Treatment of Dyslipidaemia in Children
Abstract
:1. Introduction
2. Pathophysiology
3. Paediatric Guidelines
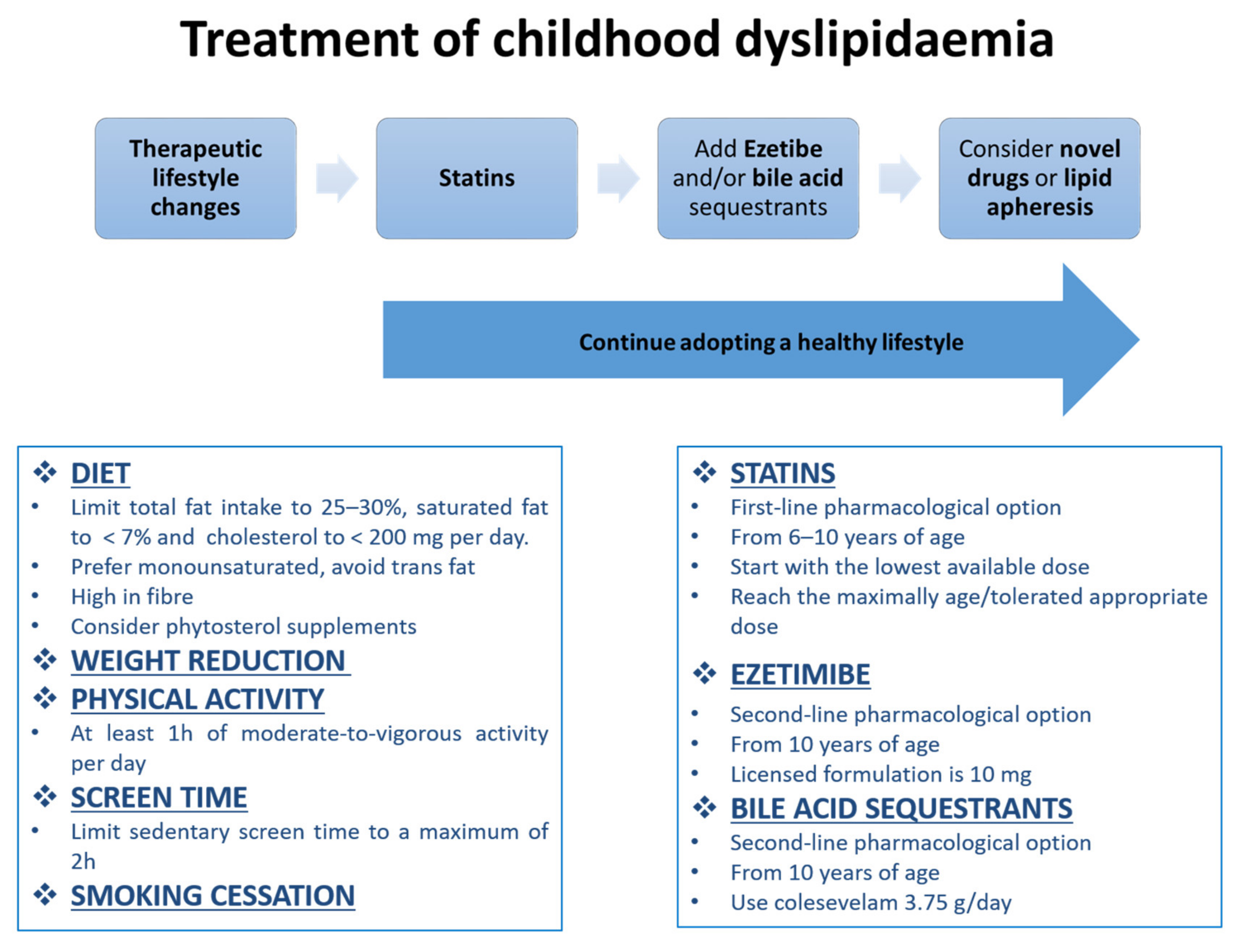
4. Management of Dyslipidaemia in Children
4.1. Non-Pharmacological Approaches
4.2. Family-Based Approach
4.3. Pharmacological Treatment
4.3.1. Approved Pharmacological Treatment for Children
Statins
Ezetimibe and Bile Acid Sequestrants
4.3.2. Non-Approved Pharmacological Treatment for Children
Fibrates and Niacin
4.3.3. Additional Lipid-Lowering Options
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Benjamin, E.J.; Virani, S.S.; Callaway, C.W.; Chamberlain, A.M.; Chang, A.R.; Cheng, S.; Chiuve, S.E.; Cushman, M.; Delling, F.N.; Deo, R.; et al. Heart disease and stroke statistics—2018 update: A report from the American Heart Association. Circulation 2018, 137, e493. [Google Scholar] [CrossRef]
- Mangili, L. High Prevalence of Dyslipidemia in Children and Adolescents: Opportunity for Prevention. Arq. Bras. Cardiol. 2020, 114, 57–58. [Google Scholar] [CrossRef]
- National Heart, Lung, and Blood Institute. Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents: Summary Report. Pediatrics 2011, 128 (Suppl. S5), S213–S256. [Google Scholar] [CrossRef] [Green Version]
- Françoso, L.A.; Coates, V. Anatomicopathological evidence of the beginning of atherosclerosis in infancy and adolescence. Arq. Bras. Cardiol. 2002, 78, 137–142. [Google Scholar] [CrossRef] [Green Version]
- Linton, M.F.; Yancey, P.G.; Davies, S.S.; Jerome, W.G.; Linton, E.F.; Song, W.L.; Doran, A.C.; Vickers, K.C. The Role of Lipids and Lipoproteins in Atherosclerosis; MDText.com, Inc: South Dartmouth, MA, USA, 2019. [Google Scholar]
- De Ferranti, S.D.; Steinberger, J.; Ameduri, R.; Baker, A.; Gooding, H.; Kelly, A.S.; Mietus-Snyder, M.; Mitsnefes, M.M.; Peterson, A.L.; St-Pierre, J.; et al. Cardiovascular Risk Reduction in High-Risk Pediatric Patients: A Scientific Statement From the American Heart Association. Circulation 2019, 139, e603–e634. [Google Scholar] [CrossRef] [PubMed]
- De Ferranti, S.D.; Rodday, A.M.; Mendelson, M.M.; Wong, J.B.; Leslie, L.K.; Sheldrick, C. Prevalence of Familial Hypercholesterolemia in the 1999 to 2012 United States National Health and Nutrition Examination Surveys (NHANES). Circulation 2016, 133, 1067–1072. [Google Scholar] [CrossRef] [PubMed]
- Skinner, A.C.; Perrin, E.M.; Skelton, J.A. Prevalence of obesity and severe obesity in US children, 1999–2014. Obesity 2016, 24, 1116–1123. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Garrido-Miguel, M.; Cavero-Redondo, I.; Álvarez-Bueno, C.; Rodríguez-Artalejo, F.; Moreno, L.A.; Ruiz, J.R.; Ahrens, W.; Martínez-Vizcaíno, V. Prevalence and Trends of Overweight and Obesity in European Children From 1999 to 2016: A Systematic Review and Meta-analysis. JAMA Pediatr. 2019, 173, e192430. [Google Scholar] [CrossRef]
- Elkins, C.; Fruh, S.; Jones, L.; Bydalek, K. Clinical Practice Recommendations for Pediatric Dyslipidemia. J. Pediatr. Health Care 2019, 33, 494–504. [Google Scholar] [CrossRef] [Green Version]
- Belay, B.; Belamarich, P.F.; Tom-Revzon, C. The use of statins in pediatrics: Knowledge base, limitations, and future directions. Pediatrics 2007, 119, 370–380. [Google Scholar] [CrossRef]
- Daniels, S.R. Pediatric guidelines for dyslipidemia. J. Clin. Lipidol. 2015, 9 (Suppl. S5), S5–S10. [Google Scholar] [CrossRef]
- National Cholesterol Education Program (NCEP). Highlights of the report of the Expert Panel on Blood Cholesterol Levels in Children and Adolescents. Pediatrics 1992, 89, 495–501. [Google Scholar]
