Effective Detection and Monitoring of Glioma Using [18F]FPIA PET Imaging
Abstract
:1. Introduction
2. Materials and Methods
2.1. Radiotracer Synthesis
2.2. Cell Culture
2.3. Tumor Models
2.4. Imaging
2.5. [18F]FPIA Biodistribution
2.6. Effect of Etomoxir on [18F]FPIA Tumor Uptake
2.7. Immunohistochemistry
2.8. Statistical Analyses
3. Results
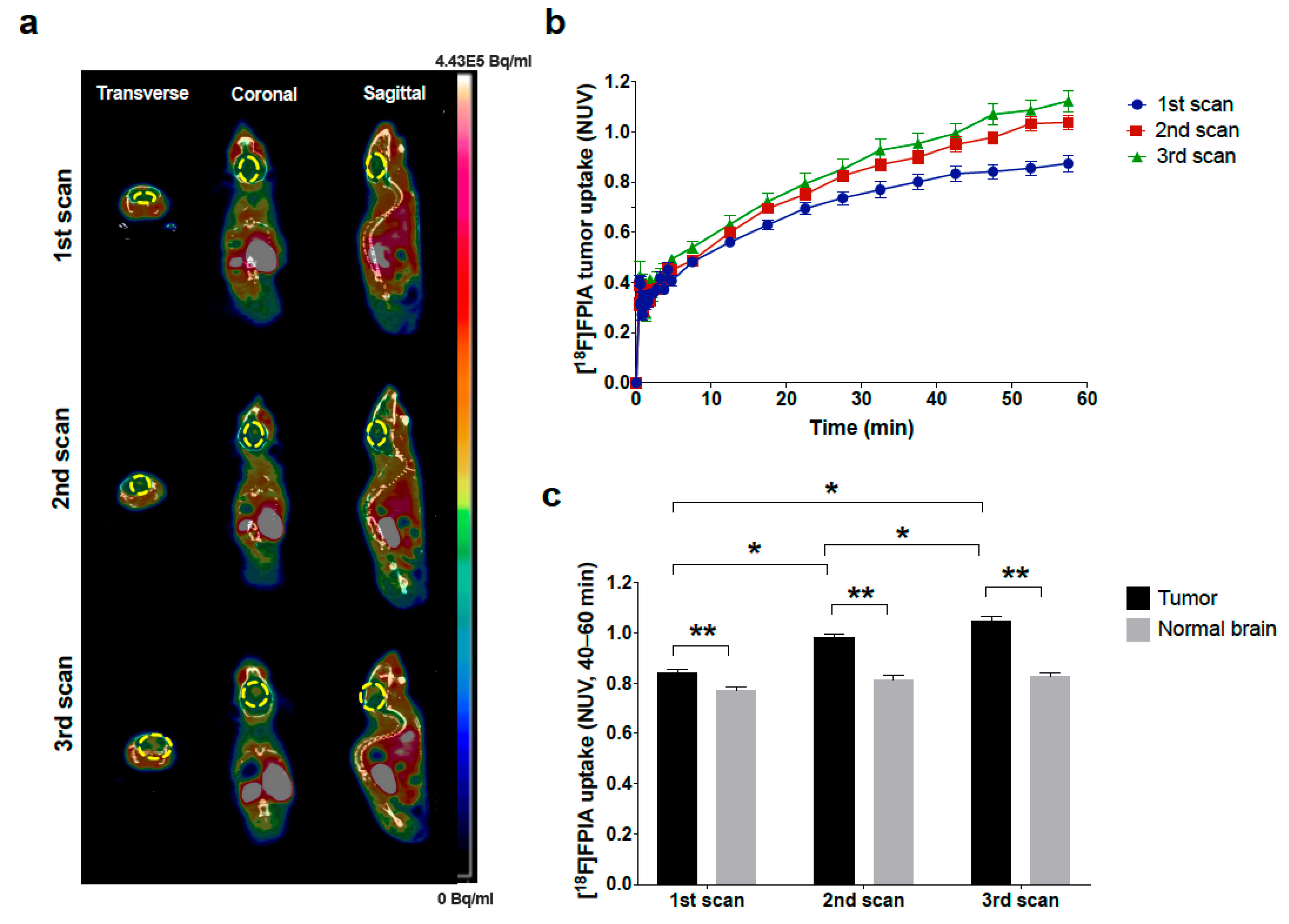
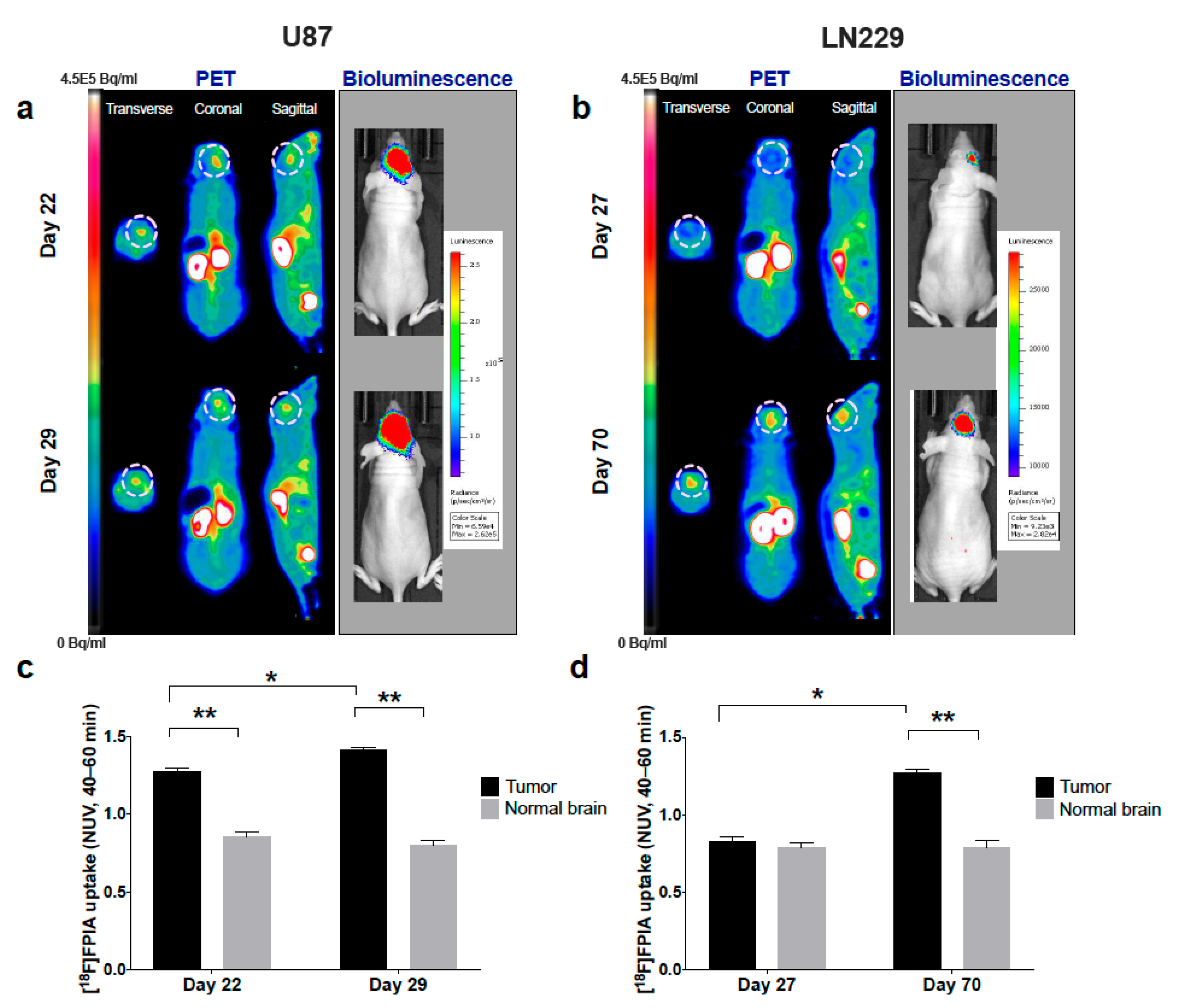
3.1. [18F]FPIA Uptake Reflected Orthotopic Glioma Growth
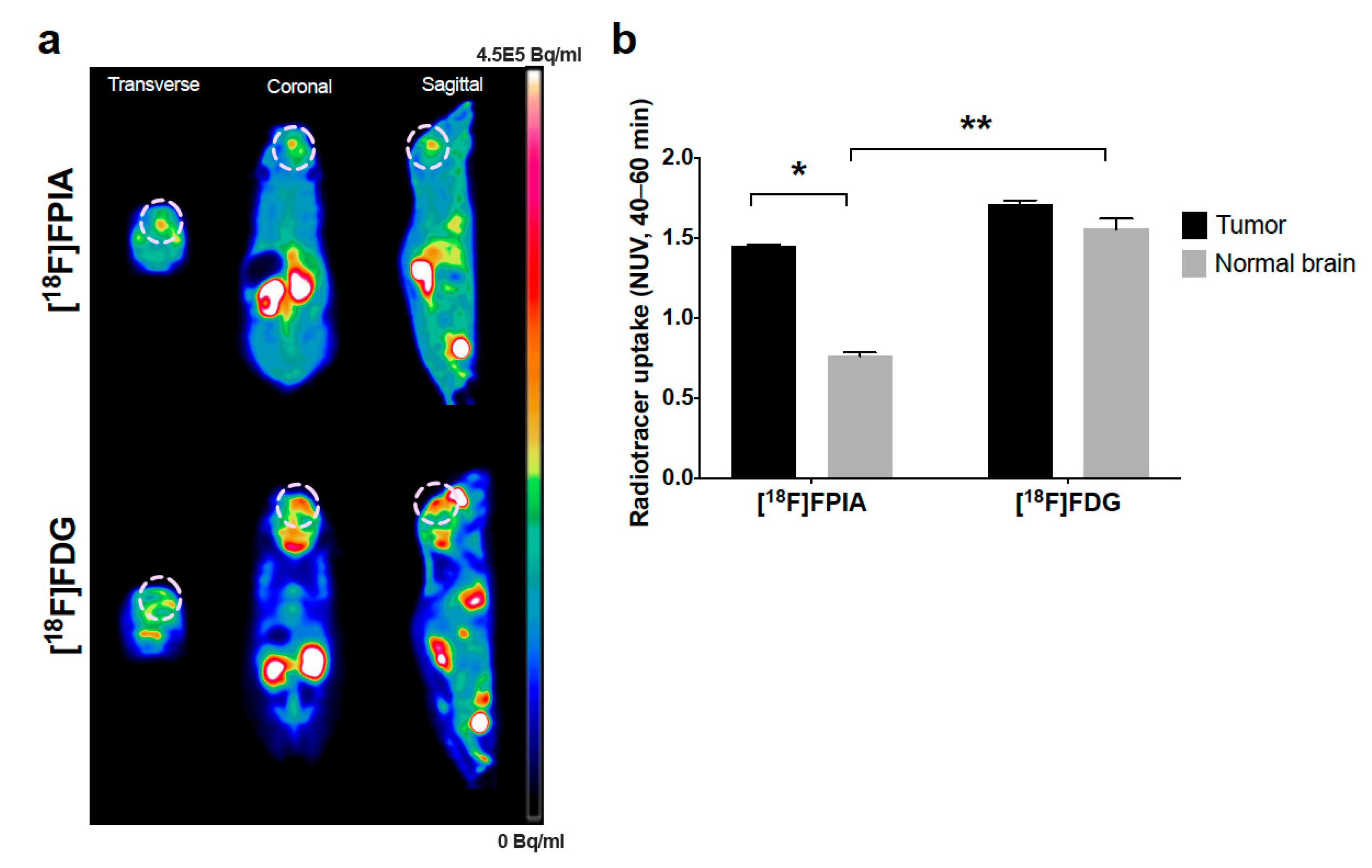
3.2. PET Imaging Showed Higher Tumor-to-Normal Brain Uptake of [18F]FPIA Compared with [18F]FDG
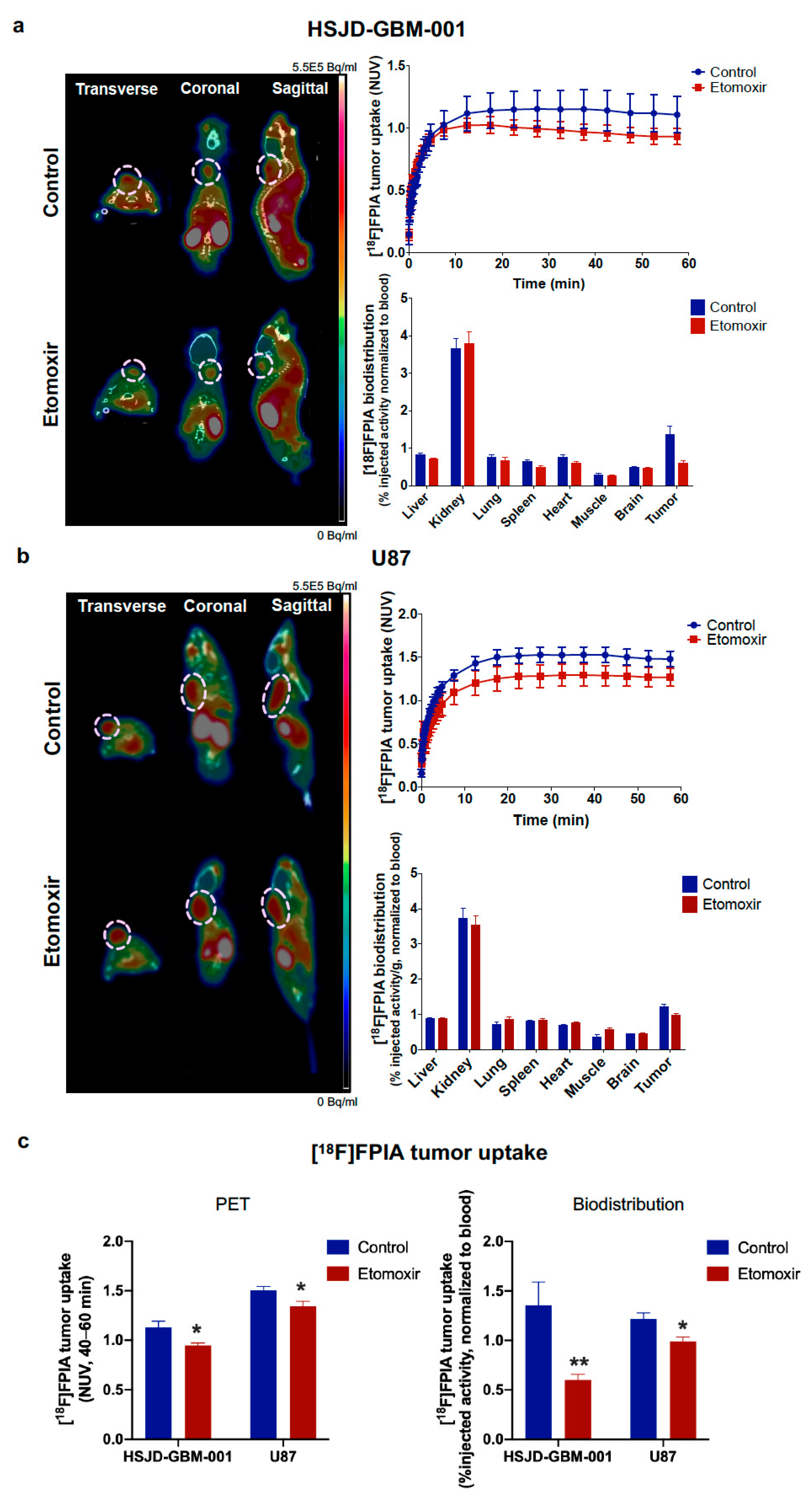
3.3. Effect of Etomoxir on [18F]FPIA Tumor Uptake
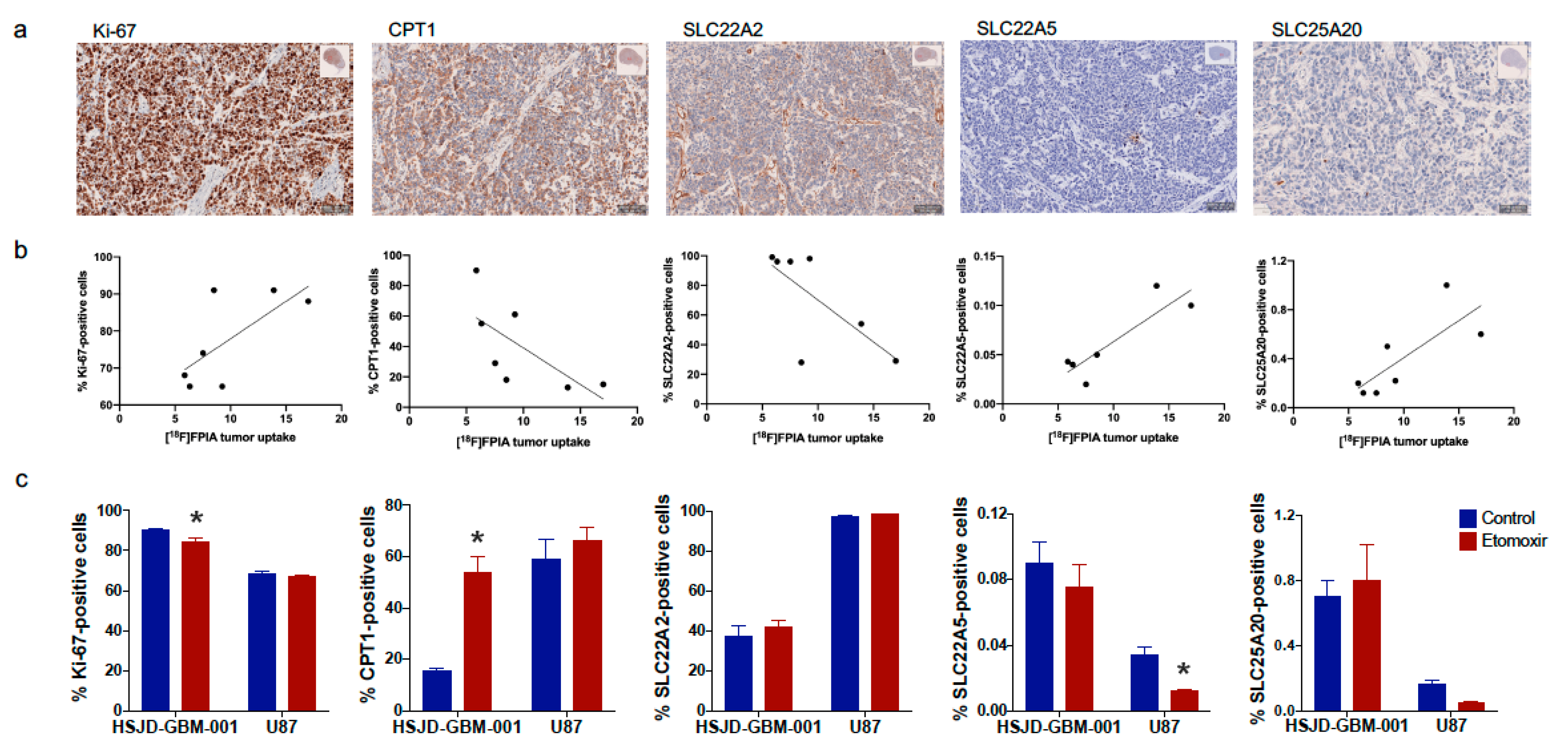
3.4. [18F]FPIA Uptake Correlated with Tumor Proliferation and Expression of Lipid Metabolism-Associated Proteins
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dolecek, T.A.; Propp, J.M.; Stroup, N.E.; Kruchko, C. CBTRUS statistical report: Primary brain and central nervous system tumors diagnosed in the United States in 2005-2009. Neuro-Oncology 2012, 14 (Suppl. 5), v1–v49. [Google Scholar] [CrossRef] [PubMed]
- Omuro, A.; De Angelis, L.M. Glioblastoma and Other Malignant Gliomas: A Clinical ReviewGlioblastoma and Other Malignant GliomasGlioblastoma and Other Malignant Gliomas. JAMA 2013, 310, 1842–1850. [Google Scholar] [CrossRef] [PubMed]
