The Quiet Epidemic: An Overview of Emerging Qualitative Research Trends on Sedentary Behavior in Aging Populations
Abstract
1. Breaking Ground on Sedentary Behavior: An Introduction to a Silent Threat
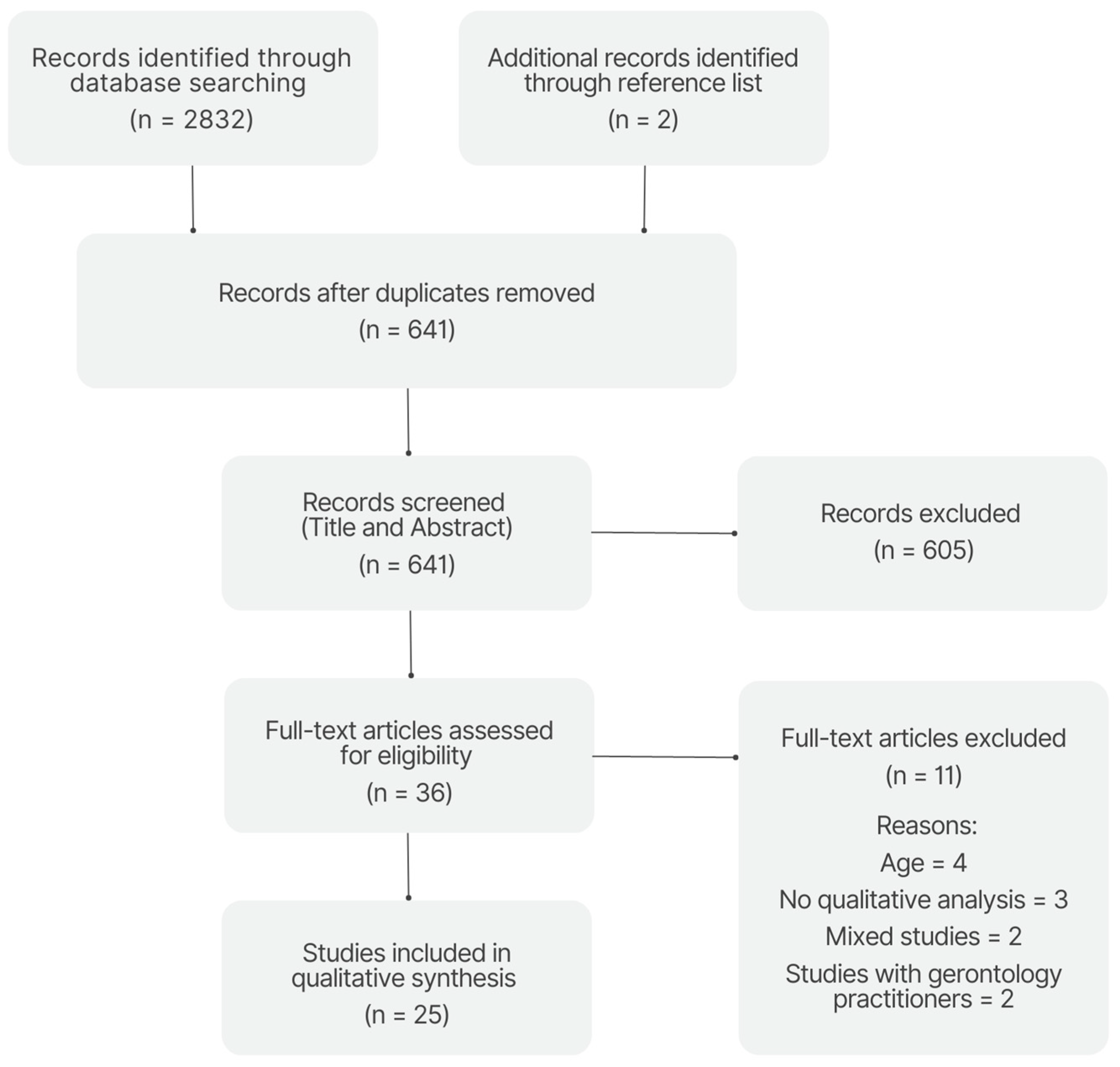
2. Crafting the Map: Eligibility Criteria, Search Strategy, Study Selection, Data Extraction and Analysis
3. From Palette to Canvas: Study Characteristics
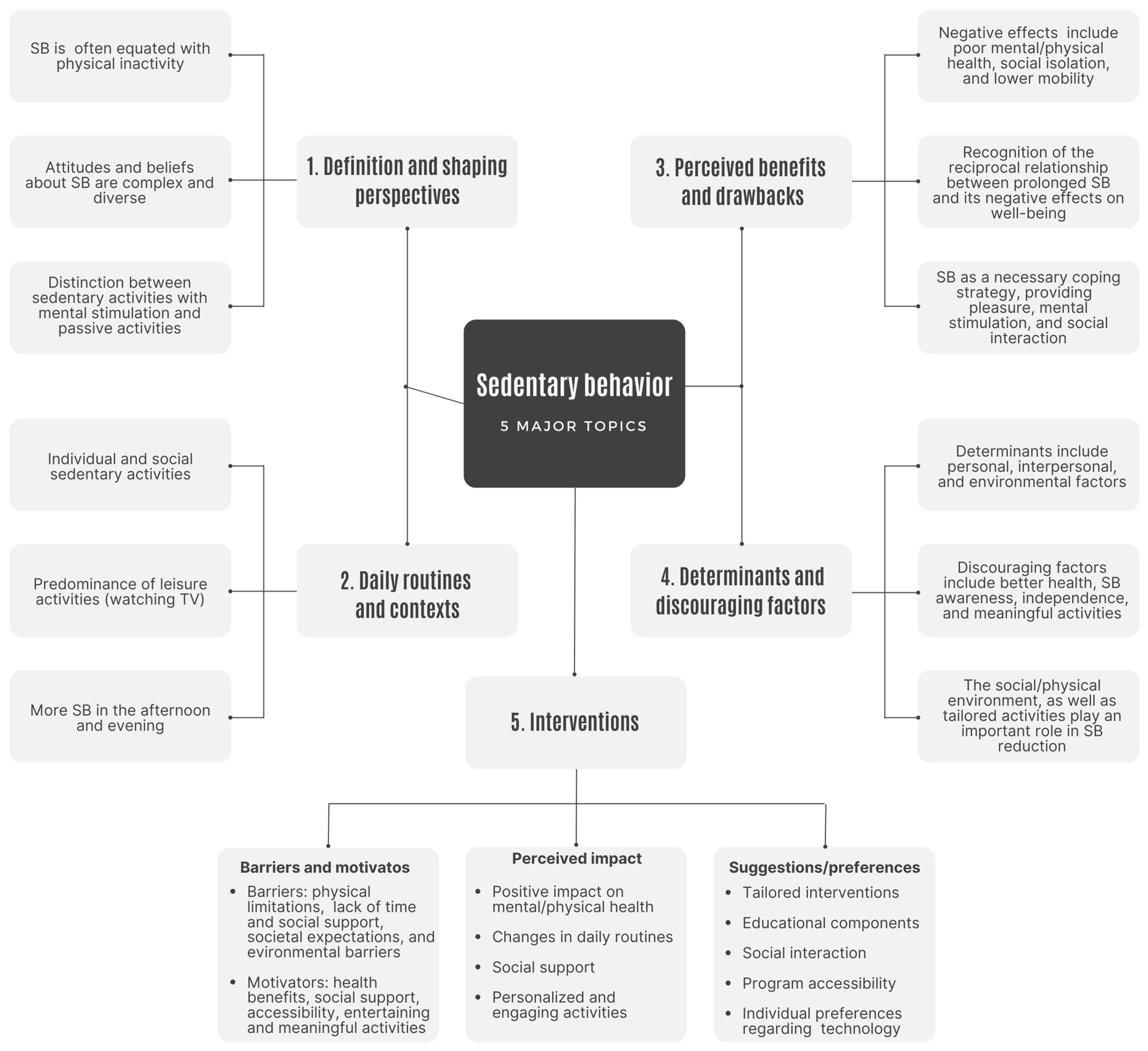
4. Cracking the Code of Sedentary Behavior: Key Themes Explored and Discussed
4.1. Definition and Shaping Perspectives on Sedentary Behavior
4.2. Sedentary Behavior Awareness: Daily Routines and Contexts
4.3. The Dual Nature of Sedentary Behavior: Perceived Benefits and Drawbacks
4.4. Delving into Sedentary Behavior: Determinants and Discouraging Factors
4.4.1. Determinants
4.4.2. Discouraging Factors
4.5. Breaking the Sedentary Spell: Interventions
4.5.1. Barriers and Facilitators to Participating in Sedentary Behavior Interventions
4.5.2. Impacts of Sedentary Behavior Interventions
4.5.3. Interests and Preferences for a Sedentary Behavior Intervention
5. Insights from Qualitative Research on Sedentary Behavior: A Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Diaz, K.M.; Howard, V.J.; Hutto, B.; Colabianchi, N.; Vena, J.E.; Safford, M.M.; Blair, S.N.; Hooker, S.P. Patterns of Sedentary Behavior and Mortality in U.S. Middle-Aged and Older Adults: A National Cohort Study. Ann. Intern. Med. 2017, 167, 465–475. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Lee, E. The Association Between Elderly People’s Sedentary Behaviors and Their Health-Related Quality of Life: Focusing on Comparing the Young-Old and the Old-Old. Health Qual. Life Outcomes 2019, 17, 131. [Google Scholar] [CrossRef] [PubMed]
- Matthews, C.E. Minimizing Risk Associated with Sedentary Behavior: Should We Focus on Physical Activity, Sitting, or Both? J. Am. Coll. Cardiol. 2019, 73, 2073–2075. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, M.S.; Aubert, S.; Barnes, J.D.; Saunders, T.J.; Carson, V.; Latimer-Cheung, A.; Chastin, S.; Altenburg, T.M.; Chinapaw, M.J.M. Sedentary Behavior Research Network (SBRN)—Terminology Consensus Project process and outcome. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 75. [Google Scholar] [CrossRef]
- Owen, N.; Healy, G.N.; Dempsey, P.C.; Salmon, J.; Timperio, A.; Clark, B.K.; Goode, A.D.; Koorts, H.; Ridgers, N.D.; Hadgraft, N.T.; et al. Sedentary Behavior and Public Health: Integrating the Evidence and Identifying Potential Solutions. Ann. Rev. Public Health 2020, 41, 265–287. [Google Scholar] [CrossRef]
- Katzmarzyk, P.T.; Church, T.S.; Craig, C.L.; Bouchard, C. Sitting Time and Mortality from All Causes, Cardiovascular Disease, and Cancer. Med. Sci. Sports Exerc. 2009, 41, 998–1005. [Google Scholar] [CrossRef]
- Thorp, A.A.; Owen, N.; Neuhaus, M.; Dunstan, D.W. Sedentary Behaviors and Subsequent Health Outcomes in Adults: A Systematic Review of Longitudinal Studies, 1996-2011. Am. J. Prev. Med. 2011, 41, 207–215. [Google Scholar] [CrossRef]
- Wilmot, E.G.; Edwardson, C.L.; Achana, F.A.; Davies, M.J.; Gorely, T.; Gray, L.J.; Khunti, K.; Yates, T.; Biddle, S.J. Sedentary Time in Adults and the Association with Diabetes, Cardiovascular Disease and Death: Systematic Review and Meta-analysis. Diabetologia 2012, 55, 2895–2905. [Google Scholar] [CrossRef]
- McGowan, L.J.; Powell, R.; French, D.P. Older Adults’ Construal of Sedentary Behaviour: Implications for Reducing Sedentary Behaviour in Older Adult Populations. J. Health Psychol. 2021, 26, 2186–2199. [Google Scholar] [CrossRef]
- Hallgren, M.; Owen, N.; Stubbs, B.; Zeebari, Z.; Vancampfort, D.; Schuch, F.; Bellocco, R.; Dunstan, D.; Trolle Lagerros, Y. Passive and Mentally-Active Sedentary Behaviors and Incident Major Depressive Disorder: A 13-Year Cohort Study. J. Affect. Disord. 2018, 241, 579–585. [Google Scholar] [CrossRef]
- Hallgren, M.; Dunstan, D.W.; Owen, N. Passive Versus Mentally Active Sedentary Behaviors and Depression. Exerc. Sport Sci. Rev. 2020, 48, 20–27. [Google Scholar] [CrossRef]
