Mechanisms of Social Interaction and Virtual Connections as Strong Predictors of Wellbeing of Older Adults
Abstract
:1. Introduction
1.1. Study Purpose
1.2. Background
1.3. Facets of Social Support
1.3.1. Participatory Activities and Related Perceptions
1.3.2. Technology Use
1.3.3. Cognition
1.3.4. Community Engagement
1.3.5. Mobility
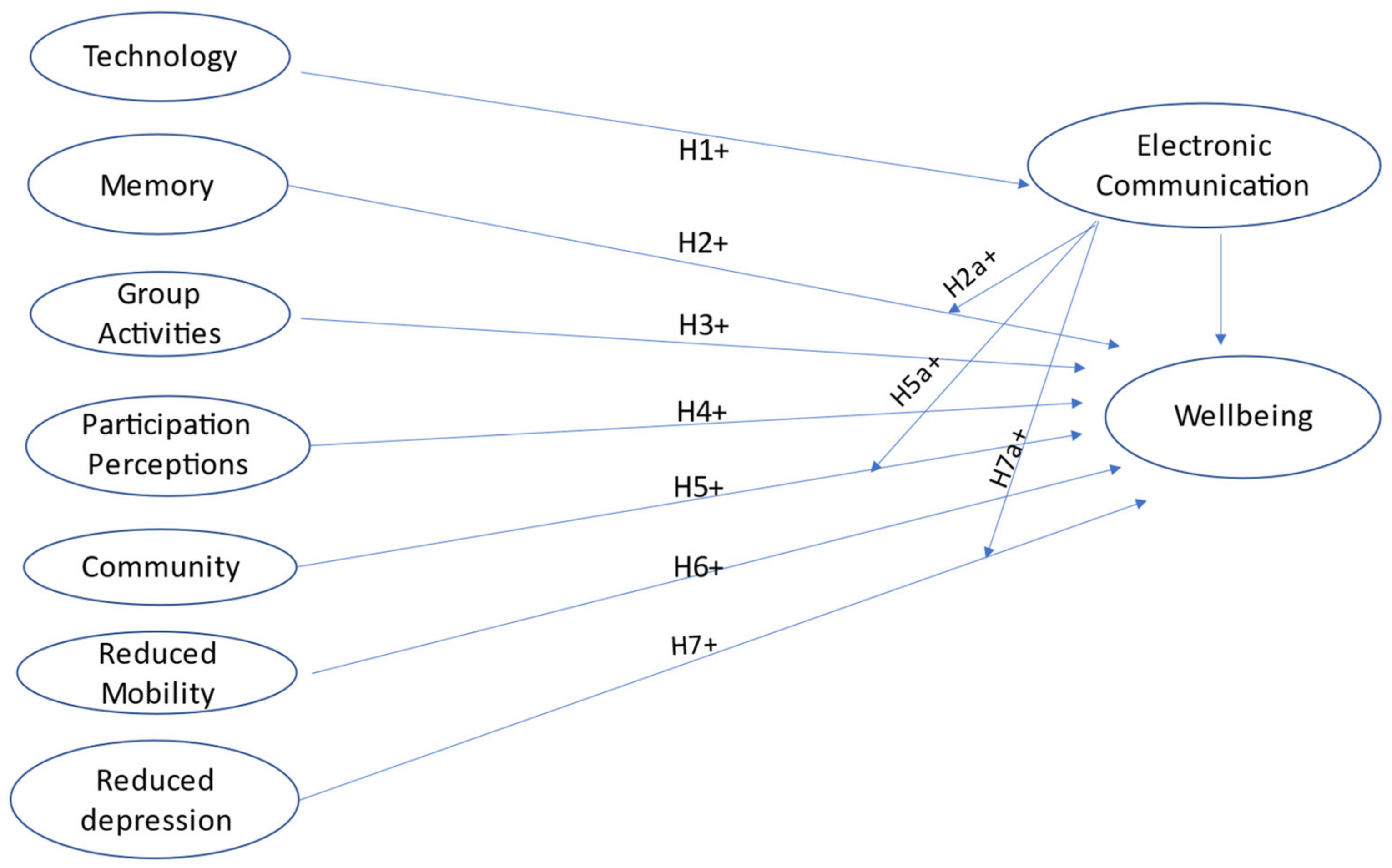
1.4. Research Question and Hypothesis
1.5. Theoretical Foundation
2. Methods
2.1. Design, Setting, and Sample
2.2. Data Cleaning
2.3. Measures
2.3.1. Wellbeing
2.3.2. Technology
2.3.3. Participation
2.3.4. Community
2.3.5. Reduced Mobility
2.3.6. Reduced Depression
2.3.7. Memory
2.4. Analysis Method
3. Results
3.1. Initial Analyses
3.2. Model Reliability and Validity
3.3. Model Analysis
4. Discussion
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Tang, B.; Li, Z. A Country-Level Empirical Study on the Fiscal Effect of Elderly Population Health: The Mediating Role of Healthcare Resources. Healthcare 2022, 10, 30. [Google Scholar] [CrossRef] [PubMed]
- Pohl, J.S.; Cochrane, B.B.; Schepp, K.G.; Woods, N.F. Measuring social isolation in the national health and aging trends study. Res. Gerontol. Nurs. 2017, 10, 277–287. [Google Scholar] [CrossRef] [PubMed]
