Assessing the Impact of a Global Health Fellowship on Pharmacists’ Leadership Skills and Consideration of Benefits to the National Health Service (NHS) in the United Kingdom
Abstract
:1. Introduction
1.1. A Health Partnerships Approach to Supporting Antimicrobial Stewardship in Four African Countries: The Commonwealth Partnerships for Antimicrobial Stewardship (CwPAMS)
1.2. Pharmacy Leaders and the NHS
1.3. Chief Pharmaceutical Officer’s Global Health (CPhOGH) Fellowship Programme
2. Materials and Methods
2.1. Pre- and Post-Fellowship Self-Assessment by Fellows
2.2. Assessment by Senior Colleagues
- Teamwork;
- Influencing for results;
- Vision, Motivation and capability;
- Inspiring shared purpose;
- Managing change;
- Innovative working and practice.
2.3. Distribution of Questionnaires
2.4. Data about Contributions, Achievements, and Communications of CPhOGH Fellows
2.5. Data Analysis
3. Results
3.1. CPhOGH Fellows
3.2. Self-Assessment
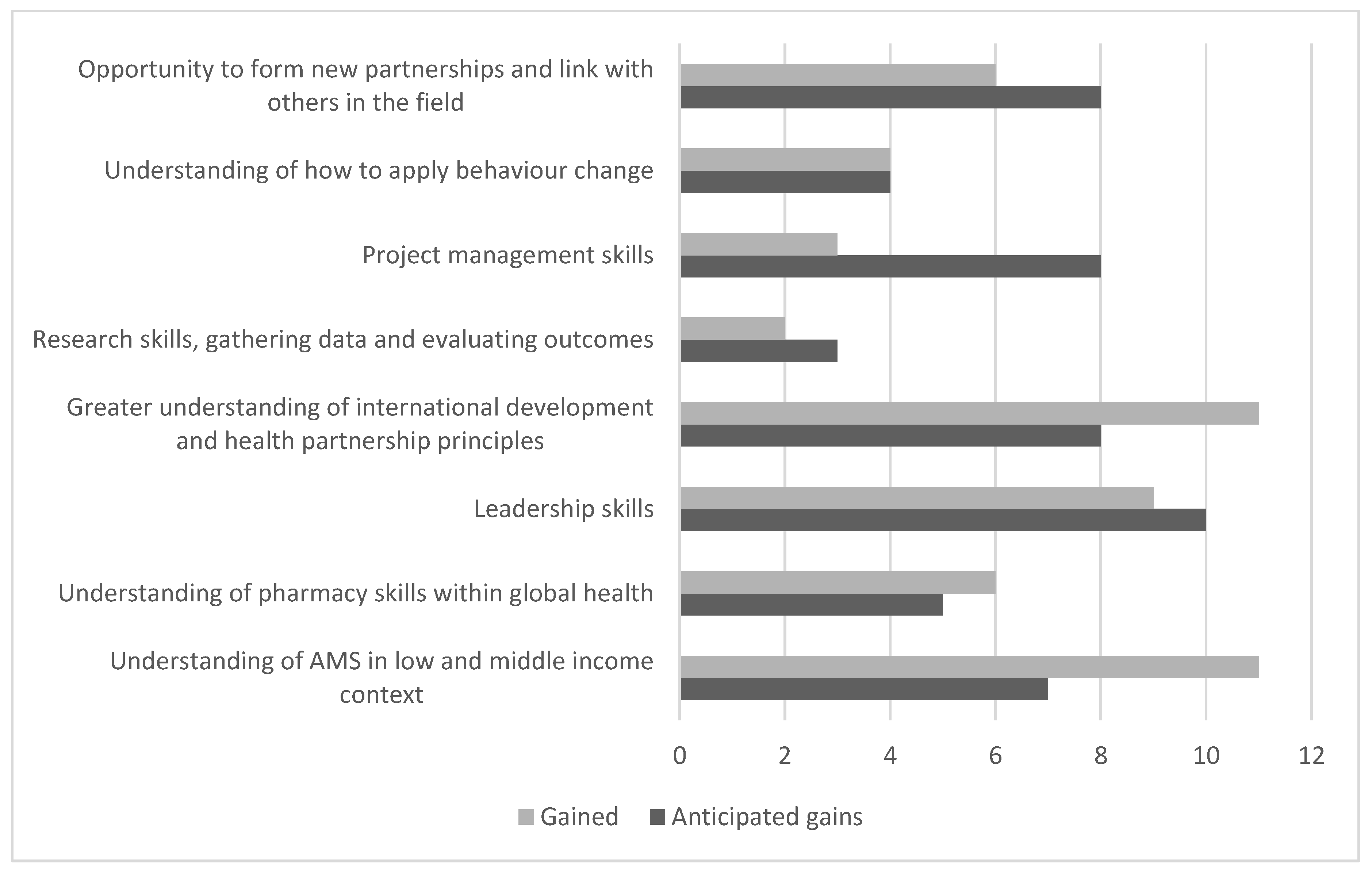
3.2.1. Expected Goals of the Fellowship Year
“Vastly useful and applicable. I feel I learned more than I taught during my visit! Although I do believe we made a difference for our partnership as well.”
