Mechanistic Insights and Potential Therapeutic Approaches in PolyQ Diseases via Autophagy
Abstract
1. Introduction
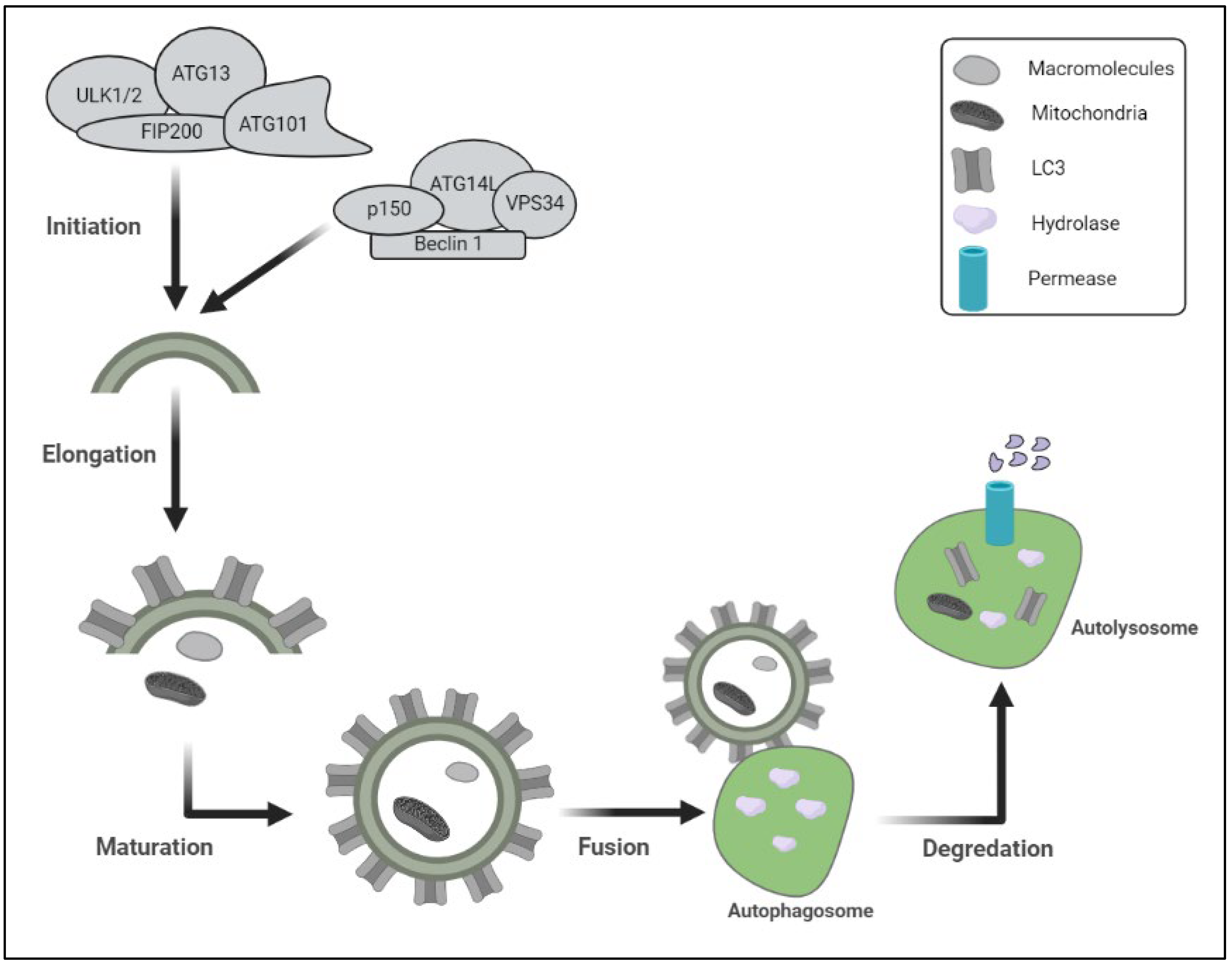
2. Mechanism of Autophagy
3. PolyQ Diseases, Their Pathophysiology, and Therapeutics
4. Autophagy Dysfunction in Polyglutamine Disease
4.1. Huntington’s Disease
4.2. Spinal and Bulbar Muscular Atrophy
4.3. Spinocerebellar Ataxia Type 1
4.4. Spinocerebellar Ataxia Type 2
4.5. Spinocerebellar Ataxia Type 3
4.6. Spinocerebellar Ataxia Type 7
4.7. Spinocerebellar Ataxia Type 17
4.8. Dentatorubral Pallidoluysian Atrophy (DRPLA)
5. Intracellular Quality Control of Disordered Proteins by Autophagy
6. Autophagy Modulators as Therapeutics against polyQ Diseases
7. Discussion
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lu, X.; Zhang, J.; Ding, Y.; Wu, J.; Chen, G. Novel Therapeutic Strategies for Ischemic Stroke: Recent Insights into Autophagy. Oxid. Med. Cell. Longev. 2022, 2022, 3450207. [Google Scholar] [CrossRef] [PubMed]
- De Duve, C.; Wattiaux, R. Functions of lysosomes. Annu. Rev. Physiol. 1966, 28, 435–492. [Google Scholar] [CrossRef] [PubMed]
- Klionsky, D.J.; Emr, S.D. Autophagy as a regulated pathway of cellular degradation. Science 2000, 290, 1717–1721. [Google Scholar] [CrossRef] [PubMed]
- Yang, Z.; Klionsky, D.J. An overview of the molecular mechanism of autophagy. Curr. Top. Microbiol. Immunol. 2009, 335, 1–32. [Google Scholar] [PubMed]
- Deter, R.L.; Baudhuin, P.; de Duve, C. Participation of lysosomes in cellular autophagy induced in rat liver by glucagon. J. Cell Biol. 1967, 35, C11. [Google Scholar] [CrossRef]
- Mizushima, N.; Ohsumi, Y.; Yoshimori, T. Autophagosome formation in mammalian cells. Cell Struct. Funct. 2002, 27, 421–429. [Google Scholar] [CrossRef]
- Meijer, A.J.; Codogno, P. Regulation and role of autophagy in mammalian cells. Int. J. Biochem. Cell Biol. 2004, 36, 2445–2462. [Google Scholar] [CrossRef]
- Di Malta, C.; Cinque, L.; Settembre, C. Transcriptional regulation of autophagy: Mechanisms and diseases. Front. Cell Dev. Biol. 2019, 7, 114. [Google Scholar] [CrossRef]
- Sun, K.; Deng, W.; Zhang, S.; Cai, N.; Jiao, S.; Song, J.; Wei, L. Paradoxical roles of autophagy in different stages of tumorigenesis: Protector for normal or cancer cells. Cell Biosci. 2013, 3, 35. [Google Scholar] [CrossRef]
- Vidal, R.L.; Matus, S.; Bargsted, L.; Hetz, C. Targeting autophagy in neurodegenerative diseases. Trends Pharmacol. Sci. 2014, 35, 583–591. [Google Scholar] [CrossRef]
- Yang, Y.; Klionsky, D.J. Autophagy and disease: Unanswered questions. Cell Death Differ. 2020, 27, 858–871. [Google Scholar] [CrossRef] [PubMed]
- Nah, J.; Yuan, J.; Jung, Y.K. Autophagy in neurodegenerative diseases: From mechanism to therapeutic approach. Mol. Cells 2015, 38, 381. [Google Scholar] [CrossRef] [PubMed]
- Wong, E.; Cuervo, A.M. Integration of clearance mechanisms: The proteasome and autophagy. Cold Spring Harb. Perspect. Biol. 2010, 2, a006734. [Google Scholar] [CrossRef]
- Ravikumar, B.; Duden, R.; Rubinsztein, D.C. Aggregate-prone proteins with polyglutamine and polyalanine expansions are degraded by autophagy. Hum. Mol. Genet. 2002, 11, 1107–1117. [Google Scholar] [CrossRef]
