How Income Inequality and Race Concentrate Depression in Low-Income Women in the US; 2005–2016
Abstract
:1. Background
2. Aims
3. Methods
3.1. Data and Study Population
3.2. Measures
3.3. Main Independent Variable
3.4. Covariate
3.5. Analytic Strategy
4. Results
4.1. Descriptive Analysis Results
4.2. Depressive Symptoms and PIR Categories
4.3. Association between Poverty Income Ratio Levels and Depressive Symptoms in NBRG
4.4. Association between Depressive Symptoms and Race/Ethnicity
4.5. Association between Poverty Income Ratio Levels and Probablity of Being Depressed
4.6. Depressive Symptoms and Income Inequality
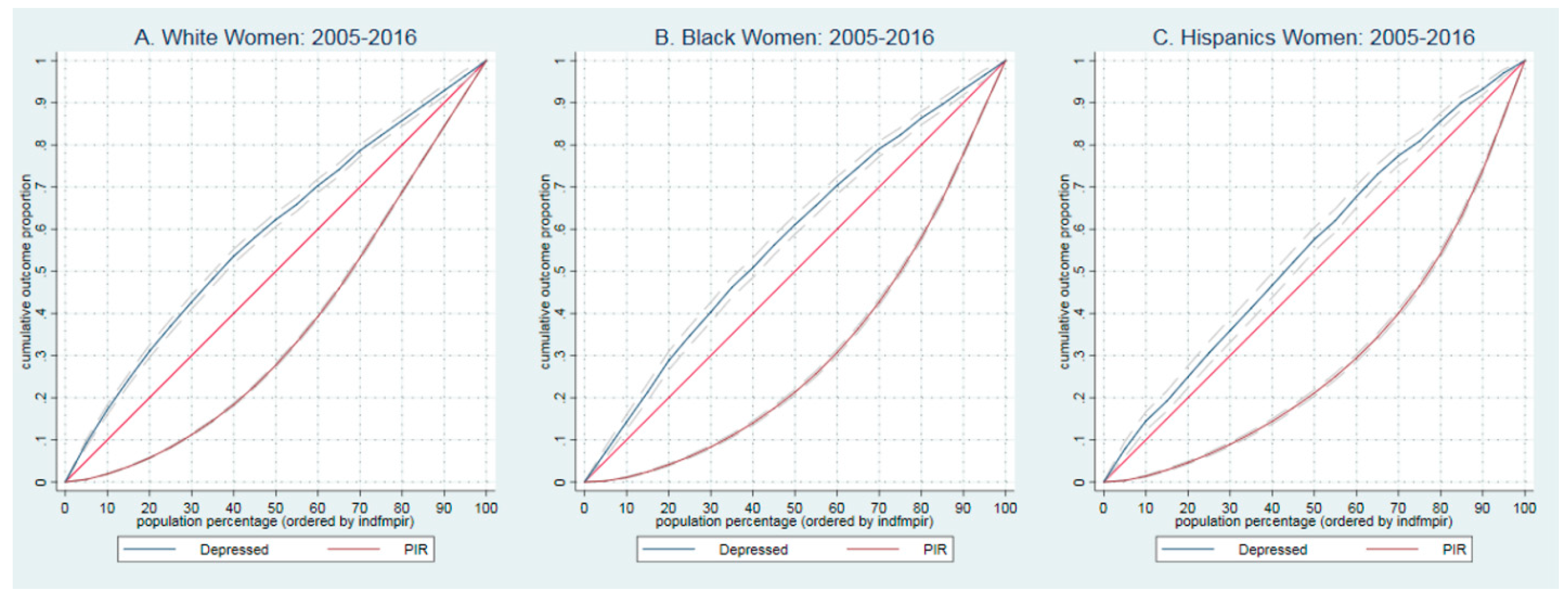
4.7. Concentration of Depressive Symptoms among Poor and Rich Population
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Year | PIR-Categories | All Women | Race and Ethnicity | ||
|---|---|---|---|---|---|
| WNH | BNH | Hispanics | |||
| 2005–2006 | Low-PIR | 13.6% | 18.7% | 10.9% | 8.9% |
| 2007–2008 | 19.0% | 27.5% | 17.7% | 17.3% | |
| 2009–2010 | 21.0% | 19.5% | 24.3% | 21.1% | |
| 2011–2012 | 18.2% | 20.5% | 17.1% | 20.5% | |
| 2013–2014 | 17.2% | 21.1% | 18.4% | 17.1% | |
| 2015–2016 | 18.0% | 27.3% | 15.6% | 14.9% | |
| 2005–2006 | Medium-PIR | 10.0% | 7.6% | 10.4% | 8.2% |
| 2007–2008 | 11.8% | 11.1% | 11.9% | 15.7% | |
| 2009–2010 | 9.7% | 10.5% | 10.6% | 11.8% | |
| 2011–2012 | 12.1% | 13.5% | 11.5% | 16.7% | |
| 2013–2014 | 12.3% | 16.3% | 12.1% | 12.8% | |
| 2015–2016 | 8.1% | 12.4% | 7.3% | 9.2% | |
| 2005–2006 | High-PIR | 3.4% | 2.6% | 7.3% | 3.8% |
