Effectiveness of Nature-Based Interventions in Reducing Agitation Among Older Adults with Dementia: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Inclusion Criteria
2.2. Search Strategy
2.3. Data Collection Process and Data Items
2.4. Quality Assessment of Eligible Studies
2.5. Data Synthesis and Analysis
2.6. Sensitivity Analysis
3. Results
3.1. Study Selection
3.2. Study Characteristics
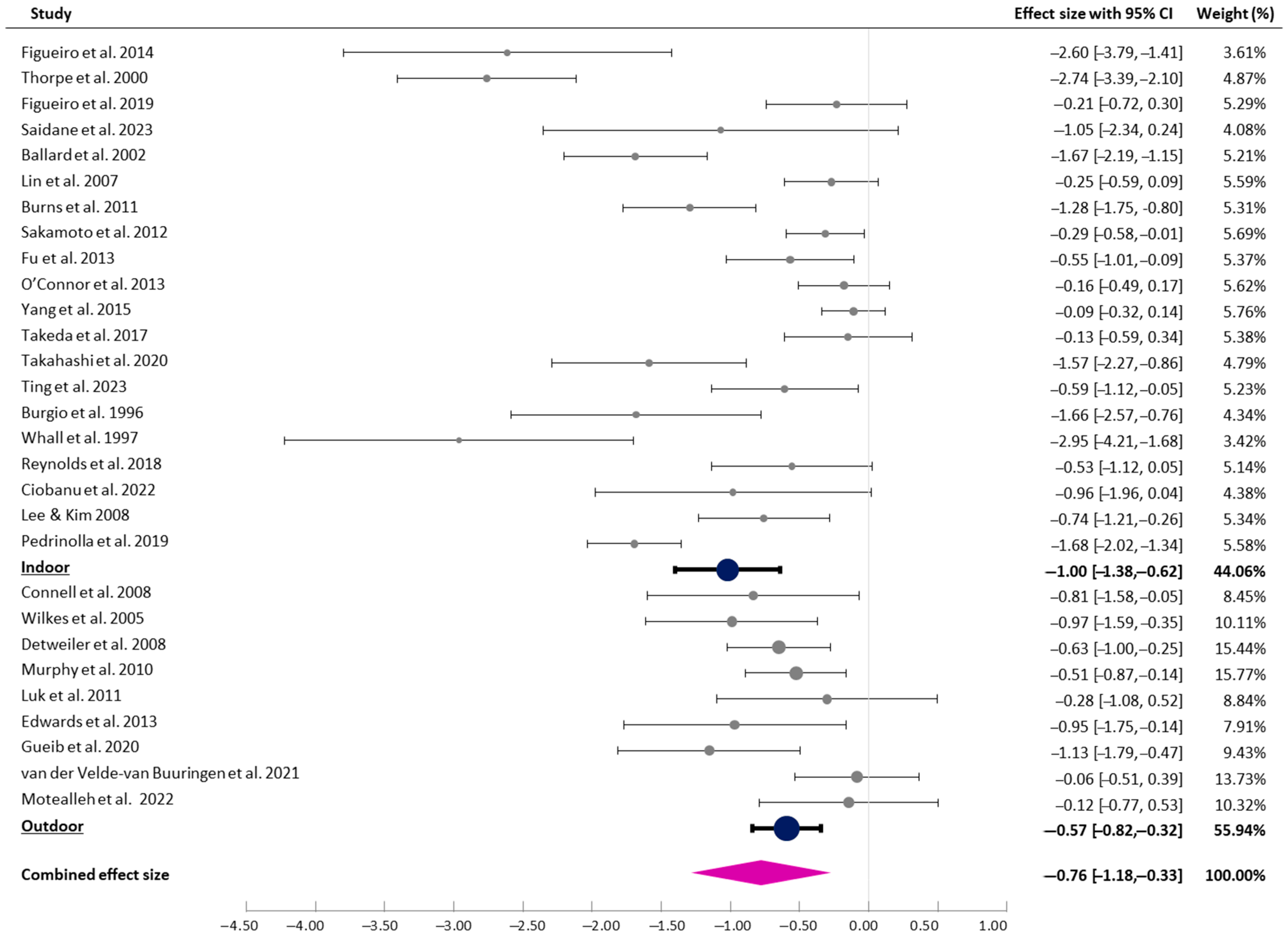
3.3. Immediate Effects of Interventions
3.4. Subgroup Analyses
3.4.1. Intervention Settings
3.4.2. The Presence of Social Interaction
3.4.3. Types of Experiences with Nature
3.4.4. Duration of Interventions
4. Discussion
4.1. The Effect of Intervention Settings
4.2. The Effect of Social Interaction
4.3. Limitations of This Study
4.4. Recommendations for Future Research and Practice
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A. Quality Assessment of Methodological Quality
| Study | Q1 | Q2 | Q3 | Q4 | Q5 | Q6 | Q7 | Q8 | Q9 | Q10 | Q11 | Q12 | Q13 | Total (%) | Methodological Quality |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Figueiro et al., 2019 [32] | Y | U | Y | Y | N/A | N/A | U | Y | Y | Y | Y | Y | Y | 69 | Adequate |
| Ballard et al., 2002 [38] | Y | Y | U | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 92 | Strong |
| Lin et al., 2007 [39] | Y | U | Y | Y | U | Y | U | Y | Y | Y | Y | Y | Y | 77 | Moderate |
| Burns et al., 2011 [40] | Y | Y | U | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | 85 | Moderate |
| Sakamoto et al., 2012 [41] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 100 | Strong |
| Fu et al., 2013 [31] | Y | U | U | Y | U | Y | U | Y | Y | Y | N | Y | Y | 62 | Adequate |
| O’Connor et al., 2013 [42] | Y | Y | Y | Y | N | Y | N | Y | Y | Y | N | Y | Y | 77 | Moderate |
| Yang et al., 2015 [43] | Y | Y | N | Y | U | Y | U | Y | Y | Y | Y | Y | Y | 77 | Moderate |
| Takahashi et al., 2020 [45] | U | U | Y | Y | N/A | Y | U | Y | Y | Y | Y | Y | U | 62 | Adequate |
| Pedrinolla et al., 2019 [51] | Y | U | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 92 | Strong |
| Luk et al., 2011 [55] | U | U | Y | Y | U | U | N | Y | Y | Y | Y | Y | Y | 62 | Adequate |
| Study | Q1 | Q2 | Q3 | Q4 | Q5 | Q6 | Q7 | Q8 | Q9 | Total (%) | Methodological Quality |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Figueiro et al., 2014 [29] | Y | N | Y | Y | Y | Y | Y | Y | Y | 89 | Strong |
| Saidane et al., 2023 [36] | Y | N | Y | N | Y | Y | Y | Y | Y | 78 | Moderate |
| Thorpe et al., 2000 [33] | Y | N | Y | Y | Y | Y | Y | Y | Y | 89 | Strong |
| Figueiro et al., 2020 [34] | Y | N | Y | Y | Y | Y | Y | Y | Y | 89 | Strong |
| Figueiro and Kales 2021 [35] | Y | Y | Y | N | Y | Y | U | Y | Y | 78 | Moderate |
| Connell et al., 2007 [37] | Y | Y | Y | Y | Y | Y | U | Y | Y | 89 | Strong |
| Takeda et al., 2017 [44] | Y | N | Y | Y | Y | Y | Y | Y | Y | 89 | Strong |
| Ting et al., 2023 [46] | Y | Y | Y | Y | Y | Y | U | Y | Y | 89 | Strong |
| Burgio et al., 1996 [47] | Y | N | Y | Y | Y | Y | Y | Y | Y | 89 | Strong |
