Effects of Exercise Programs on Anxiety in Individuals with Disabilities: A Systematic Review with a Meta-Analysis
Abstract
1. Introduction
2. Methods
2.1. Eligibility Criteria
2.2. Information Sources and Research Strategies
2.3. Inclusion Criteria
2.4. Exclusion Criteria
2.5. Data Extraction Process
2.6. Methodological Quality Assessment
2.7. Statistical Analysis
3. Results
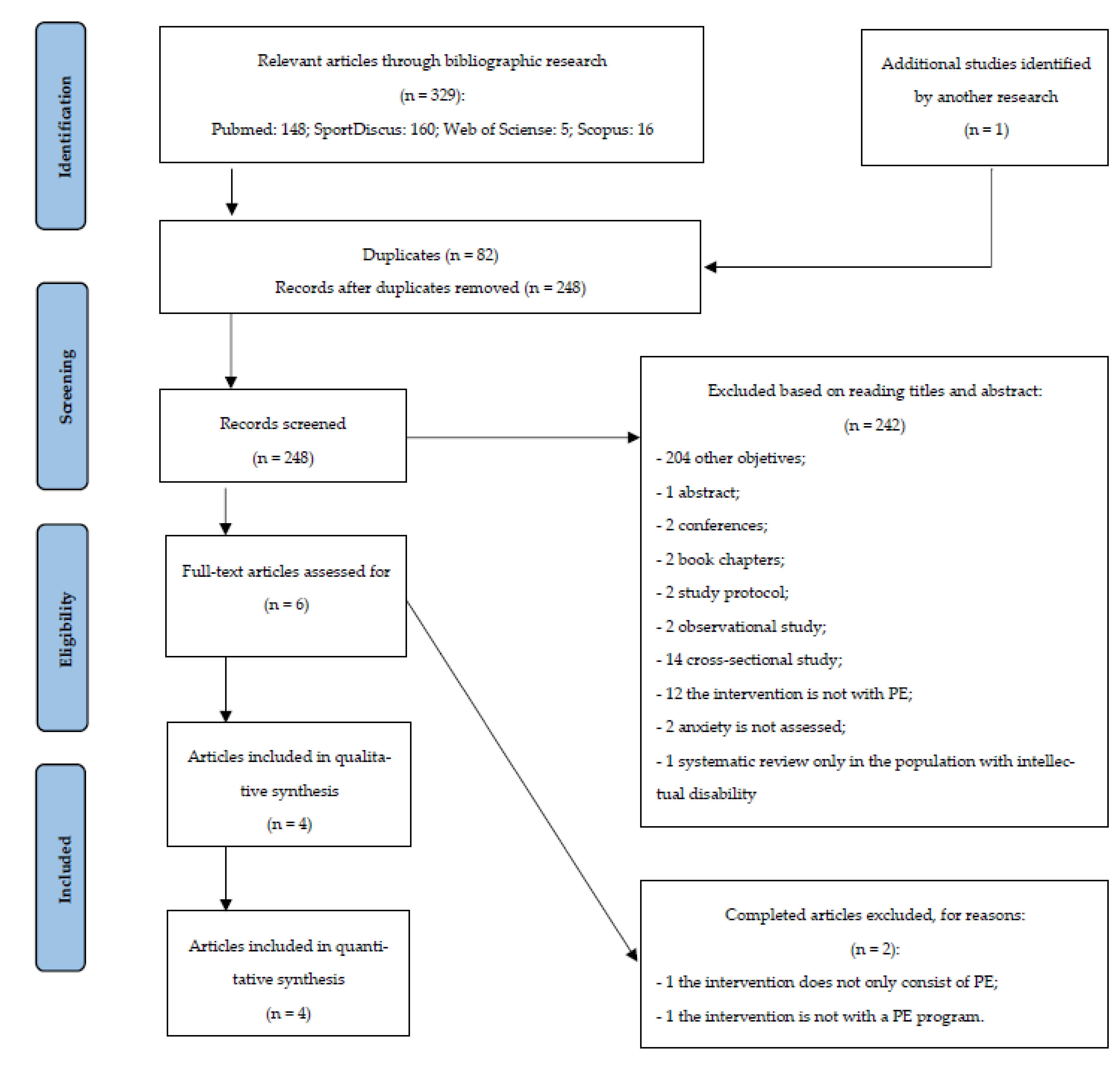
3.1. Selection of Studies
| Author, Year, Country | Aims | Participants | Type of Study | Assessment Instruments/Technique | Duration/Frequency | Exercises and Intensity |
|---|---|---|---|---|---|---|
| Barak et al. [40] Israel | Effects of Boccia on psychosocial outcomes in persons with severe disabilities. | N = 43; AA: 45.60 ± 10.95 y;multiple disabilities. | (A) Competition boccia group without professional supervision (N = 9); (B) professionally supervised competition bocce (N = 7); (C) recreational/leisure bocce (N = 14); and (D) control (N = 13). | State–Trait Anxiety Inventory; State–Trait Anxiety and Trait Anxiety Scale (36–38)—self-reports. | 16 weeks; Groups A and B trained 3 × week; 90 min/session. | Groups A and B: Throwing balls to different targets; technical and tactical exercises; training and competition