Effectiveness of Cognitive Behaviour Therapy for Mothers of Children with Food Allergy: A Case Series
Abstract
:1. Introduction
2. Methods
2.1. Design
2.2. Participants
2.2.1. Inclusion Criteria
2.2.2. Exclusion Criteria
2.3. Materials
2.3.1. Demographic and Food Allergy Questionnaire
2.3.2. Hospital Anxiety and Depression Scale (HADS)
2.3.3. Perceived Stress Scale (PSS-14)
2.3.4. Food Allergy Quality of Life-Parental Burden Scale (FAQL-PB)
2.3.5. The World Health Organisation QoL Scale (Brief Version) (WHOQOL-BREF)
2.3.6. Penn State Worry Questionnaire (PSWQ)
2.3.7. General Health Questionnaire-12 (GHQ-12)
2.3.8. Problems and Targets
2.4. Procedure
2.5. Data Analysis
3. Results
3.1. Demographic and Food Allergy Details of Parents and Children
| Parent and Child Characteristics | CBT Group | Control Group |
|---|---|---|
| Parents (n) | 5 | 6 |
| Sex (n%) female | 5 (100.0) | 6 (100) |
| Ethnic origin (n%) White British | 5 (100) | 6 (100) |
| Age, mean in years (SD) | 38.80 (4.38) | 33.00 (8.46) |
| Food Allergic Child | ||
| Sex (n%) male | 3 (60.0) | 3 (50.0) |
| female | 2 (40.0) | 3 (50.0) |
| Age, mean in years (SD) | 6.60 (3.36) | 5.00 (3.58) |
| Age range in years | 2–9 | 2–12 |
| Time since diagnosis, mean in years (SD) | 5.67 (3.23) | 3.87 (2.59) |
| Food Allergy, n (%) | ||
| Peanut | 3 (60.0) | 4 (66.67) |
| Treenuts | 3 (60.0) | 2 (33.33) |
| Egg | 5 (100.0) | 0 |
| Milk | 3 (60.0) | 3 (50.0) |
| Fish | 0 | 0 |
| Soy | 0 | 2 (33.33) |
| Tomato | 0 | 1 (16.67) |
| Number of Food Allergies, n (%) | ||
| 1 food | 1 (20.0) | 2 (33.33) |
| 2 foods | 1 (20.0) | 3 (50.0) |
| 3+ foods | 3 (60.0) | 1 (16.67) |
| Type of Symptoms, n (%) | ||
| Respiratory | 4 (80.0) | 4 (66.67) |
| Swelling of face, lips, tongue, eyes | 2 (40.0) | 4 (66.67) |
| Gastrointestinal | 5 (100.0) | 5 (83.33) |
| Skin rash/hives | 3 (60.0) | 5 (83.33) |
| History of anaphylaxis | 3 (60.0) | 2 (33.33) |
| Presence of Asthma, Hayfever, Eczema | 5 (100.0) | 6 (100.0) |
| Medication Prescribed, n (%) | ||
| Adrenalin auto-injector | 3 (60.0) | 2 (33.33) |
| Antihistamines | 6 (100.0) | 6 (100.0) |
3.2. A CBT Model for Parents of Children with Food Allergy
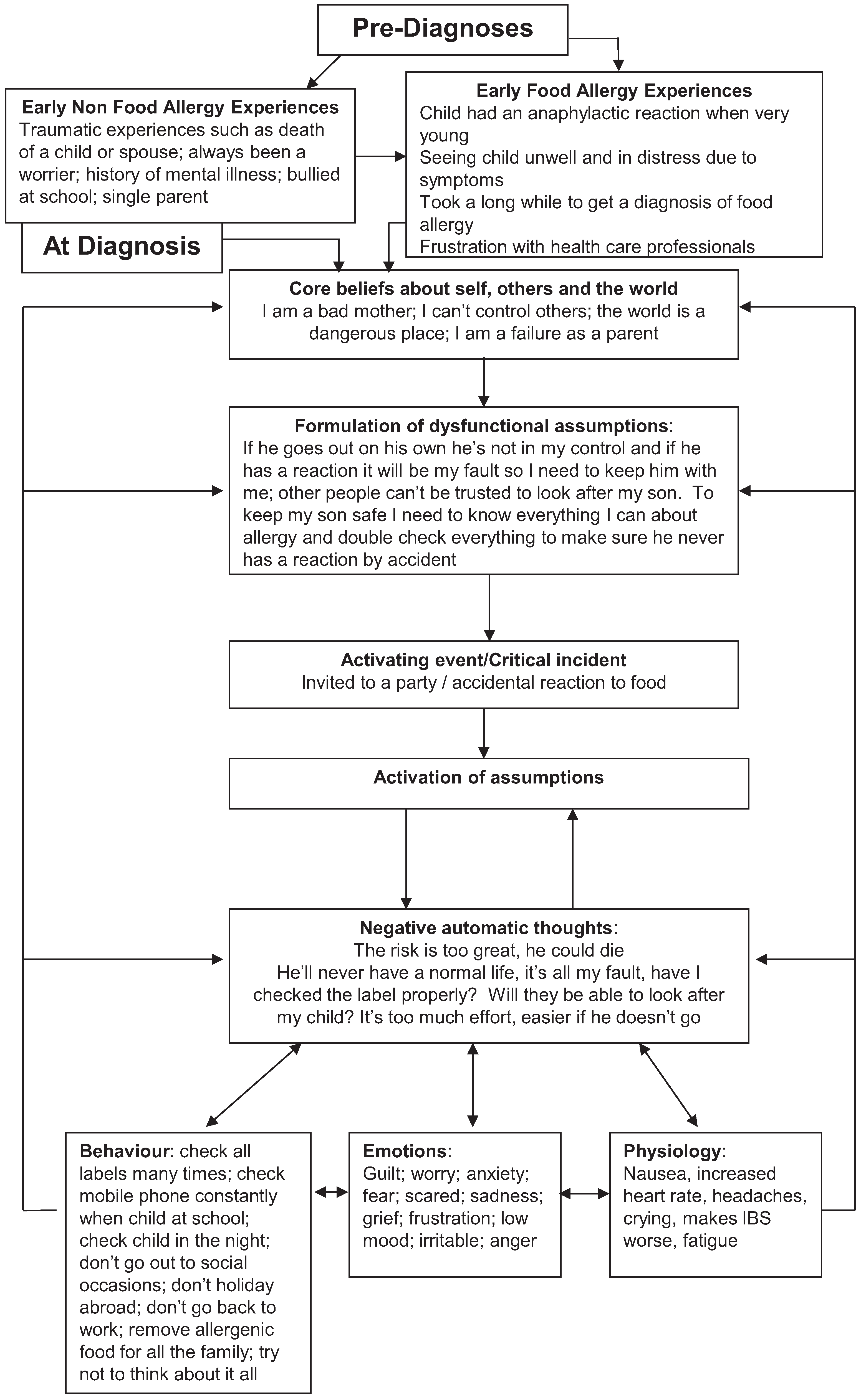
3.3. Problems and Targets and Interventions Used
| Problem Statements |
|---|
| I feel very anxious and cry when I think about what might happen if my son has a serious reaction as I feel as if I won’t know what to do and he might die, so I try not to think about it or talk about it. |
| I am very anxious when my son is not with me and I worry that he might eat something he shouldn’t and have a bad reaction, so I check my mobile every ten minutes in case I have missed a call about him, which makes me more anxious and I can’t concentrate on my work. |
