Links between Autism Spectrum Disorder Diagnostic Status and Family Quality of Life
Abstract
:1. Introduction
- How does the presence of ASD diagnosis impact upon family quality of life and stress?
- How is the relationship between diagnostic status and quality of life/stress mediated by: severity of ASD; presence of challenging behaviours; access to services?
- What are the characteristics of a young person with signs of ASD that is not diagnosed?
2. Results
- Having additional needs, a negative SCQ screening score and no diagnosis of ASD (n = 41).
- Having additional needs, a positive SCQ screening score and an existing clinical diagnosis of ASD (n = 18).
- Having additional needs, a positive SCQ screening score but no existing clinical diagnosis of ASD (n = 17).
- Typically developing (TD), age-matched controls (n = 17).
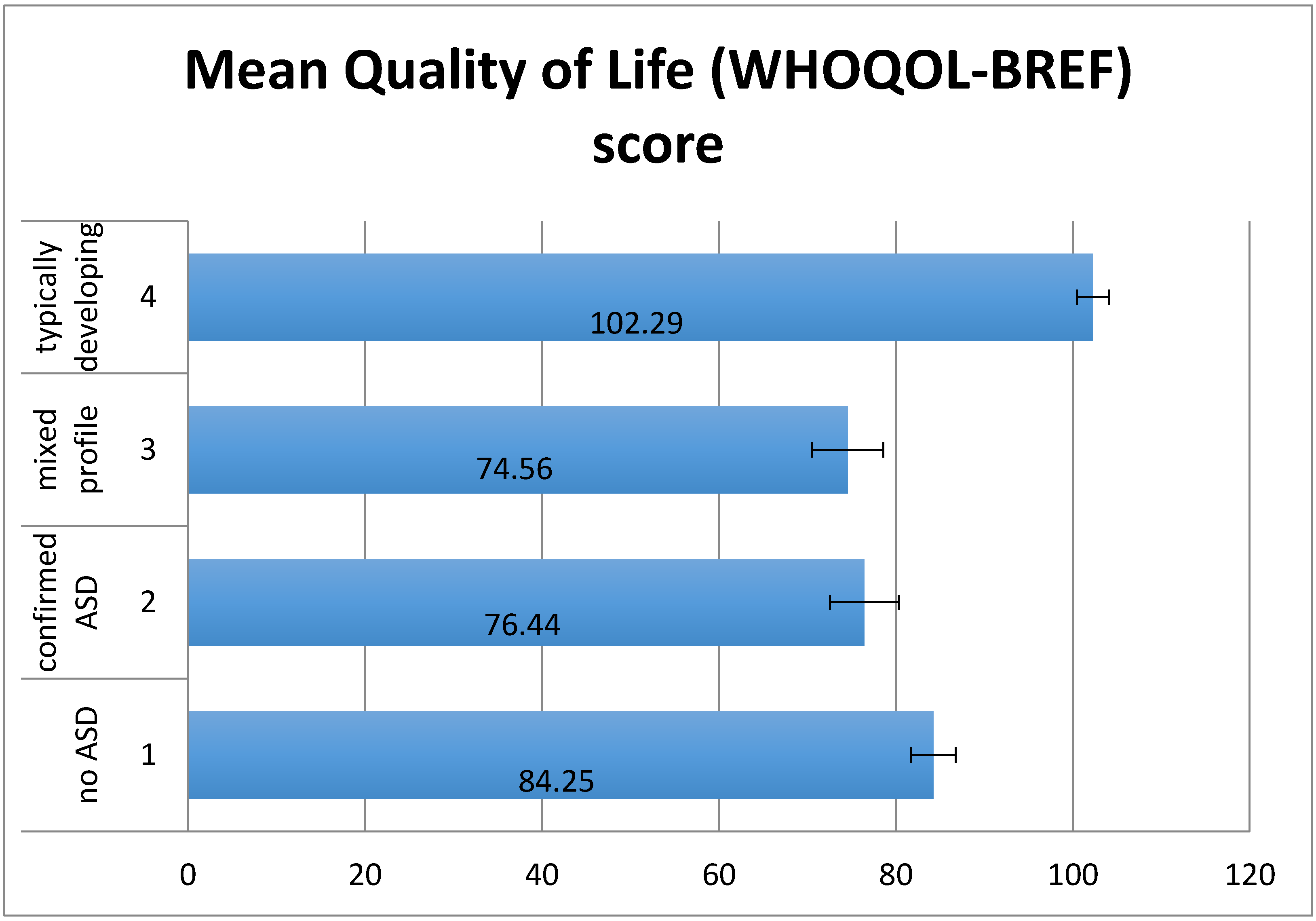
2.1. Impact of ASD Diagnosis on Maternal Quality of Life and Stress
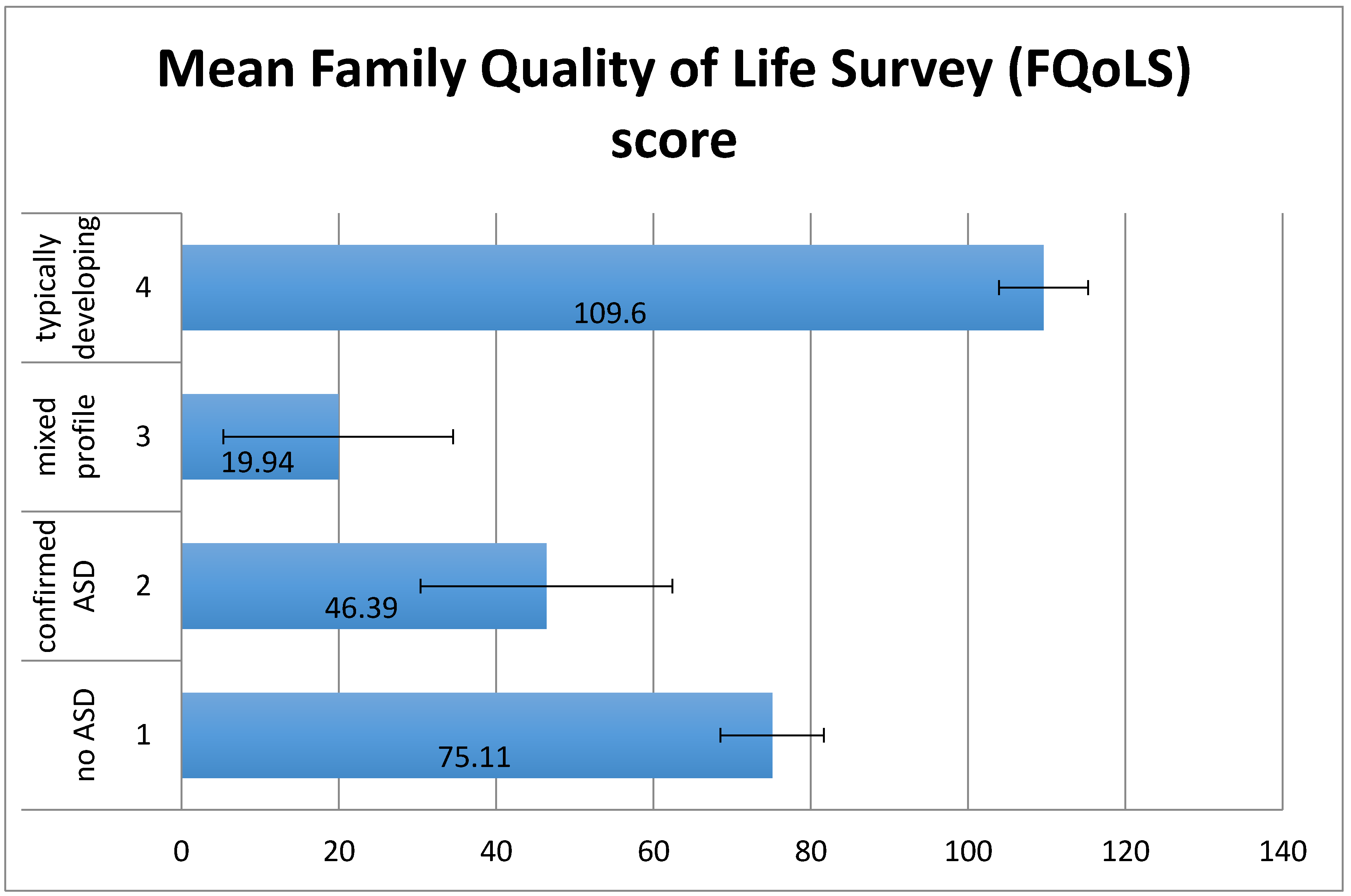
2.2. Impact of ASD Diagnosis on Family Quality of Life
2.3. Impact of ASD Features, Challenging Behaviour and Service Access
2.4. Characteristics of Participants with and without an ASD Diagnosis
3. Discussion
What Factors Explain Group Differences?