- Tamir, I.; Heiss, G.; Glueck, C.J.; Christensen, B.; Kwiterovich, P.; Rifkind, B.M. Lipid and lipoprotein distributions in white children ages 6–19 yr. The Lipid Research Clinics Program Prevalence Study. J. Chronic. Dis. 1981, 34, 27–39. [Google Scholar] [CrossRef]
- American Academy of Pediatrics; Committee on Nutrition. Cholesterol in childhood. Pediatrics 1998, 101 Pt 1, 141–147. [Google Scholar]
- Daniels, S.R.; Greer, F.R. Lipid Screening and cardiovascular health in childhood. Pediatrics 2008, 122, 198–208. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gidding, S.S.; Dennison, B.A.; Birch, L.L.; Daniels, S.R.; Gillman, M.W.; Lichtenstein, A.H.; Rattay, K.T.; Steinberger, J.; Stettler, N.; Van Horn, L.; et al. Dietary recommendations for children and adolescents: A guide for practitioners: Consensus statement from the American Heart Association. Circulation 2005, 112, 2061–2075. [Google Scholar] [CrossRef] [PubMed]
- McCrindle, B.W.; Urbina, E.M.; Dennison, B.A.; Jacobson, M.S.; Steinberger, J.; Rocchini, A.P.; Hayman, L.L.; Daniels, S.R.; American Heart Association Atherosclerosis, Hypertension, and Obesity in Youth Committee; American Heart Association Council of Cardiovascular Disease in the Young; et al. Drug therapy of high-risk lipid abnormalities in children and adolescents: A scientific statement from the American Heart Association Atherosclerosis, Hypertension, and Obesity in Youth Committee, Council of Cardiovascular Disease in the Young, with the Council on Cardiovascular Nursing. Circulation 2007, 115, 1948–1967. [Google Scholar] [PubMed] [Green Version]
- Miller, M.L.; Wright, C.C.; Browne, B. Lipid-lowering medications for children and adolescents. J. Clin. Lipidol. 2015, 9, S67–S76. [Google Scholar] [CrossRef]
- Elkins, C.; Friedrich, D. Hypertriglyceridemia: A review of the evidence. Nurse Pract. 2018, 43, 22–29. [Google Scholar] [CrossRef]
- Stewart, J.; McCallin, T.; Martinez, J.; Chacko, S.; Yusuf, S. Hyperlipidemia. Pediatr. Rev. 2020, 41, 393–402. [Google Scholar] [CrossRef] [PubMed]
- Moon, R.Y. Task Force on Sudden Infant Death Syndrome. SIDS and Other Sleep-Related Infant Deaths: Updated 2016 Recommendations for a Safe Infant Sleeping Environment. Pediatrics 2016, 138, e20162938. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Manousaki, D.; Quality Cohort Collaborative Group; Barnett, T.; Mathieu, M.-E.; Maximova, K.; Simoneau, G.; Harnois-Leblanc, S.; Benedetti, A.; McGrath, J.; Henderson, M. Tune out and turn in: The influence of television viewing and sleep on lipid profiles in children. Int. J. Obes. 2020, 44, 1173–1184. [Google Scholar] [CrossRef] [PubMed]
- Estruch, R.; Ros, E.; Salas-Salvadó, J.; Covas, M.-I.; Corella, D.; Arós, F.; Gómez-Gracia, E.; Ruiz-Gutiérrez, V.; Fiol, M.; Lapetra, J.; et al. Primary Prevention of Cardiovascular Disease with a Mediterranean Diet Supplemented with Extra-Virgin Olive Oil or Nuts. N. Engl. J. Med. 2018, 378, e34. [Google Scholar] [CrossRef] [PubMed]
- Giannini, C.; Diesse, L.; D’Adamo, E.; Chiavaroli, V.; de Giorgis, T.; Di Iorio, C.; Chiarelli, F.; Mohn, A. Influence of the Mediterranean diet on carotid intima-media thickness in hypercholesterolaemic children: A 12-month intervention study. Nutr. Metab. Cardiovasc. Dis. 2014, 24, 75–82. [Google Scholar] [CrossRef]
- McCord, M.; Lee, L. Dyslipidemia in children. Nonpharmacologic approaches for early intervention. Adv. NPs PAs 2011, 2, 29. [Google Scholar]
- Corkins, M.R.; Daniels, S.R.; de Ferranti, S.D.; Golden, N.H.; Kim, J.H.; Magge, S.N.; Schwarzenberg, S.J. Nutrition in Children and Adolescents. Med. Clin. N. Am. 2016, 100, 1217–1235. [Google Scholar] [CrossRef]
- Yoon, J.M. Dyslipidemia in Children and Adolescents: When and How to Diagnose and Treat? Pediatr. Gastroenterol. Hepatol. Nutr. 2014, 17, 85–92. [Google Scholar] [CrossRef] [Green Version]