| I worry about how my daughter will cope as she gets older and more independent and wants to go out on her own with her friends. I am scared she won’t know what to do if she has a bad reaction so I find it hard to let her have some control over what she eats. |
| I feel guilty asking other people to look after my daughter as they need to know what she can and cannot eat and how to give her an injection of adrenaline if she has a bad reaction, so most of the time I don’t let her go and stay with other people and that makes me feel guilty too. |
| When we are going through a bad time with my daughter’s eczema I don’t get a lot of sleep and during the day I can feel really frustrated and angry and I shout at my daughter, which makes me feel guilty as she gets upset. |
| I feel very anxious when we go out for the day as I have to do all the planning and work out what my son will be able to eat, I don’t get much help with this and I get frustrated and angry about that. |
3.4. Impact of CBT on Quality of Life
| Target Statements | Interventions Used |
|---|---|
| I would like to feel less anxious about my son having a bad reaction and be more confident in knowing what to do if he does | 1. Graded exposure to information about anaphylactic shock to reduce anxiety, including watching educational videos |
| 2. Psychoeducation about what might happen if a child goes into anaphylactic shock | |
| 3. Role play using a trainer AAI with the parent and therapist | |
| 4. Role play using a trainer AAI by the parent with their child | |
| I would like to worry less about my child becoming more independent as he gets older and trust him to take more responsibility for his allergies | 1. Worry tree to help decide what worries are controllable and what to do about them |
| 2. Behavioural experiment to see what happens if | |
| a. they allow child to read own food labels and decide what they can eat | |
| b. let child remember their medication and put their own creams on for their eczema | |
| 3. Role play with child showing their friends how to use the trainer AAI in an emergency | |
| I would like to be able to leave my child with people and not feel guilty about this, so that I have more time for myself, and worry less when he’s not with me | 1. Psychoeducation and role play regarding how parent might teach someone else what they need to know about their child’s allergy and use of an AAI |
| 2. Behaviour experiment to test out consequences of leaving child with someone else | |
| 3. Exploration of dysfunctional ways of thinking and making assumptions based on mind reading of others | |
| I would like to be able to learn how to cope with things when my child is having a bad time with her eczema and not feel angry, upset or low | 1. Diary to keep a log of mood |
| 2. Diary to log positive events and emotions in order to raise mood and self-esteem | |
| 3. Challenging negative automatic thoughts such as “I cannot cope with this” and looking at evidence for and against such thoughts | |
