Influence of the Severity of Osteogenesis Imperfecta on Cranial Measurements †
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Sample and Controls
2.3. Data Collection
2.4. Statistical Analysis
- -
- Descriptive statistics of quantitative and qualitative variables.
- -
- Student’s t test for the comparison of two means; Mann–Whitney U test for non-normal distributions; Shapiro–Wilk test to determine normality.
- -
- ANOVA for the comparison of multiple means. In the case of non-homogeneous variances, robust tests of equality of means were used: the Welch and Brown–Forsythe tests. When the data did not come from a normal distribution, we used the Kruskal–Wallis test to compare multiple means.
- -
- Pearson correlation test to study the correlation with age, applying regression lines and analysis of covariance (ANCOVA), to the variables where correlation with age was observed.
3. Results
3.1. CCJ Measurements on MRI
3.2. CCJ Measurements on Lateral Skull Radiographs
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Rouvière, H.; Delmas, A. [Anatomía Humana Descriptiva Topográfica y Funcional]. Topographic and Functional Descriptive Human Anatomy, 11th ed.; Masson: Barcelona, Spain, 2005. [Google Scholar]
- Boleaga-Durán, B.; Suárez, E.; Tomasini, P.; Reyes, J. [Anatomía y patología de la unión craneovertebral]. Anatomy and pathology of the craniovertebral junction. An. Radiol. México 2006, 2, 153–170. [Google Scholar]
- Ludwig, K.; Seiltgens, C.; Ibba, A.; Saran, N.; Ouellet, J.A.; Glorieux, F.; Rauch, F. Craniocervical abnormalities in osteogenesis imperfecta type V. Osteoporos. Int. 2022, 33, 177–183. [Google Scholar] [CrossRef] [PubMed]
- Wadanamby, S.; El Garwany, S.; Connolly, D.; Arundel, P.; Bishop, N.J.; DeVile, C.J.; Calder, A.D.; Crowe, B.; Burren, C.P.; Saraff, V. Highly Specialised Service for Severe, Complex and Atypical Osteogenesis Imperfecta (NHS England); Offiah AC. Monitoring Skull Base Abnormalities in Children with Osteogenesis Imperfecta—Review of Current Practice and a Suggested Clinical Pathway. Bone 2022, 154, 116235. [Google Scholar] [CrossRef] [PubMed]
