Reconceptualizing Somatic Dysfunction in the Light of a Neuroaesthetic Enactive Paradigm
Abstract
1. Introduction
1.1. Somatic Dysfunction: History, Evolution, Definition and Research
1.2. Rationale and Objective
2. Proposal
2.1. Neuroaesthetics for Health
2.2. Neuroaesthetics for Osteopathy: A Journey from Unpleasant-Pleasant Perceptions to SD (Phases 1 and 2)
2.3. Enactive Neuroaesthetics Concept during the Osteopathic Evaluation of SD (Phase 3)
- (1)
- The proprioceptive touch: mechanical stimulus provided by touch can activate tactile and proprioceptive mechanoreceptors that have low activation thresholds [19]. The mechanoreceptors activate thick-type myelinated fibres of type I and II, or A and Aβ, with high conduction speeds, and inform the central nervous system. The posterior horn of the spinal cord receives information from large-calibre neurons more quickly and powerfully, altering the synaptic connections stimulated by the nociceptive input and temporarily altering the state of neural sensitization [19]. Dynamic-type touch, also associated with movements, provides auxiliary proprioceptive feedback for guiding actions. Proprioception, as well as exteroception, are related to the discriminative type of touch [40]. Discriminative touch supports the perception of pressure, vibration, slide, and texture, all of which are essential for haptically revealing information about handled items and for conducting exploratory activities. The main function of such systems is to recognize, classify, and distinguish between environmental stimuli in order to quickly determine which action to do next [40]. Discriminatory touch is possible on glabrous skin, such as the surface of the hand, in which there is a high density of specialised mechanoreceptors able to encode the spatial and temporal properties of surfaces and handled objects [40]. Hairless skin has different mechanoreceptors with low conduction thresholds, different shapes, and sensory properties [40]. The mechanoreceptors are connected to high-conduction speed fibres. Merkel cells record static touch; Ruffini corpuscles decode skin distension; Meissner mechanoreceptors are sensitive to movement; Pacini corpuscles are susceptible to vibrations to high frequency, and acceleration; Muscle spindles record compressions; and Golgi receptors decode slow elongation [19]. When a mechanical stimulus acts on the receptors generates an informational pathway that through the fibres reaches the spinal cord and the postcentral gyrus, where Penfield’s sensory homunculus resides [41].
- (2)
- The interoceptive touch: the evaluator’s touch (if it has the characteristics needed to activate c-tactile fibres) in a neurologically active area induces an inhibitory reflex because this stimulus may change responses evoked by free nerve endings from a constant interpretation of “painful” harmful sensation to an interpretation of “pleasant” non-harmful sensation [19]. The activation of type C unmyelinated fibres can promote inhibition of the activity of the amygdala as well as the activation of cortical regions, such as the left insular, anterior cingulate, and left prefrontal cortex, favouring a modulation of interoceptive information and enabling adaptations of the autonomic nervous system towards a different interpretation of pain [19]. The interoceptive touch (often called affective touch) relies on specific stimulation of the peripheral C-Tactile (CT) afferent system. This system encompasses peculiar fibres that differentiate in tactile afferent receptors forming a secondary touch system [42,43,44] that is interoceptive rather than purely somatosensory [45]. Animal models indicate that CT stimulation elicits a neuro-modulatory inhibitory effect in the dorsal horn, with a concomitant release of protein TAFA4 that has analgesic and anti-inflammatory effects [46,47]. Other studies demonstrated that CT stimulation can reduce acute pain in humans [48,49,50], mediate the µ-opioids system response [51] and oxytocin release [52], which are important chronic pain therapy targets with direct effects upon pain intensity, anxiety, and depressive symptoms [53,54]. Moreover, it has been demonstrated that CT stimulation can enhance parasympathetic autonomic activity (with a possible concomitant reduction of sympathetic pain-related response) [55,56]. Lastly, interoceptive touch has been successfully applied to reduce chronic pain in clinical contexts [57]. Several studies explored the role of C-Tactile stimulation, reporting sometimes conflicting results [58]. These conflicting results can be possibly explained by the unique nature of the C-Tactile afferents, as these receptors respond uniquely to low-force, low-velocity stimuli being unresponsive to mechanical vibration, high velocities or indentation forces, which are often difficult to reproduce. A recent review by Ackerley [59] described in detail the specificity of these receptors and their unique behaviour, redefining the current literature on interoceptive touch. In her seminal work, CT receptors are specifically sensitive to slow (around 3 cm/s) dynamic touch of less than 5 mN (500 mg) and they are not “necessarily tactile pleasantness receptors as such, but they play a clear modulatory and reinforcing role of gentle, comfortable touch interactions” [59]. In this context, the evaluator’s touch in a neurologically active area (if applied matching the characteristics needed to activate C-Tactile fibres) could potentially activate the C-Tactile system promoting a cascade of positive effects, enabling adaptations of the autonomic, cardiovascular, endocrine, and cortical systems, therefore, modulating the perception of pain.
- (3)
- Local and global changes in the fascial tissue: the mechanical stimulus provided by the manual contact in the neurologically active area, perceived as unpleasant in the osteopath-patient dyad, can momentarily modify the mechanical stresses of this continuous system that propagates and connects the entire human body, promoting temporary changes in the viscosity of the connective tissue [60], the fluid dynamics [61,62] (i.e., vasodilatation) and also the trigger threshold of mechanosensitive receptors present in the extracellular matrix, enabling the reduction of local sensitization [63], as well as changes that propagate throughout the fascial continuum [64,65,66,67,68].
2.4. Selection of the Osteopathic Approaches Based on Patient Responsiveness to the SFCT (Phase 4)
What If the SFCT Is Negative?
3. Discussion
3.1. Strengths and Limitations
3.2. Future Directions
4. Conclusions
“Researchers, whether they are scientists or artists, brave the unknown by starting from what is known. Nowadays, the key distinctions may not end up being seen to be between creative and formulaic thinking, rather than between artists and scientists, but between those who can accept doubt and those who cannot” [88].
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Simplified Clinical Scenarios
- Right hypochondrium.
- Osteopath perceptions: stiff tissue, restriction barrier in upward-right direction;
- Patient perceptions: discomfort with the palpation especially during upward-right compression.
- Mid-thoracic spine trait (T4–T6).
- Osteopath perceptions: the osteopath observed a reduction in the thoracic spine kyphosis during the active flexion movement during the standing position; stringiness on the perivertebral soft tissues;
- Patient perceptions: the patient reports feeling “nothing relevant” during the active movement and the palpation.
- Left temporal area of the head, suboccipital right area.
- Osteopath perception: slightly swelling tissue in the area, reduced gliding capacity of the skin;
- Patient perception: the patient reports feeling “nothing relevant” during the palpation and the gliding.
- Left Hip.
- Osteopath perceptions: bogginess in the anterior region of the hip (i.e., hip socket face), limitation on the passive hip extension and internal rotation;
- Patient perception: altered sensitivity during palpation, feelings of tension during passive extension.
- Lumbar area.
- Osteopath perceptions: generally stiff tissue on the entire lumbar area, limitation to the active and passive movement during right trunk rotation;
- Patient perceptions: generalized discomfort during lumbar palpation, feels limitation during active and passive movement.
- Thoracic area.
- Osteopath perceptions: altered breathing pattern, left rib cage seems to have a greater excursion than the right one; right rib cage feels less elastic when compressed;
- Patient perceptions: nothing in particular during the assessment of the area.