| I would like to look back on the time when my daughter was tiny and very ill with her allergy and not get upset about it and remember the good times | 1. Emotional writing and re-living of past experiences to reduce grief associated with traumatic experiences |
| 2. Recording positive experiences from the past and the positive consequences that have occurred because of the food allergy, such as a better relationship with grandparents |
| Participant | N of Problems | Baseline | End of Treatment | Change Score | |||
|---|---|---|---|---|---|---|---|
| Behaviour | Discomfort | Behaviour | Discomfort | Behaviour | Discomfort | ||
| 1 | 4 | 7.0 | 7.5 | 4.0 | 4.5 | 3.0 | 3.0 |
| 2 | 4 | 5.5 | 6.25 | 1.5 | 2.25 | 4.0 | 4.0 |
| 3 | 3 | 7.3 | 8.0 | 3.7 | 3.3 | 3.6 | 4.7 |
| 4 | 3 | 6.0 | 8.0 | 2.0 | 2.0 | 4.0 | 6.0 |
| 5 | 4 | 7.5 | 7.5 | 2.75 | 3.5 | 4.75 | 4.0 |
| Total | 6.66 | 7.45 | 2.79 | 3.11 | 3.87 | 4.34 | |
| N of Targets | Baseline | End of Treatment | Change Score | ||||
| Behaviour | Discomfort | Behaviour | Discomfort | Behaviour | Discomfort | ||
| 1 | 4 | 8.0 | 8.0 | 2.0 | 2.0 | 6.0 | 6.0 |
| 2 | 4 | 5.75 | 5.25 | 1.25 | 1.75 | 4.5 | 3.5 |
| 3 | 3 | 7.0 | 7.0 | 4.3 | 3.7 | 2.7 | 3.3 |
| 4 | 4 | 7.75 | 8.0 | 1.25 | 1.25 | 6.5 | 6.75 |
| 5 | 4 | 7.75 | 7.75 | 2.75 | 3.25 | 4.75 | 4.5 |
| Total | 7.25 | 7.20 | 2.31 | 2.39 | 4.89 | 4.81 | |
3.5. Impact of CBT on Psychological Distress
4. Discussion
4.1. A New CBT Model for Parents of Children with Food Allergy
4.2. Psychological Outcomes for Parents of Food Allergic Children
4.3. Quality of Life for Parents of Food Allergic Children
4.4. Limitations of the Study and Areas for Further Research
4.5. Implications of the Results for Clinical Practice
5. Conclusions
Supplementary Files
Supplementary File 1Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| AAI | Adrenaline auto-injector |
| CBT | Cognitive Behaviour Therapy |
| FAQL-PB | Food Allergy Quality of Life-Parental Burden questionnaire |
| GHQ-12 | General Health Questionnaire |
| HADS | Hospital Anxiety and Depression Scale |
| PSS | Perceived Stress Scale |
| PWSQ | Penn State Worry Questionnaire |
| QoL | Quality of Life |
| WHOQoL-BREF | World Health Organisation Quality of Life Scale |
References
- Sicherer, S.H. Epidemiology of food allergy. J. Allergy Clin. Immunol. 2011, 127, 594–602. [Google Scholar] [CrossRef] [PubMed]
- Kotz, D.; Simpson, C.R.; Sheikh, A. Incidence, prevalence, and trends of general practitioner-recorded diagnosis of peanut allergy in England, 2001 to 2005. J. Allergy Clin. Immunol. 2011, 127, 623–630. [Google Scholar] [CrossRef] [PubMed]
- Cummings, A.; Knibb, R.C.; King, R.; Lucas, J. The psychosocial impact of food allergy on children and adolescents: A review. Allergy 2010, 65, 933–945. [Google Scholar] [CrossRef] [PubMed]
