Psychological Wellbeing of Parents with Infants Admitted to the Neonatal Intensive Care Unit during SARS-CoV-2 Pandemic
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants
2.3. Data Collection
- (1)
- (2)
- The State-Trait Anxiety Inventory (STAI) [22] measures symptoms of anxiety in adults. It consists of two sub-scales of 20 items respectively evaluating “state anxiety” (STAI-S anxiety in a specific situation) and “trait anxiety” (STAI-T anxiety as a general trait). Each item is based on four levels of response. A score from 40 to 50 indicates mild anxiety, 51 to 60 moderate anxiety, and >60 severe anxiety.
- (3)
- The Parental Stressor Scale: NICU (PSS: NICU) [23,24] measures stress experienced by parents during hospitalization related to parental role alteration (PRA), infant behavior and appearance (IBA), and sights and sounds of the unit (SS). Parents are asked to rate items on a five-point scale ranging from 1 (not at all stressful) to 5 (extremely stressful). An item on perceived overall parental stress is also present.
- (4)
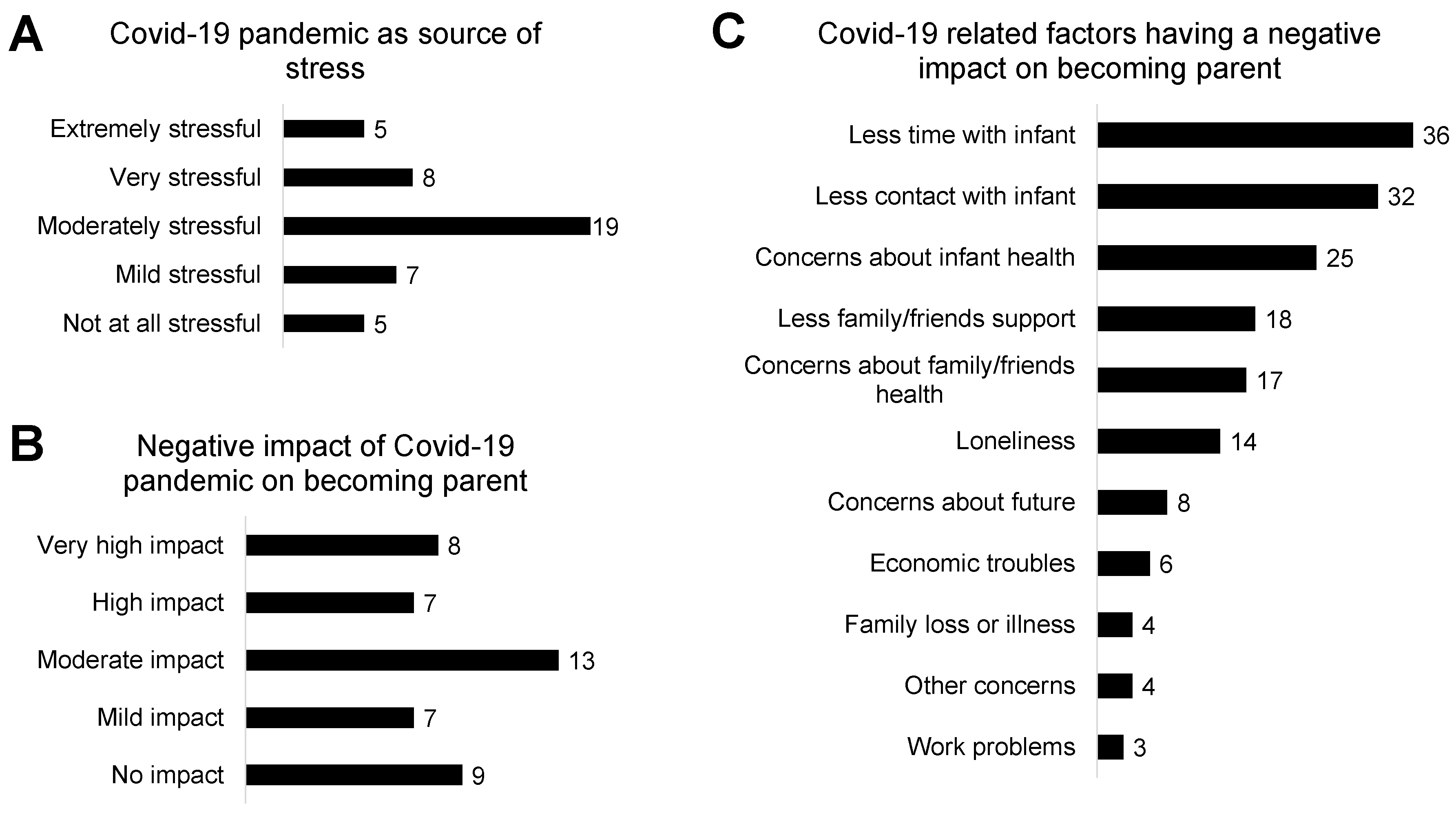
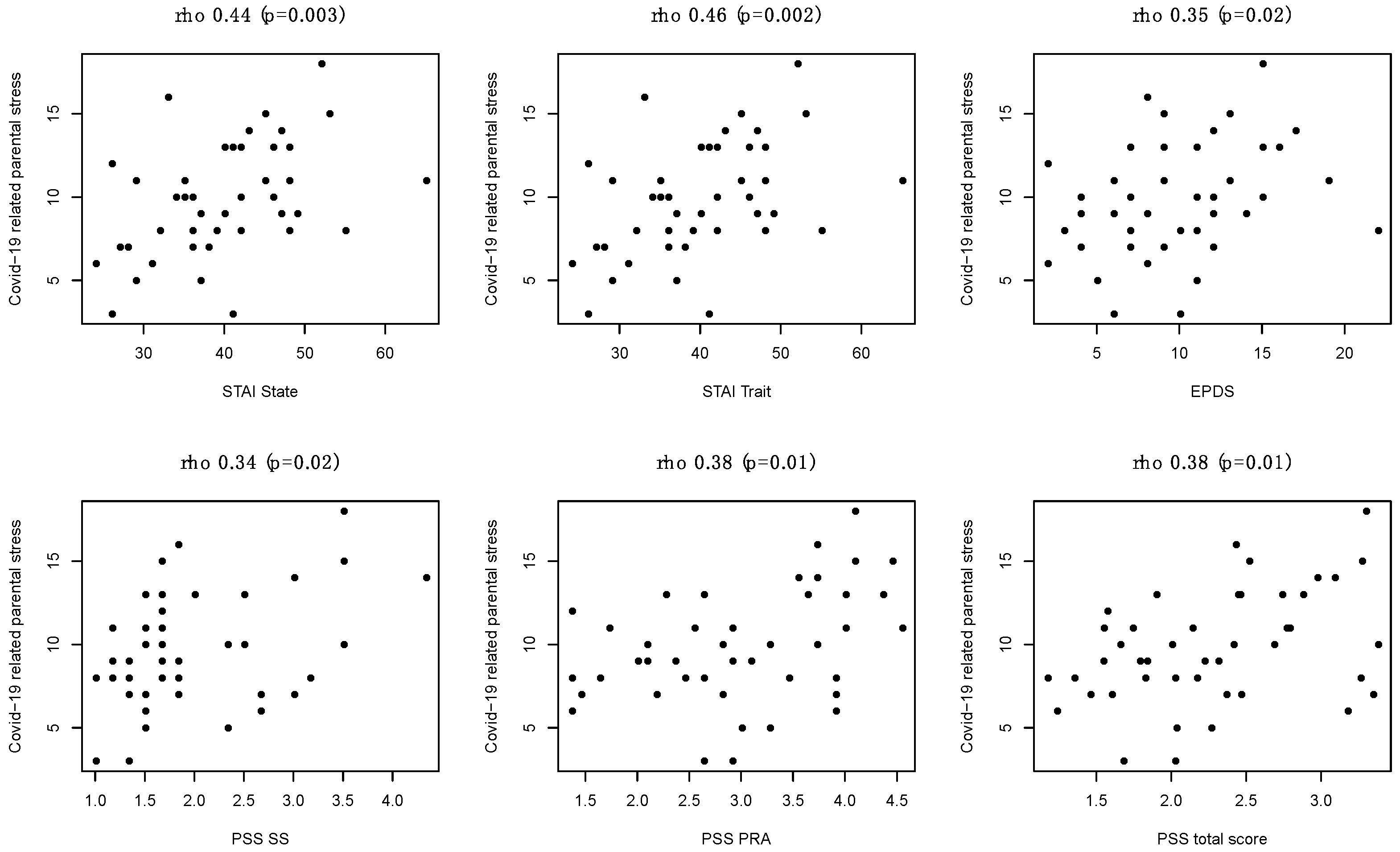
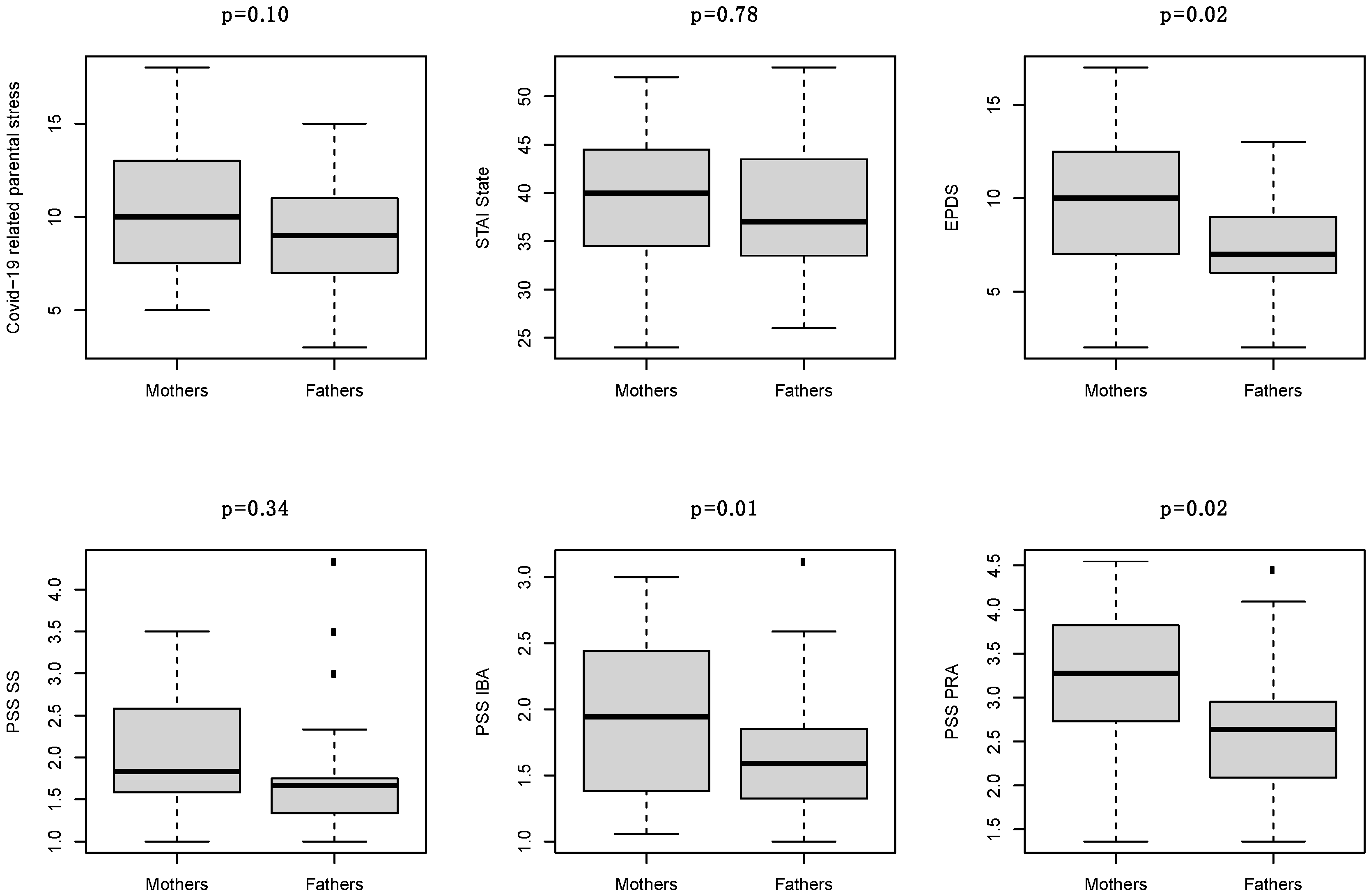
- An ad hoc questionnaire has been developed to assess the COVID-19 related parental stress. The tool, shown in Supplementary Table S1, consists of two items asking to be answered on a Likert scale from 1 (not at all) to 5 (extremely) and one item considering the presence or absence of 10 stress factors plus an additional one that the respondents can express (other). The instrument focuses on the impact of the COVID-19 pandemic, in terms of stress, on the experience of becoming parent. The questions were designed based on the literature [25,26] and clinical experience. The score ranges from 2 to 21. Socio-demographic and clinical data were collected through a crosscheck between parents’ reports and medical records.
