Outcome Quality of Inpatient and Day-Clinic Treatment in Child and Adolescent Psychiatry—A Naturalistic Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Measures
2.2. Instruments
2.3. Statistical Analysis
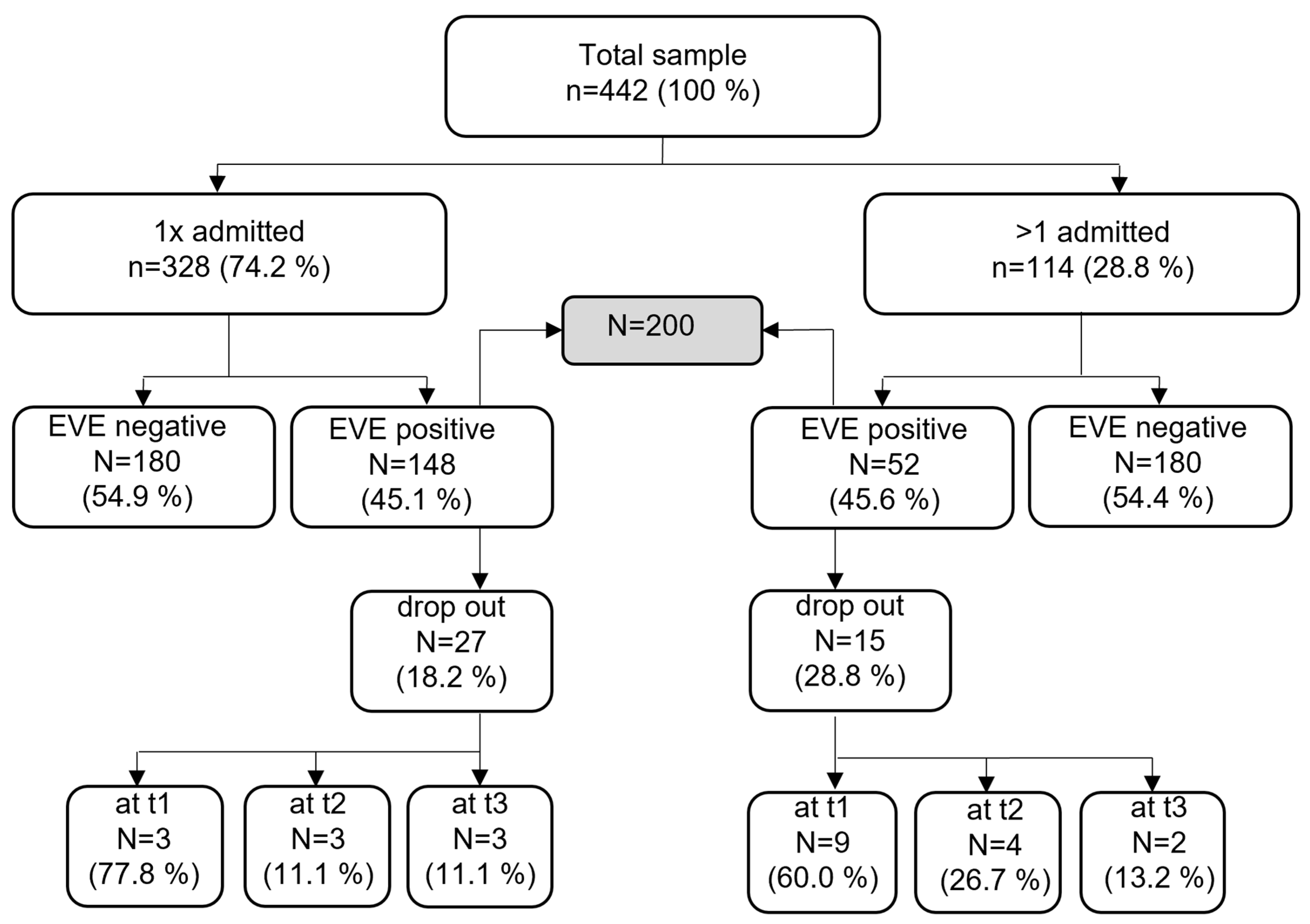
Sample Characteristics
3. Results
3.1. Treatment Success—Reduction of Psychopathology
3.2. Treatment Satisfaction
3.3. Quality of Life
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Sample Characteristics | Total Sample | Sample with Positive EVE | Sample with Negative EVE | |
|---|---|---|---|---|
| n (%) | n (%) | n (%) | ||
| (Total) Age | 442 (100) | 200 (100) | 242 (100) | |
| ≤6 years (Children 2) | 5 (1.1) | 4 (2) | 1 (0.4) | |
| ≥7 to ≤13 years (underage minors 2) | 105 (23.8) | 45 (22.5) | 60 (24.8) | |
| ≥14 to ≤17 years (minors of age 3) | 311 (70.4) | 135 (67.5) | 176 (72.7) | |
| ≥18 years (Adults 3) | 21 (4.8) | 16 (8) | 5 (2.1) | |
| Sex | ||||
| female | 250 (56.6) | 120 (60) | 130 (53.7) | |
| male | 192 (43.4) | 80 (40) | 112 (46.3) | |
| Diagnosis 1 at T2 | - | 197 (98.5) | 0 (0) | |
| F3 | 23 (11.5) | |||
| F4 | 74 (37.0) | |||
| F5 | 33 (16.5) | |||
| F9 | 50 (25.0) | |||
| Other (F1, F2, F6, F8) | 17 (8.5) | |||
| Missing | 3 (1.5) | |||
| Hospitalization form | ||||
| planned | 133 (30.1) | 98 (49) | 35 (14.5) | |
| unplanned | 309 (69.9) | 102 (51) | 207 (85.5) | |
| Type of stay | ||||
| Crisis stay | 322 (72.9) | 114 (57) | 208 (86) | |
| Orientation stay | 97 (21.9) | 67 (33.5) | 30 (12.4) | |
| Project stay | 23 (5.2) | 19 (9.5) | 4 (1.7) | |
| Department | ||||
| Day-clinical stay | 63 (14.3) | 46 (23) | 17 (7) | |
| In-patient stay | 379 (85.7) | 154 (77) | 225 (93) | |