- Karalis, D.G. A review of clinical practice guidelines for the management of hypertriglyceridemia: A focus on high dose ome-ga-3 fatty acids. Adv. Ther. 2017, 34, 300–323. [Google Scholar] [CrossRef] [Green Version]
- Skulas-Ray, A.C.; Wilson, P.W.F.; Harris, W.S.; Brinton, E.A.; Kris-Etherton, P.M.; Richter, C.K.; Jacobson, T.A.; Engler, M.B.; Miller, M.; Robinson, J.G.; et al. Omega-3 Fatty Acids for the Management of Hypertriglyceridemia: A Science Advisory From the American Heart Association. Circulation 2019, 140, e673–e691. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gylling, H.; Plat, J.; Turley, S.D.; Ginsberg, H.N.; Ellegård, L.; Jessup, W.; Jones, P.J.H.; Lütjohann, D.; März, W.; Masana, L.; et al. Plant sterols and plant stanols in the management of dyslipidaemia and prevention of cardiovascular disease. Atherosclerosis 2014, 232, 346–360. [Google Scholar] [CrossRef]
- Writing Group for the DISC Collaborative Research Group. Efficacy and safety of lowering dietary intake of fat and cholesterol in children with elevated low-density lipoprotein cholesterol: The Dietary Intervention Study in Children (DISC). JAMA 1995, 273, 1429–1435. [Google Scholar] [CrossRef] [PubMed]
- Niinikoski, H.; Lagström, H.; Jokinen, E.; Siltala, M.; Rönnemaa, T.; Viikari, J.; Raitakari, O.T.; Jula, A.; Marniemi, J.; Nanto-Salonen, K.; et al. Impact of Repeated Dietary Counseling Between Infancy and 14 Years of Age on Dietary Intakes and Serum Lipids and Lipoproteins: the STRIP study. Circulation 2007, 116, 1032–1040. [Google Scholar] [CrossRef] [Green Version]
- Matthews, L.A.; Rovio, S.P.; Jaakkola, J.M.; Niinikoski, H.; Lagström, H.; Jula, A.; Viikari, J.S.A.; Rönnemaa, T.; Simell, O.; Raitakari, O.T.; et al. Longitudinal effect of 20-year infancy-onset dietary intervention on food consumption and nutrient intake: The randomized controlled STRIP study. Eur. J. Clin. Nutr. 2019, 73, 937–949. [Google Scholar] [CrossRef] [PubMed]
- Niinikoski, H.; Pahkala, K.; Ala-Korpela, M.; Viikari, J.; Rönnemaa, T.; Lagström, H.; Jokinen, E.; Jula, A.; Savolainen, M.J.; Simell, O.; et al. Effect of Repeated Dietary Counseling on Serum Lipoproteins From Infancy to Adulthood. Pediatrics 2012, 129, e704–e713. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Harada-Shiba, M.; Arai, H.; Ishigaki, Y.; Ishibashi, S.; Okamura, T.; Ogura, M.; Dobashi, K.; Nohara, A.; Bujo, H.; Miyauchi, K.; et al. Guidelines for Diagnosis and Treatment of Familial Hypercholesterolemia 2017. J. Atheroscler. Thromb. 2018, 25, 751–770. [Google Scholar] [CrossRef] [Green Version]
- Lampropoulou, M.; Chaini, M.; Rigopoulos, N.; Evangeliou, A.; Papadopoulou-Legbelou, K.; Koutelidakis, A.E. Association between Serum Lipid Levels in Greek Children with Dyslipidemia and Mediterranean Diet Adherence, Dietary Habits, Lifestyle and Family Socioeconomic Factors. Nutrients 2020, 12, 1600. [Google Scholar] [CrossRef] [PubMed]
- West, S.L.; Banks, L.; Schneiderman, J.E.; Caterini, J.E.; Stephens, S.; White, G.; Dogra, S.; Wells, G.D. Physical activity for children with chronic disease; a narrative review and practical applications. BMC Pediatr. 2019, 19, 1–18. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lobelo, F.; Muth, N.D.; Hanson, S.; Nemeth, B.A.; Council on Sports Medicine and Fitness; Section On Obesity. Physical Activity Assessment and Counseling in Pediatric Clinical Settings. Pediatrics 2020, 145, e20193992. [Google Scholar] [CrossRef] [Green Version]
- LeBlanc, A.; Janssen, I. Dose-response relationship between physical activity and dyslipidemia in youth. Can. J. Cardiol. 2010, 26, e201–e205. [Google Scholar] [CrossRef]