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Roque, A.T.F.; Lasiuk, G.C.; Radünz, V.; Hegadoren, K. Scoping Review of the Mental Health of Parents of Infants in the NICU. JOGNN J. Obstet. Gynecol. Neonatal Nurs. 2017, 46, 576–587. [Google Scholar] [CrossRef] [Green Version]
- Tandberg, B.S.; Flacking, R.; Markestad, T.; Grundt, H.; Moen, A. Parent psychological wellbeing in a single-family room versus an open bay neonatal intensive care unit. PLoS ONE 2019, 14, e0224488. [Google Scholar]
- Erdei, C.; Liu, C.H. The downstream effects of COVID-19: A call for supporting family wellbeing in the NICU. J. Perinatol. 2020, 40, 1283–1285. [Google Scholar] [CrossRef]
- Rogers, C.E.; Kidokoro, H.; Wallendorf, M.; Inder, T.E. Identifying mothers of very preterm infants at-risk for postpartum depression and anxiety before discharge. J. Perinatol. 2013, 33, 171–176. [Google Scholar] [CrossRef] [Green Version]
- Treyvaud, K.; Lee, K.J.; Doyle, L.W.; Anderson, P.J. Very preterm birth influences parental mental health and family outcomes seven years after birth. J. Pediatr. 2014, 164, 515–521. [Google Scholar] [CrossRef] [Green Version]
- Bergman, N.J.; Ludwig, R.J.; Westrup, B.; Welch, M.G. Nurturescience versus neuroscience: A case for rethinking perinatal mother–infant behaviors and relationship. Birth Defects Res. 2019, 111, 1110–1127. [Google Scholar] [CrossRef]
- McManus, B.M.; Poehlmann, J. Parent-child interaction, maternal depressive symptoms and preterm infant cognitive function. Infant Behav. Dev. 2012, 35, 489–498. [Google Scholar] [CrossRef] [Green Version]
- Turpin, H.; Urben, S.; Ansermet, F.; Borghini, A.; Murray, M.M.; Müller-Nix, C. The interplay between prematurity, maternal stress and children’s intelligence quotient at age 11: A longitudinal study. Sci. Rep. 2019, 9, 1–9. [Google Scholar] [CrossRef]