- Hallgren, M.; Nguyen, T.T.; Owen, N.; Stubbs, B.; Vancampfort, D.; Lundin, A.; Dunstan, D.; Bellocco, R.; Lagerros, Y.T. Cross-Sectional and Prospective Relationships of Passive and Mentally Active Sedentary Behaviours and Physical Activity with Depression. Br. J. Psychiatry 2020, 217, 413–419. [Google Scholar] [CrossRef]
- Saunders, T.J.; McIsaac, T.; Douillette, K.; Gaulton, N.; Hunter, S.; Rhodes, R.E.; Prince, S.A.; Carson, V.; Chaput, J.P.; Chastin, S.; et al. Sedentary Behaviour and Health in Adults: An Overview of Systematic Reviews. Appl. Physiol. Nutr. Metab. 2020, 45, S197–S217. [Google Scholar] [CrossRef]
- O’Neill, C.; Dogra, S. Different Types of Sedentary Activities and Their Association with Perceived Health and Wellness Among Middle-Aged and Older Adults: A Cross-Sectional Analysis. Am. J. Health Promot. 2016, 30, 314–322. [Google Scholar] [CrossRef]
- Ramalho, A.; Petrica, J.; Serrano, J.; Paulo, R.; Duarte-Mendes, P.; Rosado, A. Consequences of Sedentary Behavior on Psychosocial Well-Being: A Qualitative Study with Older Adults Residing in Portugal. Retos 2021, 42, 198–211. [Google Scholar] [CrossRef]
- LeBlanc, A.G.; Gunnell, K.E.; Prince, S.A.; Saunders, T.J.; Barnes, J.D.; Chaput, J.P. The Ubiquity of the Screen: An Overview of the Risks and Benefits of Screen Time in Our Modern World. Transl. J. Am. Coll. Sports Med. 2017, 2, 104–113. [Google Scholar]
- Owen, N.; Healy, G.N.; Matthews, C.E.; Dunstan, D.W. Too Much Sitting: The Population Health Science of Sedentary Behaviour. Exerc. Sport Sci. Rev. 2010, 38, 105–113. [Google Scholar] [CrossRef]
- Taylor, W.; Rix, K.; Gibson, A.; Paxton, R. Sedentary Behavior and Health Outcomes in Older Adults: A Systematic Review. AIMS Med. Sci. 2020, 7, 10–39. [Google Scholar] [CrossRef]
- De Rezende, L.F.; Rey-López, J.P.; Matsudo, V.K.; do Carmo Luiz, O. Sedentary Behavior and Health Outcomes Among Older Adults: A Systematic Review. BMC Public Health 2014, 14, 333. [Google Scholar] [CrossRef]
- Ramalho, A.; Petrica, J.; Rosado, A. Sedentary Behaviors and Psychological Outcomes Among Older Adults: A Systematic Review. Motricidade 2018, 14, 73–85. [Google Scholar] [CrossRef]
- Olanrewaju, O.; Stockwell, S.; Stubbs, B.; Smith, L. Sedentary Behaviours, Cognitive Function, and Possible Mechanisms in Older Adults: A Systematic Review. Aging Clin. Exp. Res. 2020, 32, 969–984. [Google Scholar] [CrossRef] [PubMed]
- Harvey, J.A.; Chastin, S.F.; Skelton, D.A. Prevalence of Sedentary Behavior in Older Adults: A Systematic Review. Int. J. Environ. Res. Public Health 2013, 10, 6645–6661. [Google Scholar] [CrossRef] [PubMed]
- Harvey, J.; Chastin, S.; Skelton, D. How Sedentary are Older People? A Systematic Review of the Amount of Sedentary Behaviour. J. Aging Phys. Act. 2015, 23, 471–487. [Google Scholar] [CrossRef] [PubMed]
- Heesch, K.C.; Hill, R.L.; Aguilar-Farias, N.; van Uffelen, J.; Pavey, T. Validity of Objective Methods for Measuring Sedentary Behaviour in Older Adults: A Systematic Review. Int. J. Environ. Res. Public Health 2018, 15, 119. [Google Scholar] [CrossRef]
- Zusman, E.Z.; Dawes, M.G.; Edwards, N.; Ashe, M.C. A Systematic Review of Evidence for Older Adults’ Sedentary Behavior and Physical Activity after Hip Fracture. Clin. Rehabil. 2018, 32, 679–691. [Google Scholar] [CrossRef]
- Chastin, S.F.; Buck, C.; Freiberger, E.; Murphy, M.; Brug, J.; Cardon, G.; O’Donoghue, G.; Pigeot, I.; Oppert, J.M.; DEDIPAC Consortium. Systematic Literature Review of Determinants of Sedentary Behaviour in Older Adults: A DEDIPAC Study. Int. J. Environ. Res. Public Health 2015, 12, 127. [Google Scholar] [CrossRef]
- Compernolle, S.; De Cocker, K.; Cardon, G.; De Bourdeaudhuij, I.; Van Dyck, D. Older Adults’ Perceptions of Sedentary Behavior: A Systematic Review and Thematic Synthesis of Qualitative Studies. Gerontologist 2020, 60, e572–e582. [Google Scholar] [CrossRef]
- Rollo, S.; Gaston, A.; Prapavessis, H. Cognitive and Motivational Factors Associated with Sedentary Behavior: A Systematic Review. AIMS Public Health 2016, 3, 956–984. [Google Scholar] [CrossRef]
- Chase, J.D.; Otmanowski, J.; Rowland, S.; Cooper, P.S. A Systematic Review and Meta-Analysis of Interventions to Reduce Sedentary Behavior among Older Adults. Transl. Behav. Med. 2020, 10, 1078–1085. [Google Scholar] [CrossRef]
