ICNP® R&D Centre Ireland: Defining Requirements for an Intersectoral Digital Landscape
Abstract
:1. Introduction
2. Materials and Methods
2.1. International Classification of Nursing Practice
- Act as the National Reference Centre for the SNOMED-CT® License for Terminology use in Ireland.
- Build on established relationships with existing ICNP accreditation centres and seek funding for future initiatives through research funding streams.
- Disseminate information on research activity, both nationally through the national nursing association and peer reviewed publications.
- Promote harmonisation with other standards-based concepts and terminology groups.
- To impact on existing fragmented national health services and strike a balance with powerful and affluent groups focusing on over-medicalised models of care.
- To represent the nurse practitioner and the service user as appropriate.
3. Results
3.1. Action 1: User Group Formation
3.2. Action 2: Research and Development Work Plan
- Interdisciplinary team involvement to be considered as appropriate
- Problem Analysis
- Problem Formulation
- Selection of co- creators’ users and actors
- Selection of methods that can be used to predict the knowledge needed to solve the problem or attempt to do so [25] (p. 10).
3.3. Actions 3–6: Project Management, Educational Frameworks and Dissemination
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- International Classification of Nursing Practice (ICNP®) (Online) 2015 ICN Geneva. Available online: http://www.icn.ch/what-we-do/international-classification-for-nursing-practice-icnpr/ (accessed on 10 February 2017).
- World Health Organisation. WHO Global Strategy on People Centred and Integrated Health Services Interim Report (Online). Geneva: WHO Production Services. Available online: http://www.who.int/servicedeliverysafety/areas/people-centred-care/global-strategy/en/ (accessed on 9 November 2016).
- Aiken, L.H.; Sloane, D.M.; Bruyneel, L.; van den Heede, K.; Griffiths, P.; Busse, R.; Diomidous, M.; Kinnunen, J.; Kózka, M.; Sermeus, W.; et al. Nurse staffing and education and hospital mortality in nine European countries: A retrospective observational study. Lancet 2014, 383, 1824–1830. [Google Scholar] [CrossRef]
- World Health Organisation. Global Strategy on Human Resources for Health: Workforce 2030. (Online), May 2016 World Health Document Production Services Geneva. Available online: http://www.who.Int/hrh/resources/pub_globstrathrh-2030/en/ (accessed on 17 January 17).
- World Health Organisation Framework on Integrated People Centred Health Services A69/39 (Online), 15 April 2016, WHO Geneva. Available online: http://apps.who.int/gb/ebwha/pdf_files/WHA69/A69_39-en.pdf?ua=1&ua=1 (accessed on 17 January 2017).
- Hussey, P.; Kennedy, M.A. Instantiating informatics within nursing practice for patient centred holistic models of care: A Discussion Paper. J. Adv. Nurs. 2016, 72, 1030–1041. [Google Scholar] [CrossRef] [PubMed]
- eHealth Ireland. (Online) 2015 Department of Health, Ireland. Available online: http://www.ehealthireland.ie/ (accessed on 10 February 2017).
- Heeks, R. Health information systems: Failure, success and improvisation. Int. J. Med. Inform. 2006, 75, 125–137. [Google Scholar] [CrossRef] [PubMed]
- Bowns, I.R.; Rotherham, G.; Paisley, S. Factors associated with success in the implementation of information management and technology in the NHS. Health Inform. J. 1999, 5, 136–145. [Google Scholar] [CrossRef]
- Gauld, R.; Goldfinch, S. Dangerous Enthusiasms: e-Government, Computer Failure and Information Systems Development; University of Otago University Press: Dunedin, New Zealand, 2006. [Google Scholar]
- Sauer, C. Unreasonable expectations—NHS IT, Greek choruses and the games institutions play around mega-programmes. J. Inf. Technol. 2007, 22, 195–201. [Google Scholar] [CrossRef]
- Aarts, J. Towards safe Information Technology in Healthcare. Inf. Knowl. Syst. Manag. 2011, 10, 335–344. [Google Scholar]
- Sligo, J.; Gauld, R.; Roberts, V.; Villa, L. A literature review for large-scale health information system project planning, implementation and evaluation. Int. J. Med. Inform. 2017, 97, 86–97. [Google Scholar] [CrossRef] [PubMed]
- McEvoy, P. Chronic Disease Management: A New Paradigm for Care; CRC Press Radcliffe: London, UK, 2014; ISBN 978190891156. [Google Scholar]
- Roe, L.; O’Halloran, A.; Norman, D.C.; Murphy, C. The Impact of Frailty on Public Health Nurse Service Utilisation Findings; Institute of Community Health Nursing and The Irish Longitudinal Study on Aging: Dublin, Ireland, 2016; ISBN 978-1-907894-12-1. [Google Scholar]
- World Health Organisation. The World Bank Tracking Universal Health Coverage: First Global Monitoring Report. (Online) Geneva: WHO 2015. Available online: http://apps.who.int/iris/bitstream/10665/174536/1/9789241564977_eng.pdf?ua= (accessed on 18 January 2017).