“I have gained more skills and knowledge than I anticipated through the Fellowship”.
“Will enable me to confidently apply for funding for future projects.”
3.2.2. Measuring the Outcomes of Volunteering for Education Tool (MOVE-iT)
3.2.3. Leadership Development, Experience, and Knowledge
“I have been able to apply aspects of the leadership skills and knowledge I gained through undertaking the Fellowship to facilitate antimicrobial stewardship work streams which are important to my organisation.”
“I have definitely applied the leadership skills learnt through the facilitator study days…. I have also learnt the importance of reflection when things do not always go to plan. I have learnt new ways to deal with conflict which has helped my personal development and ensure that I am able to work effectively.”
“I have adapted the flow of work in our team, I am more able to delegate tasks and together we regularly discuss our roles and responsibilities, which has made us more productive as a team.”
“I felt the Fellowship has been worthwhile because it introduced me to the leadership course and a tool for me to assess my own leadership skills, identify my gap and act on it.”
“I have become involved in a research project with health psychologists teaching AMS and behaviour change. I never would have imagined doing this prior to the Fellowship!”
“Engagement of the NHS with higher education institutions and improved understanding and participation in research.”
3.3. Assessment by Senior Colleagues
3.4. Impact of the CPhOGH Fellowship on the Performance of Participating Pharmacists from a Senior Perspective
“Professionally the Fellow is more confident, able to allow their voice to be heard. The Fellow has developed their ability to manage change and people skills and works confidently within wider teams.”
“Professionally the Fellow is more confident, more strategic in their thoughts and planning, ambitious and excited for improvement. The Fellow has developed their networks extensively, working across networks globally with ease.”
“Increased confidence in ability to adapt to new situations and different environments. Ability to manage stressful situations and turn them to an advantage.”
“Confidence, ability to think outside the box and use successful techniques in a different context.”
“It has been a pleasure to watch the Fellow grow during the year and overall, this programme has been a positive influence on the department as a whole.”
3.5. Contributions, Achievements and Communications
4. Discussion
5. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Global Action Plan on Antimicrobial Resistance. Available online: https://apps.who.int/iris/bitstream/handle/10665/193736/9789241509763_eng.pdf?sequence=1 (accessed on 21 August 2020).
- Department of Health and Social Care. Tackling Antimicrobial Resistance 2019–2024. The UK’s Five-Year National Action Plan, HM Government. 24 January 2019. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/784894/UK_AMR_5_year_national_action_plan.pdf (accessed on 21 August 2020).
- Department of Health and Social Care. Contained and Controlled. The UK’s 20-Year Vision for Antimicrobial Resistance, HM Government. 24 January 2019. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/773065/uk-20-year-vision-for-antimicrobial-resistance.pdf (accessed on 21 August 2020).
- National Health Service. Long Term Plan, Updated 21 August 2019. Available online: https://www.longtermplan.nhs.uk/wp-content/uploads/2019/08/nhs-long-term-plan-version-1.2.pdf (accessed on 21 August 2020).
- Hand, K. Antibiotic pharmacists in the ascendancy. J. Antimicrob. Chemother. 2007, 60, i73–i76. [Google Scholar] [CrossRef] [PubMed]
- Gilchrist, M.; Wade, P.; Ashiru-Oredope, D.; Howard, P.; Sneddon, J.; Whitney, L.; Wickens, H. Antimicrobial Stewardship from Policy to Practice: Experiences from UK Antimicrobial Pharmacists. Infect. Dis. Ther. 2015, 4, 51–64. [Google Scholar] [CrossRef] [Green Version]
- Commonwealth Partnerships for Antimicrobial Stewardship. Available online: https://commonwealthpharmacy.org/commonwealth-partnerships-for-antimicrobial-stewardship/ (accessed on 22 August 2020).