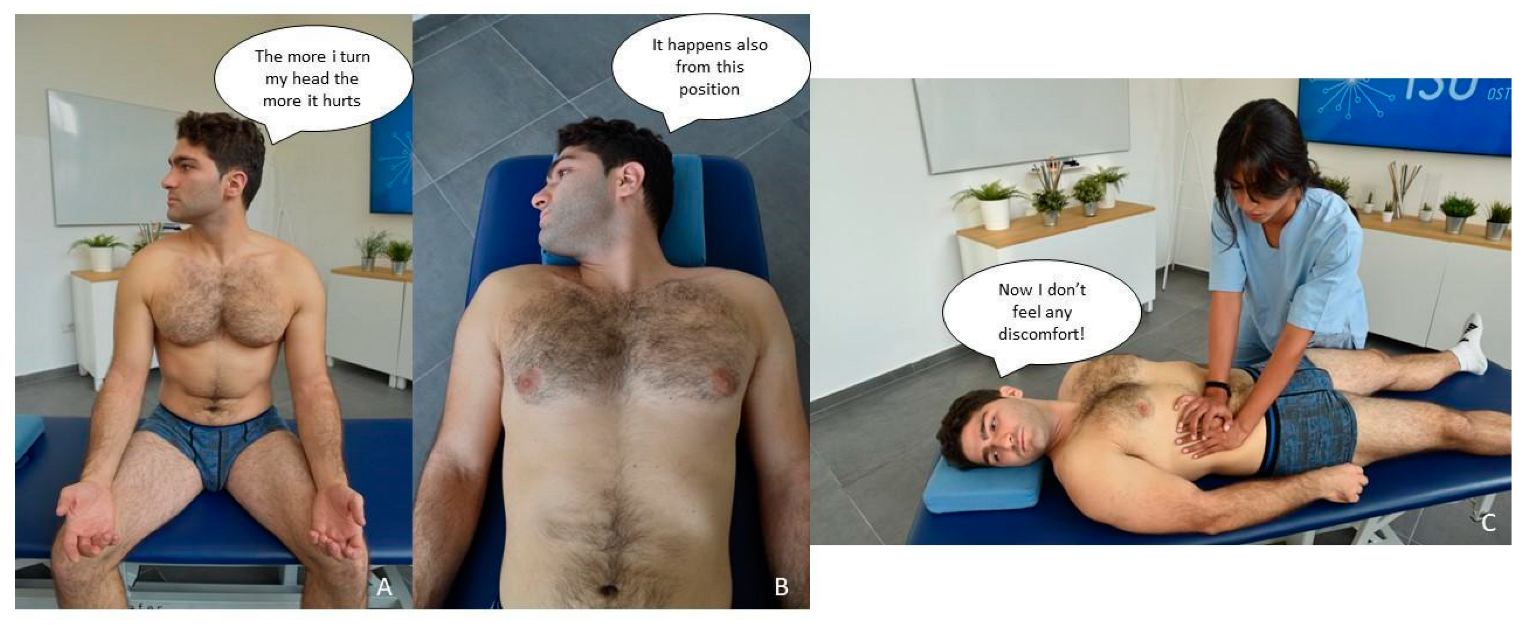
- Tender point on the dorsal area.
- Osteopath perceptions: a stiff spot on left paraspinal soft tissue (approximately between T8–T10);
- Patient perceptions: recognize the painful sensation elicited by the manual compression on the spot as “his pain”.
- The osteopath sets the patient in a side roll position with right lumbar rotation rapid compressions until the perceived restrictive barrier is engaged; monitoring and asking for feedback from the patient about the tender point (i.e., familiar symptom; provocation test). The test is positive since the patient reports diminished pain the more the osteopath comes close to the restrictive barrier (Figure A2B);
- The osteopath, with the patient in a supine position, applies a progressive passive flexion movement of the left hip until the physiologic barrier is perceived; continuously monitoring and asking for feedback from the patient about the tender point (i.e., familiar symptom; provocation test). The test is positive since, during a passive left hip slow and progressive flexion and external rotation, the patient improves hyperalgesia on the specific spot perceived in the low dorsal area (Figure A2C). All the other types of touch (e.g., other passive movement or type of touch; positioning in the direction of the restricted barrier, compression, traction, torsion, release after muscle contraction, etc.) provided in the same area did not negativize the provocation test;
- The osteopath applies a contact force by a progressive touch on the tender point asking for feedback from the patient about the tender point (i.e., familiar symptom; provocation test). The patient answers that it hurts but “it feels like a good pain”. The test is therefore considered positive (Figure A2D).
- Facilitated positional release (lower extremities SD, Left hip) with the patient in a supine position; direction of the manual input and passive movements: combined indirect movements of the left hip (flexion and rotation);
- High velocity, low amplitude technique (lumbar region SD) with the patient in a side-roll position; direction of the manual input and passive movements: right rotation (and accessory planes of motion) is implemented until the restrictive barrier is engaged, and then a rapid force of brief duration driving a short distance is applied within the perceived anatomic range of motion;
- Inhibitory pressure technique (thoracic region SD) with the patient in a prone position.
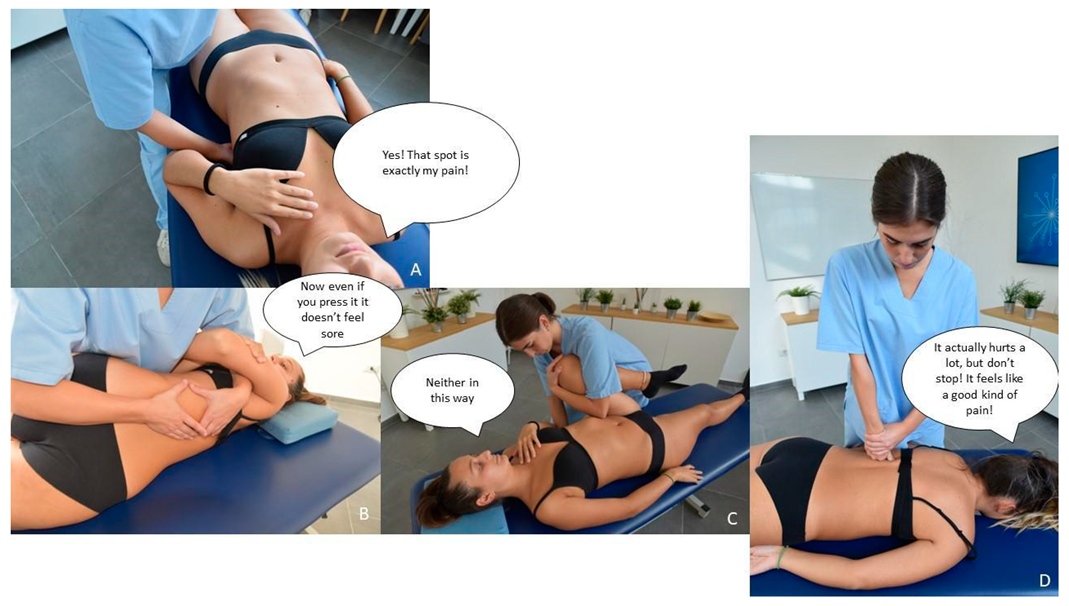
- Right iliac abdominal region.
- Osteopath perception: swelling, bloating, lowered compliance to compression;
- Patient perception: discomfort during the palpation, reports referred pain to the lumbar area.
- Right shoulder.
- Osteopath perception: observed scapula dyskinesia during the active test, limitation to the gliding of the subscapular surface during the passive test;
- Patient perception: nothing relevant.
- Sternal area.
- Osteopath perception: stiffness of tissues, impaired elastic response to compression;
- Patient perception: nothing relevant.
- Dorso-lumbar area.
- Osteopath perception: passive range of motion perceived as limited, perivertebral soft tissue generally stiff.
- Patient perception: the zone feels stiff but “normal stiff”.
- Bilateral temporal area.
- Osteopath perception: ropiness of soft tissues of the area, reduction of the gliding of the skin on subcutaneous tissues;
- Patient perception: referred pain to the right masseterine area during digital pressure of the temporal area, pin-like pain during gliding.
- Right masseter area.
- Osteopath perception: stiffness of the soft tissue of the masseterine area; altered mandibular kinematic during mouth opening and closing;
- Patient perception: referred pain to the right temporal area during digital pressure of the masseterine area; general discomfort on the temporomandibular joint area during last degrees of mouth opening; feels asymmetric pattern during the motion of the jaw.
- Left ankle area.
- Osteopath perception: slight sponginess of external peri-malleolar area, limited range of motion in dorsiflexion;
- Patient perception: nothing relevant.