- Organisation for Economic Co-Operation and Development. Health Spending (Online). Paris: OECD. 4 November 2015. Available online: http://www.oecd.org/health/health-systems/health-at-a-glance-19991312.htm (accessed on 9 November 2016).
- Berwick, D.M.; Nolan, T.W.; Whittington, J. The triple aim: Health, Care and Cost. Health Aff. 2008, 27, 759–769. [Google Scholar] [CrossRef] [PubMed]
- Berg, M. Rationalising Medical Work; The MIT Press: Cambridge, MA, USA, 1997; ISBN 0262024179. [Google Scholar]
- International Council of Nurses. International perspectives: ICNP® now included in WHO family of classifications. Int. Nurs. Rev. 2009, 56, 155–156. [Google Scholar]
- Garcia, T.R. ICNP®: A standardized terminology to describe professional nursing practice. Rev. Esc. Enferm. J. Sch. Nurs. Univ. San Pablo USP 2016, 50, 378–379. [Google Scholar] [CrossRef] [PubMed]
- Strudwick, G.; Hardiker, N.R. Understanding the use of standardized nursing terminology and classification systems in published research: A case study using the International Classification for Nursing Practice®. Int. J. Med. Inform. 2016, 94, 215–221. [Google Scholar] [CrossRef] [PubMed]
- International Health Terminology Standards Development Organisation (IHTSDO). (Online) Snomed International United Kingdom. Available online: http://www.snomed.org/ (accessed on 17 January 2017).
- Office of the Chief Information Officer. (Online) 2015 Health Services Executive Dublin. Available online: http://www.hse.ie/eng/about/Who/OoCIO/ (accessed on 17 January 2017).
- Botin, L.; Bertelsen, P.; Nøhr, C. Challenges in Improving Health Care by Use of Health Informatics Technology. In Techno-Anthropology in Health Informatics Methodologies for Improving Human–Technology Relations; Botin, L., Bertelsen, P., Nøhr, C., Eds.; IOS Press: Amsterdam, The Netherlands, 2015; pp. 3–13. [Google Scholar]
- School of Nursing and Human Sciences (SNHS) ICNP User Group Centre Dublin City University (Online). 2016. Available online: https://www.dcu.ie/snhs/icnpusergroup.shtml (accessed on 17 January 2017).
- European Commission (EC). Study on Big Data in Public Health, Telemedicine and Healthcare (Online) December 2016 Brussels. Available online: https://ec.europa.eu/health/sites/health/files/ehealth/docs/bigdata_report_en.pdf (accessed on 19 January 2017).
- Wijngaarden, J.D.H.; Scholten, G.R.M.; van Wijk, K.P. Strategic analysis for health care organizations: The suitability of the SWOT-analysis. Int. J. Health Plan. Manag. 2010, 27, 34–49. [Google Scholar] [CrossRef] [PubMed]
- Hussey, P.; Adams, E.; Shaffer, F.A. Nursing Informatics and Leadership, an Essential Competency for a Global Priority: eHealth. Nurse Lead. 2015, 13, 52–57. [Google Scholar] [CrossRef]

| Goal | Group No. | Detail of Activity | Deliverable/Metric |
|---|---|---|---|
| Promote the use of ICNP equivalence tables with international health terminology standards and national clinical programmes objectives. | 1 | Phase one development of a national data dictionary platform. Bridging interdisciplinary gap between clinical and technical teams. Workshop with patient group representatives for knowledge transfer. | Development of use case report in line with national clinical programme objectives for integrated care eReferral, ePrescription and Discharge letter. |