- Stockwell, S.; Schofield, P.; Fisher, A.; Firth, J.; Jackson, S.E.; Stubbs, B.; Smith, L. Digital Behavior Change Interventions to Promote Physical Activity and/or Reduce Sedentary Behavior in Older Adults: A Systematic Review and Meta-Analysis. Exp. Gerontol. 2019, 120, 68–87. [Google Scholar] [CrossRef]
- Aunger, J.A.; Doody, P.; Greig, C.A. Interventions Targeting Sedentary Behavior in Non-Working Older Adults: A Systematic Review. Maturitas 2018, 116, 89–99. [Google Scholar] [CrossRef]
- Bishop, D. An Applied Research Model for the Sport Sciences. Sports Med. 2008, 38, 253–263. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.; Ioannidis, J.; Clarke, M.; Devereaux, P.; Kleijnen, J.; Moher, D. The PRISMA Statement for Reporting Systematic Reviews and Meta-Analyses of Studies That Evaluate Health Care Interventions: Explanation and Elaboration. Ann. Intern. Med. 2009, 151, 65–94. [Google Scholar] [CrossRef]
- Munn, Z.; Peters, M.; Stern, C.; Tufanaru, C.; McArthur, A.; Aromataris, E. Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med. Res. Methodol. 2018, 18, 143. [Google Scholar] [CrossRef]
- Cooke, A.; Smith, D.; Booth, A. Beyond PICO: The SPIDER Tool for Qualitative Evidence Synthesis. Qual. Health Res. 2012, 22, 1435–1443. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Using Thematic Analysis in Psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Biswas, A.; Faulkner, G.E.; Oh, P.I.; Alter, D.A. Patient and Practitioner Perspectives on Reducing Sedentary Behavior at an Exercise-Based Cardiac Rehabilitation Program. Disabil. Rehabil. 2018, 40, 2267–2274. [Google Scholar] [CrossRef] [PubMed]
- Brookfield, K.; Fitzsimons, C.; Scott, I.; Mead, G.; Starr, J.; Thin, N.; Ward Thompson, C. The Home as Enabler of More Active Lifestyles Among Older People. Build Res. Inf. 2015, 43, 616–630. [Google Scholar] [CrossRef]
- Chastin, S.F.; Fitzpatrick, N.; Andrews, M.; DiCroce, N. Determinants of Sedentary Behavior, Motivation, Barriers and Strategies to Reduce Sitting Time in Older Women: A Qualitative Investigation. Int. J. Environ. Res. Public Health 2014, 11, 773–791. [Google Scholar] [CrossRef]
- Collins, L.; Pope, J.P. Why I Get Up Off My Butt: Older Adults’ Motives to Limit Their Sedentary Behavior. J. Aging Phys. Act. 2021, 29, 984–992. [Google Scholar] [CrossRef] [PubMed]
- Eklund, C.; Elfström, M.L.; von Heideken Wågert, P.; Söderlund, A.; Gustavsson, C.; Cederbom, S.; Thunborg, C.; Lööf, H. The Meaning of Sedentary Behavior as Experienced by People in the Transition From Working Life to Retirement: An Empirical Phenomenological Study. Phys. Ther. 2021, 101, pzab117. [Google Scholar] [CrossRef]
- Gour, P.; Choudhary, A.; Sahoo, K.C.; Jirwe, M.; Hallgren, M.; Diwan, V.K.; Mahadik, V.K.; Diwan, V. Experience of Elderly People Regarding the Effect of Yoga/Light Exercise on Sedentary Behavior: A Longitudinal Qualitative Study in Madhya Pradesh, India. Geriatrics 2020, 5, 103. [Google Scholar] [CrossRef]
- Greenwood-Hickman, M.A.; Renz, A.; Rosenberg, D.E. Motivators and Barriers to Reducing Sedentary Behavior among Overweight and Obese Older Adults. Gerontologist 2016, 56, 660–668. [Google Scholar] [CrossRef]
- Kotlarczyk, M.P.; Hergenroeder, A.L.; Gibbs, B.B.; Cameron, F.A.; Hamm, M.E.; Brach, J.S. Personal and Environmental Contributors to Sedentary Behavior of Older Adults in Independent and Assisted Living Facilities. Int. J. Environ. Res. Public Health 2020, 17, 6415. [Google Scholar] [CrossRef]
- Leask, C.F.; Sandlund, M.; Skelton, D.A.; Tulle, E.; Chastin, S.F. Modifying Older Adults’ Daily Sedentary Behaviour Using an Asset-based Solution: Views from Older Adults. AIMS Public Health 2016, 3, 542–554. [Google Scholar] [CrossRef]
- Leask, C.F.; Sandlund, M.; Skelton, D.A.; Chastin, S.F. Co-creating a Tailored Public Health Intervention to Reduce Older Adults’ Sedentary Behaviour. Health Educ. J. 2017, 76, 595–608. [Google Scholar] [CrossRef]
- Matson, T.E.; Renz, A.D.; Takemoto, M.L.; McClure, J.B.; Rosenberg, D.E. Acceptability of a Sitting Reduction Intervention for Older Adults With Obesity. BMC Public Health 2018, 18, 706. [Google Scholar] [CrossRef]