- Piercy, K.L.; Troiano, R.P.; Ballard, R.M.; Carlson, S.A.; Fulton, J.E.; Galuska, D.A.; George, S.M.; Olson, R.D. The Physical Activity Guidelines for Americans. JAMA 2018, 320, 2020–2028. [Google Scholar] [CrossRef]
- Fruh, S.M. Obesity: Risk factors, complications, and strategies for sustainable long-term weight management. J. Am. Assoc. Nurse Pract. 2017, 29 (Suppl. S1), S3–S14. [Google Scholar] [CrossRef] [PubMed]
- Valaiyapathi, B.; Sunil, B.; Ashraf, A.P. Approach to Hypertriglyceridemia in the Pediatric Population. Pediatr. Rev. 2017, 38, 424–434, Erratum in 2017, 38, 498. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- National Lipid Association. Lifestyle Changes to Reduce Triglycerides. 2016. Available online: www.lipid.org/sites/default/files/NLAClinician’s-Lifestyle-Modification-Toolbox.pdf (accessed on 17 July 2016).
- Horning, M.L.; Fulkerson, J.A.; Friend, S.; Story, M. Reasons Parents Buy Prepackaged, Processed Meals: It Is More Complicated Than “I Don’t Have Time”. J. Nutr. Educ. Behav. 2017, 49, 60–66.e1. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Trofholz, A.C.; Tate, A.D.; Draxten, M.L.; Neumark-Sztainer, D.; Berge, J.M. Home food environment factors associated with the presence of fruit and vegetables at dinner: A direct observational study. Appetite 2016, 96, 526–532. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Patrick, H.; Nicklas, T.A. A Review of Family and Social Determinants of Children’s Eating Patterns and Diet Quality. J. Am. Coll. Nutr. 2005, 24, 83–92. Available online: https://www.ncbi.nlm.nih.gov/pubmed/15798074 (accessed on 15 April 2020). [CrossRef]
- Loth, K.; Friend, S.; Horning, M.; Neumark-Sztainer, D.; Fulkerson, J. Directive and non-directive food-related parenting practices: Associations between an expanded conceptualization of food-related parenting practices and child dietary intake and weight outcomes. Appetite 2016, 107, 188–195. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Savage, J.S.; Fisher, J.O.; Birch, L.L. Parental Influence on Eating Behavior: Conception to Adolescence. J. Law Med. Ethics 2007, 35, 22–34. [Google Scholar] [CrossRef] [Green Version]
- Gidding, S. Special Commentary: Is diet management helpful in familial hypercholesterolemia? Curr. Opin. Clin. Nutr. Metab. Care 2019, 22, 135–140. [Google Scholar] [CrossRef]
- King, K.; Macken, A.; Blake, O.; O’Gorman, C.S. Cholesterol screening and statin use in children: A literature review. Ir. J. Med. Sci. 2019, 188, 179–188. [Google Scholar] [CrossRef]
- Cohen, H.; The Mighty Medic Satellite Research Group for Pediatric Dyslipidemia; Stefanutti, C. Current Approach to the Diagnosis and Treatment of Heterozygote and Homozygous FH Children and Adolescents. Curr. Atheroscler. Rep. 2021, 23, 1–14. [Google Scholar] [CrossRef]
- Ferrari, F.; Martins, V.M.; Rocha, V.Z.; Santos, R.D. Advances with lipid-lowering drugs for pediatric patients with familial hypercholesterolemia. Expert Opin. Pharmacother. 2021, 22, 483–495. [Google Scholar] [CrossRef]
- Pinal-Fernandez, I.; Casal-Dominguez, M.; Mammen, A.L. Statins: Pros and cons. Med. Clin. 2018, 150, 398–402. [Google Scholar] [CrossRef]
- Vuorio, A.; Kuoppala, J.; Kovanen, P.T.; Humphries, S.; Tonstad, S.; Wiegman, A.; Drogari, E.; Ramaswami, U. Statins for children with familial hypercholesterolemia. Cochrane Database Syst. Rev. 2019, 2019. [Google Scholar] [CrossRef]
- Kusters, D.M.; Avis, H.J.; De Groot, E.; Wijburg, F.A.; Kastelein, J.J.P.; Wiegman, A.; Hutten, B.A. Ten-Year Follow-Up after Initiation of Statin Therapy in Children with Familial Hypercholesterolemia. JAMA 2014, 312, 1055–1057. [Google Scholar] [CrossRef]