- Ostrom, Q.T.; Gittleman, H.; Barnholtz-Sloan, J.S.; Wolinsky, Y.; Kruchko, C.; Xu, J.; Kromer, C. CBTRUS Statistical Report: Primary Brain and Other Central Nervous System Tumors Diagnosed in the United States in 2009–2013. Neuro. Oncol. 2016, 18, v1–v75. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jansen, N.L.; Graute, V.; Armbruster, L.; Suchorska, B.; Lutz, J.; Eigenbrod, S.; Cumming, P.; Bartenstein, P.; Tonn, J.-C.; Kreth, F.W.; et al. MRI-suspected low-grade glioma: Is there a need to perform dynamic FET PET? Eur. J. Nucl. Med. Mol. Imaging 2012, 39, 1021–1029. [Google Scholar] [CrossRef]
- Hygino da Cruz, L.C.; Rodriguez, I.; Domingues, R.C.; Gasparetto, E.L.; Sorensen, A.G. Pseudoprogression and Pseudoresponse: Imaging Challenges in the Assessment of Posttreatment Glioma. Am. J. Neuroradiol. 2011, 32, 1978. [Google Scholar] [CrossRef] [Green Version]
- Booth, T.C.; Larkin, T.J.; Yuan, Y.; Kettunen, M.I.; Dawson, S.N.; Scoffings, D.; Canuto, H.C.; Vowler, S.L.; Kirschenlohr, H.; Hobson, M.P.; et al. Analysis of heterogeneity in T2-weighted MR images can differentiate pseudoprogression from progression in glioblastoma. PLoS ONE 2017, 12, e0176528. [Google Scholar] [CrossRef] [PubMed]
- Clark, P.M.; Mai, W.X.; Cloughesy, T.F.; Nathanson, D.A. Emerging Approaches for Targeting Metabolic Vulnerabilities in Malignant Glioma. Curr. Neurol. Neurosci. Rep. 2016, 16, 17. [Google Scholar] [CrossRef]
- Lin, H.; Patel, S.; Affleck, V.S.; Wilson, I.; Turnbull, D.M.; Joshi, A.R.; Maxwell, R.; Stoll, E.A. Fatty acid oxidation is required for the respiration and proliferation of malignant glioma cells. Neuro. Oncol. 2017, 19, 43–54. [Google Scholar] [CrossRef] [Green Version]