- Monkhouse, A.; Sadler, L.; Boyd, A.; Kitsell, F. The Improving Global Health Fellowship: A qualitative analysis of innovative leadership development for NHS healthcare professionals. Glob. Health 2018, 14, 69. [Google Scholar] [CrossRef]
- Tropical Health and Education Trust. Health Partnership Scheme Impact Report 2011–2019. Available online: https://www.thet.org/wp-content/uploads/2017/09/20443_HPS_Impact_Report-2019-8.pdf (accessed on 20 August 2020).
- Care Quality Commission; Public Health England; National Health Service. Five Year Forward View; NHS: England, UIK, 2015. Available online: https://www.england.nhs.uk/wp-content/uploads/2014/10/5yfv-web.pdf (accessed on 27 May 2021).
- Francis, R. Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry, Executive Summary. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/279124/0947.pdf (accessed on 23 March 2021).
- Department of Health. High-Quality Care for All: NHS Next Stage Review Final Report. CM 7432; The Stationary Office: London, UK, 2008. Available online: https://www.gov.uk/government/publications/high-quality-care-for-all-nhs-next-stage-review-final-report (accessed on 20 March 2020).
- Rose, L. Better Leadership for Tomorrow NHS Leadership Review. 2015. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/445738/Lord_Rose_NHS_Report_acc.pdf (accessed on 30 June 2021).
- Department of Health; NHS Improvement. Developing People—Improving Care. National Improvement and Leadership Development Board. Available online: https://improvement.nhs.uk/documents/542/Developing_People-Improving_Care-010216.pdf (accessed on 20 March 2021).
- Kline, R. Leadership in the NHS. BMJ Lead. 2019, 3, 129–132. [Google Scholar] [CrossRef]
- NHS Leadership Academy. Leadership Framework—A Summary. Available online: https://www.leadershipacademy.nhs.uk/wp-content/uploads/2012/11/NHSLeadership-Framework-LeadershipFramework-Summary.pdf (accessed on 18 March 2021).
- NHS Leadership Academy. Healthcare Leadership Model. In The Nine Dimensions of Leadership Behaviour; NHS Leadership Academy: England, UK, 2013. Available online: https://www.leadershipacademy.nhs.uk/wp-content/uploads/2014/10/NHSLeadership-LeadershipModel-colour.pdf (accessed on 21 August 2020).
- Royal Pharmaceutical Society. Leadership Development Framework. January 2015. Available online: https://www.rpharms.com/resources/frameworks/leadership-development-framework (accessed on 1 April 2021).
- Royal Pharmaceutical Society. The Pharmacy Contribution to Antimicrobial Stewardship. September 2017. Available online: https://www.rpharms.com/recognition/all-our-campaigns/policy-a-z/antimicrobial-stewardship (accessed on 1 April 2021).
- International Pharmaceutical Federation (FIP) Development Goals. 2020. Available online: https://www.fip.org/fip-development-goals (accessed on 20 May 2021).
- NHS Health Education England. Improving Global Health through Leadership. Development Programme. Available online: https://www.hee.nhs.uk/our-work/global-engagement/improving-global-health-through-leadership-development-programme-0 (accessed on 28 May 2021).
- Faculty of Medical Leadership and Management. Chief Pharmaceutical Officer’s Clinical Fellow Scheme. Available online: https://www.fmlm.ac.uk/CFS-pharmacy (accessed on 28 May 2021).
- Briggs, K.; Briggs Myers, I. The Myers-Briggs Type Indicator. 2015. Available online: https://www.myersbriggs.org/my-mbti-personality-type/mbti-basics/thinking-or-feeling.htm (accessed on 20 March 2021).
- NHS Leadership Academy. The Edward Jenner Programme. Available online: https://www.leadershipacademy.nhs.uk/programmes/the-edward-jenner-programme/ (accessed on 14 April 2021).
- Tyler, N.; Collares, C.; Byrne, G.; Byrne-Davis, L. Measuring the outcomes of volunteering for education: Development and pilot of a tool to assess healthcare professionals’ personal and professional development from international volunteering. BMJ Open 2019, 9, e028206. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bertrum, D. Likert Scales. Available online: http://poincare.matf.bg.ac.rs/~kristina/topic-dane-likert.pdf (accessed on 21 August 2020).
- Royal Pharmaceutical Society (RPS) Faculty Peer Assessment Tool. Available online: https://www.rpharms.com/development/credentialing/faculty/10-week-plan (accessed on 26 February 2020). Used with permission from the Royal Pharmaceutical Society.