| Duration of stay | ||||
| ≤1 day | 96 (21.7) | 5 (2.5) | 91 (37.6) | |
| ≥2 to ≤7 days | 132 (29.9) | 33 (16.5) | 99 (40.9) | |
| ≥8 to ≤41 days | 105 (23.8) | 68 (34) | 37 (15.3) | |
| ≥42 days | 109 (24.7) | 94 (47) | 15 (6.2) | |
| Legal basis of inpatient admission 1 | - | 192 (100) | 0 (0) | |
| voluntary | 152 (79.2) | |||
| according to § 8 UBG | 25 (13) | |||
| according to § 9 UBG | 1 (0.5) | |||
| by court order | 1 (0.5) | |||
| other | 13 (6.8) | |||
| Legal duty of custody 1 | - | 192 (100) | 0 (0) | |
| father | 9 (4.7) | |||
| mother | 69 (35.9) | |||
| both parents | 97 (50.5) | |||
| youth welfare | 7 (3.6) | |||
| other | 10 (5.2) | |||
| Parents’ school-leaving qualification 1 | - | 368 (100) | 0 (0) | |
| No school-leaving qualification | Mother | 2 (0.5) | ||
| Father | 0 (0) | |||
| Special education school | Mother | 1 (0.3) | ||
| Father | 2 (0.5) | |||
| Secondary school | Mother | 41 (11.1) | ||
| Father | 19 (5.2) | |||
| Apprenticeship | Mother | 63 (17.1) | ||
| Father | 71 (19.3) | |||
| Abitur/A-Level/vocational baccalaureate diploma | Mother | 38 (10.3) | ||
| Father | 26 (7.1) | |||
| University degree | Mother | 22 (6) | ||
| Father | 26 (7.1) | |||
| Unknown | Mother | 17 (4.6) | ||
| Father | 40 (10.9) | |||
References
- Ärzteausbildungsordnung (Medical Doctors’ Education Regulation). Regulation of the Federal Minister of Health on Training as a General Practitioner and as a Specialist; 2015,) StF: BGBl. II Nr. 147/2015 §15(1)13. Available online: https://www.ris.bka.gv.at/GeltendeFassung.wxe?Abfrage=Bundesnormen&Gesetzesnummer=20009186 (accessed on 10 October 2021).
