Specialized Rehabilitation Programs for Children and Adolescents with Severe Disabling Chronic Pain: Indications, Treatment and Outcomes
Abstract
:1. Introduction
2. Method
3. Results
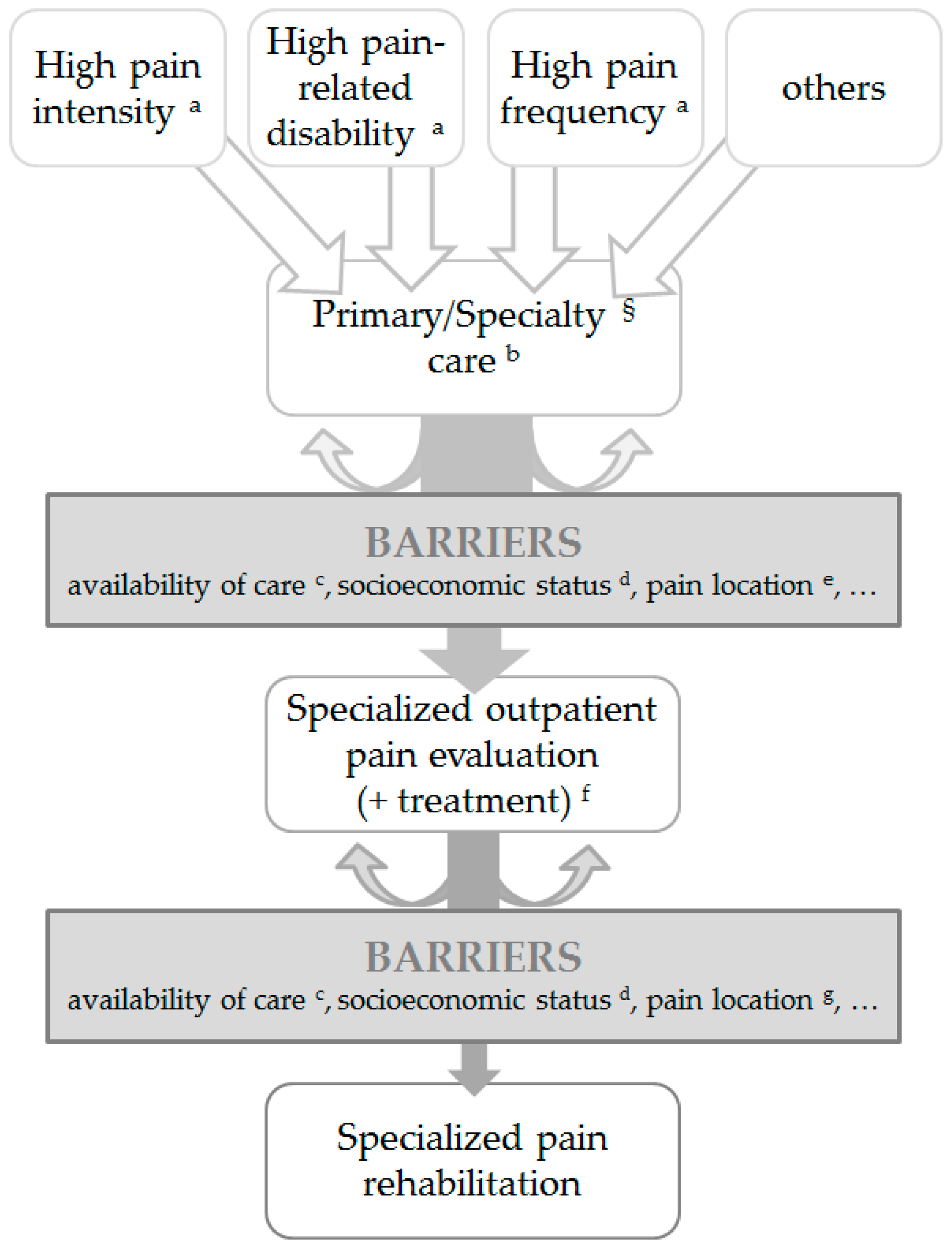
3.1. Indications for Specialized Rehabilitation Programs
3.2. Treatment Components of Specialized Rehabilitation Programs
3.3. Outcomes of Specialized Rehabilitation Programs
- Pain intensity. The systematic review showed large short-term reductions in pain intensity [36]. More recent studies confirm these short-term reductions in pain intensity [28,34,43]. Several studies also provide evidence for long-term reductions (12 to 24–42 months after treatment) of pain intensity [16,28,34,47,52,53].
