Evaluation of the Potential Risk of Mortality from SARS-CoV-2 Infection in Hospitalized Patients According to the Charlson Comorbidity Index
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Sample Size Calculation
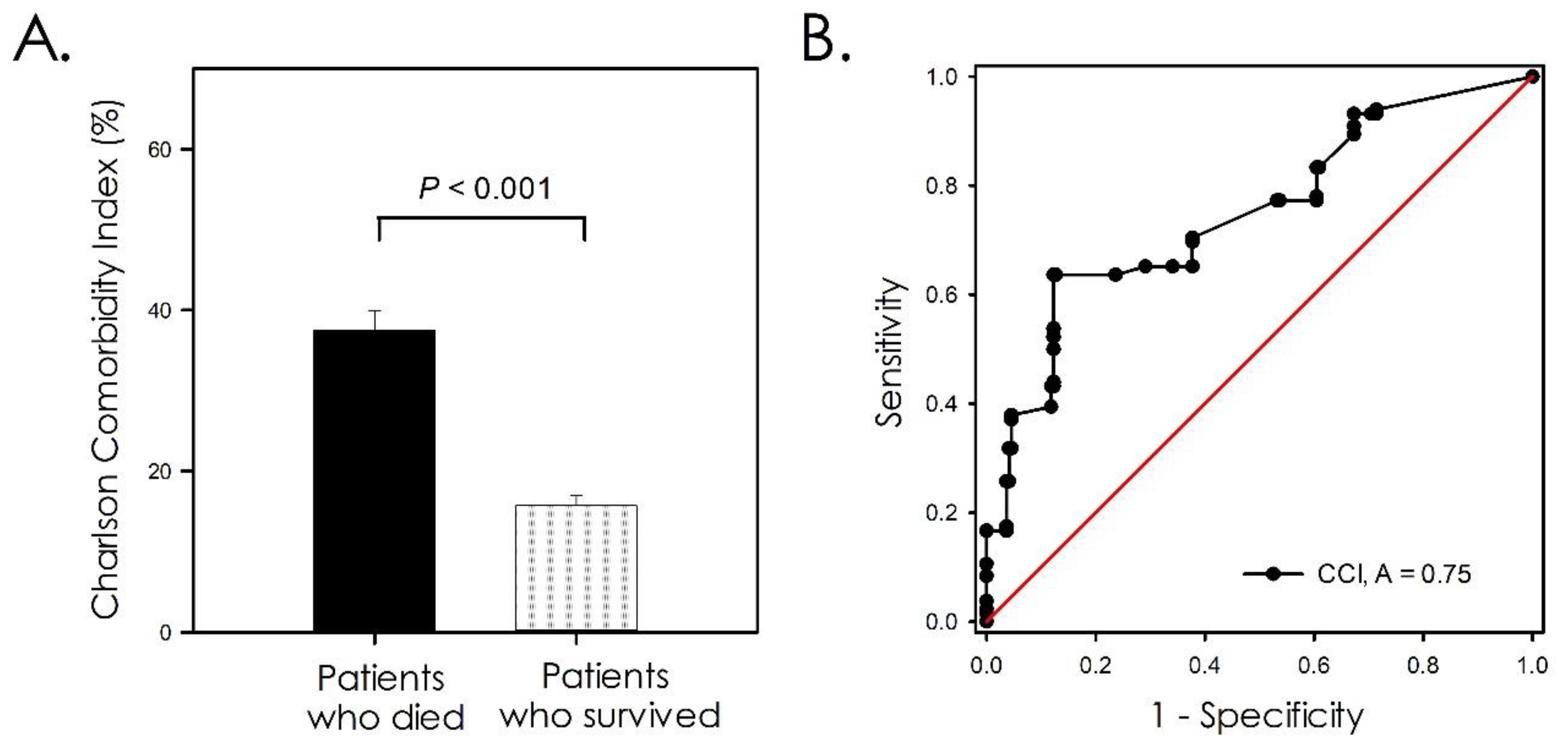
2.3. Charlson Comorbidity Index (CCI)
2.4. Data Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Holshue, M.L.; DeBolt, C.; Lindquist, S.; Lofy, K.H.; Wiesman, J.; Bruce, H.; Spitters, C.; Ericson, K.; Wilkerson, S.; Tural, A.; et al. First Case of 2019 Novel Coronavirus in the United States. N. Engl. J. Med. 2020, 382, 929–936. [Google Scholar] [CrossRef] [PubMed]
- Parry, J. China coronavirus: Cases surge as official admits human to human transmission. BMJ 2020, 368, m236. [Google Scholar] [CrossRef] [Green Version]
- Silverstein, W.K.; Stroud, L.; Cleghorn, G.E.; Leis, J.A. First imported case of 2019 novel coronavirus in Canada, presenting as mild pneumonia. Lancet 2020, 395, 734. [Google Scholar] [CrossRef]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [Green Version]
- Zhang, J.J.; Dong, X.; Cao, Y.Y.; Yuan, Y.D.; Yang, Y.B.; Yan, Y.Q.; Akdis, C.A.; Gao, Y.D. Clinical characteristics of 140 patients infected with SARS-CoV-2 in Wuhan, China. Allergy 2020, 75, 1730–1741. [Google Scholar] [CrossRef] [PubMed]
- Ren, X.; Glende, J.; Al-Falah, M.; de Vries, V.; Schwegmann-Wessels, C.; Qu, X.; Tan, L.; Tschernig, T.; Deng, H.; Naim, H.Y.; et al. Analysis of ACE2 in polarized epithelial cells: Surface expression and function as receptor for severe acute respiratory syndrome-associated coronavirus. J. Gen. Virol. 2006, 87, 1691–1695. [Google Scholar] [CrossRef] [PubMed]
- Zhou, P.; Yang, X.L.; Wang, X.G.; Hu, B.; Zhang, L.; Zhang, W.; Si, H.R.; Zhu, Y.; Li, B.; Huang, C.L.; et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020, 579, 270–273. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jin, Y.H.; Cai, L.; Cheng, Z.S.; Cheng, H.; Deng, T.; Fan, Y.P.; Fang, C.; Huang, D.; Huang, L.Q.; Huang, Q.; et al. A rapid advice guideline for the diagnosis and treatment of 2019 novel coronavirus (2019-nCoV) infected pneumonia (standard version). Mil. Med. Res. 2020, 7, 4. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Callender, L.A.; Curran, M.; Bates, S.M.; Mairesse, M.; Weigandt, J.; Betts, C.J. The Impact of Pre-existing Comorbidities and Therapeutic Interventions on COVID-19. Front. Immunol. 2020, 11, 1991. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Zheng, Y.; Gou, X.; Pu, K.; Chen, Z.; Guo, Q.; Ji, R.; Wang, H.; Wang, Y.; Zhou, Y. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: A systematic review and meta-analysis. Int. J. Infect. Dis. IJID Off. Publ. Int. Soc. Infect. Dis. 2020, 94, 91–95. [Google Scholar] [CrossRef] [PubMed]