- Ravikumar, B.; Vacher, C.; Berger, Z.; Davies, J.E.; Luo, S.; Oroz, L.G.; Rubinsztein, D.C. Inhibition of mTOR induces autophagy and reduces toxicity of polyglutamine expansions in fly and mouse models of Huntington disease. Nat. Genet. 2004, 36, 585. [Google Scholar] [CrossRef]
- Cuervo, A.M. Chaperone-mediated autophagy: Selectivity pays off. Trends Endocrinol. Metab. 2010, 21, 142–150. [Google Scholar] [CrossRef] [PubMed]
- Pereira, M.L.; Mendonça, R.D.; Zanoteli, E. Intragenic variants in the SMN1 gene determine the clinical phenotype in 5q spinal muscular atrophy. Neurol. Genet. 2020, 6, e505. [Google Scholar]
- Panda, S.P.; Agrawal, M. The interplay of epilepsy with impaired mitophagy and autophagy linked dementia (MAD): A review of therapeutic approaches. Mitochondrion 2022, 66, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Michalik, A.; Van Broeckhoven, C. Pathogenesis of polyglutamine disorders: Aggregation revisited. Hum. Mol. Genet. 2003, 12 (Suppl. S2), R173–R186. [Google Scholar] [CrossRef] [PubMed]
- Yamin, G.; Ono, K.; Inayathullah, M.; Teplow, D.B. Amyloid β-protein assembly as a therapeutic target of Alzheimer’s disease. Curr. Pharm. Des. 2008, 14, 3231–3246. [Google Scholar] [CrossRef]
- Workman, R.J. Structure and Thermodynamics of Polyglutamine Peptides and Amyloid Fibrils via Metadynamics and Molecular Dynamics Simulations. Ph.D. Dissertation, Duquesne University, Pittsburgh, PA, USA, 2018. [Google Scholar]
- Baud, A.; Derbis, M.; Tutak, K.; Sobczak, K. Partners in crime: Proteins implicated in RNA repeat expansion diseases. Wiley Interdiscip. Rev. RNA 2002, 13, e1709. [Google Scholar] [CrossRef] [PubMed]
- Cortes, C.J.; La Spada, A.R. Autophagy in polyglutamine disease: Imposing order on disorder or contributing to the chaos? Mol. Cell. Neurosci. 2015, 66, 53–61. [Google Scholar] [CrossRef] [PubMed]
- Shibata, M.; Lu, T.; Furuya, T.; Degterev, A.; Mizushima, N.; Yoshimori, T.; Yuan, J. Regulation of intracellular accumulation of mutant Huntingtin by Beclin 1. J. Biol. Chem. 2006, 281, 14474–14485. [Google Scholar] [CrossRef] [PubMed]
- Rubinsztein, D.C. Lessons from animal models of Huntington’s disease. Trends Genet. 2002, 18, 202–209. [Google Scholar] [CrossRef]
- Cortes, C.J.; La Spada, A.R. The many faces of autophagy dysfunction in Huntington’s disease: From mechanism to therapy. Drug Discov. Today 2014, 19, 963–971. [Google Scholar] [CrossRef]
- Choi, A.M.; Ryter, S.W.; Levine, B. Autophagy in human health and disease. N. Engl. J. Med. 2013, 368, 651–662. [Google Scholar] [CrossRef]
- Lee, J.A. Autophagy in neurodegeneration: Two sides of the same coin. BMB Rep. 2009, 42, 324–330. [Google Scholar] [CrossRef]
- Huang, J.; Klionsky, D.J. Autophagy and human disease. Cell Cycle 2007, 6, 1837–1849. [Google Scholar] [CrossRef]
- Gutiérrez Ángel, S. Mutant Huntingtin Toxicity Modifiers Revealed by a Spatiotemporal Proteomic Profiling. Ph.D. Dissertation, Ludwig Maximilian University of Munich, München, Germany, 2019. [Google Scholar]
- Wang, Y.; Lin, F.; Qin, Z.H. The role of post-translational modifications of huntingtin in the pathogenesis of Huntington’s disease. Neurosci. Bull. 2010, 26, 153–162. [Google Scholar] [CrossRef]
- Toivonen, J. A Model for Mitochondrial Deafness in Flies. Expression and Mutation Analysis of Mitoribosomal Protein S12; Tampere University Press: Tampere, Finland, 2003. [Google Scholar]