- Pike, L.S.; Smift, A.L.; Croteau, N.J.; Ferrick, D.A.; Wu, M. Inhibition of fatty acid oxidation by etomoxir impairs NADPH production and increases reactive oxygen species resulting in ATP depletion and cell death in human glioblastoma cells. Biochim. Biophys. Acta (BBA) Bioenerg. 2011, 1807, 726–734. [Google Scholar] [CrossRef] [Green Version]
- Kambach, D.M.; Halim, A.S.; Cauer, A.G.; Sun, Q.; Tristan, C.A.; Celiku, O.; Kesarwala, A.H.; Shankavaram, U.; Batchelor, E.; Stommel, J.M. Disabled cell density sensing leads to dysregulated cholesterol synthesis in glioblastoma. Oncotarget 2017, 8, 14860–14875. [Google Scholar] [CrossRef]
- Mullen, P.J.; Yu, R.; Longo, J.; Archer, M.C.; Penn, L.Z. The interplay between cell signalling and the mevalonate pathway in cancer. Nat. Rev. Cancer 2016, 16, 718. [Google Scholar] [CrossRef]
- Mashimo, T.; Pichumani, K.; Vemireddy, V.; Hatanpaa, K.J.; Singh, D.K.; Sirasanagandla, S.; Nannepaga, S.; Piccirillo, S.G.; Kovacs, Z.; Foong, C.; et al. Acetate is a bioenergetic substrate for human glioblastoma and brain metastases. Cell 2014, 159, 1603–1614. [Google Scholar] [CrossRef] [Green Version]
- Maher, E.A.; Marin-Valencia, I.; Bachoo, R.M.; Mashimo, T.; Raisanen, J.; Hatanpaa, K.J.; Jindal, A.; Jeffrey, F.M.; Choi, C.; Madden, C.; et al. Metabolism of [U-13 C]glucose in human brain tumors in vivo. NMR Biomed. 2012, 25, 1234–1244. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yoshii, Y.; Furukawa, T.; Saga, T.; Fujibayashi, Y. Acetate/acetyl-CoA metabolism associated with cancer fatty acid synthesis: Overview and application. Cancer Lett. 2015, 356, 211–216. [Google Scholar] [CrossRef] [PubMed]