games. Groups A and B: Strength training (2 × week; 60 min/session). All groups participated in a rehabilitation program. Recreational participants were included in the training that emphasized tactics (2 × week), but not in the games and not in one specific training schedule. |
| Carraro and Gobbi [41] Italy | Investigating the effects of a 12-week exercise program on anxiety states in a group of adults with intellectual disability. | N = 27 (♂ = 16; ♀ = 11); AA: 40.1 ± 6.2 y;mild-to-moderate ID. | Experimental study; random groups: Training (N = 14) and control (N = 13). | Zung Self-Rating Anxiety Scale (Zung, 1971)—self-completion scale adapted for DID (Lindsay & Michie, 1988); Trace State Anxiety Inventory Form Y (STAI-Y (Spielberg, 1989)—self-completed; | 12 weeks; 2 × week; 60 min/session. | Individual or paired movements using different equipment (balls, ropes, dumbbells, etc.), group cooperative situations, and adapted games. |
| Hardoy et al. [42] Italy | Evaluating the efficacy of an introductory mini tennis program as a therapeutic aid in the psychosocial rehabilitation of participants affected by mild-to-moderate ID. | N = 24; AA: 27.25 ± 8.45 y; mild ID. | Non-randomized controlled experimental study; division of groups: Training (N = 12) and control (N = 12). | Assessment and Information Rating Profile—anxiety subscale (Bouras, N. and Drummond, C. 1989) | 24 weeks; 2 × week; 180 min/session. | Phase-divided PE program: 1st phase: Exercises to familiarize participants with equipment (ball, wooden paddles, and racket); 2nd phase: Development of coordination skills (oculo-manual, general dynamics, and temporal-spatial skills); 3rd phase: Learning basic tennis techniques. |
| Salehpoor et al. [43] Iran | Investigating the effect of exercise on the anxiety of adolescents with intellectual disabilities. | N = 30 ♀; A: 15–21 y; mild ID. | Quasi-experimental study; random groups: Training (N = 15) and control (N = 15). | Zung Self-Rating Anxiety Scale (1997)—self-completion. | 8 weeks; 3 × week; 60 min/session. | Rhythmic aerobic exercises were performed (20 min); strength exercises (20 min)—exercise with dumbbells, ropes, and balls. |
3.2. Origin
3.3. Participants
3.4. Assessment Instruments/Technique
3.5. PE Program
3.6. Quality of Studies
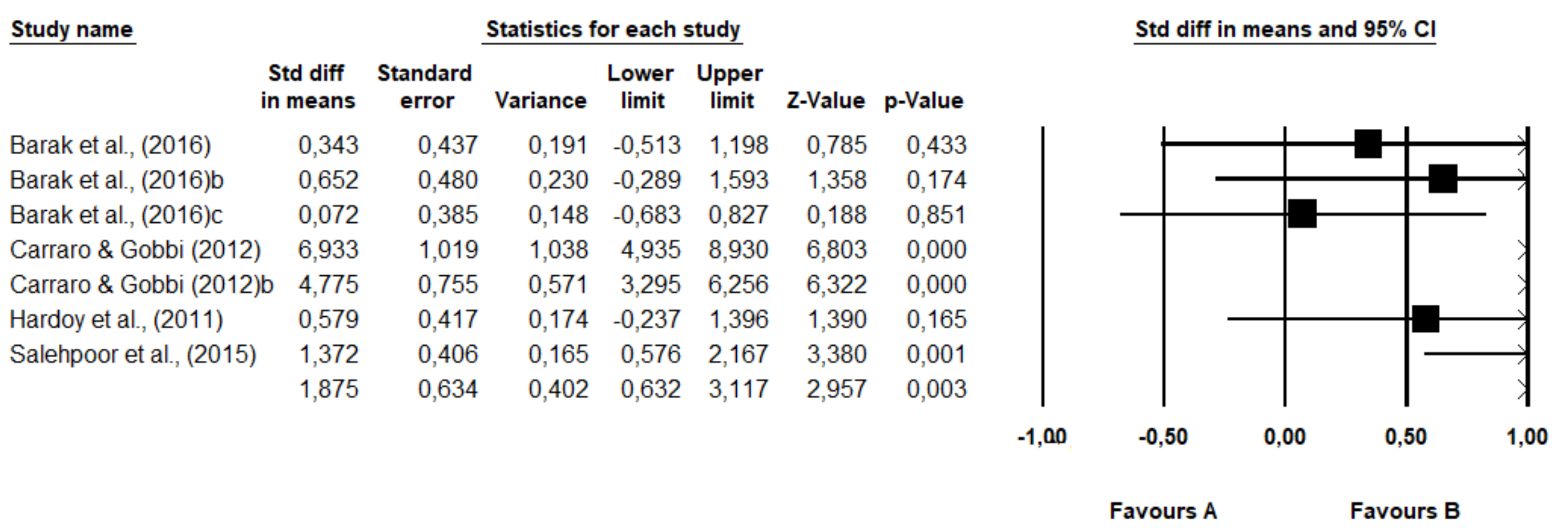
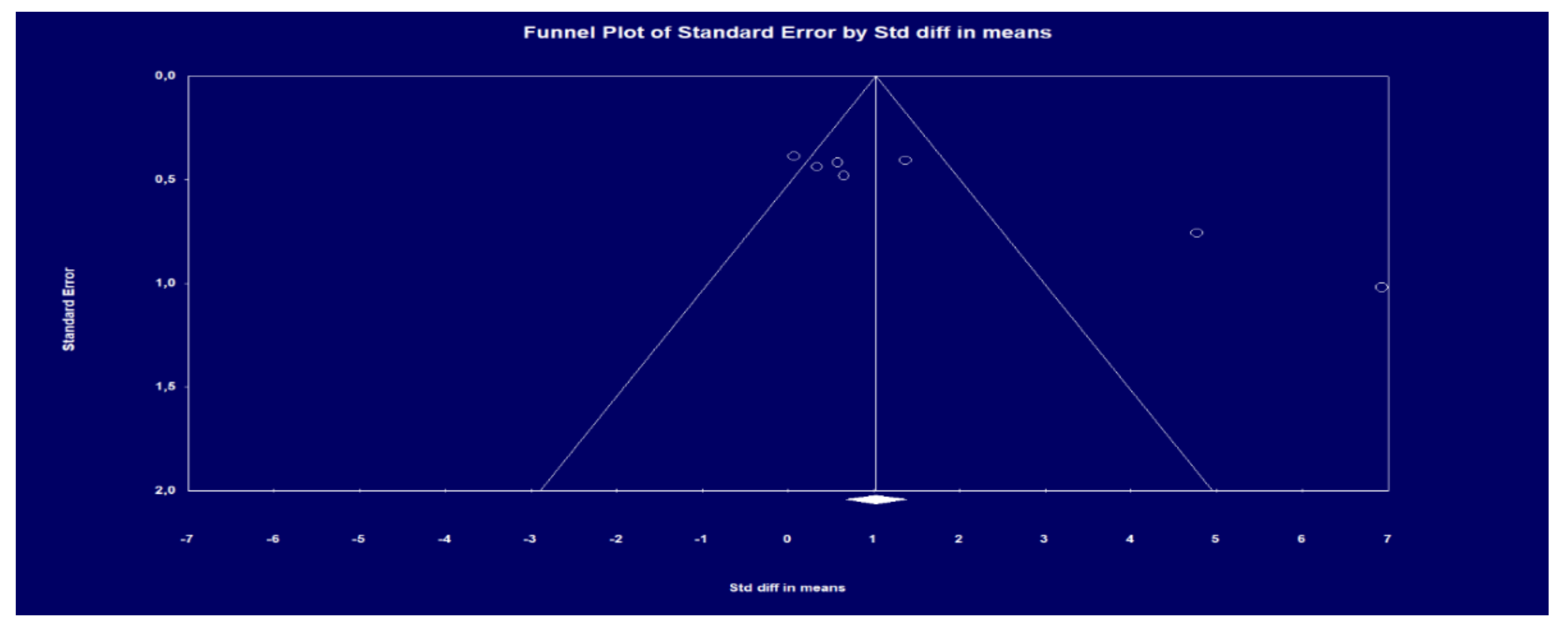
3.7. Results of the Interventions
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (DSM–5); American Psychiatric Association: Washington DC, USA, 2013.