- Pinter, N.K.; McVige, J.; Mechtler, L. Basilar Invagination, Basilar Impression, and Platybasia: Clinical and Imaging Aspects. Curr. Pain. Headache Rep. 2016, 20, 49. [Google Scholar] [CrossRef]
- Gremminger, V.L.; Phillips, C.L. Impact of Intrinsic Muscle Weakness on Muscle-Bone Crosstalk in Osteogenesis Imperfecta. Int. J. Mol. Sci. 2021, 22, 4963. [Google Scholar] [CrossRef]
- Janus, G.J.; Engelbert, R.H.; Beek, E.; Gooskens, R.H.; Pruijs, J.E. Osteogenesis imperfecta in childhood: MR imaging of basilar impression. Eur. J. Radiol. 2003, 47, 19–24. [Google Scholar] [CrossRef]
- Ibrahim, A.G.; Crockard, H.A. Basilar impression and osteogenesis imperfecta: A 21-year retrospective review of outcomes in 20 pacients. J. Neurosurg. Spine 2007, 7, 594–600. [Google Scholar] [CrossRef]
- Menezes, A. Specific entities affecting the craniocervical region. Osteogenesis imperfecta and related osteochondrodysplasias: Medical and surgical management of basilar impression. Childs Nerv. Syst. 2008, 24, 1169–1172. [Google Scholar] [CrossRef]
- Smoker, W.; Khanna, G. Imaging the craniocervical junction. Childs Nerv. Syst. 2008, 24, 1123–1145. [Google Scholar] [CrossRef]
- Arponen, H.; Mäkitie, O.; Haukka, J.; Ranta, H.; Ekholm, M.; Mäyränpää, M.K.; Kaitila, I.; Waltimo-Sirén, J. Prevalence and natural course of craniocervical junction anomalies during growth in patients with osteogenesis imperfecta. J. Bone Miner. Res. 2012, 27, 1142–1149. [Google Scholar] [CrossRef]
- Sillence, D.O. Craniocervical abnormalities in osteogenesis imperfecta: Genetic and molecular correlation. Pediatr. Radiol. 1994, 24, 427–430. [Google Scholar] [CrossRef] [PubMed]
- McAllion, S.J.; Paterson, C.R. Causes of death in osteogenesis imperfecta. J. Clin. Pathol. 1996, 49, 627–630. [Google Scholar] [CrossRef] [PubMed]
- Jannelli, G.; Moiraghi, A.; Paun, L.; Tessitore, E.; Dayer, R.; Bartoli, A. Severe Basilar impression in osteogenesis imperfecta treated with halo gravity traction, occipitocervicothoracic fusion, foramen magnum and upper cervical decompression and expansive duroplasty: A technical note. Childs Nerv. Syst. 2022, 38, 991–995. [Google Scholar] [CrossRef] [PubMed]