- Dejager, S.; Bry-Gauillard, H.; Bruckert, E.; Eymard, B.; Salachas, F.; LeGuern, E.; Turpin, G. A comprehensive endocrine description of Kennedy’s disease revealing androgen insensitivity linked to CAG repeat length. J. Clin. Endocrinol. Metab. 2002, 87, 3893–3901. [Google Scholar]
- Taylor, J.P.; Tanaka, F.; Robitschek, J.; Sandoval, C.M.; Taye, A.; Markovic-Plese, S.; Fischbeck, K.H. Aggresomes protect cells by enhancing the degradation of toxic polyglutamine-containing protein. Hum. Mol. Genet. 2003, 12, 749–757. [Google Scholar] [CrossRef] [PubMed]
- Rusmini, P.; Bolzoni, E.; Crippa, V.; Onesto, E.; Sau, D.; Galbiati, M.; Poletti, A. Proteasomal and autophagic degradative activities in spinal and bulbar muscular atrophy. Neurobiol. Dis. 2010, 40, 361–369. [Google Scholar] [CrossRef] [PubMed]
- My, A.; Luong, J.K.; Bhati, K.K.; Batoko, H. Cargo receptors and adaptors for selective autophagy in plant cells. FEBS Lett. 2022, 596, 2104–2132. [Google Scholar]
- Ma, X.; Liu, H.; Murphy, J.T.; Foyil, S.R.; Godar, R.J.; Abuirqeba, H.; Weinheimer, C.J.; Barger, P.M.; Diwan, A. Regulation of the transcription factor EB-PGC1α axis by beclin-1 controls mitochondrial quality and cardiomyocyte death under stress. Mol. Cell. Biol. 2015, 35, 956–976. [Google Scholar] [CrossRef]
- Cetrullo, S.; D’Adamo, S.; Tantini, B.; Borzi, R.M.; Flamigni, F. mTOR, AMPK, and Sirt1: Key players in metabolic stress management. Crit. Rev. Eukaryot. Gene Expr. 2015, 25, 59–75. [Google Scholar] [CrossRef]
- Gomez-Pastor, R.; Burchfiel, E.T.; Thiele, D.J. Regulation of heat shock transcription factors and their roles in physiology and disease. Nat. Rev. Mol. Cell Biol. 2018, 19, 4–19. [Google Scholar] [CrossRef]
- Pandey, U.B.; Nie, Z.; Batlevi, Y.; McCray, B.A.; Ritson, G.P.; Nedelsky, N.B.; Padmanabhan, R. HDAC6 rescues neurodegeneration and provides an essential link between autophagy and the UPS. Nature 2007, 447, 860. [Google Scholar] [CrossRef]
- Mulakkal, N.C.; Nagy, P.; Takats, S.; Tusco, R.; Juhász, G.; Nezis, I.P. Autophagy in Drosophila: From historical studies to current knowledge. BioMed Res. Int. 2014, 2014, 273473. [Google Scholar]
- Matilla-Dueñas, A.; Goold, R.; Giunti, P. Clinical, genetic, molecular, and pathophysiological insights into spinocerebellar ataxia type 1. Cerebellum 2008, 7, 106. [Google Scholar] [CrossRef]
- Corazzari, M.; Fimia, G.M.; Lovat, P.; Piacentini, M. Why is autophagy important for melanoma? Molecular mechanisms and therapeutic implications. In Seminars in Cancer Biology; Academic Press: Cambridge, MA, USA, 2013; Volume 23, pp. 337–343. [Google Scholar]
- Schaaf, M.B.; Keulers, T.G.; Vooijs, M.A.; Rouschop, K.M. LC3/GABARAP family proteins: Autophagy-(un) related functions. FASEB J. 2016, 30, 3961–3978. [Google Scholar] [CrossRef]
- Heintze, J.M. The Role of Ribose-5-Phosphate ISomerase A in the Regulation of Autophagy. Ph.D. Dissertation, University College London, London, UK, 2016. [Google Scholar]
- Agrotis, A.; Pengo, N.; Burden, J.J.; Ketteler, R. Redundancy of human ATG4 protease isoforms in autophagy and LC3/GABARAP processing revealed in cells. Autophagy 2019, 15, 976–997. [Google Scholar] [CrossRef] [PubMed]
