The Impact of COVID-19 School Closure on Child and Adolescent Health: A Rapid Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Strategy and Selection Criteria
2.2. Inclusion and Exclusion Criteria
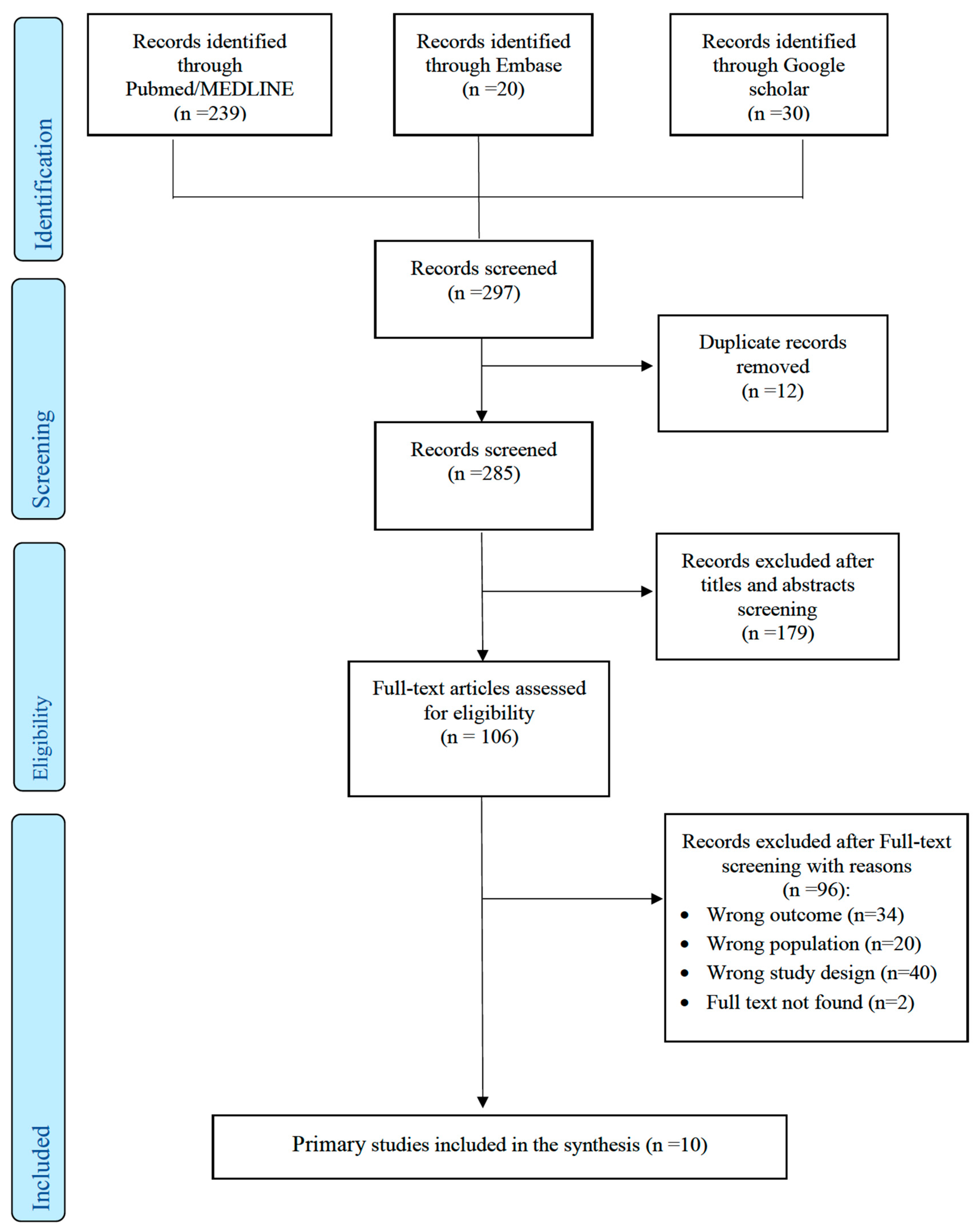
2.3. Data Screening
2.4. Data Extraction
2.5. Methodological Quality Assessment
2.6. Data Synthesis
3. Results
3.1. The Impact on Child and Adolescent Mental Health
3.2. The Impact on Child and Adolescent Physical Health
3.3. The Impact on Child and Adolescent Accessibility Issues Related to Learning, Healthcare Services, Nutrition, and Dedicated Services for Special Groups
3.4. Quality Assessment
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- UNESCO. Education: From Disruption to Recovery. Available online: https://en.unesco.org/covid19/educationresponse (accessed on 30 September 2020).