- Philipp, J.; Zeiler, M.; Waldherr, K.; Nitsch, M.; Dür, W.; Karwautz, A.; Wagner, G. The Mental Health in Austrian Teenagers (MHAT)-Study: Preliminary results from a pilot study. Neuropsychiatrie 2014, 28, 198–207. [Google Scholar] [CrossRef]
- Beck, N.; Warnke, A. Youth welfare needs after inpatient child and adolescent psychiatric treatment. Zschr. Kinder Und Jugen Psychiatr. Psychother. 2009, 37, 57–67. [Google Scholar] [CrossRef]
- Fliedl, R.; Ecker, B.; Karwautz, A. Child and adolescent psychiatric care 2019 in Austria—Steps of care, current state and lookout. Neuropsychiatrie 2020, 34, 179–188. [Google Scholar] [CrossRef]
- Bickman, L.; Noser, K. Meeting the challenges in the delivery of child and adolescent mental health services in the next millennium: The continuous quality improvement approach. Appl. Prev. Psychol. 1999, 8, 247–255. [Google Scholar] [CrossRef]
- Kunkel, S.; Rosenquist, U.; Westerling, R. The structure of quality systems is important to the process and outcome, an empirical study of 386 hospital departments in Sweden. BMC Health Serv. Res. 2007, 7, 104. [Google Scholar] [CrossRef]
- Thun-Hohenstein, L. Care situation of psychologically conspicuous and sick children and adolescents. In Kindermedizin–Werte Versus Ökonomie; Kerbl, R., Thun-Hohenstein, L., Vavrik, K., Waldhauser, F., Eds.; Springer: Berlin/Heidelberg, Germany, 2008; pp. 163–175. [Google Scholar]
- de Shazer, S.; Berg, I.K.; Lipchik, E.; Nunnally, E.; Molnar, A.; Gingerich, W.; Weiner-Davis, M. Brief Therapy: Focused Solution Development. Fam. Process. 1986, 25, 207–221. [Google Scholar] [CrossRef] [PubMed]
- Schweitzer, J.; Beher, S.; Sydow, K.; Retzlaff, R. Systemic therapy / family therapy. Psychotherapeutenjournal 2007, 1, 4–19. [Google Scholar]
- Walter, G. Inpatient treatment as transition. Systeme 1998, 12, 52–62. [Google Scholar]
- Working Group Systemic Therapy. Statement on the Theory and Practice of Systemic Therapy. 2009. Available online: https://www.dgsf.org/themen/berufspolitik/berufspolitik-bis2005/agst_stellungn_wiss_beirat.html (accessed on 25 June 2020).
- Rotthaus, W. Systemic child and adolescent psychiatry and psychotherapy. In Paar-Und Familientherapie; Wirsching, M., Scheib, P., Eds.; Springer: Berlin/Heidelberg, Germany, 2002; pp. 525–535. [Google Scholar]
- Thun-Hohenstein, L. Participation of children and adolescents in child and adolescent psychiatry. Paediatr. Paedol. 2014, 49, 42–47. [Google Scholar] [CrossRef]
- Heekerens, H.P. From the laboratory to the field. Psychotherapeut 2005, 50, 357–366. [Google Scholar] [CrossRef]
- Falissard, B. How should we evaluate non-pharmacological treatments in child and adolescent psychiatry. Eur. Child Adolesc. Psychiatry 2015, 24, 1011–1013. [Google Scholar] [CrossRef][Green Version]
- Mattejat, F.; Trosse, M.; John, K.; Bachmann, M.; Remschmidt, H. Model Research Project on the Quality of Outpatient Child and Adolescent Psychiatric Treatments, Final Report; Görich & Weiershäuser: Marburg, Germany, 2006. [Google Scholar]
- Mattejat, F.; Remschmidt, H. The assessment of therapy outcome in child and adolescent psychiatry under naturalistic conditions—Conception and implementation of the Marburg System of Quality Assurance and Therapy Evaluation. Z. Kinder Jugendpsychiatrie Psychother. 2006, 34, 445–454. [Google Scholar] [CrossRef]
- Katzenschläger, P.; Fliedl, R.; Popow, C.; Kundi, M. Quality of life and satisfaction with inpatient treatment in adolescents with psychiatric disorders. Neuropsychiatrie 2018, 32, 75–83. [Google Scholar] [CrossRef]
- Reinelt, P.D. Treatment Assessment and Quality of Life in Child and Adolescent Psychiatry Inventories, Progress and Correlation Analyses. Bachelor’ Thesis, University of Klagenfurt, Klagenfurt, Austria, 2010. Available online: https://netlibrary.aau.at/obvuklhs/content/titleinfo/2413418 (accessed on 25 June 2021).