4. Materials and Methods
4.1. Participants and Procedure
4.2. Measures
4.2.1. Background Questionnaire
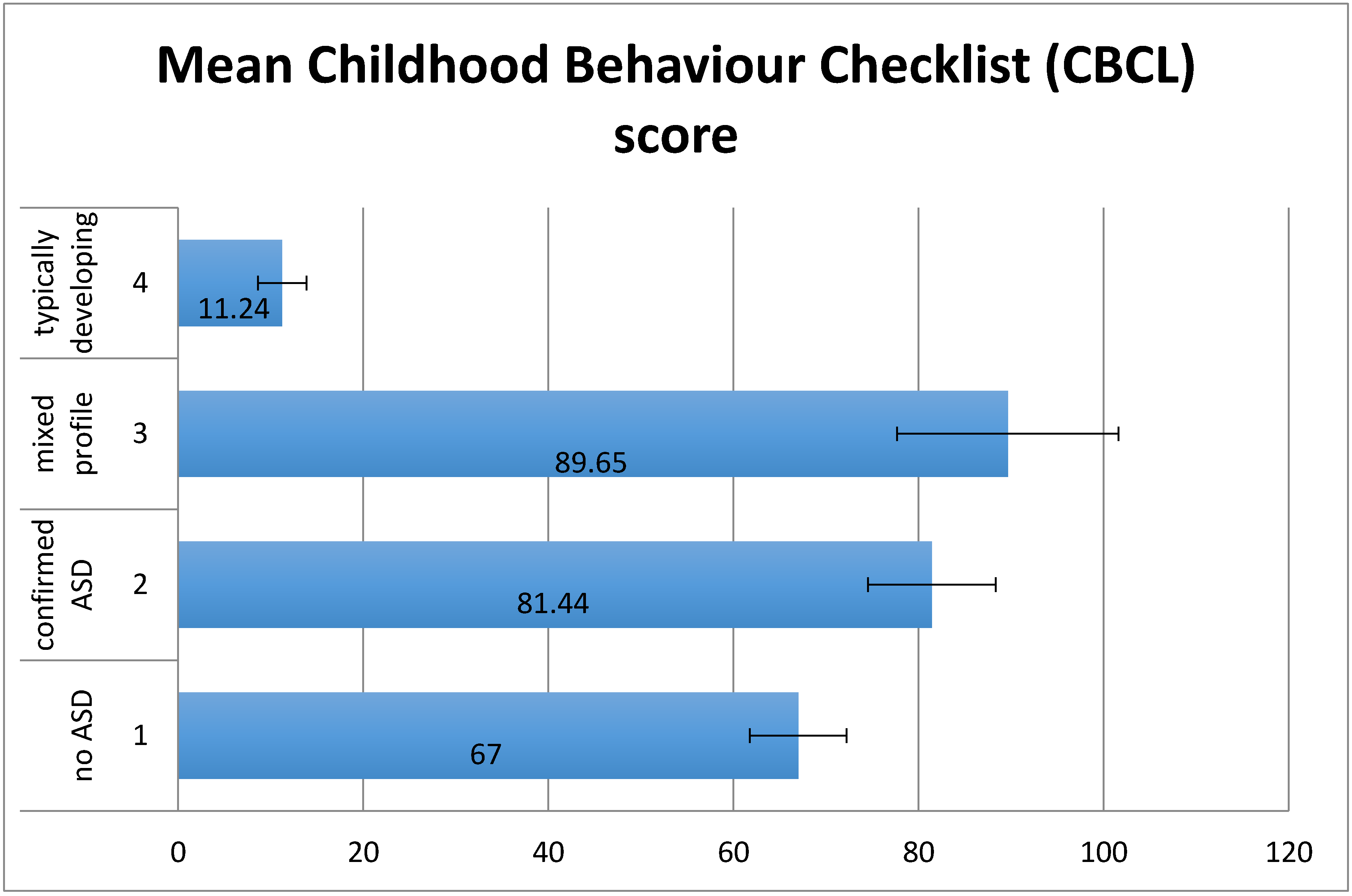
4.2.2. Child Behaviour Checklist (CBCL)
4.2.3. Social Communication Questionnaire (SCQ)
4.2.4. Quality of Life; WHOQOL-BREF
4.2.5. Family Quality of Life Survey (FQoLS)
4.2.6. Family Stress and Coping Interview (FSCI)
4.3. Data Analysis
Acknowledgments
Author Contributions
Conflicts of Interest
References
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders (5th ed.); American Psychiatric Publishing: Washington, DC, USA, 2013. [Google Scholar]
- Elsabbagh, M.; Divan, G.; Koh, Y.J.; Kim, Y.S.; Kauchali, S.; Marcin, C.; Montiel-Nava, C.; Patel, V.; Paula, C.S.; Wang, C.; et al. Global prevalence of autism and other pervasive developmental disorders. Autism Res. 2012, 5, 160–179. [Google Scholar]
- Simonoff, E.; Pickles, A.; Charman, T.; Chandler, S.; Loucas, T.; Baird, G. Psychiatric disorders in children with autism spectrum disorders: Prevalence, comorbidity, and associated factors in a population-derived sample. J. Am. Acad. Child Adolesc. Psychiatry 2008, 47, 921–929. [Google Scholar] [CrossRef] [PubMed]
- McClintock, K.; Hall, S.; Oliver, C. Risk markers associated with challenging behaviours in people with intellectual disabilities: A meta-analytic study. J. Intellect Disabil. Res. 2003, 47, 405–416. [Google Scholar] [CrossRef] [PubMed]
- Matson, J.L.; Rivet, T.T. Characteristics of challenging behaviours in adults with autistic disorder, PDD-NOS, and intellectual disability. J. Intellect Dev. Disabil. 2008, 33, 323–329. [Google Scholar] [CrossRef] [PubMed]
- Stores, R.; Stores, G.; Fellows, B.; Buckley, S. Daytime behaviour problems and maternal stress in children with down’s syndrome, their siblings, and non- intellectually disabled and other intellectually disabled peers. J. Intellect Disabil. Res. 1998, 42, 228–237. [Google Scholar] [CrossRef] [PubMed]
- Zablotsky, B.; Anderson, C.; Law, P. The association between child autism symptomatology, maternal quality of life, and risk for depression. J. Autism Dev. Disord. 2013, 43, 1946–1955. [Google Scholar] [CrossRef] [PubMed]
- Fombonne, E.; Simmons, H.; Ford, T.; Meltzer, H.; Goodman, R. Prevalence of pervasive developmental disorders in the british nationwide survey of child mental health. J. Am. Acad. Child Adolesc. Psychiatry 2001, 40, 820–827. [Google Scholar] [CrossRef] [PubMed]