- Satisfaction with treatment, symptoms and adverse events. None of the studies investigated satisfaction with treatment or treatment-emergent symptoms and adverse events as outcome measures.
- Physical functioning. There was a large effect for the reduction of pain-related disability described in the systematic review [36]. Significant short-term effects were also found in more recent studies [28,43]. Studies also reported positive long-term effects (12 months after treatment) of rehabilitation programs on pain-related disability [28,47,52,53].
- Emotional functioning. The systematic review revealed a moderate effect for reduction in general anxiety, a large effect for reduction in pain-specific fear and a small to moderate effect for the reduction in depressive symptoms [36]. Benore et al. [43] replicated the short-term effects of specialized rehabilitation programs on general anxiety and on pain-specific anxiety. Sherry et al. [28] found positive short-term effects on emotional functioning that remained stable up to one year after treatment. Two more studies reported significant long-term reductions (12 months after treatment) in anxiety and depression [52,53].
- Role functioning. According to the systematic review, school attendance as the recommended measure of role functioning [46] was significantly improved by intensive treatment with moderate to large effect sizes [36]. Recent studies replicated these short-term effects [28,34,43]. Several studies further supported the long-term effectiveness (12 to 24–42 months after treatment) of intensive pain treatment on reducing school absence [28,34,47,52,53].
- Sleep. Only three studies used sleep as an outcome measure. All reported improvements in sleep disturbances [44,49,50]. One study further found stable short-term improvements in sleep onset delay, sleep duration, night waking and daytime sleepiness and an overall reduction in the use of sleep medication [44]. However, these results were based on self-report and not on validated objective measures such as actigraphy or sleep recording [46].
- Economic factors. A small number of studies investigated the economic effects of intensive pain treatment in terms of health care utilization and indirect costs. Significant reductions were found for health care utilization, in both the short and long term (12 to 24–42 month after treatment) [16,34,48,52]. Indirect costs, such as lost work days [16,34,52] and parental subjective financial burden [52], also showed significant reductions. Evans et al. [16] concluded that chronic pain rehabilitation is a cost-effective treatment for pediatric chronic pain.
- Regarding moderators of treatment outcome, the results indicated that sex [38,47], fear of pain [51], pretreatment functional impairment [53], psychological comorbidities [43,53], sleep habits [44] and patients’ readiness to self-manage pain [37] were associated with treatment outcomes. Poorer treatment outcomes were associated with female sex [38,47], high levels of fear of pain [51], low levels of school absence before treatment [53] and high levels of anxiety and depression [53]. Furthermore, decreases in anxiety [43], increases in readiness to self-manage pain [37] and improvements in sleep habits, such as sleep duration, night-waking or sleep onset, showed associations with better treatment outcomes [44].