- Matilla-Dueñas, A.; Ashizawa, T.; Brice, A.; Magri, S.; McFarland, K.N.; Pandolfo, M.; Pulst, S.M.; Riess, O.; Rubinsztein, D.C.; Schmidt, J.; et al. Consensus paper: Pathological mechanisms underlying neurodegeneration in spinocerebellar ataxias. Cerebellum 2014, 13, 269–302. [Google Scholar] [CrossRef] [PubMed]
- Ding, Y.; Adachi, H.; Katsuno, M.; Sahashi, K.; Kondo, N.; Iida, M.; Tohnai, G.; Nakatsuji, H.; Sobue, G. BIIB021, a synthetic Hsp90 inhibitor, induces mutant ataxin-1 degradation through the activation of heat shock factor 1. Neuroscience 2016, 327, 20–31. [Google Scholar] [CrossRef] [PubMed]
- Egorova, P.A.; Bezprozvanny, I.B. Molecular mechanisms and therapeutics for spinocerebellar ataxia type 2. Neurotherapeutics 2019, 16, 1050–1073. [Google Scholar] [CrossRef]
- Marcelo, A.; Afonso, I.T.; Afonso-Reis, R.; Brito, D.V.; Costa, R.G.; Rosa, A.; Nóbrega, C. Autophagy in Spinocerebellar ataxia type 2, a dysregulated pathway, and a target for therapy. Cell Death Dis. 2021, 12, 1117. [Google Scholar] [CrossRef] [PubMed]
- Underwood, B.R.; Imarisio, S.; Fleming, A.; Rose, C.; Krishna, G.; Heard, P.; Quick, M.; Korolchuk, V.I.; Renna, M.; Sarkar, S.; et al. Antioxidants can inhibit basal autophagy and enhance neurodegeneration in models of polyglutamine disease. Hum. Mol. Genet. 2010, 19, 3413–3429. [Google Scholar] [CrossRef]
- Puorro, G.; Marsili, A.; Sapone, F.; Pane, C.; De Rosa, A.; Peluso, S.; Saccà, F. Peripheral markers of autophagy in polyglutamine diseases. Neurol. Sci. 2018, 39, 149–152. [Google Scholar] [CrossRef]
- La Spada, A.R.; Taylor, J.P. Repeat expansion disease: Progress and puzzles in disease pathogenesis. Nat. Rev. Genet. 2010, 11, 247. [Google Scholar] [CrossRef]
- Burnett, B.; Li, F.; Pittman, R.N. The polyglutamine neurodegenerative protein ataxin-3 binds polyubiquitylated proteins and has ubiquitin protease activity. Hum. Mol. Genet. 2003, 12, 3195–3205. [Google Scholar] [CrossRef]
- Menzies, F.M.; Huebener, J.; Renna, M.; Bonin, M.; Riess, O.; Rubinsztein, D.C. Autophagy induction reduces mutant ataxin-3 levels and toxicity in a mouse model of spinocerebellar ataxia type 3. Brain 2009, 133, 93–104. [Google Scholar] [CrossRef]
- Bilen, J.; Bonini, N.M. Genome-wide screen for modifiers of ataxin-3 neurodegeneration in Drosophila. PLoS Genet. 2007, 3, e177. [Google Scholar] [CrossRef] [PubMed]
- Niewiadomska-Cimicka, A.; Trottier, Y. Molecular targets and therapeutic strategies in spinocerebellar ataxia type 7. Neurotherapeutics 2019, 16, 1074–1096. [Google Scholar] [CrossRef] [PubMed]
- De Michele, G.; Galatolo, D.; Barghigiani, M.; Iacovo, D.D.; Trovato, R.; Tessa, A.; Salvatore, E.; Filla, A.; De Michele, G.; Santorelli, F.M. Spinocerebellar ataxia type 48: Last but not least. Neurol. Sci. 2020, 41, 2423–2432. [Google Scholar] [CrossRef] [PubMed]
- Niu, C.; Prakash, T.P.; Kim, A.; Quach, J.L.; Huryn, L.A.; Yang, Y.; Lopez, E.; Jazayeri, A.; Hung, G.; Sopher, B.L.; et al. Antisense oligonucleotides targeting mutant Ataxin-7 restore visual function in a mouse model of spinocerebellar ataxia type 7. Sci. Transl. Med. 2018, 10, eaap8677. [Google Scholar] [CrossRef]
- Barthet, V.J.; Ryan, K.M. Autophagy in neurodegeneration: Can’t digest it, spit it out! Trends Cell Biol. 2018, 28, 171–173. [Google Scholar] [CrossRef]
- Paulson, H.L. The spinocerebellar ataxias. J. Neuro Ophthalmol. 2009, 29, 227–237. [Google Scholar] [CrossRef]