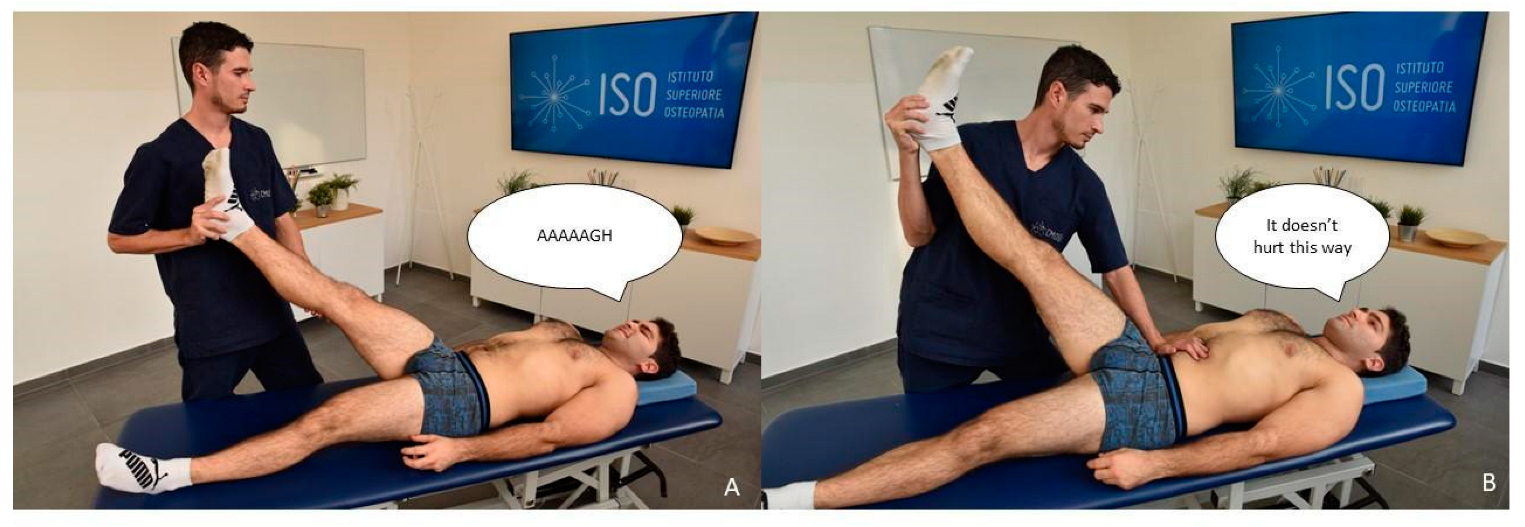
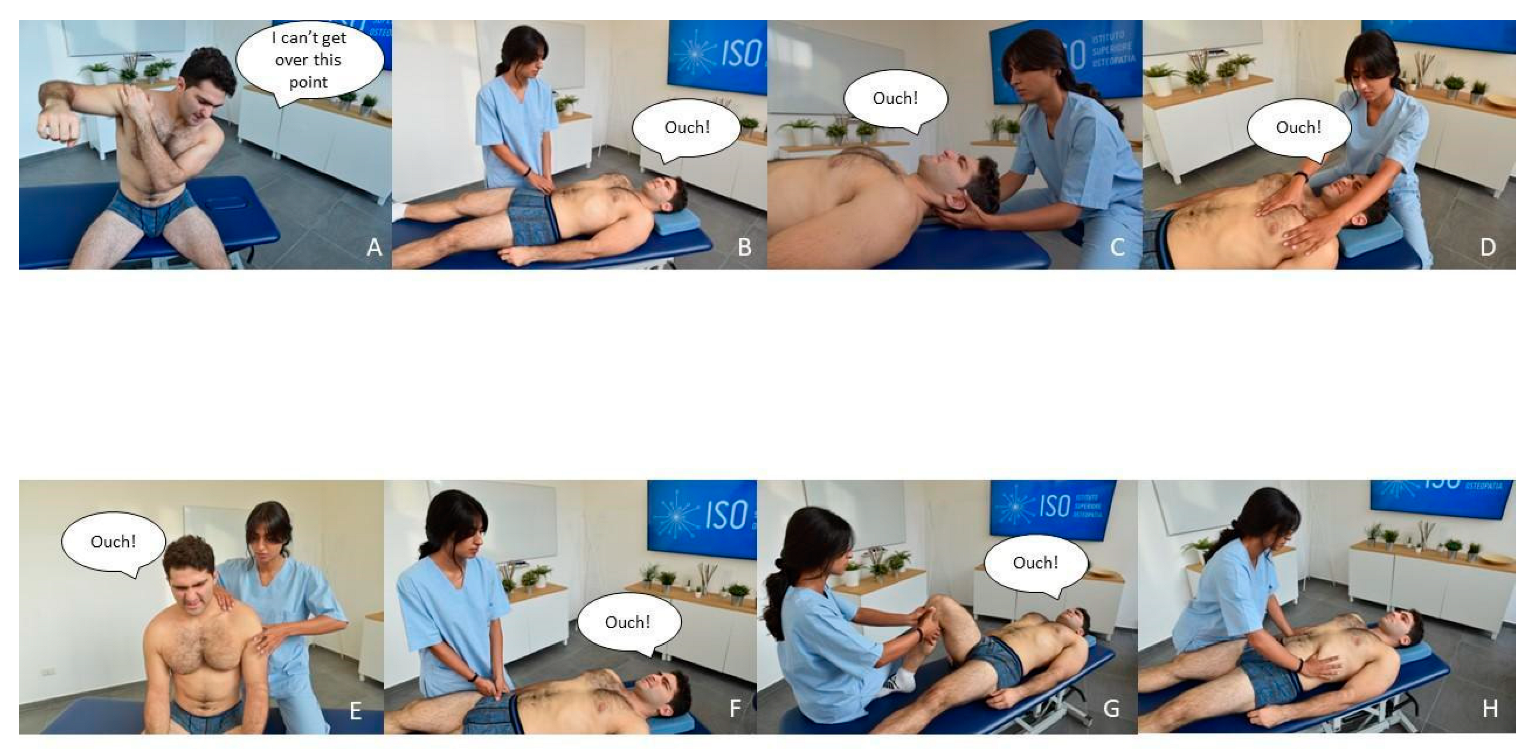
- Familiar Symptom: reduced range of motion of flexion and abduction of the right shoulder (Figure A5A);
- Comparable sign: symmetrical tender points located both above and below the waist around the neck, chest, shoulders, hips, and knees (Severe pain, 7 on a 0–10 pain scale) (Figure A5B–G);
- Manual assessment tests of central sensitization [143]: positive (hypersensitivity to a stimulus was demonstrated at both symptomatic and distant sites).
- Occipital area
- Osteopath perception: augmented stiffness in the area, reduced gliding capacity of the skin;
- Patient perception: the patient reports feeling “dizzy” during the palpation of the occipital area.
- Thoracic area
- Osteopath perceptions: altered breathing rate (rate of 12 breaths per minute), augmented stiffness in the whole rib cage, decreased range of motion in the right rib cage;
- Patient perceptions: nothing in particular during the assessment of the area.
- Generalized fascial pattern (spiral and back functional lines—myofascial chains)
- Osteopath perception: preferred direction of motion throughout the spiral and functional back lines [144];
- Patient perception: perception of passive or active positioning as antalgic postures (alternating progressive slow positioning to maximize tension, stretch, and then release).
References
- Liem, T.A.T. Still’s Osteopathic Lesion Theory and Evidence-Based Models Supporting the Emerged Concept of Somatic Dysfunction. J. Am. Osteopath Assoc. 2016, 116, 654–661. [Google Scholar] [CrossRef]
- ICD-10-CM Diagnosis Code M99.0: Segmental and Somatic Dysfunction. 2021. Available online: https://www.icd10data.com/ICD10CM/Codes/M00-M99/M99-M99/M99-/M99.0 (accessed on 22 July 2021).
