [Google Scholar] [CrossRef] [PubMed]
- Lira-Junior, R.; Figueredo, C.M. Periodontal and inflammatory bowel diseases: Is there evidence of complex pathogenic interactions? World J. Gastroenterol. 2016, 22, 7963–7972. [Google Scholar] [CrossRef]
- Kabbani, T.A.; Koutroubakis, I.E.; Schoen, R.E.; Ramos-Rivers, C.; Shah, N.; Swoger, J.; Regueiro, M.; Barrie, A.; Schwartz, M.; Hashash, J.G.; et al. Association of Vitamin D level with clinical status in inflammatory bowel disease: A 5-year longitudinal study. Am. J. Gastroenterol. 2016. [Google Scholar] [CrossRef]
- Schroth, R.J.; Rabbani, R.; Loewen, G.; Moffatt, M.E. Vitamin D and Dental Caries in Children. J. Dent. Res. 2016. [Google Scholar] [CrossRef]
- Rowland, M.; Fleming, P.; Bourke, B. Looking in the mouth for Crohn’s disease. Inflamm. Bowel Dis. 2010, 16, 332–337. [Google Scholar] [CrossRef]
- Campisi, G.; Giovannelli, L. Controversies surrounding human papilloma virus infection, head & neck vs oral cancer, implications for prophylaxis and treatment. Head Neck Oncol. 2009, 1, 8. [Google Scholar] [CrossRef]
- Vial, T.; Descotes, J. Immunosuppressive drugs and cancer. Toxicology 2003, 185, 229–240. [Google Scholar] [CrossRef]
- Katsanos, K.H.; Roda, G.; Brygo, A.; Delaporte, E.; Colombel, J.F. Oral cancer and oral precancerous lesions in inflammatory bowel diseases: A systematic review. J. Crohn’s Colitis 2015, 9, 1043–1052. [Google Scholar] [CrossRef]
- Mowat, C.; Cole, A.; Windsor, A.; Ahmad, T.; Arnott, I.; Driscoll, R.; Mitton, S.; Orchard, T.; Rutter, M.; Younge, L.; et al. Guidelines for the management of inflammatory bowel disease in adults. Gut 2011, 60, 571–607. [Google Scholar] [CrossRef] [PubMed]
- Cammarota, T.; Ribaldone, D.G.; Resegotti, A.; Repici, A.; Danese, S.; Fiorino, G.; Sarno, A.; Robotti, D.; Debani, P.; Bonenti, G.; et al. Role of bowel ultrasound as a predictor of surgical recurrence of Crohn’s disease. Scand. J. Gastroenterol. 2013, 48. [Google Scholar] [CrossRef] [PubMed]
- Sarno, A.; Varello, S.; Debani, P.; Bonenti, G.; Robotti, D. Intestinal ultrasonography in adults with Crohn’s disease: A 2020 update. Minerva Gastroenterol. Dietol. 2019, 65, 335–345. [Google Scholar] [CrossRef]
- Gatti, M.; Allois, L.; Carisio, A.; Dianzani, C.; Garcia Martinez, M.; Ruggirello, I.; Varello, S.; Darvizeh, F.; Faletti, R. Magnetic resonance enterography. Minerva Gastroenterol. Dietol. 2019, 65, 319–334. [Google Scholar] [CrossRef] [PubMed]
- Panés, J.; Bouzas, R.; Chaparro, M.; García-Sánchez, V.; Gisbert, J.P.; Martínez de Guereñu, B.; Mendoza, J.L.; Paredes, J.M.; Quiroga, S.; Ripollés, T.; et al. Systematic review: The use of ultrasonography, computed tomography and magnetic resonance imaging for the diagnosis, assessment of activity and abdominal complications of Crohn’s disease. Aliment. Pharmacol. Ther. 2011, 34, 125–145. [Google Scholar] [CrossRef]
- Kallenberg, C.G.M.; Heeringa, P.; Stegeman, C.A. Mechanisms of disease: Pathogenesis and treatment of ANCA-associated vasculitides. Nat. Clin. Pract. Rheumatol. 2006, 2, 661–670. [Google Scholar] [CrossRef]
- Papp, M.; Norman, G.L.; Altorjay, I.; Lakatos, P.L. Utility of serological markers in inflammatory bowel diseases: gadget or magic? World J. Gastroenterol. 2007, 13, 2028–2036. [Google Scholar] [CrossRef]