- NHS Health Research Authority. Is My Study Research Decision Tool. Available online: http://www.hra-decisiontools.org.uk/research/result7.html (accessed on 16 June 2021).
- West, M.; Armit, K.; Loewenthal, L.; Eckert, R.; West, T.; Lee, A. Leadership and Leadership Development in Health Care. 2015. Available online: https://www.kingsfund.org.uk/sites/files/kf/field/field_publication_file/leadership-leadership-development-health-care-feb-2015.pdf (accessed on 24 May 2017).
- Kluger, A.N.; DeNisi, A. The effects of feedback interventions on performance: A historical review, a meta-analysis, and a preliminary feedback intervention theory. Psychol. Bull. 1996, 119, 254–284. [Google Scholar] [CrossRef]
- Seifert, C.F.; Yukl, G.; Mcdonald, R.A. Effects of multisource feedback and a feedback facilitator on the influence behavior of managers toward subordinates. J. Appl. Psychol. 2003, 88, 561–569. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- MacPhail, A.; Young, C.; Ibrahim, J.E. Workplace-based clinical leadership training increases willingness to lead. Leadersh. Health Serv. 2015, 28, 100–118. [Google Scholar] [CrossRef] [PubMed]
- Bhandari, A.; Wagner, T. Self-reported utilization of health care services: Improving measurement and accuracy. Med. Care Res. Rev. 2006, 63, 217–235. [Google Scholar] [CrossRef] [PubMed]
- Mianda, S.; Voce, A. Developing and evaluating clinical leadership interventions for frontline healthcare providers: A review of the literature. BMC Health Serv. Res. 2018, 18, 747. [Google Scholar] [CrossRef] [PubMed]
| Pre-Fellowship | Post-Fellowship | p-Values | |||||
|---|---|---|---|---|---|---|---|
| Mean | Median | Standard Deviation | Mean | Median | Standard Deviation | ||
| Confidence | 53.31 | 52 | 6.23 | 58.69 | 61 | 4.81 | 0.001 |
| Teaching | 17.31 | 18.5 | 2.75 | 19.13 | 19 | 1.89 | 0.012 |
| Behaviour change | 19.31 | 19 | 5.50 | 22.88 | 24.5 | 5.56 | <0.001 |
| Management | 17.50 | 18 | 3.39 | 19.81 | 21 | 1.83 | 0.003 |
| Attitude to work | 35.81 | 36 | 3.56 | 38.00 | 37 | 3.41 | 0.064 |
| Difficult communication | 15.00 | 15 | 4.07 | 18.44 | 18.5 | 2.99 | 0.006 |
| Activities | Pre CPhOGH (n = 15) | Post CPhOGH (n = 16) | ||||
|---|---|---|---|---|---|---|
| Yes | No | Yes (through Fellowship) | Yes (Alternative Route) | No | Not Answered | |
| 360 Assessment Questionnaire | 4 | 11 | 7 | 3 | 6 | |
| NHS Healthcare Leadership Model Self-Assessment | 2 | 13 | 15 | 1 | ||
| Other leadership self-assessment | 5 | 10 | 7 | 1 | 5 | 3 |
| Project Management Course | 6 | 9 | 10 | 6 | ||
| Myers–Briggs Type Indicator questionnaire | 8 | 7 | 15 | 1 | ||
| Other personality type indicator questionnaire | 5 | 10 | 2 | 3 | 11 | |
| A formal/semi-formal discussion with a mentor for your professional activities | 5 | 10 | 16 | |||
| Written a project plan | 10 | 5 | 15 | 1 | ||
| Formally led a project or project deliverable | 11 | 4 | 15 | 1 | ||
| Led a quality improvement project | 10 | 5 | 7 | 4 | 5 | |
| Activities Undertaken for the Last 12 Months (June 2019–June 2020) | N = 16 (New Experience) |
|---|---|
| Publication/presentation of work at a conference | 12 (3) |
| Publication of work for a journal | 9 (3) |
| Publication/presentation of work within Trust setting | 13 (3) |
| Promotion of work on social media | 11 (6) |
| Collaboration on work within Trust | 13 (2) |
| Collaboration on work at a regional/local level (outside Trust) | 12 (3) |
| Collaboration on work at a national level | 13 (7) |
| Collaboration on work at an international level | 13 (7) |
| Utilised a mentor | 15 (8) |
| Become a mentor | 6 (4) |
| Changed job role | 7 |
| Had a promotion | 5 |
| Undertaken Faculty assessment | 4 (1) |
| Written a business case | 7 (1) |
| Undertaken an audit | 14 |
| Undertaken a project with a focus on quality improvement | 12 (1) |
| Undertaken teaching | 16 |
| Enrolled or undertaken a leadership course | 14 (9) |
| Reflecting between June 2019–June 2020 State How Much You Agree with the Following Statement (n = 16) | Strongly Agree/Agree | Somewhat Agree | Neutral | SomewhatDisagree | Strongly Disagree/Disagree |
|---|---|---|---|---|---|
| I undertake more MDT work compared to a year ago. | 7 | 2 | 4 | 1 | 2 |
| I am more likely to work with other disciplines on a regular basis | 8 | 3 | 3 | 2 | |
| I have worked across disciplines in delivering AMS/IPC | 14 | 1 | 1 | ||
| I find myself working more with different professional groups | 11 | 2 | 1 | 2 | |
| I am more confident to approach people I have never worked with before compared to a year ago | 14 | 1 | 1 | ||
| I am happy to work with/approach people who work outside the NHS in order to collaborate compared to a year ago. | 14 | 1 | 1 | ||