- King, R.M.; Knibb, R.C.; Hourihane, J.O. Impact of peanut allergy on quality of life, stress and anxiety in the family. Allergy 2009, 64, 461–468. [Google Scholar] [CrossRef] [PubMed]
- Cummings, A.; Knibb, R.C.; Erlewyn-Lajeunesse, M.; King, R.; Hich, G.; Lucas, J. Management of nut allergy influences quality of life and anxiety in children and their mothers. Pediatr. Allergy Immunol. 2010, 21, 586–594. [Google Scholar] [CrossRef] [PubMed]
- Akeson, N.; Worth, A.; Sheikh, A. The psychosocial impact of anaphylaxis on young people and their parents. Clin. Exp. Allergy 2007, 37, 1213–1220. [Google Scholar] [CrossRef] [PubMed]
- Gillespie, C.A.; Woodgate, R.L.; Chalmers, K.I.; Watson, W.T. “Living with risk”: Mothering a child with food-induced anaphylaxis. J. Pediatr. Nurs. 2007, 22, 30–42. [Google Scholar] [CrossRef] [PubMed]
- Boyce, J.A.; Assa’ad, A.; Burks, A.W.; Jones, S.M.; Sampson, H.A.; Wood, R.A.; Plaut, M.; Cooper, S.F.; Fenton, M.J.; Arshad, S.H.; et al. Guidelines for the diagnosis and management of food allergy in the United States: Report of the NIAID-Sponsored expert panel. J. Allergy Clin. Immunol. 2010, 126, S1–S58. [Google Scholar] [CrossRef] [PubMed]
- Knibb, R.C.; Semper, H. Impact of suspected food allergy on emotional distress and family life of parents prior to allergy diagnosis. Pediatr. Allergy Immunol. 2013, 24, 798–803. [Google Scholar] [CrossRef] [PubMed]
- LeBovidge, J.S.; Timmons, K.; Rich, C. Evaluation of a group intervention for children with food allergy and their parents. Ann. Allergy Asthma Immunol. 2008, 101, 160–165. [Google Scholar] [CrossRef]
- Polloni, L.; Lazzarotto, F.; Bonaguro, R.; Toniolo, A.; Celegato, N.; Muraro, A. Psychological care of food allergic children and their families: An exploratory analysis. Pediatr. Allergy Immunol. 2014, 26, 80–92. [Google Scholar] [CrossRef] [PubMed]
- Starcevic, M. Anxiety states: A review of conceptual and treatment issues. Curr. Opin. Psychiatry 2006, 19, 79–83. [Google Scholar] [CrossRef] [PubMed]
- Hunot, V.; Churchill, R.; Teixeira, V.; de Lima, M. Psychological therapies for generalised anxiety disorders. Cochrane Database Syst. Rev. 2007. [Google Scholar] [CrossRef]
- Ross, C.J.M.; Davis, T.M.A.; MacDonald, G.F. Cognitive-behavioural treatment combined with asthma education for adults with asthma and coexisting panic disorder. Clin. Nurs. Res. 2005, 14, 131–157. [Google Scholar] [CrossRef] [PubMed]
- Coventry, P.A.; Gellatly, J.L. Improving outcomes for COPD patients with mild-to-moderate anxiety and depression: A systematic review of cognitive behavioural therapy. Br. J. Health Psychol. 2008, 13, 381–400. [Google Scholar] [CrossRef] [PubMed]
- Pu, C.; van den Bergh, O.; Lemaigre, V.; Demedts, M.; Verleden, G. Evaluation of an individualised asthma programme directed at behavioural change. Eur. Respir. J. 2003, 21, 109–115. [Google Scholar]