- Radaelli, G.; Sausen, G.; Cesa, C.C.; Santos, F.D.S.; Portal, V.L.; Neyeloff, J.; Pellanda, L.C. Statin Treatments And Dosages In Children With Familial Hypercholesterolemia: Meta-Analysis. Arq. Bras. Cardiol. 2018, 111, 810–821. [Google Scholar] [CrossRef] [PubMed]
- Anagnostis, P.; Vaitsi, K.; Kleitsioti, P.; Mantsiou, C.; Pavlogiannis, K.; Athyros, V.G.; Mikhailidis, D.P.; Goulis, D.G. Efficacy and safety of statin use in children and adolescents with familial hypercholesterolaemia: A systematic review and meta-analysis of randomized-controlled trials. Endocrine 2020, 69, 249–261. [Google Scholar] [CrossRef] [PubMed]
- Luirink, I.K.; Wiegman, A.; Kusters, D.M.; Hof, M.H.; Groothoff, J.W.; De Groot, E.; Kastelein, J.J.; Hutten, B.A. 20-Year Follow-up of Statins in Children with Familial Hypercholesterolemia. N. Engl. J. Med. 2019, 381, 1547–1556. [Google Scholar] [CrossRef] [PubMed]
- Grundy, S.M.; Stone, N.J.; Bailey, A.L.; Beam, C.; Birtcher, K.K.; Blumenthal, R.S.; Braun, L.T.; de Ferranti, S.; Faiella-Tommasino, J.; Forman, D.E.; et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J. Am. Coll. Cardiol. 2019, 73, 3168–3209, Erratum in 2019, 73, 3234–3237. [Google Scholar] [CrossRef]
- Mach, F.; Baigent, C.; Catapano, A.L.; Koskinas, K.C.; Casula, M.; Badimon, L.; Chapman, M.J.; De Backer, G.G.; Delgado, V.; Ference, B.A.; et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: Lipid modification to reduce cardio-vascular risk. Eur. Heart J. 2020, 41, 111–188, Erratum in 2020, 41, 4255. [Google Scholar] [CrossRef]
- Ramaswami, U.; Humphries, S.E.; Priestley-Barnham, L.; Green, P.; Wald, D.S.; Capps, N.; Anderson, M.; Dale, P.; Morris, A.A. Current management of children and young people with heterozygous familial hypercholesterolaemia—HEART UK statement of care. Atherosclerosis 2019, 290, 1–8. [Google Scholar] [CrossRef]
- Wiegman, A. Lipid Screening, Action, and Follow-up in Children and Adolescents. Curr. Cardiol. Rep. 2018, 20, 80. [Google Scholar] [CrossRef] [PubMed]
- Maliachova, O. Familial Hypercholesterolemia in Children and Adolescents: Diagnosis and Treatment. Curr. Pharm. Des. 2018, 24, 3672–3677. [Google Scholar] [CrossRef] [PubMed]
- Balla, S.; Ekpo, E.P.; Wilemon, K.A.; Knowles, J.W.; Rodriguez, F. Women Living with Familial Hypercholesterolemia: Challenges and Considerations Surrounding Their Care. Curr. Atheroscler. Rep. 2020, 22, 60. [Google Scholar] [CrossRef] [PubMed]
- Mendelson, M.M.; Regh, T.; Chan, J.; Baker, A.; Ryan, H.H.; Palumbo, N.; Johnson, P.K.; Griggs, S.; Boghani, M.; Desai, N.K.; et al. Correlates of Achieving Statin Therapy Goals in Children and Adolescents with Dyslipidemia. J. Pediatr. 2016, 178, 149–155.e9. [Google Scholar] [CrossRef] [Green Version]
- Tada, H.; Takamura, M.; Kawashiri, M.-A. Familial Hypercholesterolemia: A Narrative Review on Diagnosis and Management Strategies for Children and Adolescents. Vasc. Health Risk Manag. 2021, 17, 59–67. [Google Scholar] [CrossRef]
- Hammersley, D.; Signy, M. Ezetimibe: An update on its clinical usefulness in specific patient groups. Ther. Adv. Chronic Dis. 2017, 8, 4–11. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kusters, D.M.; Caceres, M.; Coll, M.; Cuffie, C.; Gagné, C.; Jacobson, M.S.; Kwiterovich, P.O.; Lee, R.; Lowe, R.S.; Massaad, R.; et al. Efficacy and Safety of Ezetimibe Monotherapy in Children with Heterozygous Familial or Nonfamilial Hypercholesterolemia. J. Pediatr. 2015, 166, 1377–1384.e3. [Google Scholar] [CrossRef]
- Van der Graaf, A.; Cuffie-Jackson, C.; Vissers, M.N.; Trip, M.D.; Gagné, C.; Shi, G.; Veltri, E.; Avis, H.J.; Kastelein, J.J. Efficacy and Safety of Coadministration of Ezetimibe and Simvastatin in Adolescents with Heterozygous Familial Hypercholesterolemia. J. Am. Coll. Cardiol. 2008, 52, 1421–1429. [Google Scholar] [CrossRef] [Green Version]
