Predict Health Care Accessibility for Texas Medicaid Gap
Abstract
1. Introduction
2. Materials and Methods
2.1. Data
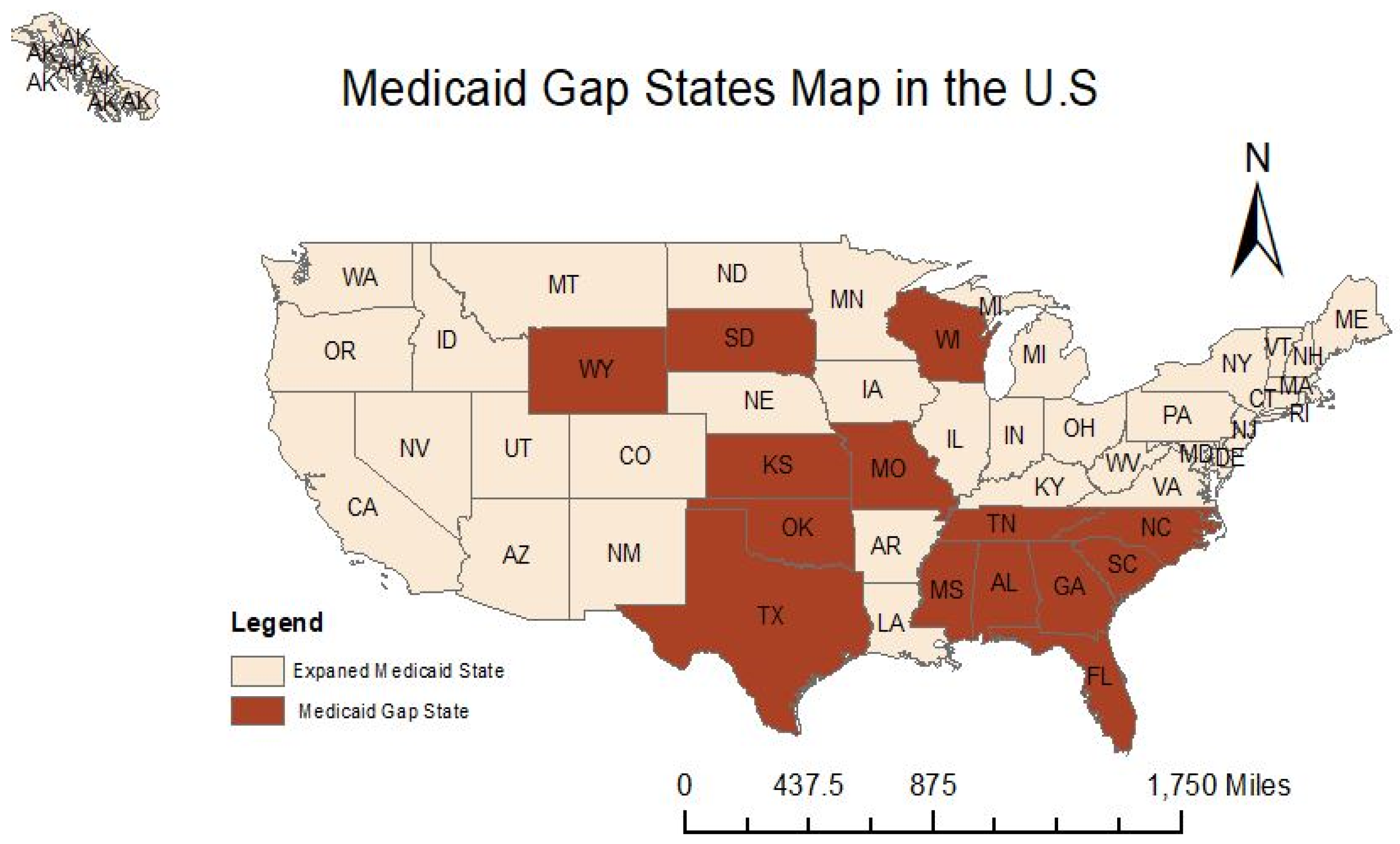
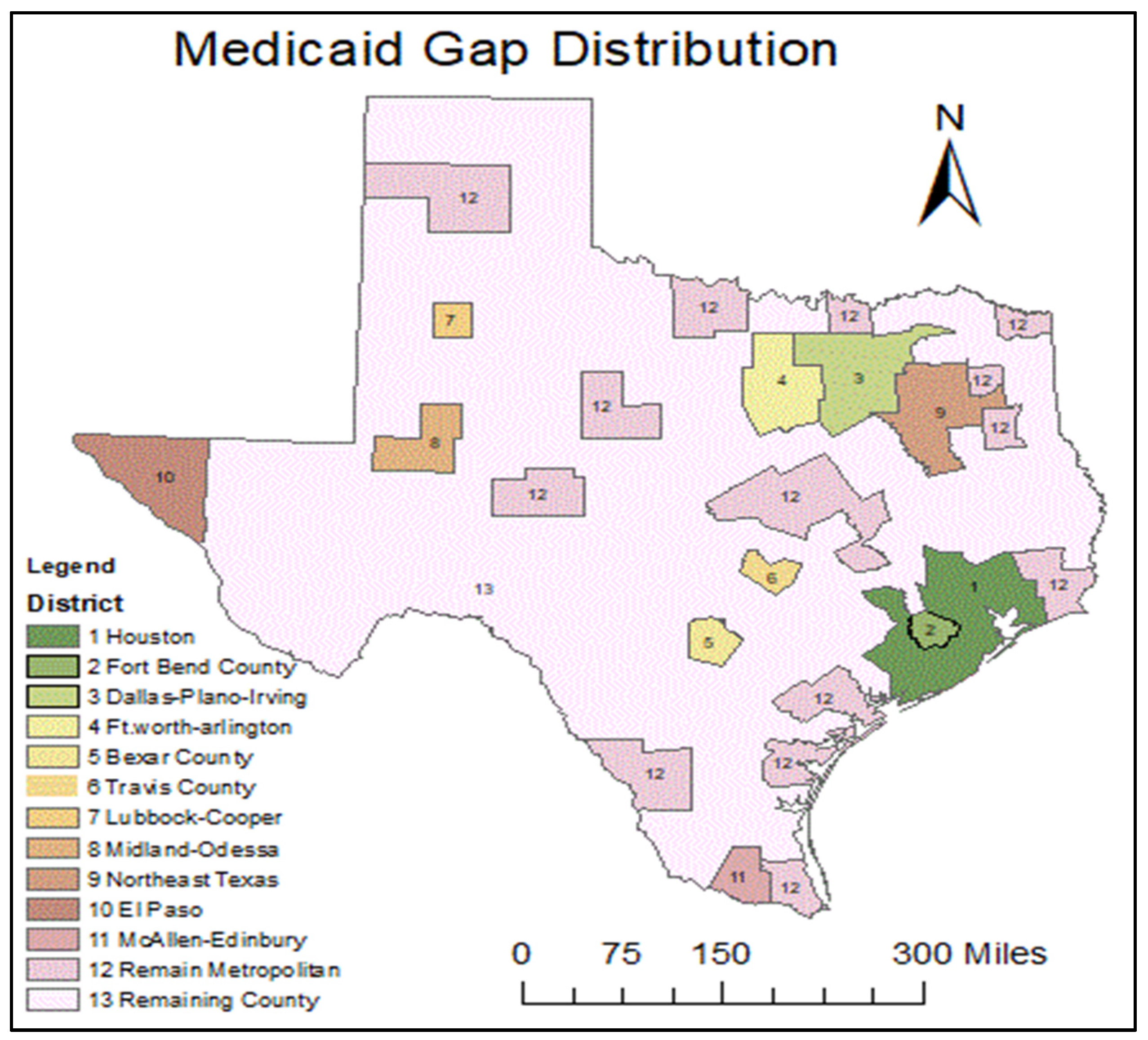
2.2. Data Spatial Representation
2.3. PCA-LA Rationale
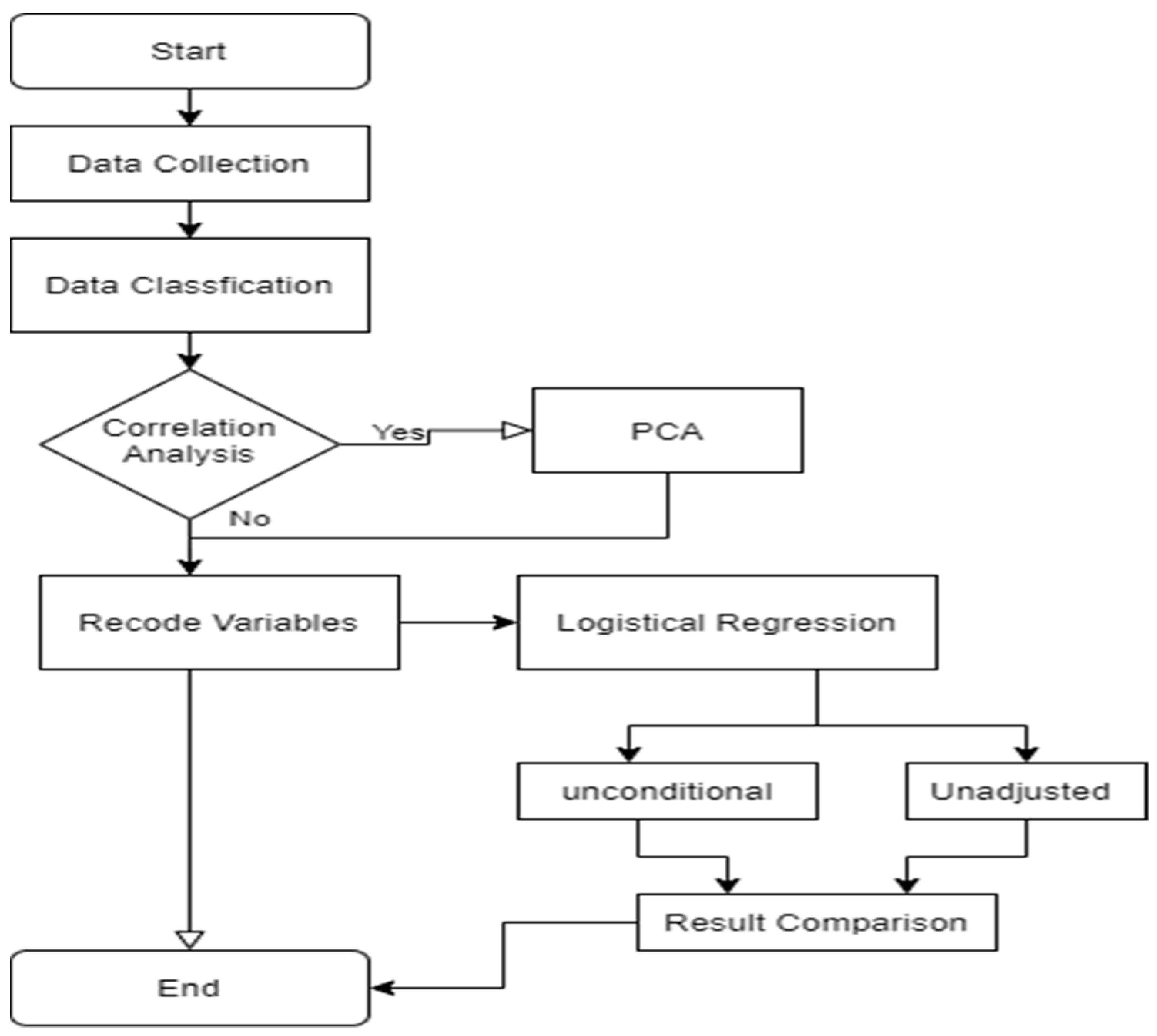
2.4. PCA-LA Analysis Procedure
- (1)
- Pearson correlation analysis in dependent variables. The bivariate Pearson correlation is used to estimate correlations among pairs of variables. The coefficients are revealed whether a statistically significant linear relationship exists between two continuous variables, as well as directions and strengths of a linear relationship. In the SPSS environment, the function of a bivariate is completed by choosing the correlate option of the analyzing menus [17].
