Proposed Lyme Disease Guidelines and Psychiatric Illnesses
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. The Disclaimer, Guidelines or an Imposed Standard?
3.2. Laboratory Testing in the Proposed Guidelines
- Quote: “For the diagnosis of Lyme disease, the 2-tier serologic testing protocol for Lyme disease has a number of shortcomings including low sensitivity in early disease”. [20] (Wormser GP et al., 2012). This is by Wormser, Aguaro-Rosenfeld and Steere, all co-authors of the proposed 2020 IDSA guidelines. The paper gives specific sensitivities which not only show the method has low sensitivity for early disease but also in the general case where sensitivity is 50.6%. That is 50% of all patients with Lyme disease will not be treated for the disease based on the guidelines.
- Quote: “The sensitivity of C6 testing (69.5%) was greater than that of 2-tier testing (38.9%).” (Wormser GP et al., 2008). This is again by Wormser and Aguero-Rosenfeld [21].
- For early stage disease, when it is most important to diagnose the disease for successful treatment, Branda, Lantos, Strle and Steere, who are all authors of the new guidelines, stated: “Sensitivity of the various MTTT (Modified Two-Tier Test) protocols in patients with acute erythema migrans ranged from 36% (95% confidence interval [CI], 25–50%) to 54% (95% CI, 42–67%), compared with 25% (95% CI, 16–38%) using the conventional protocol.” (Branda JA. et al. 2017) [22].
- In a paper published by Branda with co-authors Aguero-Rosenfeld, Wormser and Steere, the sensitivity of the two tier test for acute cases was 30% and for convalescent cases was 59%, and it was recommended that the test be replaced by a more sensitive one. (J. A. Branda et al., 2010) Of note is that four of the study authors are authors of the proposed 2020 IDSA guideline [23].