| I have started managing a new aspect of service. | 10 | 2 | 2 | 2 | |
| I recognise the need to review/manage /introduce a new aspect of service. | 12 | 2 | 1 | 1 | |
| I have become more involved in research. | 7 | 3 | 2 | 1 | 3 |
| I have made changes to the way in which I work as a team | 12 | 3 | 1 | ||
| I have made changes to the way in which I engage with others in the work environment. | 13 | 3 | |||
| I have made changes to the way in which I teach | 13 | 2 | 1 | ||
| I have made changes to the way in which I engage with the wider Trust/ organisation. | 10 | 1 | 2 | 3 | |
| I have made changes to the way I practice. | 13 | 1 | 1 | 1 | |
| I have made changes to the way in which I engage with others outside a work environment. | 12 | 2 | 1 | 1 |
| Themes from Open Questions | Selected Quotes |
|---|---|
| Career development In addition to the seven CPhOGH Fellows who reported a change in job role and the five CPhOGH Fellows who reported a promotion (Table 3), the written feedback supports improved development and professional progression through the experiences of the Fellowship programme. | “It has also given me the confidence to apply for a managerial role, I wouldn’t have considered only months before.” “I have had opportunities e.g. projects with significant budgets which I believe I may not have been offered if it weren’t for the Fellowship” “The Fellowship has empowered me to push myself further and broaden my horizons.” “It has provided me with the tools for the next stage of my pharmacy career.” “Lots of experiences during the last year motivated me to change role. Fellowship was one of them.” |
| Job satisfaction/motivation The results of the MOVE-iT tool, shown in Table 1, do not indicate a significant change in attitude to work. However, the following statements suggest improved job satisfaction, pro-active working and motivation. | “Improvements in staff happiness and retention.” “Increased confidence. Increased motivation” “The Fellowship has given me another focus and has improved my motivation and job satisfaction in my role.” “I’ve expanded my goals and through the support of my peers and Fellows I have achieved things I would never have dreamed of 18 months ago.” “The CwPAMs projects and CPhOGH Fellowship has offered unique opportunities for us which have been very enjoyable. They have encouraged me to work hard and with more enthusiasm than before and I feel very happy and proud to work within the pharmacy profession.” |
| Communication skills Improvements in managing challenging conversations and difficult people were reported in the post-CPhOGH Fellows MOVE-iT survey when compared to the baseline (Table 1). This is further substantiated by the following: | “My improved negotiation and communication skills, especially in tricky circumstances” “The coaching on the Fellowship weekend really allowed me to explore this in a safe environment and practice difficult conversations” “Coaching course delivered on the Fellowship weekend. This was amazing and has really improved my confidence and communication style.” “I have learnt new ways to deal with conflict which has helped my personal development and ensure that I am able to work effectively.” |
| Networking Collaboration within Trusts, at a regional, national and international level, was reported by the majority of CPhOGH Fellows (Table 3). Stronger and more cohesive networks were developed locally as illustrated. Collaborations across sectors and specialties and outside the NHS were also fostered as described in Table 4 and by these CPhOGH Fellows: | “The networks I have made also were useful in other areas of healthcare. Such as project plans for in house service development.” “Wider network which I can call on to enhance what we are doing at work.” “felt more empowered to work differently and innovatively within and outside our organisation.” “It has connected me to inspiring and like-minded colleagues who all have a passion for improving global health in particular focusing on AMR.” “I feel more confident to network now and have learnt a huge amount from positive role models outside of healthcare.” “Greater collaboration. I have paired up the Uganda researchers with colleagues in South Africa to write a grant proposal.” “Improved ability of staff involved to work beyond the traditional boundaries and to consider how collaborative efforts can provide further benefits to all.” |