4. Discussion
4.1. Indications for Specialized Rehabilitation Programs
4.2. Treatment Components of Specialized Rehabilitation Programs
4.3. Outcomes of Specialized Rehabilitation Programs
4.4. Recommendations for Future Research and Patient Care
4.5. Limitations
Author Contributions
Conflicts of Interest
References
- Huguet, A.; Miro, J. The severity of chronic paediatric pain: An epidemiological study. J. Pain 2008, 9, 226–236. [Google Scholar] [CrossRef] [PubMed]
- Zernikow, B.; Wager, J.; Hechler, T.; Hasan, C.; Rohr, U.; Dobe, M.; Meyer, A.; Hübner-Möhler, B.; Wamsler, C.; Blankenburg, M. Characteristics of highly impaired children with severe chronic pain: A 5-year retrospective study on 2249 pediatric pain patients. BMC Pediatr. 2012, 12, 54. [Google Scholar] [CrossRef] [PubMed]
- Logan, D.E.; Simsons, L.E.; Stein, M.J.; Chastain, L. School impairment in adolescents with chronic pain. J. Pain 2008, 9, 407–416. [Google Scholar] [CrossRef] [PubMed]
- Wager, J.; Hechler, T.; Darlington, A.S.; Hirschfeld, G.; Vocks, S.; Zernikow, B. Classifying the severity of paediatric chronic pain—An application of the chronic pain grading. Eur. J. Pain 2013, 17, 1393–1402. [Google Scholar] [CrossRef] [PubMed]
- Voerman, J.S.; de Klerk, C.; Vander Heyden, K.M.; Passchier, J.; Idema, W.; Timman, R.; Jolles, J. Pain is associated with poorer grades, reduced emotional well-being, and attention problems in adolescents. Clin J. Pain 2016. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brna, P.; Dooley, J.; Gordon, K.; Dewan, T. The prognosis of childhood headache: A 20-year follow-up. Arch. Pediatr. Adolesc. Med. 2005, 159, 1157–1160. [Google Scholar] [CrossRef] [PubMed]
- Hestbaek, L.; Leboeuf-Yde, C.; Kyvik, K.O.; Manniche, C. The course of low back pain from adolescence to adulthood: Eight-year follow-up of 9600 twins. Spine (Phila Pa 1976) 2006, 31, 468–472. [Google Scholar] [CrossRef] [PubMed]
- Walker, L.S.; Dengler-Crish, C.M.; Rippel, S.; Bruehl, S. Functional abdominal pain in childhood and adolescence increases risk for chronic pain in adulthood. Pain 2010, 150, 568–572. [Google Scholar] [CrossRef] [PubMed]
- Ellert, U.; Neuhauser, H.; Roth-Isigkeit, A. [pain in children and adolescents in Germany: The prevalence and usage of medical services. Results of the german health interview and examination survey for children and adolescents (KiGGs)]. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 2007, 50, 711–717. [Google Scholar] [CrossRef] [PubMed]
- Perquin, C.W.; Hunfeld, J.A.; Hazebroek-Kampschreur, A.A.; van Suijlekom-Smit, L.W.; Passchier, J.; Koes, B.W.; van der Wouden, J.C. Insights in the use of health care services in chronic benign pain in childhood and adolescence. Pain 2001, 94, 205–213. [Google Scholar] [CrossRef]
- Toliver-Sokol, M.; Murray, C.B.; Wilson, A.C.; Lewandowski, A.; Palermo, T.M. Patterns and predictors of health service utilization in adolescents with pain: Comparison between a community and a clinical pain sample. J. Pain 2011, 12, 747–755. [Google Scholar] [CrossRef] [PubMed]
- Hirschfeld, G.; Wager, J.; Zernikow, B. Physician consultation in young children with recurrent pain—A population-based study. PeerJ 2015, 3, e916. [Google Scholar] [CrossRef] [PubMed]
- Grumbach, K.; Bodenheimer, T. The organization of health care. JAMA 1995, 273, 160–167. [Google Scholar] [CrossRef] [PubMed]
- Mossialos, E.; Wenzl, M.; Osborn, R.; Anderson, C. International Profiles of Health Care Systems, 2015; The Commonwealth Fund: New York, NY, USA, 2016. [Google Scholar]
- Groenewald, C.B.; Essner, B.S.; Wright, D.; Fesinmeyer, M.D.; Palermo, T.M. The economic costs of chronic pain among a cohort of treatment-seeking adolescents in the united states. J. Pain 2014, 15, 925–933. [Google Scholar] [CrossRef] [PubMed]
- Evans, J.R.; Benore, E.; Banez, G.A. The cost-effectiveness of intensive interdisciplinary pediatric chronic pain rehabilitation. J. Pediatr. Psychol. 2016, 41, 849–856. [Google Scholar] [CrossRef] [PubMed]