- Gao, X.; Hu, P.; He, Y.; Liao, S.; Peng, S.; Chen, M. Diagnostic role of anti-saccharomyces cerevisiae and antineutrophil cytoplasmic autoantibodies in inflammatory bowel disease. Zhonghua Nei Ke Za Zhi 2005, 44, 428–430. [Google Scholar] [CrossRef]
- Sandborn, W.J.; Loftus, E.V.; Colombel, J.F.; Fleming, K.A.; Seibold, F.; Homburger, H.A.; Sendid, B.; Chapman, R.W.; Tremaine, W.J.; Kaul, D.K.; et al. Evaluation of serologic disease markers in a population-based cohort of patients with ulcerative colitis and Crohn’s disease. Inflamm. Bowel Dis. 2001, 7, 192–201. [Google Scholar] [CrossRef]
- Simondi, D.; Mengozzi, G.; Betteto, S.; Bonardi, R.; Ghignone, R.P.; Fagoonee, S.; Pellicano, R.; Sguazzini, C.; Pagni, R.; Rizzetto, M.; et al. Antiglycan antibodies as serological markers in the differential diagnosis of inflammatory bowel disease. Inflamm. Bowel Dis. 2008, 14, 645–651. [Google Scholar] [CrossRef]
- Malickova, K.; Lakatos, P.L.; Bortlik, M.; Komarek, V.; Janatkova, I.; Lukas, M. Anticarbohydrate antibodies as markers of inflammatory bowel disease in a Central European cohort. Eur. J. Gastroenterol. Hepatol. 2010. [Google Scholar] [CrossRef] [PubMed]
- Amcoff, K.; Joossens, M.; Pierik, M.J.; Jonkers, D.; Bohr, J.; Joossens, S.; Romberg-Camps, M.; Nyhlin, N.; Wickbom, A.; Rutgeerts, P.J.; et al. Concordance in Anti-OmpC and Anti-I2 Indicate the Influence of Genetic Predisposition: Results of a European Study of Twins with Crohn’s Disease. J. Crohns. Colitis 2016, 10, 695–702. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Caviglia, G.P.; Ribaldone, D.G.; Rosso, C.; Saracco, G.M.; Astegiano, M.; Pellicano, R. Fecal calprotectin: Beyond intestinal organic diseases. Panminerva Med. 2018, 60, 29–34. [Google Scholar] [CrossRef] [PubMed]
- Berntzen, H.B.; Fagerhol, M.K. L1, a major granulocyte protein: Antigenic properties of its subunits. Scand. J. Clin. Lab. Invest. 1988, 48, 647–652. [Google Scholar] [CrossRef]
- Foell, D.; Wittkowski, H.; Roth, J. Monitoring disease activity by stool analyses: From occult blood to molecular markers of intestinal inflammation and damage. Gut 2009, 58, 859–868. [Google Scholar] [CrossRef]
- Voganatsi, A.; Panyutich, A.; Miyasaki, K.T.; Murthy, R.K. Mechanism of extracellular release of human neutrophil calprotectin complex. J. Leukoc. Biol. 2001. [Google Scholar] [CrossRef]
- Burri, E.; Beglinger, C. Faecal calprotectin in the diagnosis of inflammatory bowel disease. Biochem. Med. 2011, 245–253. [Google Scholar] [CrossRef]
- Sydora, M.J.; Sydora, B.C.; Fedorak, R.N. Validation of a point-of-care desk top device to quantitate fecal calprotectin and distinguish inflammatory bowel disease from irritable bowel syndrome. J. Crohns. Colitis 2012, 6, 207–214. [Google Scholar] [CrossRef]
- Koulaouzidis, A.; Douglas, S.; Rogers, M.A.; Arnott, I.D.; Plevris, J.N. Fecal calprotectin: A selection tool for small bowel capsule endoscopy in suspected IBD with prior negative bi-directional endoscopy. Scand. J. Gastroenterol. 2011, 46, 561–566. [Google Scholar] [CrossRef]
- Wright, E.K. Calprotectin or Lactoferrin: Do They Help. Dig. Dis. 2016, 34, 98–104. [Google Scholar] [CrossRef]
- Ojha, J.; Cohen, D.M.; Islam, N.M.; Stewart, C.M.; Katz, J.; Bhattacharyya, I. Gingival involvement in Crohn disease. J. Am. Dent. Assoc. 2007. [Google Scholar] [CrossRef] [PubMed]
