Hospice and Palliative Care during Disasters: A Systematic Review
Abstract
:1. Introduction
2. Methods
2.1. Eligibility Criteria
2.2. Information Sources and Search Strategy
2.3. Selection Process
2.4. Data Extraction
2.5. Quality Appraisal
2.6. Data Synthesis
3. Results
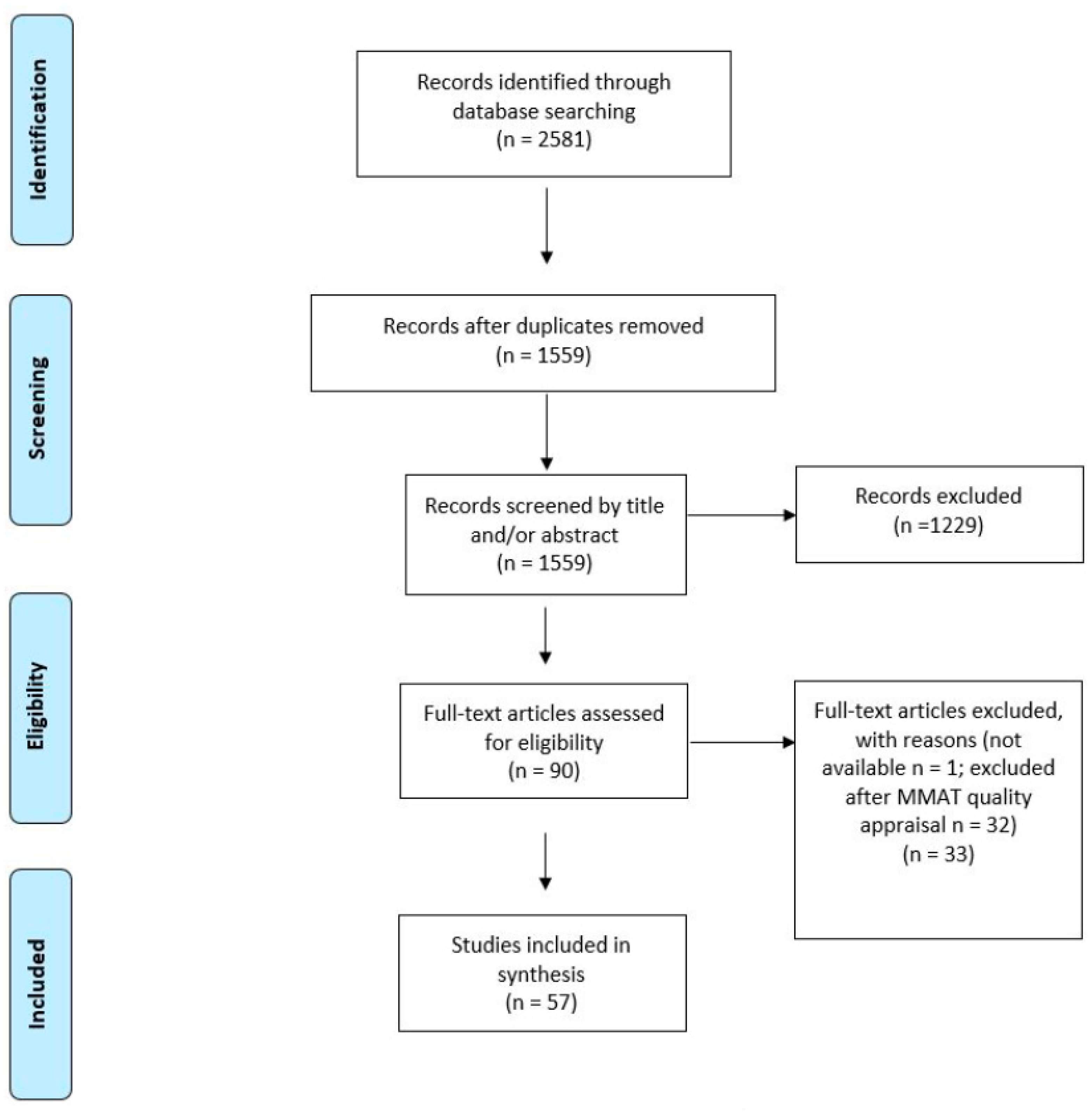
3.1. Study Selection
3.2. Study Characteristics
| Author | Country & Year | Design | Sample |
|---|---|---|---|
| Aaronson et al. [25] | USA 2021 | Interview study/ semi-structured interviews | ED and PC clinicians (n = 31) |
| Baker Rogers et al. [26] | USA 2022 | Online survey | Members of the AAHPM and the HPNA (n = 83) |
| Becqué et al. [27] | Netherlands 2022 | Interview study/in-depth narrative interviews | Purposively sampled bereaved relatives of patients who died during the COVID-19 Pandemic (n = 25) |
| Beltran-Aroca et al. [28] | Spain 2021 | Retrospective observational cohort study | PC internal management database including all cancer patients treated in the period 2018–2021 (n = 1967) |
| Bradshaw et al. [29] | United Kingdom 2022 | Qualitative multiple case study using semi-structured interviews | PC professionals (n = 24) |
| Bradshaw et al. [30] | United Kingdom 2021 | Online survey | Palliative/hospice services (n = 277) |
| Chen et al. [20] | Taiwan 2006 | Descriptive study | Comparison of in-patient admissions during 2002 and 2003 from the National Health Insurance Research Database with before-and-after comparisons |
| Chisbert-Alapont et al. [31] | Spain 2021 | Cross-sectional descriptive study | Nursing professionals (n = 238) |
| Chou et al. [32] | Taiwan 2020 | Cohort study | All patients cared for at Taipei Hospital from 2019 to 2020 (n = 19,900) |
| Costantini et al. [33] | Italy 2020 | Cross-sectional telephone survey | Purposively sampled hospices (n = 16) |
| Doherty et al. [24] | Bangladesh 2020 | Cross-sectional study with closed-ended interview questioning | Convenience sampling of individuals with serious health problems (n = 156) and caregivers (n = 155) |
| Dunleavy et al. [34] | United Kingdom 2021 | Online multinational cross-sectional survey | Hospice and specialist PC providers (n = 458) |
| Finuf et al. [35] | USA 2022 | Online survey | Members of palliative medical teams among 14 hospitals (n = 64) |
| Fish and Lloyd [36] | Scotland 2022 | Interview study/in-depth narrative interviews | PC doctors (n = 8) |
| Franchini et al. [37] | Italy 2022 | Survey/semi-structured telephone interviews | Home palliative care professionals; physicians (n = 15) and nurses (n = 15) |
| Garcia et al. [38] | Brazil 2022 | Descriptive, cross-sectional survey with an online questionnaire | Healthcare professionals (n = 336) |
| Garner et al. [39] | United Kingdom 2022 | Mixed-method | Online survey with UK hospices (n = 143); qualitative interviews with hospice professionals (n = 24) |
| Gerlach et al. [40] | Germany 2022 | Interview study/ semi-structured interviews | Patients (n = 15) and family caregivers (n = 16) |
| Gonella et al. [41] | Italy 2022 | Descriptive interview-study/inductive thematic analysis | Healthcare professionals (n = 21) |
| Hanna et al. [42] | United Kingdom 2021 | Interview study/ semi-structured interviews | Health and social care professionals supporting dying patients (n = 16) |
| Hanna et al. [43] | United Kingdom 2021 | Interview study/ semi-structured interviews | Bereaved family members (n = 19) |
| Hanna et al. [44] | United Kingdom 2022 | Interview study/semi-structured interviews | Family carers (n = 26) and care home staff (n = 16) |
| Hasson et al. [45] | United Kingdom 2022 | Online census survey | Managers of hospices (n = 150) |
| Haydar et al. [46] | USA 2020 | Retrospective single-center study | Patients with COVID-19 (n = 242) |
| Hunt et al. [21] | Canada 2020 | Interview study/ in-depth interviews | Humanitarian policy-makers and healthcare professionals (n = 24) |
