Understanding the Links between Inferring Mental States, Empathy, and Burnout in Medical Contexts
Abstract
1. Introduction
2. Materials and Methods
2.1. Procedure and Participants
2.2. Ethical Approval
2.3. Instruments
3. Results
3.1. Descriptive Statistics and Zero-Order Correlations
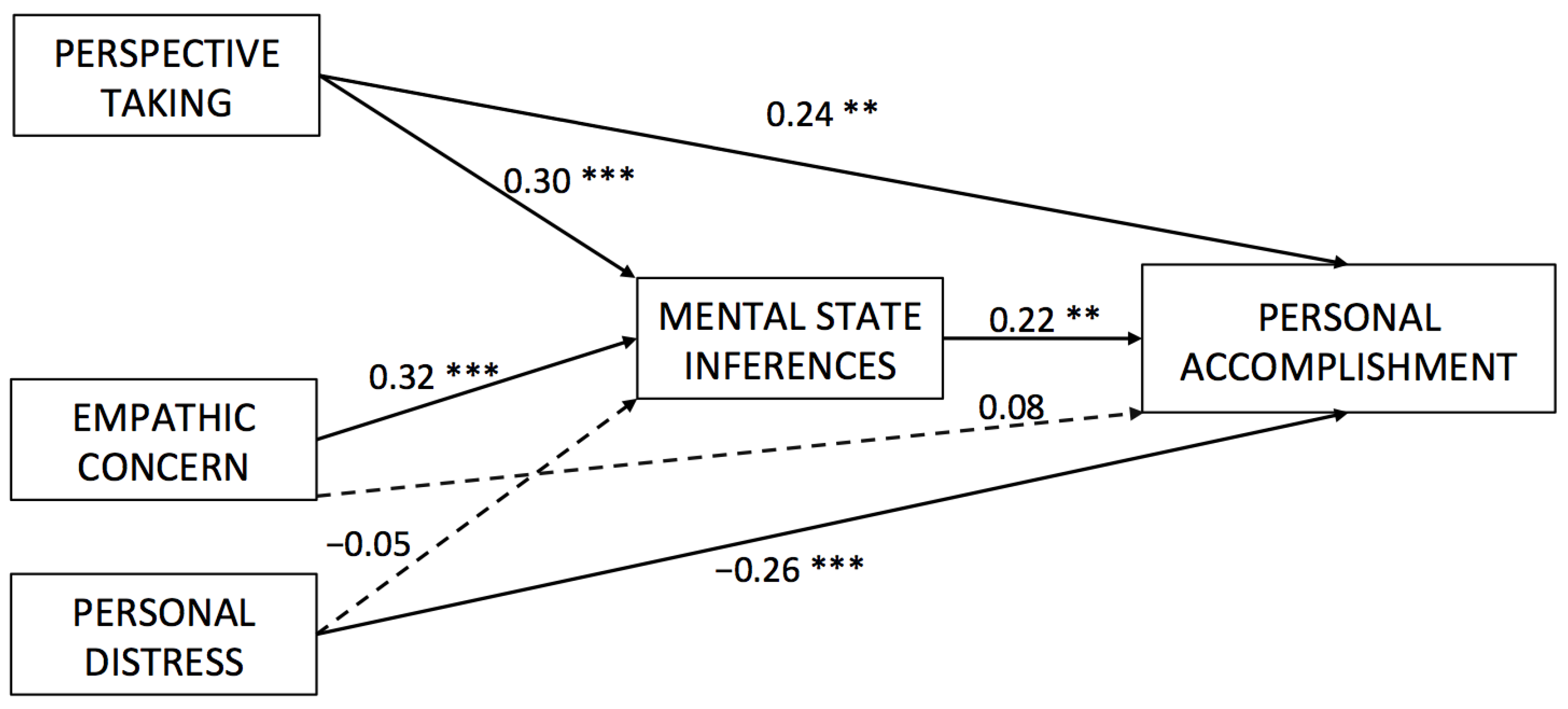
3.2. Paths from Empathy to Burnout
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Paths | Estimate | z-Value | P (>|z|) | Std | 95% CI |
|---|---|---|---|---|---|
| EmoCon→EmoExh | 0.085 | 0.991 | 0.991 | 0.085 | [−0.083, 0.252] |
| PerTak→EmoExh | 0.085 | −0.397 | 0.692 | −0.034 | [−0.201, 0.134] |
| PerDis→EmoExh | 0.077 | 3.905 | 0.000 | 0.302 | [0.150, 0.454] |
| EmoCon→InfMen | 0.072 | 4.292 | 0.000 | 0.307 | [0.167, 0.447] |
| PerTak→InfMen | 0.074 | 4.371 | 0.000 | 0.323 | [0.178, 0.467] |
| PerDis→InfMen | 0.079 | −0.478 | 0.633 | −0.038 | [−0.192, 0.116] |
| EmoExh→InfMen | 0.094 | 1.565 | 0.118 | 0.147 | [−0.037, 0.331] |
| Paths | Estimate | z-Value | P (>|z|) | Std | 95% CI |
|---|---|---|---|---|---|
| EmoCon→PerAcc | 0.070 | 1.195 | 0.232 | 0.084 | [−0.054, 0.022] |
| PerTak→PerAcc | 0.069 | 3.442 | 0.001 | 0.237 | [0.102, 0.372] |
| PerDis→PerAcc | 0.071 | −3.710 | 0.000 | −0.263 | [−0.401, −0.124] |
| EmoCon→InfMen | 0.070 | 4.563 | 0.000 | 0.322 | [0.183, 0.460] |
| PerTak→InfMen | 0.077 | 3.917 | 0.000 | 0.302 | [0.151, 0.453] |
| PerDis→InfMen | 0.073 | −0.626 | 0.531 | −0.045 | [−0.188, 0.097] |
| PerAcc→InfMen | 0.085 | 2.616 | 0.009 | 0.223 | [0.056, 0.390] |
| Paths | Estimate | z-Value | P (>|z|) | Std | 95% CI |
|---|---|---|---|---|---|
| EmoCon→Dep | 0.102 | −1.451 | 0.147 | −0.148 | [−0.347, 0.052] |
| PerTak→Dep | 0.089 | −2.510 | 0.012 | −0.224 | [−0.399, −0.049] |
| PerDis→Dep | 0.078 | 1.049 | 0.294 | 0.082 | [−0.071, 0.234] |
| EmoCon→InfMen | 0.067 | 4.727 | 0.000 | 0.315 | [0.185, 0.446] |
| PerTak→InfMen | 0.073 | 4.334 | 0.000 | 0.317 | [0.173, 0.460] |
| PerDis→InfMen | 0.075 | −0.575 | 0.565 | −0.043 | [−0.191, 0.105] |
| Dep→InfMen | 0.101 | 0.209 | 0.834 | 0.021 | [−0.177, 0.220] |
References
- Shapiro, J.; McDonald, T.B. Supporting clinicians during Covid-19 and beyond—Learning from past failures and envisioning new strategies. N. Engl. J. Med. 2020, 383, e142. [Google Scholar] [CrossRef] [PubMed]
- Gleichgerrcht, E.; Decety, J. The costs of empathy among health professionals. In Empathy: From Bench to Bedside; Decety, J., Ed.; MIT Press: Cambridge, MA, USA, 2012; pp. 245–261. [Google Scholar]
- Gleichgerrcht, E.; Decety, J. Empathy in clinical practice: How individual dispositions, gender, and experience moderate empathic concern, burnout, and emotional distress in physicians. PLoS ONE 2013, 8, e61526. [Google Scholar] [CrossRef] [PubMed]