- Jackson, C.; Mangtani, P.; Hawker, J.; Olowokure, B.; Vynnycky, E. The Effects of School Closures on Influenza Outbreaks and Pandemics: Systematic Review of Simulation Studies. PLoS ONE 2014, 9, e97297. [Google Scholar] [CrossRef] [PubMed]
- Jackson, C.; Vynnycky, E.; Hawker, J.; Olowokure, B.; Mangtani, P. School closures and influenza: Systematic review of epi-demiological studies. BMJ Open 2013, 3. [Google Scholar] [CrossRef] [PubMed]
- Principi, N.; Esposito, S.; Gasparini, R.; Marchisio, P.; Crovari, P. Burden of influenza in healthy children and their households. Arch. Dis. Child. 2004, 89, 1002–1007. [Google Scholar] [CrossRef]
- Zhang, J.; Litvinova, M.; Liang, Y.; Wang, Y.; Wang, W.; Zhao, S.; Wu, Q.; Merler, S.; Viboud, C.; Vespignani, A.; et al. Age profile of susceptibility, mixing, and social distancing shape the dynamics of the novel coronavirus disease 2019 outbreak in China. medRxiv 2020. [Google Scholar] [CrossRef]
- Heavey, L.; Casey, G.; Kelly, C.; Kelly, D.; McDarby, G. No evidence of secondary transmission of COVID-19 from children attending school in Ireland, 2020. Eurosurveillance 2020, 25, 2000903. [Google Scholar] [CrossRef] [PubMed]
- Anderson, R.M.; Heesterbeek, H.; Klinkenberg, D.; Hollingsworth, T.D. How will country-based mitigation measures influence the course of the COVID-19 epidemic? Lancet 2020, 395, 931–934. [Google Scholar] [CrossRef]
- Xu, B.; Kraemer, M.U.G. Open access epidemiological data from the COVID-19 outbreak. Lancet Infect. Dis. 2020, 20, 534. [Google Scholar] [CrossRef]
- Bacete, F.J.G.; Perrin, G.M.; Schneider, B.H.; Blanchard, C. Effects of School on the Well-Being of Children and Adolescents. In Handbook of Child Well-Being: Theories, Methods and Policies in Global Perspective; Ben-Arieh, A., Casas, F., Frønes, I., Korbin, J.E., Eds.; Springer: Dordrecht, The Netherlands, 2014; pp. 1251–1305. [Google Scholar]
- Kidger, J.; Araya, R.; Donovan, J.; Gunnell, D. The Effect of the School Environment on the Emotional Health of Adolescents: A Systematic Review. Pediatrics 2012, 129, 925–949. [Google Scholar] [CrossRef]
- Zimmo, L.; Farooq, A.; Almudahka, F.; Ibrahim, I.; Al-Kuwari, M.G. School-time physical activity among Arab elementary school children in Qatar. BMC Pediatr. 2017, 17, 76. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Comprehensive School Physical Activity Programs: A Guide for Schools; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2013. [Google Scholar]
- Phelps, C.; Sperry, L.L. Children and the COVID-19 pandemic. Psychol. Trauma Theory Res. Pract. Policy 2020, 12, S73–S75. [Google Scholar] [CrossRef]
- Lee, J. Mental health effects of school closures during COVID-19. Lancet Child Adolesc. Health 2020, 4, 421. [Google Scholar] [CrossRef]
- Mayurasakorn, K.; Pinsawas, B.; Mongkolsucharitkul, P.; Sranacharoenpong, K.; Damapong, S.N. School closure, COVID-19 and lunch programme: Unprecedented undernutrition crisis in low-middle income countries. J. Paediatr. Child Health 2020. [Google Scholar] [CrossRef]