- Cobanoglu, M.; Bauer, J.M.; Campbell, J.W.; Shah, S.A. Basilar impression in osteogenesis imperfecta treated with staged halo traction and posterior decompression with short-segment fusion. J. Craniovertebr. Junction Spine 2018, 9, 212–215. [Google Scholar] [CrossRef]
- Sawin, P.D.; Menezes, A.H. Basilar invagination in osteogenesis imperfecta and related osteochondrodysplasias: Medical and surgical management. J. Neurosurg. 1997, 86, 950–960. [Google Scholar] [CrossRef]
- Hayes, M.; Parker, G.; Ell, J.; Sillence, D. Basilar impression complicating osteogenesis imperfecta type IV: The clinical and neuroradiological findings in four cases. J. Neurol. Neurosurg. Psychiatry 1999, 66, 357–364. [Google Scholar] [CrossRef]
- Léotard, A.; Taytard, J.; Aouate, M.; Boule, M.; Forin, V.; Lallemant-Dudek, P. Diagnosis, follow-up and management of sleep-disordered breathing in children with osteogenesis imperfecta. Ann. Phys. Rehabil. Med. 2018, 61, 135–139. [Google Scholar] [CrossRef]
- Smoker, W.R.; Keyes, W.D.; Dunn, V.D.; Menezes, A.H. MRI versus conventional radiologic examinations in the evaluation of the craniovertebral and cervicomedullary junction. Radiographics 1986, 6, 953–994. [Google Scholar] [CrossRef]
- Kovero, O.; Pynnönen, S.; Kuurila-svahn, K.; Kaitila, I.; Waltimo-sirén, J. Skull base abnormalities in osteogenesis imperfecta: A cephalometric evaluation of 54 patients and 108 control volunteers. J. Neurosurg. 2006, 105, 361–370. [Google Scholar] [CrossRef]
- Arponen, H.; Elf, H.; Evälahti, M.; Waltimo-Sirén, J. Reliability of cranial base measurements on lateral skull radiographs. Orthod. Craniofac. Res. 2008, 11, 201–210. [Google Scholar] [CrossRef]
- Kwong, Y.; Rao, N.; Latief, K. Craniometric measurements in the assessment of craniovertebral settling: Are they still relevant in the age of cross-sectional imaging? AJR Am. J. Roentgenol. 2011, 196, W421–W425. [Google Scholar] [CrossRef]