- Halpern, J. Clinical empathy in medical care. In Empathy: From Bench to Bedside; Decety, J., Ed.; MIT Press: Cambridge, MA, USA, 2012; pp. 229–244. [Google Scholar]
- Rothschild, B. Help for the Helper: The Psychophysiology of Compassion Fatigue and Vicarious Trauma; WW Norton & Company: New York, NY, USA, 2006. [Google Scholar]
- Aström, S.; Norberg, A.; Nilsson, M.; Winblad, B. Tedium among personnel working with geriatric patients. Scand. J. Caring Sci. 1987, 1, 125–132. [Google Scholar] [CrossRef] [PubMed]
- Ferri, P.; Guerra, E.; Marcheselli, L.; Cunico, L.; Di Lorenzo, R. Empathy and burnout: An analytic cross-sectional study among nurses and nursing students. Acta Bio-Med. Atenei Parm. 2015, 86, 104–115. [Google Scholar]
- Hoffman, M.I. Empathy and Moral Development: Implications for Caring and Justice; Cambridge University Press: New York, NY, USA, 2000. [Google Scholar]
- Mercer, S.W.; Reynolds, W.J. Empathy and quality of care. Br. J. Gen. Pract. 2002, 52, S9–S12. [Google Scholar] [PubMed]
- Picard, J.; Catu-Pinault, A.; Boujut, E.; Botella, M.; Jaury, P.; Zenasni, F. Burnout, empathy and their relationships: A qualitative study with residents in General Medicine. Psychol. Health Med. 2015, 21, 354–361. [Google Scholar] [CrossRef]
- Davis, M.H. A multidimensional approach to individual differences in empathy. JSAS 1980, 10, 85. [Google Scholar]
- Batson, C.D. These things called empathy. In The Social Neuroscience of Empathy; Decety, J., Ickes, W., Eds.; MIT Press: Cambridge, MA, USA, 2009; pp. 3–15. [Google Scholar]
- Decety, J. The neuroevolution of empathy. Ann. N. Y. Acad. Sci. 2011, 1231, 35–45. [Google Scholar] [CrossRef]
- Decety, J.; Cowell, J.M. The complex relation between morality and empathy. Trends Cogn. Sci. 2014, 18, 337–339. [Google Scholar] [CrossRef]
- Decety, J.; Smith, K.E.; Norman, G.J.; Halpern, J. A social neuroscience perspective on clinical empathy. World Psychiatry 2014, 13, 233–237. [Google Scholar] [CrossRef]
- Singer, T.; Lamm, C. The social neuroscience of empathy. Ann. N. Y. Acad. Sci. 2009, 1156, 81–96. [Google Scholar] [CrossRef] [PubMed]
- Völlm, B.A.; Taylor, A.N.; Richardson, P.; Corcoran, R.; Stirling, J.; McKie, S.; Deakin, J.F.; Elliott, R. Neuronal correlates of theory of mind and empathy: A functional magnetic resonance imaging study in a nonverbal task. NeuroImage 2006, 29, 90–98. [Google Scholar] [CrossRef] [PubMed]
- Epley, N.; Waytz, A. Mind perception. In Handbook of Social Psychology; Wiley: New York, NY, USA, 2010; pp. 498–541. [Google Scholar]