| Whall et al., 1997 [48] | Y | Y | Y | Y | Y | Y | Y | Y | Y | 100 | Strong |
| Reynolds et al., 2018 [49] | Y | N | Y | U | Y | Y | Y | Y | Y | 78 | Moderate |
| Ciobanu et al., 2022 [30] | Y | N | Y | U | Y | Y | U | Y | Y | 67 | Adequate |
| Lee & Kim 2008 [50] | Y | N | Y | U | Y | Y | Y | Y | Y | 78 | Moderate |
| Wilkes et al., 2005 [52] | Y | N | Y | N | Y | Y | U | Y | Y | 67 | Adequate |
| Detweiler et al., 2008 [53] | Y | N | Y | Y | Y | Y | Y | Y | Y | 89 | Moderate |
| Murphy et al., 2010 [54] | Y | N | Y | U | Y | Y | U | Y | Y | 67 | Adequate |
| Edwards et al., 2012 [56] | Y | N | Y | N | Y | Y | Y | Y | Y | 78 | Moderate |
| Gueib et al., 2020 [7] | Y | Y | Y | Y | Y | Y | U | Y | Y | 89 | Strong |
| van der Velde-van Buuringen et al., 2021 [8] | Y | N | Y | Y | Y | Y | Y | Y | Y | 89 | Moderate |
| Motealleh et al., 2022 [9] | Y | N | Y | Y | Y | Y | U | Y | Y | 78 | Moderate |
References
- Cerejeira, J.; Lagarto, L.; Mukaetova-Ladinska, E.B. Behavioral and psychological symptoms of dementia. Front. Neurol. 2012, 3, 73. [Google Scholar] [CrossRef] [PubMed]
- Jamieson, H.; Abey-Nesbit, R.; Nishtala, P.S.; Allore, H.; Han, L.; Deely, J.M.; Pickering, J.W. Predictors of residential care admission in community-dwelling older people with dementia. J. Am. Med. Dir. Assoc. 2020, 21, 1665–1670. [Google Scholar] [CrossRef] [PubMed]
- Bossen, A. The importance of getting back to nature for people with dementia. J. Gerontol. Nurs. 2010, 36, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Marquardt, G.; Bueter, K.; Motzek, T. Impact of the design of the built environment on people with dementia: An evidence-based review. Health Environ. Res. Des. J. 2014, 8, 127–157. [Google Scholar] [CrossRef] [PubMed]
- Chaudhury, H.; Cooke, H.A.; Cowie, H.; Razaghi, L. The Influence of the Physical Environment on Residents with Dementia in Long-Term Care Settings: A Review of the Empirical Literature. Gerontologist 2018, 58, e325–e337. [Google Scholar] [CrossRef] [PubMed]
- Barrett, P.; Sharma, M.; Zeisel, J. Optimal spaces for those living with dementia: Principles and evidence. Build. Res. Inf. 2019, 47, 734–746. [Google Scholar] [CrossRef]
- Gueib, C.; Pop, A.; Bannay, A.; Nassau, E.; Fescharek, R.; Gil, R.; Luc, A.; Rivasseau Jonveaux, T. Impact of a healing garden on self-consciousness in patients with advanced Alzheimer’s disease: An exploratory study. J. Alzheimer’s Dis. 2020, 75, 1283–1300. [Google Scholar] [CrossRef] [PubMed]
- van der Velde-van Buuringen, M.; Achterberg, W.P.; Caljouw, M.A.A. Daily garden use and quality of life in persons with advanced dementia living in a nursing home: A feasibility study. Nurs. Open 2021, 8, 1243–1253. [Google Scholar] [CrossRef] [PubMed]
- Motealleh, P.; Moyle, W.; Jones, C.; Dupre, K. The Impact of a Dementia-Friendly Garden Design on People With Dementia in a Residential Aged Care Facility: A Case Study. Health Environ. Res. Des. J. 2022, 15, 196–218. [Google Scholar] [CrossRef] [PubMed]
- Wilson, E.O. Biophilia; Harvard University Press: London, UK, 1986. [Google Scholar]
