Climate Change and Children’s Health: A Commentary
Abstract
:1. Science and Its Limitations
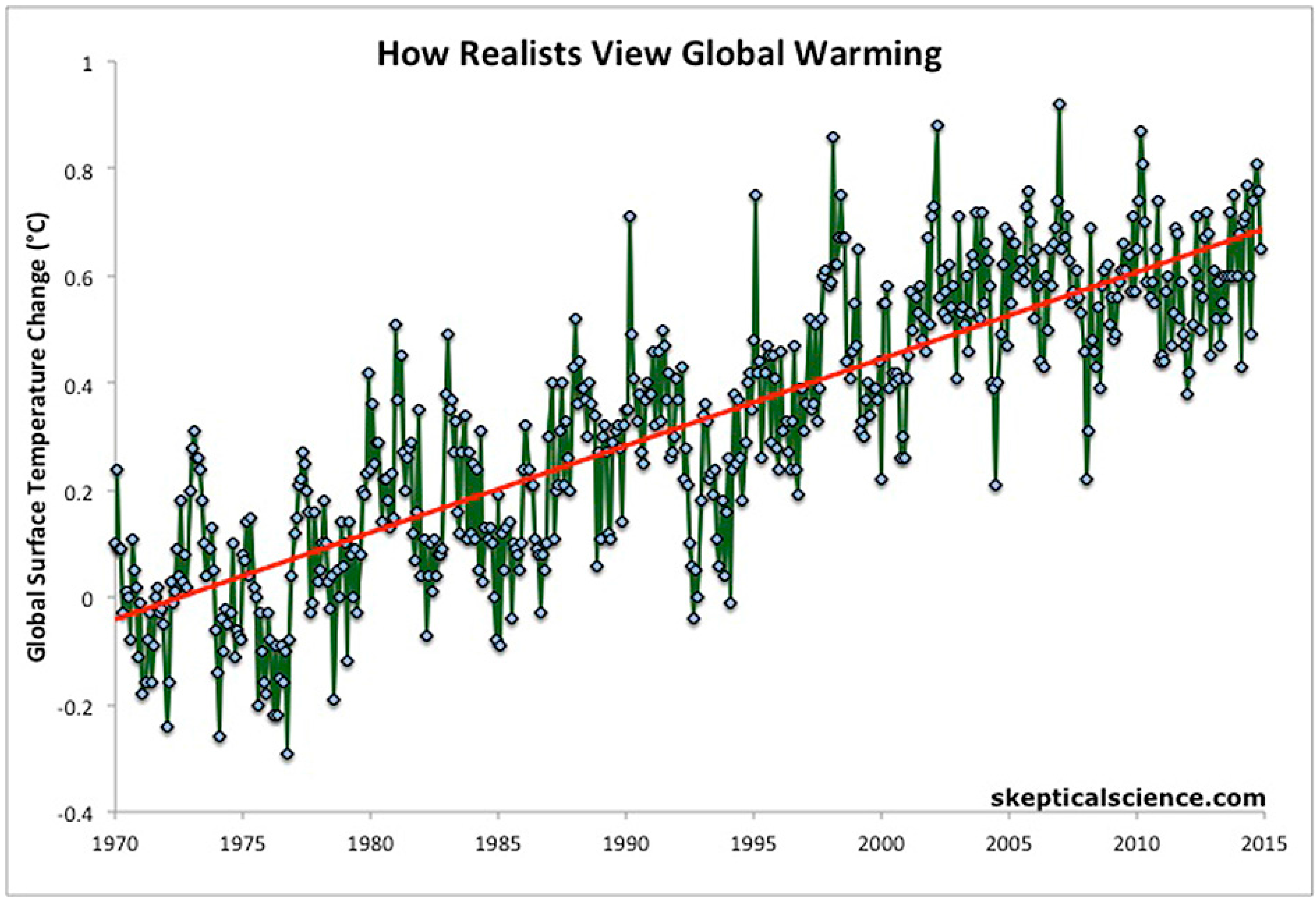
2. Wicked Problems Facing Society
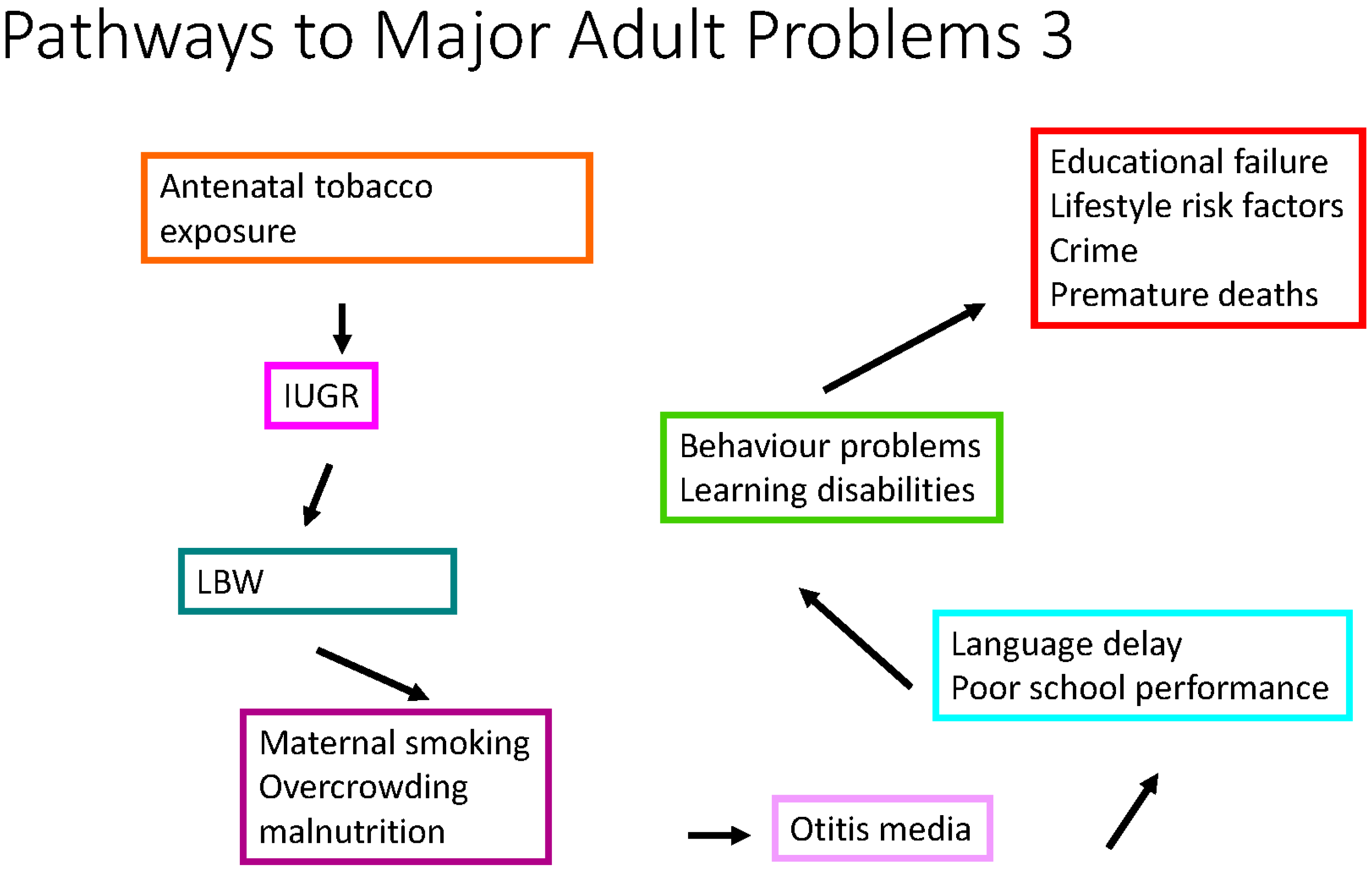
3. Climate Change and Child Health
“Exposure to media ensures that children cannot escape hearing that their future and that of other species is at stake, and that the window of opportunity to avoid dramatic climate impacts is closing. The psychological health of our children is a priority, but denial of the truth exposes our children to even greater risk”.[21]