- Harris, L.T.; Fiske, S.T. Social neuroscience evidence for dehumanised perception. Eur. Rev. Soc. Psychol. 2009, 20, 192–231. [Google Scholar] [CrossRef]
- Gray, H.M.; Gray, K.; Wegner, D.M. Dimensions of mind perception. Science 2007, 315, 619. [Google Scholar] [CrossRef] [PubMed]
- Fiske, S.T.; Taylor, S.E. Social Cognition, 2nd ed.; Mcgraw-Hill: New York, NY, USA, 1991. [Google Scholar]
- Fiske, S.T.; Taylor, S.E. (Eds.) Attention and encoding. In Social Cognition: From Brains to Culture; McGraw-Hill: New York, NY, USA, 2008; pp. 51–74. [Google Scholar]
- Herrmann, E.; Call, J.; Hernàndez-Lloreda, M.V.; Hare, B.; Tomasello, M. Humans have evolved specialized skills of social cognition: The cultural intelligence hypothesis. Science 2007, 317, 1360–1366. [Google Scholar] [CrossRef]
- Saxe, R. Uniquely human social cognition. Curr. Opin. Neurobiol. 2006, 16, 235–239. [Google Scholar] [CrossRef]
- Waytz, A.; Schroeder, J.; Epley, N. The lesser minds problem. In Humanness and Dehumanization; Bain, P.G., Vaes, J., Leyens, J.-P., Eds.; Psychology Press: New York, NY, USA, 2014; pp. 49–67. [Google Scholar]
- Fiske, S.T. Varieties of (de) humanization: Divided by competition and status. In Objectification and (De) Humanization; Gervais, S.J., Ed.; Springer: New York, NY, USA, 2013; pp. 53–71. [Google Scholar]
- Harris, L.T.; Fiske, S.T. Dehumanizing the lowest of the low: Neuroimaging responses to extreme out-groups. Psychol. Sci. 2006, 17, 847–853. [Google Scholar] [CrossRef]
- Harris, L.T.; Fiske, S.T. Perceiving humanity or not: A social neuroscience approach to dehumanized perception. In Social Neuroscience: Toward Understanding the Underpinnings of the Social Mind; Todorov, A., Fiske, S., Eds.; Oxford University Press: Oxford, UK, 2011; pp. 123–134. [Google Scholar]
- Haslam, N. Dehumanization: An integrative review. Pers. Soc. Psychol. Rev. 2006, 10, 252–264. [Google Scholar] [CrossRef]
- Haslam, N.; Loughnan, S. Dehumanization and infrahumanization. Annu. Rev. Psychol. 2014, 65, 399–423. [Google Scholar] [CrossRef]
- Leyens, J.-P.; Rodríguez-Pérez, A.; Rodríguez-Torres, R.; Gaunt, R.; Paladino, M.P.; Vaes, J. Psychological essentialism and the differential attribution of uniquely human emotions to ingroups and outgroups. Eur. J. Soc. Psychol. 2001, 31, 395–411. [Google Scholar] [CrossRef]
- Buffone, A.E.; Poulin, M.; Delury, S.; Ministero, L.; Morrisson, C.; Scalco, M. Don’t walk in her shoes! Different forms of perspective taking affect stress physiology. J. Exp. Soc. Psychol. 2017, 72, 161–168. [Google Scholar] [CrossRef]
- Dvash, J.; Shamay-Tsoory, S.G. Theory of Mind and empathy as multidimensional constructs: Neurological foundations. Top. Lang. Disord. 2014, 34, 282–295. [Google Scholar] [CrossRef]