- Smith, E.J.; Marcum, C.S.; Boessen, A.; Almquist, Z.W.; Hipp, J.R.; Nagle, N.N.; Butts, C.T. The relationship of age to personal network size, relational multiplexity, and proximity to alters in the Western United States. J. Gerontol. Ser. Psychol. Sci. Soc. Sci. 2015, 70, 91–99. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ribeiro, O.; Araújo, L.; Figueiredo, D.; Paúl, C.; Teixeira, L. The Caregiver Support Ratio in Europe: Estimating the Future of Potentially (Un)Available Caregivers. Healthcare 2022, 10, 11. [Google Scholar] [CrossRef]
- Losada-Baltar, A.; Jiménez-Gonzalo, L.; Gallego-Alberto, L.; Pedroso-Chaparro, M.D.S.; Fernandes-Pires, J.; Márquez-González, M. “We’re staying at home”. Association of self-perceptions of aging, personal and family resources and loneliness with psychological distress during the lock-down period of COVID-19. J. Gerontol. Ser. B 2020, 76, e10–e16. [Google Scholar] [CrossRef] [Green Version]
- Taylor, H.O.; Taylor, R.J.; Nguyen, A.W.; Chatters, L. Social isolation, depression, and psychological distress among older adults. J. Aging Health 2018, 30, 229–246. [Google Scholar] [CrossRef]
- HealthyPeople.gov. Available online: https://www.healthypeople.gov/2020/topics-objectives/topic/health-related-quality-of-life-well-being (accessed on 20 February 2022).