- Zander, C.; Takahashi, J.; El Hachimi, K.H.; Fujigasaki, H.; Albanese, V.; Lebre, A.S.; Stevanin, G.; Duyckaerts, C.; Brice, A. Similarities between spinocerebellar ataxia type 7 (SCA7) cell models and human brain: Proteins recruited in inclusions and activation of caspase-3. Hum. Mol. Genet. 2001, 10, 2569–2579. [Google Scholar] [CrossRef]
- Uversky, V.N.; Na, I.; Landau, S.K.; Schenck, O.R. Highly disordered proteins in prostate cancer. Curr. Protein Pept. Sci. 2017, 18, 453–481. [Google Scholar] [CrossRef]
- Min, H.J.; Ko, E.A.; Wu, J.; Kim, E.S.; Kwon, M.K.; Kwak, M.S.; Choi, J.E.; Lee, J.E.; Shin, J.S. Chaperone-like activity of high-mobility group box 1 protein and its role in reducing the formation of polyglutamine aggregates. J. Immunol. 2013, 190, 1797–1806. [Google Scholar] [CrossRef] [PubMed]
- Calabrese, V.; Lodi, R.; Tonon, C.; D’Agata, V.; Sapienza, M.; Scapagnini, G.; Mangiameli, A.; Pennisi, G.; Stella, A.G.; Butterfield, D.A. Oxidative stress, mitochondrial dysfunction and cellular stress response in Friedreich’s ataxia. J. Neurol. Sci. 2005, 233, 145–162. [Google Scholar] [CrossRef]
- Toth, M.E.; Gonda, S.; Vigh, L.; Santha, M. Neuroprotective effect of small heat shock protein, Hsp27, after acute and chronic alcohol administration. Cell Stress Chaperones 2010, 15, 807–817. [Google Scholar] [CrossRef] [PubMed]
- Amin, A.; Perera, N.D.; Beart, P.M.; Turner, B.J.; Shabanpoor, F. Amyotrophic Lateral Sclerosis and Autophagy: Dysfunction and Therapeutic Targeting. Cells 2020, 9, 2413. [Google Scholar] [CrossRef] [PubMed]
- Evers, M.M.; Pepers, B.A.; van Deutekom, J.C.; Mulders, S.A.; den Dunnen, J.T.; Aartsma-Rus, A.; van Ommen, G.J.; van Roon-Mom, W.M. Targeting several CAG expansion diseases by a single antisense oligonucleotide. PLoS ONE 2011, 6, e24308. [Google Scholar] [CrossRef] [PubMed]
- Ueno, T.; Komatsu, M. Monitoring autophagy flux and activity: Principles and applications. Bioessays 2020, 42, 2000122. [Google Scholar] [CrossRef] [PubMed]
- Karabiyik, C.; Frake, R.A.; Park, S.J.; Pavel, M.; Rubinsztein, D.C. Autophagy in ageing and ageing-related neurodegenerative diseases. Ageing Neurodegener. Dis. 2021, 1, 2. [Google Scholar] [CrossRef]
- Kim, T.; Song, B.; Lee, I.S. Drosophila glia: Models for human neurodevelopmental and neurodegenerative disorders. Int. J. Mol. Sci. 2020, 21, 4859. [Google Scholar] [CrossRef] [PubMed]
- Perera, R.M.; Zoncu, R. The lysosome as a regulatory hub. Annu. Rev. Cell Dev. Biol. 2016, 32, 223–253. [Google Scholar] [CrossRef]
- Fujikake, N.; Shin, M.; Shimizu, S. Association between autophagy and neurodegenerative diseases. Front. Neurosci. 2018, 12, 255. [Google Scholar] [CrossRef]
- Zatyka, M.; Sarkar, S.; Barrett, T. Autophagy in rare (nonlysosomal) neurodegenerative diseases. J. Mol. Biol. 2020, 432, 2735–2753. [Google Scholar] [CrossRef]
- Spada, A.R.; Wilson, E.M.; Lubahn, D.B.; Harding, A.E.; Fischbeck, K.H. Androgen receptor gene mutations in X-linked spinal and bulbar muscular atrophy. Nature 1991, 352, 77–79. [Google Scholar] [CrossRef]
- Ren, H.; Hao, Z.; Wang, G. Autophagy and polyglutamine disease. In Autophagy: Biology and Diseases; Springer: Berlin/Heidelberg, Germany, 2020; pp. 149–161. [Google Scholar]