- McCain, J.E.; Caissie, L.; Edwards, J.; Handrigan, G.; McGibbon, C.; Hebert, J.; Gallibois, M.; Cooling, K.M.; Read, E.; Sénéchal, M.; et al. Long-Term Care Residents’ Acceptance of a Standing Intervention: A Qualitative Intrinsic Case Study. Geriatr. Nurs. 2023, 50, 94–101. [Google Scholar] [CrossRef]
- McEwan, T.; Tam-Seto, L.; Dogra, S. Perceptions of Sedentary Behavior Among Socially Engaged Older Adults. Gerontologist 2017, 57, 735–744. [Google Scholar] [CrossRef]
- McGowan, L.J.; Powell, R.; French, D.P. How Acceptable is Reducing Sedentary Behavior to Older Adults? Perceptions and Experiences Across Diverse Socioeconomic Areas. J. Aging Phys. Act. 2019, 27, 642–652. [Google Scholar] [CrossRef]
- Moraes, S.A.; Furlanetto, E.C.; Ricci, N.A.; Perracini, M.R. Sedentary Behavior: Barriers and Facilitators among Older Adults after Hip Fracture Surgery. A Qualitative Study. Braz. J. Phys. Ther. 2020, 24, 407–414. [Google Scholar] [CrossRef]
- Nuwere, E.; Barone Gibbs, B.; Toto, P.E.; Taverno Ross, S.E. Planning for a Healthy Aging Program to Reduce Sedentary Behavior: Perceptions among Diverse Older Adults. Int. J. Environ. Res. Public Health 2022, 19, 6068. [Google Scholar] [CrossRef] [PubMed]
- Palmer, V.J.; Gray, C.M.; Fitzsimons, C.F.; Mutrie, N.; Wyke, S.; Deary, I.J.; Der, G.; Chastin, S.F.M.; Skelton, D.A.; Seniors USP Team. What Do Older People Do When Sitting and Why? Implications for Decreasing Sedentary Behavior. Gerontologist 2019, 59, 686–697. [Google Scholar] [CrossRef] [PubMed]
- Palmer, V.J.; Gray, C.M.; Fitzsimons, C.; Mutrie, N.; Wyke, S.; Der, G.; Chastin, S.F.M.; Skelton, D.A. Sitting as a Moral Practice: Older Adults’ Accounts from Qualitative Interviews on Sedentary Behaviours. Sociol. Health Illn. 2021, 43, 2102–2120. [Google Scholar] [CrossRef] [PubMed]
- Tam-Seto, L.; Weir, P.; Dogra, S. Factors Influencing Sedentary Behaviour in Older Adults: An Ecological Approach. AIMS Public Health 2016, 3, 555–572. [Google Scholar] [CrossRef] [PubMed]
- Trinh, L.; Arbour-Nicitopoulos, K.P.; Sabiston, C.M.; Alibhai, S.M.; Jones, J.M.; Berry, S.R.; Loblaw, A.; Faulkner, G.E. A Qualitative Study Exploring the Perceptions of Sedentary Behavior in Prostate Cancer Survivors Receiving Androgen-Deprivation Therapy. Oncol. Nurs. Forum 2015, 42, 398–406. [Google Scholar] [CrossRef]
- Van Dyck, D.; Mertens, L.; Cardon, G.; De Cocker, K.; De Bourdeaudhuij, I. Opinions Toward Physical Activity, Sedentary Behavior, and Interventions to Stimulate Active Living During Early Retirement: A Qualitative Study in Recently Retired Adults. J. Aging Phys. Act. 2017, 25, 277–286. [Google Scholar] [CrossRef]
- Voss, M.L.; Pope, J.P.; Copeland, J.L. Reducing Sedentary Time among Older Adults in Assisted Living: Perceptions, Barriers, and Motivators. Int. J. Environ. Res. Public Health 2020, 17, 717. [Google Scholar] [CrossRef]
- Webber, S.C.; Ripat, J.D.; Pachu, N.S.; Strachan, S.M. Exploring Physical Activity and Sedentary Behaviour: Perspectives of Individuals with Osteoarthritis and Knee Arthroplasty. Disabil. Rehabil. 2020, 42, 1971–1978. [Google Scholar] [CrossRef]
- Webster, K.E.; Seng, J.S.; Gallagher, N.A.; Gothe, N.P.; Colabianchi, N.; Smith, E.M.L.; Ploutz-Snyder, R.; Larson, J.L. Physical Activity Programming for Older Adults in Assisted Living: Residents’ Perspectives. West J. Nurs. Res. 2023, 45, 105–116. [Google Scholar] [CrossRef]
- Sedentary Behavior Research Network. Letter to the Editor: Standardized Use of the Terms “Sedentary” and “Sedentary Behaviours”. Appl. Physiol. Nutr. Metab. 2012, 37, 540–542. [Google Scholar] [CrossRef]
- Haslam, S.A.; Jetten, J.; Postmes, T.; Haslam, C. Social Identity, Health and Well-Being: An Emerging Agenda for Applied Psychology. Appl. Psychol. Int. Rev. 2009, 58, 1–23. [Google Scholar] [CrossRef]
- Weiss, D.; Sassenberg, K.; Freund, A.M. When Feeling Different Pays Off: How Older Adults Can Counteract Negative Age-Related Information. Psychol. Aging 2013, 28, 1140–1146. [Google Scholar] [CrossRef]
- Wurm, S.; Tesch-Römer, C.; Tomasik, M.J. Longitudinal Findings on Aging-Related Cognitions, Control Beliefs, and Health in Later Life. J. Gerontol. B Psychol. Sci. Soc. Sci. 2007, 62, P156–P164. [Google Scholar] [CrossRef]