| 2007–2008 | 4.8% | 5.2% | 6.5% | 7.4% | |
| 2009–2010 | 7.0% | 5.0% | 9.0% | 9.1% | |
| 2011–2012 | 4.5% | 3.8% | 5.8% | 5.8% | |
| 2013–2014 | 5.7% | 6.1% | 6.1% | 5.8% | |
| 2015–2016 | 4.9% | 4.6% | 3.4% | 6.4% | |
References
- Clarke, T.; Schiller, J.; Boersma, P. Early Release of Selected Estimates Based on Data from the 2019 National Health Interview Survey; Division of Health Interview Statistics, National Center for Health Statistics, Centers for Disease Control and Prevention, Hyattsville, Maryland, USA: 2020. Available online: https://www.cdc.gov/nchs/data/nhis/earlyrelease/EarlyRelease202009-508.pdf (accessed on 9 June 2022).
- Greenberg, P.E.; Fournier, A.A.; Sisitsky, T.; Simes, M.; Berman, R.; Koenigsberg, S.H.; Kessler, R.C. The Economic Burden of Adults with Major Depressive Disorder in the United States (2010 and 2018). Pharm. Econ. 2021, 39, 653–665. [Google Scholar] [CrossRef]
- O’Neill, A. Gross Domestic Product (GDP) of the United States at Current Prices from 1986 to 2026. 2021. Available online: https://www.statista.com/statistics/263591/gross-domestic-product-gdp-of-the-united-states/ (accessed on 9 June 2022).
- Substance Abuse and Mental Health Services Administration. Key Substance Use and Mental Health Indicators in the United States: Results from the 2019 National Survey on Drug Use and Health; Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration: Rockville, MD, USA, 2020. Available online: https://www.samhsa.gov/data/sites/default/files/reports/rpt29393/2019NSDUHFFRPDFWHTML/2019NSDUHFFR1PDFW090120.pdf (accessed on 9 June 2022).