- Christoff, K. Dehumanization in organizational settings: Some scientific and ethical considerations. Front. Hum. Neurosci. 2014, 8, 748. [Google Scholar] [CrossRef]
- Halpern, J. What is clinical empathy? J. Gen. Intern. Med. 2003, 18, 670–674. [Google Scholar] [CrossRef] [PubMed]
- Lamothe, M.; Boujut, E.; Zenasni, F.; Sultan, S. To be or not to be empathic: The combined role of empathic concern and perspective taking in understanding burnout in general practice. BMC Fam. Pract. 2014, 15, 15. [Google Scholar] [CrossRef]
- Capozza, D.; Falvo, R.; Boin, J.; Colledani, D. Dehumanization in medical contexts: An expanding research field. Test. Psychom. Methodol. Appl. Psychol. 2016, 23, 545–559. [Google Scholar]
- Decety, J.; Yang, C.-Y.; Cheng, Y. Physicians down-regulate their pain empathy response: An event-related brain potential study. NeuroImage 2010, 50, 1676–1682. [Google Scholar] [CrossRef]
- Vaes, J.; Muratore, M. Defensive dehumanization in the medical practice: A cross-sectional study from a health care worker’s perspective. Br. J. Soc. Psychol. 2013, 52, 180–190. [Google Scholar] [CrossRef]
- Fitzgerald-Yau, N.; Egan, J. Defense styles mediate the association between empathy and burnout among nurses. J. Nerv. Ment. Dis. 2018, 206, 555–561. [Google Scholar] [CrossRef]
- Duarte, J.; Pinto-Gouveia, J. The role of psychological factors in oncology nurses’ burnout and compassion fatigue symptoms. Eur. J. Oncol. Nurs. 2017, 28, 114–121. [Google Scholar] [CrossRef]
- Thomas, J. Association of personal distress with burnout, compassion fatigue, and compassion satisfaction among clinical social workers. J. Soc. Serv. Res. 2013, 39, 365–379. [Google Scholar] [CrossRef]
- Von Harscher, H.; Desmarais, N.; Dollinger, R.; Grossman, S.; Aldana, S. The impact of empathy on burnout in medical students: New findings. Psychol. Health Med. 2018, 23, 295–303. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Albéniz, A.; De Paúl, J.; Etxeberría, J.; Montes, M.P.; Torres, E. Adaptación de interpersonal reactivity index (IRI) al español. Psicothema 2003, 15, 267–272. [Google Scholar]
- Egleichgerrcht, E.; Edecety, J. The relationship between different facets of empathy, pain perception and compassion fatigue among physicians. Front. Behav. Neurosci. 2014, 8, 243. [Google Scholar] [CrossRef]
- Maslach, C.; Jackson, S.E. Inventario Burnout de Maslach (MBI): Síndrome del Quemado por Estrés Laboral Asistencial; TEA Ediciones: Madrid, Spain, 1997. [Google Scholar]
- Hernández, J.; Betancort, M. ULLRToolbox. 2016. Available online: https://sites.google.com/site/ullrtoolbox/ (accessed on 21 September 2020).