- Wolf, L.C.; Noh, S.; Fisman, S.N.; Speechley, M. Psychological effects of parenting stress on parents of autistic children. J. Autism Dev. Disord. 1989, 19, 157–166. [Google Scholar] [CrossRef] [PubMed]
- Dillenburger, K.; Jordan, J.A.; McKerr, L.; Keenan, M. The millennium child with autism: Early childhood trajectories for health, education and economic wellbeing. Dev. Neurorehabil. 2015, 18, 37–46. [Google Scholar] [CrossRef] [PubMed]
- Blacher, J.; McIntyre, L.L. Syndrome specificity and behavioural disorders in young adults with intellectual disability: Cultural differences in family impact. J. Intellect Disabil. Res. 2006, 50, 184–198. [Google Scholar] [CrossRef] [PubMed]
- Douma, J.C.; Dekker, M.C.; Koot, H.M. Supporting parents of youths with intellectual disabilities and psychopathology. J. Intellect Disabil. Res. 2006, 50, 570–581. [Google Scholar] [CrossRef] [PubMed]
- Hassall, R.; Rose, J.; McDonald, J. Parenting stress in mothers of children with an intellectual disability: The effects of parental cognitions in relation to child characteristics and family support. J. Intellect Disabil. Res. 2005, 49, 405–418. [Google Scholar] [CrossRef] [PubMed]
- Autistic Spectrum Disorders Needs Assessment Report (2001): Scottish Executive Report on Implementation and Next Steps; Scottish Executive: Edinburgh, Scotland, 2006.
- McKenzie, K.; Forsyth, K.; O’Hare, A.; McClure, I.; Rutherford, M.; Murray, A.; Irvine, L. Factors influencing waiting times for diagnosis of autism spectrum disorder in children and adults. Res. Dev. Disabil. 2015, 45–46, 300–306. [Google Scholar] [CrossRef] [PubMed]
- Keenan, M.; Dillenburger, K.; Doherty, A.; Byrne, T.; Gallagher, S. The experiences of parents during diagnosis and forward planning for children with autism spectrum disorder. J. Appl. Res. Intellect Disabil. 2010, 23, 390–397. [Google Scholar] [CrossRef]
- Crane, L.; Chester, J.W.; Goddard, L.; Henry, L.A.; Hill, E. Experiences of autism diagnosis: A survey of over 1000 parents in the united kingdom. Autism 2016, 20, 153–162. [Google Scholar] [CrossRef] [PubMed]
- Howlin, P.; Moore, A. Diagnosis in autism: A survey of over 1200 patients in the uk. Autism 1997, 1, 135–162. [Google Scholar] [CrossRef]