- Noske, D.P.; Van Royen, B.J.; Bron, J.L.; Vandertop, W.P. Basilar impression in osteogenesis imperfecta: Can it be treated with halo traction and posterior fusion? Acta Neurochir. 2006, 148, 1301–1305. [Google Scholar] [CrossRef] [PubMed]
- Riew, K.D.; Hilibrand, A.S.; Palumbo, M.A.; Sethi, N.; Bohlman, H.H. Diagnosing basilar invagination in the rheumatoid patient: The reliability of radiographic criteria. J. Bone Joint Surg. Am. 2001, 83, 194–200. [Google Scholar] [CrossRef] [PubMed]
- Engelbert, R.H.; Gerver, W.J.; Breslau-Siderius, L.J.; van der Graaf, Y.; Pruijs, H.E.; van Doorne, J.M.; Beemer, F.A.; Helders, P.J. Spinal complications in osteogénesis imperfecta: 47 patients 1–16 years of age. Acta Orthop. Scand. 1998, 69, 283–286. [Google Scholar] [CrossRef] [PubMed]
- Cheung, M.S.; Arponen, H.; Roughley, P.; Azouz, M.E.; Glorieux, F.H.; Waltimo-Sirén, J.; Rauch, F. Cranial base abnormalities in osteogenesis imperfecta: Phenotypic and genotypic determinants. J. Bone Miner. Res. 2011, 26, 405–413. [Google Scholar] [CrossRef] [PubMed]
- Aldana, A.; Báez, J.; Sandoval, C.; Vergara, C.; Cauvi, D.; Fernández de la Reguera, A. Asociación entre maloclusiones y posición de cabeza y cuello [Association between malocclusion and position of the head and neck]. Int. J. Odontostomat 2011, 5, 119–125. [Google Scholar] [CrossRef]
- Heredia Rizo, A.M.; Albornoz Cabello, M.; Piña Pozo, F.; Luque Carrasco, A. La postura del segmento craneocervical y su relación con la oclusión dental y la aplicación de ortodoncia: Estudio de revisión. [Craniocervical segment posture and its relationship to dental occlusion and orthodontic application: A review study]. Osteopat. Científica 2010, 5, 89–96. [Google Scholar] [CrossRef]
- De Nova-García, M.J.; Bernal-Barroso, F.; Mourelle-Martínez, M.R.; Gallardo-López, N.E.; Diéguez-Pérez, M.; Feijoo-García, G.; Burgueño-Torres, L. Evaluation of the Severity of Malocclusion in Children with Osteogenesis Imperfecta. J. Clin. Med. 2022, 11, 4862. [Google Scholar] [CrossRef]