- Zbar, A.P.; Ben-Horin, S.; Beer-Gabel, M.; Eliakim, R. Oral Crohn’s disease: Is it a separable disease from orofacial granulomatosis? A review. J. Crohns. Colitis 2012, 6, 135–142. [Google Scholar] [CrossRef] [PubMed]
- Bishop, R.P.; Brewster, A.C.; Antonioli, D.A. Crohn’s disease of the mouth. Gastroenterology 1972, 62, 302–306. [Google Scholar] [CrossRef]
- Bradley, P.J.; Ferlito, A.; Devaney, K.O.; Rinaldo, A. Crohn’s disease manifesting in the head and neck. Acta Otolaryngol. 2004, 124, 237–241. [Google Scholar] [CrossRef]
- Khouri, J.M.; Bohane, T.D.; Day, A.S. Is orofacial granulomatosis in children a feature of Crohn’s disease? Acta Paediatr. Int. J. Paediatr. 2005. [Google Scholar] [CrossRef]
| Lesion | Location | Features |
|---|---|---|
| Cobblestoning | Posterior buccal mucosa | Fissured swollen mucosa with corrugation and hyperplastic |
| Indurated tag-like lesions | Labial and buccal vestibules; retromolar region | Hyperplastic edge firm or boggy |
| Mucogingivitis | Whole gingiva | Gingiva edematous, granular and hyperplastic |
| Others: Lip swelling with vertical fissures Deep linear ulceration Edema of the face | Lips, tongue, buccal sulci, face |
| Lesion | Location | Features |
|---|---|---|
| Aphtous stomatitis | Anywhere in the oral cavity | Shallow round ulcerations with central fibrinous exudate surrounded by an erythematous border |
| Pyostomatitis vegetans | Labial gingiva, buccal and labial mucosa; less common: tongue, soft and hard palate | Erythematous and thickened oral mucosa with multiple pustules and superficial erosions |
| Angular cheilitis | Corner of the oral cavity | Erythema at the corners of the mouth with or without painful fissures and sores |
| Others: Glossitis Periodontitis and dental caries Perioral dermatitis Recurrent buccal abscesses Submandibolar lymphoadenopathy Salivary duct fistula | Oral mucosa, gingiva, tongue, teeth, periodontal tissue, alveolar bone, perioral skin, palate, lips, lymph nodes, salivary glands |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ribaldone, D.G.; Brigo, S.; Mangia, M.; Saracco, G.M.; Astegiano, M.; Pellicano, R. Oral Manifestations of Inflammatory Bowel Disease and the Role of Non-Invasive Surrogate Markers of Disease Activity. Medicines 2020, 7, 33. https://doi.org/10.3390/medicines7060033
Ribaldone DG, Brigo S, Mangia M, Saracco GM, Astegiano M, Pellicano R. Oral Manifestations of Inflammatory Bowel Disease and the Role of Non-Invasive Surrogate Markers of Disease Activity. Medicines. 2020; 7(6):33. https://doi.org/10.3390/medicines7060033
Chicago/Turabian StyleRibaldone, Davide Giuseppe, Selvaggia Brigo, Michela Mangia, Giorgio Maria Saracco, Marco Astegiano, and Rinaldo Pellicano. 2020. "Oral Manifestations of Inflammatory Bowel Disease and the Role of Non-Invasive Surrogate Markers of Disease Activity" Medicines 7, no. 6: 33. https://doi.org/10.3390/medicines7060033
APA StyleRibaldone, D. G., Brigo, S., Mangia, M., Saracco, G. M., Astegiano, M., & Pellicano, R. (2020). Oral Manifestations of Inflammatory Bowel Disease and the Role of Non-Invasive Surrogate Markers of Disease Activity. Medicines, 7(6), 33. https://doi.org/10.3390/medicines7060033