- Choe, E.Y.; Jorgensen, A.; Sheffield, D. Does a natural environment enhance the effectiveness of Mindfulness-Based Stress Reduction (MBSR)? Examining the mental health and wellbeing, and nature connectedness benefits. Landsc. Urban Plan. 2020, 202, 103886. [Google Scholar] [CrossRef]
- Hartig, T.; Mitchell, R.; De Vries, S.; Frumkin, H. Nature and health. Annu. Rev. Public Health 2014, 35, 207–228. [Google Scholar] [CrossRef] [PubMed]
- Maller, C.; Townsend, M.; Pryor, A.; Brown, P.; St Leger, L. Healthy nature healthy people:‘contact with nature’as an upstream health promotion intervention for populations. Health Promot. Int. 2006, 21, 45–54. [Google Scholar] [CrossRef] [PubMed]
- Orr, N.; Wagstaffe, A.; Briscoe, S.; Garside, R. How do older people describe their sensory experiences of the natural world? A systematic review of the qualitative evidence. BMC Geriatr. 2016, 16, 116. [Google Scholar] [CrossRef] [PubMed]
- Bennett, J.; Wolverson, E.; Price, E. Me, myself, and nature: Living with dementia and connecting with the natural world—More than a breath of fresh air? A literature review. Dementia 2022, 21, 2351–2376. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez, M.T.; Kirkevold, M. Benefits of sensory garden and horticultural activities in dementia care: A modified scoping review. J. Clin. Nurs. 2014, 23, 2698–2715. [Google Scholar] [CrossRef] [PubMed]
- Murroni, V.; Cavalli, R.; Basso, A.; Borella, E.; Meneghetti, C.; Melendugno, A.; Pazzaglia, F. Effectiveness of therapeutic gardens for people with dementia: A systematic review. Int. J. Environ. Res. Public Health 2021, 18, 9595. [Google Scholar] [CrossRef] [PubMed]
- Motealleh, P.; Moyle, W.; Jones, C.; Dupre, K. Creating a dementia-friendly environment through the use of outdoor natural landscape design intervention in long-term care facilities: A narrative review. Health Place 2019, 58, 102148. [Google Scholar] [CrossRef] [PubMed]
- Kellert, S.; Calabrese, E. The Practice of Biophilic Design; Terrapin Bright LLC: London, UK, 2015; Volume 3. [Google Scholar]
- Goudriaan, I.; van Boekel, L.C.; Verbiest, M.E.A.; van Hoof, J.; Luijkx, K.G. Dementia enlightened?! a systematic literature review of the influence of indoor environmental light on the health of older persons with dementia in long-term care facilities. Clin. Interv. Aging 2021, 16, 909–937. [Google Scholar] [CrossRef] [PubMed]
- D’Andrea, F.; Tischler, V.; Dening, T.; Churchill, A. Olfactory stimulation for people with dementia: A rapid review. Dementia 2022, 21, 1800–1824. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Yuan, X. Smellscape as a healing factor in institutional gardens to enhance health and well-being for older people with dementia: A scoping review. J. Clin. Nurs. 2024, 33, 454–468. [Google Scholar] [CrossRef] [PubMed]
- Al Ghassani, A.; Rababa, M.; Abu Khait, A. Agitation in people with dementia: A concept analysis. Nurs. Forum 2021, 56, 1015–1023. [Google Scholar] [CrossRef] [PubMed]