- (2)
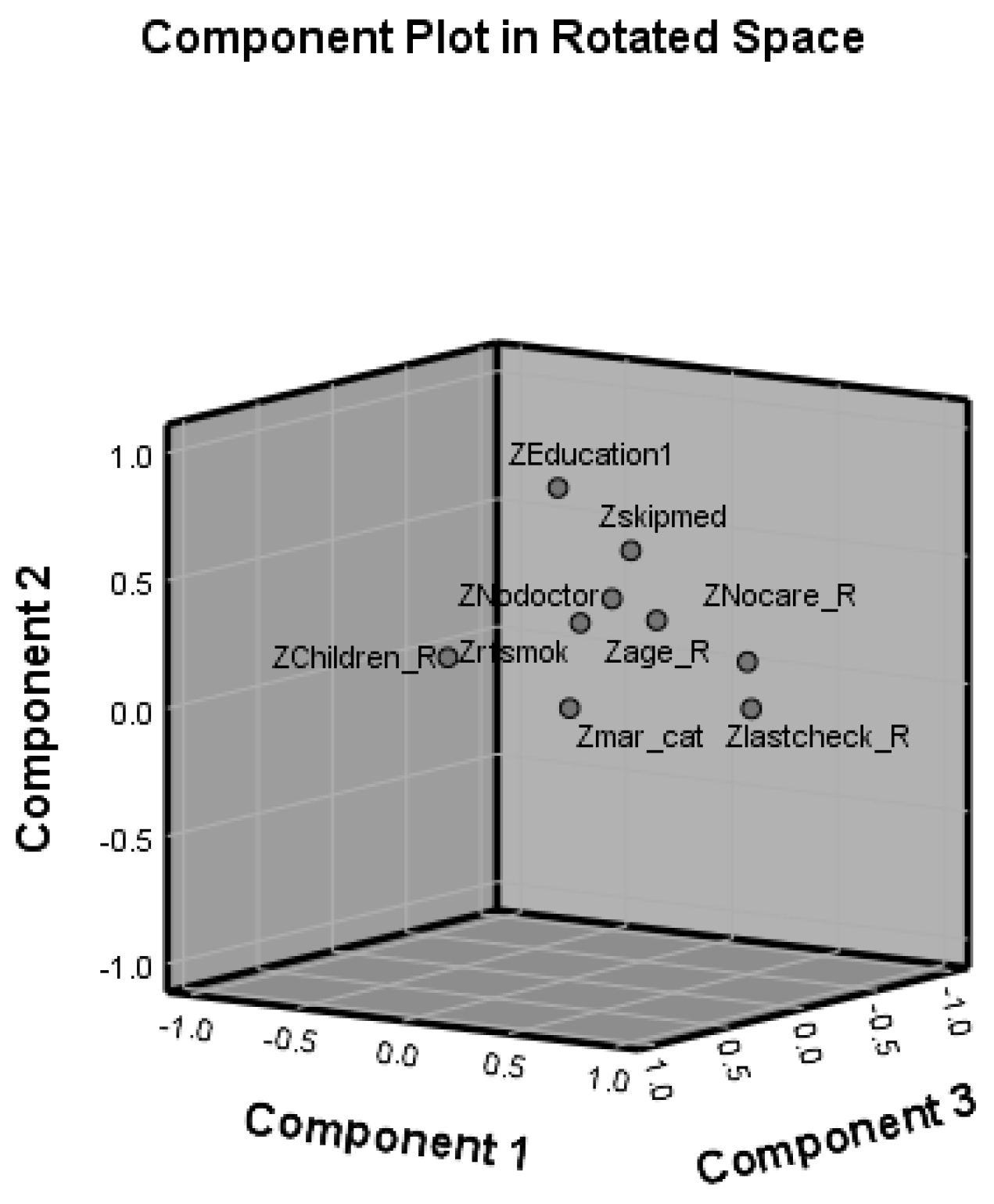
- PCA to extract major components. Based on correlation analysis, we performed nine explanatory variables to extract component factors using PCA. The dataset was examined using Kaiser–Meyer–Olkin (KMO) and Bartlett’s Test of Sphericity. The KMO test compares the correlation statistics to identify if the variables include sufficient differences to extract unique factors. A KMO value of 0.56 for nine explanatory variables is more than the cutoff value of 0.7. The Bartlett’s Test of Sphericity (BTS) value of 0.0 was significant (p < 0.001), validating that correlation between variables does exist in the population. Communality is a common variance between 0 and 1, using the remaining variables as factors, which was used to determine if any variables should be excluded from the factor analysis. A 0.7 cutoff is used to determine the significance of explanatory variables [18]. Using an eigenvalue threshold greater than 1.0, four factors are identified that could explain a cumulative 64.7% of the variance after six iterations (Figure 3). A varimax rotation was used to assist in the interpretation of the PCA analysis. The rotated component matrix was examined for variables with a cutoff of 0.7.
- (3)
- Perform logistical regression on major components. Geographic disparities in health care are well noted [19,20,21,22], but seldom research has shown healthcare spending varies by geographical location in the Medicaid gap via statistical analysis. Even some ethnic groups may be under-represented in the Medicaid expansion population because they are more likely to live in states that have not expanded Medicaid [23,24]. Current studies highlighted the policy adjustment from the qualitative analysis [25,26,27,28] except for Spencer et al. (2019). Despite the Medicaid Gap population in North Carolina for health access was conducted in Statistical inference, counter-comparative multi-variated indexes were not involved [29]. In addition, potential risks of chronic diseases were not estimated in the research. Most importantly, multicollinearity issues are not mentioned, which is a phenomenon that undermines the statistical significance of an independent variable, increases the standard deviation of variables, as well as the inverse direction of coefficients [30,31,32]. Logistical regression is generally popular in the application of epidemiology [33,34,35,36]; most research investigated models without eliminating multicollinearity among variables. PCA is one of the effective ways to reduce dimensionality and minimize multicollinearity. Currently published articles of logistical regression based on PCA are focused on genome-wide association studies [37] and disease research, such as gestational diabetes mellitus [38] and nephropathy [39]. Health care accessibility for the Texas Medicaid Gap took advantage of principal component analysis (PCA) to eliminate multicollinearity negative effects and to compare comprehensive social-economic impacts between unadjusted conditions and adjusted conditions. Therefore, PCA-based LA health access analysis of the medical gap is beneficial to provide scientific evidence regarding whether implementing ACA or not, to balance Medicaid policies in the U.S.
- (4)
- T-tests and F-tests were used to validate the significance of the model. T-test compares the means of two independent groups in order to determine whether there is statistical evidence that the associated population means are significantly different. In SPSS, the “Independent-Samples t-test” function is selected in the “compare mean” default of analyzing menu [40]. In addition, the F-test can be used for determining whether the variances of two groups differ from each other. In the SPSS environment, “One-way analysis of variance (ANOVA Analysis)” is selected as “Homogeneity of variance test” in “compare means” of “options” [41].
3. Results
3.1. Sample Description
3.1.1. Health Care Access
3.1.2. Demographic Status
3.1.3. Economic, Educational, and Marital Status
3.1.4. Space–Time Sample Change
3.2. Correlation
3.3. PCA Results
3.4. Logistical Regression Analysis
3.4.1. Health Conditions
3.4.2. Demographic Impacts
3.4.3. Education Impacts
3.4.4. Marital Status Impacts
3.5. The Result of the T-Test and F-Test
4. Discussion
5. Conclusions
5.1. Limitation
5.2. Implication
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Serban, N. Healthcare System Access: Measurement, Inference, and Intervention, 1st ed.; Wiley: Hoboken, NJ, USA, 2020. [Google Scholar]
- Schembri, S.; Ghaddar, S. The Affordable Care Act, the Medicaid Coverage Gap, and Hispanic Consumers: A Phenomenology of Obamacare. J. Consum. Aff. 2018, 52, 138–165. [Google Scholar] [CrossRef]
- Kenneth, L.J.; Stephen, L.W. Healthcare in the United States: Clinical, Financial, and Operational Dimensions; Health Administration Press: Chicago, IL, USA, 2021. [Google Scholar]
- Johnson, T. Analysis: Healthcare Should Be a Right, but the U.S. Doesn’t Have a System; ABC News: New York, NY, USA, 2017; Available online: http://abcnews.go.com/Health/analysis-health-care-us-system/story?id=51281693 (accessed on 11 September 2021).