- A report based on the work of Leeflang et al. (2016) [24] indicated that data from 15 studies of the sensitivity of the two-tier test varied from 4% to 50%. A quotation from the report was: “Goossens et al. (2000) evaluated two-tiered tests in early and in late LB. The results were comparable to those for the study with healthy controls, except that there was more variation in specificity. None of the evaluations revealed sensitivity above 50% (one was 50%).” (Zeller and Van Bortel, 2016) [25].
- A statistical analysis of the two-tier test demonstrated that it generated up to 500 times more false negative results than HIV testing. (Cook and Puri, 2017) [26].
3.3. Testing Adult Patients with Psychiatric Illness for Lyme Disease
3.4. Testing Children with Developmental, Behavioral or Psychiatric Disorders for Lyme Disease
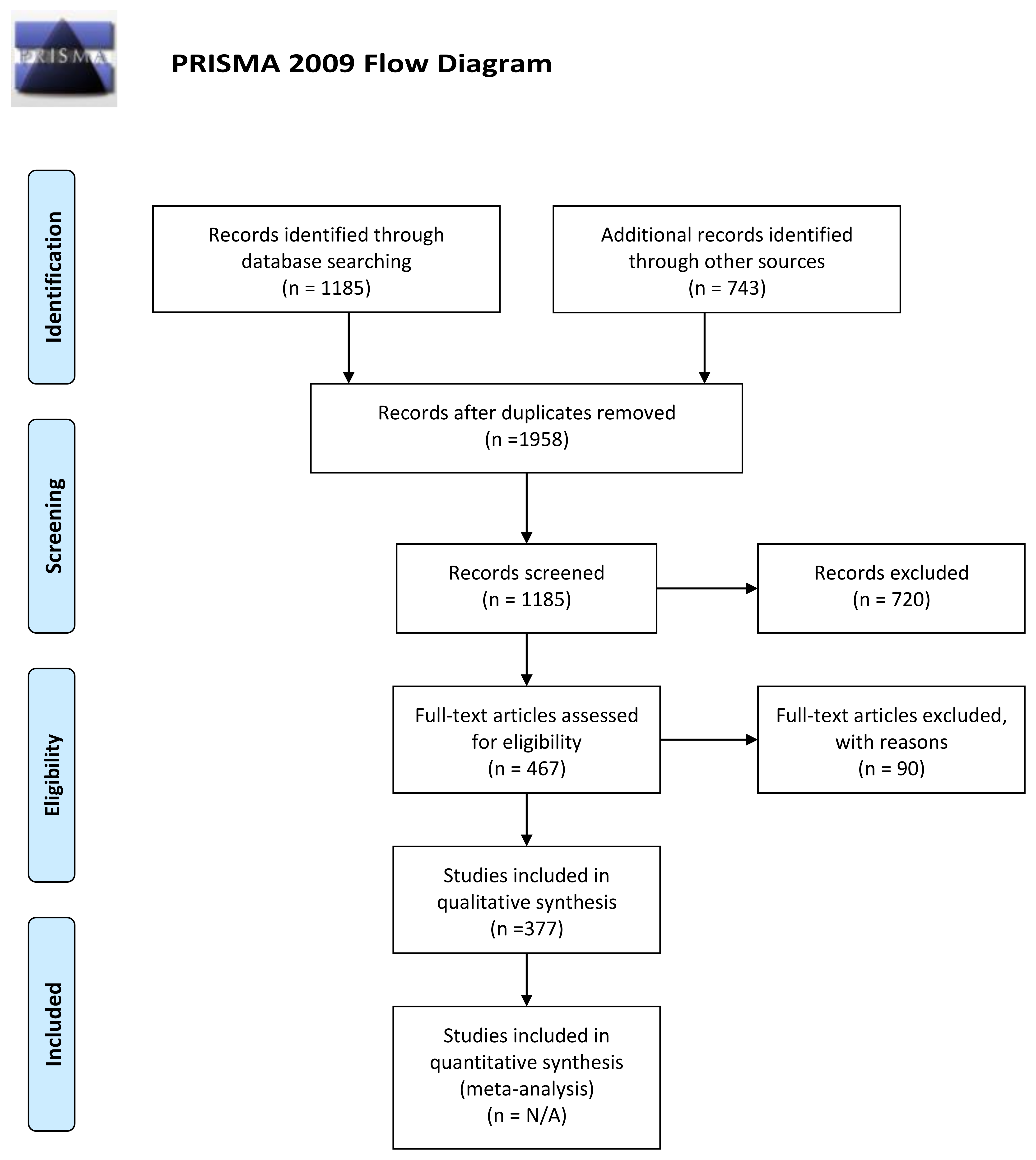
3.5. Systematic Review of Lyme Disease Causing Psychiatric Illness
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- IDSA/AAN/ACR. Draft Lyme Disease Guidelines. Available online: https://www.idsociety.org/practice-guideline/Lyme-Disease-Guideline-Public-Comments/ (accessed on 4 August 2019).
- Koons, C. Latest Suicide Data Show the Depth of U.S. Mental Health Crisis. Bloomberg Businessweek. 20 June 2019. Available online: https://www.bloomberg.com/news/articles/2019-06-20/latest-suicide-data-show-the-depth-of-u-s-mental-health-crisis (accessed on 4 August 2019).
