Oral Mucosa Could Be an Infectious Target of SARS-CoV-2
Abstract
:1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wang, C.; Horby, P.W.; Hayden, F.G.; Gao, G.F. A novel coronavirus outbreak of global health concern. Lancet 2020, 395, 470–473. [Google Scholar] [CrossRef] [Green Version]
- Takahashi, Y.; Watanabe, N.; Kamio, N.; Kobayashi, R.; Iinuma, T.; Imai, K. Aspiration of periodontopathic bacteria due to poor oral hygiene potentially contributes to the aggravation of COVID-19. J. Oral Sci. 2020, 63, 1–3. [Google Scholar] [CrossRef]
- Gupta, S.; Mohindra, R.; Chauhan, P.K.; Singla, V.; Goyal, K.; Sahni, V.; Gaur, R.; Verma, D.K.; Ghosh, A.; Soni, R.K.; et al. SARS-CoV-2 Detection in Gingival Crevicular Fluid. J. Dent. Res. 2021, 100, 187–193. [Google Scholar] [CrossRef]
- Xu, H.; Zhong, L.; Deng, J.; Peng, J.; Dan, H.; Zeng, X.; Li, T.; Chen, Q. High expression of ACE2 receptor of 2019-nCoV on the epithelial cells of oral mucosa. Int. J. Oral Sci. 2020, 12, 8. [Google Scholar] [CrossRef]
- Xiang, Z.; Koo, H.; Chen, Q.; Zhou, X.; Liu, Y.; Simon-Soro, A. Potential implications of SARS-CoV-2 oral infection in the host microbiota. J. Oral Microbiol. 2020, 13, 1853451. [Google Scholar] [CrossRef]
- Sakaguchi, W.; Kubota, N.; Shimizu, T.; Saruta, J.; Fuchida, S.; Kawata, A.; Yamamoto, Y.; Sugimoto, M.; Yakeishi, M.; Tsukinoki, K. Existence of SARS-CoV-2 Entry Molecules in the Oral Cavity. Int. J. Mol. Sci. 2020, 21, 6000. [Google Scholar] [CrossRef]
- Huang, N.; Pérez, P.; Kato, T.; Mikami, Y.; Okuda, K.; Gilmore, R.C.; Conde, C.D.; Gasmi, B.; Stein, S.; Beach, M.; et al. SARS-CoV-2 infection of the oral cavity and saliva. Nat. Med. 2021, 27, 892–903. [Google Scholar] [CrossRef]
- Hayama, F.H.; Motta, A.C.; Silva Ade, P.; Migliari, D.A. Liquid-based preparations versus conventional cytology: Specimen adequacy and diagnostic agreement in oral lesions. Med. Oral Patol. Oral Cir. Bucal 2005, 10, 115–122. [Google Scholar] [PubMed]