- Kaufman, E.L.; Tress, J.; Sherry, D.D. Trends in medicalization of children with amplified musculoskeletal pain syndrome. Pain Med. 2016. [Google Scholar] [CrossRef] [PubMed]
- Ho, I.K.; Goldschneider, K.R.; Kashikar-Zuck, S.; Kotagal, U.; Tessman, C.; Jones, B. Healthcare utilization and indirect burden among families of pediatric patients with chronic pain. J. Musculoskelet. Pain 2008, 16, 155–164. [Google Scholar] [CrossRef]
- Ruhe, A.; Wager, J.; Hirschfeld, G.; Zernikow, B. Household income determines access to specialized pediatric chronic pain treatment in Germany. BMC Health Serv. Res. 2016, 16, 140. [Google Scholar] [CrossRef] [PubMed]
- Wager, J.; Ruhe, A.; Hirschfeld, G.; Wamsler, C.; Dobe, M.; Hechler, T.; Zernikow, B. Influence of parental occupation on access to specialised treatment for paediatric chronic pain: A retrospective study. Schmerz 2013, 27, 305–311. [Google Scholar] [CrossRef] [PubMed]
- Peng, P.; Choiniere, M.; Dion, D.; Intrater, H.; LeFort, S.; Lynch, M.; Ong, M.; Rashiq, S.; Tkachuk, G.; Veillette, Y.; et al. Challenges in accessing multidisciplinary pain treatment facilities in Canada. Can. J. Anaesth. 2007, 54, 985–991. [Google Scholar] [CrossRef] [PubMed]
- Stinson, J.; White, M.; Isaac, L.; Campbell, F.; Brown, S.; Ruskin, D.; Gordon, A.; Galonski, M.; Pink, L.; Buckley, N. Understanding the information and service needs of young adults with chronic pain: Perspectives of young adults and their providers. Clin. J. Pain 2013, 29, 600–612. [Google Scholar] [CrossRef] [PubMed]
- Stinson, J.N.; Lalloo, C.; Harris, L.; Isaac, L.; Campbell, F.; Brown, S.; Ruskin, D.; Gordon, A.; Galonski, M.; Pink, L.R. iCcanCope with Pain™: User-centred design of a web-and mobile-based self-management program for youth with chronic pain based on identified health care needs. Pain Res. Manag. 2014, 19, 257–265. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Wager, J.; Zernikow, B. Chronic pain treatment in children and adolescents: Less is good, more is sometimes better. BMC Pediatr. 2014, 14, 262. [Google Scholar] [CrossRef] [PubMed]
- Simons, L.E.; Sieberg, C.B.; Pielech, M.; Conroy, C.; Logan, D.E. What does it take? Comparing intensive rehabilitation to outpatient treatment for children with significant pain-related disability. J. Pediatr. Psychol. 2013, 38, 213–223. [Google Scholar] [CrossRef] [PubMed]
- Claar, R.L.; Kaczynski, K.J.; Minster, A.; Donald-Nolan, L.; LeBel, A.A. School functioning and chronic tension headaches in adolescents: Improvement only after multidisciplinary evaluation. J. Child. Neurol. 2013, 28, 719–724. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Martin, A.; Blankenburg, M.; Schroeder, S.; Kosfelder, J.; Hölscher, L.; Denecke, H.; Zernikow, B. Specialized multimodal outpatient treatment for children with chronic pain: Treatment pathways and long-term outcome. Eur. J. Pain 2011, 15, 976–984. [Google Scholar] [CrossRef] [PubMed]
- Sherry, D.D.; Brake, L.; Tress, J.L.; Sherker, J.; Fash, K.; Ferry, K.; Weiss, P.F. The treatment of juvenile fibromyalgia with an intensive physical and psychosocial program. J. Pediatr. 2015, 167, 731–737. [Google Scholar] [CrossRef] [PubMed]
- International Association for the Study of Pain. Pain Treatment Services. 2009. Available online: http://www.iasp-pain.org/Education/Content.aspx?ItemNumber=1381 (accessed on 1 August 2016).
- Lynch-Jordan, A.M.; Kashikar-Zuck, S.; Crosby, L.E.; Lopez, W.L.; Smolyansky, B.H.; Parkins, I.S.; Luzader, C.P.; Hartman, A.; Guilfoyle, S.M.; Powers, S.W. Applying quality improvement methods to implement a measurement system for chronic pain-related disability. J. Pediatr. Psychol. 2009, 35, 32–41. [Google Scholar] [CrossRef] [PubMed]
- American Pain Society—Pediatric Chronic Pain Task Force. Assessment and Management of Children with Chronic Pain—A Position Statement from the American Pain Society, 2012.