- Howlin, P.; Asgharian, A. The diagnosis of autism and asperger syndrome: Findings from a survey of 770 families. Dev. Med. Child Neurol. 1999, 41, 834–839. [Google Scholar] [CrossRef] [PubMed]
- Berument, S.R.M.; Lord, C.; Pickles, A.; Bailey, A. Autism screening questionnaire: Diagnostic validity. Br. J. Psychiatry 1999, 175, 444–451. [Google Scholar] [CrossRef] [PubMed]
- Wechsler, D. Wechsler adult intelligence scale, 3rd ed.; The Psychological Corporation: London, UK, 1999. [Google Scholar]
- Wechsler, D. Wechsler intelligence scale for children, 3rd ed.; The Psychological Corporation: London, UK, 1992. [Google Scholar]
- Lecavalier, L.; Leone, S.; Wiltz, J. The impact of behaviour problems on caregiver stress in young people with autism spectrum disorders. J. Intellect Disabil. Res. 2006, 50, 172–183. [Google Scholar] [CrossRef] [PubMed]
- Chamak, B.; Bonniau, B.; Oudaya, L.; Ehrenberg, A. The autism diagnostic experiences of french parents. Autism 2011, 15, 83–97. [Google Scholar] [CrossRef] [PubMed]
- Baker, B.L.; Blacher, J.; Crnic, K.A.; Edelbrock, C. Behavior problems and parenting stress in families of three-year-old children with and without developmental delays. Am. J. Ment. Retard. 2002, 107, 433–444. [Google Scholar] [CrossRef]
- Reilly, C.; Senior, J.; Murtagh, L. ASD, ADHD, mental health conditions and psychopharmacology in neurogenetic syndromes: Parent survey. J. Intellect Disabil. Res. 2015, 59, 307–318. [Google Scholar] [CrossRef] [PubMed]
- Rush, K.S.; Bowman, L.G.; Eidman, S.L.; Toole, L.M.; Mortenson, B.P. Assessing psychopathology in individuals with developmental disabilities. Behav. Modif. 2004, 28, 621–637. [Google Scholar] [CrossRef]
- Johnstone, E.C.; Owens, D.; Hoare, P.; Gaur, S.; Spencer, M.D.; Stanfield, A.; Moffat, V.; Harris, J.M.; Brearley, N.; Miller, P.M.; et al. Schizotypal cognitions as a predictor of psychopathology in adolescents with mild intellectual impairment. Br. J. Psychiatry 2007, 191, 484–492. [Google Scholar] [CrossRef] [PubMed]
- Achenbach, T.M. Manual for the child behavior checklist/4–18 and 1991 profile; University of Vermont, Department of Psychiatry: Burlington, Vermont, 1991. [Google Scholar]