| Jansky et al. [47] | Germany 2021 | Interview study/focus groups/guided interviews | Representatives of SPHC teams (n = 18) and stakeholders (n = 5) |
| Kates et al. [48] | USA 2020 | Cross-sectional survey | Hospice and PC workforce (n = 36) |
| Klinger et al. [49] | Germany 2022 | Interview study/semi-structured expert interviews | People involved in pandemic management as a staff member attached to a healthcare facility or public institution (n = 41) |
| Lalani et al. [50] | USA 2022 | Interview study/ qualitative interviews | PC professionals in rural areas (n = 15) |
| Leong et al. [22] | Singapore 2004 | Interview study/semi-structured interviews | PC professionals (n = 8) |
| Lin et al. [51] | Taiwan 2021 | Online cross-sectional survey | Subscribers (n = 1551) and organizational members (n = 185) of APHPCN |
| Macchi et al. [52] | Italy 2021 | Qualitative study | Patients (n = 108) and carers (n = 90) |
| Mitchell et al. [53] | United Kingdom 2022 | Cross-sectional online survey | Community nurses (n = 387); general practitioners (n = 156) and ‚other’ (n = 16) |
| Mitchinson et al. [54] | United Kingdom 2021 | Semi-structured telephone interviews | Healthcare workers (n = 22/100 interviews mentioning death) |
| Nestor et al. [55] | Ireland 2021 | Cross-sectional study using standardized questionnaires | Healthcare professionals (n = 250) |
| Nyblom et al. [56] | Sweden 2022 | Interview study/semi-structured interviews | Patients (n = 22) and carers (n = 17) |
| Obata et al. [57] | USA 2020 | Descriptive study | Clinical characteristics and comparisons between patients (n = 225) with COVID 19 with and without PC team consults |
| Oluyase et al. [58] | Multinational 2021 | Online survey | Palliative care services (n = 458; UK n = 277; rest of Europe n = 85; rest of world n = 95) |
| Onwuteaka-Philipsen et al. [59] | Netherlands 2021 | Observational online questionnaire survey | Healthcare professionals (n = 747) |
| Pastrana et al. [60] | Multinational 2021 | Semi-structured online survey | PC professionals (n = 77) from 41 countries |
| Prokopová et al. [61] | Czech Republic 2022 | Cross-sectional study | Healthcare professionals working in intensive care units (n = 313) |
| Rowe et al. [62] | USA 2021 | Interview study/semi-structured interviews | PC clinicians (n = 25) |
| Sabolish et al. [63] | USA 2022 | Retrospective exploratory study | Patients with PC consult (n = 174) and patients without PC consult (n = 152) |
| Samala et al. [64] | USA 2021 | Cross-sectional study | Healthcare professionals (n = 64) |
| Schallenburger et al. [65] | Germany 2022 | Interview study/ semi-structured online focus groups | Healthcare workers (n = 31) |
| Schloesser et al. [66] | Germany 2021 | Post-bereavement online survey with free text options | Bereaved relatives (n = 81) from people who died during the pandemic with and without SARS-CoV2 |
| Schneider et al. [23] | Switzerland 2018 | Interview study/in-depth interviews | Expatriate health workers (n = 15) working with Médecins sans Frontières |
| Schoenherr et al. [67] | USA 2020 | Evaluation of a pilot program for proactive identification of PC needs | Patients with COVID-19 (n = 29) |
| Seibel et al. [68] | Germany 2022 | Interview study/qualitative interviews | Manager and health care workers (n = 29) |
| Selman et al. [69] | United Kingdom 2022 | Open-web survey | Bereaved people (n = 711) |
| Sleeman et al. [70] | United Kingdom 2022 | Cross-sectional online survey | PC services (n = 277) |
| Strang et al. [71] | Sweden 2020 | Descriptive national registry data study | All registered patients who died of COVID-19 either in nursing homes or hospitals |
| Tanzi et al. [72] | Italy 2020 | Single holistic case study design | Physicians (n = 9) and nurses (n = 22) |
