Effects of Mobile-Based Rehabilitation in Adolescent Football Players with Recurrent Lateral Ankle Sprains during the COVID-19 Pandemic
Abstract
1. Introduction
2. Materials and Methods
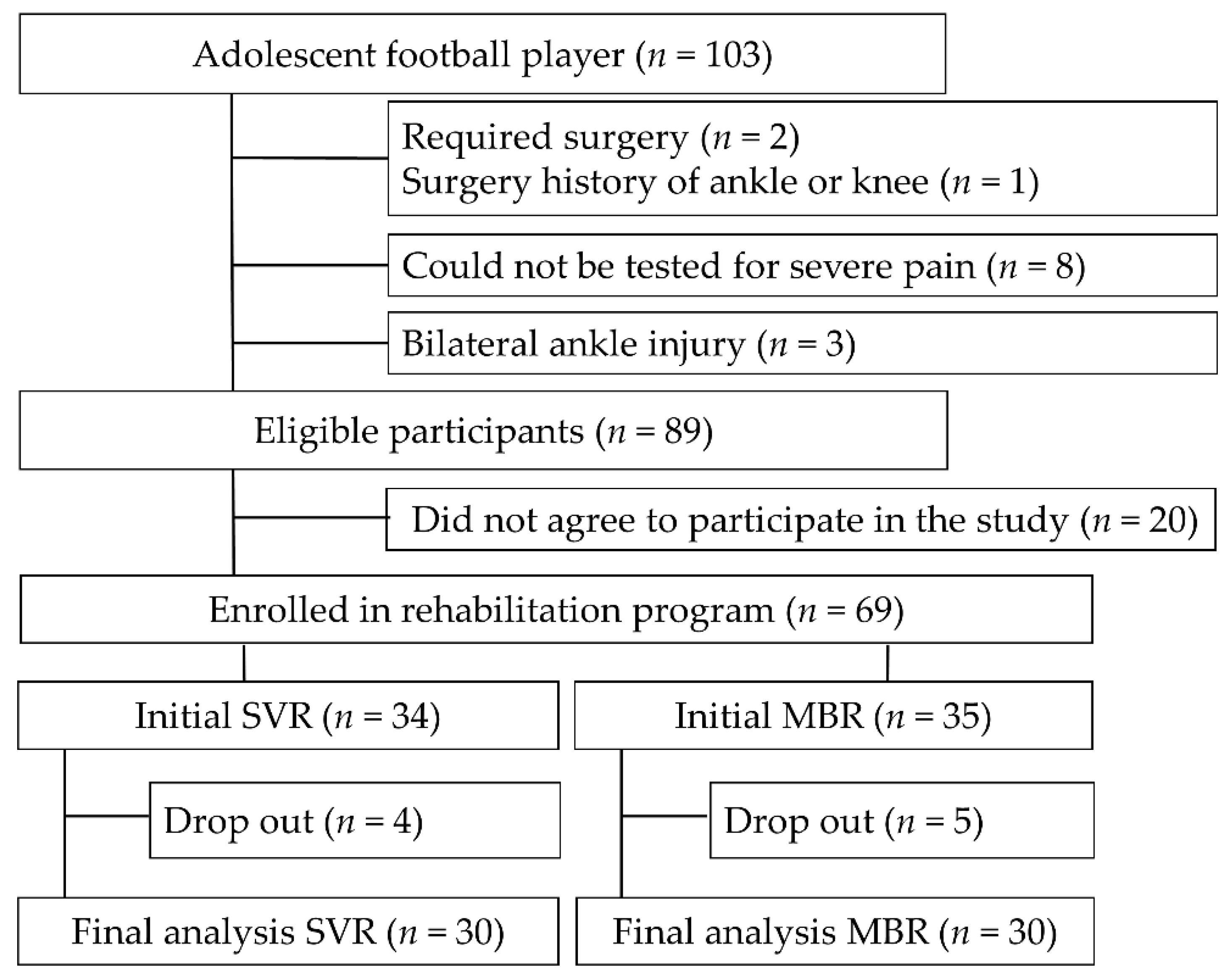
2.1. Participants
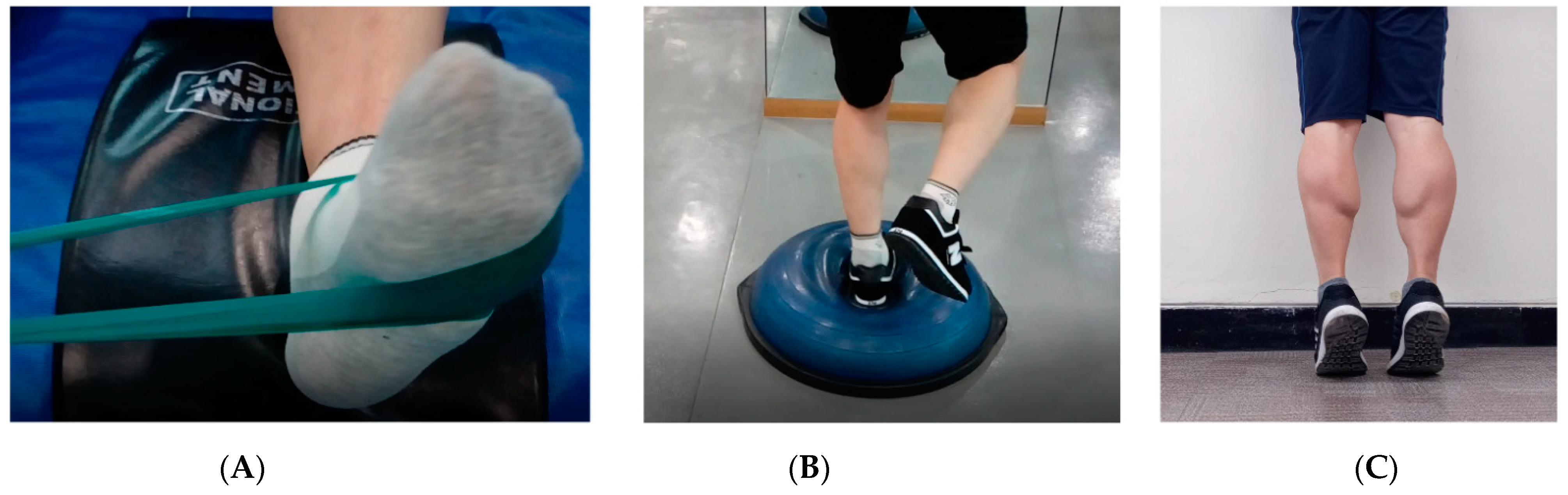
2.2. Rehabilitation Program
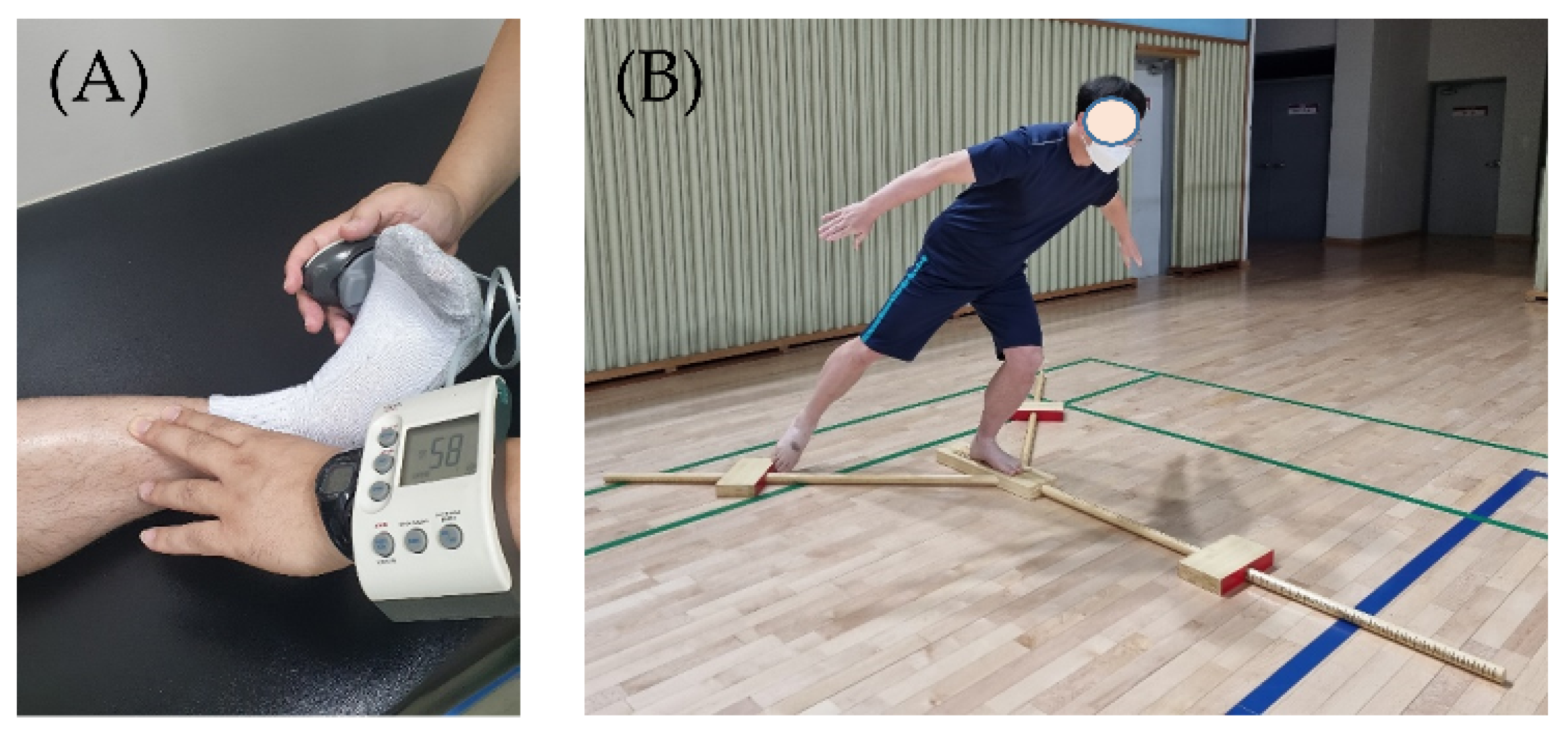
2.3. Ankle Strength Test
2.4. Y-Balance Test
2.5. Self-Evaluation Using Questionnaires
2.6. Data Analysis
3. Results
3.1. General Characteristics of Participants
3.2. Ankle Strength Test Using Hand Held Dynamometer
3.3. Dynamic Balance with Y-Balance Test
3.4. Foot and Ankle Outcome Score Questionnaire
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Francavilla, C.V.; Sessa, F.; Salerno, M.; Albano, G.D.; Villano, I.; Messina, G.; Triolo, F.; Todaro, L.; Ruberto, M.; Marsala, G. Influence of football on physiological cardiac indexes in professional and young athletes. Front. Physiol. 2018, 9, 153–160. [Google Scholar] [CrossRef] [PubMed]
- Kofotolis, N.D.; Kellis, E.; Vlachopoulos, S.P. Ankle sprain injuries and risk factors in amateur soccer players during a 2-year period. Am. J. Sports Med. 2007, 35, 458–466. [Google Scholar] [CrossRef]
- Waterman, B.R.; Owens, B.D.; Davey, S.; Zacchilli, M.A.; Belmont, P.J., Jr. The epidemiology of ankle sprains in the United States. JBJS 2010, 92, 2279–2284. [Google Scholar] [CrossRef] [PubMed]
- Gallenberger, K.; Yoganandan, N.; Pintar, F. Biomechanics of foot/ankle trauma with variable energy impacts. Ann. Adv. Automot. Med. 2013, 57, 123. [Google Scholar] [PubMed]
- Doherty, C.; Bleakley, C.; Hertel, J.; Caulfield, B.; Ryan, J.; Delahunt, E. Locomotive biomechanics in persons with chronic ankle instability and lateral ankle sprain copers. J. Sci. Med. Sport 2016, 19, 524–530. [Google Scholar] [CrossRef]
- Doherty, C.; Bleakley, C.; Delahunt, E.; Holden, S. Treatment and prevention of acute and recurrent ankle sprain: An overview of systematic reviews with meta-analysis. Br. J. Sports Med. 2017, 51, 113–125. [Google Scholar] [CrossRef]
