Extending Adjuvant Endocrine Therapy for 10 Years: A Mixed-Methods Analysis of Women’s Decision Making in an Online Breast Cancer Forum
Abstract
1. Introduction
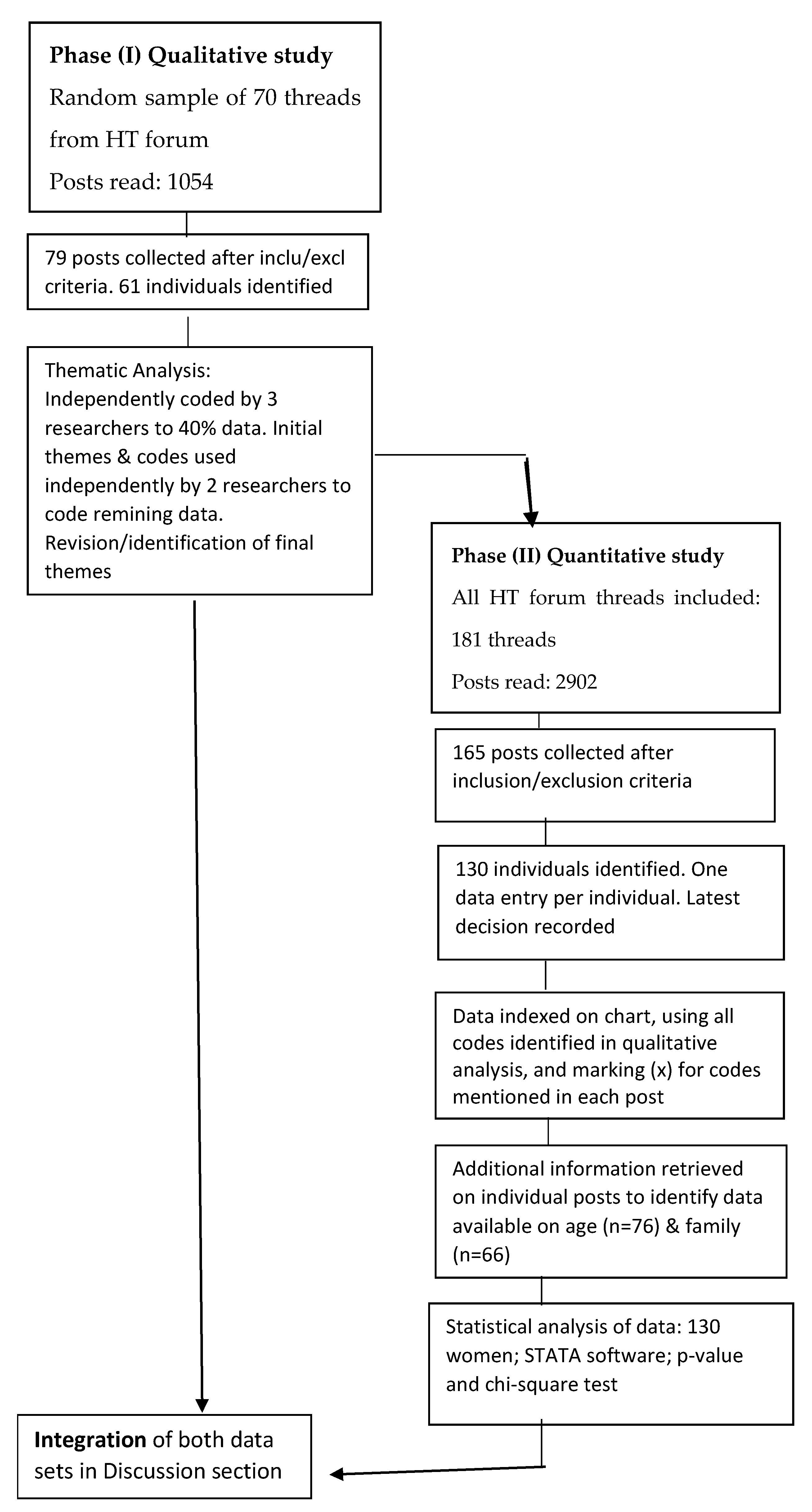
2. Materials and Methods
2.1. Study Setting
2.2. Qualitative Phase (I)
2.3. Quantitative Phase (II)
2.4. Data Integration
3. Results
3.1. Qualitative Analysis
3.1.1. Disappointment
I have taken Arimidex for two and a half years. When I consulted my doctor about all the awful side effects, and what would happen if I stopped taking it, he replied that the protocol had changed and now it is for 10 years!! I started crying…I was devastated by the prospect of “living” that way.(Helen, G1, 3+ years, discontinued)
I was resigned to the side effects as I expected to be done after 5 years, only to be told current research and statistics indicate 10 years to be better than 5.(Myriam, G2, 5+ years, continued)
3.1.2. Key Drivers of Decision Making
Fear of Recurrence/Necessity Beliefs
When I was about to complete my 5 years, I had mixed feelings. On the one hand, it would have been great to give up all medication and return to my former self (hopefully). On the other, I just wasn’t prepared to take the chance… No, I’m not happy taking the drug, but it beats the alternative.(Andrea, G1, 5 years, continued)
I did a full body scan and became worried that the cancer may have come back. I decided that there was no point in being worried and so I’m now back on the drug until I am due to finish next year.(Adele, G3, 9 years, continued)
I’m now living in fear of recurrence. I’ve been off tamoxifen for months now. I sympathise with you all.(Linda, G2, 7 years, discontinued)
I am worried as my oncologist wants me on the medication for 10 years, but there’s no way... I just hope my decision is the right one.(Laura, G3, 4 years, discontinued)
Side Effects/QOL
I just been informed that the guidelines have changed, and that I will need to continue with the medication for a total of 10 years! I said ‘NO’. I used to be very active and fit when I started treatment at 52 years old. Now, after 4 years, I’m unable to do any of the activities I used to do and enjoy! I am 56 but feeling 96! I work FT, but by midday, I’m really fading and struggling to concentrate. The challenging thing is: we have life (and I’ve lost dear friends through breast cancer) but without the quality, leaving a yoyo of emotions. Inside, I’m jumping for joy, but the Letrozole prevents me from doing the physical jumping! Good luck everyone.(Elizabeth, G1, 3 years, discontinued)
I’ve been on Tamoxifen for 7 years and I decided to come off. I’m 52, but felt like an old woman. I even struggled to get out of the bath. So I discussed stopping taking TAM with my consultant and he said yes. […](Linda, G2, 7 years, discontinued)