- Voelker, J.; Kuvadia, H.; Cai, Q.; Wang, K.; Daly, E.; Pesa, J.; Wilkinson, S.T. United States national trends in prevalence of major depressive episode and co-occurring suicidal ideation and treatment resistance among adults. J. Affect. Disord. Rep. 2021, 5, 100172. [Google Scholar] [CrossRef]
- Steffen, A.; Nübel, J.; Jacobi, F.; Bätzing, J.; Holstiege, J. Mental and somatic comorbidity of depression: A comprehensive cross-sectional analysis of 202 diagnosis groups using German nationwide ambulatory claims data. BMC Psychiatry 2020, 20, 142. [Google Scholar] [CrossRef] [Green Version]
- Ge, X.; Conger, R.D.; Elder, G.H., Jr. Pubertal transition, stressful life events, and the emergence of gender differences in adolescent depressive symptoms. Dev. Psychol. 2001, 37, 404–417. [Google Scholar] [CrossRef]
- Kuehner, C. Why is depression more common among women than among men? Lancet Psychiatry 2017, 4, 146–158. [Google Scholar] [CrossRef]
- Villarroel, M.; Terlizzi, E. Symptoms of Depression among Adults: United States, 2019; National Center for Health Statistics: Hyattsville, MD, USA, 2020. [Google Scholar]
- Fins, A. National Snapshot: Poverty among Women & Families, 2020; National Women’s Law Center: Washington, DC, USA, 2020. [Google Scholar]
- Barroso, A.; Brown, A. Gender Pay Gap in US Held Steady in 2020; Pew Research Center: Washington, DC, USA, 2021. [Google Scholar]
- Groh, C.J. Poverty, mental health, and women: Implications for psychiatric nurses in primary care settings. J. Am. Psychiatr. Nurses Assoc. 2007, 13, 267–274. [Google Scholar] [CrossRef]
- NCCFCA. National Center on Caregiving at Family Caregiver Alliance. Women and Caregiving: Facts and Figures. 2015. Available online: https://www.caregiver.org/resource/women-and-caregiving-facts-and-figures/ (accessed on 9 June 2022).
- Borah, M.; Knabe, A.; Pahlke, K. Parental time restrictions and the cost of children: Insights from a survey among mothers. J. Econ. Inequal. 2021, 19, 73–95. [Google Scholar] [CrossRef]
- Kaiser Family Foundation (KFF). Mental Health and Substance Use State Fact Sheets. 2021. Available online: https://www.kff.org/statedata/mental-health-and-substance-use-state-fact-sheets/ (accessed on 9 June 2022).
- Vyas, C.M.; Donneyong, M.; Mischoulon, D.; Chang, G.; Gibson, H.; Cook, N.R.; Manson, J.E.; Reynolds, C.F.; Okereke, O.I. Association of race and ethnicity with late-life depression severity, symptom burden, and care. JAMA Netw. Open. 2020, 3, e201606. [Google Scholar] [CrossRef]
- Simpson, S.M.; Krishnan, L.L.; Kunik, M.E.; Ruiz, P. Racial disparities in diagnosis and treatment of depression: A literature review. Psychiatr. Q. 2007, 78, 3–14. [Google Scholar] [CrossRef]
- Noroña-Zhou, A.; Aran, Ö.; Garcia, S.E.; Haraden, D.; Perzow, S.E.; Demers, C.H.; Hennessey, E.M.P.; Donis, S.M.; Kurtz, M.; Hankin, B.L.; et al. Experiences of Discrimination and Depression Trajectories over Pregnancy. Women’s Health Issues 2022, 32, 147–155. [Google Scholar] [CrossRef]
- Wassertheil-Smoller, S.; Arredondo, E.M.; Cai, J.; Castaneda, S.F.; Choca, J.P.; Gallo, L.C.; Jung, M.; LaVange, L.M.; Lee-Rey, E.T.; Mosley, T., Jr.; et al. Depression, anxiety, antidepressant use, and cardiovascular disease among Hispanic men and women of different national backgrounds: Results from the Hispanic Community Health Study/Study of Latinos. Ann. Epidemiol. 2014, 24, 822–830. [Google Scholar] [CrossRef] [Green Version]
- Kim, H.J.; Park, E.; Storr, C.L.; Tran, K.; Juon, H.-S. Depression among Asian-American adults in the community: Systematic review and meta-analysis. PLoS ONE 2015, 10, e0127760. [Google Scholar] [CrossRef] [Green Version]
- McGuire, T.G.; Miranda, J. New evidence regarding racial and ethnic disparities in mental health: Policy implications. Health Aff. 2008, 27, 393–403. [Google Scholar] [CrossRef] [Green Version]
- Haithcoat, T.L.; Avery, E.E.; Bowers, K.A.; Hammer, R.D.; Shyu, C.-R. Income inequality and health: Expanding our understanding of state-level effects by using a geospatial big data approach. Soc. Sci. Comput. Rev. 2021, 39, 543–561. [Google Scholar] [CrossRef]
- Lovasi, G.S.; Schwartz-Soicher, O.; Quinn, J.W.; Berger, D.K.; Neckerman, K.M.; Jaslow, R.; Lee, K.K.; Rundle, A. Neighborhood safety and green space as predictors of obesity among preschool children from low-income families in New York City. Prev. Med. 2013, 57, 189–193. [Google Scholar] [CrossRef] [Green Version]
- Zipf, G.; Chiappa, M.; Porter, K.S.; Ostchega, Y.; Lewis, B.G.; Dostal, J. National Health and Nutrition Examination Survey: Plan and Operations, 1999–2010. National Center for Health Statistics. Vital Health Statistics. 2013. Available online: https://www.cdc.gov/nchs/data/series/sr_01/sr01_056.pdf (accessed on 9 June 2022).