- Guan, W.J.; Liang, W.H.; He, J.X.; Zhong, N.S. Cardiovascular comorbidity and its impact on patients with COVID-19. Eur. Respir. J. 2020, 55, 2001227. [Google Scholar] [CrossRef] [PubMed]
- Posso, M.; Comas, M.; Roman, M.; Domingo, L.; Louro, J.; Gonzalez, C.; Sala, M.; Angles, A.; Cirera, I.; Cots, F.; et al. Comorbidities and Mortality in Patients With COVID-19 Aged 60 Years and Older in a University Hospital in Spain. Arch. De Bronconeumol. 2020, 56, 756–758. [Google Scholar] [CrossRef]
- Singh, A.K.; Gupta, R.; Misra, A. Comorbidities in COVID-19: Outcomes in hypertensive cohort and controversies with renin angiotensin system blockers. Diabetes Metab. Syndr. 2020, 14, 283–287. [Google Scholar] [CrossRef] [PubMed]
- Zuin, M.; Rigatelli, G.; Zuliani, G.; Rigatelli, A.; Mazza, A.; Roncon, L. Arterial hypertension and risk of death in patients with COVID-19 infection: Systematic review and meta-analysis. J. Infect. 2020, 81, e84–e86. [Google Scholar] [CrossRef]
- Guo, T.; Fan, Y.; Chen, M.; Wu, X.; Zhang, L.; He, T.; Wang, H.; Wan, J.; Wang, X.; Lu, Z. Cardiovascular Implications of Fatal Outcomes of Patients With Coronavirus Disease 2019 (COVID-19). JAMA Cardiol. 2020, 5, 811–818. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Batiha, G.E.; Gari, A.; Elshony, N.; Shaheen, H.M.; Abubakar, M.B.; Adeyemi, S.B.; Al-Kuraishy, H.M. Hypertension and its management in COVID-19 patients: The assorted view. Int. J. Cardiol. Cardiovasc. Risk Prev. 2021, 11, 200121. [Google Scholar] [CrossRef] [PubMed]
- Fadini, G.P.; Morieri, M.L.; Longato, E.; Avogaro, A. Prevalence and impact of diabetes among people infected with SARS-CoV-2. J. Endocrinol. Investig. 2020, 43, 867–869. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pavlov, V.A. The evolving obesity challenge: Targeting the vagus nerve and the inflammatory reflex in the response. Pharmacol. Ther. 2021, 222, 107794. [Google Scholar] [CrossRef] [PubMed]
- Stefan, N.; Birkenfeld, A.L.; Schulze, M.B. Global pandemics interconnected—Obesity, impaired metabolic health and COVID-19. Nat. Rev. Endocrinol. 2021, 17, 135–149. [Google Scholar] [CrossRef] [PubMed]
- Herrmann, E.; de Ledinghen, V.; Cassinotto, C.; Chu, W.C.; Leung, V.Y.; Ferraioli, G.; Filice, C.; Castera, L.; Vilgrain, V.; Ronot, M.; et al. Assessment of biopsy-proven liver fibrosis by two-dimensional shear wave elastography: An individual patient data-based meta-analysis. Hepatology 2018, 67, 260–272. [Google Scholar] [CrossRef] [PubMed]
- Kruglikov, I.L.; Scherer, P.E. The Role of Adipocytes and Adipocyte-Like Cells in the Severity of COVID-19 Infections. Obesity 2020, 28, 1187–1190. [Google Scholar] [CrossRef] [PubMed]