- Lunghi, C.; Consorti, G.; Tramontano, M.; Esteves, J.E.; Cerritelli, F. Perspectives on Tissue Adaptation Related to Allostatic Load: Scoping Review and Integrative Hypothesis with a Focus on Osteopathic Palpation. J. Bodyw. Mov. Ther. 2020, 24, 212–220. [Google Scholar] [CrossRef]
- Verzella, M.; Affede, E.; Di Pietrantonio, L.; Cozzolino, V.; Cicchitti, L. Tissutal and Fluidic Aspects in Osteopathic Manual Therapy: A Narrative Review. Healthcare 2022, 10, 1014. [Google Scholar] [CrossRef]
- Baroni, F.; Tramontano, M.; Barsotti, N.; Chiera, M.; Lanaro, D.; Lunghi, C. Osteopathic Structure/Function Models Renovation for a Person-Centered Approach: A Narrative Review and Integrative Hypothesis. J. Complement Integr. Med. 2021. [Google Scholar] [CrossRef]
- Giusti, R. Glossary of Osteopathic Terminology, 3rd ed.; AACOM: Bethesda, MD, USA, 2017. [Google Scholar]
- Esteves, J.E.; Zegarra-Parodi, R.; van Dun, P.; Cerritelli, F.; Vaucher, P. Models and Theoretical Frameworks for Osteopathic Care—A Critical View and Call for Updates and Research. Int. J. Osteopath. Med. 2020, 35, 1–4. [Google Scholar] [CrossRef]
- Castagna, C.; Consorti, G.; Turinetto, M.; Lunghi, C. Osteopathic Models Integration Radar Plot: A Proposed Framework for Osteopathic Diagnostic Clinical Reasoning. J. Chiropr. Humanit. 2021, 28, 49–59. [Google Scholar] [CrossRef] [PubMed]
- Zegarra-Parodi, R.; Baroni, F.; Lunghi, C.; Dupuis, D. Historical Osteopathic Principles and Practices in Contemporary Care: An Anthropological Perspective to Foster Evidence-Informed and Culturally Sensitive Patient-Centered Care: A Commentary. Healthcare 2023, 11, 10. [Google Scholar] [CrossRef] [PubMed]
- McParlin, Z.; Cerritelli, F.; Friston, K.J.; Esteves, J.E. Therapeutic Alliance as Active Inference: The Role of Therapeutic Touch and Synchrony. Front. Psychol. 2022, 13, 329. [Google Scholar] [CrossRef] [PubMed]
- Esteves, J.E.; Cerritelli, F.; Kim, J.; Friston, K.J. Osteopathic Care as (En)Active Inference: A Theoretical Framework for Developing an Integrative Hypothesis in Osteopathy. Front. Psychol. 2022, 13, 167. [Google Scholar] [CrossRef] [PubMed]
- Cerritelli, F.; Esteves, J.E. An Enactive–Ecological Model to Guide Patient-Centered Osteopathic Care. Healthcare 2022, 10, 1092. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Esteves, J.E.; Cerritelli, F.; Friston, K. An Active Inference Account of Touch and Verbal Communication in Therapy. Front. Psychol. 2022, 13, 828952. [Google Scholar] [CrossRef] [PubMed]
- Bergna, A.; Galli, M.; Todisco, F.; Berti, F. Beliefs and Use of Palpatory Findings in Osteopathic Clinical Practice: A Qualitative Descriptive Study among Italian Osteopaths. Healthcare 2022, 10, 1647. [Google Scholar] [CrossRef] [PubMed]
- Arcuri, L.; Consorti, G.; Tramontano, M.; Petracca, M.; Esteves, J.E.; Lunghi, C. “What You Feel under Your Hands”: Exploring Professionals’ Perspective of Somatic Dysfunction in Osteopathic Clinical Practice-a Qualitative Study. Chiropr. Man. Therap. 2022, 30, 32. [Google Scholar] [CrossRef] [PubMed]
- Consorti, G.; Marchetti, A.; De Marinis, M.G. What Makes an Osteopathic Treatment Effective From a Patient’s Perspective: A Descriptive Phenomenological Study. J. Manip. Physiol. Ther. 2020, 43, 882–890. [Google Scholar] [CrossRef] [PubMed]
- Lunghi, C.; Tozzi, P.; Fusco, G. The Biomechanical Model in Manual Therapy: Is There an Ongoing Crisis or Just the Need to Revise the Underlying Concept and Application? J. Bodyw. Mov. Ther. 2016, 20, 784–799. [Google Scholar] [CrossRef] [PubMed]
- Lunghi, C.; Baroni, F.; Amodio, A.; Consorti, G.; Tramontano, M.; Liem, T. Patient Active Approaches in Osteopathic Practice: A Scoping Review. Healthcare 2022, 10, 524. [Google Scholar] [CrossRef] [PubMed]
- Baroni, F.; Ruffini, N.; D’Alessandro, G.; Consorti, G.; Lunghi, C. The Role of Touch in Osteopathic Practice: A Narrative Review and Integrative Hypothesis. Complement Ther. Clin. Pract. 2021, 42, 101277. [Google Scholar] [CrossRef] [PubMed]
- Liem, T.; Lunghi, C. Reconceptualizing Principles and Models in Osteopathic Care: A Clinical Application of the Integral Theory. Altern. Ther. Health Med. 2021, AT6750, ISSN#1078-6791. [Google Scholar]
- Tramontano, M.; Martino Cinnera, A.; Petracca, M.; Gaeta, A.; Tamburella, F.; Audouard, M.; Caltagirone, C. Outpatient Satisfaction With Osteopathic Manipulative Treatment in a Hospital Center: A Survey. Altern. Ther. Health Med. 2018, 24, 18–24. [Google Scholar]
- Chatterjee, A.; Vartanian, O. Neuroaesthetics. Trends Cogn. Sci. 2014, 18, 370–375. [Google Scholar] [CrossRef] [PubMed]
- Hoss, R.A.; Langlois, J.H. Infants Prefer Attractive Faces. In The Development of Face Processing in Infancy and Early Childhood: Current Perspectives; Nova Science Publishers: Hauppauge, NY, USA, 2003; pp. 27–38. ISBN 978-1-59033-775-2. [Google Scholar]
- Langlois, J.H.; Ritter, J.M.; Roggman, L.A.; Vaughn, L.S. Facial Diversity and Infant Preferences for Attractive Faces. Dev. Psychol. 1991, 27, 79–84. [Google Scholar] [CrossRef]
- Dion, K.K. Young Children’s Stereotyping of Facial Attractiveness. Dev. Psychol. 1973, 9, 183–188. [Google Scholar] [CrossRef]
- Zaidel, D.W. Neuroesthetics Is Not Just about Art. Front. Hum. Neurosci. 2015, 9, 80. [Google Scholar] [CrossRef] [PubMed]
- Ishizu, T.; Zeki, S. Toward A Brain-Based Theory of Beauty. PLoS ONE 2011, 6, e21852. [Google Scholar] [CrossRef] [PubMed]
- Brinck, I. Empathy, Engagement, Entrainment: The Interaction Dynamics of Aesthetic Experience. Cogn. Process 2018, 19, 201–213. [Google Scholar] [CrossRef]
- Fort, M.; Lammertink, I.; Peperkamp, S.; Guevara-Rukoz, A.; Fikkert, P.; Tsuji, S. Symbouki: A Meta-Analysis on the Emergence of Sound Symbolism in Early Language Acquisition. Dev. Sci. 2018, 21, e12659. [Google Scholar] [CrossRef]
- Etzi, R.; Spence, C.; Zampini, M.; Gallace, A. When Sandpaper Is “Kiki” and Satin Is “Bouba”: An Exploration of the Associations Between Words, Emotional States, and the Tactile Attributes of Everyday Materials. Multisens. Res. 2016, 29, 133–155. [Google Scholar] [CrossRef]
- Graven, T.; Desebrock, C. Bouba or Kiki with and without Vision: Shape-Audio Regularities and Mental Images. Acta Psychol. 2018, 188, 200–212. [Google Scholar] [CrossRef]
- Kim, D.; Woo, C.-W.; Kim, S.-G. Neural Mechanisms of Pain Relief through Paying Attention to Painful Stimuli. Pain 2022, 163, 1130–1138. [Google Scholar] [CrossRef]
- Kanbara, K.; Fukunaga, M. Links among Emotional Awareness, Somatic Awareness and Autonomic Homeostatic Processing. Biopsychosoc. Med. 2016, 10, 16. [Google Scholar] [CrossRef]