- Paul, A.R.; McKechanie, A.G.; Johnstone, E.C.; Owens, D.G.; Stanfield, A.C. Brief report: The association of autistic traits and behavioural patterns in adolescents receiving special educational assistance. J. Autism Dev. Disord. 2015, 45, 3055–3060. [Google Scholar] [CrossRef] [PubMed]
- Johnstone, E.C.; Ebmeier, K.P.; Miller, P.; Owens, D.G.; Lawrie, S.M. Predicting schizophrenia: Findings from the Edinburgh high-risk study. Br. J. Psychiatry 2005, 186, 18–25. [Google Scholar] [CrossRef] [PubMed]
- Schachter, D.C.; Pless, I.B.; Bruck, M. The prevalence and correlates of behaviour problems in learning disabled children. Can. J. Psychiatry 1991, 36, 323–331. [Google Scholar] [PubMed]
- Crijnen, A.A.; Achenbach, T.M.; Verhulst, F.C. Problems reported by parents of children in multiple cultures: The child behavior checklist syndrome constructs. Am. J. Psychiatry 1999, 156, 569–574. [Google Scholar] [PubMed]
- Lord, C.; Rutter, M.; Le Couteur, A. Autism diagnostic interview-revised: A revised version of a diagnostic interview for caregivers of individuals with possible pervasive developmental disorders. J. Autism Dev. Disord. 1994, 24, 659–685. [Google Scholar] [CrossRef] [PubMed]
- WHOQOL Group. Development of the World Health Organization WHOQOL-BREF quality of life assessment. Psychol. Med. 1998, 28, 551–558. [Google Scholar]
- WHOQOL Group. The World Health Organization Quality of Life assessment (WHOQOL): Position paper from the World Health Organization. Soc. Sci. Med. 1995, 41, 1403–1409. [Google Scholar]
- Skevington, S.M.; Lofty, M.; O’Connell, K.A. The World Health Organization’s WHOQOL-BREF quality of life assessment: Psychometric properties and results of the international field trial. A report from the WHOQOL group. Qual. Life Res. 2004, 13, 299–310. [Google Scholar] [CrossRef] [PubMed]
- Poston, D.; Turnbull, A.; Park, J.; Mannan, H.; Marquis, J.; Wang, M. Family quality of life: A qualitative inquiry. Ment. Retard 2003, 41, 313–328. [Google Scholar] [CrossRef]
- Park, J.; Hoffman, L.; Marquis, J.; Turnbull, A.P.; Poston, D.; Mannan, H.; Wang, M.; Nelson, L.L. Toward assessing family outcomes of service delivery: Validation of a family quality of life survey. J. Intellect Disabil. Res. 2003, 47, 367–384. [Google Scholar] [CrossRef] [PubMed]