| Varani et al. [73] | Italy 2021 | Online survey | PC physicians and nurses (n = 145) working in home assistance compared to data collected in 2016 in the same setting (n = 179) |
| Wind et al. [74] | Denmark 2022 | Semi-structured telephone interviews | Family carers (n = 15) |
| Yildiz et al. [75] | Netherlands 2022 | Open observational online survey | Bereaved family members and friends (n = 393); relatives who lost a family member or friend at home (n = 68); in a hospital (n = 114), nursing home (n = 176) or hospice (n = 35) |
| Zheng et al. [76] | China 2020 | Cross-sectional study | Healthcare professionals (n = 281) |
3.3. Results of Syntheses
3.3.1. Disruption of the System
Underutilization and Shift from Hospitals to Home Services
Disruption of Social Connectedness
Dehumanization of Care
Lack of Resources
Lack of Information and Expertise
3.3.2. Setting-Specific Differences
Preferred Place of Death
Home Palliative Care during Disasters: Between Benefit and Burden
Cultural, Organizational, and Funding Differences in Disaster Response
3.3.3. Emotional Challenges
3.3.4. System Adaptation
4. Discussion
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| MeSH-search-combinations (each combined with ‘AND’) | |
| Palliative care; Palliative medicine; Terminal care; End of life care; Hospices; Hospice care; Hospice and palliative care nursing | Disasters; Eruption, volcanic; Earthquakes; Floods; Hurricane; Drought; Droughts; Typhoon; Avalanche; Cyclonic storms; Pandemics; Epidemics; Warfare and armed conflicts; Terrorism; Weapons; Radioactive hazard release |
| Additional textword search in databases and alert (APA PsycArticles, APA PsycInfo, CINAHL, MEDLINE, SocINDEX) | |
| (palliative care or palliative medicine or end of life care or terminal care or terminal care or hospice care or hospices or hospice and palliative care nursing) AND (disaster or crisis) AND (eruption* or earthquake* or flood* or hurricane* or drought* or cyclonic storm* or typhoon* or avalanche* or cyclone* or pandemic* or epidemic* or war* or armed conflict* or terrorism or weapon* or accident* or power failure or famine or civil war or war) | |
References
- WHO & EHA. Disasters & Emergencies Definitions. Training Package. 2002. Available online: https://lms.must.ac.ug/claroline/backends/download.php?url=Lzc2NTZfd2hhdF9pc19kaXNhc3Rlci5wZGY%3D&cidReset=true&cidReq=BALFP3209_001 (accessed on 20 August 2023).
- United Nations Office for Disaster Risk Reduction (UNDRR). Terminology Disaster. Available online: https://www.undrr.org/terminology/disaster (accessed on 22 February 2023).
- Lancet, T. Palliative care and the COVID-19 pandemic. Lancet 2020, 395, 1168. [Google Scholar] [CrossRef] [PubMed]
- Shaluf, I. An Overview on Disasters. Disaster Prev. Manag. 2007, 16, 687–703. [Google Scholar] [CrossRef]
- CRED. Human Cost of Natural Disasters 2015. A Global Perspective. 2015. Available online: https://climate-adapt.eea.europa.eu/en/metadata/publications/the-human-cost-of-natural-disasters-2015-a-global-perspective/11258275 (accessed on 23 February 2023).
- UN. Sendai Framework for Disaster Risk Reduction 2015–2030; The United Nations Office for Disaster Risk Reduction: Geneva, Switzerland, 2015. Available online: https://www.preventionweb.net/files/43291_sendaiframeworkfordrren.pdf?_gl=1*1451gp*_ga*NDQ5MjIxMzAxLjE2NzcxNjI2OTk.*_ga_D8G5WXP6YM*MTY3NzE2OTI4NC4yLjEuMTY3NzE2OTUwMy4wLjAuMA (accessed on 22 February 2023).
- WHO. Building Health Systems Resilience for Universal Health Coverage and Health Security during the COVID-19 Pandemic and Beyond. 2021. Available online: https://www.who.int/publications/i/item/WHO-UHL-PHC-SP-2021.01 (accessed on 23 February 2023).
- WHO. Integrating Palliative Care and Symptom Relief into the Response to Humanitarian Emergencies and Crises: A WHO guide. 2018. Available online: https://www.who.int/publications/i/item/9789241514460 (accessed on 23 February 2023).