- Huhtala, M.; Korja, R.; Lehtonen, L.; Haataja, L.; Lapinleimu, H.; Rautava, P.; PIPARI Study Group. Associations between parental psychological well-being and socio-emotional development in 5-year-old preterm children. Early Hum. Dev. 2014, 90, 119–124. [Google Scholar] [CrossRef]
- Hall, S.L.; Cross, J.; Selix, N.W.; Patterson, C.; Segre, L.; Chuffo-Siewert, R.; Geller, P.A.; Martin, M.L. Recommendations for enhancing psychosocial support of NICU parents through staff education and support. J. Perinatol. 2015, 35, S29–S36. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Treyvaud, K.; Spittle, A.; Anderson, P.J.; O’Brien, K. A multilayered approach is needed in the NICU to support parents after the preterm birth of their infant. Early Hum. Dev. 2019, 139, 104838. [Google Scholar] [CrossRef]
- Murray, P.D.; Swanson, J.R. Visitation restrictions: Is it right and how do we support families in the NICU during COVID-19? J. Perinatol. 2020, 40, 1576–1581. [Google Scholar] [CrossRef]
- Bembich, S.; Tripani, A.; Mastromarino, S.; di Risio, G.; Castelpietra, E.; Risso, F.M. Parents experiencing NICU visit restrictions due to COVID-19 pandemic. Acta Paediatr. Int. J. Paediatr. 2020. [Google Scholar] [CrossRef]
- Carter, B.S.; Willis, T.; Knackstedt, A. Neonatal family-centered care in a pandemic. J. Perinatol. 2021, 41, 1177–1179. [Google Scholar] [CrossRef]
- SIN-Società Italiana di Neonatologia. 2021. Available online: https://www.sin-neonatologia.it (accessed on 25 August 2021).
- COVID-19–EFCNI. [Online]. Available online: https://www.efcni.org/health-topics/covid-19-faq/ (accessed on 25 August 2021).
- Ionio, C.; Colombo, C.; Brazzoduro, V.; Mascheroni, E.; Confalonieri, E.; Castoldi, F.; Lista, G. Mothers and fathers in nicu: The impact of preterm birth on parental distress. Eur. J. Psychol. 2016, 12, 604–621. [Google Scholar] [CrossRef] [Green Version]