- Deuerling, L.; Gaida, K.; Neumann, H.; Remmerbach, T.W. Evaluation of the Accuracy of Liquid-Based Oral Brush Cytology in Screening for Oral Squamous Cell Carcinoma. Cancers 2019, 11, 1813. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lao, W.P.; Imam, S.A.; Nguyen, S.A. Anosmia, hyposmia, and dysgeusia as indicators for positive SARS-CoV-2 infection. World J. Otorhinolaryngol. Head Neck Surg. 2020, 6 (Suppl. 1), S22–S25. [Google Scholar] [CrossRef] [PubMed]
- Meinhardt, J.; Radke, J.; Dittmayer, C.; Franz, J.; Thomas, C.; Mothes, R.; Laue, M.; Schneider, J.; Brünink, S.; Greuel, S.; et al. Olfactory transmucosal SARS-CoV-2 invasion as a port of central nervous system entry in individuals with COVID-19. Nat. Neurosci. 2021, 24, 168–175. [Google Scholar] [CrossRef]
- Meunier, N.; Briand, L.; Jacquin-Piques, A.; Brondel, L.; Pénicaud, L. COVID 19-Induced Smell and Taste Impairments: Putative Impact on Physiology. Front. Physiol. 2020, 11, 625110. [Google Scholar] [CrossRef] [PubMed]
- Urata, S.; Maruyama, J.; Kishimoto-Urata, M.; Sattler, R.A.; Cook, R.; Lin, N.; Yamasoba, T.; Makishima, T.; Paessler, S. Regeneration Profiles of Olfactory Epithelium after SARS-CoV-2 Infection in Golden Syrian Hamsters. ACS Chem. Neurosci. 2021, 12, 589–595. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Zhou, J.; Marshall, B.; Rekaya, R.; Ye, K.; Liu, H.X. SARS-CoV-2 Receptor ACE2 Is Enriched in a Subpopulation of Mouse Tongue Epithelial Cells in Nongustatory Papillae but Not in Taste Buds or Embryonic Oral Epithelium. ACS Pharmacol. Transl. Sci. 2020, 3, 749–758. [Google Scholar] [CrossRef]
- Brandão, T.B.; Gueiros, L.A.; Melo, T.S.; Prado-Ribeiro, A.C.; Nesrallah, A.; Prado, G.V.B.; Santos-Silva, A.R.; Migliorati, C.A. Oral lesions in patients with SARS-CoV-2 infection: Could the oral cavity be a target organ? Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2020, 131, e45–e51. [Google Scholar] [CrossRef] [PubMed]
- Sawa, Y.; Ibaragi, S.; Okui, T.; Yamashita, J.; Ikebe, T.; Harada, H. Expression of SARS-CoV-2 entry factors in human oral tissue. J. Anat. 2021, 238, 1341–1354. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Wei, Q.; Alvarez, X.; Wang, H.; Du, Y.; Zhu, H.; Jiang, H.; Zhou, J.; Lam, P.; Zhang, L.; et al. Epithelial cells lining salivary gland ducts are early target cells of severe acute respiratory syndrome coronavirus infection in the upper respiratory tracts of rhesus macaques. J. Virol. 2011, 85, 4025–4030. [Google Scholar] [CrossRef] [Green Version]