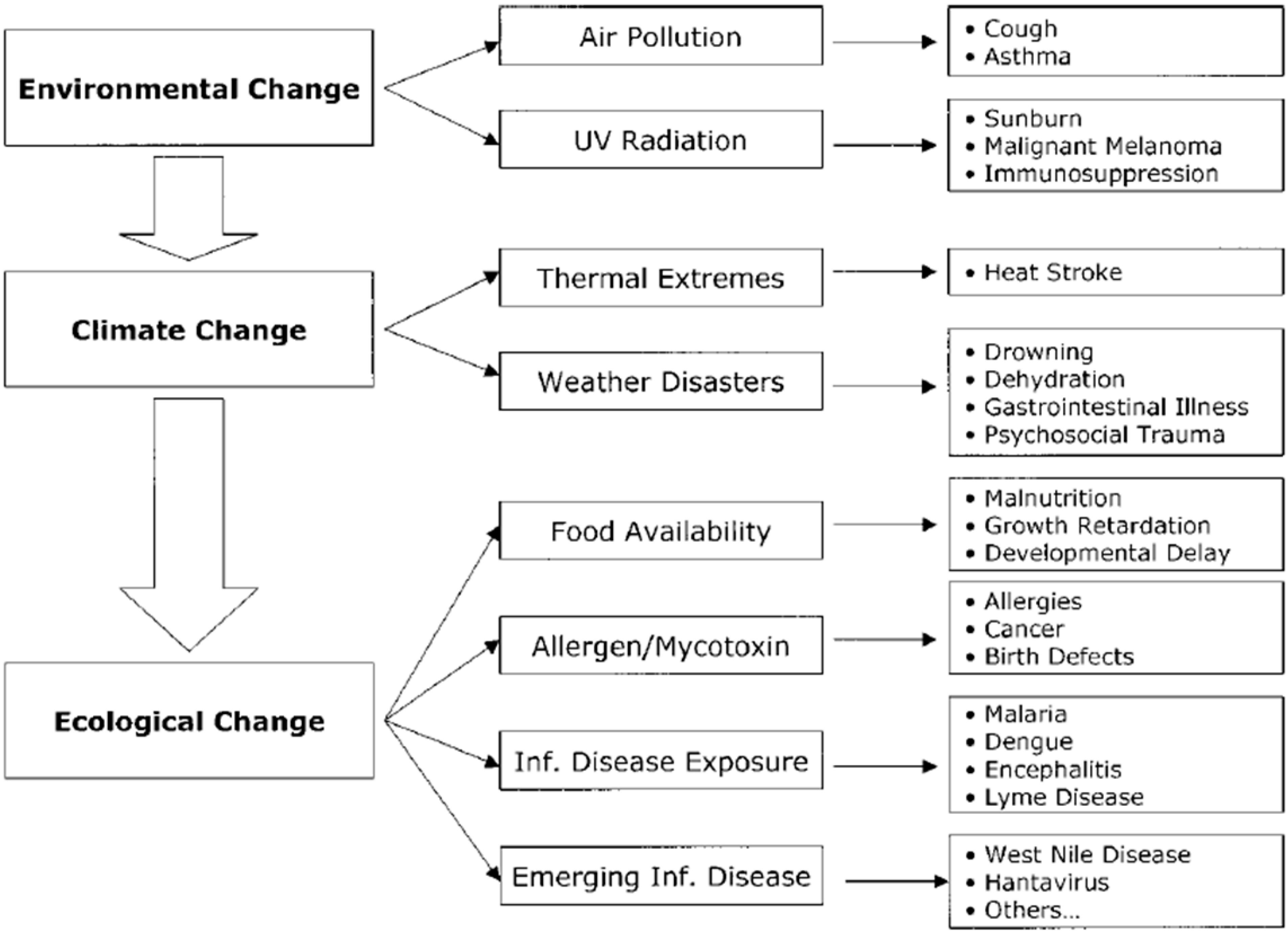
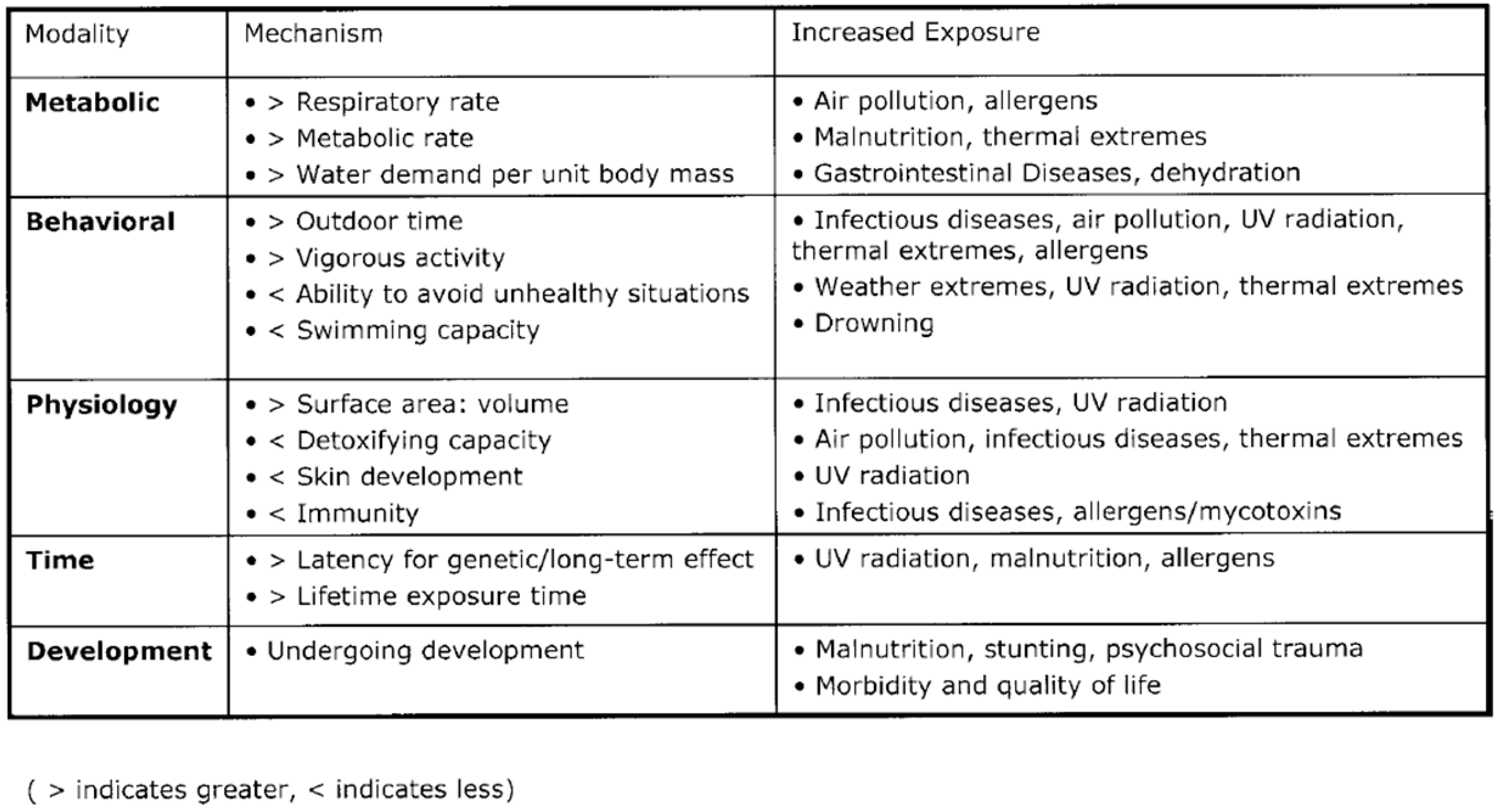
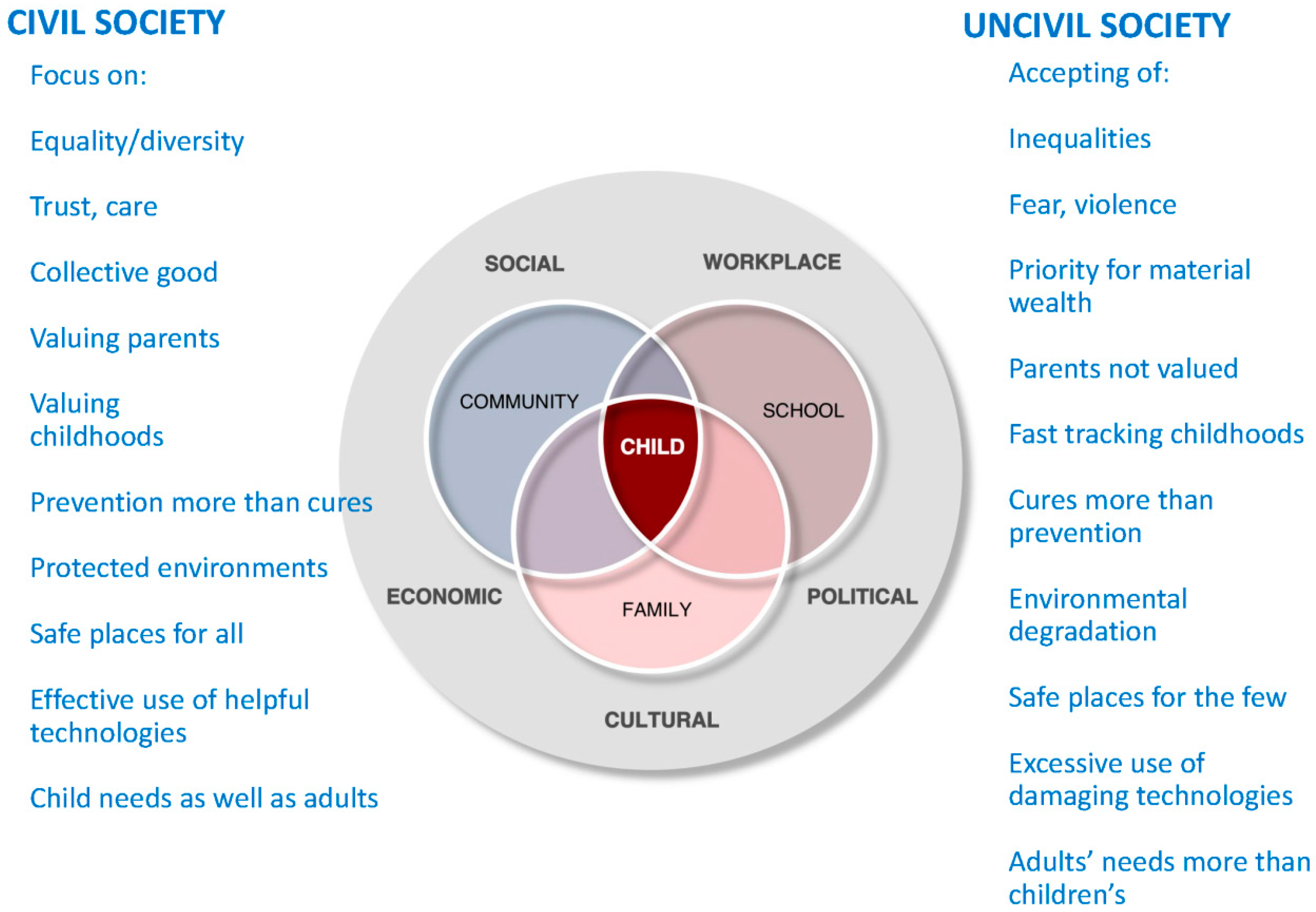
4. Towards a More Civil Society
“We are witnesses to a dramatic expansion of market-based economies whose capacity for wealth generation is awesome in comparison to both the distant and the recent past. At the same time, there is a growing perception of substantial threats to the health and wellbeing of today’s children and youth in the very societies that benefit most from this abundance”.[42]