- Ionio, C.; Mascheroni, E.; Colombo, C.; Castoldi, F.; Lista, G. Stress and feelings in mothers and fathers in NICU: Identifying risk factors for early interventions. Prim. Heal. Care Res. Dev. 2019, 20, 1–7. [Google Scholar] [CrossRef] [Green Version]
- Trumello, C.; Candelori, C.; Cofini, M.; Cimino, S.; Cerniglia, L.; Paciello, M.; Babore, A. Mothers’ depression, anxiety, and mental representations after preterm birth: A study during the infant’s hospitalization in a neonatal intensive care unit. Front. Public Health 2018, 6, 359. [Google Scholar] [CrossRef] [PubMed]
- Carpiniello, B.; Pariante, C.M.; Serri, F.; Costa, G.; Carta, M.G. Validation of the Edinburgh postnatal depression scale in Italy. J. Psychosom. Obstet. Gynaecol. 1997, 18, 280–285. [Google Scholar] [CrossRef] [PubMed]
- Cox, J.L.; Holden, J.M.; Sagovsky, R. Detection of Postnatal Depression: Development of the 10-item Edinburgh Postnatal Depression scale. Br. J. Psychiatry 1987, 150, 782–786. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Spielberger, C.D. Manual for the State-Trait Anxiety Inventory (STAI Form Y); Consulting Psycologists Press: Palo Alto, CA, USA, 1983. [Google Scholar]
- Montirosso, R.; Provenzi, L.; Calciolari, G.; Borgatti, R. Measuring maternal stress and perceived support in 25 Italian NICUs. Acta Paediatr. Int. J. Paediatr. 2012, 101, 136–142. [Google Scholar] [CrossRef]
- Carter, M.C.; Miles, M.S. The Parental Stressor Scale: Pediatric Intensive Care Unit. Matern. Child. Nurs. J. 1989, 18, 187–198. [Google Scholar]
- Vanaken, L.; Scheveneels, S.; Belmans, E.; Hermans, D. Validation of the Impact of Event Scale With Modifications for COVID-19 (IES-COVID19). Front. Psychiatry 2020, 11, 738. [Google Scholar] [CrossRef] [PubMed]
- Ostacoli, L.; Cosma, S.; Bevilacqua, F.; Berchialla, P.; Bovetti, M.; Carosso, A.R.; Malandrone, F.; Carletto, S.; Benedetto, C. Psychosocial factors associated with postpartum psychological distress during the COVID-19 pandemic: A cross-sectional study. BMC Pregnancy Childbirth 2020, 20, 703. [Google Scholar] [CrossRef] [PubMed]