- NHANES. Analytic Guidelines, 2011–2014 and 2015–2016 (14 December 2018). National Health and Nutrition Examination Survey. 2018. Available online: https://wwwn.cdc.gov/nchs/data/nhanes/2011-2012/analyticguidelines/analytic_guidelines_11_16.pdf (accessed on 9 June 2022).
- Ettman, C.K.; Abdalla, S.M.; Cohen, G.H.; Sampson, L.; Vivier, P.M.; Galea, S. Prevalence of depression symptoms in US adults before and during the COVID-19 pandemic. JAMA Netw. Open. 2020, 3, e2019686. [Google Scholar] [CrossRef]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Census; United States Census Bureau. Poverty Thresholds (Last Revised: 9 August 2021). Available online: https://www.census.gov/data/tables/time-series/demo/income-poverty/historical-poverty-thresholds.html (accessed on 9 June 2022).
- UCLA. How Can I Analyze Count Data in Stata? Advanced Research Computing Satistical Methods and Data Analytics. 2021. Available online: https://stats.oarc.ucla.edu/stata/faq/how-can-i-analyze-count-data-in-stata/ (accessed on 9 June 2022).
- STATA. STATA. Stata.com. 2018. Negative Binomial Regression Model. 30 July 2018. Available online: https://www.stata.com/manuals13/rnbreg.pdf (accessed on 9 June 2022).
- Thorpe, R.J., Jr.; Parker, L.J.; Cobb, R.J.; Dillard, F.; Bowie, J. Association between discrimination and obesity in African-American men. Biodemography Soc. Biol. 2017, 63, 253–261. [Google Scholar] [CrossRef]
- McNutt, L.-A.; Wu, C.; Xue, X.; Hafner, J.P. Estimating the relative risk in cohort studies and clinical trials of common outcomes. Am. J. Epidemiol. 2003, 157, 940–943. [Google Scholar] [CrossRef]
- Haughton, J.; Khandker, S.R. Handbook on Poverty+ Inequality; World Bank Publications: Washington, DC, USA, 2009. [Google Scholar]
- Jann, B. Estimating Lorenz and concentration curves. Stata J. 2016, 16, 837–866. [Google Scholar] [CrossRef] [Green Version]
- Vilda, D.; Wallace, M.; Dyer, L.; Harville, E.; Theall, K. Income inequality and racial disparities in pregnancy-related mortality in the US. SSM-Popul. Health 2019, 9, 100477. [Google Scholar] [CrossRef]
- Han, L.; Zhan, Y.; Li, W.; Xu, Y.; Xu, Y.; Zhao, J. Associations Between the Perceived Severity of the COVID-19 Pandemic, Cyberchondria, Depression, Anxiety, Stress, and Lockdown Experience: Cross-sectional Survey Study. JMIR Public Health Surveill. 2021, 7, e31052. [Google Scholar] [CrossRef]
- Cooksey-Stowers, K.; Schwartz, M.B.; Brownell, K.D. Food swamps predict obesity rates better than food deserts in the United States. Int. J. Environ. Res. Public Health 2017, 14, 1366. [Google Scholar] [CrossRef] [Green Version]