- Bachmann, M.; Bachmann, C.J.; John, K.; Heinzel-Gutenbrunner, M.; Remschmidt, H.; Mattejat, F. The effectiveness of child and adolescent psychiatric treatments in a naturalistic outpatient setting. World Psychiatry 2010, 9, 111–117. [Google Scholar] [CrossRef][Green Version]
- Bredel, S.; Brunner, R.; Haffner, J.; Resch, F. Treatment success, treatment experience and treatment satisfaction from the point of view of patients, parents and therapists—results of an evaluative study from inpatient child and adolescent psychiatry. Prax. Kinder Jugendpsychiatrie Psychol. 2004, 53, 256–276. [Google Scholar]
- Fleischhaker, C.; Bock, K.; Hennighausen, K.; Horwath, D.; Kuhn-Hennighausen, C.; Rauh, R.; Wewetzer, G.; Drömann, S.; Schulz, E. 20-year catamnesis of the child and adolescent psychiatric and psychosomatic clinic Haus Vogt. Z. Kinder Jugendpsychiatrie Psychother. 2008, 36, 191–203. [Google Scholar] [CrossRef] [PubMed]
- Gutknecht, H. Patients’ evaluation of day-to-day clinical treatment–aspects of treatment experiences and changes experienced. Psychiatr. Prax. 2005, 32, 342–348. [Google Scholar] [CrossRef]
- Cropp, C.; Streeck-Fischer, A.; Jaeger, U.; Masuhr, O.; Schröder, A.; Leichsenring, F. The relationship between treatment experience and treatment success in inpatient psychotherapy with children and adolescents. Z. Kinder Jugendpsychiatrie Psychother. 2008, 36, 205–213. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, S.; Busner, J.; Chibnall, J.; Kang, G. Consumer satisfaction at a child and adolescent state psychiatric hospital. Psychiatr. Serv. 2001, 52, 202–206. [Google Scholar] [CrossRef] [PubMed]
- Renneberg, B.; Lippke, S. Quality of life. In Gesundheitspsychologie; Renneberg, B., Hammelstein, P., Eds.; Springer: Berlin/Heidelberg, Germany, 2006; pp. 29–33. [Google Scholar]
- Reinecke, M.A.; Shirk, S.R. Psychotherapy with adolescents. In Oxford Textbook of Psychotherapy; Gabbard, G.O., Beck, J.S., Holmes, J., Eds.; University Press Oxford: Oxford, UK, 2005; pp. 353–366. [Google Scholar]
- Jozefiak, T.; Larsson, B.; Wichstrøm, L.; Wallander, J.; Mattejat, F. Quality of Life as reported by children and parents: A comparison between students and child psychiatric outpatients. Health Qual. Life Outcomes 2010, 8, 136. [Google Scholar] [CrossRef]
- Balazs, J.; Miklosi, M.; Halasz, J.; Horváth, L.O.; Szentiványi, D.; Vida, P. Suicidal Risk, Psychopathology, and Quality of Life in a Clinical Population of Adolescents. Front. Psychiatry 2018, 9, 17. [Google Scholar] [CrossRef] [PubMed]
- Bastiaansen, D.; Koot, H.M.; Ferdinand, R.F. Determinants of quality of life in children with psychiatric disorders. Qual. Life Res. 2005, 14, 1599–1612. [Google Scholar] [CrossRef]
- Baumgarten, F.; Cohrdes, C.; Schienkiewitz, A.; Thamm, R.; Meyrose, A.K.; Ravens-Sieberer, U. Health-related quality of life and its relation to chronic diseases and mental health problems among children and adolescents: Results from KiGGS Wave 2. Bundesgesundheitsblatt Gesundh. Gesundh. 2019, 62, 1205–1214. [Google Scholar] [CrossRef] [PubMed]
- Mattejat, F.; Simon, B.; König, U.; Quaschner, K.; Barchewitz, C.; Felbel DKatzenski, B. Quality of life in mentally ill children and adolescents: Results of the first multicenter study with the inventory for recording the quality of life in children and adolescents (ILK). J. Child Adolesc. Psychiatry Psychother. 2003, 31, 293–303. [Google Scholar] [CrossRef]