| Global Health and Frugal Innovation/Working with limited resources The CPhOGH Fellows demonstrated a greater ability to work within the confines of limited resources as indicated by the greater agreement with the statements in the MOVE-iT (Table 1). Examples of benefits of this in the UK setting are illustrated here: | “In addition, having increased understanding of the global health context has helped me believe that anything is achievable with the resources in the UK, you just need the will to make change.” “Ability to produce outcomes and results in a very resource limited setting” “Greater awareness of how LMIC institutions are run and how cohesive relations are built. This is something that can benefit NHS organisations” “More appreciation of what the NHS has to offer (as a patient and an employee) and how improvements do not always require money and more often, a better understanding of how things actually work in practice.” “The opportunity to participate in the CwPAMs project and the CPhOGH Fellowship has been eye opening. I have learnt how to improvise and find solution despite limited resources. I also learnt to be more adaptive to the environment and change way of working depending on the local context. This has been very useful given the COVID-19 pandemic.” “It has been worthwhile, as it has given me greater exposure to the way in which a pharmacists role can be done even with great lack of resource. It has shown me how when undertaking the role of a leader you are able to accomplish a lot, despite any challenges.” |
| Education and training All CPhOGH Fellows considered education and training to be part of their job roles prior to the Fellowship and CwPAMS experiences (Table 3). However, improvements in confidence and adaptation of teaching methods, including the use of behaviour change techniques, were reported by the majority of CPhOGH Fellows (Table 1 and Table 4). Delivery and provision of education and training was also reported to be further reaching. This is highlighted here: | “The key benefits to my trust is the Fellowship has changed the way we conduct education and training through the introduction of behaviour change.” “…. link with partnership and UK local university school of pharmacy to support overseas opportunities for undergraduate programme” “Far greater understanding of requirements to deliver high quality education at scale” “Together with colleagues in Uganda we developed a MOOC that has been accessed in 50 countries by over 2000 learners on AMS.” “education strategies have changed to move away from didactic teaching to more workshop type training and in addition our work has made the team more visible in the trust. It also has embedded AMS into the long-term strategy of all areas.” |
| Resilience When the CPhOGH Fellows were asked how they believed they had coped with the COVID-19 pandemic in April and May 2020, five answered extremely well, seven answered very well and three answered somewhat well. One CPhOGH Fellow did not respond. For some CPhOGH Fellows, they reported that they used their experiences of working in new and uncertain areas during their CwPAMS placements to be helpful: | “ a better sense of self-awareness (after a lot of reading/research into this area, borne from the Fellowship study days)” “I built upon my experience in my new role and also the increased leadership skills I have been building on during the Fellowship which helped me to cope when I was redeployed to a clinical role during COVID.” Others considered perspective of the situation to be important and utilised the leadership and educational skills they had developed: “I think the experiences of the past year have helped in dealing with the COVID19 emergency response and this has put into context what is important in life.” “Positive outlook. Good communication. Open teamwork. Task delegation. Feeling prepared by having additional teaching.” “I was re-deployed to support a clinical research team and having international experience…during the Fellowship and working with and managing international teams helped me cope with being in a new environment and responding to new and as yet unknown research needs and questions.” “Leadership demonstrated by caring for my colleagues and my team’s mental health and wellbeing. I take the time to listen and be there for colleagues, despite my very busy schedule.” |
| Statement | Pre CPhOGH (n = 25) | Post CPhOGH (n = 26) | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Essential | Proficient | Strong | Exceptional | U/C* | Essential | Proficient | Strong | Exceptional | U/C* | |
| Teamwork | ||||||||||
| The pharmacist listens attentively to other team members and values their suggestions | 3 | 17 | 5 | 1 | 10 | 15 | ||||
| The pharmacist is an established and effective member of a multidisciplinary team | 2 | 4 | 15 | 4 | 1 | 10 | 15 | |||
| The pharmacist is consulted for advice which requires their in-depth professional expertise | 1 | 6 | 12 | 6 | 10 | 16 | ||||