- Von Hippel, P.T.; Workman, J. From Kindergarten Through Second Grade, U.S. Children’s Obesity Prevalence Grows Only during Summer Vacations. Obesity 2016, 24, 2296–2300. [Google Scholar] [CrossRef]
- Franckle, R.; Adler, R.; Davison, K. Accelerated weight gain among children during summer versus school year and related racial/ethnic disparities: A systematic review. Prev. Chronic Dis. 2014, 11, E101. [Google Scholar] [CrossRef]
- Wang, Y.C.; Vine, S.; Hsiao, A.; Rundle, A.; Goldsmith, J. Weight-Related Behaviors When Children Are in School Versus on Summer Breaks: Does Income Matter? J. Sch. Health 2015, 85, 458–466. [Google Scholar] [CrossRef] [PubMed]
- Araújo, L.A.; Veloso, C.F.; Souza, M.C.; Azevedo, J.M.C.; Tarro, G. The potential impact of the COVID-19 pandemic on child growth and development: A systematic review. J. Pediatr. 2020. [Google Scholar] [CrossRef]
- Caffo, E.; Scandroglio, F.; Asta, L. Debate: COVID-19 and psychological well-being of children and adolescents in Italy. Child Adolesc. Ment. Health 2020. [Google Scholar] [CrossRef] [PubMed]
- Araújo, F.J.O.; de Lima, L.S.A.; Cidade, P.I.M.; Nobre, C.B.; Neto, M.L.R. Impact Of Sars-Cov-2 and Its Reverberation in Global Higher Education and Mental Health. Psychiatry Res. 2020, 288, 112977. [Google Scholar] [CrossRef] [PubMed]
- Bahn, G.H. Coronavirus Disease 2019, School Closures, and Children’s Mental Health. J. Korean Acad. Child Adolesc. Psychiatry 2020, 31, 74–79. [Google Scholar] [CrossRef] [PubMed]
- Chrisman, A.K. Debate: #Together despite the distance. Child Adolesc. Ment. Health 2020. [Google Scholar] [CrossRef]
- Esposito, S.; Principi, N. School Closure during the Coronavirus Disease 2019 (COVID-19) Pandemic: An Effective Intervention at the Global Level? JAMA Pediatr. 2020. [Google Scholar] [CrossRef] [PubMed]
- Fantini, M.P.; Reno, C.; Biserni, G.B.; Savoia, E.; Lanari, M. COVID-19 and the re-opening of schools: A policy maker’s dilemma. Ital. J. Pediatr. 2020, 46, 79. [Google Scholar] [CrossRef] [PubMed]
- Margaritis, I.; Houdart, S.; El Ouadrhiri, Y.; Bigard, X.; Vuillemin, A.; Duché, P. How to deal with COVID-19 epidemic-related lockdown physical inactivity and sedentary increase in youth? Adaptation of Anses’ benchmarks. Arch. Public Health 2020, 78, 52. [Google Scholar] [CrossRef]
- Nagata, J.M.; Abdel Magid, H.S.; Gabriel, K.P. Screen time for children and adolescents during the COVID-19 pandemic. Obesity 2020. [Google Scholar] [CrossRef]
- Featherstone, R.M.; Dryden, D.M.; Foisy, M.; Guise, J.M.; Mitchell, M.D.; Paynter, R.A.; Robinson, K.A.; Umscheid, C.A.; Hartling, L. Advancing knowledge of rapid reviews: An analysis of results, conclusions and recommendations from published review articles examining rapid reviews. Syst. Rev. 2015, 4, 50. [Google Scholar] [CrossRef]
- Garritty, C.G.G.; Kamel, C.; King, V.J.; Nussbaumer-Streit, B.; Stevens, A.H.C.; Affengruber, L. Guidance from the Cochrane Rapid Reviews Methods Group; Cochrane Rapid Reviews: London, UK, 2020; Available online: https://methods.cochrane.org/rapidreviews/sites/methods.cochrane.org.rapidreviews/files/public/uploads/cochrane_rr_-_guidance-23mar2020-final.pdf (accessed on 30 September 2020).