- Michener, J.D. Politics, Pandemic, and Racial Justice through the Lens of Medicaid. Am. J. Public Health 2021, 111, 643–646. [Google Scholar] [CrossRef]
- Kissick, W.L. Medicine’s dilemmas: Infinite needs versus finite resources. J. Econ. Lit. 1995, 33, 331–332. [Google Scholar]
- U.S. Govt. Accountability Office. Medicaid: State and Federal Actions Have Been Taken to Improve Children’s Access to Dental Services, but Gaps Remain: Report to Congressional Requesters; U.S. Govt. Accountability Office: Washington, DC, USA, 2009.
- United States Government Accountability Office. Medicaid and Insurance Exchanges: Additional Federal Controls Needed to Minimize the Potential for Gaps and Duplication in Coverage: Report to Congressional Requesters; United States Government Accountability Office: Washington, DC, USA, 2015.
- Albertson, E.M.; Scannell, C.; Ashtari, N.; Barnert, E. Eliminating Gaps in Medicaid Coverage during Reentry after Incarceration. Am. J. Public Health 2020, 110, 317–321. [Google Scholar] [CrossRef]
- Spencer, J.C.; Gertner, A.K.; Silberman, P.J. Health Status and Access to Care for the North Carolina Medicaid Gap Population. N. C. Med. J. 2019, 80, 269–275. [Google Scholar] [CrossRef]
- Rawal, P.H. The Affordable Care Act: Examining the Facts; ABC-CLIO: Santa Barbara, CA, USA, 2016. [Google Scholar]
- U.S. Government Printing Office. The Affordable Care Act: The Impact of Health Insurance Reform on Health Care Consumers: Hearing of the Committee on Health, Education, Labor, and Pensions, United States Senate, One Hundred Twelfth Congress, First Session, 27 January 2011; U.S. Government Printing Office: Washington, DC, USA, 2013.
- Selena Simmons-Duffin. 12 Holdout States Haven’t Expanded Medicaid, Leaving 2 Million People in Limbo. All Things Consid. NPR 2021. Available online: https://search-ebscohost-com.libproxy.txstate.edu/login.aspx?direct=true&db=n5h&AN=6XN2021070113&site=eds-live&scope=site (accessed on 9 July 2021).
- Rowland, D.; Lyons, B. Medicaid’s Role in Health Reform and Closing the Coverage Gap. J. Law Med. Ethics 2016, 44, 580–584. [Google Scholar] [CrossRef]
- Curtis, M.L.; Eschiti, V.S. Geographic Health Disparities: Satellite clinics for cancer care in rural communities. Clin. J. Oncol. Nurs. 2018, 22, 500–506. [Google Scholar] [CrossRef] [PubMed]
- Srinivas, K.; Madhukar Rao, G.; Vengatesan, K.; Shivkumar Tanesh, P.; Kumar, A.; Yuvaraj, S. An implementation of subsidy prediction system using machine learning logistical regression algorithm. Adv. Math. Sci. J. 2020, 9, 3407–3415. [Google Scholar] [CrossRef]
- Qiu, J.L.; Zheng, J.N.; Zhang, Y. Application of modified logistic regression model in the analysis of epidemiology. China Trop. Med. 2005, 5, 207–209. [Google Scholar]
- Weaver, B.; Wuensch, K.L. SPSS and SAS programs for comparing Pearson correlations and OLS regression coefficients. Behav. Res. Methods 2013, 45, 880–895. [Google Scholar] [CrossRef]
- Hickman, D.T.; Chow, T.E. Development of a Composite Model of Quality of Life: A Case Study in Austin, Texas. GISci. Remote Sens. 2012, 49, 802–821. [Google Scholar] [CrossRef]
- Yemisrach, A.D.; Okwaraji, B.; Tigabu, Z.; Persson, L.A.; Alemu, K. Geographic differences in maternal and child health care utilization in four Ethiopian regions; a cross-sectional study. Int. J. Equity Health 2019, 18, 173. [Google Scholar] [CrossRef]
- Pinheiro, L.C.; Reshetnyak, E.; Safford, M.M.; Nanus, D.; Kern, L.M. Healthcare fragmentation and cardiovascular risk control among older cancer survivors in the Reasons for Geographic and Racial Differences in Stroke (REGARDS) study. J. Cancer Surviv. Res. Pract. 2021, 15, 325–332. [Google Scholar] [CrossRef]
- Nwangwu-Ike, N.; Chan, J.; Gant, Z.; Johnson, S.; Balaji, A.B. An examination of geographic differences in social determinants of health among women with diagnosed HIV in the United States and Puerto Rico, 2017. Open AIDS J. 2021, 15, 10–20. [Google Scholar] [CrossRef]
- Courtemanche, C.; Marton, J.; Ukert, B.; Yelowitz, A.; Zapata, D.; Fazlul, I. The three-year impact of the Affordable Care Act on disparities in insurance coverage. Health Serv. Res. 2019, 54 (Suppl. S1), 307–316. [Google Scholar] [CrossRef]
- Chang, T.; Davis, M. Potential adult Medicaid beneficiaries under the Patient Protection and Affordable Care Act compared with current adult Medicaid beneficiaries. Ann. Fam. Med. 2013, 11, 406–411. [Google Scholar] [CrossRef]
- Pilon, D.; El Khoury, A.C.; Manceur, A.M.; Zhdanava, M.; Benson, C.; Lefebvre, P.; Doshi, J.A. Are Medicaid Coverage Gaps Associated with Higher Health Care Resource Utilization and Costs in Patients with Schizophrenia? Popul. Health Manag. 2020, 23, 234–242. [Google Scholar] [CrossRef] [PubMed]
- Ariel, C. Beneficiary Groups Oppose Verifying Income of Those in Medicaid Gap. Inside CMS 2017, 20, 5–6. [Google Scholar]
- Rosenbaum, S.; Wilensky, G. Closing the Medicaid Coverage Gap: Options for Reform. Health Aff. 2020, 39, 514–518. [Google Scholar] [CrossRef]
- Yocom, C.L. Medicaid: Federal Oversight of Payments and Program Integrity Needs Improvement: Testimony before the Subcommittees on Health Care, District of Columbia, Census and the National Archives and Regulatory Affairs, Stimulus Oversight and Government Spending, Committee on Oversight and Government Reform, House of Representatives, Testimony: GAO-12-674T; U.S. Govt. Accountability Office: Washington, DC, USA, 2012.