- Christafore, D.; Leguizamon, S. Neighbourhood inequality spillover effects of gentrification. Pap. Reg. Sci. 2019, 98, 1469–1484. [Google Scholar] [CrossRef]
- Chen, Z.; Crawford, C.A.G. The role of geographic scale in testing the income inequality hypothesis as an explanation of health disparities. Soc. Sci. Med. 2012, 75, 1022–1031. [Google Scholar] [CrossRef]
- Assari, S.; Lankarani, M.M.; Caldwell, C.H. Does discrimination explain high risk of depression among high-income African American men? Behav. Sci. 2018, 8, 40. [Google Scholar] [CrossRef] [Green Version]
- Deaton, A. Inevitable Inequality? American Association for the Advancement of Science: Washington, DC, USA, 2014. [Google Scholar]
- Deaton, A.; Lubotsky, D. Mortality, inequality and race in American cities and states. Soc. Sci. Med. 2003, 56, 1139–1153. [Google Scholar] [CrossRef] [Green Version]
- Akinyemiju, T.; Jha, M.; Moore, J.X.; Pisu, M. Disparities in the prevalence of comorbidities among US adults by state Medicaid expansion status. Prev. Med. 2016, 88, 196–202. [Google Scholar] [CrossRef] [Green Version]
- Busch, F. Gender segregation, occupational sorting, and growth of wage disparities between women. Demography 2020, 57, 1063–1088. [Google Scholar] [CrossRef]
- Steege, A.L.; Baron, S.L.; Marsh, S.M.; Menéndez, C.C.; Myers, J.R. Examining occupational health and safety disparities using national data: A cause for continuing concern. Am. J. Ind. Med. 2014, 57, 527–538. [Google Scholar] [CrossRef] [Green Version]
- Khullar, D.; Chokshi, D.A. Health, income, & poverty: Where we are & what could help. Health Aff. 2018. Available online: https://www.healthaffairs.org/do/10.1377/hpb20180817.901935/ (accessed on 9 June 2022).
- Levecque, K.; Lodewyckx, I.; Vranken, J. Depression and generalised anxiety in the general population in Belgium: A comparison between native and immigrant groups. J. Affect. Disord. 2007, 97, 229–239. [Google Scholar] [CrossRef]
- Patel, V.; Burns, J.K.; Dhingra, M.; Tarver, L.; Kohrt, B.A.; Lund, C. Income inequality and depression: A systematic review and meta-analysis of the association and a scoping review of mechanisms. World Psychiatry 2018, 17, 76–89. [Google Scholar] [CrossRef]
- Steptoe, A.; Tsuda, A.; Tanaka, Y. Depressive symptoms, socio-economic background, sense of control, and cultural factors in university students from 23 countries. Int. J. Behav. Med. 2007, 14, 97–107. [Google Scholar] [CrossRef]

| White NH (n = 5666) | Black NH (n = 2617) | Hispanics (n = 3137) | All (N = 11,420) | |||||
|---|---|---|---|---|---|---|---|---|
| Mean/% | (SD) | Mean/% | (SD) | Mean/% | (SD) | Mean/% | (SD) | |
| Section A: Depressive Symptoms | ||||||||