- Halladay, C.W.; Trikalinos, T.A.; Schmid, I.T.; Schmid, C.H.; Dahabreh, I.J. Using data sources beyond PubMed has a modest impact on the results of systematic reviews of therapeutic interventions. J. Clin. Epidemiol. 2015, 68, 1076–1084. [Google Scholar] [CrossRef]
- Bain, P. Research Guides: Systematic Reviews and Meta Analysis: Databases and Sources. Available online: https://guides.library.harvard.edu/meta-analysis (accessed on 15 February 2021).
- Nourbakhsh, E.; Nugent, R.; Wang, H.; Cevik, C.; Nugent, K. Medical literature searches: A comparison of PubMed and Google Scholar. Health Inf. Libr. J. 2012, 29, 214–222. [Google Scholar] [CrossRef]
- MacIntyre, C.R.; Chughtai, A.A. Facemasks for the prevention of infection in healthcare and community settings. BMJ 2015, 350, h694. [Google Scholar] [CrossRef]
- Chaabna, K.; Doraiswamy, S.; Mamtani, R.; Cheema, S. Facemask use in community settings to prevent respiratory infection transmission: A rapid review and meta-analysis. Int. J. Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Di Giorgio, E.; Di Riso, D.; Mioni, G.; Cellini, N. The interplay between mothers’ and children behavioral and psychological factors during COVID-19: An Italian study. Eur. Child Adolesc. Psychiatry 2020. [Google Scholar] [CrossRef]
- Baron, E.J.; Goldstein, E.G.; Wallace, C.T. Suffering in silence: How COVID-19 school closures inhibit the reporting of child maltreatment. J. Public Econ. 2020, 190, 104258. [Google Scholar] [CrossRef] [PubMed]
- Isumi, A.; Doi, S.; Yamaoka, Y.; Takahashi, K.; Fujiwara, T. Do suicide rates in children and adolescents change during school closure in Japan? The acute effect of the first wave of COVID-19 pandemic on child and adolescent mental health. Child Abus. Negl. 2020, 110, 104680. [Google Scholar] [CrossRef]
- An, R. Projecting the impact of the coronavirus disease-19 pandemic on childhood obesity in the United States: A microsimulation model. J. Sport Health Sci. 2020. [Google Scholar] [CrossRef] [PubMed]
- Angoulvant, F.; Ouldali, N.; Yang, D.D.; Filser, M.; Gajdos, V.; Rybak, A.; Guedj, R.; Soussan-Banini, V.; Basmaci, R.; Lefevre-Utile, A.; et al. COVID-19 pandemic: Impact caused by school closure and national lockdown on pediatric visits and admissions for viral and non-viral infections, a time series analysis. Clin. Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Ijadi-Maghsoodi, R.; Harrison, D.; Kelman, A.; Kataoka, S.; Langley, A.K.; Ramos, N.; Cugley, G.M.; Alquijay, M.A.; Tate, K.; Lester, P.; et al. Leveraging a public-public partnership in Los Angeles County to address COVID-19 for children, youth, and families in underresourced communities. Psychol. Trauma Theory Res. Pract. Policy 2020, 12, 457–460. [Google Scholar] [CrossRef] [PubMed]
- Masonbrink, A.R.; Hurley, E. Advocating for Children during the COVID-19 School Closures. Pediatrics 2020. [Google Scholar] [CrossRef] [PubMed]
- Kılınçel, Ş.; Kılınçel, O.; Muratdağı, G.; Aydın, A.; Usta, M.B. Factors affecting the anxiety levels of adolescents in home-quarantine during COVID-19 pandemic in Turkey. Asia-Pac. Psychiatry 2020, e12406. [Google Scholar] [CrossRef]
- Schlegelmilch, J.; Douglas, C. Initial Coronavirus Disease-2019 Closure Strategies Adopted by a Convenience Sample of US School Districts: Directions for Future Research. Disaster Med. Public Health Prep. 2020, 14, e17–e18. [Google Scholar] [CrossRef] [PubMed]
- Galea, S.; Merchant, R.M.; Lurie, N. The Mental Health Consequences of COVID-19 and Physical Distancing: The Need for Prevention and Early Intervention. JAMA Intern. Med. 2020, 180, 817–818. [Google Scholar] [CrossRef]
- Neria, Y.; Nandi, A.; Galea, S. Post-traumatic stress disorder following disasters: A systematic review. Psychol. Med. 2008, 38, 467–480. [Google Scholar] [CrossRef]
- Hiraoka, D.; Tomoda, A. Relationship between parenting stress and school closures due to the COVID-19 pandemic. Psychiatry Clin. Neurosci. 2020, 74, 497–498. [Google Scholar] [CrossRef] [PubMed]
- Stewart, H.; Watson, N.; Campbell, M. The cost of school holidays for children from low income families. Childhood 2018, 25, 516–529. [Google Scholar] [CrossRef] [PubMed]
- Courtemanche, C.; Garuccio, J.; Le, A.; Pinkston, J.; Yelowitz, A. Strong Social Distancing Measures In The United States Reduced The COVID-19 Growth Rate. Health Aff. 2020, 39, 1237–1246. [Google Scholar] [CrossRef] [PubMed]