- Shin, W.H.; Park, J.H.; Chung, K.C. The central regulator p62 between ubiquitin proteasome system and autophagy and its role in the mitophagy and Parkinson’s disease. BMB Rep. 2020, 53, 56. [Google Scholar] [CrossRef] [PubMed]
- Fornai, F.; Longone, P.; Ferrucci, M.; Lenzi, P.; Isidoro, C.; Ruggieri, S.; Paparelli, A. Autophagy and amyotrophic lateral sclerosis: The multiple roles of lithium. Autophagy 2008, 4, 527–530. [Google Scholar] [CrossRef] [PubMed]
- Berger, Z.; Ravikumar, B.; Menzies, F.M.; Oroz, L.G.; Underwood, B.R.; Pangalos, M.N.; Rubinsztein, D.C. Rapamycin alleviates toxicity of different aggregate-prone proteins. Hum. Mol. Genet. 2006, 15, 433–442. [Google Scholar] [CrossRef] [PubMed]
- De Bosch, B.J.; Heitmeier, M.R.; Mayer, A.L.; Higgins, C.B.; Crowley, J.R.; Kraft, T.E.; Moley, K.H. Trehalose inhibits solute carrier 2A (SLC2A) proteins to induce autophagy and prevent hepatic steatosis. Sci. Signal. 2016, 9, ra21. [Google Scholar]
- Garratt, M.; Nakagawa, S.; Simons, M.J. Comparative idiosyncrasies in life extension by reduced mTOR signalling and its distinctiveness from dietary restriction. Aging Cell. 2016. [Google Scholar] [CrossRef]
- Evers, M.M.; Toonen, L.J.; van Roon-Mom, W. Ataxin-3 protein and RNA toxicity in spinocerebellar ataxia type 3: Current insights and emerging therapeutic strategies. Mol. Neurobiol. 2014, 49, 1513–1531. [Google Scholar] [CrossRef]
- Deshmukh, A.L.; Porro, A.; Mohiuddin, M.; Lanni, S.; Panigrahi, G.B.; Caron, M.C.; Masson, J.Y.; Sartori, A.A.; Pearson, C.E. FAN1, a DNA repair nuclease, as a modifier of repeat expansion disorders. J. Huntingt. Dis. 2021, 10, 95–122. [Google Scholar] [CrossRef]
- Pasquali, L.; Busceti, C.L.; Fulceri, F.; Paparelli, A.; Fornai, F. Intracellular pathways underlying the effects of lithium. Behav. Pharmacol. 2010, 21, 473–492. [Google Scholar] [CrossRef]
- He, S.; Li, Q.; Jiang, X.; Lu, X.; Feng, F.; Qu, W.; Chen, Y.; Sun, H. Design of small molecule autophagy modulators: A promising druggable strategy. J. Med. Chem. 2017, 61, 4656–4687. [Google Scholar] [CrossRef]
- RamaKrishnan, A.M.; Sankaranarayanan, K. Understanding autoimmunity: The ion channel perspective. Autoimmun. Rev. 2016, 15, 585–620. [Google Scholar] [CrossRef]
- Cárdenas, C.; Miller, R.A.; Smith, I.; Bui, T.; Molgó, J.; Müller, M.; Foskett, J.K. Essential regulation of cell bioenergetics by constitutive InsP3 receptor Ca2+ transfer to mitochondria. Cell 2010, 142, 270–283. [Google Scholar] [CrossRef] [PubMed]
- Meier, J.L.; Grose, C. Focus: Drug Development: Variable Effects of Autophagy Induction by Trehalose on Herpesviruses Depending on Conditions of Infection. Yale, J. Biol. Med. 2017, 90, 25. [Google Scholar] [PubMed]
- Chang, C.C.; Lin, T.C.; Ho, H.L.; Kuo, C.Y.; Li, H.H.; Korolenko, T.A.; Lin, C.L. GLP-1 analogue liraglutide attenuates mutant huntingtin-induced neurotoxicity by restoration of neuronal insulin signaling. Int. J. Mol. Sci. 2018, 19, 2505. [Google Scholar] [CrossRef] [PubMed]
- Ju, T.C.; Chen, H.M.; Lin, J.T.; Chang, C.P.; Chang, W.C.; Kang, J.J.; Chern, Y. Nuclear translocation of AMPK-α1 potentiates striatal neurodegeneration in Huntington’s disease. J. Cell Biol. 2011, 194, 209–227. [Google Scholar] [CrossRef] [PubMed]
- Takei, N.; Nawa, H. mTOR signaling and its roles in normal and abnormal brain development. Front. Mol. Neurosci. 2014, 7, 28. [Google Scholar] [CrossRef]