- Zahodne, L.B.; Zajacova, A. Education and Cognitive Aging: An Introduction to the Special Section. J. Gerontol. Ser. B 2020, 75, e78–e80. [Google Scholar] [CrossRef]
- Park, N.S. The relationship of social engagement to psychological well-being of older adults in assisted living facilities. J. Appl. Gerontol. 2009, 28, 461–481. [Google Scholar] [CrossRef]
- Alsmadi, D.; Prybutok, V. Sharing and storage behavior via cloud computing: Security and privacy in research and practice. Comput. Hum. Behav. 2018, 85, 218–226. [Google Scholar] [CrossRef]
- Zhang, T.; Wang, X.; Xu, Y. Multidomain Social Determinants of Depressive Symptoms for the Elderly with Chronic Diseases: Evidence from the China Health and Retirement Longitudinal Study. Healthcare 2021, 9, 1765. [Google Scholar] [CrossRef]
- Schrempft, S.; Jackowska, M.; Hamer, M.; Steptoe, A. Associations between social isolation, loneliness, and objective physical activity in older men and women. BMC Public Health 2019, 19, 74. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Byun, M.; Kim, E.; Ahn, H. Factors Contributing to Poor Self-Rated Health in Older Adults with Lower Income. Healthcare 2021, 9, 1515. [Google Scholar] [CrossRef] [PubMed]
- O’Conor, R.; Martynenko, M.; Gagnon, M.; Hauser, D.; Young, E.; Lurio, J. Supporting Asthma Self-Management Behaviors Among Aging Adults (SAMBA) investigators: A qualitative investigation of the impact of asthma and self-management strategies among older adults. J. Asthma 2017, 54, 39–45. [Google Scholar] [CrossRef]
- Sen, K.; Prybutok, G. A quality mobility program reduces elderly social isolation. Act. Adapt. Aging 2019, 45, 14–26. [Google Scholar] [CrossRef]
- McCartan, C.; Adell, T.; Cameron, J.; Davidson, G.; Knifton, L.; McDaid, S.; Mulholland, C. A scoping review of international policy responses to mental health recovery during the COVID-19 pandemic. Health Res. Policy Syst. 2021, 19, 58. [Google Scholar] [CrossRef] [PubMed]
- Pettigrew, S.; Donovan, R.; Boldy, D.; Newton, R. Older people’s perceived causes of and strategies for dealing with social isolation. Aging Ment. Health 2014, 18, 914–920. [Google Scholar] [CrossRef] [PubMed]
- Park, N.S.; Jang, Y.; Lee, B.S.; Ko, J.E.; Haley, W.E.; Chiriboga, D.A. An empirical typology of social networks and its association with physical and mental health: A study with older Korean immigrants. J. Gerontol. Ser. B Psychol. Sci. Soc. Sci. 2015, 70, 67–76. [Google Scholar] [CrossRef] [Green Version]
- Schwaba, T.; Bleidorn, W. Log on and prosper? Little evidence for co-development between psychological adjustment and technology use in older adulthood. J. Gerontol. Ser. B 2020, 76, 67–77. [Google Scholar] [CrossRef]
- Petrescu-Prahova, M.; Osterhage, K.; Taylor, J.O.; Painter, I.; Choi, Y.; Turner, A.M. Older adult health-related support networks: Implications for the design of digital communication tools. Innov. Aging 2020, 4, igaa020. [Google Scholar] [CrossRef]
- Chen, Y.R.; Schulz, P.J. The effect of information communication technology interventions on reducing social isolation in the elderly: A systematic review. J. Med. Internet Res. 2016, 18, e18. [Google Scholar] [CrossRef]
- Wunsch, K.; Hughes, C.M. Age-related decline in anticipatory motor planning and its relation to cognitive and motor skill proficiency. Front. Aging Neurosci. 2017, 9, 283. [Google Scholar]
- Morton, T.A.; Wilson, N.; Haslam, C.; Birney, M.; Kingston, R.; McCloskey, L.G. Activating and guiding the engagement of seniors with online social networking: Experimental findings from the AGES 2.0 project. J. Aging Health 2018, 30, 27–51. [Google Scholar] [CrossRef] [PubMed]
- LaMonica, H.M.; English, A.; Hickie, I.B.; Ip, J.; Ireland, C.; West, S.; Gibson, A.A. Examining Internet and eHealth practices and preferences: Survey study of Australian older adults with subjective memory complaints, mild cognitive impairment, or dementia. J. Med. Internet Res. 2017, 19, e358. [Google Scholar] [CrossRef] [Green Version]
- Mitzner, T.L.; Stuck, R.; Hartley, J.Q.; Beer, J.M.; Rogers, W.A. Acceptance of televideo technology by adults aging with a mobility impairment for health and wellness interventions. J. Rehabil. Assist. Technol. Eng. 2017, 4, 2055668317692755. [Google Scholar] [CrossRef] [Green Version]