Just about to turn 57 years old, but I’m feeling, thinking and moving like an old lady. I can’t walk properly, and I’m in constant pain. I understand that the Anastrozole is helping to keep me alive, but at what cost? It’s a trade-off, stay alive, but without quality of life, or risk it and enjoy living? The question is ‘What to do’?(Anne, G3, 8 years, undecided)
I have been taking Tamoxifen for 6 years. Now ready to come off!! I have many side effects (hot flashes, pain in my legs and bones, dizziness, blurry vision, but I manage with it). My main concern is the risk of endometrial cancer as my uterine lining continues to grow.(Jo, G2, 6 years, discontinued)
Impact of Family
The side effects were a pain… but I told myself… you have lots to lose if you don’t take the drugs. My cancer was the ‘spreading fast’ type, and I had a child of 13 years old then. I am a single mum, and looking into her heartbroken eyes, made me realised I needed to do the tamoxifen, whether I liked it or not. I don’t regret the choice I made, because I’m in remission and it has been almost 10 years.(Hannah, G3, 9 years, discontinued a few months earlier)
I am 68 and without family. My quality of life is very important. I’ve read about the treatment being for 5 or 10 years. I’d probably live into my 80s, maybe in poor health, with some problem or other.(Mia, G3, about to start, undecided)
3.1.3. Lack of Support or Information from Healthcare Team
Nobody will give me a straight answer regarding my risk of recurrence if I stop Tamoxifen after 5 years.(Louise, G1, 5 years, undecided)
I wonder why, since the oncologists knew about doing 10 years before my diagnosis, which they did, why wait until now? when I am about to complete my treatment. Now they say ‘oh, do more years’.(Jasmine, G1, 5 years, undecided)
At one point, I told my oncologist that I felt depressed, and she prescribed me anti-depressants...however, I didn’t take them, I didn’t think she actually understood my needs.(Karim, G1, 3 years, discontinued)
I have the feeling that doctors don’t really understand what side effects are… They just follow what they learn from studies and protocols.(Jasmine, G1, 5 years, undecided)
My oncologist didn’t think the tamoxifen was giving me pain in my calf muscles as I’ve been taken it for 4 years. He insisted I would have noticed the pain sooner. He was WRONG. I am still doing physiotherapy to deal with all the damage caused by the drug in my legs. In 2 months since I stopped taking it, the pain has not come back.(Rosa, G1, 4 years, discontinued)
3.1.4. Utilising Risk Information
I heard about the predict tool, asked my new oncologist why I didn’t have the Ki67 data, and he told me that I didn’t need it as I was low risk for recurrence. I was shocked about doctors not telling me this. He agreed I will stop taking it. … Now I am happy to be called ‘non-compliant’ and hope I had been proactive sooner.(Karim, G1, 3+ years, discontinued)