- Barker, T.H.; Stone, J.C.; Sears, K.; Klugar, M.; Leonardi-Bee, J.; Tufanaru, C.; Aromataris, E.; Munn, Z. Revising the JBI quantitative critical appraisal tools to improve their applicability: An overview of methods and the development process. JBI Evid. Synth. 2023, 21, 478–493. [Google Scholar] [CrossRef] [PubMed]
- Suurmond, R.; van Rhee, H.; Hak, T. Introduction, comparison, and validation of Meta-Essentials: A free and simple tool for meta-analysis. Res. Synth. Methods 2017, 8, 537–553. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J. Statistical power analysis. Curr. Dir. Psychol. Sci. 1992, 1, 98–101. [Google Scholar] [CrossRef]
- Duval, S.; Tweedie, R. Trim and Fill: A Simple Funnel-Plot-Based Method. Biometrics 2000, 56, 455–463. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.T.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions; Cochrane: London, UK, 2011. [Google Scholar]
- Figueiro, M.G.; Plitnick, B.A.; Lok, A.; Jones, G.E.; Higgins, P.; Hornick, T.R.; Rea, M.S. Tailored lighting intervention improves measures of sleep, depression, and agitation in persons with Alzheimer’s disease and related dementia living in long-term care facilities. Clin. Interv. Aging 2014, 9, 1527–1537. [Google Scholar] [CrossRef] [PubMed]
- Ciobanu, I.; Draghici, R.; Marin, A.G.; Zamfir, M.V.; Iliescu, A.; Zamfir, M.; Goodall, G.; Popescu, M.N.; Serrano, J.; Berteanu, M. Case series of an ICT-based multimodal intervention program for people with major neurocognitive disorders: The SENSE-GARDEN project. J. Gerontol. Geriatr. Med. 2022, 8, 2. [Google Scholar]
- Fu, C.Y.; Moyle, W.; Cooke, M. A randomised controlled trial of the use of aromatherapy and hand massage to reduce disruptive behaviour in people with dementia. BMC Complement. Altern. Med. 2013, 13, 165. [Google Scholar] [CrossRef] [PubMed]
- Figueiro, M.G.; Plitnick, B.; Roohan, C.; Sahin, L.; Kalsher, M.; Rea, M.S. Effects of a Tailored Lighting Intervention on Sleep Quality, Rest—Activity, Mood, and Behavior in Older Adults With Alzheimer Disease and Related Dementias: A Randomized Clinical Trial. J. Clin. Sleep Med. 2019, 15, 1757–1767. [Google Scholar] [CrossRef] [PubMed]
- Thorpe, L.; Middleton, J.; Russell, G.; Stewart, N. Bright light therapy for demented nursing home patients with behavioral disturbance. Am. J. Alzheimers Dis. Other Demen 2000, 15, 18–26. [Google Scholar] [CrossRef]
- Figueiro, M.G.; Sahin, L.; Kalsher, M.; Plitnick, B.; Rea, M.S. Long-Term, All-Day Exposure to Circadian-Effective Light Improves Sleep, Mood, and Behavior in Persons with Dementia. J. Alzheimers Dis. Rep. 2020, 4, 297–312. [Google Scholar] [CrossRef] [PubMed]
- Figueiro, M.G.; Kales, H.C. Lighting and Alzheimer’s disease and related dementias: Spotlight on sleep and depression. Light. Res. Technol. 2021, 53, 405–422. [Google Scholar] [CrossRef] [PubMed]
- Saidane, H.A.; Rasmussen, T.; Andersen, K.; Iversen, H.K.; West, A.S. An Explorative Investigation of the Effect of Naturalistic Light on Agitation-Associated Behavior in Nursing Home Residents With Dementia: A Pilot Study. Health Environ. Res. Des. J. 2023, 16, 146–154. [Google Scholar] [CrossRef] [PubMed]