- Steptoe, A.; Shankar, A.; Demakakos, P.; Wardle, J. Social isolation, loneliness, and all-cause mortality in older men and women. Proc. Natl. Acad. Sci. USA 2013, 110, 5797–5801. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- O’Connor, R.C.; Wetherall, K.; Cleare, S.; McClelland, H.; Melson, A.J.; Niedzwiedz, C.L.; Robb, K.A. Mental health and well-being during the COVID-19 pandemic: Longitudinal analyses of adults in the UK COVID-19 Mental Health & Wellbeing study. Br. J. Psychiatry 2021, 218, 326–333. [Google Scholar] [PubMed]
- Hand, C.; Rudman, D.L.; Huot, S.; Pack, R.; Gilliland, J. Enacting agency: Exploring how older adults shape their neighbourhoods. Ageing Soc. 2020, 40, 565–583. [Google Scholar] [CrossRef] [Green Version]
- Rosenkoetter, M.M.; McKethan, T.; Chernecky, C.; Looney, S. Assessment of the psychosocial adjustment of well elderly residing in retirement communities. Issues Ment. Health Nurs. 2016, 37, 858–867. [Google Scholar] [CrossRef] [PubMed]
- Mulholland, F.; Jackson, J. The experience of older adults with anxiety and depression living in the community: Aging, occupation and mental wellbeing. Br. J. Occup. Ther. 2018, 81, 657–666. [Google Scholar] [CrossRef]
- Qin, W.; Xiang, X.; Taylor, H. Driving cessation and social isolation in older adults. J. Aging Health 2020, 32, 962–971. [Google Scholar] [CrossRef]
- Li, M.; Tilahun, N. Time use, disability, and mobility of older Americans. Transp. Res. Rec. 2017, 2650, 58–65. [Google Scholar] [CrossRef]
- Nagamatsu, L.S.; Weinstein, A.M.; Erickson, K.I.; Fanning, J.; Awick, E.A.; Kramer, A.F.; McAuley, E. Exercise mode moderates the relationship between mobility and basal ganglia volume in healthy older adults. J. Am. Geriatr. Soc. 2016, 64, 102–108. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gómez, C.A.; Kleinman, D.V.; Pronk, N.; Gordon, G.L.W.; Ochiai, E.; Blakey, C.; Brewer, K.H. Practice Full Report: Addressing Health Equity and Social Determinants of Health Through Healthy People 2030. J. Public Health Manag. Pract. 2021, 27, S249. [Google Scholar] [PubMed]
- National Academies of Sciences, Engineering, and Medicine. Criteria for Selecting the Leading Health Indicators for Healthy People 2030; The National Academies Press: Washington, DC, USA, 2020. [Google Scholar]
- Havighurst, R.J. Successful aging. Processes Aging Soc. Psychol. Perspect. 1963, 1, 299–320. [Google Scholar]
- Holt-Lunstad, J.; Smith, T.B.; Baker, M.; Harris, T.; Stephenson, D. Loneliness and social isolation as risk factors for mortality: A meta-analytic review. Perspect. Psychol. Sci. 2015, 10, 227–237. [Google Scholar] [CrossRef] [Green Version]
- Zhong, B.L.; Chen, S.L.; Tu, X.; Conwell, Y. Loneliness and cognitive function in older adults: Findings from the Chinese longitudinal healthy longevity survey. J. Gerontol. Ser. B 2017, 72, 120–128. [Google Scholar] [CrossRef]
- Homans, G.C. Social Behavior: Its Elementary Forms; Harcourt Brace Jovanovich: New York, NY, USA, 1974. [Google Scholar]
- Zacher, H.; Rudolph, C.W. Successful aging at work and beyond: A review and critical perspective. In Age Diversity in the Workplace: An Organizational Perspective; Emerald Publishing Limited: Bradford, UK, 2017; pp. 35–64. [Google Scholar]
- Podsakoff, P.M.; Organ, D.W. Self-reports in organizational research: Problems and prospects. J. Manag. 1986, 12, 531–544. [Google Scholar] [CrossRef]
- Lecce, S.; Ceccato, I.; Rosi, A.; Bianco, F.; Bottiroli, S.; Cavallini, E. Theory of mind plasticity in aging: The role of baseline, verbal knowledge, and executive functions. Neuropsychol. Rehabil. 2019, 29, 440–455. [Google Scholar] [CrossRef]
- DeMatteis, J.; Freedman, V.A.; Kasper, J.D. National Health and Aging Trends Study (NHATS) Round 5 Sample Design and Selection. In NHATS Technical Paper #16; Johns Hopkins University School of Public Health: Baltimore, MD, USA, 2016; Available online: https://www.nhats.org/scripts/sampling/NHATS_Round5_Sample_Design_Rev12_12_17.pdf (accessed on 20 February 2022).