- Clement, J.; Jacobi, M.; Greenwood, B.N. Patient access to chronic medications during the Covid-19 pandemic: Evidence from a comprehensive dataset of US insurance claims. PLoS ONE 2021, 16, e0249453. [Google Scholar] [CrossRef]
- Baird, G.L.; Bieber, S.L. The goldilocks dilemma: Impacts of multicollinearity—A comparison of simple linear regression, multiple regression, and ordered variable regression models. J. Mod. Appl. Stat. Methods 2016, 15, 332–357. [Google Scholar] [CrossRef]
- Ariyajunya, B.; Chen, Y.; Chen, V.C.P.; Kim, S.B.; Rosenberger, J. Addressing state space multicollinearity in solving an ozone pollution dynamic control problem. Eur. J. Oper. Res. 2021, 289, 683–695. [Google Scholar] [CrossRef]
- Schwarz, C.; Schwarz, A.; Black, W.C. Examining the impact of multicollinearity in discovering higher-order factor models. Commun. Assoc. Inf. Syst. 2014, 34, 1191–1208. [Google Scholar] [CrossRef]
- Gong, X.; Lin, Y.; Zhan, F.B. Industrial air pollution and low birth weight: A case-control study in Texas, USA. Environ. Sci. Pollut. Res. 2018, 25, 30375–30389. [Google Scholar] [CrossRef]
- Martin, M.; Woodbury, D.; Glogower, Y.; Duguid, M.; Frey, B.; Ashton, M. Within-gap position shapes fifty years of forest dynamics in a temperate hardwood forest in Connecticut, USA. For. Ecol. Manag. 2021, 494, 119311. [Google Scholar] [CrossRef]
- Long, M.; Ghisari, M.; Kjeldsen, L.; Wielsøe, M.; Nørgaard-Pedersen, B.; Mortensen, E.L.; Abdallah, M.W.; Bonefeld-Jørgensen, E.C. Autism spectrum disorders, endocrine disrupting compounds, and heavy metals in amniotic fluid: A case-control study. Mol. Autism 2019, 10, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Passamonti, S.M.; Cannavò, A.; Panigada, M.; Trunzo, V.; Bottazzi, A.; Longobardi, A.; Buonocore, R.; Fiorattini, A.; Torelli, R.; Piccolo, G.; et al. Donation after circulatory death (DCD) and liver transplantation: A cohort study. Transpl. Int. Off. J. Eur. Soc. Organ Transplant. 2021, 34, 1271–1280. [Google Scholar] [CrossRef]
- Chen, Z.; Liu, F.; Li, B.; Peng, X.; Fan, L.; Luo, A. Prediction of hot spot areas of hemorrhagic fever with renal syndrome in Hunan Province based on an information quantity model and logistical regression model. PLoS Negl. Trop. Dis. 2020, 14, e0008939. [Google Scholar] [CrossRef] [PubMed]
- Yi, H.; Zhao, Y.; Zhang, R.; Dai, J.; Jin, G.; Ma, H.; Wu, T.; Hu, Z.; Lin, D.; Shen, H. Comparison of dimension reduction-based logistic regression models for case-control genome-wide association study: Principal components analysis vs. partial least squares. J. Biomed. Res. 2015, 29, 298–307. [Google Scholar] [CrossRef]
- Wang, Y.; Zhang, P.; Chen, X.; Wu, W.; Feng, Y.; Yang, H.; Li, M.; Xie, B.; Guo, P.; Warren, J.L.; et al. Multiple metal concentrations and gestational diabetes mellitus in Taiyuan, China. Chemosphere 2015, 237, 124412. [Google Scholar] [CrossRef]
- Tápanes, F.J.; Vásquez, M.; Ramírez, R.; Matheus, C.; Rodríguez, M.A.; Bianco, N. Cluster Analysis of Antinuclear Autoantibodies in the Prognosis of SLE Nephropathy: Are Anti-Extractable Nuclear Antibodies Protective? Lupus 2000, 9, 437–444. [Google Scholar] [CrossRef] [PubMed]
- Howard, W.; Odum Institute for Research in Social Science; Shi, F. Learn about Single Mean t-Test in SPSS with Data from the Behavioral Risk Factor Surveillance System (2015)/Feng Shi. 2019. Available online: https://doi-org.libproxy.txstate.edu/http://methods.sagepub.com/dataset/singlet-in-brfss-2015 (accessed on 11 September 2021).
- Bortz, J.; Schuster, C. Statistik für Human- und Sozialwissenschaftler; Springer: Berlin, Germay, 2010. [Google Scholar]
- Horowitz, L.M.; de Sales French, R. Interpersonal problems of people who describe themselves as lonely. J. Consult. Clin. Psychol. 1979, 47, 762–764. [Google Scholar] [CrossRef] [PubMed]
- Domènech-Abella, J.; Switsers, L.; Mundó, J.; Dierckx, E.; Dury, S.; De Donder, L. The association between perceived social and physical environment and mental health among older adults: Mediating effects of loneliness. Aging Ment. Health 2021, 25, 962–968. [Google Scholar] [CrossRef] [PubMed]
- Midi, H.; Sarkar, S.K.; Rana, S. Collinearity diagnostics of binary logistic regression model. J. Interdiscip. Math. 2010, 13, 253–267. [Google Scholar] [CrossRef]
- Guide to Clinical Preventive Services: Periodic Updates, 3rd ed.; U.S. Department of Health and Human Services, Agency for Healthcare Research and Quality: Washington, DC, USA, 2004.