- Shenoy, A.; Ismaily, M.; Bajaj, M. Diabetes and covid-19: A global health challenge. BMJ Open Diabetes Res. Care 2020, 8, e001450. [Google Scholar] [CrossRef] [PubMed]
- Umpierrez, G.E.; Isaacs, S.D.; Bazargan, N.; You, X.; Thaler, L.M.; Kitabchi, A.E. Hyperglycemia: An independent marker of in-hospital mortality in patients with undiagnosed diabetes. J. Clin. Endocrinol. Metab. 2002, 87, 978–982. [Google Scholar] [CrossRef] [PubMed]
- Henry, B.M.; Lippi, G. Chronic kidney disease is associated with severe coronavirus disease 2019 (COVID-19) infection. Int. Urol. Nephrol. 2020, 52, 1193–1194. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fanelli, V.; Fiorentino, M.; Cantaluppi, V.; Gesualdo, L.; Stallone, G.; Ronco, C.; Castellano, G. Acute kidney injury in SARS-CoV-2 infected patients. Crit. Care 2020, 24, 155. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Richardson, S.; Hirsch, J.S.; Narasimhan, M.; Crawford, J.M.; McGinn, T.; Davidson, K.W.; the Northwell, C.-R.C.; Barnaby, D.P.; Becker, L.B.; Chelico, J.D.; et al. Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area. JAMA 2020, 323, 2052–2059. [Google Scholar] [CrossRef]
- Zou, X.; Chen, K.; Zou, J.; Han, P.; Hao, J.; Han, Z. Single-cell RNA-seq data analysis on the receptor ACE2 expression reveals the potential risk of different human organs vulnerable to 2019-nCoV infection. Front. Med. 2020, 14, 185–192. [Google Scholar] [CrossRef] [Green Version]
- Ejaz, H.; Alsrhani, A.; Zafar, A.; Javed, H.; Junaid, K.; Abdalla, A.E.; Abosalif, K.O.A.; Ahmed, Z.; Younas, S. COVID-19 and comorbidities: Deleterious impact on infected patients. J. Infect. Public Health 2020, 13, 1833–1839. [Google Scholar] [CrossRef]
- Mahmoodpoor, A.; Hosseini, M.; Soltani-Zangbar, S.; Sanaie, S.; Aghebati-Maleki, L.; Saghaleini, S.H.; Ostadi, Z.; Hajivalili, M.; Bayatmakoo, Z.; Haji-Fatahaliha, M.; et al. Reduction and exhausted features of T lymphocytes under serological changes, and prognostic factors in COVID-19 progression. Mol. Immunol. 2021, 138, 121–127. [Google Scholar] [CrossRef]
- Zhang, X.; Wu, K.; Wang, D.; Yue, X.; Song, D.; Zhu, Y.; Wu, J. Nucleocapsid protein of SARS-CoV activates interleukin-6 expression through cellular transcription factor NF-kappaB. Virology 2007, 365, 324–335. [Google Scholar] [CrossRef] [Green Version]
- Fang, X.; Gao, J.; Zheng, H.; Li, B.; Kong, L.; Zhang, Y.; Wang, W.; Zeng, Y.; Ye, L. The membrane protein of SARS-CoV suppresses NF-kappaB activation. J. Med. Virol. 2007, 79, 1431–1439. [Google Scholar] [CrossRef]
- Ulhaq, Z.S.; Soraya, G.V. Interleukin-6 as a potential biomarker of COVID-19 progression. Med. Et Mal. Infect. 2020, 50, 382–383. [Google Scholar] [CrossRef]