- Rosseel, Y. Lavaan: An R package for structural equation modeling. Version 0.5-12 (BETA). J. Stat. Softw. 2012, 48, 1–36. [Google Scholar] [CrossRef]
- Hayes, A.F. Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach; The Guilford Press: New York, NY, USA, 2013. [Google Scholar]
- Haque, O.S.; Waytz, A. Dehumanization in medicine: Causes, solutions, and functions. Perspect. Psychol. Sci. 2012, 7, 176–186. [Google Scholar] [CrossRef]
- Davis, M.H. The effects of dispositional empathy on emotional reactions and helping: A multidimensional approach. J. Pers. 1983, 51, 167–184. [Google Scholar] [CrossRef]
- Decety, J. Empathy in medicine: What it is, and how much we really need it. Am. J. Med. 2020, 133, 561–566. [Google Scholar] [CrossRef]
- Hojat, M. Empathy in Health Professions Education and Patient Care; Springer Nature: New York, NY, USA, 2016. [Google Scholar]
- Hojat, M.; DeSantis, J.; Shannon, S.C.; Mortensen, L.H.; Speicher, M.R.; Bragan, L.; LaNoue, M.; Calabrese, L.H. The Jefferson scale of empathy: A nationwide study of measurement properties, underlying components, latent variable structure, and national norms in medical students. Adv. Health Sci. Educ. 2018, 23, 899–920. [Google Scholar] [CrossRef]
- Moudatsou, M.; Stavropoulou, A.; Philalithis, A.; Koukouli, S. The role of empathy in health and social care professionals. Healthcare 2020, 8, 26. [Google Scholar] [CrossRef]
- Preusche, I.; Lamm, C. Reflections on empathy in medical education: What can we learn from social neurosciences? Adv. Health Sci. Educ. 2016, 21, 235–249. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, J. The paradox of teaching empathy in medical education. In Empathy: From Bench to Bedside; Decety, J., Ed.; MIT Press: Cambridge, MA, USA, 2012; pp. 275–300. [Google Scholar]
- Lamothe, M.; Rondeau, É.; Malboeuf-Hurtubise, C.; Duval, M.; Sultan, S. Outcomes of MBSR or MBSR-based interventions in health care providers: A systematic review with a focus on empathy and emotional competencies. Complement. Ther. Med. 2016, 24, 19–28. [Google Scholar] [CrossRef] [PubMed]
- Levett-Jones, T.; Cant, R.; Lapkin, S. A systematic review of the effectiveness of empathy education for undergraduate nursing students. Nurse Educ. Today 2019, 75, 80–94. [Google Scholar] [CrossRef] [PubMed]
- Ford, R.; Bammer, G. A research routine to assess bias introduced by low response rates in postal surveys. Nurse Res. 2009, 17, 44–53. [Google Scholar] [CrossRef] [PubMed]
| Frequency (n) | Percentage (%) | Mean | SD | Range | |
|---|---|---|---|---|---|
| Age | 44.6 | 10.46 | 23–65 | ||
| Gender | |||||
| Female | 142 | 77.2 | |||
| Male | 42 | 22.8 | |||
| Working experience (years) | |||||
| Nurses | 105 | 56.8 | 19.24 | 11.31 | 1–41 |
| Doctors | 56 | 30.3 | 20.80 | 9.88 | 1–40 |
| Nursing assistants | 13 | 7.6 | 13.69 | 11.31 | 1–33 |
| Other categories | 10 | 5.4 | 20.30 | 9.35 | 2–33 |