- Herzog, M.M.; Kerr, Z.Y.; Marshall, S.W.; Wikstrom, E.A. Epidemiology of ankle sprains and chronic ankle instability. J. Athl. Train. 2019, 54, 603–610. [Google Scholar] [CrossRef]
- Gruskay, J.A.; Brusalis, C.M.; Heath, M.R.; Fabricant, P.D. Pediatric and adolescent ankle instability: Diagnosis and treatment options. Curr. Opin. Pediatrics 2019, 31, 69–78. [Google Scholar] [CrossRef]
- Hiller, C.E.; Refshauge, K.M.; Herbert, R.D.; Kilbreath, S.L. Intrinsic predictors of lateral ankle sprain in adolescent dancers: A prospective cohort study. Clin. J. Sport Med. 2008, 18, 44–48. [Google Scholar] [CrossRef]
- Feger, M.A.; Glaviano, N.R.; Donovan, L.; Hart, J.M.; Saliba, S.A.; Park, J.S.; Hertel, J. Current trends in the management of lateral ankle sprain in the United States. Clin. J. Sport Med. 2017, 27, 145–152. [Google Scholar] [CrossRef]
- Vuurberg, G.; Hoorntje, A.; Wink, L.M.; Van Der Doelen, B.F.; Van Den Bekerom, M.P.; Dekker, R.; Van Dijk, C.N.; Krips, R.; Loogman, M.C.; Ridderikhof, M.L. Diagnosis, treatment and prevention of ankle sprains: Update of an evidence-based clinical guideline. Br. J. Sports Med. 2018, 52, 956. [Google Scholar] [CrossRef] [PubMed]
- Caldemeyer, L.E.; Brown, S.M.; Mulcahey, M.K. Neuromuscular training for the prevention of ankle sprains in female athletes: A systematic review. Phys. Sportsmed. 2020, 48, 363–369. [Google Scholar] [CrossRef] [PubMed]
- McKeon, J.M.M.; Bush, H.M.; Reed, A.; Whittington, A.; Uhl, T.L.; McKeon, P.O. Return-to-play probabilities following new versus recurrent ankle sprains in high school athletes. J. Sci. Med. Sport 2014, 17, 23–28. [Google Scholar] [CrossRef] [PubMed]
- Mulcahey, M.K.; Gianakos, A.L.; Mercurio, A.; Rodeo, S.; Sutton, K.M. Sports medicine considerations during the COVID-19 pandemic. Am. J. Sports Med. 2021, 49, 512–521. [Google Scholar] [CrossRef] [PubMed]