- Zheng, M.; Wang, X.; Guo, H.; Fan, Y.; Song, Z.; Lu, Z.; Wang, J.; Zheng, C.; Dong, L.; Ma, Y.; et al. The Cytokine Profiles and Immune Response Are Increased in COVID-19 Patients with Type 2 Diabetes Mellitus. J. Diabetes Res. 2021, 2021, 9526701. [Google Scholar] [CrossRef]
- Lelis, D.F.; Freitas, D.F.; Machado, A.S.; Crespo, T.S.; Santos, S.H.S. Angiotensin-(1-7), Adipokines and Inflammation. Metab. Clin. Exp. 2019, 95, 36–45. [Google Scholar] [CrossRef]
- Ryan, D.H.; Ravussin, E.; Heymsfield, S. COVID 19 and the Patient with Obesity—The Editors Speak Out. Obesity 2020, 28, 847. [Google Scholar] [CrossRef] [Green Version]
- Gallo Marin, B.; Aghagoli, G.; Lavine, K.; Yang, L.; Siff, E.J.; Chiang, S.S.; Salazar-Mather, T.P.; Dumenco, L.; Savaria, M.C.; Aung, S.N.; et al. Predictors of COVID-19 severity: A literature review. Rev. Med. Virol. 2021, 31, 1–10. [Google Scholar] [CrossRef]
- Providencia, R.; Boveda, S.; Lambiase, P.; Defaye, P.; Algalarrondo, V.; Sadoul, N.; Piot, O.; Klug, D.; Perier, M.C.; Bouzeman, A.; et al. Prediction of Nonarrhythmic Mortality in Primary Prevention Implantable Cardioverter-Defibrillator Patients With Ischemic and Nonischemic Cardiomyopathy. JACC. Clin. Electrophysiol. 2015, 1, 29–37. [Google Scholar] [CrossRef] [PubMed]
- Bouleti, C.; Himbert, D.; Iung, B.; Alos, B.; Kerneis, C.; Ghodbane, W.; Messika-Zeitoun, D.; Brochet, E.; Fassa, A.A.; Depoix, J.P.; et al. Long-term outcome after transcatheter aortic valve implantation. Heart 2015, 101, 936–942. [Google Scholar] [CrossRef]
- Tuty Kuswardhani, R.A.; Henrina, J.; Pranata, R.; Anthonius Lim, M.; Lawrensia, S.; Suastika, K. Charlson comorbidity index and a composite of poor outcomes in COVID-19 patients: A systematic review and meta-analysis. Diabetes Metab. Syndr. 2020, 14, 2103–2109. [Google Scholar] [CrossRef]
- Varol, Y.; Hakoglu, B.; Kadri Cirak, A.; Polat, G.; Komurcuoglu, B.; Akkol, B.; Atasoy, C.; Bayramic, E.; Balci, G.; Ataman, S.; et al. The impact of charlson comorbidity index on mortality from SARS-CoV-2 virus infection and A novel COVID-19 mortality index: CoLACD. Int. J. Clin. Pract. 2021, 75, e13858. [Google Scholar] [CrossRef]
- Bannay, A.; Chaignot, C.; Blotiere, P.O.; Basson, M.; Weill, A.; Ricordeau, P.; Alla, F. The Best Use of the Charlson Comorbidity Index With Electronic Health Care Database to Predict Mortality. Med. Care 2016, 54, 188–194. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Fierro, M.L.; Rios-Jasso, J.; Garza-Veloz, I.; Reyes-Veyna, L.; Cerda-Luna, R.M.; Duque-Jara, I.; Galvan-Jimenez, M.; Ramirez-Hernandez, L.A.; Morales-Esquivel, A.; Ortiz-Castro, Y.; et al. The role of close contacts of COVID-19 patients in the SARS-CoV-2 transmission: An emphasis on the percentage of nonevaluated positivity in Mexico. Am. J. Infect. Control 2021, 49, 15–20. [Google Scholar] [CrossRef] [PubMed]