- Connell, B.R.; Sanford, J.A.; Lewis, D. Therapeutic effects of an outdoor activity program on nursing home residents with Dementia. Outdoor Environ. People Dement. 2007, 21, 194–209. [Google Scholar] [CrossRef]
- Ballard, C.G.; O’Brien, J.T.; Reichelt, K.; Perry, E.K. Aromatherapy as a safe and effective treatment for the management of agitation in severe dementia: The results of a double-blind, placebo-controlled trial with Melissa. J. Clin. Psychiatry 2002, 63, 553–558. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.W.K.; Chan, W.C.; Ng, B.F.L.; Lam, L.C.W. Efficacy of aromatherapy (Lavandula angustifolia) as an intervention for agitated behaviours in Chinese older persons with dementia: A cross-over randomized trial. Int. J. Geriatr. Psychiatry 2007, 22, 405–410. [Google Scholar] [CrossRef] [PubMed]
- Burns, A.; Perry, E.; Holmes, C.; Francis, P.; Morris, J.; Howes, M.J.R.; Chazot, P.; Lees, G.; Ballard, C. A double-blind placebo-controlled randomized trial of melissa officinalis oil and donepezil for the treatment of agitation in Alzheimer’s disease. Dement. Geriatr. Cogn. Disord. 2011, 31, 158–164. [Google Scholar] [CrossRef] [PubMed]
- Sakamoto, Y.; Ebihara, S.; Ebihara, T.; Tomita, N.; Toba, K.; Freeman, S.; Arai, H.; Kohzuki, M. Fall prevention using olfactory stimulation with lavender odor in elderly nursing home residents: A randomized controlled trial. J. Am. Geriatr. Soc. 2012, 60, 1005–1011. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, D.W.; Eppingstall, B.; Taffe, J.; van der Ploeg, E.S. A randomized, controlled cross-over trial of dermally-applied lavender (Lavandula angustifolia) oil as a treatment of agitated behaviour in dementia. BMC Complement. Altern. Med. 2013, 13, 315. [Google Scholar] [CrossRef] [PubMed]
- Yang, M.H.; Lin, L.C.; Wu, S.C.; Chiu, J.H.; Wang, P.N.; Lin, J.G. Comparison of the efficacy of aroma-acupressure and aromatherapy for the treatment of dementia-associated agitation. BMC Complement. Altern. Med. 2015, 15, 93. [Google Scholar] [CrossRef] [PubMed]
- Takeda, A.; Watanuki, E.; Koyama, S. Effects of inhalation aromatherapy on symptoms of sleep disturbance in the elderly with dementia. Evid.-Based Complement. Altern. Med. 2017, 2017, 1902807. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, Y.; Shindo, S.; Kanbayashi, T.; Takeshima, M.; Imanishi, A.; Mishima, K. Examination of the influence of cedar fragrance on cognitive function and behavioral and psychological symptoms of dementia in Alzheimer type dementia. Neuropsychopharmacol. Rep. 2020, 40, 10–15. [Google Scholar] [CrossRef] [PubMed]
- Ting, Y.Y.; Tien, Y.; Huang, H.P. Effects of aromatherapy on agitation in patients with dementia in the community: A quasi-experimental study. Geriatr. Nurs. 2023, 51, 422–428. [Google Scholar] [CrossRef] [PubMed]
- Burgio, L.D.; Butler, F.R.; Roth, D.L.; Michael Hardin, J.; Hsu, C.C.; Ung, K. Agitation in nursing home residents: The role of gender and social context. Int. Psychogeriatr. 2000, 12, 495–511. [Google Scholar] [CrossRef] [PubMed]