- Parry, G.D.; Cooper, C.L.; Moore, J.M.; Yadegarfar, G.; Campbell, M.J.; Esmonde, L.; Morice, A.H.; Hutchcroft, B.J. Cognitive behavioural intervention for adults with anxiety complications of asthma: Prospective randomised trial. Respir. Med. 2010, 106, 802–810. [Google Scholar] [CrossRef] [PubMed]
- Wong, F.K.D.; Poon, A. Cognitive behavioural group treatment for Chinese parents with children with developmental disabilities in Melbourne, Australia: An efficacy study. Aust. N. Z. J. Psychiatry 2010, 44, 742–749. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders-Revised, 4th ed.; American Psychiatric Press: Washington, DC, USA, 2000. [Google Scholar]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Moorey, S.; Greer, S.; Watson, M.; Gorman, C.; Rowden, L.; Tunmore, R.; Robertson, B.; Bliss, J. The factor structure and factor stability of the hospital anxiety and depression scale in patients with cancer. Br. J. Psychiatry 1991, 158, 255–259. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Kamarck, T.; Mermelstein, R. A global measure of perceived stress. J. Health Soc. Behav. 1983, 24, 385–396. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Williamson, G.M. The Social Psychology of Health; Sage: London, UK, 1988. [Google Scholar]
- Cohen, B.L.; Noone, S.; Munoz-Furlong, A.; Sicherer, S.H. Development of a questionnaire to measure quality of life in families with a child with food allergy. J. Allergy Clin. Immunol. 2004, 114, 1159–1163. [Google Scholar] [CrossRef] [PubMed]
- Knibb, R.C.; Stalker, C. Validation of the food allergy quality of life-parental burden questionnaire in the UK. Qual. Life Res. 2013, 22, 1841–1849. [Google Scholar] [CrossRef] [PubMed]
- Skevington, S.M.; Lotfy, M.; O’Connell, K.A. The World Health Organization’s WHOQOL-BREF quality of life assessment: Psychometric properties and results of the international field trial. A report from the WHOQOL Group. Qual. Life Res. 2004, 13, 299–310. [Google Scholar] [CrossRef] [PubMed]
- Meyer, T.J.; Miller, M.L.; Metzger, R.L.; Borkovec, T.D. Development and validation of the penn state worry questionnaire. Behav. Res. Ther. 1990, 28, 487–495. [Google Scholar] [CrossRef]
- Goldberg, D.; Williams, P. A User’s Guide to the General Health Questionnaire; NFER-Nelson: Slough, UK, 1988. [Google Scholar]
- Richards, D.A.; McDonald, B. Behavioural Psychotherapy: A Handbook for Nurses; Sage: London, UK, 1990. [Google Scholar]
- Grant, A.; Townend, M.; Mills, J.; Cockx, A. Assessment and Case Formulation in Cognitive Behavioural Therapy; Sage: London, UK, 2008. [Google Scholar]
- Field, A. Discovering Statistics Using IBM SPSS Statistics, 4th ed.; Sage: London, UK, 2013. [Google Scholar]
- Westbrook, D.; Kennerley, H.; Kirk, J. An Introduction to Cognitive Behaviour Therapy: Skills and Applications; Sage: London, UK, 2007. [Google Scholar]
- Williams, N.A.; Parra, G.R.; Elkin, T.D. Subjective distress and emotional resources in parents of children with food allergy. Child. Health Care 2009, 38, 213–227. [Google Scholar] [CrossRef]