“Yet the gross national product does not allow for the health of our children, the quality of their education, or the joy of their play. It does not include the beauty of our poetry or the strength of our marriages; the intelligence of our public debate or the integrity of our public officials. It measures neither our wit nor our courage; neither our wisdom nor our learning; neither our compassion nor our devotion to our country; it measures everything, in short, except that which makes life worthwhile. And it tells us everything about America except why we are proud that we are Americans.”.Robert F. Kennedy Address, University of Kansas, Lawrence, Kansas, March 18, 1968 [43]
5. Conclusions
“In the long run, the harm to human health from climate change is more than an avoidable burden of suffering, injury, illness and premature death. It signals that our mismanagement of the world’s climate and environment is weakening the foundations of health and longevity”.[55]
Author Contributions
Conflicts of Interest
References
- National Oceanic and Atmospheric Administration (NOAA). State of the Climate: Global Analysis for Annual 2014. Available online: http://www.ncdc.noaa.gov/sotc/global/201413 (accessed on 17 August 2015).
- National Oceanic and Atmospheric Administration. Global Summary Information—July 2015. Available online: https://www.ncdc.noaa.gov/sotc/summary-info/global/201507 (accessed on 24 August 2015).
- BoM. Annual Climate Statement 2014. Available online: http://www.bom.gov.au/climate/current/annual/aus/ (accessed on 17 August 2015).
- CSIRO and BoM State of the Climate 2014. Available online: http://www.bom.gov.au/state-of-the-climate/ (accessed on 20 August 2015).