| The pharmacist consistently works effectively across boundaries to build relationships and share information, plans and resources. | 2 | 6 | 9 | 7 | 1 | 1 | 5 | 19 | 1 | |
| U/C* Unable to comment | ||||||||||
| Supporting quotes “…. ability to network and be collegiate widens the scope and impact of Fellow work, and the Fellow is fundamental in keeping our team connected and on task.” “Their positive, "can-do" attitude and unrelenting support for ALL members of the team means you can face any challenge with them!” “The Fellow is a core member of and contributor to the Antimicrobial Stewardship Committee…. developed strong working relationships with clinicians, pharmacists and specialist nurses in both hospital and community settings…. taken an active leadership role in the Trust response to COVID-19 working across site and specialities.” “The Fellow has always been strong team player and has developed strong networks…sought for expert clinical advice at a National level” | ||||||||||
| Influencing for Results | ||||||||||
| The pharmacist is able to share issues and information to help others understand his/her point of view | 1 | 11 | 8 | 5 | 3 | 11 | 12 | |||
| The pharmacist tailors his/her communication group or presentation according to the audience or stakeholder. | 4 | 8 | 9 | 3 | 1 | 2 | 14 | 10 | ||
| The pharmacist directly or indirectly links different working groups across the organisation to achieve a common goal. | 3 | 7 | 9 | 5 | 1 | 6 | 9 | 11 | ||
| The pharmacist gains reputational influence by sharing experience and best practice nationally | 3 | 5 | 10 | 4 | 3 | 5 | 6 | 14 | 1 | |
| U/C* Unable to comment | ||||||||||
| Supporting quotes “The Fellow is able to communicate and build relationships with anyone, irrespective of position or background. They have been proactive in sharing theirs and the team’s work both locally and at conferences.” “The Fellow has worked hard to establish their place in the team with confidence, they now have a much stronger voice in our QI huddles and across the department” “As Lead Antimicrobial Pharmacist the Fellow has to communicate with a variety of professionals in a number of different settings, all of whom may have differing agendas e.g. harmonisation of antimicrobial guidelines following the merger of two large hospital Trusts….has spoken at national conferences and set up a professional Twitter account for dissemination and sharing of information and networking.” | ||||||||||
| Vision, Motivation and Developing Capability | ||||||||||
| The pharmacist creates a clear vision of the future for his/ her team in accordance with the organisations vision. | 3 | 12 | 7 | 3 | 1 | 3 | 11 | 11 | ||
| The pharmacist often looks for opportunities to develop him/herself and learn things outside his/her comfort zone. | 2 | 11 | 9 | 3 | 3 | 9 | 14 | |||
| The pharmacist often provides constructive feedback to his/her team to help them focus on the right area in order to develop professionally | 4 | 6 | 6 | 3 | 6 | 1 | 6 | 8 | 6 | 5 |
| The pharmacist is involved in strategy planning | 4 | 7 | 9 | 2 | 3 | 2 | 4 | 11 | 8 | 1 |
| U/C* Unable to comment | ||||||||||
| Supporting quotes “The Fellow sees the bigger picture but is also able to hone in on the key steps required to implement change and is detail-orientated when it is appropriate.” “very sensible and objective in discussions, also very good at providing feedback, identifying colleagues who need support and providing help to the best of their abilities.” “The Fellow has taken on the responsibility of being a diploma tutor…….and also actively engages with other diploma students and gives constructive and positive development suggestions.” “Lead role in development of Antimicrobial Stewardship strategy…. involvement in Trust Infection Service strategy working group” “The Fellow has been pivotal in planning the next steps of the project and disseminating the links work at a national level” | ||||||||||
| Inspiring shared purpose | ||||||||||
| The pharmacist demonstrates the characteristics of a role model of the Pharmacy profession. | 1 | 4 | 12 | 6 | 2 | 9 | 16 | 1 | ||
| The pharmacist inspires others, even when they are under pressure, by helping them to focus on the value of their contribution | 1 | 10 | 8 | 6 | 3 | 10 | 13 | |||
| The pharmacist supports his/her colleagues to keep challenging others cohesively to achieve a shared purpose. | 1 | 10 | 9 | 5 | 3 | 12 | 11 | |||
| U/C* Unable to comment | ||||||||||