- Wagner, D.; Marsoner, K.; Tomberger, A.; Haybaeck, J.; Haas, J.; Werkgartner, G.; Cerwenka, H.; Bacher, H.; Mischinger, H.J.; Kornprat, P. Low skeletal muscle mass outperforms the Charlson Comorbidity Index in risk prediction in patients undergoing pancreatic resections. Eur. J. Surg. Oncol. J. Eur. Soc. Surg. Oncol. Br. Assoc. Surg. Oncol. 2018, 44, 658–663. [Google Scholar] [CrossRef] [PubMed]
- Baldwin, S.A.; Murray, D.M.; Shadish, W.R. Empirically supported treatments or type I errors? Problems with the analysis of data from group-administered treatments. J. Consult. Clin. Psychol. 2005, 73, 924–935. [Google Scholar] [CrossRef] [PubMed]
- Pals, S.L.; Wiegand, R.E.; Murray, D.M. Ignoring the group in group-level HIV/AIDS intervention trials: A review of reported design and analytic methods. AIDS 2011, 25, 989–996. [Google Scholar] [CrossRef]
- Quan, H.; Li, B.; Couris, C.M.; Fushimi, K.; Graham, P.; Hider, P.; Januel, J.M.; Sundararajan, V. Updating and validating the Charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am. J. Epidemiol. 2011, 173, 676–682. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jassal, S.V.; Schaubel, D.E.; Fenton, S.S. Baseline comorbidity in kidney transplant recipients: A comparison of comorbidity indices. Am. J. Kidney Dis. Off. J. Natl. Kidney Found. 2005, 46, 136–142. [Google Scholar] [CrossRef] [PubMed]
- Olsson, T.; Terent, A.; Lind, L. Charlson Comorbidity Index can add prognostic information to Rapid Emergency Medicine Score as a predictor of long-term mortality. Eur. J. Emerg. Med. Off. J. Eur. Soc. Emerg. Med. 2005, 12, 220–224. [Google Scholar] [CrossRef]
- Murray, S.B.; Bates, D.W.; Ngo, L.; Ufberg, J.W.; Shapiro, N.I. Charlson Index is associated with one-year mortality in emergency department patients with suspected infection. Acad. Emerg. Med. Off. J. Soc. Acad. Emerg. Med. 2006, 13, 530–536. [Google Scholar] [CrossRef]
- Frenkel, W.J.; Jongerius, E.J.; Mandjes-van Uitert, M.J.; van Munster, B.C.; de Rooij, S.E. Validation of the Charlson Comorbidity Index in acutely hospitalized elderly adults: A prospective cohort study. J. Am. Geriatr. Soc. 2014, 62, 342–346. [Google Scholar] [CrossRef]
- Shao, W.; Zhang, Z.; Zhang, J.; Feng, H.; Liang, C.; Liu, D. Charlson comorbidity index as a predictor of short-term outcomes after pulmonary resection. J. Thorac. Dis. 2020, 12, 6670–6679. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Z.; Peng, F.; Xu, B.; Zhao, J.; Liu, H.; Peng, J.; Li, Q.; Jiang, C.; Zhou, Y.; Liu, S.; et al. Risk factors of critical & mortal COVID-19 cases: A systematic literature review and meta-analysis. J. Infect. 2020, 81, e16–e25. [Google Scholar] [CrossRef]