- Thompson, L.; Kumar, A. Responses to Health Promotion Campaigns: Resistance, Denial and Othering. Crit. Public Health 2011, 21, 105–117. [Google Scholar] [CrossRef]
- Tulle, E. Physical Activity and Sedentary Behaviour: A Vital Politics of Old Age? In Physical Activity and Sport in Later Life; Tulle, E., Phoenix, C., Eds.; Springer: Cham, Switzerland, 2015; pp. 9–20. [Google Scholar]
- Greenberg, J.; Arndt, J. Terror Management Theory. In Handbook of Theories of Social Psychology; Van Lange, P.A.M., Kruglanski, A.W., Higgins, E.T., Eds.; Sage Publications Ltd.: London, UK, 2012; pp. 398–415. [Google Scholar]
- Hamer, M.; Stamatakis, E. Prospective Study of Sedentary Behavior, Risk of Depression, and Cognitive Impairment. Med. Sci. Sports Exerc. 2014, 46, 718–723. [Google Scholar] [CrossRef]
- Huang, Y.; Li, L.; Gan, Y.; Wang, C.; Jiang, H.; Cao, S.; Lu, Z. Sedentary Behaviors and Risk of Depression: A Meta-Analysis of Prospective Studies. Transl. Psychiatry 2020, 10, 26. [Google Scholar] [CrossRef]
- Festinger, L. A Theory of Cognitive Dissonance; Stanford University Press: Stanford, CA, USA, 1957. [Google Scholar]
- Compernolle, S.; DeSmet, A.; Poppe, L.; Crombez, G.; De Bourdeaudhuij, I.; Cardon, G.; Van Dyck, D. Effectiveness of Interventions Using Self-Monitoring to Reduce Sedentary Behavior in Adults: A Systematic Review and Meta-Analysis. Int. J. Behav. Nutr. Phys. Act. 2019, 16, 63. [Google Scholar] [CrossRef]
- Pedišić, Ž.; Dumuid, D.; Olds, T. Integrating Sleep, Sedentary Behaviour, and Physical Activity Research in the Emerging Field of Time-Use Epidemiology: Definitions, Concepts, Statistical Methods, Theoretical Framework, and Future Directions. Kinesiology 2017, 49, 1–18. [Google Scholar]
- Ross, R.; Chaput, J.P.; Giangregorio, L.M.; Janssen, I.; Saunders, T.J.; Kho, M.E.; Tremblay, M.S. Canadian 24-Hour Movement Guidelines for Adults Aged 18–64 Years and Adults aged 65 Years or Older: An Integration of Physical Activity, Sedentary Behaviour, and Sleep. Appl. Physiol. Nutr. Metab. 2020, 45, S57–S102. [Google Scholar] [CrossRef]
- Phoenix, C.; Bell, S.L. Beyond “Move More”: Feeling the Rhythms of Physical Activity in Mid and Later-Life. Soc. Sci. Med. 2018, 231, 47–54. [Google Scholar] [CrossRef] [PubMed]
- Rawlings, G.H.; Williams, R.K.; Clarke, D.J.; English, C.; Fitzsimons, C.; Holloway, I.; Lawton, R.; Mead, G.; Patel, A.; Forster, A. Exploring Adults’ Experiences of Sedentary Behaviour and Participation in Non-workplace Interventions Designed to Reduce Sedentary Behaviour: A Thematic Synthesis of Qualitative Studies. BMC Public Health 2019, 19, 1099. [Google Scholar] [CrossRef]
- Bronfenbrenner, U. The Ecology of Human Development: Experiments by Nature and Design; Harvard University Press: Cambridge, MA, USA, 1979. [Google Scholar]
- Bauman, A.; Reis, R.; Sallis, J.; Wells, J.; Loos, R.; Martin, B. Correlates of Physical Activity: Why Are Some People Physically Active and Others Not? Lancet 2012, 380, 258–271. [Google Scholar] [CrossRef] [PubMed]
- Ottenvall Hammar, I.; Dahlin-Ivanoff, S.; Wilhelmson, K.; Eklund, K. Self-Determination among Community-Dwelling Older Persons: Explanatory Factors. Scand. J. Occup. Ther. 2016, 23, 198–206. [Google Scholar] [CrossRef]
- Barnett, I.; van Sluijs, E.M.F.; Ogilvie, D. Physical Activity and Transitioning to Retirement: A Systematic Review. Am. J. Prev. Med. 2012, 43, 329–336. [Google Scholar] [CrossRef] [PubMed]
- Sebastião, E.; Pak, J.; Benner, J.D.; Nakamura, P.M.; Papini, C.B. Magnitude and Composition of Sedentary Behavior in Older Adults Living in a Retirement Community. J. Community Health 2019, 44, 805–814. [Google Scholar] [CrossRef]
- Kikuchi, H.; Inoue, S.; Fukushima, N.; Takamiya, T.; Odagiri, Y.; Ohya, Y.; Amagasa, S.; Oka, K.; Owen, N. Social Participation Among Older Adults not Engaged in Full- or Part-Time Work is Associated with More Physical Activity and Less Sedentary Time. Geriatr. Gerontol. Int. 2017, 17, 1921–1927. [Google Scholar] [CrossRef]
- Michie, S.; van Stralen, M.M.; West, R. The Behaviour Change Wheel: A New Method for Characterising and Designing Behaviour Change Interventions. Implement. Sci. 2011, 6, 42. [Google Scholar] [CrossRef]
- Deci, E.L.; Ryan, R.M. Intrinsic Motivation and Self-Determination in Human Behavior; Springer Science & Business Media: Berlin, Germany, 1985. [Google Scholar]