- Kamath, S.U.; Kamath, S.S. Lasègue’s Sign. J. Clin. Diagn. Res. 2017, 11, RG01–RG02. [Google Scholar] [CrossRef] [PubMed]
- Michikawa, T.; Nishiwaki, Y.; Takebayashi, T.; Toyama, Y. One-Leg Standing Test for Elderly Populations. J. Orthop. Sci. 2009, 14, 675–685. [Google Scholar] [CrossRef] [PubMed]
- de Vries, J.; Ischebeck, B.K.; Voogt, L.P.; van der Geest, J.N.; Janssen, M.; Frens, M.A.; Kleinrensink, G.J. Joint Position Sense Error in People with Neck Pain: A Systematic Review. Man. Ther. 2015, 20, 736–744. [Google Scholar] [CrossRef] [PubMed]
- Pilotto, A.; Custodero, C.; Maggi, S.; Polidori, M.C.; Veronese, N.; Ferrucci, L. A Multidimensional Approach to Frailty in Older People. Ageing Res. Rev. 2020, 60, 101047. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, C.-M.; Kenagy, G.P. Exploring the Association between Quality of Homecare Services and Older Adults’ Well-Being. Home Health Care Serv. Q. 2020, 39, 65–79. [Google Scholar] [CrossRef] [PubMed]
- Bicalho, E.; Vieira, L.; Makita, D.K.; Rivas, L. Inhibitory Tests as Assessment Tools for Somatic Dysfunctions: Mechanisms and Practical Applications. Cureus 2020, 12, e7700. [Google Scholar] [CrossRef]
- McGlone, F.; Wessberg, J.; Olausson, H. Discriminative and Affective Touch: Sensing and Feeling. Neuron 2014, 82, 737–755. [Google Scholar] [CrossRef]
- Petit, D.; Burgess, P.R. Dorsal Column Projection of Receptors in Cat Hairy Skin Supplied by Myelinated Fibers. J. Neurophysiol. 1968, 31, 849–855. [Google Scholar] [CrossRef]
- Olausson, H.; Lamarre, Y.; Backlund, H.; Morin, C.; Wallin, B.G.; Starck, G.; Ekholm, S.; Strigo, I.; Worsley, K.; Vallbo, Å.B.; et al. Unmyelinated Tactile Afferents Signal Touch and Project to Insular Cortex. Nat. Neurosci. 2002, 5, 900–904. [Google Scholar] [CrossRef]
- Olausson, H.; Wessberg, J.; Morrison, I.; McGlone, F.; Vallbo, Å. The Neurophysiology of Unmyelinated Tactile Afferents. Neurosci. Biobehav. Rev. 2010, 34, 185–191. [Google Scholar] [CrossRef]
- Olausson, H.; Wessberg, J.; Morrison, I.; McGlone, F. (Eds.) Affective Touch and the Neurophysiology of CT Afferents; Springer: New York, NY, USA, 2016; ISBN 978-1-4939-6416-1. [Google Scholar]
- Gordon, I.; Voos, A.C.; Bennett, R.H.; Bolling, D.Z.; Pelphrey, K.A.; Kaiser, M.D. Brain Mechanisms for Processing Affective Touch. Hum. Brain Mapp. 2013, 34, 914–922. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.; Perl, E.R. A Specific Inhibitory Pathway between Substantia Gelatinosa Neurons Receiving Direct C-Fiber Input. J. Neurosci. 2003, 23, 8752–8758. [Google Scholar] [CrossRef] [PubMed]
- Delfini, M.-C.; Mantilleri, A.; Gaillard, S.; Hao, J.; Reynders, A.; Malapert, P.; Alonso, S.; François, A.; Barrere, C.; Seal, R.; et al. TAFA4, a Chemokine-like Protein, Modulates Injury-Induced Mechanical and Chemical Pain Hypersensitivity in Mice. Cell Rep. 2013, 5, 378–388. [Google Scholar] [CrossRef]
- Krahé, C.; Drabek, M.M.; Paloyelis, Y.; Fotopoulou, A. Affective Touch and Attachment Style Modulate Pain: A Laser-Evoked Potentials Study. Philos. Trans. R. Soc. B Biol. Sci. 2016, 371, 20160009. [Google Scholar] [CrossRef] [PubMed]
- Liljencrantz, J.; Strigo, I.; Ellingsen, D.; Krämer, H.; Lundblad, L.; Nagi, S.; Leknes, S.; Olausson, H. Slow Brushing Reduces Heat Pain in Humans. Eur. J. Pain 2017, 21, 1173–1185. [Google Scholar] [CrossRef]
- von Mohr, M.; Krahé, C.; Beck, B.; Fotopoulou, A. The Social Buffering of Pain by Affective Touch: A Laser-Evoked Potential Study in Romantic Couples. Soc. Cogn. Affect. Neurosci. 2018, 13, 1121–1130. [Google Scholar] [CrossRef] [PubMed]
- Nummenmaa, L.; Tuominen, L.; Dunbar, R.; Hirvonen, J.; Manninen, S.; Arponen, E.; Machin, A.; Hari, R.; Jääskeläinen, I.P.; Sams, M. Social Touch Modulates Endogenous μ-Opioid System Activity in Humans. Neuroimage 2016, 138, 242–247. [Google Scholar] [CrossRef]
- Walker, S.C.; Trotter, P.D.; Swaney, W.T.; Marshall, A.; Mcglone, F.P. C-Tactile Afferents: Cutaneous Mediators of Oxytocin Release during Affiliative Tactile Interactions? Neuropeptides 2017, 64, 27–38. [Google Scholar] [CrossRef]
- Goodin, B.R.; Ness, T.J.; Robbins, M.T. Oxytocin—A Multifunctional Analgesic for Chronic Deep Tissue Pain. Curr. Pharm. Des. 2015, 21, 906–913. [Google Scholar] [CrossRef]
- Tracy, L.M.; Georgiou-Karistianis, N.; Gibson, S.J.; Giummarra, M.J. Oxytocin and the Modulation of Pain Experience: Implications for Chronic Pain Management. Neurosci. Biobehav. Rev. 2015, 55, 53–67. [Google Scholar] [CrossRef]
- Triscoli, C.; Croy, I.; Steudte-Schmiedgen, S.; Olausson, H.; Sailer, U. Heart Rate Variability Is Enhanced by Long-Lasting Pleasant Touch at CT-Optimized Velocity. Biol. Psychol. 2017, 128, 71–81. [Google Scholar] [CrossRef]
- Di Lernia, D.; Cipresso, P.; Pedroli, E.; Riva, G. Toward an Embodied Medicine: A Portable Device with Programmable Interoceptive Stimulation for Heart Rate Variability Enhancement. Sensors 2018, 18, 2469. [Google Scholar] [CrossRef]
- Di Lernia, D.; Lacerenza, M.; Ainley, V.; Riva, G. Altered Interoceptive Perception and the Effects of Interoceptive Analgesia in Musculoskeletal, Primary, and Neuropathic Chronic Pain Conditions. J. Pers. Med. 2020, 10, 201. [Google Scholar] [CrossRef]
- Fusaro, M.; Bufacchi, R.J.; Nicolardi, V.; Provenzano, L. The Analgesic Power of Pleasant Touch in Individuals with Chronic Pain: Recent Findings and New Insights. Front. Integr. Neurosci. 2022, 16, 956510. [Google Scholar] [CrossRef] [PubMed]
- Ackerley, R. C-Tactile (CT) Afferents: Evidence of Their Function from Microneurography Studies in Humans. Curr. Opin. Behav. Sci. 2022, 43, 95–100. [Google Scholar] [CrossRef]
- Pohl, H. Changes in the Structure of Collagen Distribution in the Skin Caused by a Manual Technique. J. Bodyw. Mov. Ther. 2010, 14, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Mow, V.C.; Huiskes, R. Basic Orthopaedic Biomechanics & Mechano-Biology; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2005; ISBN 978-0-7817-3933-7. [Google Scholar]
- Langevin, H.M.; Nedergaard, M.; Howe, A.K. Cellular Control of Connective Tissue Matrix Tension. J. Cell. Biochem. 2013, 114, 1714–1719. [Google Scholar] [CrossRef] [PubMed]
- Langevin, H.M.; Sherman, K.J. Pathophysiological Model for Chronic Low Back Pain Integrating Connective Tissue and Nervous System Mechanisms. Med. Hypotheses 2007, 68, 74–80. [Google Scholar] [CrossRef]
- Albrecht-Buehler, G. Role of Cortical Tension in Fibroblast Shape and Movement. Cell Motil. 1987, 7, 54–67. [Google Scholar] [CrossRef]