- Mo, P.; Xing, Y.; Xiao, Y.; Deng, L.; Zhao, Q.; Wang, H.; Xiong, Y.; Cheng, Z.; Gao, S.; Liang, K.; et al. Clinical characteristics of refractory COVID-19 pneumonia in Wuhan, China. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2020, 73, e4208–e4213. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lighter, J.; Phillips, M.; Hochman, S.; Sterling, S.; Johnson, D.; Francois, F.; Stachel, A. Obesity in Patients Younger Than 60 Years Is a Risk Factor for COVID-19 Hospital Admission. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2020, 71, 896–897. [Google Scholar] [CrossRef] [Green Version]
- Kulcsar, K.A.; Coleman, C.M.; Beck, S.E.; Frieman, M.B. Comorbid diabetes results in immune dysregulation and enhanced disease severity following MERS-CoV infection. JCI Insight 2019, 4, e131774. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Muniyappa, R.; Gubbi, S. COVID-19 pandemic, coronaviruses, and diabetes mellitus. Am. J. Physiol. Endocrinol. Metab. 2020, 318, E736–E741. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yan, T.; Xiao, R.; Wang, N.; Shang, R.; Lin, G. Obesity and severe coronavirus disease 2019: Molecular mechanisms, paths forward, and therapeutic opportunities. Theranostics 2021, 11, 8234–8253. [Google Scholar] [CrossRef]
- Pranata, R.; Huang, I.; Lim, M.A.; Wahjoepramono, E.J.; July, J. Impact of cerebrovascular and cardiovascular diseases on mortality and severity of COVID-19-systematic review, meta-analysis, and meta-regression. J. Stroke Cereb. Dis. 2020, 29, 104949. [Google Scholar] [CrossRef] [PubMed]
- Yonas, E.; Alwi, I.; Pranata, R.; Huang, I.; Lim, M.A.; Gutierrez, E.J.; Yamin, M.; Siswanto, B.B.; Virani, S.S. Effect of heart failure on the outcome of COVID-19—A meta analysis and systematic review. Am. J. Emerg. Med. 2021, 46, 204–211. [Google Scholar] [CrossRef] [PubMed]
- Lim, M.A.; Huang, I.; Yonas, E.; Vania, R.; Pranata, R. A wave of non-communicable diseases following the COVID-19 pandemic. Diabetes Metab. Syndr. 2020, 14, 979–980. [Google Scholar] [CrossRef] [PubMed]
- Pranata, R.; Lim, M.A.; Yonas, E.; Vania, R.; Lukito, A.A.; Siswanto, B.B.; Meyer, M. Body mass index and outcome in patients with COVID-19: A dose-response meta-analysis. Diabetes Metab. 2021, 47, 101178. [Google Scholar] [CrossRef]