- Keith, T.Z. Multiple Regression and Beyond: An Introduction to Multiple Regression and Structural Equation Modeling; Routledge: London, UK, 2019. [Google Scholar]
- Faul, F.; Erdfelder, E.; Buchner, A.; Lang, A.G. Statistical power analyses using G*Power 3.1: Tests for correlation and regression analyses. Behav. Res. Methods 2009, 41, 1149–1160. [Google Scholar] [CrossRef] [Green Version]
- Siemsen, E.; Roth, A.; Oliveira, P. Common method bias in regression models with linear, quadratic, and interaction effects. Organ. Res. Methods 2010, 13, 456–476. [Google Scholar] [CrossRef]
- Harman, H.H. Modern Factor Analysis, 3rd ed.; University of Chicago Press: Chicago, IL, USA, 1976. [Google Scholar]
- Podsakoff, P.M.; MacKenzie, S.B.; Lee, J.Y.; Podsakoff, N.P. Common method biases in behavioral research: A critical review of the literature and recommended remedies. J. Appl. Psychol. 2003, 88, 879. [Google Scholar] [CrossRef] [PubMed]
- Freedman, D.A. As others see us: A case study in path analysis. J. Educ. Stat. 1987, 12, 101–128. [Google Scholar] [CrossRef] [Green Version]
- Lumley, T.; Diehr, P.; Emerson, S.; Chen, L. The importance of the normality assumption in large public health data sets. Annu. Rev. Public Health 2002, 23, 151–169. [Google Scholar] [CrossRef] [PubMed]
- Berk, R.A. Simple linear regression. In Regression Analysis: A Constructive Critique; Sage Publications, Inc.: Thousand Oaks, CA, USA, 2003. [Google Scholar]
- Hair, J.F.; Sarstedt, M.; Ringle, C.M.; Mena, J.A. An assessment of the use of partial least squares structural equation modeling in marketing research. J. Acad. Mark. Sci. 2012, 40, 414–433. [Google Scholar] [CrossRef]
- Rosales, A.; Fernández-Ardèvol, M. Beyond WhatsApp: Older people and smartphones. Rom. J. Commun. Public Relat. 2016, 18, 27–47. [Google Scholar] [CrossRef]
- Findlay, R.A. Interventions to reduce social isolation amongst older people: Where is the evidence? Ageing Soc. 2003, 23, 647–658. [Google Scholar] [CrossRef] [Green Version]
- Sanford, A.M.; Berg-Weger, M.; Lundy, J.; Morley, J.E. Aging friendly health systems. J. Nutr. Health Aging 2019, 23, 119–121. [Google Scholar] [CrossRef] [Green Version]
- Minkler, M.; Wallerstein, N. (Eds.) Community-Based Participatory Research for Health: From Process to Outcomes; John Wiley & Sons: New York, NY, USA, 2011. [Google Scholar]
- Wallerstein, N.B.; Duran, B. Using community-based participatory research to address health disparities. Health Promot. Pract. 2006, 7, 312–323. [Google Scholar] [CrossRef]
- Joshi, A.; Thorpe, L.; Waldron, L. Population Health Informatics; Jones & Bartlett Learning: Burlington, MA, USA, 2017. [Google Scholar]
- Cudjoe, T.K.; Roth, D.L.; Szanton, S.L.; Wolff, J.L.; Boyd, C.M.; Thorpe, R.J., Jr. The epidemiology of social isolation: National health and aging trends study. J. Gerontol. Ser. B 2002, 75, 107–113. [Google Scholar] [CrossRef] [Green Version]