- Schug, Z.T.; Vande Voorde, J.; Gottlieb, E. The metabolic fate of acetate in cancer. Nat. Rev. Cancer 2016, 16, 708. [Google Scholar] [CrossRef] [PubMed]
- Vāvere, A.L.; Kridel, S.J.; Wheeler, F.B.; Lewis, J.S. 1-11C-Acetate as a PET Radiopharmaceutical for Imaging Fatty Acid Synthase Expression in Prostate Cancer. J. Nucl. Med. 2008, 49, 327. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pisaneschi, F.; Witney, T.H.; Iddon, L.; Aboagye, E.O. Synthesis of [18F]fluoro-pivalic acid: An improved PET imaging probe for the fatty acid synthesis pathway in tumours. MedChemComm 2013, 4, 1350–1353. [Google Scholar] [CrossRef]
- Witney, T.H.; Pisaneschi, F.; Alam, I.S.; Trousil, S.; Kaliszczak, M.; Twyman, F.; Brickute, D.; Nguyen, Q.-D.; Schug, Z.; Gottlieb, E.; et al. Preclinical Evaluation of 3-18F-Fluoro-2,2-Dimethylpropionic Acid as an Imaging Agent for Tumor Detection. J. Nucl. Med. 2014, 55, 1506–1512. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brass, E.P. Pivalate-generating prodrugs and carnitine homeostasis in man. Pharm. Rev. 2002, 54, 589–598. [Google Scholar] [CrossRef]
- Melegh, B.; Kerner, J.; Bieber, L.L. Pivampicillin-promoted excretion of pivaloylcarnitine in humans. Biochem. Pharmacol. 1987, 36, 3405–3409. [Google Scholar] [CrossRef]