- Marshall, I.J.; Marshall, R.; Wallace, B.C.; Brassey, J.; Thomas, J. Rapid reviews may produce different results to systematic reviews: A meta-epidemiological study. J. Clin. Epidemiol. 2019, 109, 30–41. [Google Scholar] [CrossRef]
- Gartlehner, G.; Affengruber, L.; Titscher, V.; Noel-Storr, A.; Dooley, G.; Ballarini, N.; König, F. Single-reviewer abstract screening missed 13 percent of relevant studies: A crowd-based, randomized controlled trial. J. Clin. Epidemiol. 2020, 121, 20–28. [Google Scholar] [CrossRef] [PubMed]
| Publication Country Data Source | Study Design/Analysis | Population Characteristics | Types of Interventions Duration of School Closure | Outcomes | Findings |
|---|---|---|---|---|---|
| An, R., 2020 [38] USA Early Childhood Longitudinal Study | Microsimulation model | Children in kindergarten class of 2010–2011 (n = 15,631) were followed from kindergarten through 5th grade 6–10 years | Scenario 1: 2-month nationwide school closure (April and May 2020) with COVID-19 vs. 2-months nationwide school closure in April and May 2020 without COVID-19 | Increase in the body mass index z-scores Childhood obesity prevalence | An increase in the mean BMIz by 0.056 unit An increase in childhood obesity prevalence by 0.640 percentage points |
| Scenario 2: Scenario 1 + 10% reduction in daily physical activity in the summer from June to August | Increase in the body mass index z-scores Childhood obesity prevalence | An increase in the mean BMIz by 0.084 An increase in childhood obesity prevalence by 0.972 percentage points | |||
| Scenario 3: Scenario 2 + 2-month school closure in September and October; November and December | Increase in the body mass index z-scores Childhood obesity prevalence | An increase in the mean BMIz by 0.141 units An increase in childhood obesity prevalence by 1.676 percentage points | |||
| Scenario 4: Scenario 3 + 2-month school closure in November and December | Increase in the body mass index z-scores Childhood obesity prevalence | An increase in the mean BMIz by 0.198 units An increase in childhood obesity prevalence by 2.373 percentage points | |||
| Comparison of the control scenario without the COVID-19 pandemic and the 4 alternative scenarios with COVID-19 | Childhood obesity (BMIz in the 95th percentile or higher in the growth chart) | “Compared to girls and non-Hispanic whites and Asians, the impact of COVID-19 on childhood obesity was modestly larger among boys and non-Hispanic blacks and Hispanics, respectively.” | |||
| Angoulvant, F., 2020 [39] France French surveillance data for pediatric emergency department (PED) visits and related hospital admissions | Quasi-experimental time series analysis | 871,543 pediatric emergency department (PED) visits | School closure + lockdown 18 March 2020 to 19 April 2020. One week after the start of the lockdown | Number of hospital admissions | “A decrease of −45% in hospital admissions in the period from 1 January 2017 to 17 March 2020 and from 18 March 2020 to 19 April 2020.” |
| number of pediatric emergency department (PED) visits for gastroenteritis, bronchiolitis, common cold, acute otitis media | “A decrease of −68% in the overall number of PEDs visits in the period from 1 January 2017 to 17 March 2020 and from 18 March 2020 to 19 April 2020.” “A significant decrease over 70% of acute gastro-enteritis, common cold, bronchiolitis and acute otitis media compared to the expected values. Urinary tract infections were not impacted by the lockdown both regarding overall PEDs visits (−16.4% [−40.8; +6.4]) and hospital admissions (+20.7% [−27.0; +58.5]).” | ||||
| Ijadi-Maghsoodi, R., 2020 [40] Los Angeles, USA Los Angeles County (LAC) Department of Mental Health (DMH) and its network of community mental health clinics providing critical services to youth and families | Report | Youth and families during the pandemic | School closures in the county | Accessibility to resources | “Teachers expressed concerns about under resourced students facing barriers to accessing virtual learning, heightened student anxiety, and difficulty connecting to students in need, all compounded by a compressed timeline. This includes digital disparities and lack of access to computer technology among families and providers.” |