Apparently, aromatase inhibitors give me 1% greater survival over a 5-year period and 2% survival if I take it for 10 years. My only concern is I don’t know if this is a very small risk and could stop taking it, or if 1 in 100 is a big risk…I wonder how you make a decision?(Sofia, G1, 4 years, undecided)
3.1.5. Coping Mechanisms
My oncologist at some point switched me to Exemestane…I take the brand name and feel so much better. Maybe you could find out and give it a try. All the best.(Diana, G3, 5+ years, continued)
I am doing my best to jot down the name of the brands that works better for me, if there is one, and I am confused.(Martha, G3, 6 weeks, continued)
For a few months I took a different brand, and suddenly I suffered depression and stronger joint pain, etc., but this went away as soon as I got back to my usual brand.(Mary, G3, 5 months, continued)
I noticed many women give up Anastrozole because they can’t tolerate the side effects, but I think that is worst, as it increases the risk of recurrence due to oestrogens rising again. It’s better to take one every other day, so at least you don’t give it up completely.(Sandra, G3, a few months, continued)
I started acupuncture las week at my hospital’s centre. So far, I haven’t had night sweats and my hot flushes are fewer in the past days. I have to take the medication for 10 years as I am high risk. Coming off the drug is not an option!(Maribelle, G3, 2 months, continued)
3.2. Quantitative Analysis
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Early Breast Cancer Trialists’ Collaborative Group (EBCTCG). Effects of chemotherapy and hormonal therapy for early breast cancer on recurrence and 15-year survival: An overview of the randomised trials. Lancet 2005, 365, 1687–1717. [Google Scholar] [CrossRef]
- Early Breast Cancer Trialists’ Collaborative Group (EBCTCG). Aromatase inhibitors versus tamoxifen in early breast cancer: Patient-level meta-analysis of the randomised trials. Lancet 2015, 386, 1341–1352. [Google Scholar] [CrossRef]
- Pan, H.; Gray, R.; Braybrooke, J.; Davies, C.; Taylor, C.; McGale, P.; Peto, R.; Pritchard, K.I.; Bergh, J.; Dowsett, M.; et al. 20-Year Risks of Breast-Cancer Recurrence after Stopping Endocrine Therapy at 5 Years. N. Engl. J. Med. 2017, 377, 1836–1846. [Google Scholar] [CrossRef]
- Davies, C.; Pan, H.; Godwin, J.; Gray, R.; Arriagada, R.; Raina, V.; Abraham, M.; Alencar, V.H.M.; Badran, A.; Bonfill, X.; et al. Long-term effects of continuing adjuvant tamoxifen to 10 years versus stopping at 5 years after diagnosis of oestrogen receptor-positive breast cancer: ATLAS, a randomised trial. Lancet 2013, 381, 805–816. [Google Scholar] [CrossRef]