- Whall, A.L.; Black, M.E.; Groh, C.J.; Yankou, D.J.; Kupferschmid, B.J.; Foster, N.L. Aggression. The effect of natural environments upon agitation and aggression in late stage dementia patients. Am. J. Alzheimer’s Dis. 1997, 12, 216–220. [Google Scholar] [CrossRef]
- Reynolds, L.; Rodiek, S.; Lininger, M.; Mcculley, M.A. Can a Virtual Nature Experience Reduce Anxiety and Agitation in People With Dementia? J. Hous. Elder. 2018, 32, 176–193. [Google Scholar] [CrossRef]
- Lee, Y.; Kim, S. Effects of indoor gardening on sleep, agitation, and cognition in dementia patients—A pilot study. Int. J. Geriatr. Psychiatry 2008, 23, 485–489. [Google Scholar] [CrossRef] [PubMed]
- Pedrinolla, A.; Tamburin, S.; Brasioli, A.; Sollima, A.; Fonte, C.; Muti, E.; Smania, N.; Schena, F.; Venturelli, M. An Indoor Therapeutic Garden for Behavioral Symptoms in Alzheimer’s Disease: A Randomized Controlled Trial. J. Alzheimer’s Dis. 2019, 71, 813–823. [Google Scholar] [CrossRef] [PubMed]
- Wilkes, L.; Fleming, A.; Wilkes, B.L.; Cioffi, J.M.; Le Miere, J. Environment in reducing agitation in dementia Environmental approach to reducing agitation in older persons with dementia in a nursing home. Australas. J. Ageing 2005, 24, 141–145. [Google Scholar] [CrossRef]
- Detweiler, M.B.; Murphy, P.F.; Myers, L.C.; Kim, K.Y. Does a wander garden influence inappropriate behaviors in dementia residents? Am. J. Alzheimers Dis. Other Demen. 2008, 23, 31–45. [Google Scholar] [CrossRef] [PubMed]
- Murphy, P.F.; Miyazaki, Y.; Detweiler, M.B.; Kim, K.Y. Longitudinal analysis of differential effects on agitation of a therapeutic wander garden for dementia patients based on ambulation ability. Dementia 2010, 9, 355–373. [Google Scholar] [CrossRef]
- Luk, K.Y.; Lai, K.Y.C.; Li, C.C.; Cheung, W.H.; Lam, S.M.R.; Li, H.Y.; Ng, K.P.; Shiu, W.H.; So, C.Y.; Wan, S.F. The effect of horticultural activities on agitation in nursing home residents with dementia. Int. J. Geriatr. Psychiatry 2011, 26, 435–436. [Google Scholar] [CrossRef] [PubMed]
- Edwards, C.A.; McDonnell, C.; Merl, H. An evaluation of a therapeutic garden’s influence on the quality of life of aged care residents with dementia. Dementia 2012, 12, 494–510. [Google Scholar] [CrossRef] [PubMed]
- Richardson, M.; Butler, C.W. Nature connectedness and biophilic design. Build. Res. Inf. 2022, 50, 36–42. [Google Scholar] [CrossRef]
- Fleming, R.; Purandare, N. Long-term care for people with dementia: Environmental design guidelines. Int. Psychogeriatr. 2010, 22, 1084–1095. [Google Scholar] [CrossRef] [PubMed]
- Kolanowski, A.; Litaker, M. Social interaction, premorbid personality, and agitation in nursing home residents with dementia. Arch. Psychiatr. Nurs. 2006, 20, 12–20. [Google Scholar] [CrossRef] [PubMed]
- Zeisel, J.; Silverstein, N.M.; Hyde, J.; Levkoff, S.; Lawton, M.P.; Holmes, W. Environmental correlates to behavioral health outcomes in Alzheimer’s special care units. Gerontologist 2003, 43, 697–711. [Google Scholar] [CrossRef] [PubMed]