- Kelly, M.E.; Duff, H.; Kelly, S.; Power, J.E.M.; Brennan, S.; Lawlor, B.A.; Loughrey, D.G. The impact of social activities, social networks, social support and social relationships on the cognitive functioning of healthy older adults: A systematic review. Syst. Rev. 2017, 6, 259. [Google Scholar] [CrossRef]
- Wardle, J.; von Wagner, C. Internet use, social engagement and health literacy decline during ageing in a longitudinal cohort of older English adults. J. Epidemiol. Community Health 2015, 69, 278–283. [Google Scholar]
- Sen, K.; Prybutok, G.; Prybutok, V. The use of digital technology for social wellbeing reduces social isolation in older adults: A systematic review. SSM-Popul. Health 2021, 17, 101020. [Google Scholar] [CrossRef] [PubMed]
- Flores-Martin, D.; Rojo, J.; Moguel, E.; Berrocal, J.; Murillo, J.M. Smart nursing homes: Self-management architecture based on iot and machine learning for rural areas. Wirel. Commun. Mob. Comput. 2021, 2021, 8874988. [Google Scholar] [CrossRef]
- Kastner, M.; Makarski, J.; Hayden, L.; Hamid, J.S.; Holroyd-Leduc, J.; Twohig, M.; Straus, S.E. Effectiveness of an eHealth self-management tool for older adults with multimorbidity (KeepWell): Protocol for a hybrid effectiveness–implementation randomised controlled trial. BMJ Open 2021, 11, e048350. [Google Scholar] [CrossRef] [PubMed]
| Domain | Indicators of the Social Inclusion (NHATS Interview Items) | Most Positive Response |
|---|---|---|
| Community | People know each other well | Yes |
| People are willing to help each other | ||
| People can be trusted | ||
| Depression | Little interest and pleasure | Not at all |
| Down, depressed, and hopeless | ||
| Nervous; anxious | ||
| Unable to stop worry | ||
| Technology | Working cell phone | Yes |
| One phone other than cell | ||
| Has a working computer | ||
| Has a tablet computer | ||
| Online computer use | ||
| Email/Text | Use of email or text messages | Yes |
| Self-Perceived Memory | Rate your memory | Excellent |
| Often, memory problems interfere | ||
| Mobility | Help to go outside | Yes |
| Get help inside | ||
| Family and friends provide help and drive | ||
| Walk to places | ||
| Get ride from family and friends | ||
| Group Activities | Ever attend religious services | Yes |
| Ever visit friends and family | ||
| Club meetings and group activities | ||
| Ever go out for enjoyment | ||
| Ever go walking | ||
| Get to do favorite activity last year | ||
| Perception of Group Activities | How important to participate in clubs and groups | Agree a lot |
| How important to visit friends and family | ||
| How important are religious services | ||
| How important to go out for enjoyment | ||
| Wellbeing | Life has meaning and purpose | Every Day |
| Feels confident | ||
| Often feels full of life | ||
| Often feels upset |
| Items | Mean | Std. Deviation | Cronbach’s Alpha (α) |
|---|---|---|---|
| Technology | 0.62 | 0.234 | 0.709 |
| Self-perceived memory | 3.61 | 0.891 | 0.781 |