- Ryan, R.M.; Deci, E.L. Self-Determination Theory and the Facilitation of Intrinsic Motivation, Social Development, and Well-Being. Am. Psychol. 2000, 55, 68–78. [Google Scholar] [CrossRef]
- Owen, N.; Sugiyama, T.; Eakin, E.E.; Gardiner, P.A.; Tremblay, M.S.; Sallis, J.F. Adults’ Sedentary Behavior Determinants and Interventions. Am. J. Prev. Med. 2011, 41, 189–196. [Google Scholar] [CrossRef]
- Michie, S.; Atkins, L.; West, R. The Behaviour Change Wheel: A Guide to Designing Interventions; Silverback Publishing: London, UK, 2014. [Google Scholar]
- Lewin, S.; Glenton, C. Are we Entering a New Era for Qualitative Research? Using Qualitative Evidence to Support Guidance And Guideline Development by the World Health Organization. Int. J. Equity Health 2018, 17, 126. [Google Scholar] [CrossRef]
- Ramalho, A.; Petrica, J. Knowledge in Motion: A Comprehensive Review of Evidence-Based Human Kinetics. Int. J. Environ. Res. Public Health 2023, 20, 6020. [Google Scholar] [CrossRef]
| 1. Sedentary lifestyle [MeSH Terms] 2. (((sedentary behavior [tiab]) OR sedentary behaviour [tiab]) OR sedentary lifestyle [tiab]) 3. prolonged sitting [tiab] 4. Computer [MeSH Terms] 5. ((computer use [tiab]) OR computer usage [tiab]) OR computer time [tiab] 6. Television [MeSH Terms] 7. ((television viewing [tiab]) OR television watching [tiab]) OR television time [tiab] 8. ((TV viewing [tiab]) OR TV watching [tiab]) OR TV time [tiab] 9. ((screen watching [tiab]) OR screen use [tiab]) OR screen time [tiab] 10. ((screen entertainment [tiab]) OR screen behaviour [tiab]) OR screen behavior [tiab] 11. reading time [tiab] 12. automobile driving [MeSH Terms] 13. transport time [tiab] |
| AND |
| 14. qualitative research [MeSH Terms] 15. ethnography [tiab] 16. phenomenology [tiab] 17. life stories [tiab] 18. grounded theory [tiab] 19. case studies [tiab] 20. focus groups [tiab] 21. descriptive qualitative study [tiab] 22. qualitative investigation [tiab] 23. qualitative analysis [MeSH Terms] 24. thematic analysis [tiab] 25. content analysis [tiab] 26. interpretive phenomenological analysis [tiab] 27. thematic synthesis [tiab] 28. narrative analysis [tiab] 29. interviews [MeSH Terms] 30. in-depth interviews [MeSH Terms] 31. structured interviews [tiab] 32. semi-structured interviews [tiab] 33. unstructured interviews [tiab] 34. ((observation [tiab]) OR participant observation [tiab]) |
| AND |
| 35. aging [MeSH Terms] 36. (senior [tiab]) OR senior citizens [tiab] 37. older adult [tiab] 38. elderly [tiab] 39. older people [tiab] 40. geriatric OR geriatrics |
| Author (Year/Country) | Research Purposes | Study Population | Data Collection | Data Analysis | Major Themes |
|---|---|---|---|---|---|
| Biswas et al. (2018) Canada [37] | To explore the level of awareness among cardiac rehabilitation patients and the staff regarding SB, as well as the perceived facilitators and barriers to reducing SB | Cardiac rehabilitation patients n = 15 (47% male) 63.00 (±10.6) | Semi-structured interview | Thematic analysis | Benefits/Drawbacks Determinants/Discouragers |
| Brookfield et al. (2015) UK [38] | To examine older adults’ experiences of their home environment and its influence on their physical activity and SB | Older adults: healthy volunteers stroke survivors, and people with dementia n = 22 (27% male) | Semi-structured interview and focus group | Inductive thematic analysis | Daily routines/Contexts |
| Chastin et al. (2014) UK [39] | To capture older adults’ perspectives and opinions on the factors that influence their sedentary behavior | Healthy, community-dwelling older women n = 9 (0% male) 79.44 (±7.75) | Semi-structured interview | Framework analysis and inductive thematic analysis | Definition/Perspectives Daily routines/Contexts Benefits/Drawbacks Determinants/Discouragers |
| Collins & Pope (2021) USA [40] | To examine the degree to which older adults internalize their motives for limiting SB, consistent with self-determination theory | Community-dwelling older adults n = 27 | Focus group | Thematic analysis | Determinants/Discouragers |