- Bellelli, G.; Frisoni, G.B.; Bianchetti, A.; Boffelli, S.; Guerrini, G.B.; Scotuzzi, A.; Ranieri, P.; Ritondale, G.; Guglielmi, L.; Fusari, A.; et al. Special care units for demented patients: A multicenter study. Gerontologist 1998, 38, 456–462. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Alessi, C.A.; Yoon, E.J.; Schnelle, J.F.; Al-Samarrai, N.R.; Cruise, P.A. A randomized trial of a combined physical activity and environmental intervention in nursing home residents: Do sleep and agitation improve? J. Am. Geriatr. Soc. 1999, 47, 784–791. [Google Scholar] [CrossRef] [PubMed]
- Alessi, C.A.; Martin, J.L.; Webber, A.P.; Cynthia Kim, E.; Harker, J.O.; Josephson, K.R. Randomized, controlled trial of a nonpharmacological intervention to improve abnormal sleep/wake patterns in nursing home residents. J. Am. Geriatr. Soc. 2005, 53, 803–810. [Google Scholar] [CrossRef] [PubMed]




| Author | Country | Study Design | Sample | Intervention | Duration | Scale Used |
|---|---|---|---|---|---|---|
| Figueiro et al. (2014) [29] | USA | Quasi-experimental design | n = 14, mean age 86.9 ± 4.4 | Naturalistic lighting (Circadian Stimulus) | 4 weeks | CMAI |
| Figueiro et al. (2019) [32] | USA | RCT | n = 46, mean age 85.1 ± 7.1 | Naturalistic lighting (Circadian Stimulus) | 4 weeks | CMAI |
| Thorpe et al. (2000) [33] | Canada | Quasi-experimental design | n = 16, mean age > 65 | Naturalistic lighting (Circadian Stimulus) | 1 week | CMAI |
| Figueiro et al. (2020) [34] | USA | Quasi-experimental design | n = 47, mean age 85.3 ± 7.1 | Naturalistic lighting (Circadian Stimulus) | 25 weeks | CMAI |
| Figueiro and Kales (2021) [35] | USA | Quasi-experimental design | n = 46, mean age 85.1 ± 7.1 | Naturalistic lighting (Circadian Stimulus) | 4 weeks | CMAI |
| Saidane et al. (2023) [36] | Denmark | Quasi-experimental design | n = 5, mean age > 65 | Naturalistic lighting (Circadian Stimulus) | 6 months | CMAI |
| Connell, Sanford and Lewis (2007) [37] | USA | Quasi-experimental design | n = 10, mean age 79.7 ± 8.3 | Bright light exposure (via outdoor) | 10 days | CMAI |
| Ballard et al. (2002) [38] | UK | RCT | n = 36, mean age 78.5 ± 8.1 | Olfactory stimulation | 4 weeks | CMAI |
| Lin et al. (2007) [39] | Hong Kong | RCT | n = 35, mean age 78.20 ± 3.79 | Olfactory stimulation | 3 weeks | NPI |
| Burns et al. (2011) [40] | UK | RCT | n = 32, mean age 85.6 ± 12.6 | Olfactory stimulation | 12 weeks | NPI |
| Sakamoto et al. (2012) [41] | Japan | RCT | n = 51, mean age 84.2 ± 7.8 | Olfactory stimulation | 12 months | CMAI |
| Fu, Moyle and Cooke (2013) [31] | Australia | RCT | n = 22, mean age 84.0 ± 6.36 | Olfactory stimulation | 6 weeks | CMAI |
| O’Connor et al. (2013) [42] | Australia | RCT | n = 37, mean age 77.6 ± 9.40 | Olfactory stimulation | 1 week | CMAI |
| Yang et al. (2015) [43] | Taiwan | RCT | n = 73, mean age 83.67 ± 4.96 | Olfactory stimulation | 4 weeks | CMAI |
| Takeda, Watanuki and Koyama (2017) [44] | Japan | Quasi-experimental design | n = 19, mean age 80.7± 9.1 | Olfactory stimulation | 20 days | NPI |
| Takahashi et al. (2020) [45] | Japan | RCT | n = 19, mean age 76.2 ± 9.8 | Olfactory stimulation | 8 weeks | NPI |