- Simpson, H.; Neria, Y.; Lewis-Fernández, R.; Schneier, F. Anxiety Disorders: Theory, Research and Clinical Perspectives; Cambridge University Press: New York, NY, USA, 2010. [Google Scholar]
- Kessler, R.C.; Aguilar-Gaxiola, S.; Alonso, J.; Chatterji, S.; Lee, S.; Ormel, J.; Ustün, T.B.; Wang, P.S. The global burden of mental disorders: An update from the WHO World Mental Health (WMH) surveys. Epidemiol. Psichiatr. Soc. 2009, 18, 23–33. [Google Scholar] [CrossRef]
- Whiteford, H.A.; Ferrari, A.J.; Degenhardt, L.; Feigin, V.; Vos, T. The Global Burden of Mental, Neurological and Substance Use Disorders: An Analysis from the Global Burden of Disease Study 2010. PLoS ONE 2015, 10, e0116820. [Google Scholar] [CrossRef] [PubMed]
- Wittchen, H.U.; Jacobi, F.; Rehm, J.; Gustavsson, A.; Svensson, M.; Jönsson, B.; Olesen, J.; Allgulander, C.; Alonso, J.; Faravelli, C.; et al. The size and burden of mental disorders and other disorders of the brain in Europe 2010. Eur. Neuropsychopharmacol. 2011, 21, 655–679. [Google Scholar] [CrossRef] [PubMed]
- Remes, O.; Brayne, C.; Vander, L.R.; Lafortune, L. A systematic review of reviews on the prevalence of anxiety disorders in adult populations. Brain Behav. 2016, 6, e00497. [Google Scholar] [CrossRef] [PubMed]
- Maïano, C.; Coutu, S.; Tracey, D.; Bouchard, S.; Lepage, G.; Morin, A.J.S.; Moullec, G. Prevalence of anxiety and depressive disorders among youth with intellectual disabilities: A systematic review and meta-analysis. J. Affect. Disord 2018, 236, 230–242. [Google Scholar] [CrossRef]
- Binder, K.W.; Wrzesińska, M.A.; Kocur, J. Anxiety in persons with visual impairment. Psychiatr. Pol. 2020, 54, 279–288. [Google Scholar] [CrossRef] [PubMed]
- Shoham, N.; Lewis, G.; Favarato, G.; Cooper, C. Prevalence of anxiety disorders and symptoms in people with hearing impairment: A systematic review. Soc. Psychiatry Psychiatr. Epidemiol. 2019, 54, 649–660. [Google Scholar] [CrossRef] [PubMed]
- Jones, K.H.; Jones, P.A.; Middleton, R.M.; Ford, D.V.; Tuite-Dalton, K.; Lockhart-Jones, H.; Peng, J.; Lyons, R.A.; John, A.; Noble, J.G. Physical Disability, Anxiety and Depression in People with MS: An Internet-Based Survey via the UK MS Register. PLoS ONE 2014, 9, e104604. [Google Scholar] [CrossRef] [PubMed]
- Smith, K.J.; Peterson, M.D.; O’Connell, N.E.; Victor, C.; Liverani, S.; Anokye, N.; Ryan, J.M. Risk of Depression and Anxiety in Adults With Cerebral Palsy. JAMA Neurol. 2019, 76, 294–300. [Google Scholar] [CrossRef]
- Stein, M.B.; Roy-Byrne, P.P.; Craske, M.G.; Bystritsky, A.; Sullivan, G.; Pyne, J.M.; Katon, W.; Sherbourne, C.D. Functional impact and health utility of anxiety disorders in primary care outpatients. Med. Care 2005, 43, 1164–1170. [Google Scholar] [CrossRef]
- Haller, H.; Cramer, H.; Lauche, R.; Gass, F.; Dobos, G.J. The prevalence and burden of subthreshold generalized anxiety disorder: A systematic review. BMC Psychiatry 2014, 14, 128. [Google Scholar] [CrossRef]