- Logan, D.E.; Carpino, E.A.; Chiang, G.; Condon, M.; Firn, E.; Gaughan, V.J.; Hogan, M.; Leslie, D.S.; Olson, K.; Sager, S. A day-hospital approach to treatment of pediatric complex regional pain syndrome: Initial functional outcomes. Clin. J. Pain 2012, 28, 766–774. [Google Scholar] [CrossRef] [PubMed]
- Weiss, K.E.; Hahn, A.; Wallace, D.P.; Biggs, B.; Bruce, B.K.; Harrison, T.E. Acceptance of pain: Associations with depression, catastrophizing, and functional disability among children and adolescents in an interdisciplinary chronic pain rehabilitation program. J. Pediatr. Psychol. 2013, 38, 756–765. [Google Scholar] [CrossRef] [PubMed]
- Banez, G.A.; Frazier, T.W.; Wojtowicz, A.A.; Buchannan, K.; Henry, D.E.; Benore, E. Chronic pain in children and adolescents: 24–42 month outcomes of an inpatient/day hospital interdisciplinary pain rehabilitation program. J. Pediatr. Rehabil. Med. Inderdiscip. Approach 2014, 7, 197–206. [Google Scholar]
- Eccleston, C.; Malleson, P.; Clinch, J.; Connell, H.; Sourbut, C. Chronic pain in adolescents: Evaluation of a programme of interdisciplinary cognitive behaviour therapy. Arch. Dis. Child. 2003, 88, 881–885. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Kanstrup, M.; Holley, A.L.; Simons, L.E.; Wicksell, R.; Hirschfeld, G.; Zernikow, B. Systematic review on intensive interdisciplinary pain treatment of children with chronic pain. Pediatrics 2015, 136, 115–127. [Google Scholar] [CrossRef] [PubMed]
- Logan, D.E.; Conroy, C.; Sieberg, C.B.; Simons, L.E. Changes in willingness to self-manage pain among children and adolescents and their parents enrolled in an intensive interdisciplinary pediatric pain treatment program. Pain 2012, 153, 1863–1870. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Kosfelder, J.; Vocks, S.; Mönninger, T.; Blankenburg, M.; Dobe, M.; Gerlach, A.L.; Denecke, H.; Zernikow, B. Changes in pain-related coping strategies and their importance for treatment outcome following multimodal inpatient treatment: Does sex matter? J. Pain 2010, 11, 472–483. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Dobe, M.; Damschen, U.; Blankenburg, M.; Schroeder, S.; Kosfelder, J.; Zernikow, B. The pain provocation technique for adolescents with chronic pain: Preliminary evidence for its effectiveness. Pain Med. 2010, 11, 897–910. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Dobe, M.; Kosfelder, J.; Damschen, U.; Hübner, B.; Blankenburg, M.; Sauer, C.; Zernikow, B. Effectiveness of a three-week multimodal inpatient pain treatment for adolescents suffering from chronic pain: Statistical and clinical significance. Clin. J. Pain 2009, 25, 156–166. [Google Scholar] [CrossRef] [PubMed]
- Dobe, M.; Damschen, U.; Reiffer-Wiesel, B.; Sauer, C.; Zernikow, B. [Multimodal inpatient pain treatment in children—Results of a three-week program]. Schmerz 2006, 20, 51–60. [Google Scholar] [CrossRef] [PubMed]
- Dobe, M.; Hechler, T.; Behlert, J.; Kosfelder, J. [Pain therapy with children and adolescents severely disabled due to chronic pain—Long-term outcome after inpatient pain therapy]. Schmerz 2011, 25, 411–422. [Google Scholar] [CrossRef] [PubMed]
- Benore, E.; D’Auria, A.; Banez, G.A.; Worley, S.; Tang, A. The influence of anxiety reduction on clinical response to pediatric chronic pain rehabilitation. Clin. J. Pain 2015, 31, 375–383. [Google Scholar] [CrossRef] [PubMed]
- Logan, D.E.; Sieberg, C.B.; Conroy, C.; Smith, K.; Odell, S.; Sethna, N. Changes in sleep habits in adolescents during intensive interdisciplinary pediatric pain rehabilitation. J. Youth Adolesc. 2015, 44, 543–555. [Google Scholar] [CrossRef] [PubMed]
- Dobe, M.; Zernikow, B. Practical Treatment Options for Chronic Pain in Children and Adolescents: An Interdisciplinary Therapy Manual; Springer: Berlin/Heidelberg, Germany, 2013; Volume 1, pp. 1–268. [Google Scholar]