- Goss, P.E.; Ingle, J.N.; Pritchard, K.I.; Robert, N.J.; Muss, H.; Gralow, J.; Gelmon, K.; Whelan, T.; Strasser-Weippl, K.; Rubin, S.; et al. Extending Aromatase-Inhibitor Adjuvant Therapy to 10 Years. N. Engl. J. Med. 2016, 375, 209–219. [Google Scholar] [CrossRef]
- Bartlett, J.; Sgroi, D.; Treuner, K.; Zhang, Y.; Ahmed, I.; Piper, T.; Salunga, R.; Brachtel, E.; Pirrie, S.; Schnabel, C.; et al. Breast Cancer Index and prediction of benefit from extended endocrine therapy in breast cancer patients treated in the Adjuvant Tamoxifen—To Offer More? (aTTom) trial. Ann. Oncol. 2019, 30, 1776–1783. [Google Scholar] [CrossRef] [PubMed]
- Henry, N.L. Endocrine Therapy Toxicity: Management Options. Am. Soc. Clin. Oncol. Educ. Book 2014, 34, e25–e30. [Google Scholar] [CrossRef]
- Moon, Z.; Moss-Morris, R.; Hunter, M.S.; Carlisle, S.; Hughes, L.D. Barriers and facilitators of adjuvant hormone therapy adherence and persistence in women with breast cancer: A systematic review. Patient Prefer. Adherence 2017, 11, 305–322. [Google Scholar] [CrossRef] [PubMed]
- Beryl, L.L.; Rendle, K.A.S.; Halley, M.C.; Gillespie, K.A.; May, S.G.; Glover, J.; Yu, P.; Chattopadhyay, R.; Frosch, D.L. Mapping the Decision-Making Process for Adjuvant Endocrine Therapy for Breast Cancer. Med Decis. Mak. 2016, 37, 79–90. [Google Scholar] [CrossRef]
- National Institute of Clinical Excellence. Early and Locally Advanced Breast Cancer: Diagnosis and Management. NICE Guide-Line. 18 July 2018. Available online: https://www.nice.org.uk/guidance/ng101/resources/early-and-locally-advanced-breast-cancer-diagnosis-and-management-pdf-66141532913605 (accessed on 12 April 2021).
- Richman, J.; Dowsett, M. Beyond 5 years: Enduring risk of recurrence in oestrogen receptor-positive breast cancer. Nat. Rev. Clin. Oncol. 2019, 16, 296–311. [Google Scholar] [CrossRef]
- Wishart, G.; Bajdik, C.; Azzato, E.; Dicks, E.; Greenberg, D.; Rashbass, J.; Caldas, C.; Pharoah, P. A population-based validation of the prognostic model PREDICT for early breast cancer. Eur. J. Surg. Oncol. 2011, 37, 411–417. [Google Scholar] [CrossRef]
- NHS: Predict Breast Cancer. Available online: https://breast.predict.nhs.uk/tool (accessed on 20 April 2021).
- Dowsett, M.; Sestak, I.; Regan, M.M.; Dodson, A.; Viale, G.; Thürlimann, B.; Colleoni, M.; Cuzick, J. Integration of Clinical Variables for the Prediction of Late Distant Recurrence in Patients with Estrogen Receptor–Positive Breast Cancer Treated with 5 Years of Endocrine Therapy: CTS5. J. Clin. Oncol. 2018, 36, 1941–1948. [Google Scholar] [CrossRef]
- Noordhoek, I.; Blok, E.J.; Kranenbarg, E.M.-K.; Putter, H.; Carpentier, M.D.-D.; Rutgers, E.J.T.; Seynaeve, C.; Bartlett, J.M.S.; Vannetzel, J.-M.; Rea, D.W.; et al. Overestimation of Late Distant Recurrences in High-Risk Patients with ER-Positive Breast Cancer: Validity and Accuracy of the CTS5 Risk Score in the TEAM and IDEAL Trials. J. Clin. Oncol. 2020, 38. [Google Scholar] [CrossRef] [PubMed]