- Bransfield, R.C. Neuropsychiatric Lyme Borreliosis: An Overview with a Focus on a Specialty Psychiatrist’s Clinical Practice. Healthcare 2018, 6, 104. [Google Scholar] [CrossRef] [PubMed]
- Bransfield, R.C. Suicide and Lyme and associated diseases. Neuropsychiatr. Dis. Treat. 2017, 13, 1575–1587. [Google Scholar] [CrossRef] [PubMed]
- Wormser, G.P.; Dattwyler, R.J.; Shapiro, E.D.; Halperin, J.J.; Steere, A.C.; Klempner, M.S.; Krause, P.J.; Bakken, J.S.; Strle, F.; Stanek, G.; et al. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: Clinical practice guidelines by the Infectious Diseases Society of America. Clin. Infect. Dis. 2006, 43, 1089–1134. [Google Scholar] [CrossRef] [PubMed]
- Johnson, L.; Stricker, R.B. The Infectious Diseases Society of America Lyme guidelines: A cautionary tale about the development of clinical practice guidelines. Philos. Ethics Humanit. Med. 2010, 5, 9. [Google Scholar] [CrossRef] [PubMed]
- Delong, A.K.; Blossom, B.; Maloney, E.L.; Phillips, S.E. Antibiotic retreatment of Lyme disease in patients with persistent symptoms: A biostatistical review of randomized, placebo-controlled, clinical trials. Contemp. Clin. Trials 2012, 33, 1132–1142. [Google Scholar] [CrossRef] [PubMed]
- Cameron, D.J. Generalizability in two clinical trials of Lyme disease. Epidemiol. Perspect. Innov. 2006, 3, 12. [Google Scholar] [CrossRef][Green Version]
- Khan, A.R.; Khan, S.; Zimmerman, V.; Baddour, L.M.; Tleyjeh, I.M. Quality and strength of evidence of the Infectious Diseases Society of America clinical practice guidelines. Clin. Infect. Dis. 2010, 51, 1147–1156. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.H.; Vielemeyer, O. Analysis of overall level of evidence behind Infectious Diseases Society of America practice guidelines. Arch. Intern. Med. 2011, 171, 18–22. [Google Scholar] [CrossRef]
- Lenzer, J.; Hoffman, J.R.; Furberg, C.D.; Ioannidis, J.P.; Guideline Panel Review Working Group. Ensuring the integrity of clinical practice guidelines: A tool for protecting patients. BMJ 2013, 347, f5535. [Google Scholar] [CrossRef]
- Davidsson, M. The Financial Implications of a Well-Hidden and Ignored Chronic Lyme Disease Pandemic. Healthcare 2018, 6, 16. [Google Scholar] [CrossRef]
- Graham, R.; Mancher, M.; Miller Wolman, D.; Greenfield, S.; Steinberg, E. (Eds.) Institute of Medicine (US) Committee on Standards for Developing Trustworthy Clinical Practice Guidelines; National Academies Press: Washington, DC, USA, 2011. [Google Scholar]
- A Lawsuit on Behalf of Lyme Disease Patients. Available online: https://www.thefirstepidemic.com/lyme-lawsuit (accessed on 4 August 2019).
- Tick-Borne Disease Working Group Report to Congress. pp. 72–74. Available online: https://www.hhs.gov/sites/default/files/tbdwg-report-to-congress-2018.pdf (accessed on 4 August 2019).
- How Many People Get Lyme Disease? CDC, 2018. Available online: https://www.cdc.gov/lyme/stats/humancases.html (accessed on 4 August 2019).
- Sears, C. Letter to: Tickborne Disease Working Group Office of the Assistant Secretary for Health U.S. Department of Health and Human Services. 2018. Available online: https://www.idsociety.org/globalassets/idsa/policy--advocacy/current_topics_and_issues/emerging_infections_and_biothreats/agency-efforts/112618-idsa-comments-on-tickborne-disease-working-group-report.pdf (accessed on 4 August 2019).
- CDC. Lyme Disease Case Definition. Available online: https://www.cdc.gov/lyme/stats/forms.html (accessed on 4 August 2019).