- McGrath, P.J.; Walco, G.A.; Turk, D.C.; Dworkin, R.H.; Brown, M.T.; Davidson, K.; Eccleston, C.; Finley, A.G.; Goldschneider, K.; Haverkos, L.; et al. Core outcome domains and measures for pediatric acute and chronic/recurrent pain clinical trials: Pedimmpact recommendations. J. Pain 2008, 9, 771–783. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Blankenburg, M.; Dobe, M.; Kosfelder, J.; Hübner, B.; Zernikow, B. Effectiveness of a multimodal inpatient treatment for pediatric chronic pain: A comparison between children and adolescents. Eur. J. Pain 2010, 14, 97.e1–97.e9. [Google Scholar] [CrossRef] [PubMed]
- Gauntlett-Gilbert, J.; Connell, H.; Clinch, J.; McCracken, L.M. Acceptance and values-based treatment of adolescents with chronic pain: Outcomes and their relationship to acceptance. J. Pediatr. Psychol. 2013, 38, 72–81. [Google Scholar] [CrossRef] [PubMed]
- Maynard, C.S.; Amari, A.; Wieczorek, B.; Christensen, J.R.; Slifer, K.J. Interdisciplinary behavioral rehabilitation of pediatric pain-associated disability: Retrospective review of an inpatient treatment protocol. J. Pediatr. Psychol. 2010, 35, 128–137. [Google Scholar] [CrossRef] [PubMed]
- Chalkiadis, G.A. Management of chronic pain in children. Med. J. Aust. 2001, 175, 476–479. [Google Scholar] [PubMed]
- Simons, L.E.; Kaczynski, K.J.; Conroy, C.; Logan, D.E. Fear of pain in the context of intensive pain rehabilitation among children and adolescents with neuropathic pain: Associations with treatment response. J. Pain 2012, 13, 1151–1161. [Google Scholar] [CrossRef] [PubMed]
- Hechler, T.; Ruhe, A.; Schmidt, P.; Hirsch, J.; Wager, J.; Dobe, M.; Krummenauer, F.; Zernikow, B. Inpatient-based intensive interdisciplinary pain treatment for highly impaired children with severe chronic pain: Randomized controlled trial of efficacy and economic effects. Pain 2014, 155, 118–128. [Google Scholar] [CrossRef] [PubMed]
- Hirschfeld, G.; Hechler, T.; Dobe, M.; Wager, J.; Blankenburg, M.; Kosfelder, J.; Zernikow, B. Maintaining lasting improvements: One-year follow-up of children with severe chronic pain undergoing multimodal inpatient treatment. J. Pediatr. Psychol. 2013, 38, 224–236. [Google Scholar] [CrossRef] [PubMed]
- Eccleston, C.; Palermo, T.M.; De C Williams, A.C.; Lewandowski, A.; Morley, S.; Fisher, E.; Law, E. Psychological therapies for the management of chronic and recurrent pain in children and adolescents. Cochrane Database of Syst. Rev. 2012, 12, CD003968. [Google Scholar]
- Fisher, E.; Heathcote, L.; Palermo, T.M.; de, C.W.; Lau, J.; Eccleston, C. Systematic review and meta-analysis: Psychological therapies for children with chronic pain. J. Pediatr. Psychol. 2014, 39, 753–762. [Google Scholar] [CrossRef] [PubMed]
- Westendorp, T.; Verbunt, J.; Remerie, S.; Blécourt, A.; Baalen, B.; Smeets, R. Social functioning in adulthood: Understanding long-term outcomes of adolescents with chronic pain/fatigue treated at inpatient rehabilitation programs. Eur. J. Pain 2016, 20, 1121–1130. [Google Scholar] [CrossRef] [PubMed]
- Palermo, T.M.; Wilson, A.C.; Peters, M.; Lewandowski, A.; Somhegyi, H. Randomized controlled trial of an internet-delivered family cognitive-behavioral therapy intervention for children and adolescents with chronic pain. Pain 2009, 146, 205–213. [Google Scholar] [CrossRef] [PubMed]
- Palermo, T.M.; Law, E.F.; Fales, J.; Bromberg, M.H.; Jessen-Fiddick, T.; Tai, G. Internet-delivered cognitive-behavioral treatment for adolescents with chronic pain and their parents: A randomized controlled multicenter trial. Pain 2016, 157, 174–185. [Google Scholar] [CrossRef] [PubMed]
| Criteria | Specialized Rehabilitation Programs | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Inclusion | AUS | UK | UK | GER | USA | USA | USA | USA | USA |