- Clancy, C.; Lynch, J.; Oconnor, P.; Dowling, M. Breast cancer patients’ experiences of adherence and persistence to oral endocrine therapy: A qualitative evidence synthesis. Eur. J. Oncol. Nurs. 2020, 44, 101706. [Google Scholar] [CrossRef] [PubMed]
- Van Uden-Kraan, C.F.; Drossaert, C.H.C.; Taal, E.; Shaw, B.R.; Seydel, E.R.; van de Laar, M.A.F.J. Empowering Processes and Outcomes of Participation in Online Support Groups for Patients with Breast Cancer, Arthritis, or Fibromyalgia. Qual. Heal. Res. 2008, 18, 405–417. [Google Scholar] [CrossRef] [PubMed]
- Blank, T.O.; Schmidt, S.D.; Vangsness, S.A.; Monteiro, A.K.; Santagata, P.V. Differences among breast and prostate cancer online support groups. Comput. Hum. Behav. 2010, 26, 1400–1404. [Google Scholar] [CrossRef]
- Lovatt, M.; Bath, P.A.; Ellis, J.; Dalrymple, P.; Zdenkowski, N.; Gronlund, T. Development of Trust in an Online Breast Cancer Forum: A Qualitative Study. J. Med. Internet Res. 2017, 19, e175. [Google Scholar] [CrossRef]
- Lieberman, M.A.; Goldstein, B.A. Not all negative emotions are equal: The role of emotional expression in online support groups for women with breast cancer. Psycho-Oncology 2006, 15, 160–168. [Google Scholar] [CrossRef]
- Shim, M.; Cappella, J.N.; Han, J.Y. How Does Insightful and Emotional Disclosure Bring Potential Health Benefits? Study Based on Online Support Groups for Women with Breast Cancer. J. Commun. 2011, 61, 432–454. [Google Scholar] [CrossRef]
- Freedman, R.A.; Viswanath, K.; Vaz-Luis, I.; Keating, N.L. Learning from social media: Utilizing advanced data extraction techniques to understand barriers to breast cancer treatment. Breast Cancer Res. Treat. 2016, 158, 395–405. [Google Scholar] [CrossRef]
- Mao, J.J.; Chung, A.; Benton, A.; Hill, S.; Ungar, L.; Leonard, C.E.; Hennessy, S.; Holmes, J.H. Online discussion of drug side effects and discontinuation among breast cancer survivors. Pharmacoepidemiol. Drug Saf. 2013, 22, 256–262. [Google Scholar] [CrossRef] [PubMed]
- Yin, Z.; Xie, W.; Malin, B.A. Talking About My Care: Detecting Mentions of Hormonal Therapy Adherence Behavior in an Online Breast Cancer Community. AMIA Annu. Symp. Proc. 2018, 2017, 1868–1877. [Google Scholar] [PubMed]
- Ross, E.; Swallow, J.; Kerr, A.; Cunningham-Burley, S. Online accounts of gene expression profiling in early-stage breast cancer: Interpreting genomic testing for chemotherapy decision making. Heal. Expect. 2018, 22, 74–82. [Google Scholar] [CrossRef]
- Breast Cancer Now. Breast Cancer Now’s Forum. Available online: https://forum.breastcancernow.org/ (accessed on 1 February 2019).