- Arponen, H.; Evälahti MWaltimo-Sirén, J. Dimensions of the craniocervical junction in longitudinal analysis of normal growth. Childs Nerv. Syst. 2010, 26, 763–769. [Google Scholar] [CrossRef]
- Arponen, H.; Vuorimies, I.; Haukka, J.; Valta, H.; Waltimo-Sirén, J.; Mäkitie, O. Cranial base pathology in pediatric osteogenesis imperfecta patients treated with bisphosphonates. J. Neurosurg. Pediatr. 2015, 15, 313–320. [Google Scholar] [CrossRef]
- Pozo, J.L.; Crokard, H.A.; Ransford, A.O. Basilar impression in osteogenesis imperfecta. A report of three cases in one family. J. Bone Joint Surg. 1984, 66, 233–238. [Google Scholar] [CrossRef]
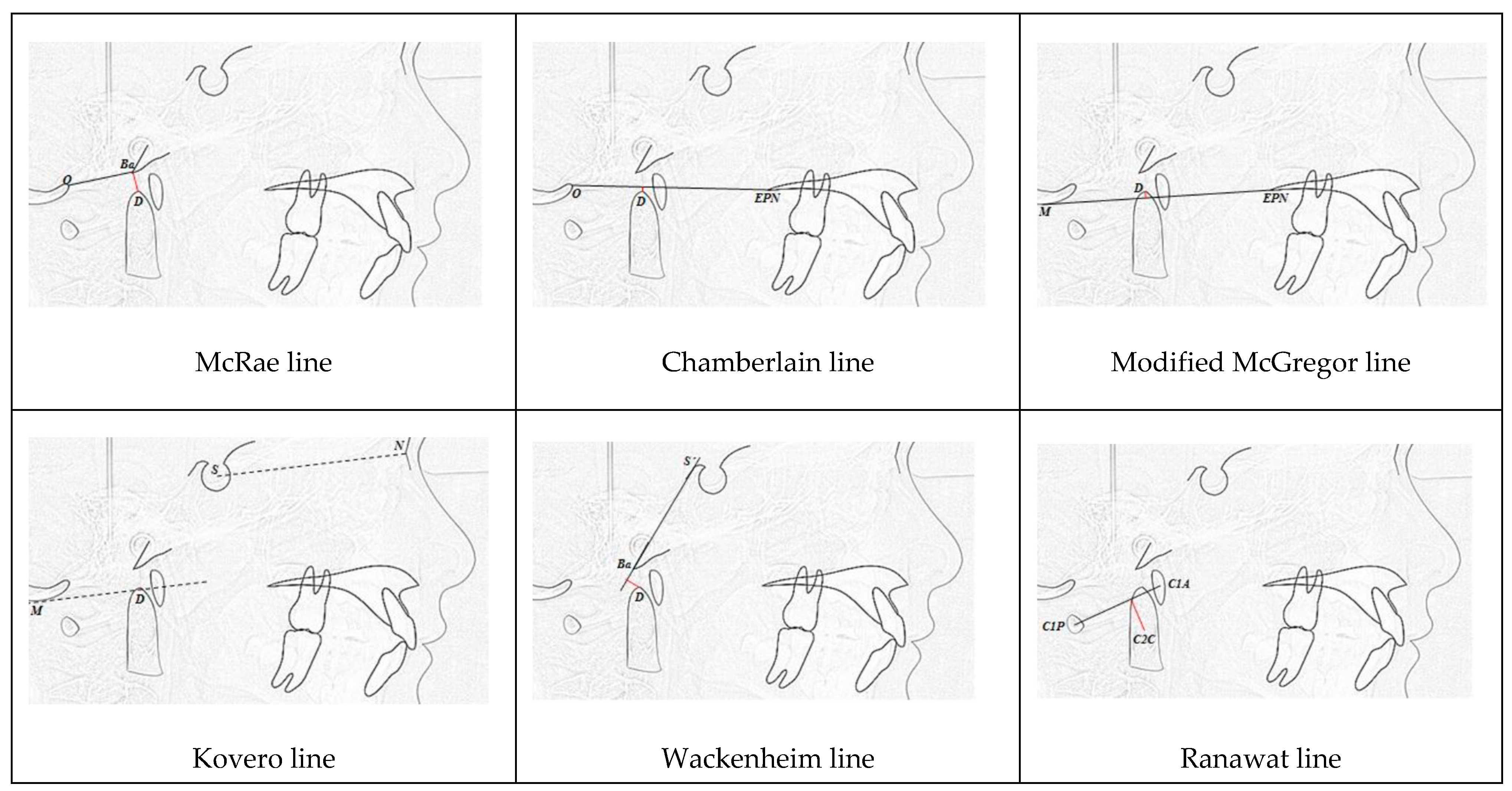
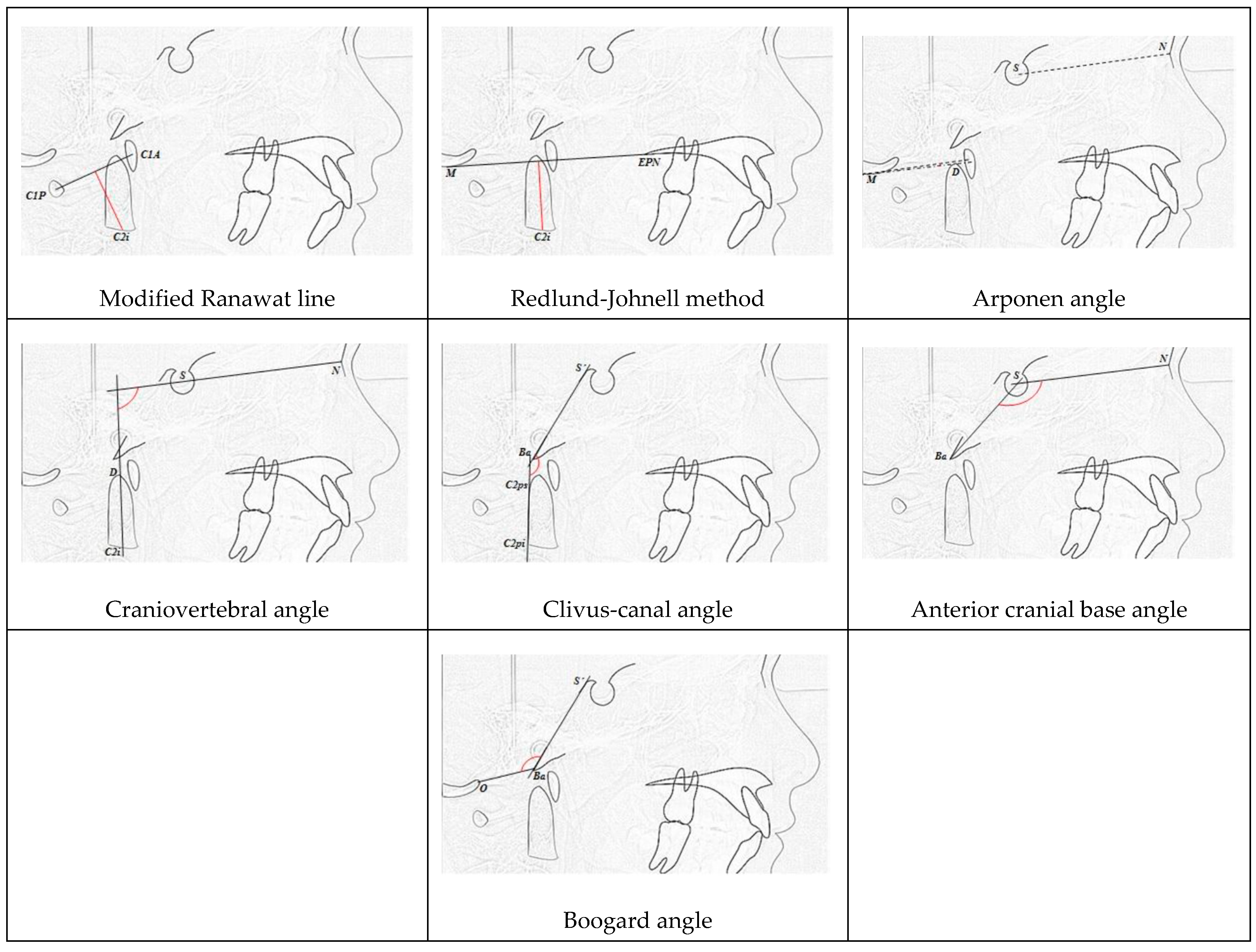
| CCJ Measurements | Controls (n = 28) | OI (n = 14) | p | ||
|---|---|---|---|---|---|
| Slight (n = 4) | Moderate (n = 4) | Severe (n = 6) | |||
| McRae | −4.87 ± 1.24 | −4.58 ± 0.77 | −3.2 ± 1 | −1.69 ± 4.31 | 0.016 * |
| Chamberlain | −2.26 ± 3.23 | −0.6 ± 2.05 | 1.95 ± 2.48 | 4.96 ± 7.35 | 0.033 |
| Modified McGregor | −1.16 ± 3.33 | 0.34 ± 2.55 | 1.76 ± 3.05 | 10.06 ± 12.81 | 0.068 |
| Kovero | −5.57 ± 4.23 | −6.48 ± 2.07 | −5.13 ± 5.03 | 5.24 ± 17.19 | 0.193 |
| Wackenheim | −2.2 ± 1.52 | −2.04 ± 0.56 | 0.38 ± 0.93 | 0.48 ± 4.49 | 0.008 * |
| Ranawat | 14.99 ± 2.04 | 13.8 ± 1.67 | 11.91 ± 1.08 | 12.2 ± 1.88 | 0.003 * |
| Modified Ranawat | 26.81 ± 2.82 | 25.08 ± 1.37 | 23.45 ± 1.36 | 23.34 ± 1.83 | 0.007 * |
| Redlund-Johnell | 34.37 ± 4.32 | 31.19 ± 3.74 | 29.54 ± 4.45 | 19.07 ± 13.17 | 0.001 * |
| Arponen | 9.76 ± 4.91 | 9.44 ± 3.59 | 6.4 ± 5.62 | 17.03 ± 13.65 | 0.072 |
| Cranio-vertebral | 90.66 ± 7.76 | 86.43 ± 1.36 | 91.95 ± 8.41 | 89.19 ± 13.15 | 0.768 |
| Clivus-canal | 153.62 ± 7.47 | 141.23 ± 2.5 | 150.41 ± 5.3 | 135.86 ± 20.47 | 0.001 * |
| Basal | 129.71 ± 6.45 | 139.1 ± 4.17 | 138.06 ± 6.86 | 151.25 ± 8.53 | 0.000 * |
| Boogard | 118.22 ± 6.24 | 126.05 ± 6.48 | 123.51 ± 6.34 | 140.63 ± 18.9 | 0.001 * |
| CCJ Measurements | Controls (n = 38) | OI (n = 14) | p | ||
|---|---|---|---|---|---|