| Masonbrink, A.R., 2020 [41] USA National data from diverse sources on Education Nutrition Physical Health Mental Health Child and Family Safety COVID-19 Response Legislation | Pre-publication Release | All children Children in poverty Children with disabilities | School closure | Challenges related to: Educational losses and attainment Accessibility to critical resources Access to the nutrition program Physical and mental health Psychological impact | “Remote learning presents a challenge for all families, those in poverty are at greater disadvantage and thus at increased risk for widening educational disparities.” “Parents in poverty are facing their own pandemic-related stressors (e.g., unemployment, at-risk jobs) and may lack the time or resources to support remote learning.” “Critical access to the nutrition programs that serve 35 million children living in poverty daily, is typically provided through schools and childcare centers.” “School closure means loss of critical resources for children with disabilities, including engagement with specialized educators and structured learning environments.” “Children now face diminished access to healthcare care because of loss of school-based services, increasing parental unemployment, loss of health insurance, and avoidance of health care settings.” “Since the pandemic began, there have been isolated reports of increased child abuse severity, however, numerous states are reporting an ominous decrease in reports to child protective services (CPS), thought to be related to under-recognition.” |
| Mayurasakorn, K.B., 2020 [15] Thailand National data and observations | Expert-viewpoint | Thai children reside in rural areas Pre-primary and primary school levels | School closure + the national school breakfast and lunch programs | Food and learning insecurity | Schools closure during COVID-19 caused two major threads: When schools close, nutrition is compromised. It is estimated that school feeding programs provide up to 30–50% of a child’s daily nutritional requirements through meals healthier than those prepared at home at the same price. Many children consume only two meals a day and one meal at school is considered high value for children’s growth and development. This would result in almost 270 million missed meals nationwide; for a child who misses school meals this may lead to a 1–2 kg weight loss over the 43 days—close to 5–10% of a child’s total body weight. School closures can bring added financial pressures and risk of child undernutrition for poorer families given the now larger costs of childcare.” “The school closures and childcare restrictions may leave children unattended at home, thereby curtailing children’s learning capacity during school closure. Extended school closures may still lead to widening the learning, health, and nutrition gaps between youth from lower-income and higher-income households. Perhaps worse than educational impediment, an end to the pandemic is yet to arrive, which may lead to grievous economic depression. This can exacerbate existing poverty and as well as children’s nutrition and learning outcomes.” |
| Snapshot of strategies/challenges Analysis | Convenience sample of 9 school districts that were closed as part of social distancing strategies Small low-density, rural school district Urban and suburban schools | School closures 16 March and 20 March 2020 | Distance learning Nutrition programs | “In a small low-density, rural school district with lower reported instances of COVID-19 at the time of implementation, students were sent home without supplemental education material or clear plans for transitioning to distance learning. In low- to middle-income communities and less affluent suburban counties, school districts provided students with study packets, accessed either online or distributed/picked up at school, given the lack of access to reliable Internet and devices.” “More affluent urban and suburban schools used online instruction platforms. Some used a blend of worksheets, online resources, and online instruction, while schools attempted to provide online-capable devices to students in need. Some broadcasted educational material through public access TV channels, social media, and on their websites, while arranging device distribution. Some were also working with Internet service providers to provide low- or no-cost Internet access. One district employed Wi-Fi-equipped school buses throughout the community for students to access. Meals were provided to students using free or reduced meal programs.” | |