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Fetters, M.D.; Curry, L.A.; Creswell, J.W. Achieving Integration in Mixed Methods Designs-Principles and Practices. Health Serv. Res. 2013, 48, 2134–2156. [Google Scholar] [CrossRef]
- Horne, R.; Weinman, J. Patients’ beliefs about prescribed medicines and their role in adherence to treatment in chronic physical illness. J. Psychosom. Res. 1999, 47, 555–567. [Google Scholar] [CrossRef]
- Moon, Z.E.; Moss-Morris, R.; Hunter, M.S.; Hughes, L.D. Understanding tamoxifen adherence in women with breast cancer: A qualitative study. Br. J. Health Psychol. 2017, 22, 978–997. [Google Scholar] [CrossRef] [PubMed]
- Corter, A.; Findlay, M.; Broom, R.; Porter, D.; Petrie, K.J. Beliefs about medicine and illness are associated with fear of cancer recurrence in women taking adjuvant endocrine therapy for breast cancer. Br. J. Health Psychol. 2012, 18, 168–181. [Google Scholar] [CrossRef]
- Eraso, Y. Oncologists’ perspectives on adherence/non-adherence to adjuvant endocrine therapy and management strategies in women with breast cancer. Patient Prefer. Adherence 2019, 13, 1311–1323. [Google Scholar] [CrossRef]
- Brett, J.; Boulton, M.; Fenlon, D.; Hulbert-Williams, N.J.; Walter, F.M.; Donnelly, P.; Lavery, B.A.; Morgan, A.; Morris, C.; Watson, E.K. Adjuvant endocrine therapy after breast cancer: A qualitative study of factors associated with adherence. Patient Prefer. Adherence 2018, 12, 291–300. [Google Scholar] [CrossRef]
- Wengström, Y.; Aapro, M.; di Priolo, S.L.; Cannon, H.; Georgiou, V. Patients’ knowledge and experience of adjuvant endocrine therapy for early breast cancer: A European study. Breast 2007, 16, 462–468. [Google Scholar] [CrossRef]
- Franzoi, M.A.; Agostinetto, E.; Perachino, M.; Del Mastro, L.; de Azambuja, E.; Vaz-Luis, I.; Partridge, A.H.; Lambertini, M. Evidence-based approaches for the management of side-effects of adjuvant endocrine therapy in patients with breast cancer. Lancet Oncol. 2021. [Google Scholar] [CrossRef]
- Van Herk-Sukel, M.P.P.; Van De Poll-Franse, L.V.; Voogd, A.C.; Nieuwenhuijzen, G.A.P.; Coebergh, J.W.W.; Herings, R.M.C. Half of breast cancer patients discontinue tamoxifen and any endocrine treatment before the end of the recommended treatment period of 5 years: A population-based analysis. Breast Cancer Res. Treat. 2010, 122, 843–851. [Google Scholar] [CrossRef] [PubMed]
- Pan, Y.; Heisig, S.R.; Von Blanckenburg, P.; Albert, U.-S.; Hadji, P.; Rief, W.; Nestoriuc, Y. Facilitating adherence to endocrine therapy in breast cancer: Stability and predictive power of treatment expectations in a 2-year prospective study. Breast Cancer Res. Treat. 2018, 168, 667–677. [Google Scholar] [CrossRef]
- Shelby, R.A.; Edmond, S.; Wren, A.A.; Keefe, F.J.; Peppercorn, J.M.; Marcom, P.K.; Blackwell, K.L.; Kimmick, G.G. Self-efficacy for coping with symptoms moderates the relationship between physical symptoms and well-being in breast cancer survivors taking adjuvant endocrine therapy. Support. Care Cancer 2014, 22, 2851–2859. [Google Scholar] [CrossRef]
- Breastcancer.ORG. Updated ASCO Guidelines Recommend Extended Hormonal Therapy with Aromatase Inhibitors for Postmenopausal Women with Hormone-Receptor-Positive Breast Cancer. Published on 29 November 2018. Available online: https://www.breastcancer.org/research-news/asco-recommends-extended-hormonal-tx-for-some (accessed on 1 May 2021).
- Davis, K.W.; Roter, D.L.; Schmidlen, T.; Scheinfeldt, L.B.; Klein, W.M. Testing a best practices risk result format to communicate genetic risks. Patient Educ. Couns. 2021, 104, 936–943. [Google Scholar] [CrossRef] [PubMed]
- NHS England. Structured Medication Reviews and Medicines Optimisation: Guidance. 2020. Available online: https://www.england.nhs.uk/publication/structured-medication-reviews-and-medicines-optimisation/ (accessed on 30 April 2021).