- Steere, A.C.; McHugh, G.; Damle, N.; Sikand, V.K. Prospective Study of Serologic Tests for Lyme Disease. Clin. Infect. Dis. 2008, 47, 188–195. [Google Scholar] [CrossRef] [PubMed]
- Wormser, G.; Schriefier, M.; Aguero-Rosenfeld, M.; Levin, A.; Steere, A.; Nadelman, R.B.; Dumler, J.S. Single-tier testing with the C6 peptide ELISA kit compared with two-tier testing for Lyme disease. Diagn. Microbiol. Infect. Dis. 2012, 75, 9–15. [Google Scholar] [CrossRef] [PubMed]
- Wormser, G.P.; Liveris, D.; Hanincová, K.; Brisson, D.; Ludin, S.; Stracuzzi, V.J.; Embers, M.E.; Philipp, M.T.; Levin, A.; Aguero-Rosenfeld, M.; et al. Effect of Borrelia burgdorferi genotype on the sensitivity of C6 and 2-tier testing in North American patients with culture-confirmed Lyme disease. Clin. Infect. Dis. 2008, 47, 910–914. [Google Scholar] [CrossRef] [PubMed]
- Branda, J.A.; Strle, K.; Nigrovic, L.E.; Lantos, P.M.; Lepore, T.J.; Damle, N.S.; Ferraro, M.J.; Steere, A.C. Evaluation of Modified 2-Tiered Serodiagnostic Testing Algorithms for Early Lyme Disease. Clin. Infect. Dis. 2017, 64, 1074–1080. [Google Scholar] [CrossRef] [PubMed]
- Branda, J.A.; Aguero-Rosenfeld, M.E.; Ferraro, M.J.; Johnson, B.J.; Wormser, G.P.; Steere, A.C. 2-tiered antibody testing for early and late Lyme disease using only an immunoglobulin G blot with the addition of a VlsE band as the second-tier test. Clin. Infect. Dis. 2010, 50, 20–26. [Google Scholar] [CrossRef] [PubMed]
- Leeflang, M.M.; Ang, C.W.; Berkhout, J.; Bijlmer, H.A.; Van Bortel, W.; Brandenburg, A.H.; Van Burgel, N.D.; Van Dam, A.P.; Dessau, R.B.; Fingerle, V.; et al. The diagnostic accuracy of serological tests for Lyme borreliosis in Europe: A systematic review and meta-analysis. BMC Infect. Dis. 2016, 16, 140. [Google Scholar] [CrossRef] [PubMed]
- Zeller, H.; Van Bortel, W. A Systematic Literature Review on the Diagnosis Accuracy of Serological Tests for Lyme Borreliosis. 2016. Available online: http://ecdc.europa.eu/en/publications/Publications/lyme-borreliosis-diagnostic-accuracy-serological-tests-systematic-review.pdf (accessed on 4 August 2019).
- Cook, M.J.; Puri, B.K. Application of Bayesian decision-making to laboratory testing for Lyme disease and comparison with testing for HIV. Int. J. Gen. Med. 2017, 10, 113–123. [Google Scholar] [CrossRef]
- Bacon, R.M.; Biggerstaff, B.J.; Schriefer, M.E.; Gilmore, R.D., Jr.; Philipp, M.T.; Steere, A.C.; Wormser, G.P.; Marques, A.R.; Johnson, B.J. Serodiagnosis of Lyme disease by kinetic enzyme-linked immunosorbent assay using recombinant VlsE1 or peptide antigens of Borrelia burgdorferi compared with 2-tiered testing using whole-cell lysates. J. Infect. Dis. 2003, 87, 1187–1199. [Google Scholar] [CrossRef]
- Cook, M.J.; Puri, B.K. Commercial test kits for detection of Lyme borreliosis: A meta-analysis of test accuracy. Int. J. Gen. Med. 2016, 9, 427–440. [Google Scholar] [CrossRef]
- An Assessment of Lyme Disease in Psychiatric Patients is Already Recommended in the American Psychiatric Association Practice Guidelines for the Evaluation of Adults, 3rd ed. Available online: https://psychiatryonline.org/doi/pdf/10.1176/appi.books.9780890426760 (accessed on 4 August 2019).
