Evaluation of Two Shaping Systems and Two Ultrasonic Irrigation Devices in Removing Root Canal Filling Material from Mesial Roots of Mandibular Molars: A Micro CT Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample Selection
2.2. Initial Preparation and Obturation
2.3. Pre-Retreatment Micro-CT Imaging
2.4. Retreatment Procedures
2.5. Post Retreatment Micro-CT Imaging
2.6. Supplementary Approach Using Passive Ultrasonic Irrigation
- (1)
- Group A: TS2 retreatment with the Endo Ultra PUI
- (2)
- Group B: TS2 retreatment with the Irrisafe PUI
- (3)
- Group C: R25 retreatment with the Endo Ultra PUI
- (4)
- Group D: R25 retreatment with the Irrisafe PUI
2.7. Post PUI Micro-CT Imaging
2.8. Micro-CT Analysis
2.9. Statistical Analysis
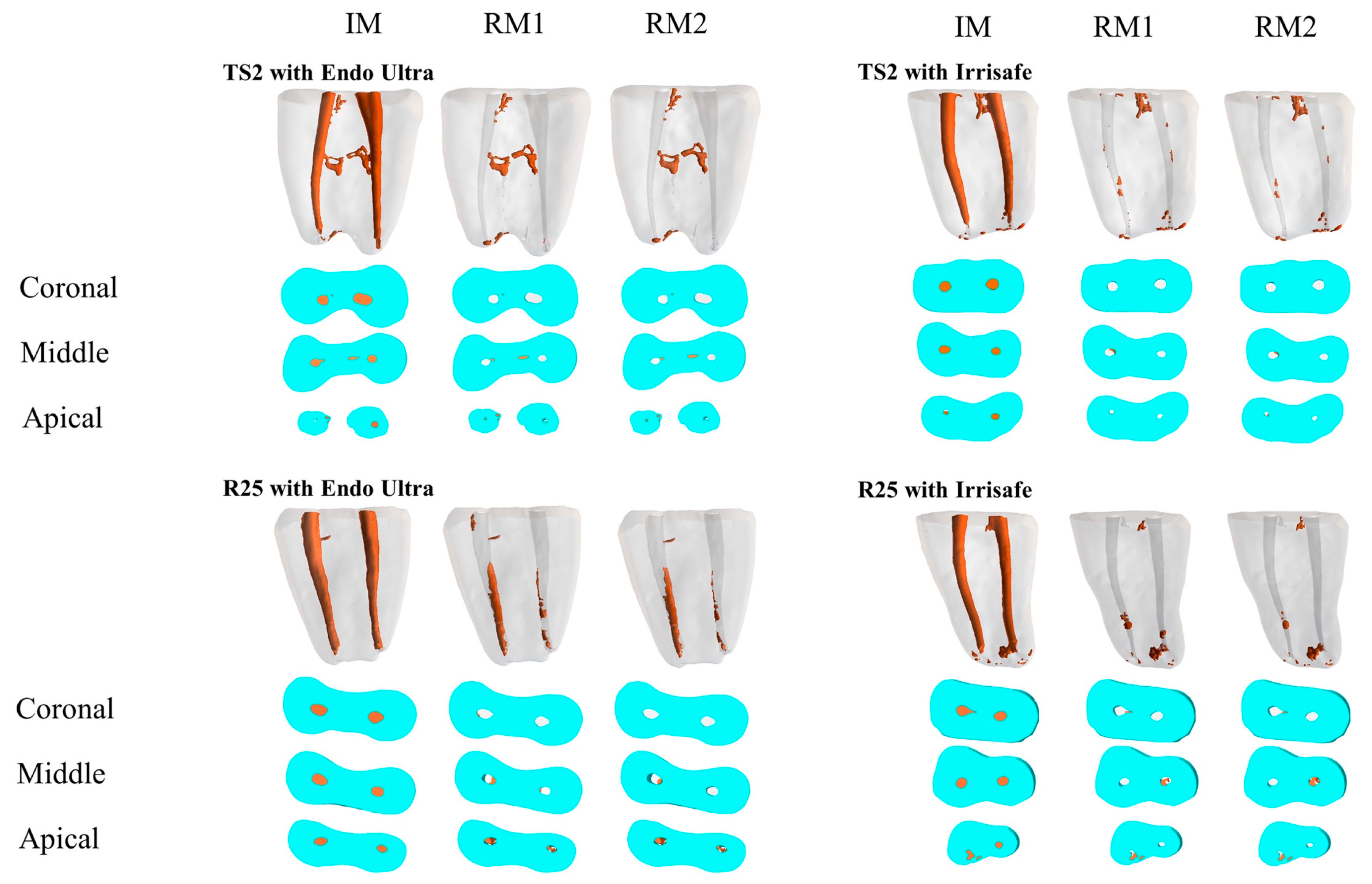
3. Results
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Kang, M.; In Jung, H.; Song, M.; Kim, S.Y.; Kim, H.C.; Kim, E. Outcome of nonsurgical retreatment and endodontic microsurgery: A meta-analysis. Clin. Oral Investig. 2015, 19, 569–582. [Google Scholar] [CrossRef] [PubMed]
- Hülsmann, M.; Drebenstedt, S.; Holscher, C. Shaping and filling root canals during root canal re-treatment. Endod. Top. 2011, 19, 74–124. [Google Scholar] [CrossRef]
- Kvist, T.; Reit, C. The perceived benefit of endodontic retreatment. Int. Endod. J. 2002, 35, 359–365. [Google Scholar] [CrossRef] [PubMed]
- Olcay, K.; Ataoglu, H.; Belli, S. Evaluation of Related Factors in the Failure of Endodontically Treated Teeth: A Cross-sectional Study. J. Endod. 2018, 44, 38–45. [Google Scholar] [CrossRef] [PubMed]
- Ozyurek, T.; Demiryurek, E.O. Efficacy of Different Nickel-Titanium Instruments in Removing Gutta-percha during Root Canal Retreatment. J. Endod. 2016, 42, 646–649. [Google Scholar] [CrossRef] [PubMed]
- Topcuoglu, H.S.; Akti, A.; Tuncay, O.; Dincer, A.N.; Duzgun, S.; Topcuoglu, G. Evaluation of debris extruded apically during the removal of root canal filling material using ProTaper, D-RaCe, and R-Endo rotary nickel-titanium retreatment instruments and hand files. J. Endod. 2014, 40, 2066–2069. [Google Scholar] [CrossRef] [PubMed]