- Wong, A.Y.-Y.; Ling, S.K.-K.; Louie, L.H.-T.; Law, G.Y.-K.; So, R.C.-H.; Lee, D.C.-W.; Yau, F.C.-F.; Yung, P.S.-H. Impact of the COVID-19 pandemic on sports and exercise. Asia-Pac. J. Sports Med. Arthrosc. Rehabil. Technol. 2020, 22, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Nussbaum, R.; Kelly, C.; Quinby, E.; Mac, A.; Parmanto, B.; Dicianno, B.E. Systematic review of mobile health applications in rehabilitation. Arch. Phys. Med. Rehabil. 2019, 100, 115–127. [Google Scholar] [CrossRef]
- Hupperets, M.D.; Verhagen, E.A.; Van Mechelen, W. Effect of unsupervised home based proprioceptive training on recurrences of ankle sprain: Randomised controlled trial. BMJ 2009, 339, b2684–b2689. [Google Scholar] [CrossRef]
- Feger, M.A.; Herb, C.C.; Fraser, J.J.; Glaviano, N.; Hertel, J. Supervised rehabilitation versus home exercise in the treatment of acute ankle sprains: A systematic review. Clin. Sports Med. 2015, 34, 329–346. [Google Scholar] [CrossRef]
- Bleakley, C.M.; Taylor, J.B.; Dischiavi, S.L.; Doherty, C.; Delahunt, E. Rehabilitation exercises reduce reinjury post ankle sprain, but the content and parameters of an optimal exercise program have yet to be established: A systematic review and meta-analysis. Arch. Phys. Med. Rehabil. 2019, 100, 1367–1375. [Google Scholar] [CrossRef]
- Wang, H.; Yu, H.; Kim, Y.H.; Kan, W. Comparison of the Effect of Resistance and Balance Training on Isokinetic Eversion Strength, Dynamic Balance, Hop Test, and Ankle Score in Ankle Sprain. Life 2021, 11, 307. [Google Scholar] [CrossRef]
- Chen, E.T.; McInnis, K.C.; Borg-Stein, J. Ankle sprains: Evaluation, rehabilitation, and prevention. Curr. Sports Med. Rep. 2019, 18, 217–223. [Google Scholar] [CrossRef] [PubMed]
- Alfuth, M.; Hahm, M.M. Reliability, comparability, and validity of foot inversion and eversion strength measurements using a hand-held dynamometer. Int. J. Sports Phys. Ther. 2016, 11, 72–84. [Google Scholar] [PubMed]
- Ancillao, A.; Palermo, E.; Rossi, S. Validation of ankle strength measurements by means of a hand-held dynamometer in adult healthy subjects. J. Sens. 2017, 2017, 1–8. [Google Scholar] [CrossRef]
- Stark, T.; Walker, B.; Phillips, J.K.; Fejer, R.; Beck, R. Hand-held dynamometry correlation with the gold standard isokinetic dynamometry: A systematic review. PM&R 2011, 3, 472–479. [Google Scholar]