- Manzalawi, R.; Alhmamey, K.; Abdelrasoul, M. Gingival bleeding associated with COVID-19 infection. Clin. Case Rep. 2020, 9, 294–297. [Google Scholar] [CrossRef]
- Santos, C.F.; Morandini, A.C.; Dionísio, T.J.; Faria, F.A.; Lima, M.C.; Figueiredo, C.M.; Colombini-Ishikiriama, B.L.; Sipert, C.R.; Maciel, R.P.; Akashi, A.P.; et al. Functional Local Renin-Angiotensin System in Human and Rat Periodontal Tissue. PLoS ONE 2015, 10, e0134601. [Google Scholar] [CrossRef]
- Hussain, M.; Jabeen, N.; Raza, F.; Shabbir, S.; Baig, A.A.; Amanullah, A.; Aziz, B. Structural variations in human ACE2 may influence its binding with SARS-CoV-2 spike protein. J. Med. Virol. 2020, 92, 1580–1586. [Google Scholar] [CrossRef] [Green Version]
- Merk, A.; Bartesaghi, A.; Banerjee, S.; Falconieri, V.; Rao, P.; Davis, M.I.; Pragani, R.; Boxer, M.B.; Earl, L.A.; Milne, J.L.S.; et al. Breaking Cryo-EM Resolution Barriers to Facilitate Drug Discovery. Cell 2016, 165, 1698–1707. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Aebersold, R.; Mann, M. Mass-spectrometric exploration of proteome structure and function. Nature 2016, 537, 347–355. [Google Scholar] [CrossRef] [PubMed]
- Lechien, J.R.; Radulesco, T.; Calvo-Henriquez, C.; Chiesa-Estomba, C.M.; Hans, S.; Barillari, M.R.; Cammaroto, G.; Descamps, G.; Hsieh, J.; Vaira, L.; et al. ACE2 & TMPRSS2 Expressions in Head & Neck Tissues: A Systematic Review. Head Neck Pathol. 2021, 15, 225–235. [Google Scholar] [CrossRef]
- Hoffmann, M.; Kleine-Weber, H.; Schroeder, S.; Krüger, N.; Herrler, T.; Erichsen, S.; Schiergens, T.S.; Herrler, G.; Wu, N.H.; Nitsche, A.; et al. SARS-CoV-2 Cell Entry Depends on ACE2 and TMPRSS2 and Is Blocked by a Clinically Proven Protease Inhibitor. Cell 2020, 181, 271–280.e8. [Google Scholar] [CrossRef]