- Workman, P.; Aboagye, E.O.; Balkwill, F.; Balmain, A.; Bruder, G.; Chaplin, D.J.; Double, J.A.; Everitt, J.; Farningham, D.A.; Glennie, M.J.; et al. Guidelines for the welfare and use of animals in cancer research. Br. J. Cancer 2010, 102, 1555–1577. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vassileva, V.; Moriyama, E.H.; De Souza, R.; Grant, J.; Allen, C.J.; Wilson, B.C.; Piquette-Miller, M. Efficacy assessment of sustained intraperitoneal paclitaxel therapy in a murine model of ovarian cancer using bioluminescent imaging. Br. J. Cancer 2008, 99, 2037–2043. [Google Scholar] [CrossRef] [PubMed]
- Vassileva, V.; Rajkumar, V.; Mazzantini, M.; Robson, M.; Badar, A.; Sharma, S.; Årstad, E.; Hochhauser, D.; Lythgoe, M.F.; Kinghorn, J.; et al. Significant Therapeutic Efficacy with Combined Radioimmunotherapy and Cetuximab in Preclinical Models of Colorectal Cancer. J. Nucl. Med. 2015, 56, 1239–1245. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yao, C.-H.; Liu, G.-Y.; Wang, R.; Moon, S.H.; Gross, R.W.; Patti, G.J. Identifying off-target effects of etomoxir reveals that carnitine palmitoyltransferase I is essential for cancer cell proliferation independent of β-oxidation. PLoS Biol. 2018, 16, e2003782. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schlaepfer, I.R.; Glodé, L.M.; Hitz, C.A.; Pac, C.T.; Boyle, K.E.; Maroni, P.; Deep, G.; Agarwal, R.; Lucia, S.M.; Cramer, S.D.; et al. Inhibition of Lipid Oxidation Increases Glucose Metabolism and Enhances 2-Deoxy-2-[(18)F]Fluoro-D-Glucose Uptake in Prostate Cancer Mouse Xenografts. Mol. Imaging Biol. 2015, 17, 529–538. [Google Scholar] [CrossRef] [Green Version]