- R Core Team. A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2020. [Google Scholar]
- Zanardo, V.; Manghina, V.; Giliberti, L.; Vettore, M.; Severino, L.; Straface, G. Psychological impact of COVID-19 quarantine measures in northeastern Italy on mothers in the immediate postpartum period. Int. J. Gynecol. Obstet. 2020, 150, 184–188. [Google Scholar] [CrossRef]
- Yan, H.; Ding, Y.; Guo, W. Mental Health of Pregnant and Postpartum Women During the Coronavirus Disease 2019 Pandemic: A Systematic Review and Meta-Analysis. Front. Psychol. 2020, 11, 3324. [Google Scholar] [CrossRef]
- Liu, C.H.; Erdei, C.; Mittal, L. Risk factors for depression, anxiety, and PTSD symptoms in perinatal women during the COVID-19 Pandemic. Psychiatry Res. 2021, 295, 113552. [Google Scholar] [CrossRef]
- Leal, P.C.; Goes, T.C.; da Silva, L.C.F.; Teixeira-Silva, F. Trait vs. state anxiety in different threatening situations. Trends Psychiatry Psychother. 2017, 39, 147–157. [Google Scholar] [CrossRef] [PubMed]
- Ionio, C.; Lista, G.; Mascheroni, E.; Olivari, M.G.; Confalonieri, E.; Mastrangelo, M.; Brazzoduro, V.; Balestriero, M.A.; Banfi, A.; Bonanomi, A.; et al. Premature birth: Complexities and difficulties in building the mother–child relationship. J. Reprod. Infant Psychol. 2017, 35, 509–523. [Google Scholar] [CrossRef]
- Alkozei, A.; McMahon, E.; Lahav, A. Stress levels and depressive symptoms in NICU mothers in the early postpartum period. J. Matern. Neonatal Med. 2014, 27, 1738–1743. [Google Scholar] [CrossRef]
- Bin-Nun, A.; Palmor-Haspal, S.; Mimouni, F.B.; Kasirer, Y.; Hammerman, C.; Tuval-Moshiach, R. Infant delivery and maternal stress during the COVID-19 pandemic: A comparison of the well-baby versus neonatal intensive care environments. J. Perinatol. 2021, 2021, 1–7. [Google Scholar]