- Peters, G.P.; Andrew, R.M.; Boden, T.; Canadell, J.G.; Ciais, P.; Le Quéré, C.; Marland, G.; Raupach, M.R.; Wilson, C. The challenge to keep global warming below 2 °C. Nat. Clim. Chang. 2013, 3, 4–6. [Google Scholar] [CrossRef]
- Raupach, M.R.; Marland, G.; Ciais, P.; Le Quéré, C.; Canadell, J.G.; Klepper, G.; Field, C.B. Global and regional drivers of accelerating CO2 emissions. Proc. Natl. Acad. Sci. USA 2007, 104, 10288–10293. [Google Scholar] [CrossRef] [PubMed]
- Greenhouse Gas Benchmark Reached. Available online: http://research.noaa.gov/News/NewsArchive/LatestNews/TabId/684/ArtMID/1768/ArticleID/11153/Greenhouse-gas-benchmark-reached-.aspx (accessed on 20 August 2015).
- Hansen, J.; Sato, M.; Kharecha, P.; Beerling, D.; Berner, R.; Masson-Delmotte, V.; Pagani, M.; Raymo, M.; Royer, D.L.; Zachos, J.C. Target atmospheric CO2: Where Should Humanity Aim? Open Atmos. Sci. J. 2008, 2, 217–231. [Google Scholar] [CrossRef]
- Braconier, H.; Nicoletti, G.; Westmore, B. Policy Challenges for the Next 50 Years; OECD: Paris, France, 2014. [Google Scholar]
- King, L.J. Combating the triple threat: The need for a one health approach. Microbio. Spectr. 2013. [Google Scholar] [CrossRef]
- de Leeuw, E.; Green, G.; Spanswick, L.; Palmer, N. Policymaking in European healthy cities. Health Promot. Int. 2015, 30, i18–i31. [Google Scholar] [CrossRef] [PubMed]
- Mahoney, G.; Stewart, A.G.; Kennedy, N.; Whitely, B.; Turner, L.; Wilkinson, E. Achieving attainable outcomes from good science in an untidy world: Case studies in land and air pollution. Environ. Geochem. Health 2015, 37, 689–706. [Google Scholar] [CrossRef] [PubMed]
- Czabanowska, K.; Rethmeier, K.A.; Lueddeke, G.; Smith, T.; Malho, A.; Otok, R.; Stankunas, M. Public health in the 21st century: Working differently means leading and learning differently. Eur. J. Public Health 2014, 24, 1047–1052. [Google Scholar] [CrossRef] [PubMed]
- Pawson, R.; Greenhalgh, J.; Brennan, C.; Glidewell, E. Do reviews of healthcare interventions teach us how to improve healthcare systems? Soc. Sci. Med. 2014, 114, 129–137. [Google Scholar] [CrossRef] [PubMed]
- Buse, C. Intersectoral action for health equity as it relates to climate change in Canada: Contributions from critical systems heuristics. J. Eval. Clin. Pract. 2013, 19, 1095–100. [Google Scholar] [CrossRef] [PubMed]
- Camillus, J. Strategy as a Wicked Problem. Harvard Bus. Rev. 2008, 86, 98–106. [Google Scholar]
- Sheffield, P.E.; Landrigan, P.J. Global climate change and children’s health: Threats and strategies for prevention. Environ. Health Perspect. 2011, 119, 291–298. [Google Scholar] [CrossRef] [PubMed]
- DARA. Climate Vulnerability Monitor 2nd Edition: A Guide to the Cold Calculus of a Hot Planet; Fundacion DARA Internacional: Madrid, Spain, 2012. [Google Scholar]
- Kiang, K.; Graham, S.; Farrant, B.M. Climate change, child health and the role of the paediatric profession in under-resourced settings. Trop. Med. Int. Health 2013, 18, 1053–1056. [Google Scholar] [CrossRef] [PubMed]
- Strazdins, L.; Friel, S.; McMichael, A.; Butler, S.W.; Hanna, E. Climate change and child health in Australia: Likely futures, new inequities? Int. Public Health J. 2011, 2, 493–500. [Google Scholar]