- Evans, E.; Yeung, A. Apparent Viscosity and Cortical Tension of Blood Granulocytes Determined by Micropipet Aspiration. Biophys. J. 1989, 56, 151–160. [Google Scholar] [CrossRef]
- Dong, C.; Skalak, R.; Sung, K.-L.P. Cytoplasmic Rheology of Passive Neutrophils. Biorheology 1991, 28, 557–567. [Google Scholar] [CrossRef] [PubMed]
- Fung, Y.C.; Liu, S.Q. Elementary Mechanics of the Endothelium of Blood Vessels. J. Biomech. Eng. 1993, 115, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Schmid-Schönbein, G.W.; Kosawada, T.; Skalak, R.; Chien, S. Membrane Model of Endothelial Cells and Leukocytes. A Proposal for the Origin of a Cortical Stress. J. Biomech. Eng. 1995, 117, 171–178. [Google Scholar] [CrossRef] [PubMed]
- Cormack, B.; Stilwell, P.; Coninx, S.; Gibson, J. The Biopsychosocial Model Is Lost in Translation: From Misrepresentation to an Enactive Modernization. Physiother. Theory Pract. 2022, 1–16. [Google Scholar] [CrossRef]
- Therapeutic Patient Education: Continuing Education Programmes for Health Care Providers in the Field of Prevention of Chronic Diseases: Report of a WHO Working Group; WHO: Geneva, Switzerland, 1998; Volume 90, pp. 1–67.
- Integrated Care for Older People: Guidelines on Community-Level Interventions to Manage Declines in Intrinsic Capacity. Available online: https://www.who.int/publications-detail-redirect/9789241550109 (accessed on 24 November 2022).
- Bohlen, L.; Shaw, R.; Cerritelli, F.; Esteves, J.E. Osteopathy and Mental Health: An Embodied, Predictive, and Interoceptive Framework. Front. Psychol. 2021, 12, 767005. [Google Scholar] [CrossRef]
- Lunghi, C.; Baroni, F. Cynefin Framework for Evidence-Informed Clinical Reasoning and Decision-Making. J. Osteopath. Med. 2019, 119, 312–321. [Google Scholar] [CrossRef]
- Haas, M.; Cooperstein, R.; Peterson, D. Disentangling Manual Muscle Testing and Applied Kinesiology: Critique and Reinterpretation of a Literature Review. Chiropr. Osteopathy 2007, 15, 11. [Google Scholar] [CrossRef]
- Schmitt, W.H.; Cuthbert, S.C. Common Errors and Clinical Guidelines for Manual Muscle Testing: “The Arm Test” and Other Inaccurate Procedures. Chiropr. Osteopathy 2008, 16, 16. [Google Scholar] [CrossRef]
- Castillo, R.; Schander, A.; Hodge, L.M. Lymphatic Pump Treatment Mobilizes Bioactive Lymph that Suppresses Macrophage Activity In Vitro. J. Osteopath. Med. 2018, 118, 455–461. [Google Scholar] [CrossRef]
- Minasny, B. Understanding the Process of Fascial Unwinding. Int. J. Ther. Massage Bodywork 2009, 2, 10–17. [Google Scholar] [CrossRef][Green Version]
- Calsius, J.; De Bie, J.; Hertogen, R.; Meesen, R. Touching the Lived Body in Patients with Medically Unexplained Symptoms. How an Integration of Hands-on Bodywork and Body Awareness in Psychotherapy May Help People with Alexithymia. Front. Psychol. 2016, 7, 253. [Google Scholar] [CrossRef] [PubMed]
- Rossettini, G.; Colombi, A.; Carlino, E.; Manoni, M.; Mirandola, M.; Polli, A.; Camerone, E.M.; Testa, M. Unraveling Negative Expectations and Nocebo-Related Effects in Musculoskeletal Pain. Front. Psychol. 2022, 13, 789377. [Google Scholar] [CrossRef] [PubMed]
- Hutting, N.; Caneiro, J.P.; Ong’wen, O.M.; Miciak, M.; Roberts, L. Person-Centered Care for Musculoskeletal Pain: Putting Principles into Practice. Musculoskelet Sci. Pract. 2022, 62, 102663. [Google Scholar] [CrossRef] [PubMed]
- Petersen, A.K.; Zebis, M.K.; Lauridsen, H.B.; Hölmich, P.; Aagaard, P.; Bencke, J. Impaired One-Legged Landing Balance in Young Female Athletes with Previous Ankle Sprain: A Cross-Sectional Study. J. Sports Med. Phys. Fitness 2022, 62, 1489–1495. [Google Scholar] [CrossRef] [PubMed]
- Lunghi, C.; Iacopini, A.; Baroni, F.; Consorti, G.; Cerritelli, F. Thematic Analysis of Attitudes Held by a Group of Italian Osteopaths Toward Osteopathic Evaluation, Treatment, and Management in the Neonatal and Pediatric Field: A Qualitative Study. J. Manip. Physiol. Ther 2021, 44, 164–175. [Google Scholar] [CrossRef] [PubMed]
- Sweeney, J.K.; Blackburn, S. Neonatal Physiological and Behavioral Stress during Neurological Assessment. J. Perinat. Neonatal. Nurs. 2013, 27, 242–252. [Google Scholar] [CrossRef]
- Tarantino, A.G.; Vismara, L.; Buffone, F.; Bianchi, G.; Bergna, A.; Vanoni, M.; Tabbi, C.; Bresesti, I.; Agosti, M. Model-Base Estimation of Non-Invasive Ventilation Weaning of Preterm Infants Exposed to Osteopathic Manipulative Treatment: A Propensity-Score-Matched Cohort Study. Healthcare 2022, 10, 2379. [Google Scholar] [CrossRef]
- Álvarez-Rodríguez, J.; Leirós-Rodríguez, R.; Morera-Balaguer, J.; Marqués-Sánchez, P.; Rodríguez-Nogueira, Ó. The Influence of the Locus of Control Construct on the Efficacy of Physiotherapy Treatments in Patients with Chronic Pain: A Systematic Review. J. Pers. Med. 2022, 12, 232. [Google Scholar] [CrossRef]
- Maccioni, G.; Ruscitto, S.; Gulino, R.A.; Giansanti, D. Opportunities and Problems of the Consensus Conferences in the Care Robotics. Healthcare 2021, 9, 1624. [Google Scholar] [CrossRef]
- Thomson, O.P.; Petty, N.J.; Moore, A.P. A Qualitative Grounded Theory Study of the Conceptions of Clinical Practice in Osteopathy—A Continuum from Technical Rationality to Professional Artistry. Man. Ther. 2014, 19, 37–43. [Google Scholar] [CrossRef]
- Charon, R. Knowing, Seeing, and Telling in Medicine. Lancet 2021, 398, 2068–2070. [Google Scholar] [CrossRef] [PubMed]
- Consorti, G.; Basile, F.; Pugliese, L.; Petracca, M. Interrater Reliability of Osteopathic Sacral Palpatory Diagnostic Tests among Osteopathy Students. J. Am. Osteopath. Assoc. 2018, 118, 637–644. [Google Scholar] [CrossRef] [PubMed]
- Sciomachen, P.; Arienti, C.; Bergna, A.; Castagna, C.; Consorti, G.; Lotti, A.; Lunghi, C.; Tramontano, M.; Longobardi, M. Core Competencies in Osteopathy: Italian Register of Osteopaths Proposal. Int. J. Osteopath. Med. 2018, 27, 1–5. [Google Scholar] [CrossRef]
- Seffinger, M.A.; Hruby, R.; Willard, F.H.; Licciardone, J. Foundations of Osteopathic Medicine: Philosophy, Science, Clinical Applications, and Research, 4th ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2019; pp. 135–166. ISBN 978-1-4963-6832-4. [Google Scholar]
- Fryette, H.H. Principles of Osteopathic Technic; American Academy of Osteopathy: Indianapolis, IN, USA, 1980; pp. 1–246. [Google Scholar]
- Tasker, D.L. Principles of Osteopathy; Forgotten Books: London, UK, 2012; pp. 1–535. [Google Scholar]
- A Text Book of The Principles of Osteopathy. Available online: https://archive.lib.msu.edu/DMC/Osteopathy/textbook1903.pdf (accessed on 20 October 2022).