- Moser, D.K.; McKinley, S.; Riegel, B.; Doering, L.V.; Meischke, H.; Pelter, M.; Patricia, D.; Kathleen, D. Relationship of persistent symptoms of anxiety to morbidity and mortality outcomes in patients with coronary heart disease. Psychosom. Med. 2011, 73, 803–809. [Google Scholar] [CrossRef] [PubMed]
- Roest, A.M.; Martens, E.J.; de Jonge, P.; Denollet, J. Anxiety and Risk of Incident Coronary Heart Disease: A Meta-Analysis. JACC 2010, 56, 38–46. [Google Scholar] [CrossRef] [PubMed]
- Tolmunen, T.; Lehto, S.M.; Julkunen, J.; Hintikka, J.; Kauhanen, J. Trait anxiety and somatic concerns associate with increased mortality risk: A 23-year follow-up in aging men. Ann. Epidemiol. 2014, 24, 463–468. [Google Scholar] [CrossRef] [PubMed]
- Aylett, E.; Small, N.; Bower, P. Exercise in the treatment of clinical anxiety in general practice – A systematic review and meta-analysis. BMC Health Serv. Res. 2018, 18, 559. [Google Scholar] [CrossRef]
- Stonerock, G.L.; Hoffman, B.M.; Smith, P.J.; Blumenthal, J.A. Exercise as Treatment for Anxiety: Systematic Review and Analysis. Ann. Behav Med. 2015, 49, 542–556. [Google Scholar] [CrossRef] [PubMed]
- Caspersen, C.J.; Powell, K.E.; Christenson, G.M. Physical activity, exercise, and physical fitness: Definitions and distinctions for health-related research. Public Health Rep. 1985, 100, 126–131. [Google Scholar] [PubMed]
- Andermo, S.; Hallgren, M.; Nguyen, T.T.D.; Jonsson, S.; Petersen, S.; Friberg, M.; Romqvist, A.; Stubbs, B.; Elinder, L.S. School-related physical activity interventions and mental health among children: A systematic review and meta-analysis. Sports Med. Open 2020, 6, 25. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Ayllon, M.; Cadenas-Sánchez, C.; Estévez-López, F.; Muñoz, N.E.; Mora-Gonzalez, J.; Migueles, J.H.; García, P.M.; Henriksson, H.; Molina, A.M.; Vizcaíno, V.M.; et al. Role of Physical Activity and Sedentary Behavior in the Mental Health of Preschoolers, Children and Adolescents: A Systematic Review and Meta-Analysis. Sports Med. 2019, 49, 1383–1410. [Google Scholar] [CrossRef] [PubMed]
- Rosenbaum, S.; Tiedemann, A.; Sherrington, C.; Curtis, J.; Ward, P.B. Physical activity interventions for people with mental illness: A systematic review and meta-analysis. J. Clin. Psychiatry 2014, 75, 964–974. [Google Scholar] [CrossRef] [PubMed]
- Esquivel, G.; Díaz-Galvis, J.; Schruers, K.; Berlanga, C.; Lara-Muñoz, C.; Griez, E. Acute exercise reduces the effects of a 35% CO2 challenge in patients with panic disorder. J. Affect. Disord 2008, 107, 217–220. [Google Scholar] [CrossRef] [PubMed]
- Strickland, J.C.; Smith, M.A. The anxiolytic effects of resistance exercise. Front. Psychol. 2014, 5, 753. [Google Scholar] [CrossRef] [PubMed]
- De Moor, M.H.M.; Beem, A.L.; Stubbe, J.H.; Boomsma, D.I.; De Geus, E.J.C. Regular exercise, anxiety, depression and personality: A population-based study. Prev. Med. 2006, 42, 273–279. [Google Scholar] [CrossRef] [PubMed]
- Goodwin, R.D. Association between physical activity and mental disorders among adults in the United States. Prev. Med. 2003, 36, 698–703. [Google Scholar] [CrossRef]