- Anderson, L.J.; Shekelle, P.; Keeler, E.; Uscher-Pines, L.; Shanman, R.; Morton, S.; Aliyev, G.; Nuckols, T.K. The Cost of Interventions to Increase Influenza Vaccination: A Systematic Review. Am. J. Prev. Med. 2018, 54, 299–315. [Google Scholar] [CrossRef] [PubMed]
- Nichol, K.L. Cost-benefit analysis of a strategy to vaccinate healthy working adults against influenza. Arch. Intern. Med. 2001, 161, 749–759. [Google Scholar] [CrossRef] [PubMed]
- Goldman, A.L.; Woolhandler, S.; Himmelstein, D.U.; Bor, D.H.; McCormick, D. Out-of-Pocket Spending and Premium Contributions after Implementation of the Affordable Care Act. JAMA Intern. Med. 2018, 178, 347–355. [Google Scholar] [CrossRef]
- Liu, C.; Rahman, A.S.; Chao, T.E. Catastrophic expenditures in California trauma patients after the Affordable Care Act: Reduced financial risk and racial disparities. Am. J. Surg. 2020, 220, 511–517. [Google Scholar] [CrossRef]
- Lopez-Santana, M. Fragmented Democracy: Medicaid, Federalism, and Unequal Politics. Publius-J. Federalism. 2020, 50. [Google Scholar] [CrossRef]
- Schneider, A.; Ingram, H. Social Construction of Target Populations: Implications for Politics and Policy. Am. Political Sci. Rev. 1993, 87, 334–347. [Google Scholar] [CrossRef]
- Sommers, B.D.; Baicker, K.; Epstein, A.M. Mortality and access to care among adults after state Medicaid expansions. N. Engl. J. Med. 2012, 367, 1025–1034. [Google Scholar] [CrossRef] [PubMed]
- Baicker, K.; Brown, J.R.; Holtz-Eakin, D.; Orszag, P. Future of Social Security, Medicare, and Medicaid: Is U.S. Entitlement Spending Sustainable? Risk Manag. Insur. Rev. 2008, 11, 1–21. [Google Scholar] [CrossRef]
- Milcent, C. Healthcare Reform in China: From Violence to Digital Healthcare; Palgrave Macmillan: London, UK, 2018. [Google Scholar]
- Liu, J. Healthcare Quality and HIT: International Standards, China Practices; CRC Press: Boca Raton, FL, USA, 2019. [Google Scholar]
- Ayenew, L.G.; Hoelscher, M.A.; Emshoff, J.G.; Kidder, D.P.; Ellis, B.A. Evaluation of the public health achievements made by projects supported by a federal contract mechanism at the Centers for Disease Control and Prevention (CDC), USA. Eval. Program Plan. 2021, 88, 101949. [Google Scholar] [CrossRef] [PubMed]
- Preker, A.S. Financing Universal Access to Healthcare: A Comparative Review of Landmark Legislative Health Reforms in the OECD; World Scientific Publishing, Co. Pte. Ltd.: Singapore, 2018. [Google Scholar]
- Cu, A.; Meister, S.; Lefebvre, B.; Ridde, V. Assessing healthcare access using the Levesque’s conceptual framework—A scoping review. Int. J. Equity Health 2021, 20, 116. [Google Scholar] [CrossRef] [PubMed]
| Year | Above-Poverty | Medicaid | Medicaid Gap | Total |
|---|---|---|---|---|
| 2013 | 638 | 6871 | 575 | 8084 |
| 2014 | 939 | 9912 | 874 | 11,725 |
| 2015 | 904 | 9481 | 764 | 11,149 |
| 2016 | 670 | 8070 | 509 | 9249 |
| 2017 | 732 | 8252 | 613 | 9597 |
| 2018 | 573 | 7370 | 472 | 8415 |
| 2019 | 2249 | 1483 | 1094 | 4826 |
| 2020 | 21 | 7 | 10 | 38 |
| Total | 6726 | 51,446 | 4911 | 63,083 |
| Predictors | Acronym | Value | AbovePoverty | Medicaid | Medicaid Gap | Interpretation |
|---|---|---|---|---|---|---|
| Health Condition | ||||||
| No regular source of care | NRC | 1 | 74.0% | 25.1% | 32.7% | No (Good) |
| No regular source of care | 2 | 26.0% | 74.9% | 67.3% | Yes (Bad) | |
| Last check-up more than a year ago | LCT | 1 | 79.9% | 76.4% | 46.0% | No (Good) |
| Last check-up more than a year ago | 2 | 20.1% | 23.6% | 54.0% | Yes (Bad) | |
| Could not see doctor due to cost | NSD | 1 | 76.6% | 81.6% | 48.1% | No (Good) |
| Could not see a doctor due to the cost | 2 | 23.4% | 18.4% | 51.9% | Yes (Bad) | |
| Skippedmedicationduetocost | SMC | 1 | 44.5% | 51.1% | 23.3% | No (Good) |
| Skipped medication due to cost | 2 | 55.5% | 48.9% | 76.7% | Yes (Bad) | |
| Cardiovascular disease | CVD | 1 | 13.5% | 10.2% | 16.1% | Yes (Bad) |
| Cardiovascular disease | 2 | 86.5% | 89.8% | 83.9% | No (Good) | |
| Diabetes | DT | 1 | 18% | 31.7% | 42.6% | Yes (Bad) |
| Diabetes | 2 | 82% | 68.3% | 47.4% | No (Good) | |
| Current smoker | CS | 1 | 79.2% | 88.1% | 75.4% | No (Good) |
| Current smoker | 2 | 20.8% | 11.9% | 24.6% | Yes (Bad) | |
| Demographic | ||||||
| Age structure | AS | 1 | 10.7% | 3.9% | 10.6% | Age (<=25) |
| Age structure | 2 | 23.4% | 12.6% | 47.3% | 25 < Age <= 44 | |
| Age structure | 3 | 17.8% | 9.4% | 21.0% | 44< Age <= 55 | |
| Age structure | 4 | 48.1% | 74.2% | 21.2% | Age (>55) | |
| Sex | SEX | 1 | 34.7% | 45.3% | 36.3% | Male |
| Sex | 2 | 65.3% | 54.7% | 63.7% | female | |
| Race | ||||||
| White | RACE | 1 | 30.9% | 50.0% | 34.3% | White |
| Hispanic | 2 | 44.7% | 31.3% | 54.0% | Hispanic | |
| Black | 3 | 20.8% | 13.0% | 8.8% | Black | |
| Other | 4 | 3.6% | 5.7% | 2.9% | Other | |
| Economic condition | ||||||
| Employment | EM | 1 | 30.3% | 54.2% | 50.5% | Yes (Good) |
| Employment | 2 | 69.7% | 45.8% | 49.5% | No (Bad) | |
| Living with dependent children | LDC | 1 | 68.5% | 81.5% | 44.5% | No (Good) |
| Living with dependent children | 2 | 31.5% | 18.5% | 55.5% | Yes (Bad) | |