- Spink, M.J.; Fotoohabadi, M.R.; Menz, H.B. Foot and ankle strength assessment using hand-held dynamometry: Reliability and age-related differences. Gerontology 2010, 56, 525–532. [Google Scholar] [CrossRef] [PubMed]
- Sökmen, B.; Witchey, R.L.; Adams, G.M.; Beam, W.C. Effects of sprint interval training with active recovery vs. endurance training on aerobic and anaerobic power, muscular strength, and sprint ability. J. Strength Cond. Res. 2018, 32, 624–631. [Google Scholar] [CrossRef]
- Coughlan, G.F.; Fullam, K.; Delahunt, E.; Gissane, C.; Caulfield, B.M. A comparison between performance on selected directions of the star excursion balance test and the Y balance test. J. Athl. Train. 2012, 47, 366–371. [Google Scholar] [CrossRef]
- van den Akker-Scheek, I.; Seldentuis, A.; Reininga, I.H.; Stevens, M. Reliability and validity of the Dutch version of the Foot and Ankle Outcome Score (FAOS). BMC Musculoskelet Disord 2013, 14, 183–188. [Google Scholar] [CrossRef]
- Simon, J.; Donahue, M.; Docherty, C. Development of the identification of functional ankle instability (IdFAI). Foot Ankle Int. 2012, 33, 755–763. [Google Scholar] [CrossRef]
- Tourné, Y.; Besse, J.-L.; Mabit, C. Chronic ankle instability. Which tests to assess the lesions? Which therapeutic options? Orthop. Traumatol. Surg. Res. 2010, 96, 433–446. [Google Scholar] [CrossRef]
- Buchner, A.; Erdfelder, E.; Faul, F.; Lang, A. G* Power 3.1 Manual; Heinrich-Heine-Universitat Dusseldorf: Düsseldorf, Germany, 2017. [Google Scholar]
- Pallant, J. SPSS Survival Manual: A Step by Step Guide to Data Analysis Using IBM SPSS; Routledge: London, UK, 2020. [Google Scholar]
- Cleland, J.A.; Mintken, P.; McDevitt, A.; Bieniek, M.; Carpenter, K.; Kulp, K.; Whitman, J.M. Manual physical therapy and exercise versus supervised home exercise in the management of patients with inversion ankle sprain: A multicenter randomized clinical trial. J. Orthop. Sports Phys. Ther. 2013, 43, 443–455. [Google Scholar] [CrossRef] [PubMed]