- Jayakody, K.; Gunadasa, S.; Hosker, C. Exercise for anxiety disorders: Systematic review. Br. J. Sports Med. 2014, 48, 187–196. [Google Scholar] [CrossRef] [PubMed]
- Bartlo, P.; Klein, P.J. Physical activity benefits and needs in adults with intellectual disabilities: Systematic review of the literature. Am. J. Intellect Dev. Disabil 2011, 116, 220–232. [Google Scholar] [CrossRef] [PubMed]
- Kapsal, N.J.; Dicke, T.; Morin, A.J.S.; Vasconcellos, D.; Maïano, C.; Lee, J.; Lonsdale, C. Effects of Physical Activity on the Physical and Psychosocial Health of Youth With Intellectual Disabilities: A Systematic Review and Meta-Analysis. J. Phys. Act. Health 2019, 16, 1187–1195. [Google Scholar] [CrossRef] [PubMed]
- Priego Quesada, J.I.; Lucas-Cuevas, A.; Belloch, S.; Perez-Soriano, P. Effects of exercise in people with cerebral palsy. A review. J. Phys. Educ. Sport 2014, 14, 36–41. [Google Scholar]
- Sweeting, J.; Merom, D.; Astuti, P.A.S.; Antoun, M.; Edwards, K.; Ding, D. Physical activity interventions for adults who are visually impaired: A systematic review and meta-analysis. BMJ Open 2020, 10, e034036. [Google Scholar] [CrossRef]
- Schalock, R.; Verdugo, M. Handbook on Quality of Life for Human Service Practitioners; American Association on Mental Retardation: Washington DC, USA, 2002. [Google Scholar]
- Moher, D.; Shamseer, L.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A.; Group, P.P. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 2015, 4, 1. [Google Scholar] [CrossRef]
- Bento, T. Revisões sistemáticas em desporto e saúde: Orientações para o planeamento, elaboração, redação e avaliação. Motricidade 2014, 10, 107–123. [Google Scholar] [CrossRef]
- Methley, A.M.; Campbell, S.; Chew-Graham, C.; McNally, R.; Cheraghi-Sohi, S. PICO, PICOS and SPIDER: A comparison study of specificity and sensitivity in three search tools for qualitative systematic reviews. BMC Health Serv. Res. 2014, 14, 579. [Google Scholar] [CrossRef] [PubMed]
- Nang, C.; Piano, B.; Lewis, A.; Lycett, K.; Woodhouse, M. Using The PICOS Model To Design And Conduct A Systematic Search: A Speech Pathology Case Study; Edith Cowan University: Perth, Australia, 2015. [Google Scholar]
- Downs, S.H.; Black, N. The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. J. Epidemiol. Community Health 1998, 52, 377–384. [Google Scholar] [CrossRef] [PubMed]
- Egger, M.; Smith, G.D.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.; Altman, D.G. Assessing Risk of Bias in Included Studies. In Cochrane Handbook for Systematic Reviews of Interventions; Higgins, J.P.T., Altman, D.G., Sterne, J.A.C., Eds.; John Wiley & Sons: Chichester, UK, 2019. [Google Scholar]
- Barak, S.; Mendoza-Laiz, N.; Fuentes, M.T.G.; Rubiera, M.; Huyzler, Y. Psychosocial effects of competitive Boccia program in persons with severe chronic disability. J. Rehabil Res. Dev. 2016, 53, 973–988. [Google Scholar] [CrossRef] [PubMed]
- Carraro, A.; Gobbi, E. Effects of an exercise programme on anxiety in adults with intellectual disabilities. Res. Dev. Disabil 2012, 33, 1221–1226. [Google Scholar] [CrossRef] [PubMed]