- Bankhead, P.; Loughrey, M.B.; Fernández, J.A.; Dombrowski, Y.; McArt, D.G.; Dunne, P.D.; McQuaid, S.; Gray, R.T.; Murray, L.J.; Coleman, H.G.; et al. QuPath: Open source software for digital pathology image analysis. Sci. Rep. 2017, 7, 16878. [Google Scholar] [CrossRef] [Green Version]
- Belohlávek, O.; Klener, J.; Vymazal, J.; Dbalý, V.; Tovarys, F. The diagnostics of recurrent gliomas using FDG-PET: Still questionable? Nucl. Med. Rev. Cent. East. Eur. 2002, 5, 127–130. [Google Scholar]
- Ohnishi, S.; Okamura, N.; Sakamoto, S.; Hasegawa, H.; Norikura, R.; Kanaoka, E.; Takahashi, K.; Horie, K.; Sakamoto, K.; Baba, T. Role of Na+/L-carnitine Transporter (OCTN2) in Renal Handling of Pivaloylcarnitine and Valproylcarnitine Formed during Pivalic Acid-containing Prodrugs and Valproic Acid Treatment. Drug Metab. Pharmacokinet. 2008, 23, 293–303. [Google Scholar] [CrossRef] [Green Version]
- Todesco, L.; Bodmer, M.; Vonwil, K.; Häussinger, D.; Krähenbühl, S. Interaction between pivaloylcarnitine and l-carnitine transport into L6 cells overexpressing hOCTN2. Chem. Biol. Interact. 2009, 180, 472–477. [Google Scholar] [CrossRef] [PubMed]
- Wright, S.H. Molecular and cellular physiology of organic cation transporter 2. Am. J. Physiol. Ren. Physiol. 2019, 317, F1669–F1679. [Google Scholar] [CrossRef] [PubMed]
- Juraszek, B.; Czarnecka-Herok, J.; Nałęcz, K.A. Glioma cells survival depends both on fatty acid oxidation and on functional carnitine transport by SLC22A5. J. Neurochem. 2020. [Google Scholar] [CrossRef]