- Flechtner, H.; Möller, K.; Kranendonk, S.; Luther, S.; Lehmkuhl, G. On the subjective quality of life of children and adolescents with mental disorders: Development and validation of a new survey instrument. Prax. Kinderpsychol. Kinderpsychiatr. 2002, 51, 77–91. [Google Scholar]
- Ravens-Sieberer, U.; Erhart, M.; Wille, N.; Bullinger, M.; BELLA Study Group. Health-related quality of life in children and adolescents in Germany: Results of the BELLA study. Europ. Child Adolesc. Psychiatr. 2008, 17, 148–156. [Google Scholar] [CrossRef] [PubMed]
- Kamp-Becker, I.; Schröder, J.; Muehlan, H.; Remschmidt, H.; Becker, K.; Bachmann, C.J. Health-related quality of life in children and adolescents with autism spectrum disorder. Z. Kinder Jugendpsychiatr Psychoth. 2011, 39, 123–131. [Google Scholar] [CrossRef]
- Döpfner, M.; Plück, J.; Kinnen, C. German School-Age Forms of the Child Behavior Checklist by Thomas, M. Achenbach: Parent Questionnaire on Child and Adolescent Behavior (CBCL/6-18R), Teacher Questionnaire on Child and Adolescent Behavior (TRF/6-18R), Questionnaire for Adolescents (YSR/11-18R]; Hogrefe: Göttingen, Germany, 2014. [Google Scholar]
- Mattejat, F.; Remschmidt, H. Questionnaires for Treatment Satisfaction; Hogrefe: Göttingen, Germany, 1998. [Google Scholar]
- Mattejat, F.; Remschmidt, H. Inventory for Quality of Life in Children and Adolescents; Huber Bern: Edison, NJ, USA, 2006. [Google Scholar]
- Becker, K.D.; Chorpita, B.F.; Daleiden, E.L. Improvement in Symptoms Versus Functioning: How do our best treatments measure up? Adm. Policy Ment. Health 2011, 38, 440–458. [Google Scholar] [CrossRef]
- Ballesteros-Urpi, A.; Slade, M.; Manley, D.; Pardo-Hernandez, H. Conceptual framework for personal recovery in mental health among children and adolescents: A systematic review and narrative synthesis protocol. BMJ Open 2019, 9, e029300. [Google Scholar] [CrossRef]
- Patton, G.C.; Coffey, C.; Romaniuk, H.; Mackinnon, A.; Carlin, J.B.; Degenhardt, L.; Olsson, C.A.; Moran, P. The prognosis of common mental disorders ion adolescents: A 14-year prospective study. Lancet 2014, 383, 1404–1411. [Google Scholar] [CrossRef]
- Schneidtinger, C.; Haslinger-Baumann, E. The lived experience of adolescent user of mental health services in Vienna, Austria: A qualitative study of personal recovery. J. Adolesc. Psychiatr. Nurs. 2019, 32, 112–121. [Google Scholar] [CrossRef] [PubMed]
- Bickman, L.; Nurcombe, B.; Townsend, C.; Belle, M.; Schut, J.; Karver, M. Consumer Measurement Systems in Child and Adolescent Mental Health; ACT: Canberra, Australia, 1998. [Google Scholar]
- Kelly, S.D.; Bickman, L. Beyond outcomes monitoring: Measurement feedback systems in child and adolescent practice. Curr. Opin. Psychiatry 2009, 22, 363–368. [Google Scholar] [CrossRef] [PubMed]
| T1 | T2 | T3 | |
|---|---|---|---|
| FBB | |||
| Therapists n (%) | 131 (68.23) | ||
| Therapists total score M (SD) | 2.79 (0.51) | ||
| Patients n (%) | 128 (66.67) | ||
| Patients total score M (SD) | 2.98 (0.65) | ||
| Main caregivers n (%) | 99 (51.6) | ||
| Main caregivers total score M (SD) | 3.28 (0.57) | ||
| CBCL n (%) | 113 (54.5) | 105 (52.5) | 96 (48) |
| Externalizing problems M (SD) | 61.89 (10.67) | 58.08 (9.74) | 57.13 (10.51) |
| Internalizing problems M (SD) | 69.73 (8.92) | 64.50 (9.27) | 61.68 (11.44) |
| Total problems M (SD) | 69.67 (8.13) | 64.23 (8.45) | 61.72 (10.83) |