- Ciottone, G.R. (Ed.) Chapter 1—Introduction to Disaster Medicine. In Ciottone’s Disaster Medicine, 2nd ed.; Elsevier: Amsterdam, The Netherlands, 2016; pp. 2–5. [Google Scholar]
- Powell, R.A.; Schwartz, L.; Nouvet, E.; Sutton, B.; Petrova, M.; Marston, J.; Munday, D.; Radbruch, L. Palliative care in humanitarian crises: Always something to offer. Lancet 2017, 389, 1498–1499. [Google Scholar] [CrossRef] [PubMed]
- Kelly, M.; Mitchell, I.; Walker, I.; Mears, J.; Scholz, B. End-of-life care in natural disasters including epidemics and pandemics: A systematic review. BMJ Support. Palliat. Care 2021, 13, 1. [Google Scholar] [CrossRef] [PubMed]
- Nouvet, E.; Sivaram, M.; Bezanson, K.; Krishnaraj, G.; Hunt, M.; de Laat, S.; Sanger, S.; Banfield, L.; Rodriguez, P.F.E.; Schwartz, L.J. Palliative care in humanitarian crises: A review of the literature. J. Int. Humanit. Action 2018, 3, 5. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Ouzzani, M.; Hammady, H.; Fedorowicz, Z.; Elmagarmid, A. Rayyan—A web and mobile app for systematic reviews. Syst. Rev. 2016, 5, 210. [Google Scholar] [CrossRef]
- Hong, Q.N.; Pluye, P.; Fàbregues, S.; Bartlett, G.; Boardman, F.; Cargo, M.; Dagenais, P.; Gagnon, M.-P.; Griffiths, F.; Nicolau, B.; et al. Improving the content validity of the mixed methods appraisal tool: A modified e-Delphi study. J. Clin. Epidemiol. 2019, 111, 49–59.e1. [Google Scholar] [CrossRef]
- Hong, Q.N.; Pluye, P.; Fàbregues, S.; Bartlett, G.; Cargo, M.; Boardman, F.; Dagenais, P.; Gagnon, M.-P.; Griffiths, F.; Nicolau, B.; et al. Mixed Methods Appraisal Tool (MMAT), Version 2018. User Guide; McGill University: Montreal, AC, Canada, 2018. [Google Scholar]
- Harden, A.; Gough, D. Quality and relevance appraisal. In An Introduction to Systematic Reviews; Gough, D., Oliver, S., Thomas, J., Eds.; Sage Publications Ltd.: Thousand Oaks, CA, USA, 2012; pp. 153–179. [Google Scholar]
- Petticrew, M.; Roberts, H. How to Appraise the Studies: An Introduction to Assessing Study Quality. In Systematic Reviews in the Social Sciences; Wiley: Hoboken, NJ, USA, 2006; pp. 125–163. [Google Scholar]
- Popay, J.; Roberts, H.; Sowden, A.; Petticrew, M.; Arai, L.; Rodgers, M.; Britten, N.; Roen, K.; Duffy, S. Guidance on the Conduct of Narrative Synthesis in Systematic Reviews. A Product from the ESRC Methods Programme; Lancaster University: Lancaster, UK, 2006; Available online: https://www.lancaster.ac.uk/media/lancaster-university/content-assets/documents/fhm/dhr/chir/NSsynthesisguidanceVersion1-April2006.pdf (accessed on 29 March 2023).
- Chen, T.-J.; Lin, M.-H.; Chou, L.-F.; Hwang, S.-J. Hospice utilization during the SARS outbreak in Taiwan. BMC Health Serv. Res. 2006, 6, 94. [Google Scholar] [CrossRef]
- Hunt, M.; Nouvet, E.; Chénier, A.; Krishnaraj, G.; Bernard, C.; Bezanson, K.; de Laat, S.; Schwartz, L. Addressing obstacles to the inclusion of palliative care in humanitarian health projects: A qualitative study of humanitarian health professionals’ and policy makers’ perceptions. Confl. Health 2020, 14, 70. [Google Scholar] [CrossRef]
- Leong, I.Y.; Lee, A.O.; Ng, T.W.; Lee, L.B.; Koh, N.Y.; Yap, E.; Guay, S.; Ng, L.M. The challenge of providing holistic care in a viral epidemic: Opportunities for palliative care. Palliat. Med. 2004, 18, 12–18. [Google Scholar] [CrossRef]
- Schneider, M.; Chappuis, F.; Pautex, S. How do expatriate health workers cope with needs to provide palliative care in humanitarian emergency assistance? A qualitative study with in-depth interviews. Palliat. Med. 2018, 32, 1567–1574. [Google Scholar] [CrossRef]
- Doherty, M.; Power, L.; Petrova, M.; Gunn, S.; Powell, R.; Coghlan, R.; Grant, L.; Sutton, B.; Khan, F. Illness-related suffering and need for palliative care in Rohingya refugees and caregivers in Bangladesh: A cross-sectional study. PLoS Med. 2020, 17, e1003011. [Google Scholar] [CrossRef] [PubMed]
- Aaronson, E.L.; Daubman, B.R.; Petrillo, L.; Bowman, J.; Ouchi, K.; Gips, A.; Traeger, L.; Jackson, V.; Grudzen, C.; Ritchie, C.S. Emerging Palliative Care Innovations in the ED: A Qualitative Analysis of Programmatic Elements During the COVID-19 Pandemic. J. Pain Symptom Manag. 2021, 62, 117–124. [Google Scholar] [CrossRef]
- Baker Rogers, J.E.; Thompson, J.M.; Mupamombe, C.T.; Vanin, J.M.; Navia, R.O. Hospice Emergency Planning and COVID-19. J. Palliat. Care 2022, 37, 34–40. [Google Scholar] [CrossRef]