- Hardoy, M.C.; Seruis, M.L.; Floris, F.; Sancassiani, F.; Moro, M.F.; Mellino, G.; Lecca, M.E.; Adamo, S.; Carta, M.G. Benefits of Exercise with Mini Tennis in Intellectual Disabilities: Effects on Body Image and Psychopathology. Clin. Pract. Epidemiol. Ment. Health 2011, 7, 157–160. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Salehpoor, M.; Salesi, M.; Hemati Alamdarloo, G. The Effect of Exercise on Anxiety of Adolescents with Intellectual Disability. Phys. Treat. Specif. Phys. Ther. J. 2015, 5, 25–32. [Google Scholar]
| Research Number | Descriptors |
|---|---|
| 1 | (“brain palsy” OR “motor disability” OR “physical disability” OR “vision impairment” OR “visual impairment” OR “vision disability” OR “intellectual disability” OR “mental retardation” OR “intellectual disabilities” OR “hearing impairment” OR “hearing disability” OR “multiple disabilities”) AND (“physical activity” OR “exercise” OR sport* OR “training”) AND (“anxiety” OR “phobia” OR “panic”) |
| Intervention Group | Control Group | Methodological Quality | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Pre-Test | Post-Test | Pre-Test | Post-Test | |||||||
| Barak et al. [40] | Assessment instruments/technique | Intervention A | Intervention B | Intervention C | Intervention A | Intervention B | Intervention C | 25.76 ± 10.34 | 25.25 ± 10.90 | Poor |
| Anxiety State | 23.55 ± 5.38 | 27.00 ± 10.27 | 30.07 ± 4.61 | 20.55 ± 7.69 | 21.28 ± 5.82 | 30.07 ± 7.93 | ||||
| Trait Anxiety | 24.44 ± 8.95 | 26.00 ± 10.68 | 30.50 ± 5.01 | NE | 25.38 ± 10.35 | NE | ||||
| Carraro and Gobbi [41] | Trait Anxiety | 59.9 ± 2.9 | 38.1 ± 2.5 | 59.8 ± 4.3 | 57.2 ± 4.3 | Good | ||||
| Zung Self-Rating Anxiety Scale | 33.86 ± 1.99 | 25.00 ± 1.62 | 33.46 ± 1.94 | 31.62 ± 1.94 | ||||||
| Hardoy et al. [42] | Assessment and Information Rating Profile Anxiety Subscale | 3.2 ± 1.8 | 2.3 ± 1.3 | 2.8 ± 2.3 | 2.8 ± 2.3 | Fair | ||||
| Salehpoor et al. [43] | Zung’s Anxiety Scale (1997) | 43.15 ± 0.96 | 36.60 ± 1.10 | 43.75 ± 1.19 | 45.91 ± 1.46 | Good | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jacinto, M.; Frontini, R.; Matos, R.; Antunes, R. Effects of Exercise Programs on Anxiety in Individuals with Disabilities: A Systematic Review with a Meta-Analysis. Healthcare 2021, 9, 1047. https://doi.org/10.3390/healthcare9081047
Jacinto M, Frontini R, Matos R, Antunes R. Effects of Exercise Programs on Anxiety in Individuals with Disabilities: A Systematic Review with a Meta-Analysis. Healthcare. 2021; 9(8):1047. https://doi.org/10.3390/healthcare9081047
Chicago/Turabian StyleJacinto, Miguel, Roberta Frontini, Rui Matos, and Raul Antunes. 2021. "Effects of Exercise Programs on Anxiety in Individuals with Disabilities: A Systematic Review with a Meta-Analysis" Healthcare 9, no. 8: 1047. https://doi.org/10.3390/healthcare9081047
APA StyleJacinto, M., Frontini, R., Matos, R., & Antunes, R. (2021). Effects of Exercise Programs on Anxiety in Individuals with Disabilities: A Systematic Review with a Meta-Analysis. Healthcare, 9(8), 1047. https://doi.org/10.3390/healthcare9081047