- Hansen, J.; Kharecha, P.; Sato, M.; Masson-Delmotte, V.; Ackerman, F.; Beerling, D.J.; Hearty, P.J.; Hoegh-Guldberg, O.; Hsu, S.; Parmesan, C.; et al. Assessing “dangerous climate change”: Required reduction of carbon emissions to protect young people, future generations and nature. PLoS ONE 2013, 8, e81648. [Google Scholar] [CrossRef] [PubMed]
- MacCracken, M.C. Climate Change Impacts Will be Pervasive. Int. Public Health J. 2011, 2, 371–376. [Google Scholar]
- Bennett, C.; Friel, S. Impacts of Climate Change on Inequities in Child Health. Children 2014, 1, 461–473. [Google Scholar] [CrossRef]
- Intergovernmental Panel on Climate Change (IPCC). Climate Change 2014: Impacts, Adaptation, and Vulnerability; Cambridge University Press: New York, NY, USA, 2014. [Google Scholar]
- The International Food Policy Research Institute (IFPRI). Climate Change: Impact on Agriculture and Costs of Adaptation; IFPRI: Washington, DC, USA, 2009. [Google Scholar]
- Myers, N. Environmental refugees: A growing phenomenon of the 21st century. Philos. Trans. R. Soc. Lond. 2002, 357, 609–613. [Google Scholar] [CrossRef] [PubMed]
- Britton, E.; Howden-Chapman, P. The Effect of Climate Change on Children Living on Pacific Islands. Int. Public Health J. 2011, 2, 459–468. [Google Scholar]
- Bunyavanich, S.; Landrigan, C.P.; McMichael, A.J.; Epstein, P.R. The Impact of Climate Change on Child Health. Ambul. Pediatr. 2003, 3, 44–52. [Google Scholar] [CrossRef]
- D’Amato, G.; Baena-Cagnani, C.E.; Cecchi, L.; Annesi-Maesano, I.; Nunes, C.; Ansotegui, I.; D’Amato, M.; Liccardi, G.; Sofia, M.; Canonica, W.G. Climate change, air pollution and extreme events leading to increasing prevalence of allergic respiratory diseases. Multidiscip. Respir. Med. 2013. [Google Scholar] [CrossRef] [PubMed]
- Lau, C.; Weinstein, P. Flooding and infectious disease in rural children: Can intervention mitigate predicted increases in disease burden? Int. Public Health J. 2011, 2, 393–404. [Google Scholar]
- Halsnæs, K.; Foyn, T.H.Y. Climate change and diarrhoeal disease: perspectives for development policies. Int. Public Health J. 2011, 2, 385–391. [Google Scholar]
- Xu, Z.; Hu, W.; Su, H.; Turner, L.R.; Ye, X.; Wang, J.; Tong, S. Extreme temperatures and paediatric emergency department admissions. J. Epidemiol. Community Health 2014, 68, 304–311. [Google Scholar] [CrossRef] [PubMed]
- Datar, A.; Liu, J.; Linnemayr, S.; Stecher, C. The impact of natural disasters on child health and investments in rural India. Soc. Sci. Med. 2013, 76, 83–91. [Google Scholar] [CrossRef] [PubMed]
- Whitmee, S.; Haines, A.; Beyrer, C.; Boltz, F.; Capon, A.G.; de Souza Dias, B.F.; Ezeh, A.; Frumkin, H.; Gong, P.; Head, P.; et al. Safeguarding human health in the Anthropocene epoch: Report of The Rockefeller Foundation–Lancet Commission on planetary health. Lancet 2015. [Google Scholar] [CrossRef]
- Kistin, E.J.; Fogarty, J.; Pokrasso, R.S.; McCally, M.; McCornick, P.G. Climate change, water resources and child health. Arch. Dis. Child. 2010, 95, 545–549. [Google Scholar] [CrossRef] [PubMed]
- Mas-Coma, S.; Valero, M.A.; Bargues, M.D. Climate change effects on trematode and nematode diseases affecting children in rural areas of developing countries. Int. Public Health J. 2011, 2, 405–430. [Google Scholar]
- Our climate, our children, our responsibility: The implications of climate change for the world’s children; UNICEF, United Nations Children’s Fund: New York, NY, USA, 2008.