- Schiller, C.E.; Meltzer-Brody, S.; Rubinow, D.R. The role of reproductive hormones in postpartum depression. CNS Spectr. 2015, 20, 48–59. [Google Scholar] [CrossRef] [PubMed]
- Leckman, J.F.; Feldman, R.; Swain, J.E.; Eicher, V.; Thompson, N.; Mayes, L.C. Primary parental preoccupation: Circuits, genes, and the crucial role of the environment. J. Neural Transm. 2004, 111, 753–771. [Google Scholar] [CrossRef] [PubMed]
- Garrison, A.M.; Kahn, J.H.; Sauer, E.M.; Florczak, M.A. Disentangling the effects of depression symptoms and adult attachment on emotional disclosure. J. Couns. Psychol. 2012, 59, 230–239. [Google Scholar] [CrossRef]
- Kirolos, S.; Sutcliffe, L.; Clausen, M.G.; Abernethy, C.; Shanmugalingam, S.; Bauwens, N.; Orme, J.; Thomson, K.; Grattan, R.; Patel, N. Asynchronous video messaging promotes family involvement and mitigates separation in neonatal care. Arch. Dis. Childhood-Fetal Neonatal Ed. 2021, 106, 172–177. [Google Scholar] [CrossRef] [PubMed]

| Variable | N (%) or Median (IQR) | |
|---|---|---|
| Parents (n = 44) | Parent: | |
| Mothers | 25 (67) | |
| Father | 19 (43) | |
| Age, years | 35 (32–39) | |
| Education level: | ||
| Primary or middle school | 12 (27) | |
| High school | 18 (41) | |
| University | 14 (32) | |
| Number of pregnancies: | ||
| One pregnancy | 28 (64) | |
| Two pregnancies | 16 (36) | |
| Visits to the infant in the NICU, n | 8 (5–14) | |
| STAI state | 42 (37–51) | |
| STAI state: | ||
| <40 | 20 (46) | |
| 40–50 | 12 (27) | |
| 51–60 | 8 (18) | |
| >60 | 4 (9) | |
| STAI trait | 40 (35–46) | |
| STAI trait: | ||
| <40 | 22 (50) | |
| 40–50 | 18 (41) | |
| 51–60 | 3 (7) | |
| >60 | 1 (2) | |
| EPDS | 9 (7–12) | |
| EPDS ≥ 13 | 10 (23) | |
| PSS-SS | 1.7 (1.5–2.4) | |
| PSS-IBA | 1.7 (1.4–2.3) | |
| PSS-PRA | 2.9 (2.3–3.7) | |
| PSS-perceived stress item | 3 (3–4) | |
| PSS-total score | 2.2 (1.8–2.7) | |