| Education | ||||||
| College graduate | ED | 1 | 45.1% | 44.2% | 28.6% | |
| High school graduate/GED | 2 | 32.1% | 34.4% | 34.1% | ||
| Did not finish high school | 3 | 22.7% | 21.4% | 37.3% | ||
| Marital status | MS | 1 | 32.1% | 60.0% | 35.4% | married |
| Marital status | 2 | 67.9% | 40.0% | 64.6% | single | |
| Health status | 1 | 67.3% | 82.1% | 27.5% | good | |
| Health status | 0 | 32.7% | 17.9% | 72.5% | poor or fair | |
| Predictors | Acronym | NRC | LCT | NSD | SMC | CS | AS | SEX | RACE | EM | LDC | ED | MS | CVD | DT |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| No regular source of care | NRC | 1/0.00 | |||||||||||||
| Last check up more than a year ago | LCT | −0.53/0.00 | |||||||||||||
| Could not see doctor due to cost | NSD | 0.25/0.00 | 0.24/0.00 | ||||||||||||
| Skipped medication due to cost | SMC | 0.10/0.00 | 0.01/0.04 | 0.27/0.00 | |||||||||||
| Current smoker | CS | −0.08/0.00 | 0.10/0.00 | 0.14/0.00 | 0.06/0.00 | ||||||||||
| Age Structure | AS | −0.17/0.00 | −0.27/0.00 | −0.16/0.00 | −0.23/0.00 | −0.03/0.00 | |||||||||
| Sex | SEX | 0.04/0.00 | −0.07/0.00 | 0.11/0.00 | 0.02/0.00 | −0.05/0.00 | 0.01/0.0.3 | ||||||||
| Race | RACE | 0.02/0.04 | 0.04/0.00 | 0.08/0.00 | 0.19/0.00 | 0.02/0.00 | −0.15/0.00 | 0.01/0.1 | |||||||
| Employment | EM | 0.09/0.00 | −0.14/0.00 | −0.02/0.00 | 0.14/0.00 | −0.02/0.00 | 0.27/0.00 | 0.17/0.00 | −0.03/0.00 | ||||||
| Living with dependent children | LDC | 0.11/0.00 | 0.16/0.00 | 0.16/0.00 | 0.17/0.00 | −0.00/0.03 | −0.44/0.00 | 0.13/0.00 | 0.11/0.00 | −0.17/0.00 | |||||
| Education | ED | 0.18/0.00 | 0.13/0.00 | 0.15/0.00 | 0.29/0.00 | 0.10/0.00 | −0.04/0.00 | 0.04/0.00 | 0.13/0.00 | 0.06/0.00 | 0.16/0.00 | ||||
| Marital status | MS | −0.07/0.00 | 0.47/0.00 | 0.10/0.00 | 0.17/0.00 | 0.12/0.00 | −0.14/0.00 | 0.10/0.00 | 0.10/0.00 | 0.06/0.00 | −0.09/0.00 | 0.06/0.00 | |||
| CVD | CVD | −0.07/0.00 | 0.07/0.00 | −0.03/0.00 | −0.03/0.00 | −0.02/0.00 | −0.09/0.00 | 0.05/0.00 | −0.01/0.24 | −0.15/0.00 | 0.05/0.00 | −0.03/0.00 | 0.01/0.01 | ||
| Diabetes | DT | −0.21/0.00 | 0.02/0.00 | −0.14/0.00 | 0.01/0.00 | 0.02/0.00 | −0.06/0.00 | −0.01/0.00 | −0.13/0.00 | −0.09/0.00 | 0.00/0.7 | −0.23/0.00 | 0.03/0.00 | 0.16/0.00 | |
| Health status | HS | −0.19/0.00 | −0.04/0.00 | 0.22/0.00 | 0.20/0.00 | 0.05/0.00 | −0.1/0.00 | 0.02/0.00 | −0.1/0.00 | 0.12/0.00 | 0.04/0.00 | −0.21/0.00 | −0.11/0.00 | −0.03/0.00 | 0.29/0.00 |
| Acronym | Extraction | Component | |||
|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | ||
| LCT | 0.849 | 0.917 | 0.053 | 0.072 | −0.010 |
| NRC | 0.878 | 0.903 | 0.236 | 0.078 | 0.032 |
| ED | 0.672 | −0.030 | 0.816 | 0.023 | −0.073 |
| SMC | 0.492 | 0.283 | 0.595 | −0.021 | 0.236 |
| NSD | 0.274 | 0.257 | 0.417 | 0.070 | 0.171 |
| AS | 0.792 | −0.168 | 0.159 | −0.840 | −0.185 |
| LDC | 0.765 | −0.018 | 0.262 | 0.682 | −0.289 |
| MS | 0.751 | 0.061 | −0.031 | 0.074 | 0.861 |
| CS | 0.356 | −0.029 | 0.265 | −0.127 | 0.518 |
| Unadjusted | Adjusted | PCA—Unadjusted | PCA—Adjusted | |||
|---|---|---|---|---|---|---|
| Variable/Factor | No. of Patients (%) | No. of Patients(N) | OR (95% CI) a | aOR (95% CI) b | aOR (95% CI) c | aOR (95% CI) d |
| No regular source of care | ||||||
| Above-poverty | ||||||
| NO—1 | 74.0% | 4046 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 26.0% | 1419 | 1.9 [1.68, 2.19] * | 3.29 [2.1, 5.12] * | 1.7 [1.54, 1.9] * | 1.33 [1.16, 1.53] * |
| Traditional Medicaid | ||||||
| NO—1 | 25.1% | 12,582 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 74.9% | 37,468 | 1.02 [0.97, 1.08] | 1.56 [0.98, 2.48] | 1.56 [0.97, 2.52] | 1.18 [0.64, 2.17] |
| Medicaid Gap | ||||||
| NO—1 | 32.7% | 1561 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 67.3% | 3213 | 1.89 [1.66, 2.16] * | 5.8 [4.01, 8.44] * | 1.47 [1.27, 1.7] * | 1.37 [1.18, 1.6] * |
| Last check-up more than a year ago | ||||||
| Above-poverty | ||||||
| NO—1 | 79.9% | 5154 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 20.1% | 1294 | 0.36 [0.24, 0.54] * | 0.35 [0.22, 0.55] * | 1.7 [1.54, 1.9] * | 1.33 [1.16, 1.53] * |
| Traditional Medicaid | ||||||
| NO—1 | 76.4% | 38,826 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 23.6% | 11,991 | 0.65 [0.61, 0.69] * | 1.78 [0.67, 4.71] | 1.56 [0.97, 2.52] | 1.18 [0.64, 2.17] |
| Medicaid Gap | ||||||
| NO—1 | 46% | 2068 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 54% | 2427 | 1.07 [0.94, 0.1.22] | 0.24 [0.17, 0.35] * | 1.47 [1.27, 1.7] * | 1.37 [1.18, 1.6] * |
| Could not see a doctor due to the cost | ||||||
| Above-poverty | ||||||
| NO—1 | 76.6% | 5129 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 23.4% | 1567 | 0.45 [0.4, 0.5] * | 0.60 [0.48, 0.75] * | ||
| Traditional Medicaid | ||||||
| NO—1 | 81.6% | 1210 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 18.4% | 273 | 0.55 [0.4, 0.76] * | 0.52 [0.35, 0.78] * | ||
| Medicaid Gap | ||||||
| NO—1 | 48.1% | 2350 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| YES—2 | 51.9% | 2539 | 0.37 [0.32, 0.42] * | 0.38 [0.32, 0.44] * | ||
| Age | ||||||
| Above-poverty | ||||||