- Benekos, T.; Kosmeri, C.; Vlahos, A.; Milionis, H. Nine-year overview of dyslipidemia management in children with heterozygous familial hypercholesterolemia: A university hospital outpatient lipid clinic project in Northwestern Greece. J. Pediatr. Endocrinol. Metab. 2020, 33, 533–538. [Google Scholar] [CrossRef]
- Tonstad, S.; Knudtzon, J.; Sivertsen, M.; Refsum, H.; Ose, L. Efficacy and safety of cholestyramine therapy in peripubertal and prepubertal children with familial hypercholesterolemia. J. Pediatr. 1996, 129, 42–49. [Google Scholar] [CrossRef]
- Perry, C.M. Colesevelam: In pediatric patients with heterozygous familial hypercholesterolemia. Pediatr. Drugs 2010, 12, 133–140. [Google Scholar] [CrossRef] [PubMed]
- Colletti, R.B.; Neufeld, E.J.; Roff, N.K.; McAuliffe, T.L.; Baker, A.L.; Newburger, J.W. Niacin treatment of hypercholesterolemia in children. Pediatrics 1993, 92, 78–82. [Google Scholar] [PubMed]
- Stefanutti, C.; Julius, U.; Watts, G.; Harada-Shiba, M.; Cossu, M.; Schettler, V.J.; De Silvestro, G.; Soran, H.; Van Lennep, J.R.; Pisciotta, L.; et al. Toward an international consensus—Integrating lipoprotein apheresis and new lipid-lowering drugs. J. Clin. Lipidol. 2017, 11, 858–871.e3. [Google Scholar] [CrossRef] [PubMed]
- Stefanutti, C.; Julius, U. Lipoprotein apheresis: State of the art and novelties. Atheroscler. Suppl. 2013, 14, 19–27. [Google Scholar] [CrossRef]
- Cuchel, M.; Bruckert, E.; Ginsberg, H.N.; Raal, F.J.; Santos, R.D.; Hegele, R.A.; Kuivenhoven, J.A.; Nordestgaard, B.G.; Descamps, O.S.; Steinhagen-Thiessen, E.; et al. Homozygous familial hypercholesterolaemia: New insights and guidance for clinicians to improve detection and clinical management. A position paper from the Consensus Panel on Familial Hypercholesterolaemia of the European Atherosclerosis Society. Eur. Heart J. 2014, 35, 2146–2157. [Google Scholar] [CrossRef]
- Luirink, I.K.; Hutten, B.A.; Greber-Platzer, S.; Kolovou, G.D.; Dann, E.J.; De Ferranti, S.D.; Taylan, C.; Bruckert, E.; Saheb, S.; Oh, J.; et al. Practice of lipoprotein apheresis and short-term efficacy in children with homozygous familial hypercholesterolemia: Data from an international registry. Atherosclerosis 2020, 299, 24–31. [Google Scholar] [CrossRef] [PubMed]
- Santos, R.D.; Stein, E.A.; Hovingh, G.K.; Blom, D.J.; Soran, H.; Watts, G.F.; López, J.A.G.; Bray, S.; Kurtz, C.E.; Hamer, A.W.; et al. Long-Term Evolocumab in Patients With Familial Hypercholesterolemia. J. Am. Coll. Cardiol. 2020, 75, 565–574. [Google Scholar] [CrossRef]
- Hovingh, G.K.; Raal, F.J.; Dent, R.; Stefanutti, C.; Descamps, O.; Masana, L.; Lira, A.; Bridges, I.; Coll, B.; Sullivan, D. Long-term safety, tolerability, and efficacy of evolocumab in patients with heterozygous familial hypercholesterolemia. J. Clin. Lipidol. 2017, 11, 1448–1457. [Google Scholar] [CrossRef]
- Santos, R.D.; Ruzza, A.; Hovingh, G.K.; Wiegman, A.; Mach, F.; Kurtz, C.E.; Hamer, A.; Bridges, I.; Bartuli, A.; Bergeron, J.; et al. Evolocumab in Pediatric Heterozygous Familial Hypercholesterolemia. N. Engl. J. Med. 2020, 383, 1317–1327. [Google Scholar] [CrossRef]
- Blom, D.J.; Harada-Shiba, M.; Rubba, P.; Gaudet, D.; Kastelein, J.J.; Charng, M.-J.; Pordy, R.; Donahue, S.; Ali, S.; Dong, Y.; et al. Efficacy and Safety of Alirocumab in Adults With Homozygous Familial Hypercholesterolemia: The ODYSSEY HoFH Trial. J. Am. Coll. Cardiol. 2020, 76, 131–142. [Google Scholar] [CrossRef]
- Hartgers, M.L.; Defesche, J.C.; Langslet, G.; Hopkins, P.N.; Kastelein, J.J.; Baccara-Dinet, M.T.; Seiz, W.; Hamon, S.; Banerjee, P.; Stefanutti, C. Alirocumab efficacy in patients with double heterozygous, compound heterozygous, or homozygous familial hypercholesterolemia. J. Clin. Lipidol. 2018, 12, 390–396.e8. [Google Scholar] [CrossRef] [Green Version]