| Infants (n = 25) | Gestational age, weeks | 34 (31–35) |
| Birth weight, grams | 2185 (1480–3100) | |
| Age at parental psychological screening, days | 13 (8–14) | |
| Perinatal information (n = 25) | Conception: | |
| Spontaneous | 20 (80) | |
| Medically assisted | 5 (20) | |
| Pregnancy: | ||
| Singleton | 22 (88) | |
| Twin | 3 (12) | |
| Delivery: | ||
| Vaginal or elective caesarean | 6 (24) | |
| Emergency caesarean | 19 (76) | |
| Diagnosis at discharge (n = 25) | RDS + prematurity | 16 (64) |
| Sepsis | 3 (12) | |
| Asphixia | 2 (8) | |
| Prematurity | 2 (8) | |
| RDS | 2 (8) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Polloni, L.; Cavallin, F.; Lolli, E.; Schiavo, R.; Bua, M.; Volpe, B.; Meneghelli, M.; Baraldi, E.; Trevisanuto, D. Psychological Wellbeing of Parents with Infants Admitted to the Neonatal Intensive Care Unit during SARS-CoV-2 Pandemic. Children 2021, 8, 755. https://doi.org/10.3390/children8090755
Polloni L, Cavallin F, Lolli E, Schiavo R, Bua M, Volpe B, Meneghelli M, Baraldi E, Trevisanuto D. Psychological Wellbeing of Parents with Infants Admitted to the Neonatal Intensive Care Unit during SARS-CoV-2 Pandemic. Children. 2021; 8(9):755. https://doi.org/10.3390/children8090755
Chicago/Turabian StylePolloni, Laura, Francesco Cavallin, Elisabetta Lolli, Rossana Schiavo, Martina Bua, Biancarosa Volpe, Marta Meneghelli, Eugenio Baraldi, and Daniele Trevisanuto. 2021. "Psychological Wellbeing of Parents with Infants Admitted to the Neonatal Intensive Care Unit during SARS-CoV-2 Pandemic" Children 8, no. 9: 755. https://doi.org/10.3390/children8090755
APA StylePolloni, L., Cavallin, F., Lolli, E., Schiavo, R., Bua, M., Volpe, B., Meneghelli, M., Baraldi, E., & Trevisanuto, D. (2021). Psychological Wellbeing of Parents with Infants Admitted to the Neonatal Intensive Care Unit during SARS-CoV-2 Pandemic. Children, 8(9), 755. https://doi.org/10.3390/children8090755