- Becqué, Y.N.; van der Geugten, W.; van der Heide, A.; Korfage, I.J.; Pasman, H.R.W.; Onwuteaka-Philipsen, B.D.; Zee, M.; Witkamp, E.; Goossensen, A. Dignity reflections based on experiences of end-of-life care during the first wave of the COVID-19 pandemic: A qualitative inquiry among bereaved relatives in the Netherlands (the CO-LIVE study). Scand. J. Caring Sci. 2022, 36, 769–781. [Google Scholar] [CrossRef]
- Beltran-Aroca, C.M.; Ruiz-Montero, R.; Llergo-Muñoz, A.; Rubio, L.; Girela-López, E. Impact of the COVID-19 Pandemic on Palliative Care in Cancer Patients in Spain. Int. J. Environ. Res. Public Health 2021, 18, 11992. [Google Scholar] [CrossRef]
- Bradshaw, A.; Dunleavy, L.; Garner, I.; Preston, N.; Bajwah, S.; Cripps, R.; Fraser, L.K.; Maddocks, M.; Hocaoglu, M.; Murtagh, F.E.M.; et al. Experiences of staff providing specialist palliative care during COVID-19: A multiple qualitative case study. J. R. Soc. Med. 2022, 115, 220–230. [Google Scholar] [CrossRef]
- Bradshaw, A.; Dunleavy, L.; Walshe, C.; Preston, N.; Cripps, R.L.; Hocaoglu, M.; Bajwah, S.; Maddocks, M.; Oluyase, A.O.; Sleeman, K.; et al. Understanding and addressing challenges for advance care planning in the COVID-19 pandemic: An analysis of the UK CovPall survey data from specialist palliative care services. Palliat. Med. 2021, 35, 1225–1237. [Google Scholar] [CrossRef]
- Chisbert-Alapont, E.; García-Salvador, I.; De La Ossa-Sendra, M.J.; García-Navarro, E.B.; De La Rica-Escuín, M. Influence of Palliative Care Training on Nurses’ Attitudes towards End-of-Life Care during the COVID-19 Pandemic in Spain. Int. J. Environ. Res. Public Health 2021, 18, 11249. [Google Scholar] [CrossRef] [PubMed]
- Chou, Y.C.; Yen, Y.F.; Feng, R.C.; Wu, M.P.; Lee, Y.L.; Chu, D.; Huang, S.J.; Curtis, J.R.; Hu, H.Y. Impact of the COVID-19 Pandemic on the Utilization of Hospice Care Services: A Cohort Study in Taiwan. J. Pain Symptom Manag. 2020, 60, e1–e6. [Google Scholar] [CrossRef] [PubMed]
- Costantini, M.; Sleeman, K.E.; Peruselli, C.; Higginson, I.J. Response and role of palliative care during the COVID-19 pandemic: A national telephone survey of hospices in Italy. Palliat. Med. 2020, 34, 889–895. [Google Scholar] [CrossRef] [PubMed]
- Dunleavy, L.; Preston, N.; Bajwah, S.; Bradshaw, A.; Cripps, R.; Fraser, L.K.; Maddocks, M.; Hocaoglu, M.; Murtagh, F.E.M.; Oluyase, A.O.; et al. ‘Necessity is the mother of invention’: Specialist palliative care service innovation and practice change in response to COVID-19. Results from a multinational survey (CovPall). Palliat. Med. 2021, 35, 814–829. [Google Scholar] [CrossRef]
- Finuf, K.D.; Lopez, S.; Carney, M.T. Coping Through COVID-19: A Mixed Method Approach to Understand How Palliative Care Teams Managed the COVID-19 Pandemic. Am. J. Hosp. Palliat. Med. 2022, 39, 874–880. [Google Scholar] [CrossRef] [PubMed]
- Fish, E.C.; Lloyd, A. Moral distress amongst palliative care doctors working during the COVID-19 pandemic: A narrative-focussed interview study. Palliat. Med. 2022, 36, 955–963. [Google Scholar] [CrossRef]
- Franchini, L.; Varani, S.; Ostan, R.; Bocchi, I.; Pannuti, R.; Biasco, G.; Bruera, E. Home palliative care professionals perception of challenges during the COVID-19 outbreak: A qualitative study. Palliat. Med. 2021, 35, 862–874. [Google Scholar] [CrossRef]
- Garcia, A.C.M.; Ferreira, A.C.G.; Silva, L.S.R.; da Conceição, V.M.; Nogueira, D.A.; Mills, J. Mindful Self-Care, Self-Compassion, and Resilience Among Palliative Care Providers During the COVID-19 Pandemic. J. Pain Symptom Manag. 2022, 64, 49–57. [Google Scholar] [CrossRef]
- Garner, I.W.; Walshe, C.; Dunleavy, L.; Bradshaw, A.; Preston, N.; Fraser, L.K.; Murtagh, F.E.M.; Oluyase, A.O.; Sleeman, K.E.; Hocaoglu, M.; et al. Charitably funded hospices and the challenges associated with the COVID-19 pandemic: A mixed-methods study (CovPall). BMC Palliat. Care 2022, 21, 176. [Google Scholar] [CrossRef]
- Gerlach, C.; Ullrich, A.; Berges, N.; Bausewein, C.; Oechsle, K.; Hodiamont, F. The Impact of the SARS-CoV-2 Pandemic on the Needs of Non-Infected Patients and Their Families in Palliative Care-Interviews with Those Concerned. J. Clin. Med. 2022, 11, 3863. [Google Scholar] [CrossRef]
- Gonella, S.; Di Giulio, P.; Antal, A.; Cornally, N.; Martin, P.; Campagna, S.; Dimonte, V. Challenges Experienced by Italian Nursing Home Staff in End-of-Life Conversations with Family Caregivers during COVID-19 Pandemic: A Qualitative Descriptive Study. Int. J. Environ. Res. Public Health 2022, 19, 2504. [Google Scholar] [CrossRef]