- Hájek, T.; Libiger, J.; Janovská, D.; Hájek, P.; Alda, M.; Höschl, C. Clinical and demographic characteristics of psychiatric patients seropositive for Borrelia burgdorferi. Eur. Psychiatry 2006, 21, 118–122. [Google Scholar] [CrossRef]
- Hájek, T.; Pasková, B.; Janovská, D.; Bahbouh, R.; Hájek, P.; Libiger, J.; Höschl, C. Higher prevalence of antibodies to Borrelia burgdorferi in psychiatric patients than in healthy subjects. Am. J. Psychiatry 2002, 159, 297–301. [Google Scholar] [CrossRef] [PubMed]
- Koola, M.M.; Sullivan, K.M.; Earl, A.K.; Feldman, S.M.; Richardson, C.; Vyas, G.R.; Wehring, H.J.; Kelly, D.L. Undiagnosed Lyme disease in adults with schizophrenia. Schizophr. Res. 2015, 168, 579–580. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Nadelman, R.B.; Herman, E.; Wormser, G.P. Screening for Lyme disease in hospitalized psychiatric patients: Prospective serosurvey in an endemic area. Mt. Sinai J. Med. 1997, 64, 409–412. [Google Scholar]
- Zomer, T.P.; Vermeeren, Y.M.; Landman, G.W.; Zwerink, M.; van Hees, B.C.; van Bemmel, T.; van Kooten, B. Depressive Symptoms in Patients Referred to a Tertiary Lyme Center: High Prevalence in Those Without Evidence of Lyme Borreliosis. Clin. Infect. Dis. 2017, 65, 1689–1694. [Google Scholar] [CrossRef] [PubMed]
- Bransfield, R.C.; Huismans, B.-D.; Phillips, S.; Scott, J.; Stricker, R. Peer-Reviewed Evidence of Persistence of Lyme Disease Spirochete Borrelia burgdorferi and Tick-Borne Diseases. Available online: https://www.ilads.org/wp-content/uploads/2018/07/CLDList-ILADS.pdf (accessed on 4 August 2019).
- Bransfield, R.C. Aggressiveness, violence, homicidality, homicide, and Lyme disease. Neuropsychiatr. Dis. Treat. 2018, 14, 693–713. [Google Scholar] [CrossRef]
- Fallon, B.A.; Levin, E.S.; Schweitzer, P.J.; Hardesty, D. Inflammation and Central Nervous System Lyme Disease. Neurobiol. Dis. 2010, 37, 534–541. [Google Scholar] [CrossRef]
- Bransfield, R.C. Relationship of Inflammation and Autoimmunity to Psychiatric Sequelae in Lyme Disease. Psychiatr. Ann. 2012, 42, 337–341. [Google Scholar] [CrossRef]
- Bransfield, R.C. The Psychoimmunology of Lyme/Tick-Borne Diseases and its Association with Neuropsychiatric Symptoms. Open Neurol. J. 2012, 6, 88–93. [Google Scholar] [CrossRef]
- Bransfield, R.C. The psychoimmunology of Lyme and associated diseases. Neurol. Psychiatry Brain Res. 2014, 20, 8. [Google Scholar] [CrossRef]
- Ramesh, G.; Didier, P.J.; England, J.D.; Santana-Gould, L.; Doyle-Meyers, L.A.; Martin, D.S.; Jacobs, M.B.; Philipp, M.T. Inflammation in the pathogenesis of Lyme neuroborreliosis. Am. J. Pathol. 2015, 185, 1344–1360. [Google Scholar] [CrossRef]
- Eckman, E.A.; Pacheco-Quinto, J.; Herdt, A.R.; Halperin, J.J. Neuroimmunomodulators in Neuroborreliosis and Lyme Encephalopathy. Clin. Infect. Dis. 2018, 67, 80–88. [Google Scholar] [CrossRef] [PubMed]
- Greenberg, R. Infections and childhood psychiatric disorders: Tick-borne illness and bipolar disorder in youth. Bipolar Disord. 2017, 3, 1. [Google Scholar] [CrossRef]