| PHQ-D Score | 3.36 | (2.87) | 3.90 | (5.59) | 3.84 | (5.80) | 3.48 | (3.70) |
| If PHQ > 10 α | 0.09 | (0.20) | 0.12 | (0.38) | 0.12 | (0.40) | 0.10 | (0.25) |
| PHQ Categories | ||||||||
| Minimal | 0.74 | (0.30) | 0.70 | (0.54) | 0.69 | (0.57) | 0.73 | (0.38) |
| Mild | 0.17 | (0.25) | 0.18 | (0.45) | 0.19 | (0.48) | 0.17 | (0.32) |
| Moderate | 0.06 | (0.16) | 0.07 | (0.30) | 0.07 | (0.32) | 0.06 | (0.20) |
| Moderate-Severe | 0.03 | (0.11) | 0.03 | (0.21) | 0.03 | (0.22) | 0.03 | (0.14) |
| Sever | 0.01 | (0.06) | 0.01 | (0.14) | 0.01 | (0.14) | 0.01 | (0.08) |
| Section B: Income and Socio-demographic | ||||||||
| PIR Categories | ||||||||
| Low PIR (0–1.12) | 0.13 | (0.23) | 0.30 | (0.53) | 0.36 | (0.59) | 0.18 | (0.33) |
| Medium PIR (1.13–2.72) | 0.29 | (0.31) | 0.35 | (0.56) | 0.38 | (0.60) | 0.30 | (0.39) |
| High PIR (2.73–5.00) | 0.59 | (0.34) | 0.35 | (0.55) | 0.26 | (0.54) | 0.52 | (0.43) |
| Socio-demographic | ||||||||
| Age (years) | 50.33 | (11.69) | 46.33 | (18.72) | 42.64 | (18.89) | 48.58 | (14.46) |
| Married | 0.63 | (0.33) | 0.38 | (0.56) | 0.61 | (0.60) | 0.60 | (0.42) |
| Educational attainment | ||||||||
| Less than high school | 0.11 | (0.21) | 0.20 | (0.47) | 0.39 | (0.60) | 0.15 | (0.31) |
| High school graduate/GED | 0.22 | (0.28) | 0.23 | (0.49) | 0.20 | (0.49) | 0.22 | (0.35) |
| Some college or AA degree | 0.35 | (0.32) | 0.37 | (0.56) | 0.28 | (0.55) | 0.34 | (0.40) |
| College graduate or above | 0.32 | (0.32) | 0.20 | (0.47) | 0.13 | (0.41) | 0.29 | (0.39) |
| Race/Ethnicity | ||||||||
| White Non-Hispanic | NA | NA | NA | NA | NA | NA | 0.75 | (0.39) |
| Black Non-Hispanic | NA | NA | NA | NA | NA | NA | 0.12 | (0.27) |
| Hispanics | NA | NA | NA | NA | NA | NA | 0.13 | (0.28) |
| Comorbidity | 1.24 | (0.99) | 1.00 | (1.48) | 0.77 | (1.42) | 1.13 | (1.19) |
| Has any health insurance coverage | 0.90 | (0.21) | 0.82 | (0.45) | 0.63 | (0.59) | 0.85 | (0.30) |
| If respondent speak English professionally | 1.00 | (0.01) | 1.00 | 0.00 | 0.73 | (0.55) | 0.97 | (0.15) |
| See a mental health professional | 0.10 | (0.20) | 0.09 | (0.33) | 0.08 | (0.34) | 0.09 | (0.25) |
| A routine place to go for healthcare | 0.93 | (0.18) | 0.92 | (0.31) | 0.80 | (0.49) | 0.91 | (0.25) |
| Employed | 0.58 | (0.34) | 0.61 | (0.57) | 0.58 | (0.61) | 0.58 | (0.42) |
| Basic Model | 2nd Model | 3rd Model | Stratified Models by Race and Ethnicity | |||
|---|---|---|---|---|---|---|
| n = 11,420 | n = 11,420 | n = 11,420 | White NH n = 5666 | Black NH n = 2617 | Hispanics n = 3137 | |
| IRR [95% CI] | IRR [95% CI] | IRR [95% CI] | IRR [95% CI] | IRR [95% CI] | IRR [95% CI] | |