- Hanna, J.R.; Rapa, E.; Dalton, L.J.; Hughes, R.; Quarmby, L.M.; McGlinchey, T.; Donnellan, W.J.; Bennett, W.J.; Mayland, C.R.; Mason, S.R. Health and social care professionals’ experiences of providing end of life care during the COVID-19 pandemic: A qualitative study. Palliat. Med. 2021, 35, 1249–1257. [Google Scholar] [CrossRef] [PubMed]
- Hanna, J.R.; Rapa, E.; Dalton, L.J.; Hughes, R.; McGlinchey, T.; Bennett, K.M.; Donnellan, W.J.; Mason, S.R.; Mayland, C.R. A qualitative study of bereaved relatives’ end of life experiences during the COVID-19 pandemic. Palliat. Med. 2021, 35, 843–851. [Google Scholar] [CrossRef] [PubMed]
- Hanna, K.; Cannon, J.; Gabbay, M.; Marlow, P.; Mason, S.; Rajagopal, M.; Shenton, J.; Tetlow, H.; Giebel, C. End of life care in UK care homes during the COVID-19 pandemic: A qualitative study. BMC Palliat. Care 2022, 21, 91. [Google Scholar] [CrossRef] [PubMed]
- Hasson, F.; Slater, P.; Fee, A.; McConnell, T.; Payne, S.; Finlay, D.A.; McIlfatrick, S. The impact of COVID-19 on out-of-hours adult hospice care: An online survey. BMC Palliat. Care 2022, 21, 94. [Google Scholar] [CrossRef] [PubMed]
- Haydar, A.; Lo, K.B.; Goyal, A.; Gul, F.; Peterson, E.; Bhargav, R.; DeJoy, R., III; Salacup, G.; Pelayo, J.; Albano, J.; et al. Palliative Care Utilization among Patients with COVID-19 in an Underserved Population: A Single-Center Retrospective Study. J. Pain Symptom Manag. 2020, 60, e18–e21. [Google Scholar] [CrossRef]
- Jansky, M.; Schade, F.; Rieder, N.; Lohrmann, D.; Gebel, C.; Kloppenburg, L.; Wedding, U.; Simon, S.T.; Bausewein, C.; Nauck, F. ‘It felt like a black hole, great uncertainty, but we have to take care for our patients’-Qualitative findings on the effects of the COVID-19 pandemic on specialist palliative home care. PLoS ONE 2021, 16, e0260767. [Google Scholar] [CrossRef]
- Kates, J.; Gerolamo, A.; Pogorzelska-Maziarz, M. The impact of COVID-19 on the hospice and palliative care workforce. Public Health Nurs. 2021, 38, 459–463. [Google Scholar] [CrossRef]
- Klinger, I.; Heckel, M.; Shahda, S.; Kriesen, U.; Schneider, C.; Kurkowski, S.; Junghanss, C.; Ostgathe, C. COVID-19: Challenges and solutions for the provision of care to seriously ill and dying people and their relatives during SARS-CoV-2 pandemic—Perspectives of pandemic response team members: A qualitative study on the basis of expert interviews (part of PallPan). Palliat. Med. 2022, 36, 1092–1103. [Google Scholar] [CrossRef]
- Lalani, N.; Cai, Y.; Wang, Y. “Hard to Say Goodbye Over iPad”: Experiences of Palliative Care Providers and Lessons Learned During the COVID-19 Pandemic in Rural Communities of Indiana, United States. J. Hosp. Palliat. Nurs. 2022, 24, E94–E100. [Google Scholar] [CrossRef]
- Lin, C.P.; Boufkhed, S.; Kizawa, Y.; Mori, M.; Hamzah, E.; Aggarwal, G.; Namisango, E.; Higgingson, I.J.; Goh, C.; Harding, R. Preparedness to Face the COVID-19 Pandemic in Hospice and Palliative Care Services in the Asia-Pacific Region: A Rapid Online Survey. Am. J. Hosp. Palliat. Care 2021, 38, 861–868. [Google Scholar] [CrossRef]
- Macchi, Z.A.; Ayele, R.; Dini, M.; Lamira, J.; Katz, M.; Pantilat, S.Z.; Jones, J.; Kluger, B.M. Lessons from the COVID-19 pandemic for improving outpatient neuropalliative care: A qualitative study of patient and caregiver perspectives. Palliat. Med. 2021, 35, 1258–1266. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, S.; Harrison, M.; Oliver, P.; Gardiner, C.; Chapman, H.; Khan, D.; Boyd, K.; Dale, J.; Barclay, S.; Mayland, C.R. Service change and innovation in community end-of-life care during the COVID-19 pandemic: Qualitative analysis of a nationwide primary care survey. Palliat. Med. 2022, 36, 161–170. [Google Scholar] [CrossRef] [PubMed]
- Mitchinson, L.; Dowrick, A.; Buck, C.; Hoernke, K.; Martin, S.; Vanderslott, S.; Robinson, H.; Rankl, F.; Manby, L.; Lewis-Jackson, S.; et al. Missing the human connection: A rapid appraisal of healthcare workers’ perceptions and experiences of providing palliative care during the COVID-19 pandemic. Palliat. Med. 2021, 35, 852–861. [Google Scholar] [CrossRef] [PubMed]
- Nestor, S.; O’Tuathaigh, C.; O’Brien, T. Assessing the impact of COVID-19 on healthcare staff at a combined elderly care and specialist palliative care facility: A cross-sectional study. Palliat. Med. 2021, 35, 1492–1501. [Google Scholar] [CrossRef] [PubMed]
- Nyblom, S.; Benkel, I.; Carling, L.; Löfdahl, E.; Molander, U.; Öhlén, J. Pandemic impact on patients with advanced non-COVID-19 illness and their family carers receiving specialised palliative home care: A qualitative study. BMJ Open 2022, 12, e059577. [Google Scholar] [CrossRef]