| Eklund et al. (2021) Sweden [41] | To gain a comprehensive understanding of SB as it relates to the transition from work to retirement, specifically how it is experienced by individuals in retirement | Retired older adults n = 14 (43% male) 70.36 | Semi-structured interview | Empirical phenomenological psychological method | Definition/Perspectives Benefits/Drawbacks Determinants/Discouragers |
| Gour et al. (2020) India [42] | To explore older adults’ views on the usefulness of yoga or light exercise and its effects on well-being and the prevention of SB | Older people who participated in an RCT intervention 66.00 | Focus group based on a semi-structured guide | Inductive content analysis | Interventions |
| Greenwood-Hickman et al. (2016) USA [43] | To examine the motivators, barriers, and effects of SB on a group of overweight and obese older adults | Overweight and obese older adults following a SB reduction intervention n = 24 (33% male) 72.00 | Semi-structured interview | Inductive thematic analysis | Determinants/Discouragers Interventions |
| Kotlarczyk et al. (2020) USA [44] | To examine the factors contributing to SB among residents of both independent and assisted living facilities | Older residents of independent and assisted living facilities n = 44 (30% male) 86.00 | Focus group | Thematic analysis | Definition/Perspectives Benefits/Drawbacks Determinants/Discouragers |
| Leask et al. (2016) UK [45] | To understand older adults’ perspectives and identify critical factors to consider when developing a solution to change daily sedentary patterns | Healthy, community-dwelling older adults n = 15 (27% male) 78.00 | Focus group based on semi-structured interview | Thematic analysis | Interventions |
| Leask et al. (2017) UK [46] | To co-create a tailored public health intervention to reduce SB in older adults | Healthy community-dwelling older adults n = 11 (46% male) 74.00 (±5.5) | Semi-structured workshop | Content analysis | Interventions |
| Matson et al. (2018) USA [47] | To explore older adults’ acceptance of a theory-based and technology-enhanced sitting reduction intervention | Obese, community-dwelling older adults n = 22 (36% male) 69.20 (±4.9) | Semi-structured interview | Inductive and deductive thematic analysis | Interventions |
| McCain et al. (2023) USA [48] | To explore the acceptability of a standing intervention among older adults living in long-term care with the guidance of the Theoretical Framework of Acceptability | Older adults living in long-term care from the intervention trial n = 10 (30% male) age 73 to 102 years | Semi-structured interview | Inductive and deductive thematic framework analysis | Interventions |
| McEwan et al. (2017) Canada [49] | To better understand older adults’ perceptions of SB, its pros and cons, and the barriers associated with reducing sedentary time | Healthy, community-dwelling older adults n = 25 (33% male) 74.00 (±8.5) | Focus group based on a semi-structured interview | Directed content analysis | Definition/Perspectives Benefits/Drawbacks Determinants/Discouragers |
| McGowan et al. (2019) UK [50] | To explore the factors influencing SB in older adults and to evaluate the acceptability of potential strategies to reduce SB | Healthy, community-dwelling older adults n = 22 (36% male) 76.00 | Semi-structured interview | Inductive thematic analysis | Definition/Perspectives Benefits/Drawbacks Determinants/Discouragers |
| McGowan et al. (2021) UK [9] | To examine older adults’ understanding of the concept of SB | Community-dwelling older adults n = 22 77.50 | Semi-structured interview | Inductive thematic analysis | Definition/Perspectives Benefits/Drawbacks Determinants/Discouragers |
| Moraes et al. (2020) Brazil [51] | To understand older adults’ experiences after hip fracture surgery considering barriers and facilitators related to SB | Older adults who had hip fracture surgery n = 11 (27% male) | Semi-structured interview | Inductive thematic analysis | Determinants/Discouragers |
| Nuwere et al. (2022) USA [52] | To understand older adults’ perceptions regarding SB and its influence on healthy aging | Community-dwelling older adults who attended two senior centers n = 46 (11% male) 75.60 (± 7.8) | Focus group based on a semi-structured discussion guide | Thematic analysis | Definition/Perspectives Daily routines/Contexts Benefits/Drawbacks Determinants/Discouragers |