- Vourganas, I.; Stankovic, V.; Stankovic, L.; Michala, A.L. Evaluation of home-based rehabilitation sensing systems with respect to standardised clinical tests. Sensors 2020, 20, 26. [Google Scholar] [CrossRef] [PubMed]
- Argent, R.; Daly, A.; Caulfield, B. Patient involvement with home-based exercise programs: Can connected health interventions influence adherence? JMIR Mhealth Uhealth 2018, 6, e47–e55. [Google Scholar] [CrossRef] [PubMed]
- De Ridder, R.; Willems, T.; Vanrenterghem, J.; Roosen, P. Effect of a home-based balance training protocol on dynamic postural control in subjects with chronic ankle instability. Int. J. Sports Med. 2015, 36, 596–602. [Google Scholar] [CrossRef] [PubMed]
- D’Hooghe, P.; Cruz, F.; Alkhelaifi, K. Return to play after a lateral ligament ankle sprain. Curr. Rev. Musculoskelet. Med. 2020, 13, 281–288. [Google Scholar] [CrossRef]
- Hubbard, T.J.; Hicks-Little, C.A. Ankle ligament healing after an acute ankle sprain: An evidence-based approach. J. Athl. Train. 2008, 43, 523–529. [Google Scholar] [CrossRef]
- Hauser, R.A.; Dolan, E.E. Ligament injury and healing: An overview of current clinical concepts. J. Prolotherapy 2011, 3, 836–846. [Google Scholar]
- Walker, A.; Hing, W.; Lorimer, A. The influence, barriers to and facilitators of anterior cruciate ligament rehabilitation adherence and participation: A scoping review. Sports Med.-Open 2020, 6, 1–22. [Google Scholar] [CrossRef]
- Guillodo, Y.; Simon, T.; Le Goff, A.; Saraux, A. Interest of rehabilitation in healing and preventing recurrence of ankle sprains. Ann. Phys. Rehabil. Med. 2013, 56, 503–514. [Google Scholar] [CrossRef][Green Version]
- Hammami, A.; Harrabi, B.; Mohr, M.; Krustrup, P. Physical activity and coronavirus disease 2019 (COVID-19): Specific recommendations for home-based physical training. Manag. Sport Leis. 2020, 18, 1–6. [Google Scholar] [CrossRef]
- de Noronha, M.; Refshauge, K.M.; Herbert, R.D.; Kilbreath, S.L. Do voluntary strength, proprioception, range of motion, or postural sway predict occurrence of lateral ankle sprain? Br. J. Sports Med. 2006, 40, 824–828. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.; Kim, Y.H.; Lee, S.; Seo, S.G. Characteristics of the balance ability and isokinetic strength in ankle sprain. Isokinet. Exerc. Sci. 2020, 28, 239–245. [Google Scholar] [CrossRef]