- Adams, W.V.; Rose, C.D.; Eppes, S.C.; Klein, J.D. Long-term cognitive effects of Lyme disease in children. Appl. Neuropsychol. 1999, 6, 39–45. [Google Scholar] [CrossRef] [PubMed]
- Askenazy, F.; Dor, E.; Benoit, M.; Dupuis, G.; Serret, S.; Myquel, M.; Seddiki, Y. Catatonia in a 14-year-old girl: Treatment with clonazepam and carbamazepine, a 10-year follow-up. Encephale 2010, 36, 46–53. [Google Scholar] [CrossRef] [PubMed]
- Belman, A.L.; Iyer, M.; Coyle, P.K.; Dattwyler, R. Neurologic manifestations in children with North American Lyme disease. Neurology 1993, 43, 2609–2614. [Google Scholar] [CrossRef] [PubMed]
- Bloom, B.J.; Wyckoff, P.M.; Meissner, H.C.; Steere, A.C. Neurocognitive abnormalities in children after classic manifestations of Lyme disease. Pediatr. Infect. Dis. J. 1998, 17, 189–196. [Google Scholar] [CrossRef]
- Bransfield, R.C. Lyme disease, comorbid tick-borne diseases, and neuropsychiatric disorders. Psychiatr. Times 2007, 24, 59–62. [Google Scholar]
- Bransfield, R.C. Preventable cases of autism: Relationship between chronic infectious disease and neurological outcome. Pediatric Health 2009, 3, 37. [Google Scholar] [CrossRef]
- Bransfield, R.C.; Kuhn, M. Autism and Lyme disease. JAMA 2013, 310, 856–857. [Google Scholar] [CrossRef]
- Bransfield, R.C. Intrusive symptoms and infectious encephalopathies. Neurol. Psychiatr. Brain Res. 2016, 22, 3–4. [Google Scholar] [CrossRef]
- Rothaus, C. A Girl with Seizures. NEJM 2015. Available online: http://blogs.nejm.org/now/index.php/a-girl-with-seizures/2015/05/22/comment-page1/#comment-225701 (accessed on 4 August 2019).
- Engman, M.-L.; Lindström, K.; Sallamba, M.; Hertz, C.; Sundberg, B.; Hansson, M.E.; Lindquist, L.; Orvell, C.; Lidefelt, K.J.; Sundin, M. One-year follow-up of tick- borne central nervous system infections in childhood. Pediatr. Infect. Dis. J. 2012, 31, 570–574. [Google Scholar] [CrossRef] [PubMed]
- Fallon, B.A.; Bird, H.; Hoven, C.; Cameron, D.; Liebowitz, M.R.; Shaffer, S. Psychiatric aspects of Lyme disease in children and adolescents: A community epidemiologic study in Westchester, New York. JSTD 1994, 1, 98–100. [Google Scholar]
- Fallon, B.A.; Kochevar, J.M.; Gaito, A.; Nields, J.A. The underdiagnosis of neuropsychiatric Lyme disease in children and adults. Psychiatr. Clin. N. Am. 1998, 21, 693–703. [Google Scholar] [CrossRef]
- Gentile, I.; Zappulo, E.; Militerni, R.; Pascotto, A.; Borgia, G.; Bravaccio, C. Etiopathogenesis of autism spectrum disorders: Fitting the pieces of the puzzle together. Med. Hypotheses 2013, 81, 26–35. [Google Scholar] [CrossRef] [PubMed]
- Kuhn, M.; Bransfield, R.C. Divergent opinions of proper Lyme disease diagnosis and implications for children co-morbid with autism spectrum disorder. Med. Hypotheses 2014, 83, 321–325. [Google Scholar] [CrossRef] [PubMed]
- Kuhn, M.; Grave, S.; Bransfield, R.; Harris, S. Long term antibiotic therapy may be an effective treatment for children co-morbid with Lyme disease and autism spectrum disorder. Med. Hypotheses 2012, 78, 606–615. [Google Scholar] [CrossRef]