- Shonkoff, J.P.; Garner, A.S. The lifelong effects of early childhood adversity and toxic stress. Pediatrics 2012, 129, e232–e246. [Google Scholar] [CrossRef] [PubMed]
- McDermott, B.M.; Lee, E.M.; Judd, M.; Gibbon, P. Posttraumatic stress disorder and general psychopathology in children and adolescents following a wildfire disaster. Can. J. Psychiatry Revue Can. Psychiatr. 2005, 50, 137–143. [Google Scholar]
- Stain, H.J.; Dean, J.; Kelly, B.; Blinkhorn, S.; Carnie, T. Climate Adversity: Yet Another Stressor for Rural Adolescents. Int. Public Health J. 2011, 2, 513–519. [Google Scholar]
- Waterston, T.; Lenton, S. Sustainable development, human induced global climate change, and the health of children. Arch. Dis. Child. 2000, 82, 95–97. [Google Scholar] [CrossRef] [PubMed]
- Keating, D.P.; Hertzman, C. Developmental Health and the Wealth of Nations: Social, Biological and Educational Dynamics; The Guilford Press: New York, NY, USA, 1999; p. 406. [Google Scholar]
- Robert F. Kennedy Speeches: Remarks at the University of Kansas, March 18, 1968. Available online: http://www.jfklibrary.org/Research/Research-Aids/Ready-Reference/RFK-Speeches/Remarks-of-Robert-F-Kennedy-at-the-University-of-Kansas-March-18-1968.aspx (accessed on 24 August 2015).
- Piketty, T. Capital in the Twenty-First Century; The Belknap Press of Harvard University Press: Cambridge, MA, USA, 2014. [Google Scholar]
- Klein, N. This Changes Everything: Capitalism vs. the Climate; Simon & Schuster: New York, NY, USA, 2014. [Google Scholar]
- Seal, A.; Vasudevan, C. Climate change and child health. Arch. Dis. Child. 2011, 96, 1162–1166. [Google Scholar] [CrossRef] [PubMed]
- Hosking, J.; Jones, R.; Percival, T.; Turner, N.; Ameratunga, S. Climate change: The implications for child health in Australasia. J. Paediatr. Child Health 2011, 47, 493–496. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, A.S.; Myers, S.S. Climate change and children’s health. Curr. Opin. Pediatr. 2011, 23, 221–226. [Google Scholar] [CrossRef] [PubMed]
- Watts, N.; Adger, W.N.; Agnolucci, P.; Blackstock, J.; Byass, P.; Cai, W.; Chaytor, S.; Colbourn, T.; Collins, M.; Cooper, A.; et al. Health and climate change: Policy responses to protect public health. Lancet 2015. [Google Scholar] [CrossRef]
- Costello, A.; Abbas, M.; Allen, A.; Ball, S.; Bell, S.; Bellamy, R.; Friel, S.; Groce, N.; Johnson, A.; Kett, M.; et al. Managing the health effects of climate change: Lancet and University College London Institute for Global Health Commission. Lancet. 2009, 373, 1693–1733. [Google Scholar] [CrossRef]
- Capital Area Health Consortium (CAHC). Climate and Health Council. Available online: http://www.climateandhealth.org/resources.html (accessed on 19 August 2015).
- Health Care Without Harm. Available online: http://greenhospitals.net/en/overview/ (accessed on 19 August 2015).
- World Health Organization and Health Care Without Harm (WHO and HCWH). Healthy Hospitals, Healthy Planet, Healthy People: Addressing Climate Change in Healthcare Settings; WHO and HCWH, 2009. [Google Scholar]
- Instituto Superior de Derecho y Economía (ISDE). International Society of Doctors for the Environment. Available online: http://www.isde.org/ (accessed on 20 August 2015).
- McMichael, A.J.; Leeder, S.R.; Armstrong, B.K.; Basten, A.; Doherty, P.C.; Douglas, R.M.; Green, A.C.; Nossal, G.J.; Shearman, D.J.; Stanley, F.J.; et al. Open letter to the Hon Tony Abbott MP. Med. J. Aust. 2014, 201. [Google Scholar] [CrossRef] [PubMed]
- The Escalator. Available online: http://www.skepticalscience.com/graphics.php?g=47 (accessed on 20 August 2015).
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stanley, F.; Farrant, B. Climate Change and Children’s Health: A Commentary. Children 2015, 2, 412-423. https://doi.org/10.3390/children2040412
Stanley F, Farrant B. Climate Change and Children’s Health: A Commentary. Children. 2015; 2(4):412-423. https://doi.org/10.3390/children2040412
Chicago/Turabian StyleStanley, Fiona, and Brad Farrant. 2015. "Climate Change and Children’s Health: A Commentary" Children 2, no. 4: 412-423. https://doi.org/10.3390/children2040412
APA StyleStanley, F., & Farrant, B. (2015). Climate Change and Children’s Health: A Commentary. Children, 2(4), 412-423. https://doi.org/10.3390/children2040412