- Springston, E.E.; Smith, B.; Shulruff, J.; Pongracic, J.; Holl, J.; Gupta, R.S. Variations in quality of life among caregivers of food allergic children. Ann. Allergy Asthma Immunol. 2010, 105, 287–294. [Google Scholar] [CrossRef] [PubMed]
- Herbert, L.J.; Dahlquist, L.M. Perceived history of anaphylaxis and parental overprotection, autonomy, anxiety and depression in food allergic young adults. J. Clin. Psychol. Med. Settings 2008, 15, 261–269. [Google Scholar] [CrossRef] [PubMed]
- Ravid, N.L.; Annunziato, R.A.; Ambrose, M.A.; Chuang, K.; Mullarkey, C.; Sicherer, S.H.; Shemesh, E.; Cox, A.L. Mental health and quality-of-life concerns related to the burden of food allergy. Immunol. Allergy Clin. North Am. 2012, 32, 83–95. [Google Scholar] [CrossRef] [PubMed]
- Rouf, K.; White, L.; Evans, K. A qualitative investigation into the maternal experience of having a young child with severe food allergy. Clin. Child. Psychol. Psychiatry 2012, 17, 49–64. [Google Scholar] [CrossRef] [PubMed]
- Prouessel, G.; Deschildre, A.; Castelain, C. Parental knowledge and use of epinephrine auto-injector for children with food allergy. Pediatr. Allergy Immunol. 2006, 17, 221–226. [Google Scholar] [CrossRef] [PubMed]
- Umasunthar, T.; Procktor, A.; Hodes, M.; Smith, J.G.; Gore, C.; Cox, H.E.; Marrs, T.; Hanna, H.; Phillips, K.; Pinto, C.; et al. Patients’ ability to treat anaphylaxis using adrenaline autoinjectors: A randomised controlled trial. Allergy 2015, 70, 855–863. [Google Scholar] [CrossRef] [PubMed]
- Roy, K.M.; Roberts, M.C. Peanut allergy in children: Relationships to health-related quality of life, anxiety and parental stress. Clin. Pediatr. 2011, 50, 1045–1051. [Google Scholar] [CrossRef] [PubMed]
- Martin, D.J.; Gorske, J.P.; Davis, M.K. Relation of the therapeutic alliance with outcome and other variables: A meta-analytic review. J. Consult. Clin. Psychol. 2000, 68, 438–450. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the author; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Knibb, R.C. Effectiveness of Cognitive Behaviour Therapy for Mothers of Children with Food Allergy: A Case Series. Healthcare 2015, 3, 1194-1211. https://doi.org/10.3390/healthcare3041194
Knibb RC. Effectiveness of Cognitive Behaviour Therapy for Mothers of Children with Food Allergy: A Case Series. Healthcare. 2015; 3(4):1194-1211. https://doi.org/10.3390/healthcare3041194
Chicago/Turabian StyleKnibb, Rebecca C. 2015. "Effectiveness of Cognitive Behaviour Therapy for Mothers of Children with Food Allergy: A Case Series" Healthcare 3, no. 4: 1194-1211. https://doi.org/10.3390/healthcare3041194
APA StyleKnibb, R. C. (2015). Effectiveness of Cognitive Behaviour Therapy for Mothers of Children with Food Allergy: A Case Series. Healthcare, 3(4), 1194-1211. https://doi.org/10.3390/healthcare3041194