- Li, M.Y.; Li, L.; Zhang, Y.; Wang, X.S. Expression of the SARS-CoV-2 cell receptor gene ACE2 in a wide variety of human tissues. Infect. Dis. Poverty 2020, 9, 45. [Google Scholar] [CrossRef] [PubMed]
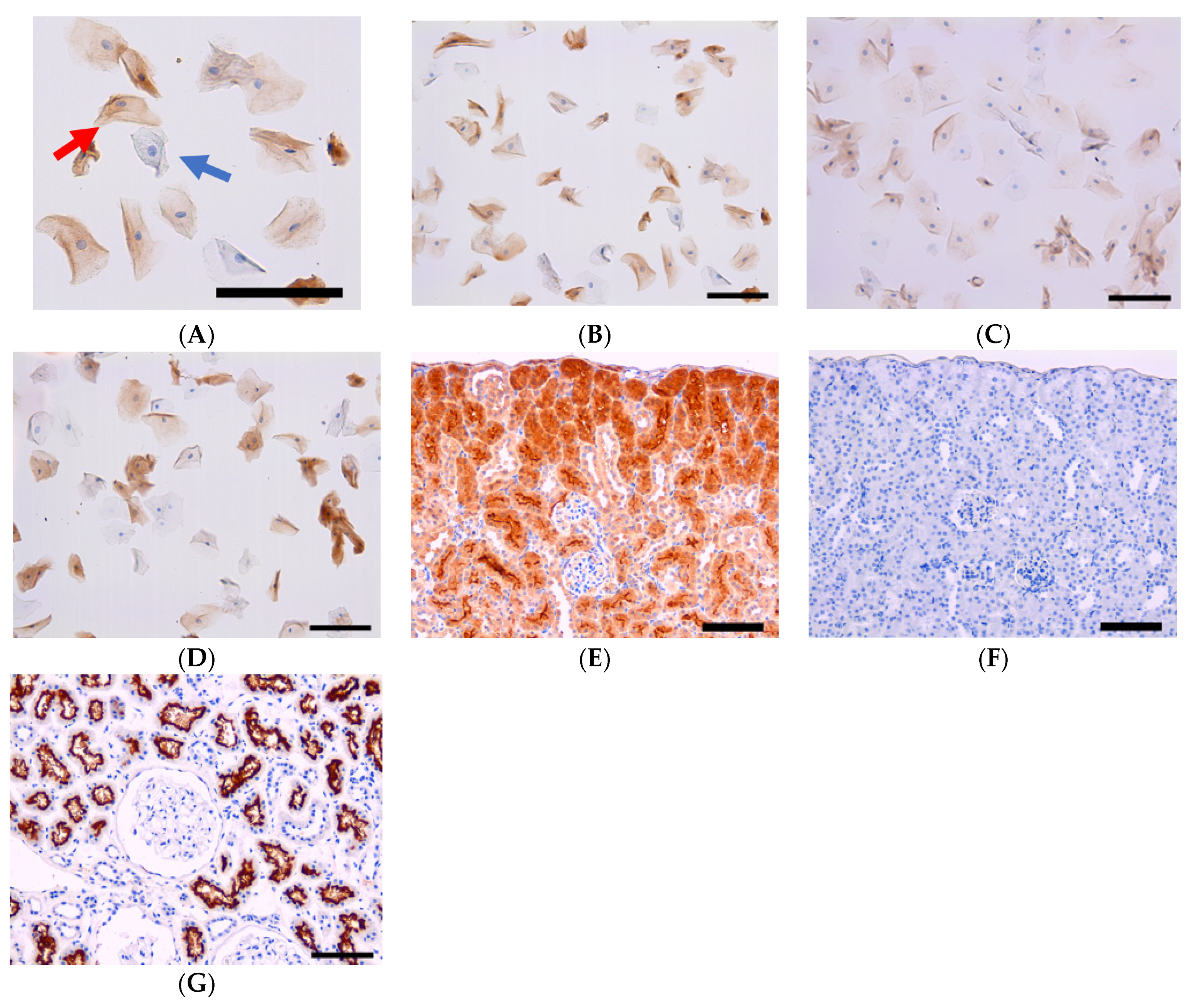
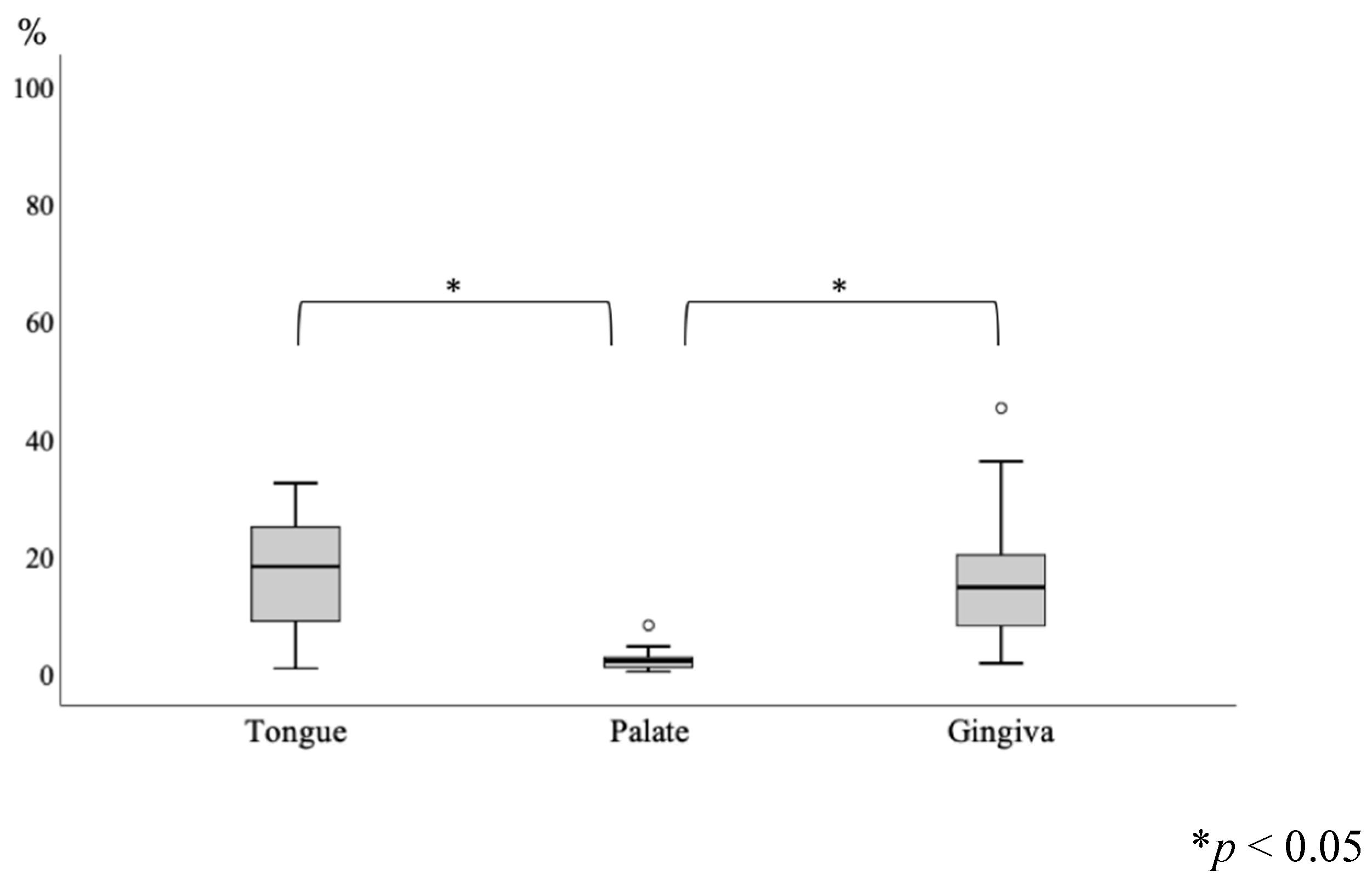
| Item | Category | N (%) or Median (Range) |
|---|---|---|
| Age | Total | 36.0 (29–43) |
| Low group (n = 9) | 29.0 (26.0–30.5) | |
| High group (n = 11) | 43.0 (38.0–55.0) | |
| Gender | Male | 10.0 (50.0%) |
| Female | 10.0 (50.0%) | |
| Medical history | Hyperuricemia | 1.0 (5.0%) |
| Dermatitis | 2.0 (10.0%) | |
| Hypertension | 1.0 (5.0%) | |
| Graves’ disease | 1.0 (5.0%) | |
| Glaucoma | 1.0 (5.0%) | |
| Asthma | 1.0 (5.0%) | |
| Regular medicine | Benzbromarone | 1.0 (5.0%) |
| Minocycline | 1.0 (5.0%) | |
| Amlodipine | 1.0 (5.0%) | |
| Drospirenone | 1.0 (5.0%) | |
| Mercazole | 1.0 (5.0%) | |
| Antihistamine | 1.0 (5.0%) | |
| Alcohol consumption | Regular drinkers | 5.0 (25.0%) |
| None or Social drinkers | 15.0 (75.0%) | |
| Smoking history | Yes | 5.0 (25.0%) |
| No | 15.0 (75.0%) | |
| Brinkman Index | Total | 0.0 (0.0–7.5) |
| Low group (n = 15) | 0.0 (0.0) | |
| High group (n = 5) | 30.0 (14.0–375.0) |
| Item | Category | Median (IQR) |
|---|---|---|
| Tongue | Total amount of cells | 2129.0 (1695.0–7497.0) |
| ACE2 receptor negative | 993.0 (556.0–1864.3) | |
| ACE2 receptor positive | 478.0 (144.3–1051.0) | |
| Positive proportion (%) | 18.2 (8.7–25.1) | |
| Palate | Total amount of cells | 2597.5 (1555.8–4029.5) |
| ACE2 receptor negative | 1498.0 (879.0–2120.0) | |
| ACE2 receptor positive | 44.5 (14.5–107.5) | |
| Positive proportion (%) | 2.0 (0.9–2.7) | |
| Gingiva | Total amount of cells | 7923.5 (5457.0–14,661.8) |
| ACE2 receptor negative | 2984.0 (1208.3–4715.0) | |
| ACE2 receptor positive | 1323.5 (629.0–2272.3) | |
| Positive proportion (%) | 14.6 (7.7–20.6) |
| Item | Category | Median (IQR) | p-Value |
|---|---|---|---|
| ACE2-receptor-positive proportion of tongue | |||
| Age | Low group | 17.7 (11.0–29.1) | 0.50 |
| High group | 18.7 (7.7–24.5) | ||
| Gender | Male | 11.2 (6.7–23.1) | 0.14 |
| Female | 19.6 (14.5–28.2) | ||