| Age (<=25)—1 | 10.7% | 718 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Age (>25 and <=44)—2 | 23.4% | 1574 | 0.26 [0.2, 0.35] * | 0.44 [0.28, 0.67] * | 0.26 [0.2, 0.35] * | 0.26 [0.19, 0.35] * |
| Age (>44 and <=55)—3 | 17.8% | 1197 | 0.11 [0.08, 0.14] * | 0.30 [0.2, 0.47] * | 0.11 [0.08, 0.14] * | 0.11 [0.08, 0.15] * |
| Age (>55)—4 | 48.1% | 3237 | 0.15 [0.11, 0.2] * | 0.23 [0.15, 0.36] * | 0.15 [0.11, 0.2] * | 0.08 [0.06, 0.11] * |
| Traditional Medicaid | ||||||
| Age (<=25)—1 | 3.9% | 58 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Age (>25 and <=44)—2 | 12.6% | 187 | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] |
| Age (>25 and <=44)—3 | 9.4% | 140 | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] |
| Age (>55)—4 | 74.2% | 1105 | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] | 0.0 [0.0, 0.0] |
| Medicaid Gap | ||||||
| Age (<=25)—1 | 10.6% | 519 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Age (>25 and <=44)—2 | 47.3% | 2321 | 0.55 [0.42, 0.73] * | 0.58 [0.42, 0.8] * | 0.55 [0.42, 0.73] * | 0.51 [0.38, 0.69] * |
| Age (>25 and <=44)—3 | 21.0% | 1032 | 0.28 [0.21, 0.37] * | 0.41 [0.29, 0.57] * | 0.28 [0.21, 0.37] * | 0.28 [0.2, 0.38] * |
| Age (>55)—4 | 21.2% | 1039 | 0.21 [0.16, 0.28] * | 0.32 [0.22, 0.45] * | 0.21 [0.16, 0.28] * | 0.18 [0.14, 0.25] * |
| Education | ||||||
| Above-poverty | ||||||
| Education (College Graduate) | 45.1% | 3033 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Education (High School Graduate/GED) | 32.1% | 2157 | 0.61 [0.54, 0.69] * | 0.81 [0.63, 1.02] | 0.61 [0.54, 0.69] * | 0.8 [0.68, 0.93] ** |
| Education (Did not finish High School) | 22.7% | 1528 | 0.42 [0.37, 0.48] * | 0.71 [0.55, 0.92] * | 0.42 [0.37, 0.48] * | 0.63 [0.53, 0.75] * |
| Traditional Medicaid | ||||||
| Education (College Graduate) | 44.2% | 658 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Education (High School Graduate/GED) | 34.4% | 513 | 0.7 [0.51, 0.96] ** | 0.62 [0.42, 0.92] * | 0.7 [0.51, 0.96] ** | 0.86 [0.48, 1.54] |
| Education (Did not finish High School) | 21.4% | 319 | 0.61 [0.43, 0.87] * | 0.6 [0.38, 0.95] * | 0.61 [0.43, 0.87] * | 0.62 [0.33, 1.17] |
| Medicaid Gap | ||||||
| Education (College Graduate) | 28.6% | 1400 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Education (High School Graduate/GED) | 34.1% | 1673 | 0.87 [0.74, 1.03] | 0.84 [0.68, 1.02] | 0.87 [0.74, 1.03] | 0.88 [0.73, 1.06] * |
| Education (Did not finish High School) | 37.3% | 1830 | 0.62 [0.53, 0.73] * | 0.63 [0.52, 0.78] * | 0.62 [0.53, 0.73] * | 0.72 [0.6, 0.86] * |
| Marital Status | ||||||
| Above-poverty | ||||||
| Married—1 | 32.1% | 2147 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Single—2 | 67.9% | 4550 | 0.69 [0.61, 0.77] * | 0.88 [0.71, 1.1] | 0.69 [0.61, 0.77] * | 0.63 [0.55, 0.72] * |
| Traditional Medicaid | ||||||
| Married—1 | 60.0% | 30,769 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Single—2 | 40.0% | 20,504 | 1.54 [1.47, 1.61] * | 0.61 [0.39, 1.0] ** | 1.54 [1.47, 1.61] * | 0.52 [0.31, 0.88] ** |
| Medicaid Gap | ||||||
| Married—1 | 35.4% | 1731 | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) | 1.00 (referent) |
| Single—2 | 64.6% | 3155 | 1.0 [0.89, 1.15] | 0.93 [0.78, 1.09] | 1.0 [0.89, 1.15] * | 0.85 [0.73, 0.98] ** |
| Components | Equal Variances | t | df | Sig. | Lower CI | Lower CI |
|---|---|---|---|---|---|---|
| Health conditions | assumed | −4.029 | 4103 | 0.000 | −0.224 | −0.077 |
| not assumed | −3.906 | 2099 | 0.000 | −0.227 | −0.075 | |
| Demographic | assumed | 8.987 | 4103 | 0.000 | 0.212 | 0.33 |
| not assumed | 9.068 | 2287 | 0.000 | 0.212 | 0.33 | |
| Education | assumed | −13.368 | 4103 | 0.000 | −0.504 | −0.375 |
| not assumed | −13.151 | 2164 | 0.000 | −0.505 | −0.374 | |
| Marital Status | assumed | 2.143 | 4103 | 0.032 | 0.006 | 0.14 |
| not assumed | 2.113 | 2176 | 0.035 | 0.005 | 0.142 |
| Components | Linear Term | df | Mean Square | F | Sig. |
|---|---|---|---|---|---|
| Combined | 716 | 0.352 | 1.998 | 0.000 | |
| Health conditions | Weighted | 1 | 3.350 | 18.990 | 0.000 |
| Deviation | 715 | 0.348 | 1.974 | 0.000 | |
| Demographic | Weighted | 1 | 16.408 | 93.014 | 0.000 |
| Deviation | 715 | 0.330 | 1.871 | 0.000 | |
| Education | Weighted | 1 | 35.476 | 201.105 | 0.000 |
| Deviation | 715 | 0.303 | 1.720 | 0.000 | |
| Marital Status | Weighted | 1 | 0.950 | 5.386 | 0.000 |
| Deviation | 715 | 0.352 | 1.993 | 0.000 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, J.; Wu, X. Predict Health Care Accessibility for Texas Medicaid Gap. Healthcare 2021, 9, 1214. https://doi.org/10.3390/healthcare9091214
Zhang J, Wu X. Predict Health Care Accessibility for Texas Medicaid Gap. Healthcare. 2021; 9(9):1214. https://doi.org/10.3390/healthcare9091214
Chicago/Turabian StyleZhang, Jinting, and Xiu Wu. 2021. "Predict Health Care Accessibility for Texas Medicaid Gap" Healthcare 9, no. 9: 1214. https://doi.org/10.3390/healthcare9091214
APA StyleZhang, J., & Wu, X. (2021). Predict Health Care Accessibility for Texas Medicaid Gap. Healthcare, 9(9), 1214. https://doi.org/10.3390/healthcare9091214