| Supporting quotes “The Fellow is supportive, encouraging and inspiring in their enthusiasm, drive and outlook.” “The Fellow responded positively to the COVID crisis, showing calm yet strong leadership for the staff delivering clinical services to ward areas.” “The Fellow has managed the recent changes in working due to COVID-19 with grace and understanding…been a role model to their colleagues. Fellow has forged strong links with psychology colleagues at the university to provide behaviour change education to Stewardship Committee members and regularly demonstrates what they has learned from these sessions in leadership role.” | ||||||||||
| Managing Change | ||||||||||
| The pharmacist is able to adapt to different way of working especially in times of crisis | 1 | 8 | 11 | 3 | 2 | 10 | 15 | 1 | ||
| The pharmacist consistently reflects on his/ her service and manages processes of change or service improvement | 4 | 4 | 11 | 3 | 3 | 1 | 16 | 7 | 2 | |
| The pharmacist applies a behaviour change approach in change management or education and training | 3 | 12 | 2 | 3 | 5 | 3 | 12 | 8 | 3 | |
| U/C* Unable to comment | ||||||||||
| Supporting quotes “The Fellow is very good at identifying the context for change and making on-going assessment of the potential impact of change.” “The Fellow has embraced new concepts of behaviour change in terms of education and training and has applied this new learning into practice.” “The Fellow has worked hard to develop their confidence and her voice in the team, now confidently able to establish their ideas into change.”“Use of QI methodology to understand problems, adapt processes and work differently.” “…. can take on a variety of challenges, whether that involves service improvement, additional clinical responsibilities or education and training.” “Working in a LMIC has provided an opportunity to apply skills in a new context and learning can be applied in future roles.” | ||||||||||
| Innovative working and practice | ||||||||||
| The pharmacist strives to improve his/her service within the limitation of resources. | 3 | 8 | 9 | 3 | 2 | 2 | 16 | 8 | ||
| The pharmacist is able to analyse essential data and utilise the results to improve services. | 2 | 8 | 8 | 4 | 3 | 3 | 13 | 8 | 2 | |
| The pharmacist is able to identify the key stakeholders and understand their agenda. | 4 | 12 | 4 | 5 | 4 | 12 | 10 | |||
| The applicant takes the lead to ensure innovation produces demonstrable improvement | 2 | 11 | 6 | 2 | 4 | 1 | 3 | 13 | 8 | 1 |
| The Fellow effectively strives to improve quality within limitations of service | 3 | 9 | 7 | 5 | 1 | 3 | 13 | 10 | ||
| The pharmacist recognises and implements innovation from the external environment. | 3 | 12 | 4 | 3 | 3 | 3 | 13 | 8 | 2 | |
| U/C* Unable to comment | ||||||||||
| Supporting quotes “The Fellow has an open mind to new ideas/innovation and change, i.e., not afraid of trying new ways of working. The Fellow has an increased awareness of stakeholder engagement and project work and in mindful of influences.” “Pushed forward with new prescribing models to address deficiencies brought about by staffing issues” “Recognises areas for improvement using resources such as audit and incident reporting, makes an action plan and delivers on these plans” “…interested in research and finding innovative ways of doing things…also good at giving due consideration to new and innovative ideas, as observed during our partnership project. I was impressed by… enthusiasm and dedication” | ||||||||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brandish, C.; Garraghan, F.; Ng, B.Y.; Russell-Hobbs, K.; Olaoye, O.; Ashiru-Oredope, D. Assessing the Impact of a Global Health Fellowship on Pharmacists’ Leadership Skills and Consideration of Benefits to the National Health Service (NHS) in the United Kingdom. Healthcare 2021, 9, 890. https://doi.org/10.3390/healthcare9070890
Brandish C, Garraghan F, Ng BY, Russell-Hobbs K, Olaoye O, Ashiru-Oredope D. Assessing the Impact of a Global Health Fellowship on Pharmacists’ Leadership Skills and Consideration of Benefits to the National Health Service (NHS) in the United Kingdom. Healthcare. 2021; 9(7):890. https://doi.org/10.3390/healthcare9070890
Chicago/Turabian StyleBrandish, Claire, Frances Garraghan, Bee Yean Ng, Kate Russell-Hobbs, Omotayo Olaoye, and Diane Ashiru-Oredope. 2021. "Assessing the Impact of a Global Health Fellowship on Pharmacists’ Leadership Skills and Consideration of Benefits to the National Health Service (NHS) in the United Kingdom" Healthcare 9, no. 7: 890. https://doi.org/10.3390/healthcare9070890
APA StyleBrandish, C., Garraghan, F., Ng, B. Y., Russell-Hobbs, K., Olaoye, O., & Ashiru-Oredope, D. (2021). Assessing the Impact of a Global Health Fellowship on Pharmacists’ Leadership Skills and Consideration of Benefits to the National Health Service (NHS) in the United Kingdom. Healthcare, 9(7), 890. https://doi.org/10.3390/healthcare9070890