- Crozeta, B.M.; Silva-Sousa, Y.T.; Leoni, G.B.; Mazzi-Chaves, J.F.; Fantinato, T.; Baratto-Filho, F.; Sousa-Neto, M.D. Micro-Computed Tomography Study of Filling Material Removal from Oval-shaped Canals by Using Rotary, Reciprocating, and Adaptive Motion Systems. J. Endod. 2016, 42, 793–797. [Google Scholar] [CrossRef] [PubMed]
- Yilmaz, F.; Koc, C.; Kamburoglu, K.; Ocak, M.; Geneci, F.; Uzuner, M.B.; Celik, H.H. Evaluation of 3 Different Retreatment Techniques in Maxillary Molar Teeth by Using Micro-computed Tomography. J. Endod. 2018, 44, 480–484. [Google Scholar] [CrossRef]
- Rios Mde, A.; Villela, A.M.; Cunha, R.S.; Velasco, R.C.; De Martin, A.S.; Kato, A.S.; Bueno, C.E. Efficacy of 2 reciprocating systems compared with a rotary retreatment system for gutta-percha removal. J. Endod. 2014, 40, 543–546. [Google Scholar] [CrossRef]
- Ma, J.; Al-Ashaw, A.J.; Shen, Y.; Gao, Y.; Yang, Y.; Zhang, C.; Haapasalo, M. Efficacy of ProTaper Universal Rotary Retreatment system for gutta-percha removal from oval root canals: A micro-computed tomography study. J. Endod. 2012, 38, 1516–1520. [Google Scholar] [CrossRef]
- Silveira, S.B.; Alves, F.R.F.; Marceliano-Alves, M.F.; Sousa, J.C.N.; Vieira, V.T.L.; Siqueira, J.F., Jr.; Lopes, H.P.; Provenzano, J.C. Removal of Root Canal Fillings in Curved Canals Using Either Mani GPR or HyFlex NT Followed by Passive Ultrasonic Irrigation. J. Endod. 2018, 44, 299.e1–303.e1. [Google Scholar] [CrossRef] [PubMed]
- Martins, M.P.; Duarte, M.A.; Cavenago, B.C.; Kato, A.S.; da Silveira Bueno, C.E. Effectiveness of the ProTaper Next and Reciproc Systems in Removing Root Canal Filling Material with Sonic or Ultrasonic Irrigation: A Micro-computed Tomographic Study. J. Endod. 2017, 43, 467–471. [Google Scholar] [CrossRef] [PubMed]
- Generali, L.; Cavani, F.; Serena, V.; Pettenati, C.; Righi, E.; Bertoldi, C. Effect of Different Irrigation Systems on Sealer Penetration into Dentinal Tubules. J. Endod. 2017, 43, 652–656. [Google Scholar] [CrossRef] [PubMed]
- Boutsioukis, C.; Verhaagen, B.; Walmsley, A.D.; Versluis, M.; van der Sluis, L.W. Measurement and visualization of file-to-wall contact during ultrasonically activated irrigation in simulated canals. Int. Endod. J. 2013, 46, 1046–1055. [Google Scholar] [CrossRef] [PubMed]