- Obata, R.; Maeda, T.; Rizk, D.; Kuno, T. Palliative Care Team Involvement in Patients With COVID-19 in New York City. Am. J. Hosp. Palliat. Care 2020, 37, 869–872. [Google Scholar] [CrossRef]
- Oluyase, A.O.; Hocaoglu, M.; Cripps, R.L.; Maddocks, M.; Walshe, C.; Fraser, L.K.; Preston, N.; Dunleavy, L.; Bradshaw, A.; Murtagh, F.E.M.; et al. The Challenges of Caring for People Dying From COVID-19: A Multinational, Observational Study (CovPall). J. Pain Symptom Manag. 2021, 62, 460–470. [Google Scholar] [CrossRef]
- Onwuteaka-Philipsen, B.D.; Pasman, H.R.W.; Korfage, I.J.; Witkamp, E.; Zee, M.; van Lent, L.G.G.; Goossensen, A.; van der Heide, A. Dying in times of the coronavirus: An online survey among healthcare professionals about end-of-life care for patients dying with and without COVID-19 (the CO-LIVE study). Palliat. Med. 2021, 35, 830–842. [Google Scholar] [CrossRef]
- Pastrana, T.; De Lima, L.; Pettus, K.; Ramsey, A.; Napier, G.; Wenk, R.; Radbruch, L. The impact of COVID-19 on palliative care workers across the world: A qualitative analysis of responses to open-ended questions. Palliat. Support. Care 2021, 19, 187–192. [Google Scholar] [CrossRef]
- Prokopová, T.; Hudec, J.; Vrbica, K.; Staŝek, J.; Pokorná, A.; Štourač, P.; Rusinová, K.; Kerpnerová, P.; Štěpánová, R.; Svobodník, A.; et al. Palliative care practice and moral distress during COVID-19 pandemic (PEOpLE-C19 study): A national, cross-sectional study in intensive care units in the Czech Republic. Crit. Care 2022, 26, 221. [Google Scholar] [CrossRef]
- Rowe, J.G.; Potts, M.; McGhie, R.; Dinh, A.; Engel, I.; England, K.; Sinclair, C.T. Palliative Care Practice During the COVID-19 Pandemic: A Descriptive Qualitative Study of Palliative Care Clinicians. J. Pain Symptom Manag. 2021, 62, 1111–1116. [Google Scholar] [CrossRef] [PubMed]
- Sabolish, R.M.; Wilson, J.M.; Caldwell, H.K. Palliative Care in a Pandemic: A Retrospective Review of the Impact of Early Palliative Care Consultation During the Coronavirus Disease 2019 Pandemic. J. Hosp. Palliat. Nurs 2022, 24, 50–56. [Google Scholar] [CrossRef] [PubMed]
- Samala, R.V.; Range, P.; Hoeksema, L.J.; Fong, K.; Shoemaker, L. Health Professionals’ Perceptions of the Contributions of Palliative Care Consultation for Patients with COVID-19. J. Palliat. Med. 2021, 24, 1872–1876. [Google Scholar] [CrossRef]
- Schallenburger, M.; Reuters, M.C.; Schwartz, J.; Fischer, M.; Roch, C.; Werner, L.; Bausewein, C.; Simon, S.T.; van Oorschot, B.; Neukirchen, M. Inpatient generalist palliative care during the SARS-CoV-2 pandemic—Experiences, challenges and potential solutions from the perspective of health care workers. BMC Palliat. Care 2022, 21, 63. [Google Scholar] [CrossRef] [PubMed]
- Schloesser, K.; Simon, S.T.; Pauli, B.; Voltz, R.; Jung, N.; Leisse, C.; van der Heide, A.; Korfage, I.J.; Pralong, A.; Bausewein, C.; et al. “Saying goodbye all alone with no close support was difficult”—Dying during the COVID-19 pandemic: An online survey among bereaved relatives about end-of-life care for patients with or without SARS-CoV2 infection. BMC Health Serv. Res. 2021, 21, 998. [Google Scholar] [CrossRef] [PubMed]
- Schoenherr, L.A.; Cook, A.; Peck, S.; Humphreys, J.; Goto, Y.; Saks, N.T.; Huddleston, L.; Elia, G.; Pantilat, S.Z. Proactive Identification of Palliative Care Needs Among Patients With COVID-19 in the ICU. J. Pain Symptom Manag. 2020, 60, e17–e21. [Google Scholar] [CrossRef]
- Seibel, K.; Couné, B.; Mueller, M.; Boehlke, C.; Simon, S.T.; Bausewein, C.; Becker, G. Implementation of an acute palliative care unit for COVID-19 patients in a tertiary hospital: Qualitative data on clinician perspectives. Palliat. Med. 2022, 36, 332–341. [Google Scholar] [CrossRef]
- Selman, L.E.; Farnell, D.; Longo, M.; Goss, S.; Seddon, K.; Torrens-Burton, A.; Mayland, C.R.; Wakefield, D.; Johnston, B.; Byrne, A.; et al. Risk factors associated with poorer experiences of end-of-life care and challenges in early bereavement: Results of a national online survey of people bereaved during the COVID-19 pandemic. Palliat. Med. 2022, 36, 717–729. [Google Scholar] [CrossRef]
- Sleeman, K.E.; Cripps, R.L.; Murtagh, F.E.M.; Oluyase, A.O.; Hocaoglu, M.B.; Maddocks, M.; Walshe, C.; Preston, N.; Dunleavy, L.; Bradshaw, A.; et al. Change in Activity of Palliative Care Services during the COVID-19 Pandemic: A Multinational Survey (CovPall). J. Palliat. Med. 2022, 25, 465–471. [Google Scholar] [CrossRef]