| PIR Categories (Ref: if PIR < 1.12) | ||||||
| Medium PIR (1.13–2.72) | 0.80 *** | 0.90 ** | 0.88 * | 0.91 | 0.94 | |
| [0.74–0.86] | [0.84–0.97] | [0.80–0.97] | [0.81–1.03] | [0.85–1.04] | ||
| High PIR (2.73–5.00) | NA | 0.59 *** | 0.76 *** | 0.73 *** | 0.83 ** | 0.82 * |
| [0.54–0.63] | [0.70–0.82] | [0.65–0.83] | [0.72–0.95] | [0.70–0.96] | ||
| Age | 1.00 * | 1.00 *** | 0.99 *** | 0.99 *** | 0.98 *** | 1.00 * |
| [1.00–1.00] | [1.00–1.00] | [0.99–0.99] | [0.99–0.99] | [0.98–0.99] | [0.99–1.00] | |
| Married | NA | 0.83 *** | 0.86 *** | 0.85 *** | 0.93 | 0.87 * |
| [0.78–0.88] | [0.81–0.91] | [0.79–0.92] | [0.84–1.03] | [0.78–0.97] | ||
| Education (Ref. Less than high school) | ||||||
| High school graduate/GED or equivalent | NA | 0.85 *** | 0.84 *** | 0.84 * | 0.71 *** | 0.92 |
| [0.77–0.93] | [0.76–0.93] | [0.74–0.97] | [0.62–0.81] | [0.80–1.05] | ||
| Some college or AA degree | NA | 0.82 *** | 0.79 *** | 0.77 *** | 0.74 *** | 0.9 |
| [0.75–0.90] | [0.72–0.86] | [0.68–0.88] | [0.64–0.85] | [0.79–1.01] | ||
| College graduate or above | NA | 0.68 *** | 0.68 *** | 0.66 *** | 0.72 *** | 0.75 ** |
| [0.62–0.74] | [0.61–0.75] | [0.58–0.76] | [0.60–0.87] | [0.62–0.91] | ||
| Race/Ethnicity (Ref. NHW) | ||||||
| Black Non-Hispanic | 1.15 *** | 0.95 | 1.03 | NA | NA | NA |
| [1.07–1.24] | [0.89–1.02] | [0.96–1.09] | ||||
| Hispanics | 1.13 ** | 0.94 | 1.01 | NA | NA | NA |
| [1.05–1.22] | [0.87–1.02] | [0.94–1.10] | ||||
| Foreign Language-English (=1, if respondent speak English professionally) | NA | 1.16 ** | 1.09 | 0.24 *** | 1.00 | 1.03 |
| [1.05–1.30] | [0.98–1.22] | [0.21–0.28] | [1.00–1.00] | [0.92–1.16] | ||
| Comorbidity | NA | NA | 1.19 *** | 1.19 *** | 1.22 *** | 1.21 *** |
| [1.17–1.22] | [1.16–1.22] | [1.17–1.26] | [1.15–1.26] | |||
| Has any health insurance coverage | NA | NA | 0.92 * | 0.88 * | 0.93 | 0.97 |
| [0.85–1.00] | [0.79–0.98] | [0.80–1.08] | [0.86–1.09] | |||
| See a mental health professional | NA | NA | 1.93 *** | 1.89 *** | 2.06 *** | 1.97 *** |
| [1.79–2.09] | [1.71–2.09] | [1.80–2.37] | [1.71–2.27] | |||
| A routine place to go for healthcare | NA | NA | 0.96 | 0.92 | 0.90 | 1.04 |
| [0.87–1.05] | [0.82–1.05] | [0.74–1.09] | [0.90–1.21] | |||
| Employed | NA | NA | 0.84 *** | 0.85 *** | 0.74 *** | 0.85 *** |
| [0.79–0.89] | [0.79–0.92] | [0.64–0.86] | [0.78–0.93] | |||
| Constant | 3.69 *** | 6.46 *** | 7.12 *** | 35.58 *** | 11.31 *** | 4.62 *** |
| [3.40–4.00] | [5.53–7.54] | [6.10–8.31] | [29.36–43.12] | [8.18–15.66] | [3.82–5.58] | |
| ln alpha | 1.32 *** | 1.21 *** | 1.05 | 1.00 | 1.11 * | 1.23 *** |
| [1.26–1.39] | [1.14–1.27] | [0.99–1.11] | [0.93–1.07] | [1.01–1.22] | [1.13–1.34] | |