- Fink, M.A.; Paland, H.; Herzog, S.; Grube, M.; Vogelgesang, S.; Weitmann, K.; Bialke, A.; Hoffmann, W.; Rauch, B.H.; Schroeder, H.W.S.; et al. L-Carnitine-Mediated Tumor Cell Protection and Poor Patient Survival Associated with OCTN2 Overexpression in Glioblastoma Multiforme. Clin. Cancer Res. 2019, 25, 2874–2886. [Google Scholar] [CrossRef]
- Nigam, S.K. The SLC22 Transporter Family: A Paradigm for the Impact of Drug Transporters on Metabolic Pathways, Signaling, and Disease. Annu. Rev. Pharm. Toxicol. 2018, 58, 663–687. [Google Scholar] [CrossRef] [PubMed]
- Schlaepfer, I.R.; Joshi, M. CPT1A-mediated Fat Oxidation, Mechanisms, and Therapeutic Potential. Endocrinology 2020, 161. [Google Scholar] [CrossRef] [PubMed]
- Floeth, F.W.; Pauleit, D.; Sabel, M.; Reifenberger, G.; Stoffels, G.; Stummer, W.; Rommel, F.; Hamacher, K.; Langen, K.J. 18F-FET PET differentiation of ring-enhancing brain lesions. J. Nucl. Med. 2006, 47, 776–782. [Google Scholar] [PubMed]
- Hutterer, M.; Nowosielski, M.; Putzer, D.; Jansen, N.L.; Seiz, M.; Schocke, M.; McCoy, M.; Göbel, G.; la Fougère, C.; Virgolini, I.J.; et al. [18F]-fluoro-ethyl-L-tyrosine PET: A valuable diagnostic tool in neuro-oncology, but not all that glitters is glioma. Neuro. Oncol. 2013, 15, 341–351. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dubash, S.R.; Keat, N.; Kozlowski, K.; Barnes, C.; Allott, L.; Brickute, D.; Hill, S.; Huiban, M.; Barwick, T.D.; Kenny, L.; et al. Clinical translation of (18)F-fluoropivalate—A PET tracer for imaging short-chain fatty acid metabolism: Safety, biodistribution, and dosimetry in fed and fasted healthy volunteers. Eur. J. Nucl. Med. Mol. Imaging 2020, 47, 2549–2561. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Marker 1 | Correlation 2 | R2; p-Value 3 |