| Slight (n = 4) | Moderate (n = 7) | Severe (n = 8) | |||
| McRae | −4.54 ± 2.56 | −5.04 ± 2.58 | −3.99 ± 2.04 | −1.93 ± 4.45 | 0.292 |
| Chamberlain | −1.72 ± 2.98 | −2.85 ± 4.24 | −0.6 ± 3.26 | −0.12 ± 5.1 | 0.639 |
| Modified McGregor | 0.13 ± 3 | −0.81 ± 4.65 | 1.54 ± 2.89 | 2.12 ± 4.59 | 0.442 |
| Kovero | −4.52 ± 3.47 | −7.1 ± 6.91 | −5.61 ± 5.05 | −5.57 ± 7.35 | 0.909 |
| Wackenheim | −3.27 ± 2.32 | −4.25 ± 2.29 | −1.84 ± 1.24 | −2.84 ± 3.33 | 0.374 |
| Ranawat | 14.33 ± 1.95 | 12.49 ± 1.96 | 12.55 ± 1.04 | 10.08 ± 1.99 | 0.000 * |
| Modified Ranawat | 26.35 ± 3.08 | 23.41 ± 3 | 24.94 ± 1.57 | 22.59 ± 2.36 | 0.000 * |
| Redlund-Johnell | 33.12 ± 5 | 29.68 ± 6.55 | 30.27 ± 4.6 | 28.79 ± 5.66 | 0.000 * |
| Arponen | 8.47 ± 4.96 | 13 ± 12.52 | 10.07 ± 6.76 | 12.88 ± 8.39 | 0.534 |
| Cranio-vertebral | 92.94 ± 7.45 | 90.43 ± 2.51 | 93.55 ± 11.66 | 102.65 ± 7.98 | 0.018 * |
| Clivus-canal | 150.26 ± 8.35 | 140.24 ± 4.19 | 139.62 ± 13.17 | 147.45 ± 7.22 | 0.011 * |
| Basal | 133.06 ± 4.87 | 143.05 ± 6.38 | 144.61 ± 4.42 | 145.43 ± 3.21 | 0.000 * |
| Boogard | 121.66 ± 6.36 | 127.14 ± 13.02 | 128.08 ± 11.8 | 127.03 ± 10.17 | 0.109 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
De Nova-García, M.J.; Sola, R.G.; Burgueño-Torres, L. Influence of the Severity of Osteogenesis Imperfecta on Cranial Measurements. Children 2023, 10, 1029. https://doi.org/10.3390/children10061029
De Nova-García MJ, Sola RG, Burgueño-Torres L. Influence of the Severity of Osteogenesis Imperfecta on Cranial Measurements. Children. 2023; 10(6):1029. https://doi.org/10.3390/children10061029
Chicago/Turabian StyleDe Nova-García, Manuel Joaquín, Rafael G. Sola, and Laura Burgueño-Torres. 2023. "Influence of the Severity of Osteogenesis Imperfecta on Cranial Measurements" Children 10, no. 6: 1029. https://doi.org/10.3390/children10061029
APA StyleDe Nova-García, M. J., Sola, R. G., & Burgueño-Torres, L. (2023). Influence of the Severity of Osteogenesis Imperfecta on Cranial Measurements. Children, 10(6), 1029. https://doi.org/10.3390/children10061029