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | |
| Pain for more than 3 months | x | x | x | ||||||
| High pain-related disability | x | x | x | x | x | x | |||
| Patient and parent motivation | x | x | x | x | |||||
| Failure of outpatient treatment | x | x | x | ||||||
| Exclusion | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| Psychiatric needs | x | x | x | ||||||
| Further assessment required | x | x | |||||||
| Medical pathology/underlying disease | x | x | |||||||
| Active malignant disease | x | x | |||||||
| Effective medical options | x | ||||||||
| Components | Specialized Rehabilitation Programs | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| AUS | UK | UK | GER | USA | USA | USA | USA | USA | |
| Structure | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| Inpatient | x | x | x | x | x | ||||
| Day-hospital | x | x | x | x | x | x | |||
| Interdisciplinary team | x | x | x | x | x | x | x | x | x |
| Psychotherapy Approach | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| Operant and cognitive behavioral therapy | x | x | x | x | x | x | x | x | x |
| Acceptance and commitment therapy | x | x | x | ||||||
| Medical Interventions | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| Medication | x | x | x | x | x | ||||
| Medical examination | x | x | x | x | |||||
| Physical therapy | x | x | x | x | x | x | x | x | x |
| Biofeedback | x | x | x | x | |||||
| Psychological Interventions | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| Education | x | x | x | x | |||||
| Relaxation techniques | x | x | x | x | x | x | |||
| Attention defocusing | x | x | x | ||||||
| Imagery | x | x | x | x | |||||
| Active daily structure | x | x | x | x | x | x | x | x | x |
| Stress management | x | x | x | x | |||||
| Problem-solving | x | x | x | ||||||
| Addressing psychological comorbidities | x | x | |||||||
| Social Interventions | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| Family sessions | x | x | x | x | x | x | x | x | |
| Parent-only sessions | x | x | x | x | x | ||||
| School reintegration | x | x | x | x | x | ||||
| Patient group sessions | x | x | x | x | x | ||||
| Other | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
| Occupational therapy | x | x | x | x | x | x | x | ||
| Recreational therapy | x | x | x | ||||||
| Hospital school program | x | x | x | ||||||
| Acupressure/acupuncture | x | x | x | ||||||
| Diet | x | x | |||||||
| Sleep hygiene | x | x | x | ||||||
| Music therapy | x | x | x | ||||||
| Art therapy | x | x | x | ||||||
| Therapeutic homework and practicing | x | x | x | ||||||
| Relapse prevention | x | x | x | x | |||||
| Follow-up care | x | x | x | ||||||
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stahlschmidt, L.; Zernikow, B.; Wager, J. Specialized Rehabilitation Programs for Children and Adolescents with Severe Disabling Chronic Pain: Indications, Treatment and Outcomes. Children 2016, 3, 33. https://doi.org/10.3390/children3040033
Stahlschmidt L, Zernikow B, Wager J. Specialized Rehabilitation Programs for Children and Adolescents with Severe Disabling Chronic Pain: Indications, Treatment and Outcomes. Children. 2016; 3(4):33. https://doi.org/10.3390/children3040033
Chicago/Turabian StyleStahlschmidt, Lorin, Boris Zernikow, and Julia Wager. 2016. "Specialized Rehabilitation Programs for Children and Adolescents with Severe Disabling Chronic Pain: Indications, Treatment and Outcomes" Children 3, no. 4: 33. https://doi.org/10.3390/children3040033
APA StyleStahlschmidt, L., Zernikow, B., & Wager, J. (2016). Specialized Rehabilitation Programs for Children and Adolescents with Severe Disabling Chronic Pain: Indications, Treatment and Outcomes. Children, 3(4), 33. https://doi.org/10.3390/children3040033