|---|---|---|
| Ki-67 | + | 0.5; <0.01 |
| CPT1 | - | 0.5; <0.01 |
| SLC22A2 | - | 0.5; 0.005 |
| SLC22A5 | + | 0.8; <0.001 |
| SLC25A20 | + | 0.6; 0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vassileva, V.; Braga, M.; Barnes, C.; Przystal, J.; Ashek, A.; Allott, L.; Brickute, D.; Abrahams, J.; Suwan, K.; Carcaboso, A.M.; et al. Effective Detection and Monitoring of Glioma Using [18F]FPIA PET Imaging. Biomedicines 2021, 9, 811. https://doi.org/10.3390/biomedicines9070811
Vassileva V, Braga M, Barnes C, Przystal J, Ashek A, Allott L, Brickute D, Abrahams J, Suwan K, Carcaboso AM, et al. Effective Detection and Monitoring of Glioma Using [18F]FPIA PET Imaging. Biomedicines. 2021; 9(7):811. https://doi.org/10.3390/biomedicines9070811
Chicago/Turabian StyleVassileva, Vessela, Marta Braga, Chris Barnes, Justyna Przystal, Ali Ashek, Louis Allott, Diana Brickute, Joel Abrahams, Keittisak Suwan, Angel M. Carcaboso, and et al. 2021. "Effective Detection and Monitoring of Glioma Using [18F]FPIA PET Imaging" Biomedicines 9, no. 7: 811. https://doi.org/10.3390/biomedicines9070811
APA StyleVassileva, V., Braga, M., Barnes, C., Przystal, J., Ashek, A., Allott, L., Brickute, D., Abrahams, J., Suwan, K., Carcaboso, A. M., Hajitou, A., & Aboagye, E. O. (2021). Effective Detection and Monitoring of Glioma Using [18F]FPIA PET Imaging. Biomedicines, 9(7), 811. https://doi.org/10.3390/biomedicines9070811