- Verhagen, E.; Bay, K. Optimising ankle sprain prevention: A critical review and practical appraisal of the literature. Br. J. Sports Med. 2010, 44, 1082–1088. [Google Scholar] [CrossRef] [PubMed]
- Mohammadi, F. Comparison of 3 preventive methods to reduce the recurrence of ankle inversion sprains in male soccer players. Am. J. Sports Med. 2007, 35, 922–926. [Google Scholar] [CrossRef] [PubMed]
- Wedderkopp, N.; Kaltoft, M.; Holm, R.; Froberg, K. Comparison of two intervention programmes in young female players in European handball–with and without ankle disc. Scand. J. Med. Sci. Sports 2003, 13, 371–375. [Google Scholar] [CrossRef] [PubMed]
- Ma, M.; Proffitt, R.; Skubic, M. Validation of a Kinect V2 based rehabilitation game. PLoS ONE 2018, 13, e0202338–e0202352. [Google Scholar] [CrossRef]


| Week | Strength Training with Band and Weight | Balance Training with BOSU | Duration and No. of Sessions |
|---|---|---|---|
| 1–2 | Band color: red Ankle inversion, eversion Squat | BOSU: hard surface One or two leg stand | 15 min 2 sessions per day |
| 3–4 | Band color: green Ankle inversion, eversion, plantarflexion Squat, heel raise | BOSU: hard surface One leg squat | 15 min 2 sessions per day |
| 5–6 | Band color: blue Ankle inversion, eversion, plantarflexion, dorsiflexion Squat, heel raise, toe up Hip abduction-adduction | BOSU: soft surface One leg squat and twist | 30 min 1 time per day |
| 7–8 | Band color: gray Ankle inversion, eversion, plantarflexion, dorsiflexion Squat, heel raise, toe up Hip abduction, adduction, flexion, extension | BOSU: soft surface One leg squat and twist Jump and change direction | 30 min 1 time per day |
| Variables | SVR (n = 30) | MBR (n = 30) | t or χ2 | p-Value | E.S |
|---|---|---|---|---|---|
| Age, years | 16.3 ± 1.2 | 16.0 ± 1.3 | 0.866 | 0.390 | 0.239 |
| Height, cm | 174.9 ± 6.7 | 173.9 ± 5.0 | 0.63.5 | 0.528 | 0.169 |