| Model 1 (n = 11,420) | Model 2 (n = 11,420) | Model 3 (n = 11,420) | Model 4 (n = 11,420) | |
|---|---|---|---|---|
| Exp(b) [95% CI] | Exp(b) [95% CI] | Exp(b) [95% CI] | Exp(b) [95% CI] | |
| PIR Categories (Ref: if PIR < 1.12) | ||||
| Medium PIR (1.13–2.72) | NA | 0.56 *** | 0.65 *** | 0.87 |
| [0.47–0.67] | [0.53–0.79] | [0.68–1.11] | ||
| High PIR (2.73–5.00) | NA | 0.21 *** | 0.32 *** | 0.56 *** |
| [0.18–0.25] | [0.26–0.40] | [0.43–0.73] | ||
| Age | 0.99 * | 0.99 * | 0.99 * | 0.98 ** |
| [0.99–1.00] | [0.99–1.00] | [0.98–1.00] | [0.97–0.99] | |
| Married | NA | NA | 0.55 *** | 0.55 *** |
| [0.43–0.70] | [0.40–0.75] | |||
| Education (Ref. Less than high school) | ||||
| High school graduate/GED or equivalent | NA | NA | 0.78 | 0.74 |
| [0.58–1.05] | [0.52–1.05] | |||
| Some college or AA degree | NA | NA | 0.68 ** | 0.63 ** |
| [0.52–0.89] | [0.46–0.86] | |||
| College graduate or above | NA | NA | 0.34 *** | 0.36 *** |
| [0.24–0.49] | [0.22–0.58] | |||
| Race/Ethnicity (Ref. NHW) | ||||
| Black Non-Hispanic | 1.34 ** | 1.08 | 0.98 | 1.15 |
| [1.12–1.60] | [0.87–1.34] | [0.75–1.28] | [0.85–1.55] | |
| Hispanics | 1.35 ** | 1 | 1.01 | 1.26 |
| [1.13–1.61] | [0.82–1.22] | [0.79–1.29] | [0.91–1.76] | |
| Foreign Language-English | NA | NA | 1.2 | 1.08 |
| [0.84–1.71] | [0.71–1.62] | |||
| Comorbidity | NA | NA | NA | 1.47 *** |
| [1.29–1.66] | ||||
| Has any health insurance coverage | NA | NA | NA | 0.66 ** |
| [0.49–0.89] | ||||
| See a mental health professional | NA | NA | NA | 4.91 *** |
| [3.32–7.25] | ||||
| A routine place to go for healthcare | NA | NA | NA | 1.13 |
| [0.78–1.65] | ||||
| Employed | NA | NA | NA | 0.68 * |
| [0.49–0.96] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zare, H.; Fugal, A.; Azadi, M.; Gaskin, D.J. How Income Inequality and Race Concentrate Depression in Low-Income Women in the US; 2005–2016. Healthcare 2022, 10, 1424. https://doi.org/10.3390/healthcare10081424
Zare H, Fugal A, Azadi M, Gaskin DJ. How Income Inequality and Race Concentrate Depression in Low-Income Women in the US; 2005–2016. Healthcare. 2022; 10(8):1424. https://doi.org/10.3390/healthcare10081424
Chicago/Turabian StyleZare, Hossein, Adriele Fugal, Mojgan Azadi, and Darrell J. Gaskin. 2022. "How Income Inequality and Race Concentrate Depression in Low-Income Women in the US; 2005–2016" Healthcare 10, no. 8: 1424. https://doi.org/10.3390/healthcare10081424
APA StyleZare, H., Fugal, A., Azadi, M., & Gaskin, D. J. (2022). How Income Inequality and Race Concentrate Depression in Low-Income Women in the US; 2005–2016. Healthcare, 10(8), 1424. https://doi.org/10.3390/healthcare10081424