- Daniels, S.; Caprio, S.; Chaudhari, U.; Manvelian, G.; Baccara-Dinet, M.T.; Brunet, A.; Scemama, M.; Loizeau, V.; Bruckert, E. PCSK9 inhibition with alirocumab in pediatric patients with heterozygous familial hypercholesterolemia: The ODYSSEY KIDS study. J. Clin. Lipidol. 2020, 14, 322–330.e5. [Google Scholar] [CrossRef]
- Raal, F.J.; Kallend, D.; Ray, K.; Turner, T.; Koenig, W.; Wright, R.S.; Wijngaard, P.L.; Curcio, D.; Jaros, M.J.; Leiter, L.A.; et al. Inclisiran for the Treatment of Heterozygous Familial Hypercholesterolemia. N. Engl. J. Med. 2020, 382, 1520–1530. [Google Scholar] [CrossRef] [PubMed]
- Raal, F.J.; Rosenson, R.S.; Reeskamp, L.F.; Hovingh, G.K.; Kastelein, J.J.; Rubba, P.; Ali, S.; Banerjee, P.; Chan, K.-C.; Gipe, D.A.; et al. Evinacumab for Homozygous Familial Hypercholesterolemia. N. Engl. J. Med. 2020, 383, 711–720. [Google Scholar] [CrossRef] [PubMed]
- Blom, D.J.; Raal, F.J.; Santos, R.D.; Marais, A.D. Lomitapide and Mipomersen—Inhibiting Microsomal Triglyceride Transfer Protein (MTP) and apoB100 Synthesis. Curr. Atheroscler. Rep. 2019, 21, 48. [Google Scholar] [CrossRef] [PubMed]
- Raal, F.J.; Braamskamp, M.J.; Selvey, S.L.; Sensinger, C.H.; Kastelein, J.J. Pediatric experience with mipomersen as adjunctive therapy for homozygous familial hypercholesterolemia. J. Clin. Lipidol. 2016, 10, 860–869. [Google Scholar] [CrossRef] [Green Version]
- Stefanutti, C. Lomitapide–a Microsomal Triglyceride Transfer Protein Inhibitor for Homozygous Familial Hypercholesterolemia. Curr. Atheroscler. Rep. 2020, 22, 1–11, Erratum in 2020, 22, 41. [Google Scholar] [CrossRef]
- Ben-Omran, T.; Masana, L.; Kolovou, G.; Ariceta, G.; Nóvoa, F.J.; Lund, A.; Bogsrud, M.P.; Araujo, M.; Hussein, O.; Ibarretxe, D.; et al. Real-World Outcomes with Lomitapide Use in Paediatric Patients with Homozygous Familial Hypercholesterolaemia. Adv. Ther. 2019, 36, 1786–1811. [Google Scholar] [CrossRef] [Green Version]
- Chacra, A.P.M.; Ferrari, M.C.; Rocha, V.Z.; Santos, R.D. Case report: The efficacy and safety of lomitapide in a homozygous familial hypercholesterolemic child. J. Clin. Lipidol. 2019, 13, 397–401. [Google Scholar] [CrossRef]
- Goldberg, A.C.; Leiter, L.A.; Stroes, E.S.G.; Baum, S.; Hanselman, J.C.; Bloedon, L.T.; Lalwani, N.D.; Patel, P.M.; Zhao, X.; Duell, P.B. Effect of Bempedoic Acid vs Placebo Added to Maximally Tolerated Statins on Low-Density Lipoprotein Cholesterol in Patients at High Risk for Cardiovascular Disease: The CLEAR Wisdom Randomized Clinical Trial. JAMA 2019, 322, 1780–1788. [Google Scholar] [CrossRef]
- Ballantyne, C.M.; Laufs, U.; Ray, K.K.; Leiter, L.; Bays, H.; Goldberg, A.C.; Stroes, E.S.; MacDougall, D.; Zhao, X.; Catapano, A.L. Bempedoic acid plus ezetimibe fixed-dose combination in patients with hypercholesterolemia and high CVD risk treated with maximally tolerated statin therapy. Eur. J. Prev. Cardiol. 2020, 27, 593–603. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Filippatos, T.D.; Kei, A.; Elisaf, M.S. Anacetrapib, a New CETP Inhibitor: The New Tool for the Management of Dyslipidemias? Diseases 2017, 5, 21. [Google Scholar] [CrossRef] [PubMed]
- Armitage, J.; Holmes, M.V.; Preiss, D. Cholesteryl Ester Transfer Protein Inhibition for Preventing Cardiovascular Events: JACC Review Topic of the Week. J. Am. Coll. Cardiol. 2019, 73, 477–487. [Google Scholar] [CrossRef] [PubMed]