| Group activities | 0.67 | 0.232 | 0.790 |
| Perception group activities | 2.19 | 0.535 | 0.697 |
| Community engagement | 2.42 | 0.547 | 0.743 |
| Reduced mobility | 0.30 | 0.219 | 0.681 |
| Reduced self-reported depression | 3.59 | 0.547 | 0.743 |
| Wellbeing | 2.69 | 0.340 | 0.749 |
| Predictors | Unstd B Coeff | Std β Coeff | t-test | Sig | VIF | Hypothesis | Supported |
|---|---|---|---|---|---|---|---|
| Technology | 0.057 | 0.039 | 2.576 | 0.010 * | 1.758 | H1 | Yes |
| Memory | 0.049 | 0.127 | 6.892 | 0.000 ** | 2.613 | H2 | Yes |
| Group activities | 0.184 | 0.125 | 8.535 | 0.000 ** | 1.660 | H3 | Yes |
| Perception of group activities | 0.061 | 0.096 | 6.787 | 0.000 ** | 1.535 | H4 | Yes |
| Community engagement | 0.068 | 0.109 | 6.577 | 0.000 ** | 2.097 | H5 | Yes |
| Reduced mobility | −0.013 | −0.009 | −0.707 | 0.000 ** | 1.143 | H6 | Yes |
| Reduced self-reported depression | 0.274 | 0.441 | 28.262 | 0.000 ** | 1.872 | H7 | Yes |
| Moderators | Unstd B Coeff | Std β Coeff | t-test | Sig | Hypothesis | Supported |
|---|---|---|---|---|---|---|
| EC x Memory | −0.010 | −0.057 | −1.068 | 0.286 | H2a | No |
| EC x Community engagement | 0.027 | 0.099 | 2.018 | 0.044 | H5a | Yes |
| EC x Reduced self-reported Depression | 0.032 | 0.167 | 2.667 | 0.008 | H7a | Yes |
| DP | CM | TE | CG | MO | GA | PGA | WB | |
|---|---|---|---|---|---|---|---|---|
| Depression (DP) | 1 | |||||||
| Community Engagement (CM)) | 0.125 ** | 1 | ||||||
| Technology (TE) | 0.208 ** | 0.130 ** | 1 | |||||
| Self-Perceived Memory (CG) | 0.317 ** | 0.096 ** | 0.227 ** | 1 | ||||
| Mobility (MO) | −0.221 ** | 00.013 | −0.185 ** | −0.149 ** | 1 | |||
| Group Activities (GA) | 0.235 ** | 0.237 ** | 0.327 ** | 0.148 ** | −0.079 ** | 1 | ||
| Perception of Group Activities (PGA) | 0.134 ** | 0.221 ** | 0.198 ** | 0.117 ** | 0.011 | 0.562 ** | 1 | |
| Wellbeing (WB) | 0.564 ** | 0.201 ** | 0.246 ** | 0.306 ** | −0.152 ** | 0.343 ** | 0.272 ** | 1 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sen, K.; Prybutok, V.; Prybutok, G.; Senn, W. Mechanisms of Social Interaction and Virtual Connections as Strong Predictors of Wellbeing of Older Adults. Healthcare 2022, 10, 553. https://doi.org/10.3390/healthcare10030553
Sen K, Prybutok V, Prybutok G, Senn W. Mechanisms of Social Interaction and Virtual Connections as Strong Predictors of Wellbeing of Older Adults. Healthcare. 2022; 10(3):553. https://doi.org/10.3390/healthcare10030553
Chicago/Turabian StyleSen, Keya, Victor Prybutok, Gayle Prybutok, and William Senn. 2022. "Mechanisms of Social Interaction and Virtual Connections as Strong Predictors of Wellbeing of Older Adults" Healthcare 10, no. 3: 553. https://doi.org/10.3390/healthcare10030553
APA StyleSen, K., Prybutok, V., Prybutok, G., & Senn, W. (2022). Mechanisms of Social Interaction and Virtual Connections as Strong Predictors of Wellbeing of Older Adults. Healthcare, 10(3), 553. https://doi.org/10.3390/healthcare10030553