| Current specialty | |||||
| Emergency and intensive care | 47 | 25.54 | |||
| Surgery and medical specialties | 30 | 16.30 | |||
| Primary care | 28 | 15.28 | |||
| Outpatient consultation, outpatient specialty clinic, central clinical division | 26 | 14.13 | |||
| Pediatrics and gynecology | 15 | 8.15 | |||
| Palliative care | 14 | 7.61 | |||
| Mental health | 10 | 5.43 | |||
| Others | 14 | 7.61 |
| Mean | SD | MenSta | PerTak | EmoCon | PerDis | EmoExh | Dep | PerAcc | |
|---|---|---|---|---|---|---|---|---|---|
| MenSta | 3.88 | 0.66 | - | ||||||
| PerTak | 3.73 | 0.77 | 0.41 *** | - | |||||
| EmoCon | 4.00 | 0.74 | 0.40 *** | 0.30 *** | - | ||||
| PerDis | 1.99 | 0.70 | −0.13 | −0.23 *** | −0.08 | - | |||
| EmoExh | 3.40 | 1.68 | 0.14 | 0.01 | 0.11 | 0.27 *** | - | ||
| Dep | 2.46 | 1.52 | −0.14 | −0.29 *** | −0.19 ** | 0.14 | 0.47 *** | - | |
| PerAcc | 6.14 | 0.99 | 0.38 *** | 0.42 ** | 0.27 *** | −0.35 *** | −0.29 *** | −0.41 *** | - |
| Estimate | z-Value | P (>|z|) | Std | 95% CI | |
|---|---|---|---|---|---|
| Paths for Emotional Exhaustion | |||||
| PerTak→InfMen→EmoExh | 0.047 | 1.334 | 0.166 | 0.036 | [−0.022, 0.117] |
| EmoCon→InfMen→EmoExh | 0.045 | 1.403 | 0.138 | 0.032 | [−0.018, 0.108] |
| PerDis→InfMen→EmoExh | −0.006 | −0.459 | 0.653 | 0.012 | [−0.029, 0.018] |
| Paths for Personal Accomplishment | |||||
| PerTak→InfMen→PerAcc | 0.067 | 2.221 | 0.026 | 0.030 | [0.008, 0.127] |
| EmoCon→InfMen→PerAcc | 0.072 | 2.338 | 0.019 | 0.031 | [0.012, 0.132] |
| PerDis→InfMen→PerAcc | −0.010 | −0.574 | 0.566 | 0.018 | [−0.045, 0.024] |
| Paths for Depersonalization | |||||
| PerTak→InfMen→Dep | 0.007 | 0.208 | 0.835 | 0.032 | [−0.056, 0.070] |
| EmoCon→InfMen→Dep | 0.007 | 0.209 | 0.835 | 0.032 | [−0.056, 0.069] |
| PerDis→InfMen→Dep | −0.001 | −0.196 | 0.845 | 0.005 | [−0.010, 0.008] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Delgado, N.; Bonache, H.; Betancort, M.; Morera, Y.; Harris, L.T. Understanding the Links between Inferring Mental States, Empathy, and Burnout in Medical Contexts. Healthcare 2021, 9, 158. https://doi.org/10.3390/healthcare9020158
Delgado N, Bonache H, Betancort M, Morera Y, Harris LT. Understanding the Links between Inferring Mental States, Empathy, and Burnout in Medical Contexts. Healthcare. 2021; 9(2):158. https://doi.org/10.3390/healthcare9020158
Chicago/Turabian StyleDelgado, Naira, Helena Bonache, Moisés Betancort, Yurena Morera, and Lasana T. Harris. 2021. "Understanding the Links between Inferring Mental States, Empathy, and Burnout in Medical Contexts" Healthcare 9, no. 2: 158. https://doi.org/10.3390/healthcare9020158
APA StyleDelgado, N., Bonache, H., Betancort, M., Morera, Y., & Harris, L. T. (2021). Understanding the Links between Inferring Mental States, Empathy, and Burnout in Medical Contexts. Healthcare, 9(2), 158. https://doi.org/10.3390/healthcare9020158