- Giorgetti, E.; Rusmini, P.; Crippa, V.; Cristofani, R.; Boncoraglio, A.; Cicardi, M.E.; Galbiati, M.; Poletti, A. Synergic prodegradative activity of Bicalutamide and trehalose on the mutant androgen receptor responsible for spinal and bulbar muscular atrophy. Hum. Mol. Genet. 2015, 24, 64–75. [Google Scholar] [CrossRef]
- Abd-Elrahman, K.S.; Hamilton, A.; Hutchinson, S.R.; Liu, F.; Russell, R.C.; Ferguson, S.S. mGluR5 antagonism increases autophagy and prevents disease progression in the zQ175 mouse model of Huntington’s disease. Sci. Signal. 2017, 10, eaan6387. [Google Scholar] [CrossRef]
- Duarte, A.I.; Sjögren, M.; Santos, M.S.; Oliveira, C.R.; Moreira, P.I.; Björkqvist, M. Dual therapy with liraglutide and ghrelin promotes brain and peripheral energy metabolism in the R6/2 mouse model of Huntington’s disease. Sci. Rep. 2018, 8, 8961. [Google Scholar] [CrossRef]
- Makpol, S. Epigenetic Changes and Its Intervention in Age-Related Neurodegenerative Diseases. Cell. Mol. Neurobiol. 2020, 42, 577–595. [Google Scholar]
- Banno, H.; Katsuno, M.; Suzuki, K.; Sobue, G. Dutasteride for spinal and bulbar muscular atrophy. Lancet Neurol. 2011, 10, 113–115. [Google Scholar] [CrossRef]
- Jenner, P.; Pratt, J.A.; Marsden, C.D. Mechanism of action of clonazepam in myoclonus in relation to effects on GABA and 5-HT. Adv. Neurol. 1986, 43, 629–643. [Google Scholar] [PubMed]
- Saxena, R.; Babadi, M.; Namvarhaghighi, H.; Roullet, F.I. Role of environmental factors and epigenetics in autism spectrum disorders. Prog. Mol. Biol. Transl. Sci. 2020, 173, 35–60. [Google Scholar] [PubMed]
- Abumossalam, A.M.; Sheta, A.F.; Ahmed, S.E.; Elhalaby, D.A.; Moawad, A.A. Extra pulmonary boosting in chronic obstructive pulmonary disease: Leverage of piracetam as an adjunctive therapy on respiratory and neuropsychiatric functions in patients with chronic obstructive pulmonary disease. Egypt. J. Chest Dis. Tuberc. 2021, 70, 60. [Google Scholar]
- Bushart, D.D.; Huang, H.; Man, L.J.; Morrison, L.M.; Shakkottai, V.G. A Chlorzoxazone-Baclofen Combination Improves Cerebellar Impairment in Spinocerebellar Ataxia Type 1. Mov. Disord. 2021, 36, 622–631. [Google Scholar] [CrossRef] [PubMed]
- Farzam, K.; Abdullah, M. Acetazolamide; StatPearls: Tampa, FL, USA, 2020. [Google Scholar]
- Bolandghamat, S.; Behnam-Rassouli, M. Recent Findings on the Effects of Pharmacological Agents on the Nerve Regeneration after Peripheral Nerve Injury. Curr. Neuropharmacol. 2020, 18, 1154–1163. [Google Scholar] [CrossRef] [PubMed]
- Mai, L.; Huang, F.; Zhu, X.; He, H.; Fan, W. Role of nerve growth factor in orofacial pain. J. Pain Res. 2020, 13, 1875. [Google Scholar] [CrossRef] [PubMed]
- La Spada, A.R. Spinocerebellar Ataxia Type 7. In Gene Reviews; University of Washington: Seattle, WA, USA, 2020. [Google Scholar]
- Shnayder, N.A.; Bochanova, E.N.; Dmitrenko, D.V.; Nasyrova, R.F. Pharmacogenetics of carbamazepine. Epilepsy Paroxysmal Cond. 2020, 11, 364–378. [Google Scholar] [CrossRef]
- Silver, J.; Blum, S. Introduction to the neuropsychiatric examination. In Oxford Textbook of Neuropsychiatry; Oxford University Press: Oxford, UK, 2020; p. 13. [Google Scholar]
- Schwitalla, J.C.; Pakusch, J.; Mücher, B.; Brückner, A.; Depke, D.A.; Fenzl, T.; De Zeeuw, C.I.; Kros, L.; Hoebeek, F.E.; Mark, M.D. Controlling absence seizures from the cerebellar nuclei via activation of the Gq signaling pathway. Cell. Mol. Life Sci. 2022, 79, 197. [Google Scholar] [CrossRef]