- Nachshen, J.S.; Woodford, L.; Minnes, P. The family stress and coping interview for families of individuals with developemntal disabilities: A lifespan perspective on family adjustment. J. Intellect Disabil. Res. 2003, 47, 285–290. [Google Scholar] [CrossRef] [PubMed]

| 1 | 2 | 3 | 4 | ||
|---|---|---|---|---|---|
| Additional Needs | Typically Developing | ||||
| −ve SCQ −ve ASD | +ve SCQ +ve ASD | +ve SCQ −ve ASD | |||
| n = 41 | n = 18 | n = 17 | n = 17 | ||
| Age * | mean | 15.60 | 16.35 | 16.06 | 15.85 |
| SD | 1.9 | 2.34 | 1.40 | 1.7 | |
| Gender | no. (%) male | 23 (56%) | 17 (95%) | 12 (71%) | 8 (47%) |
| IQ | Mean | 72.78 | 84.06 | 66.50 | 111.82 |
| SD | 16.86 | 22.08 | 9.35 | 16.88 | |
| School | Mainstream | 20 (49%) | 7 (39%) | 3 (18%) | 15 (88%) |
| Special | 17 (41%) | 9 (50%) | 11 (65%) | 0 | |
| FE College | 4 (10%) | 2 (11%) | 3 (18%) | 2 (12%) | |
| SCQ | mean | 7.53 | 22.89 | 20.06 | 0.59 |
| SD | 3.87 | 5.83 | 3.38 | 0.79 | |
| CBCL | Mean | 67.00 | 81.44 | 89.65 | 11.24 |
| SD | 33.43 | 29.29 | 49.27 | 10.85 | |
| SCQ | CBCL | WHOQOL | FQoLS | FSCI | IQ | |
|---|---|---|---|---|---|---|
| CBCL | r(76) = 0.385 * | |||||
| WHOQoL | r(75) = −0.349 * | r(75) = −0.406 * | ||||
| FQoLS | r(73) = −0.378 * | r(73) = −0.250 * | r(72) = 0.587 * | |||
| FSCI | r(74) = 0.474 * | r(74) = 0.363 * | r(74) = −0.564 * | r(71) = −0.464 * | ||
| IQ | r(65) = −0.147 | r(65) = −0.125 | r(65) = 0.028 | r(63) = −0.071 | r(64) = −0.057 | |
| Age | r(76) = 0.155 | r(76) = −0.034 | r(75) = −0.065 | r(73) = −0.204 | r(74) = 0.157 | r(65) = −0.400 |
| Control Variable | SCQ | |
|---|---|---|
| CBCL | FQoLS | −0.319 * |
| FSCI | 0.369 * |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
McKechanie, A.G.; Moffat, V.J.; Johnstone, E.C.; Fletcher-Watson, S. Links between Autism Spectrum Disorder Diagnostic Status and Family Quality of Life. Children 2017, 4, 23. https://doi.org/10.3390/children4040023
McKechanie AG, Moffat VJ, Johnstone EC, Fletcher-Watson S. Links between Autism Spectrum Disorder Diagnostic Status and Family Quality of Life. Children. 2017; 4(4):23. https://doi.org/10.3390/children4040023
Chicago/Turabian StyleMcKechanie, Andrew G., Vivien J. Moffat, Eve C. Johnstone, and Sue Fletcher-Watson. 2017. "Links between Autism Spectrum Disorder Diagnostic Status and Family Quality of Life" Children 4, no. 4: 23. https://doi.org/10.3390/children4040023