- Ito, M.K.; Santos, R.D. PCSK9 Inhibition With Monoclonal Antibodies: Modern Management of Hypercholesterolemia. J. Clin. Pharmacol. 2017, 57, 7–32. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Defesche, J.C.; Stefanutti, C.; Langslet, G.; Hopkins, P.N.; Seiz, W.; Baccara-Dinet, M.T.; Hamon, S.C.; Banerjee, P.; Kastelein, J.J. Efficacy of alirocumab in 1191 patients with a wide spectrum of mutations in genes causative for familial hypercholesterolemia. J. Clin. Lipidol. 2017, 11, 1338–1346.e7, Erratum in 2020, 14, 742. [Google Scholar] [CrossRef] [Green Version]
- Achimastos, A.; Alexandrides, T.; Alexopoulos, D.; Athyros, V.; Bargiota, A.; Bilianou, E.; Chrysochoou, C.; Drogari, E.; Elisaf, M.; Ganotakis, E.; et al. Expert consensus on the rational clinical use of proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors. Hormones 2016, 15, 8–14. [Google Scholar] [CrossRef]
- Stitziel, N.O.; Khera, A.V.; Wang, X.; Bierhals, A.J.; Vourakis, A.C.; Sperry, A.E.; Natarajan, P.; Klarin, D.; Emdin, C.A.; Zekavat, S.M.; et al. ANGPTL3 Deficiency and Protection Against Coronary Artery Disease. J. Am. Coll. Cardiol. 2017, 69, 2054–2063. [Google Scholar] [CrossRef]
- Markham, A. Bempedoic Acid: First Approval. Drugs 2020, 80, 747–753. [Google Scholar] [CrossRef]
- Nicholls, S.J.; Bubb, K. The mystery of evacetrapib—Why are CETP inhibitors failing? Expert Rev. Cardiovasc. Ther. 2020, 18, 127–130. [Google Scholar] [CrossRef]
| ACCEPTABLE | BORDERLINE | HIGH | |||||
|---|---|---|---|---|---|---|---|
| mg/dL | Percentile | mg/dL | Percentile | mg/dL | Percentile | ||
| Children and Adolescents | TC | <170 | <75th | 170–199 | 75–95th | >200 | >95th |
| LDL-C | <110 | <75th | 110–129 | 75–95th | >130 | >95th | |
| TG | |||||||
| 0–9 years | <75 | <75th | 75–99 | 75–95th | >100 | >95th | |
| 10–19 years | <90 | <75th | 90–129 | 75–95th | >130 | >95th | |
| HDL-C | >45 | >10th | 40–45 | <40 | <10th | ||
| Non-HDL-C | <120 | <75th | 120–144 | 75–95th | >145 | >95th | |
| Mechanism of Action | Mean LDL-C % Reduction | Currently Approval Status | Trials in Children | Studies | |
|---|---|---|---|---|---|
| Evolocumab | PCSK9 inhibitor | 20–55% | FH from 12 years of age | HoFH or severe HeFH from 12 years of age | Santos et al. [79] Hovingh et al. [80] Santos et al. [81] |
| Alirocumab | PCSK9 inhibitor | 21–62% | FH in adults | Severe HeFH from 8 years of age | Blom et al. [82] Hartgers et al. [83] Daniels et al. [84] |
| Inclisiran | Small interfering RNA directed against PCSK9 | 35–43% | Primary hypercholesterolemia or mixed dyslipidaemia in adults | Will be tested in paediatric HeFH in the ORION-16 study. | Raal et al. [85] |
| Evinacumab | ANGPTL3 inhibitor | 42–51% | HoFH from 12 years of age | HoFH from 12 years old | Raal et al. [86] |
| Mipomersen | Antisense APO-B synthesis inhibitor | 28% | FH from 12 years of age | HoFH and severe HeFH from 12 years of age | Blom et al. [87] Raal et al. [88] |
| Lomitapide | MTTP inhibitor | 51% | FH in adults | HoFH from 7 years of age | Stefanutti [89] Ben-Omran et al. [90] Chacra et al. [91] |
| Bempedoic acid | ACL inhibitor | 17–38% | Primary hypercholesterolemia or mixed dyslipidaemia in adults | Goldberg et al. [92] Ballantyne et al. [93] | |
| Anacetrapib | CEPT inhibitor | 40% | Not approved | Filippatos et al. [94] Armitage et al. [95] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fiorentino, R.; Chiarelli, F. Treatment of Dyslipidaemia in Children. Biomedicines 2021, 9, 1078. https://doi.org/10.3390/biomedicines9091078
Fiorentino R, Chiarelli F. Treatment of Dyslipidaemia in Children. Biomedicines. 2021; 9(9):1078. https://doi.org/10.3390/biomedicines9091078
Chicago/Turabian StyleFiorentino, Riccardo, and Francesco Chiarelli. 2021. "Treatment of Dyslipidaemia in Children" Biomedicines 9, no. 9: 1078. https://doi.org/10.3390/biomedicines9091078