- Strang, P.; Bergström, J.; Martinsson, L.; Lundström, S. Dying From COVID-19: Loneliness, End-of-Life Discussions, and Support for Patients and Their Families in Nursing Homes and Hospitals. A National Register Study. J. Pain Symptom Manag. 2020, 60, e2–e13. [Google Scholar] [CrossRef]
- Tanzi, S.; Alquati, S.; Martucci, G.; De Panfilis, L. Learning a palliative care approach during the COVID-19 pandemic: A case study in an Infectious Diseases Unit. Palliat. Med. 2020, 34, 1220–1227. [Google Scholar] [CrossRef]
- Varani, S.; Ostan, R.; Franchini, L.; Ercolani, G.; Pannuti, R.; Biasco, G.; Bruera, E. Caring Advanced Cancer Patients at Home During COVID-19 Outbreak: Burnout and Psychological Morbidity Among Palliative Care Professionals in Italy. J. Pain Symptom Manag. 2021, 61, e4–e12. [Google Scholar] [CrossRef] [PubMed]
- Wind, G.; Vedsegaard, H.W.; Marsaa, K.; True, T.S.; Konradsen, H. The significance of the COVID-19 pandemic for family caregivers of non-COVID-19 patients in need of specialized palliative care at home: A qualitative study. Int. J. Qual. Stud. Health Well-Being 2022, 17, 2113021. [Google Scholar] [CrossRef] [PubMed]
- Yildiz, B.; Korfage, I.J.; Witkamp, E.F.; Goossensen, A.; van Lent, L.G.G.; Pasman, H.R.; Onwuteaka-Philipsen, B.D.; Zee, M.; van der Heide, A. Dying in times of COVID-19: Experiences in different care settings—An online questionnaire study among bereaved relatives (the CO-LIVE study). Palliat. Med. 2022, 36, 751–761. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Z.H.; Luo, Z.C.; Zhang, Y.; Chan, W.C.H.; Li, J.Q.; Pang, J.; Jia, Y.L.; Tang, J. Hospice care self-efficacy among clinical medical staff working in the coronavirus disease 2019 (COVID-19) isolation wards of designated hospitals: A cross-sectional study. BMC Palliat Care 2020, 19, 188. [Google Scholar] [CrossRef]
- WHO. Health Systems Resilience Toolkit: A WHO Global Public Health Good to Support Building and Strengthening of Sustainable Health Systems Resilience in Countries with Various Contexts; WHO: Geneva, Switzerland, 2022. [Google Scholar]
- Khorram-Manesh, A.; Ashkenazi, M.; Djalali, A.; Ingrassia, P.L.; Friedl, T.; von Armin, G.; Lupesco, O.; Kaptan, K.; Arculeo, C.; Hreckovski, B.; et al. Education in Disaster Management and Emergencies: Defining a New European Course. Disaster Med. Public Health Prep. 2015, 9, 245–255. [Google Scholar] [CrossRef]
- Baker Rogers, J.E. Hospices and Emergency Preparedness Planning: A Scoping Review of the Literature. J. Palliat. Care 2023. [Google Scholar] [CrossRef]
| Disasters | Group | Type (Examples) |
|---|---|---|
| Disasters triggered by natural hazards * | Biological | Pandemic, epidemic, insect infestation, animal stampede |
| Geophysical | Earthquake, volcano, mass movement | |
| Meteorological | Storm | |
| Hydrological | Flood, mass movement | |
| Climatological | Extreme temperature, drought, wildfire | |
| Man-made disasters | Warfare | National conflicts, international conflicts |
| Socio-technical disaster | Technological disasters (e.g., leakage, toxic release, structure collapse), transportations disasters, production failure, public places failures |
| Main Themes | Sub-Themes |
|---|---|
| Disruption of the system | Underutilization and shift from hospitals to home services
|
Disruption of social connectedness
| |
Dehumanization of care
| |
Lack of resources
| |
Lack of information and expertise
| |
| Setting-specific differences | Hospitals and nursing homes
|
Home and community care
| |
Cultural, organizational, and funding differences in disaster response
| |
| Emotional challenges | Increased emotional demands under disaster pressure for
|
| System adaption | Implementation of low-cost and ad hoc solutions especially at micro and meso levels
|
| System preparedness | Lack of PC-specific disaster management
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Plagg, B.; Ballmann, J.; Ewers, M. Hospice and Palliative Care during Disasters: A Systematic Review. Healthcare 2023, 11, 2382. https://doi.org/10.3390/healthcare11172382
Plagg B, Ballmann J, Ewers M. Hospice and Palliative Care during Disasters: A Systematic Review. Healthcare. 2023; 11(17):2382. https://doi.org/10.3390/healthcare11172382
Chicago/Turabian StylePlagg, Barbara, Julia Ballmann, and Michael Ewers. 2023. "Hospice and Palliative Care during Disasters: A Systematic Review" Healthcare 11, no. 17: 2382. https://doi.org/10.3390/healthcare11172382
APA StylePlagg, B., Ballmann, J., & Ewers, M. (2023). Hospice and Palliative Care during Disasters: A Systematic Review. Healthcare, 11(17), 2382. https://doi.org/10.3390/healthcare11172382