| Weight, kg | 64.8 ± 9.6 | 65.3 ± 5.9 | −0.248 | 0.805 | 0.006 |
| BMI, kg/m2 | 21.1 ± 1.9 | 21.5 ± 1.2 | −1.149 | 0.255 | 0.251 |
| Lateral ankle sprain in the last month | |||||
| 1–2 times | 19 (63.3%) | 16 (53.3%) | 1.257 | 0.533 | 0.145 |
| 3–4 times | 8 (26.7%) | 12 (40.0%) | |||
| >5 times | 3 (10.0%) | 2 (6.7%) | |||
| Playing position, n (%) | |||||
| Goal keeper | 3 (10.3%) | 2 (6.7%) | 2.912 | 0.405 | 0.220 |
| Defender | 7 (23.3%) | 9 (30.0%) | |||
| Mid–fielder | 17 (56.7%) | 12 (40.0%) | |||
| Forward | 3 (10.3%) | 7 (23.3%) | |||
| Injury side, n (%) | |||||
| Right | 16 (53.3%) | 17 (56.7%) | 0.067 | 0.795 | 0.034 |
| Left | 14 (46.7%) | 13 (43.3%) |
| Subject Scoring | Week | SVR (n = 30) | MBR (n = 30) | t | p-Value | Time × Group, p | E.S |
|---|---|---|---|---|---|---|---|
| Foot and ankle outcome score | 1 | 72.0 ± 7.3 | 72.8 ± 7.2 | −0.435 | 0.655 | 0.009 | 0.297 |
| 4 | 84.0 ± 7.2 a | 77.8 ± 7.6 | 3.616 | <0.001 | |||
| 8 | 92.9 ± 4.5 b,c | 90.0 ± 4.7 b,c | 2.346 | 0.022 | |||
| p-value | <0.001 | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Qu, X.; Li, K.; Nam, S. Effects of Mobile-Based Rehabilitation in Adolescent Football Players with Recurrent Lateral Ankle Sprains during the COVID-19 Pandemic. Healthcare 2022, 10, 412. https://doi.org/10.3390/healthcare10030412
Qu X, Li K, Nam S. Effects of Mobile-Based Rehabilitation in Adolescent Football Players with Recurrent Lateral Ankle Sprains during the COVID-19 Pandemic. Healthcare. 2022; 10(3):412. https://doi.org/10.3390/healthcare10030412
Chicago/Turabian StyleQu, Xiaobo, Kai Li, and Sangcheul Nam. 2022. "Effects of Mobile-Based Rehabilitation in Adolescent Football Players with Recurrent Lateral Ankle Sprains during the COVID-19 Pandemic" Healthcare 10, no. 3: 412. https://doi.org/10.3390/healthcare10030412
APA StyleQu, X., Li, K., & Nam, S. (2022). Effects of Mobile-Based Rehabilitation in Adolescent Football Players with Recurrent Lateral Ankle Sprains during the COVID-19 Pandemic. Healthcare, 10(3), 412. https://doi.org/10.3390/healthcare10030412