| Decision on Treatment Continuation | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Continue | NOT Continue | Undecided | |||||||
| Category | Subgroup | n | n | % | n | % | n | % | p-Value 3 |
| Overall sample | 130 | 59 | 45.4 | 34 | 26.2 | 37 | 28.5 | ||
| By treatment scheme | Prescribed for 10-year treatment | 56 | 35 | 62.5 | 8 | 14.3 | 13 | 23.2 | |
| In 10-year treatment (originally 5-year) | 25 | 14 | 56.0 | 5 | 20.0 | 6 | 24.0 | ||
| Planning 10-year treatment (currently in 5-year) | 49 | 10 | 20.4 | 21 | 42.9 | 18 | 36.7 | <0.001 | |
| Treatment duration | 2-years or less | 36 | 23 | 63.9 | 2 | 5.6 | 11 | 30.6 | |
| 2–5-years | 58 | 16 | 27.6 | 24 | 41.4 | 18 | 31.0 | ||
| 5–10-years | 36 | 20 | 55.6 | 8 | 22.2 | 8 | 22.2 | 0.001 | |
| Age 1 | <50 years | 19 | 11 | 57.9 | 5 | 26.3 | 3 | 15.8 | |
| 50–60 years | 37 | 20 | 54.1 | 10 | 27.0 | 7 | 18.9 | ||
| 60+ years | 20 | 10 | 50.0 | 4 | 20.0 | 6 | 30.0 | 0.831 | |
| Family status 2 | Lives alone | 18 | 11 | 61.1 | 3 | 16.7 | 4 | 22.2 | |
| Lives with family | 48 | 30 | 62.5 | 9 | 18.8 | 9 | 18.7 | 0.944 | |
| Codes | Overall Sample (n = 130) | By Treatment Scheme | By Decision on Treatment Continuation | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Prescribed for 10-Year Treatment (n = 56) | In 10-Year Treatment (Originally 5-Year) (n = 25) | Planning 10-Year Treatment (Currently in 5-Year) (n = 49) | p-Value 1 | Continue (n = 59) | Not Continue (34) | Undecided (37) | p-Value 1 | ||
| % | % | % | % | % | % | % | |||
| Fear of cancer recurrence | 27.7 | 21.4 | 40.0 | 28.6 | 0.222 | 39.0 | 14.7 | 21.6 | 0.026 |
| Side effects of medication | 92.3 | 92.9 | 96.0 | 89.8 | 0.625 | 91.5 | 91.2 | 94.6 | 0.825 |
| Trust in drug’s effectiveness | 19.2 | 16.1 | 24.0 | 20.4 | 0.681 | 33.2 | 8.8 | 8.1 | 0.003 |
| Family as reason for treatment continuation | 5.4 | 3.6 | 8.0 | 6.1 | 0.687 | 1.7 | 5.9 | 10.8 | 0.155 |
| Using coping mechanisms to alleviate side effects | 22.3 | 25.0 | 20.0 | 20.4 | 0.813 | 32.2 | 14.7 | 13.5 | 0.047 |
| Researching the disease using reliable sources | 16.9 | 17.9 | 4.0 | 22.5 | 0.131 | 15.3 | 17.7 | 18.9 | 0.889 |
| Trust in doctor’s advise | 7.8 | 3.6 | 12.0 | 10.2 | 0.297 | 5.1 | 11.8 | 8.1 | 0.505 |
| Age as reason for treatment continuation/discontinuation | 13.9 | 16.1 | 12.0 | 12.2 | 0.815 | 11.9 | 14.7 | 16.2 | 0.823 |
| Quality of life affected by medication | 34.6 | 35.7 | 36.0 | 32.7 | 0.935 | 18.6 | 47.1 | 48.7 | 0.002 |
| Does not trust medication | 5.4 | 1.8 | 0.0 | 12.2 | 0.025 | 1.7 | 11.8 | 5.4 | 0.117 |
| Does not trust health professional | 9.2 | 3.6 | 4.0 | 18.4 | 0.020 | 0.0 | 23.5 | 10.8 | 0.001 |
| Using a test that gives information on risk of cancer recurrence | 4.6 | 5.4 | 0.0 | 6.1 | 0.465 | 1.7 | 2.9 | 10.8 | 0.101 |
| Other condition that is developed or made worse by taking the drugs | 15.4 | 14.3 | 20.0 | 14.3 | 0.776 | 13.6 | 23.5 | 10.8 | 0.290 |
| Treatment discontinued by doctor | 10.0 | 1.8 | 12.0 | 18.4 | 0.017 | 0.0 | 38.2 | 0.0 | <0.001 |