| Different Types of polyQ Diseases | Autophagy Modulators | Mode of Action | Ref. |
|---|---|---|---|
| HD | Rapamycin, CCI-779 | mTORC1 inhibition | [29] |
| Rilmenidine | AMPK activation | [29] | |
| Lithium | mTORC1 inhibition | [88] | |
| Trehalose | mTORC1 inhibition | [88] | |
| CTEP | Formation of autolysosome | [89] | |
| Liraglutide | AMPK activation | [90] | |
| Neferine | AMPK activation | [90] | |
| Histone Deacetylase Inhibitor | HDAC modulation | [91] | |
| SBMA | Dutasteride | Decreases DHT production | [92] |
| Trehalose | Androgen receptor (AR) degradation; Enhance autophagy | [92] | |
| Placebo | In primary stage decrease DHT production | [92] | |
| DRPLA | Clonazepam | Modulation of GABA function in the brain | [93] |
| Chlordiazepoxide | Increased binding of the inhibitory neurotransmitter | [93] | |
| Sodium valproate | Mediated through effects on the function of brain | [93] | |
| Piracetam | Producing a lowering of cerebral artery tonus | [94] | |
| SCA1 | Baclofen | It improves Cerebellar Impairment | [95] |
| Acetazolamide | lower blood pH and carbonic anhydrase inhibitor | [96] | |
| SCA2 | Riluzole | Inhibits the release of glutamic acid from cultured neurons | [97] |
| SCA3 | Tnezumab | Inhibiting the binding of NGF | [98] |
| Fasinumab | Inhibiting the binding of NGF | [98] | |
| SCA6 | Acetazolamide | lower blood pH and carbonic anhydrase inhibitor | [96] |
| Riluzole | Inhibits the release of glutamic acid from cultured neurons | [97] | |
| SCA7 | Amantadine | Increases dopamine release | [99] |
| Buspirone | Prevents dopamine reuptake | [100] | |
| Riluzole | Inhibits the release of glutamic acid from cultured neurons | [94] | |
| SCA17 | Sodium valproate | Mediated through effects on the function of brain | [94] |
| Carbamazepine | It reduces the release of a neurotransmitter—Glutamate | [98] | |
| Lamotrigine | Suppressing the release of the excitatory glutamate | [101] | |
| Topiramate | Control brain activity | [102] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jain, M.; Patil, N.; Abdi, G.; Abbasi Tarighat, M.; Mohammed, A.; Ahmad Mohd Zain, M.R.; Goh, K.W. Mechanistic Insights and Potential Therapeutic Approaches in PolyQ Diseases via Autophagy. Biomedicines 2023, 11, 162. https://doi.org/10.3390/biomedicines11010162
Jain M, Patil N, Abdi G, Abbasi Tarighat M, Mohammed A, Ahmad Mohd Zain MR, Goh KW. Mechanistic Insights and Potential Therapeutic Approaches in PolyQ Diseases via Autophagy. Biomedicines. 2023; 11(1):162. https://doi.org/10.3390/biomedicines11010162
Chicago/Turabian StyleJain, Mukul, Nil Patil, Gholamreza Abdi, Maryam Abbasi Tarighat, Arifullah Mohammed, Muhammad Rajaei Ahmad Mohd Zain, and Khang Wen Goh. 2023. "Mechanistic Insights and Potential Therapeutic Approaches in PolyQ Diseases via Autophagy" Biomedicines 11, no. 1: 162. https://doi.org/10.3390/biomedicines11010162
APA StyleJain, M., Patil, N., Abdi, G., Abbasi Tarighat, M., Mohammed, A., Ahmad Mohd Zain, M. R., & Goh, K. W. (2023). Mechanistic Insights and Potential Therapeutic Approaches in PolyQ Diseases via Autophagy. Biomedicines, 11(1), 162. https://doi.org/10.3390/biomedicines11010162