| Kılınçel Ş., 2020 [42] Turkey Facebook family groups, and Google Forms questionnaires sent by the child psychiatry clinic to their smartphones. Sociodemographic form, State-Trait anxiety scale, and UCLA loneliness survey were used as data collection tools. | Cross-sectional | 745 adolescents aged between 12 and 18 years 13 different schools | School closure and home-quarantine | Risk of anxiety and loneliness | “Closure of schools and home-quarantine during pandemic causes anxiety and loneliness in young people.” |
| Isumi A., 2020 [37] Japan Public data on suicide statistics Public data on population estimates | Descriptive study | Children under 20 years | School closure between January 2018 and May 2020 | Impact on suicide rates | “The first wave of the COVID-19 pandemic has not significantly affected suicide rates among children and adolescents during the school closure in Japan.” |
| Baron E.J., 2020 [36] Florida, USA Country and district-level data Florida DCF | Descriptive study | School staffing for each of the 67 counties in Florida | School closure March to April 2020 | The number of child maltreatment allegations | “A counterfactual distribution of child maltreatment allegations for March and April 2020, the first two months in which Florida schools closed. The actual number of reported allegations was approximately 15,000 less (27%) than expected for these two months.” |
| Di Giorgio E., 2020 [35] Italy Subjective Time Questionnaire (STQ) The Behavior Rating Inventory of Executive Functions—preschool version (BRIEF-P) Executive Functions (EF) Self-Control Index (ISCI) | Survey | 245 mothers and their pre-school children aged between 2 and 5 years | Closure of schools, individual home confinement, and the related social restrictions from 1st to the 9th of April (after three weeks of confinement) compared to the week before the national lockdown | Mothers and their pre-school children’s behavioral habits (i.e., sleep timing and quality, subjective time experience) and psychological well-being (i.e., emotion regulation, self-regulation capacity). | “Restrictive measures had negative effects on mothers’ and their children’s behavioral and psychological levels, with some differences depending on the mothers working situation.” “Besides their and their mothers’ sleep quality, children’s inhibitory self-control capacity seemed to be also associated with mothers’ trait emotional fatigue. Children’s sleep quality was, on average, less affected by the lockdown, although their sleep timing strongly shifted (they went to bed ~53 min and woke up ~66 min later than usual). These changes, together with reported difficulties of following routines, indicate a substantial breakdown in their daily routines.” “Mothers reported an increasing level of emotional symptoms such as sadness and frustration, whereas they perceived their children as more undisciplined and hyperactive, with a worsening inhibitory self-control capacity.” |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chaabane, S.; Doraiswamy, S.; Chaabna, K.; Mamtani, R.; Cheema, S. The Impact of COVID-19 School Closure on Child and Adolescent Health: A Rapid Systematic Review. Children 2021, 8, 415. https://doi.org/10.3390/children8050415
Chaabane S, Doraiswamy S, Chaabna K, Mamtani R, Cheema S. The Impact of COVID-19 School Closure on Child and Adolescent Health: A Rapid Systematic Review. Children. 2021; 8(5):415. https://doi.org/10.3390/children8050415
Chicago/Turabian StyleChaabane, Sonia, Sathyanarayanan Doraiswamy, Karima Chaabna, Ravinder Mamtani, and Sohaila Cheema. 2021. "The Impact of COVID-19 School Closure on Child and Adolescent Health: A Rapid Systematic Review" Children 8, no. 5: 415. https://doi.org/10.3390/children8050415
APA StyleChaabane, S., Doraiswamy, S., Chaabna, K., Mamtani, R., & Cheema, S. (2021). The Impact of COVID-19 School Closure on Child and Adolescent Health: A Rapid Systematic Review. Children, 8(5), 415. https://doi.org/10.3390/children8050415