| Brand change (use of the same drug by different brands) | 6.9 | 8.9 | 12.0 | 2.0 | 0.206 | 10.2 | 5.9 | 2.7 | 0.360 |
| Switching medication due to intolerance of the first option | 19.2 | 23.2 | 24.0 | 12.2 | 0.290 | 25.4 | 5.9 | 21.6 | 0.064 |
| Not coping with side effects | 25.4 | 28.6 | 28.0 | 20.4 | 0.597 | 8.5 | 41.2 | 37.8 | <0.001 |
| Codes | Model | Decision on Continuation | ||||||
|---|---|---|---|---|---|---|---|---|
| Continue | NOT Continue | Undecided | ||||||
| OR | OR | (95%CI) | p-Value | OR | (95%CI) | p-Value | ||
| Fear of cancer recurrence | model 1 | 1 (reference) | 0.27 | (0.09–0.80) | 0.018 | 0.43 | (0.17–1.11) | 0.080 |
| model 2 | 1 (reference) | 0.13 | (0.04–0.49) | 0.002 | 0.29 | (0.09–0.90) | 0.033 | |
| Trust in drug’s effectiveness | model 1 | 1 (reference) | 0.20 | (0.05–0.75) | 0.017 | 0.19 | (0.05–0.68) | 0.011 |
| model 2 | 1 (reference) | 0.13 | (0.03–0.61) | 0.010 | 0.12 | (0.03–0.55) | 0.006 | |
| Using coping mechanisms to alleviate side effects | model 1 | 1 (reference) | 0.36 | (0.12–1.08) | 0.070 | 0.33 | (0.11–0.98) | 0.045 |
| model 2 | 1 (reference) | 0.26 | (0.07–0.95) | 0.041 | 0.25 | (0.07–0.86) | 0.029 | |
| Quality of life affected by medication | model 1 | 1 (reference) | 3.88 | (1.52–9.93) | 0.005 | 4.13 | (1.65–10.36) | 0.002 |
| model 2 | 1 (reference) | 9.05 | (2.81–29.1) | <0.001 | 8.75 | (2.83–27.06) | <0.001 | |
| Does not trust medication or health professional | model 1 | 1 (reference) | 20.88 | (2.50–173.7) | 0.005 | 9.06 | (1.01–80.97) | 0.049 |
| model 2 | 1 (reference) | 22.79 | (1.89–279.9) | 0.014 | 14.27 | (1.06–192.0) | 0.045 | |
| Not coping with side effects | model 1 | 1 (reference) | 7.56 | (2.41–23.70) | 0.001 | 6.57 | (2.12–20.39) | 0.001 |
| model 2 | 1 (reference) | 16.47 | (4.02–67.58) | <0.001 | 12.26 | (3.17–47.37) | <0.001 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Eraso, Y.; Stefler, D.; Moon, Z.; Rossi, L.; Assefa, S. Extending Adjuvant Endocrine Therapy for 10 Years: A Mixed-Methods Analysis of Women’s Decision Making in an Online Breast Cancer Forum. Healthcare 2021, 9, 688. https://doi.org/10.3390/healthcare9060688
Eraso Y, Stefler D, Moon Z, Rossi L, Assefa S. Extending Adjuvant Endocrine Therapy for 10 Years: A Mixed-Methods Analysis of Women’s Decision Making in an Online Breast Cancer Forum. Healthcare. 2021; 9(6):688. https://doi.org/10.3390/healthcare9060688
Chicago/Turabian StyleEraso, Yolanda, Denes Stefler, Zoe Moon, Leda Rossi, and Sidona Assefa. 2021. "Extending Adjuvant Endocrine Therapy for 10 Years: A Mixed-Methods Analysis of Women’s Decision Making in an Online Breast Cancer Forum" Healthcare 9, no. 6: 688. https://doi.org/10.3390/healthcare9060688
APA StyleEraso, Y., Stefler, D., Moon, Z., Rossi, L., & Assefa, S. (2021). Extending Adjuvant Endocrine Therapy for 10 Years: A Mixed-Methods Analysis of Women’s Decision Making in an Online Breast Cancer Forum. Healthcare, 9(6), 688. https://doi.org/10.3390/healthcare9060688