| Ting, Tien and Huang, (2023) [46] | Taiwan | Quasi-experimental design | n = 17, mean age 78.35 ± 13.35 | Olfactory stimulation | 4 weeks | CMAI |
| Burgio et al. (1996) [47] | USA | Quasi-experimental design | n = 13, mean age 83.08 ± 15.92 | Nature sound | 10 days | CMAI |
| Whall et al. (1997) [48] | USA | Quasi-experimental design | n = 15, mean age > 65 | Nature image with sound | 2 weeks | CMAI |
| Reynolds et al. (2018) [49] | USA | Quasi-experimental design | n = 14, mean age 85.1 ± 4.0 | Nature image with sound | 3 days | ABS |
| Ciobanu et al. (2022) [30] | Romania | Quasi-experimental design | n = 7, mean age 71.14 ± 12.17 | Nature video with olfactory | 4 weeks | CMAI |
| Lee and Kim (2008) [50] | Korea | Quasi-experimental design | n = 23, mean age > 65 | Indoor garden | 5 weeks | CMAI |
| Pedrinolla et al. (2019) [51] | Italy | RCT | n = 82, mean age 76.40 ± 4.30 | Indoor garden | 6 months | NPI |
| Wilkes et al. (2005) [52] | Australia | Quasi-experimental design | n = 16, mean age 79.86 | Outdoor garden | 3 months | CMAI |
| Detweiler et al. (2008) [53] | USA | Quasi-experimental design | n = 34, mean age 80.72 ± 6.72 | Outdoor garden | 12 months | CMAI |
| Murphy et al. (2010) [54] | USA | Quasi-experimental design | n = 34, mean age 84.2 | Outdoor garden | 12 months | CMAI |
| Luk et al. (2011) [55] | Hong Kong | RCT | n = 7, mean age 84.9 ± 8.30 | Outdoor garden | 6 weeks | CMAI |
| Edwards, McDonnell and Merl (2012) [56] | Australia | Quasi-experimental design | n = 10, mean age > 65 | Outdoor garden | 3 months | CMAI |
| Gueib et al. (2020) [7] | France | Quasi-experimental design | n = 16, mean age 82.1 ± 7.8 | Outdoor garden | 2 weeks | NPI |
| van der Velde-van Buuringen, Achterberg and Caljouw (2021) [8] | Netherlands | Quasi-experimental design | n = 20, mean age 85.2 ± 4.9 | Outdoor garden | 2 weeks | NPI |
| Motealleh et al. (2022) [9] | Australia | Quasi-experimental design | n = 10, mean age 81 ± 10.1 | Outdoor garden | 4 weeks | CMAI |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Choe, E.Y.; Lee, J.Y.; Montayre, J. Effectiveness of Nature-Based Interventions in Reducing Agitation Among Older Adults with Dementia: A Systematic Review and Meta-Analysis. Healthcare 2025, 13, 1727. https://doi.org/10.3390/healthcare13141727
Choe EY, Lee JY, Montayre J. Effectiveness of Nature-Based Interventions in Reducing Agitation Among Older Adults with Dementia: A Systematic Review and Meta-Analysis. Healthcare. 2025; 13(14):1727. https://doi.org/10.3390/healthcare13141727
Chicago/Turabian StyleChoe, Eun Yeong, Jennifer Yoohyun Lee, and Jed Montayre. 2025. "Effectiveness of Nature-Based Interventions in Reducing Agitation Among Older Adults with Dementia: A Systematic Review and Meta-Analysis" Healthcare 13, no. 14: 1727. https://doi.org/10.3390/healthcare13141727
APA StyleChoe, E. Y., Lee, J. Y., & Montayre, J. (2025). Effectiveness of Nature-Based Interventions in Reducing Agitation Among Older Adults with Dementia: A Systematic Review and Meta-Analysis. Healthcare, 13(14), 1727. https://doi.org/10.3390/healthcare13141727