| Alcohol consumption | Regular drinkers | 18.7 (6.8–25.3) | 1.00 |
| None or Social drinkers | 17.7 (8.6–25.4) | ||
| Smoking history | Yes | 25.4 (14.0–29.1) | 0.14 |
| No | 16.2 (7.7–22.4) | ||
| Brinkman index | Low group | 16.2 (7.7–22.4) | 0.14 |
| High group | 25.4 (14.0–29.1) | ||
| ACE2-receptor-positive proportion of Palate | |||
| Age | Low group | 1.9 (0.9–3.6) | 0.94 |
| High group | 2.2 (0.9–2.7) | ||
| Gender | Male | 1.6 (0.9–2.2) | 0.19 |
| Female | 2.6 (1.1–3.2) | ||
| Alcohol consumption | Regular drinkers | 2.5 (2.1–3.0) | 0.17 |
| None or Social drinkers | 1.4 (0.8–2.7) | ||
| Smoking history | Yes | 2.2 (1.7–2.5) | 0.80 |
| No | 1.8 (0.8–3.2) | ||
| Brinkman index | Low group | 1.8 (0.8–3.2) | 0.80 |
| High group | 2.2 (1.7–2.5) | ||
| ACE2-receptor-positive proportion of Gingiva | |||
| Age | Low group | 17.1 (11.8–20.1) | 0.30 |
| High group | 11.9 (3.7–22.5) | ||
| Gender | Male | 15.6 (8.1–20.1) | 0.91 |
| Female | 13.9 (6.4–23.5) | ||
| Alcohol consumption | Regular drinkers | 11.9 (6.6–38.2) | 0.87 |
| None or Social drinkers | 15.2 (8.9–19.2) | ||
| Smoking history | Yes | 21.0 (10.0–33.9) | 0.23 |
| No | 12.6 (7.3–19.2) | ||
| Brinkman index | Low group | 12.6 (7.3–19.2) | 0.23 |
| High group | 21.0 (10.0–33.9) | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Okui, T.; Matsuda, Y.; Karino, M.; Hideshima, K.; Kanno, T. Oral Mucosa Could Be an Infectious Target of SARS-CoV-2. Healthcare 2021, 9, 1068. https://doi.org/10.3390/healthcare9081068
Okui T, Matsuda Y, Karino M, Hideshima K, Kanno T. Oral Mucosa Could Be an Infectious Target of SARS-CoV-2. Healthcare. 2021; 9(8):1068. https://doi.org/10.3390/healthcare9081068
Chicago/Turabian StyleOkui, Tatsuo, Yuhei Matsuda, Masaaki Karino, Katsumi Hideshima, and Takahiro Kanno. 2021. "Oral Mucosa Could Be an Infectious Target of SARS-CoV-2" Healthcare 9, no. 8: 1068. https://doi.org/10.3390/healthcare9081068
APA StyleOkui, T., Matsuda, Y., Karino, M., Hideshima, K., & Kanno, T. (2021). Oral Mucosa Could Be an Infectious Target of SARS-CoV-2. Healthcare, 9(8), 1068. https://doi.org/10.3390/healthcare9081068