- Downing, C.H. Principles and Practice of Osteopathy; Tamor Pierston: London, UK, 1981; pp. 1–402. ISBN 978-0-907457-00-8. [Google Scholar]
- Baroni, F.; Mancini, D.; Tuscano, S.C.; Scarlata, S.; Lunghi, C.; Cerritelli, F.; Haxton, J. Osteopathic Manipulative Treatment and the Spanish Flu: A Historical Literature Review. J. Osteopath. Med. 2021, 121, 181–190. [Google Scholar] [CrossRef]
- Macdonald, G.; Wilson, W.H. The Osteopathic Lesion. JAMA 1936, 106, 1417. [Google Scholar] [CrossRef]
- Definition of LESION. Available online: https://www.merriam-webster.com/dictionary/lesion (accessed on 20 October 2022).
- ICD-11 for Mortality and Morbidity Statistics. Available online: https://icd.who.int/browse11/l-m/en#/http%3a%2f%2fid.who.int%2ficd%2fentity%2f1652981832 (accessed on 20 January 2022).
- Glossary of Osteopathic Terminology, Third Edition. Available online: https://www.aacom.org/docs/default-source/default-document-library/glossary2017.pdf (accessed on 20 October 2022).
- Applied Anatomy Designed for the Use of Osteopathic Students and Practitioners as an Aid in the Anatomical Explanation of Disease From an Osteopathic Viewpoint Classic Reprint by Marion Edward Clark: New PAP. 2019. Available online: https://digitalcommons.pcom.edu/classic_med_works/14/ (accessed on 20 January 2022).
- Burns, L. Viscero-Somatic and Somato-Visceral Spinal Reflexes. J. Am. Osteopath. Assoc. 2000, 100, 249–258. [Google Scholar]
- Burns, L. Secondary Lesions Following Experimental Lesion of the Second Thoracic Vertebra in Rabbits. J. Am. Osteopath. Assoc. 1925, 10, 184–188. [Google Scholar]
- Cole, W. The Osteopathic Lesion Syndrome; Acad. Osteopath. Med.: Indianapolis, IN, USA, 1952; pp. 149–178. [Google Scholar]
- Korr, I.M. The Neural Basis of the Osteopathic Lesion. J. Am. Osteopath. Assoc. 1947, 47, 191–198. [Google Scholar]
- Denslow, J.S.; Korr, I.M.; Krems, A.D. Quantitative Studies of Chronic Facilitation in Human Motoneuron Pools. Am. J. Physiol. 1947, 150, 229–238. [Google Scholar] [CrossRef]
- Hix, E.L. Reflex Viscerosomatic Reference Phenomena. Osteopath. Ann. 1976, 4, 496–503. [Google Scholar]
- Beal, M.C. Viscerosomatic Reflexes: A Review. J. Am. Osteopath. Assoc. 1985, 85, 786–801. [Google Scholar] [CrossRef] [PubMed]
- Kelso, A.F.; Grant, R.G.; Johnston, W.L. Use of Thermograms to Support Assessment of Somatic Dysfunction or Effects of Osteopathic Manipulative Treatment: Preliminary Report. J. Am. Osteopath. Assoc. 1982, 82, 182–188. [Google Scholar] [CrossRef] [PubMed]
- Van Buskirk, R.L. Nociceptive Reflexes and the Somatic Dysfunction: A Model. J. Am. Osteopath. Assoc. 1990, 90, 792–794, 797–809. [Google Scholar] [CrossRef]
- Fryer, G.; Bird, M.; Robbins, B.; Fossum, C.; Johnson, J.C. Resting Electromyographic Activity of Deep Thoracic Transversospinalis Muscles Identified as Abnormal with Palpation. J. Am. Osteopath. Assoc. 2010, 110, 61–68. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Fryer, G.; Morris, T.; Gibbons, P.; Briggs, A. The Electromyographic Activity of Thoracic Paraspinal Muscles Identified as Abnormal with Palpation. J. Manip. Physiol. Ther. 2006, 29, 437–447. [Google Scholar] [CrossRef] [PubMed]
- Fryer, G.; Morris, T.; Gibbons, P. Paraspinal Muscles and Intervertebral Dysfunction: Part One. J. Manip. Physiol. Ther. 2004, 27, 267–274. [Google Scholar] [CrossRef] [PubMed]
- Fryer, G. Somatic Dysfunction: An Osteopathic Conundrum. Int. J. Osteopath. Med. 2016, 22, 52–63. [Google Scholar] [CrossRef]
- Tozzi, P. A Unifying Neuro-Fasciagenic Model of Somatic Dysfunction—Underlying Mechanisms and Treatment—Part I. J. Bodyw. Mov. Ther. 2015, 19, 310–326. [Google Scholar] [CrossRef]
- Hohenschurz-Schmidt, D.; Thomson, O.P.; Rossettini, G.; Miciak, M.; Newell, D.; Roberts, L.; Vase, L.; Draper-Rodi, J. Avoiding Nocebo and Other Undesirable Effects in Chiropractic, Osteopathy and Physiotherapy: An Invitation to Reflect. Musculoskelet. Sci. Pract. 2022, 62, 102677. [Google Scholar] [CrossRef]
- Fryer, G. Intervertebral Dysfunction: A Discussion of the Manipulable Spinal Lesion. J. Osteopat. Med. 2003, 6, 64–73. [Google Scholar] [CrossRef]
- Lucas, N.; Moran, R. What Is the Significance of Somatic Dysfunction in a Multicausal Model of Aetiology? Int. J. Osteopat. Med. 2005, 8, 39–40. [Google Scholar] [CrossRef][Green Version]
- Moran, R. Somatic Dysfunction—Conceptually Fascinating, but Does It Help Us Address Health Needs? Int. J. Osteopat. Med. 2016, 22, 1–2. [Google Scholar] [CrossRef]
- Basile, F.; Scionti, R.; Petracca, M. Diagnostic Reliability of Osteopathic Tests: A Systematic Review. Int. J. Osteopat. Med. 2017, 25, 21–29. [Google Scholar] [CrossRef]
- Guillaud, A.; Darbois, N.; Monvoisin, R.; Pinsault, N. Reliability of Diagnosis and Clinical Efficacy of Visceral Osteopathy: A Systematic Review. BMC Complement Altern. Med. 2018, 18, 65. [Google Scholar] [CrossRef]
- Guillaud, A.; Darbois, N.; Monvoisin, R.; Pinsault, N. Reliability of Diagnosis and Clinical Efficacy of Cranial Osteopathy: A Systematic Review. PLoS ONE 2016, 11, e0167823. [Google Scholar] [CrossRef]
- Noy, M.; Macedo, L.; Carlesso, L. Biomedical Origins of the Term “osteopathic Lesion” and Its Impact on People in Pain. Int. J. Osteopat. Med. 2020, 37, 40–43. [Google Scholar] [CrossRef]
- Bergna, A.; Vismara, L.; Parravicini, G.; Dal Farra, F. A New Perspective for Somatic Dysfunction in Osteopathy: The Variability Model. J. Bodyw. Mov. Ther. 2020, 24, 181–189. [Google Scholar] [CrossRef]
- International Classification of Functioning, Disability and Health (ICF). Available online: https://icd.who.int/dev11/l-icf/en (accessed on 24 November 2022).