| YSR n (%) | 164 (82) | 122 (61) | 104 (52) |
| Externalizing problems M (SD) | 58.05 (9.86) | 54.12 (9.89) | 53.02 (9.87) |
| Internalizing problems M (SD) | 65.98 (9.88) | 60.24 (11.26) | 57.47 (11.15) |
| Total problems M (SD) | 65.48 (9.06) | 59.41 (10.89) | 57.31 (10.26) |
| ILK | |||
| Main caregivers n (%) | 116 (58) | 105 (52.5) | 96 (48) |
| Problem score PR0–7 M (SD) | 3.73 (1.67) | 2.47 (1.86) | 2.55 (2.07) |
| Quality-of-life score LQ0–28 M (SD) | 16.41 (4.16) | 19.36 (3.90) | 19.47 (4.50) |
| Adolescents n (%) | 148 (74) | 111 (55.5) | 94 (47) |
| Problem score PR0–7 M (SD) | 3.34 (1.59) | 2.08 (1.97) | 1.96 (1.86) |
| Quality-of-life score LQ0–28 M (SD) | 17.55 (4.01) | 20.69 (4.48) | 21.01 (4.25) |
| Children n (%) | 28 (14) | 26 (13) | 23 (11.5) |
| Problem score PR0–7 M (SD) | 2.75 (1.69) | 2.15 (1.49) | 2.3 (2.12) |
| Quality-of-life score LQ0–28 M (SD) | 19.18 (4.36) | 21.58 (3.84) | 21.00 (5.55) |
| Measuring Instrument | Perspective | T1 Median | T2 Median | T3 Median | χ2 Test Statistics |
|---|---|---|---|---|---|
| YSR | Patients’ self-report | ||||
| YSR-INT (n = 99) | 21 | 13 | 10 | 76.85 *** | |
| YSR-EXT (n = 99) | 13 | 10 | 9 | 36.14 *** | |
| YSR-GES (n = 99) | 58 | 40 | 35 | 84.80 *** | |
| CBCL | Main caregivers’ rating | ||||
| CBCL-INT (n = 87) | 20 | 13 | 11.5 | 57.91 *** | |
| CBCL-EXT (n = 86) | 13.5 | 10 | 8.5 | 56.38 *** | |
| CBCL-GES (n = 86) | 57.5 | 37 | 34 | 80.07 *** | |
| ILK | Children’s self-report (n = 24) | ||||
| ILK-PR0–7 | 3.00 | 2.00 | 2.00 | 2.03 | |
| ILK-LQ0–28 | 19.00 | 21.00 | 22.00 | 10.17 ** | |
| Adolescents’ self-report (n = 112) | |||||
| ILK-PR0–7 | 4.00 | 2.00 | 2.00 | 78.42 *** | |
| ILK-LQ0–28 | 18.00 | 21.00 | 21.00 | 85.19 *** | |
| Main caregivers’ rating (n = 97) | |||||
| ILK-PR0–7 | 4.00 | 3.00 | 2.00 | 48.47 *** | |
| ILK-LQ0–28 | 16.00 | 20.00 | 20.00 | 63.46 *** |
| Quality Measure | Submeasure | Caregivers | Patients | ||
|---|---|---|---|---|---|
| Mean % | Mean * Mean | Mean % | Mean * Mean | ||
| Outcome Quality | personal success | 73.3 ± 13.7 | 3.2 ± 0.4 | 74.9 ± 5.0 | 3.0 ± 0.2 |
| family success | 92.1 | 3.6 ± 0.7 | 53.3 | 2.6 ± 1.3 | |
| Process Quality | relation to therapist | 83.8 ± 14.2 | 3.3 ± 0.4 | 85.4 ± 5.6 | 3.3 ± 0.1 |
| framework conditions | 81.5 ± 5.8 | 3.1 ± 0.2 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Thun-Hohenstein, L.; Weltjen, F.; Kunas, B.; Winkler, R.; Fritz, C. Outcome Quality of Inpatient and Day-Clinic Treatment in Child and Adolescent Psychiatry—A Naturalistic Study. Children 2021, 8, 1175. https://doi.org/10.3390/children8121175
Thun-Hohenstein L, Weltjen F, Kunas B, Winkler R, Fritz C. Outcome Quality of Inpatient and Day-Clinic Treatment in Child and Adolescent Psychiatry—A Naturalistic Study. Children. 2021; 8(12):1175. https://doi.org/10.3390/children8121175
Chicago/Turabian StyleThun-Hohenstein, Leonhard, Franka Weltjen, Beatrix Kunas, Roman Winkler, and Corinna Fritz. 2021. "Outcome Quality of Inpatient and Day-Clinic Treatment in Child and Adolescent Psychiatry—A Naturalistic Study" Children 8, no. 12: 1175. https://doi.org/10.3390/children8121175
APA StyleThun-Hohenstein, L., Weltjen, F., Kunas, B., Winkler, R., & Fritz, C. (2021). Outcome Quality of Inpatient and Day-Clinic Treatment in Child and Adolescent Psychiatry—A Naturalistic Study. Children, 8(12), 1175. https://doi.org/10.3390/children8121175