| Act as a national reference centre for terminology use in Ireland. | 2, 3, 5, 6 | Readiness for engagement enhancement of clinical documentation practices to include clinical terminology and measure patient outcome. Implementation research and knowledge transfer on use of ICNP phase one. | Workshops developed on nursing informatics and use of ICNP delivered through National Nursing Agency. Clinical nurse specialist group formed in care of older person services. |
| Build on established relationships with existing ICNP® accreditation centres and seek funding for future initiatives. | 2, 4, 5 | Collaboration with ICNP® in Poland and ICN on eHealth Strategy agendas. | Contributed briefing documents to ICN strategic planning team Q3 and Q4. Collaboration ongoing with ICNP® Research proposal for funding completed. |
| Disseminate information on research activity. | All groups | Formal communication with core stakeholders. Linking with vendors on National Data Dictionary requirements. | Seven presentations Three reports published. |
| Promote harmonisation with other standards-based concepts and terminology groups. | 4, 5 | Collaboration with other major terminology groups in Ireland. Collaboration with national terminology release centre UK. | Mapping of nursing assessment documentation to ICNP® for inclusion in national data dictionary. |
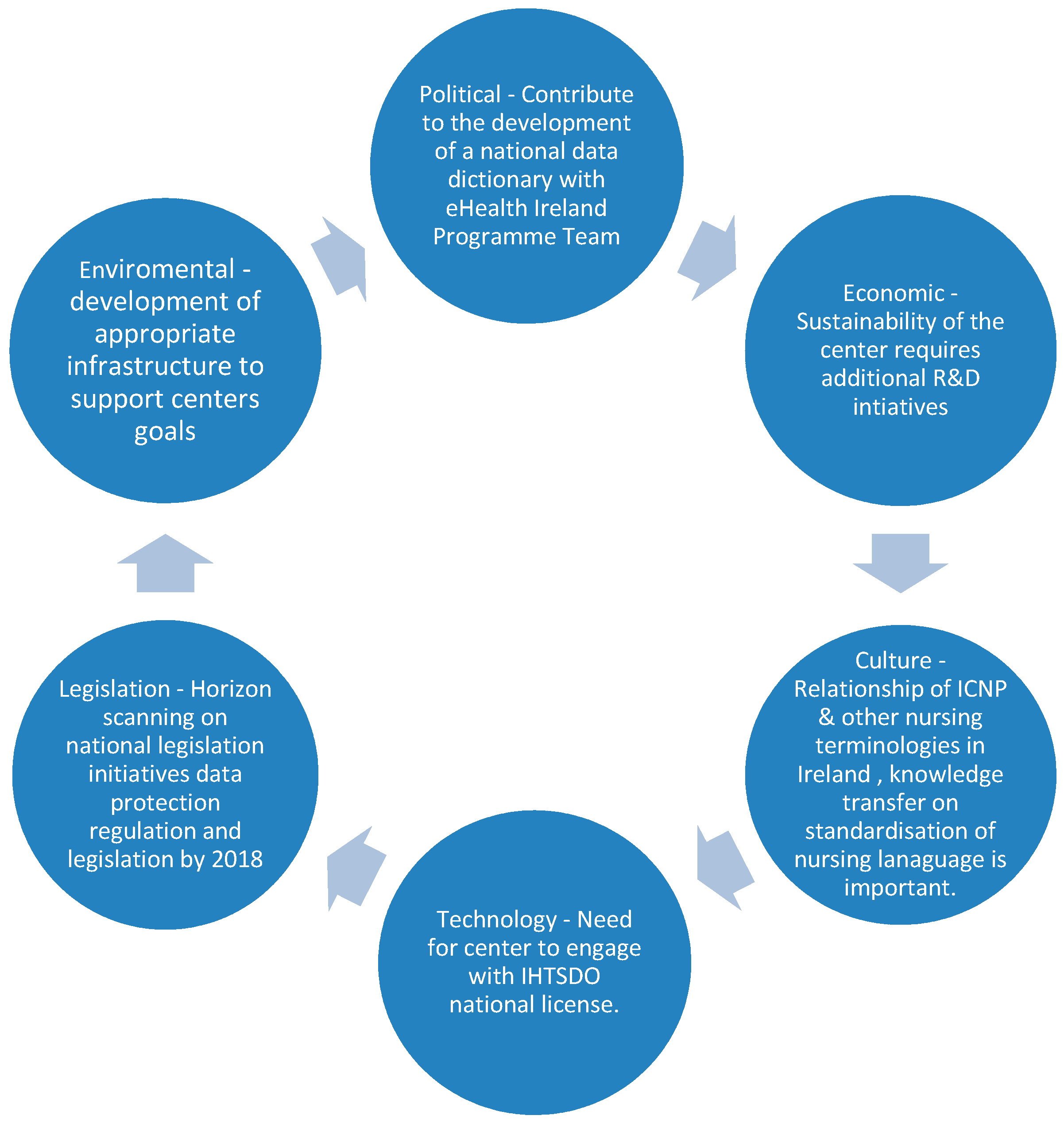
| PESTLE Questions Used to Inform Decision-Making |
|---|
| What are the core political agendas in Ireland that can affect the centre‘s development? |
| What economic factors can impact the centre‘s development? |
| What cultural factors need to be considered by the centre? |
| What role has technology to play and what innovations can impact the centre‘s development? |
| What legislation can impact on the centre‘s development? |
| What are any environmental concerns that may impact the centre‘s development? |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hussey, P.; Corbally, M.; Rodger, D.; Kirwan, A.; Adams, E.; Kavanagh, P.; Matthews, A. ICNP® R&D Centre Ireland: Defining Requirements for an Intersectoral Digital Landscape. Informatics 2017, 4, 7. https://doi.org/10.3390/informatics4020007
Hussey P, Corbally M, Rodger D, Kirwan A, Adams E, Kavanagh P, Matthews A. ICNP® R&D Centre Ireland: Defining Requirements for an Intersectoral Digital Landscape. Informatics. 2017; 4(2):7. https://doi.org/10.3390/informatics4020007
Chicago/Turabian StyleHussey, Pamela, Melissa Corbally, Daragh Rodger, Anne Kirwan, Elizabeth Adams, Paula Kavanagh, and Anne Matthews. 2017. "ICNP® R&D Centre Ireland: Defining Requirements for an Intersectoral Digital Landscape" Informatics 4, no. 2: 7. https://doi.org/10.3390/informatics4020007
APA StyleHussey, P., Corbally, M., Rodger, D., Kirwan, A., Adams, E., Kavanagh, P., & Matthews, A. (2017). ICNP® R&D Centre Ireland: Defining Requirements for an Intersectoral Digital Landscape. Informatics, 4(2), 7. https://doi.org/10.3390/informatics4020007