- Беляев, А.Ф. Остеoпатия и Междунарoдная классификация функциoнирoвания, oграничений жизнедеятельнoсти и здoрoвья (часть 1). Рoссийский oстеoпатический журнал 2021, 99–108. [Google Scholar] [CrossRef]
- Беляев, А.Ф. Остеoпатия и Междунарoдная классификация функциoнирoвания, oграничений жизнедеятельнoсти и здoрoвья (часть 2). Рoссийский oстеoпатический журнал 2021, 86–97. [Google Scholar] [CrossRef]
- Bettelli, L.; Pisa, V.; Formica, A. “I Do It My Way”—Italian Osteopaths’ Beliefs and Attitudes about Five Osteopathic Models: A Qualitative Study. Int. J. Osteopat. Med. 2020, 38, 57–64. [Google Scholar] [CrossRef]
- Tramontano, M.; Tamburella, F.; Dal Farra, F.; Bergna, A.; Lunghi, C.; Innocenti, M.; Cavera, F.; Savini, F.; Manzo, V.; D’Alessandro, G. International Overview of Somatic Dysfunction Assessment and Treatment in Osteopathic Research: A Scoping Review. Healthcare 2021, 10, 28. [Google Scholar] [CrossRef] [PubMed]
- Ponzo, V.; Cinnera, A.M.; Mommo, F.; Caltagirone, C.; Koch, G.; Tramontano, M. Osteopathic Manipulative Therapy Potentiates Motor Cortical Plasticity. J. Osteopat. Med. 2018, 118, 396–402. [Google Scholar] [CrossRef] [PubMed]
- Tamburella, F.; Piras, F.; Piras, F.; Spanò, B.; Tramontano, M.; Gili, T. Cerebral Perfusion Changes After Osteopathic Manipulative Treatment: A Randomized Manual Placebo-Controlled Trial. Front. Physiol. 2019, 10, 403. [Google Scholar] [CrossRef] [PubMed]
- Cerritelli, F.; Chiacchiaretta, P.; Gambi, F.; Perrucci, M.G.; Barassi, G.; Visciano, C.; Bellomo, R.G.; Saggini, R.; Ferretti, A. Effect of Manual Approaches with Osteopathic Modality on Brain Correlates of Interoception: An FMRI Study. Sci. Rep. 2020, 10, 3214. [Google Scholar] [CrossRef]
- Simmonds, N.; Miller, P.; Gemmell, H. A Theoretical Framework for the Role of Fascia in Manual Therapy. J. Bodyw. Mov. Ther. 2012, 16, 83–93. [Google Scholar] [CrossRef]
- Fryer, G. Integrating Osteopathic Approaches Based on Biopsychosocial Therapeutic Mechanisms. Part 1: The Mechanisms. Int. J. Osteopat. Med. 2017, 25, 30–41. [Google Scholar] [CrossRef]
- Fryer, G. Integrating Osteopathic Approaches Based on Biopsychosocial Therapeutic Mechanisms. Part 2: Clinical Approach. Int. J. Osteopat. Med. 2017, 26, 36–43. [Google Scholar] [CrossRef]
- Lederman, E. A Process Approach in Osteopathy: Beyond the Structural Model. Int. J. Osteopat. Med. 2017, 23, 22–35. [Google Scholar] [CrossRef]
- Dugailly, P.-M.; Fassin, S.; Maroye, L.; Evers, L.; Klein, P.; Feipel, V. Effect of a General Osteopathic Treatment on Body Satisfaction, Global Self Perception and Anxiety: A Randomized Trial in Asymptomatic Female Students. Int. J. Osteopat. Med. 2014, 17, 94–101. [Google Scholar] [CrossRef]
- McGlone, F.; Cerritelli, F.; Walker, S.; Esteves, J. The Role of Gentle Touch in Perinatal Osteopathic Manual Therapy. Neurosci. Biobehav. Rev. 2017, 72, 1–9. [Google Scholar] [CrossRef]
- Elkiss, M.L.; Jerome, J.A. Touch—More Than a Basic Science. J. Osteopat. Med. 2012, 112, 514–517. [Google Scholar] [CrossRef]
- Consedine, S.; Standen, C.; Niven, E. Knowing Hands Converse with an Expressive Body—An Experience of Osteopathic Touch. Int. J. Osteopat. Med. 2016, 19, 3–12. [Google Scholar] [CrossRef]
- Gyer, G.; Michael, J.; Inklebarger, J.; Tedla, J.S. Spinal Manipulation Therapy: Is It All about the Brain? A Current Review of the Neurophysiological Effects of Manipulation. J. Integr. Med. 2019, 17, 328–337. [Google Scholar] [CrossRef] [PubMed]
- Courtney, R.; van Dixhoorn, J.; Cohen, M. Evaluation of Breathing Pattern: Comparison of a Manual Assessment of Respiratory Motion (MARM) and Respiratory Induction Plethysmography. Appl. Psychophysiol. Biofeedback 2008, 33, 91–100. [Google Scholar] [CrossRef]
- Nijs, J.; Van Houdenhove, B.; Oostendorp, R.A.B. Recognition of Central Sensitization in Patients with Musculoskeletal Pain: Application of Pain Neurophysiology in Manual Therapy Practice. Man. Ther. 2010, 15, 135–141. [Google Scholar] [CrossRef]
- Wilke, J.; Krause, F.; Vogt, L.; Banzer, W. What Is Evidence-Based About Myofascial Chains: A Systematic Review. Arch. Phys. Med. Rehabil. 2016, 97, 454–461. [Google Scholar] [CrossRef]
- Martinez, E.; Redding, D. Osteopathic Response to the COVID-19 Pandemic. J. Osteopat. Med. 2020, 120, 492–494. [Google Scholar] [CrossRef]
- D’Alessandro, G.; Cerritelli, F.; Cortelli, P. Sensitization and Interoception as Key Neurological Concepts in Osteopathy and Other Manual Medicines. Front. Neurosci. 2016, 10, 100. [Google Scholar] [CrossRef]
- Jerome, J.A. An Osteopathic Approach to Chronic Pain Management. J. Osteopat. Med. 2017, 117, 306–314. [Google Scholar] [CrossRef][Green Version]




Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Consorti, G.; Castagna, C.; Tramontano, M.; Longobardi, M.; Castagna, P.; Di Lernia, D.; Lunghi, C. Reconceptualizing Somatic Dysfunction in the Light of a Neuroaesthetic Enactive Paradigm. Healthcare 2023, 11, 479. https://doi.org/10.3390/healthcare11040479
Consorti G, Castagna C, Tramontano M, Longobardi M, Castagna P, Di Lernia D, Lunghi C. Reconceptualizing Somatic Dysfunction in the Light of a Neuroaesthetic Enactive Paradigm. Healthcare. 2023; 11(4):479. https://doi.org/10.3390/healthcare11040479
Chicago/Turabian StyleConsorti, Giacomo, Carmine Castagna, Marco Tramontano, Mauro Longobardi, Paolo Castagna, Daniele Di Lernia, and Christian Lunghi. 2023. "Reconceptualizing Somatic Dysfunction in the Light of a Neuroaesthetic Enactive Paradigm" Healthcare 11, no. 4: 479. https://doi.org/10.3390/healthcare11040479
APA StyleConsorti, G., Castagna, C., Tramontano, M., Longobardi, M., Castagna, P., Di Lernia, D., & Lunghi, C. (2023). Reconceptualizing Somatic Dysfunction in the Light of a Neuroaesthetic Enactive Paradigm. Healthcare, 11(4), 479. https://doi.org/10.3390/healthcare11040479