- Schneider, S.W. A comparison of canal preparations in straight and curved root canals. Oral Surg. Oral Med. Oral Pathol. 1971, 32, 271–275. [Google Scholar] [CrossRef]
- Vertucci, F.J. Root canal anatomy of the human permanent teeth. Oral Surg. Oral Med. Oral Pathol. 1984, 58, 589–599. [Google Scholar] [CrossRef]
- Ataya, M.; Ha, J.H.; Kwak, S.W.; Abu-Tahun, I.H.; El Abed, R.; Kim, H.C. Mechanical Properties of Orifice Preflaring Nickel-titanium Rotary Instrument Heat Treated Using T-Wire Technology. J. Endod. 2018, 44, 1867–1871. [Google Scholar] [CrossRef] [PubMed]
- Otsu, N. A Threshold Selection Method from Gray-Level Histograms. IEEE Trans. Syst. Man Cybern. 1979, 9, 62–66. [Google Scholar] [CrossRef]
- Michetti, J.; Basarab, A.; Diemer, F.; Kouame, D. Comparison of an adaptive local thresholding method on CBCT and microCT endodontic images. Phys. Med. Biol. 2017, 63, 015020. [Google Scholar] [CrossRef]
- Nevares, G.; de Albuquerque, D.S.; Freire, L.G.; Romeiro, K.; Fogel, H.M.; Dos Santos, M.; Cunha, R.S. Efficacy of ProTaper NEXT Compared with Reciproc in Removing Obturation Material from Severely Curved Root Canals: A Micro-Computed Tomography Study. J. Endod. 2016, 42, 803–808. [Google Scholar] [CrossRef]
- Bernardes, R.A.; Duarte, M.A.H.; Vivan, R.R.; Alcalde, M.P.; Vasconcelos, B.C.; Bramante, C.M. Comparison of three retreatment techniques with ultrasonic activation in flattened canals using micro-computed tomography and scanning electron microscopy. Int. Endod. J. 2016, 49, 890–897. [Google Scholar] [CrossRef] [PubMed]
- Fruchi Lde, C.; Ordinola-Zapata, R.; Cavenago, B.C.; Hungaro Duarte, M.A.; Bueno, C.E.; De Martin, A.S. Efficacy of reciprocating instruments for removing filling material in curved canals obturated with a single-cone technique: A micro-computed tomographic analysis. J. Endod. 2014, 40, 1000–1004. [Google Scholar] [CrossRef]
- Brantley, W.A.; Svec, T.A.; Iijima, M.; Powers, J.M.; Grentzer, T.H. Differential scanning calorimetric studies of nickel-titanium rotary endodontic instruments after simulated clinical use. J. Endod. 2002, 28, 774–778. [Google Scholar] [CrossRef] [PubMed]
- Micro-Mega. The 2Shape Brochure. Available online: https://micro-mega.com (accessed on 20 March 2018).