| Palmer et al. (2019) UK [53] | Compare the types, context, and role of sitting activities in the daily lives of older adults who sit more or less than average | Healthy, community-dwelling older adults n = 44 (52% male) 74.60 | Semi-structured interview | Inductive thematic analysis | Definition/Perspectives Daily routines/Contexts Determinants/Discouragers |
| Palmer et al. (2021) UK [54] | To investigate how older adults make sense of their SB | Older adults who participated in a previous project n = 44 (52% male) Not reported | Semi-structured interview | Thematic analysis | Definition/Perspectives Daily routines/Contexts Benefits/Drawbacks Determinants/Discouragers |
| Tam-Seto et al. (2016) Canada [55] | To use data on perceptions of sedentary time and the programs/supports that older adults perceive as important to reducing their sedentary time | Healthy, community-dwelling older adults n = 26 (23% male) 74.00 (±8.5) | Focus group based on semi-structured interview | Directed content analysis | Determinants/Discouragers |
| Trinh et al. (2015) Canada [56] | To describe and understand the perceptions of SB and interests and preferences for a SB intervention in men undergoing androgen deprivation therapy | Male prostate cancer survivors n = 27 (100% male) 73.50 (±8.1) | Focus group interview | Deductive thematic synthesis | Definition/Perspectives Benefits/Drawbacks Interventions |
| Van Dyck et al. (2017) Belgium [57] | To obtain qualitative information on change and the specific multidimensional determinants of physical activity and SB during early retirement, on recently retired adults’ opinions of existing PA programs/interventions, and on their needs and desires for new interventions | Healthy, community-dwelling older adults n = 37 (49% male) 62.90 (±1.9); | Focus group based on semi-structured interview | Inductive and deductive thematic analysis | Definition/Perspectives Daily routines/Contexts Determinants/Discouragers |
| Voss et al. (2020) Canada [58] | To explore perceptions of sedentary time as well as barriers and motivators to reducing SB among older adults | Older adults in assisted living n = 31 (26% male) 83.50 (±6.5) | Semi-structured focus group | Thematic analysis | Definition/Perspectives Benefits/Drawbacks Determinants/Discouragers |
| Webber et al. (2020) Canada [59] | To explore the understanding of physical activity and SB, including barriers and health influences in people with osteoarthritis and knee arthroplasty | Older adults with osteoarthritis and knee arthroplasty n = 22 (36% male) 67.50 (±5.3) (pre-operative) and 67.3 (±7.0) (post-operative) | Focus group interview | Inductive thematic analysis | Definition/Perspectives Benefits/Drawbacks Determinants/Discouragers |
| Webster et al. (2023) USA [60] | To collect older adults’ in assisted living recommendations on a proposed intervention to increase self-efficacy to replace SB with light physical activity | Older adults in assisted living n = 20 (40% male) 83.1 | Interview | Content and thematic analysis | Benefits/Drawbacks Determinants/Discouragers Interventions |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ramalho, A.; Petrica, J. The Quiet Epidemic: An Overview of Emerging Qualitative Research Trends on Sedentary Behavior in Aging Populations. Healthcare 2023, 11, 2215. https://doi.org/10.3390/healthcare11152215
Ramalho A, Petrica J. The Quiet Epidemic: An Overview of Emerging Qualitative Research Trends on Sedentary Behavior in Aging Populations. Healthcare. 2023; 11(15):2215. https://doi.org/10.3390/healthcare11152215
Chicago/Turabian StyleRamalho, André, and João Petrica. 2023. "The Quiet Epidemic: An Overview of Emerging Qualitative Research Trends on Sedentary Behavior in Aging Populations" Healthcare 11, no. 15: 2215. https://doi.org/10.3390/healthcare11152215
APA StyleRamalho, A., & Petrica, J. (2023). The Quiet Epidemic: An Overview of Emerging Qualitative Research Trends on Sedentary Behavior in Aging Populations. Healthcare, 11(15), 2215. https://doi.org/10.3390/healthcare11152215