- McAuliffe, P.; Brassard, M.R.; Fallon, B. Memory and executive functions in adolescents with posttreatment Lyme disease. Appl. Neuropsych. 2008, 15, 208–219. [Google Scholar] [CrossRef]
- Moses, J.M.; Riseberg, R.S.; Mansbach, J.M. Lyme disease presenting with persistent headache. Pediatrics 2003, 112, e477–e479. [Google Scholar] [CrossRef]
- Muller, N.; Riedel, M.; Straube, A.; Gunther, W.; Wilske, B. Increased antistreptococcal antibodies in patients with Tourette’s syndrome. Psychiatry Res. 2000, 94, 43–49. [Google Scholar] [CrossRef]
- Nicolson, G.L.; Gann, R.; Nicolson, N.L.; Haier, J. Evidence for Mycoplasma, ssp., Chalmydia pneumoniae, and Human Herpes-virus 6 coinfections in blood of patients with autistic spectrum disorders. J. Neurosci. Res. 2007, 85, 1143–1148. [Google Scholar] [CrossRef]
- Riedel, M.; Straube, A.; Schwarz, M.J.; Wilske, B.; Muller, N. Lyme disease presenting as Tourette’s syndrome. Lancet 1998, 351, 418–419. [Google Scholar] [CrossRef]
- Smith, V.; Traquina, D.N. Pediatric bilateral facial paralysis. Laryngoscope 1998, 108 Pt 1, 519–523. [Google Scholar] [CrossRef]
- Tager, F.A.; Fallon, B.A.; Keilp, J.; Rissenberg, M.; Jones, C.R.; Liebowitz, M.R. A controlled study of cognitive deficits in children with chronic Lyme disease. J. Neuropsychiatr. Clin. Neurosci. 2001, 13, 500–507. [Google Scholar] [CrossRef] [PubMed]
- Tager, F.A.; Fallon, B.A. Psychiatric and cognitive features of Lyme disease. Psychiatr. Ann. 2001, 31, 173–181. [Google Scholar] [CrossRef]
- Wormser, G.P.; Weitzner, E.; McKenna, D.; Nadelman, R.B.; Scavarda, C.; Molla, I.; Dornbush, R.; Visintainer, P.; Nowakowski, J. Long-term assessment of health-related quality of life in patients with culture-confirmed early Lyme disease. Clin. Infect. Dis. 2015, 61, 244–247. [Google Scholar] [CrossRef] [PubMed]
- Hassett, A.L.; Radvanski, D.C.; Buyske, S.; Savage, S.V.; Gara, M.; Escobar, J.I.; Sigal, L.H. Role of psychiatric comorbidity in chronic Lyme disease. Arthritis Rheum. 2008, 59, 1742–1749. [Google Scholar] [CrossRef]
- Greenberg, R. Study design questions regarding long-term assessment of health-related quality of life in patients with culture-confirmed early Lyme disease. Clin. Infect. Dis. 2015, 61, 1764–1765. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; The Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) Group. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bransfield, R.C.; Cook, M.J.; Bransfield, D.R. Proposed Lyme Disease Guidelines and Psychiatric Illnesses. Healthcare 2019, 7, 105. https://doi.org/10.3390/healthcare7030105
Bransfield RC, Cook MJ, Bransfield DR. Proposed Lyme Disease Guidelines and Psychiatric Illnesses. Healthcare. 2019; 7(3):105. https://doi.org/10.3390/healthcare7030105
Chicago/Turabian StyleBransfield, Robert C., Michael J. Cook, and Douglas R. Bransfield. 2019. "Proposed Lyme Disease Guidelines and Psychiatric Illnesses" Healthcare 7, no. 3: 105. https://doi.org/10.3390/healthcare7030105
APA StyleBransfield, R. C., Cook, M. J., & Bransfield, D. R. (2019). Proposed Lyme Disease Guidelines and Psychiatric Illnesses. Healthcare, 7(3), 105. https://doi.org/10.3390/healthcare7030105