- Versluis, A.; Kim, H.C.; Lee, W.; Kim, B.M.; Lee, C.J. Flexural stiffness and stresses in nickel-titanium rotary files for various pitch and cross-sectional geometries. J. Endod. 2012, 38, 1399–1403. [Google Scholar] [CrossRef] [PubMed]
- Ye, J.; Gao, Y. Metallurgical characterization of M-Wire nickel-titanium shape memory alloy used for endodontic rotary instruments during low-cycle fatigue. J. Endod. 2012, 38, 105–107. [Google Scholar] [CrossRef] [PubMed]
- Burklein, S.; Benten, S.; Schafer, E. Quantitative evaluation of apically extruded debris with different single-file systems: Reciproc, F360 and OneShape versus Mtwo. Int. Endod. J. 2014, 47, 405–409. [Google Scholar] [CrossRef] [PubMed]
- De-Deus, G.; Neves, A.; Silva, E.J.; Mendonca, T.A.; Lourenco, C.; Calixto, C.; Lima, E.J. Apically extruded dentin debris by reciprocating single-file and multi-file rotary system. Clin. Oral Investig. 2015, 19, 357–361. [Google Scholar] [CrossRef]
- Schirrmeister, J.F.; Hermanns, P.; Meyer, K.M.; Goetz, F.; Hellwig, E. Detectability of residual Epiphany and gutta-percha after root canal retreatment using a dental operating microscope and radiographs--an ex vivo study. Int. Endod. J. 2006, 39, 558–565. [Google Scholar] [CrossRef]
- Kfir, A.; Tsesis, I.; Yakirevich, E.; Matalon, S.; Abramovitz, I. The efficacy of five techniques for removing root filling material: Microscopic versus radiographic evaluation. Int. Endod. J. 2012, 45, 35–41. [Google Scholar] [CrossRef]
- Takahashi, C.M.; Cunha, R.S.; de Martin, A.S.; Fontana, C.E.; Silveira, C.F.; da Silveira Bueno, C.E. In vitro evaluation of the effectiveness of ProTaper universal rotary retreatment system for gutta-percha removal with or without a solvent. J. Endod. 2009, 35, 1580–1583. [Google Scholar] [CrossRef]
- Zuolo, A.S.; Mello, J.E., Jr.; Cunha, R.S.; Zuolo, M.L.; Bueno, C.E. Efficacy of reciprocating and rotary techniques for removing filling material during root canal retreatment. Int. Endod. J. 2013, 46, 947–953. [Google Scholar] [CrossRef] [PubMed]
- Hassanloo, A.; Watson, P.; Finer, Y.; Friedman, S. Retreatment efficacy of the Epiphany soft resin obturation system. Int. Endod. J. 2007, 40, 633–643. [Google Scholar] [CrossRef] [PubMed]
- Roggendorf, M.J.; Legner, M.; Ebert, J.; Fillery, E.; Frankenberger, R.; Friedman, S. Micro-CT evaluation of residual material in canals filled with Activ GP or GuttaFlow following removal with NiTi instruments. Int. Endod. J. 2010, 43, 200–209. [Google Scholar] [CrossRef] [PubMed]
- Kunert, G.G.; Camargo Fontanella, V.R.; de Moura, A.A.; Barletta, F.B. Analysis of apical root transportation associated with ProTaper Universal F3 and F4 instruments by using digital subtraction radiography. J. Endod. 2010, 36, 1052–1055. [Google Scholar] [CrossRef] [PubMed]
- Alves, F.R.; Marceliano-Alves, M.F.; Sousa, J.C.; Silveira, S.B.; Provenzano, J.C.; Siqueira, J.F., Jr. Removal of Root Canal Fillings in Curved Canals Using Either Reciprocating Single- or Rotary Multi-instrument Systems and a Supplementary Step with the XP-Endo Finisher. J. Endod. 2016, 42, 1114–1119. [Google Scholar] [CrossRef] [PubMed]
- Cavenago, B.C.; Ordinola-Zapata, R.; Duarte, M.A.; del Carpio-Perochena, A.E.; Villas-Boas, M.H.; Marciano, M.A.; Bramante, C.M.; Moraes, I.G. Efficacy of xylene and passive ultrasonic irrigation on remaining root filling material during retreatment of anatomically complex teeth. Int. Endod. J. 2014, 47, 1078–1083. [Google Scholar] [CrossRef] [PubMed]
- Da Rosa, R.A.; Santini, M.F.; Cavenago, B.C.; Pereira, J.R.; Duarte, M.A.; So, M.V. Micro-CT Evaluation of Root Filling Removal after Three Stages of Retreatment Procedure. Braz. Dent. J. 2015, 26, 612–618. [Google Scholar] [CrossRef]
- Barreto, M.S.; Rosa, R.A.; Santini, M.F.; Cavenago, B.C.; Duarte, M.A.; Bier, C.A.; So, M.V. Efficacy of ultrasonic activation of NaOCl and orange oil in removing filling material from mesial canals of mandibular molars with and without isthmus. J. Appl. Oral Sci. 2016, 24, 37–44. [Google Scholar] [CrossRef]
- Friedman, S.; Moshonov, J.; Trope, M. Residue of gutta-percha and a glass ionomer cement sealer following root canal retreatment. Int. Endod. J. 1993, 26, 169–172. [Google Scholar] [CrossRef]
| Groups | n | IM | RM1 | RM2 | % |
|---|---|---|---|---|---|
| TS2 with Endo Ultra | 22 | 2.50 ± 0.37 | 0.10 ± 0.07 | 0.08 ± 0.05 | 3.45 ± 2.62 |
| TS2 with Irrisafe | 22 | 2.52 ± 0.36 | 0.16 ± 0.13 | 0.13 ± 0.125 | 4.87 ± 4.66 |
| R25 with Endo Ultra | 22 | 2.34 ± 0.49 | 0.27 ± 0.22 | 0.20 ± 0.18 | 9.42 ± 8.22 |
| R25 with Irrisafe | 22 | 2.35 ± 0.36 | 0.22 ± 0.22 | 0.18 ± 0.18 | 7.54 ± 6.96 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kaloustian, M.K.; Nehme, W.; El Hachem, C.; Zogheib, C.; Ghosn, N.; Michetti, J.; Naaman, A.; Diemer, F. Evaluation of Two Shaping Systems and Two Ultrasonic Irrigation Devices in Removing Root Canal Filling Material from Mesial Roots of Mandibular Molars: A Micro CT Study. Dent. J. 2019, 7, 2. https://doi.org/10.3390/dj7010002
Kaloustian MK, Nehme W, El Hachem C, Zogheib C, Ghosn N, Michetti J, Naaman A, Diemer F. Evaluation of Two Shaping Systems and Two Ultrasonic Irrigation Devices in Removing Root Canal Filling Material from Mesial Roots of Mandibular Molars: A Micro CT Study. Dentistry Journal. 2019; 7(1):2. https://doi.org/10.3390/dj7010002
Chicago/Turabian StyleKaloustian, Marc Krikor, Walid Nehme, Claire El Hachem, Carla Zogheib, Nabil Ghosn, Jérôme Michetti, Alfred Naaman, and Franck Diemer. 2019. "Evaluation of Two Shaping Systems and Two Ultrasonic Irrigation Devices in Removing Root Canal Filling Material from Mesial Roots of Mandibular Molars: A Micro CT Study" Dentistry Journal 7, no. 1: 2. https://doi.org/10.3390/dj7010002
APA StyleKaloustian, M. K., Nehme, W., El Hachem, C., Zogheib, C., Ghosn, N., Michetti, J., Naaman, A., & Diemer, F. (2019). Evaluation of Two Shaping Systems and Two Ultrasonic Irrigation Devices in Removing Root Canal Filling Material from Mesial Roots of Mandibular Molars: A Micro CT Study. Dentistry Journal, 7(1), 2. https://doi.org/10.3390/dj7010002