- Lim, M.A.; Pranata, R. Coronavirus disease 2019 (COVID-19) markedly increased mortality in patients with hip fracture—A systematic review and meta-analysis. J. Clin. Orthop. Trauma 2021, 12, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Austin, S.R.; Wong, Y.N.; Uzzo, R.G.; Beck, J.R.; Egleston, B.L. Why Summary Comorbidity Measures Such As the Charlson Comorbidity Index and Elixhauser Score Work. Med. Care 2015, 53, e65–e72. [Google Scholar] [CrossRef] [Green Version]
- Lee, S.J.; Lindquist, K.; Segal, M.R.; Covinsky, K.E. Development and validation of a prognostic index for 4-year mortality in older adults. JAMA 2006, 295, 801–808. [Google Scholar] [CrossRef] [Green Version]
- Wagner, D.P.; Draper, E.A. Acute physiology and chronic health evaluation (APACHE II) and Medicare reimbursement. Health Care Financ. Rev. 1984, 1984, 91–105. [Google Scholar]
- Knaus, W.A.; Draper, E.A.; Wagner, D.P.; Zimmerman, J.E. APACHE II: A severity of disease classification system. Crit. Care Med. 1985, 13, 818–829. [Google Scholar] [CrossRef] [PubMed]
- Le Gall, J.R.; Lemeshow, S.; Saulnier, F. A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study. JAMA 1993, 270, 2957–2963. [Google Scholar] [CrossRef] [PubMed]
- Lemeshow, S.; Teres, D.; Klar, J.; Avrunin, J.S.; Gehlbach, S.H.; Rapoport, J. Mortality Probability Models (MPM II) based on an international cohort of intensive care unit patients. JAMA 1993, 270, 2478–2486. [Google Scholar] [CrossRef]
- Lemeshow, S.; Le Gall, J.R. Modeling the severity of illness of ICU patients. A systems update. JAMA 1994, 272, 1049–1055. [Google Scholar] [CrossRef] [PubMed]
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C.R. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic Dis. 1987, 40, 373–383. [Google Scholar] [CrossRef]
- Gong, J.; Ou, J.; Qiu, X.; Jie, Y.; Chen, Y.; Yuan, L.; Cao, J.; Tan, M.; Xu, W.; Zheng, F.; et al. A Tool for Early Prediction of Severe Coronavirus Disease 2019 (COVID-19): A Multicenter Study Using the Risk Nomogram in Wuhan and Guangdong, China. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2020, 71, 833–840. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hu, X.; Deng, Y.; Wang, J.; Li, H.; Li, M.; Lu, Z. Short term outcome and risk factors for mortality in adults with critical severe acute respiratory syndrome (SARS). J. Huazhong Univ. Sci. Technology. Med. Sci. Hua Zhong Ke Ji Da Xue Xue Bao. Yi Xue Ying De Wen Ban Huazhong Keji Daxue Xuebao. Yixue Yingdewen Ban 2004, 24, 514–517. [Google Scholar] [CrossRef] [Green Version]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- King, J.T., Jr.; Yoon, J.S.; Rentsch, C.T.; Tate, J.P.; Park, L.S.; Kidwai-Khan, F.; Skanderson, M.; Hauser, R.G.; Jacobson, D.A.; Erdos, J.; et al. Development and validation of a 30-day mortality index based on pre-existing medical administrative data from 13,323 COVID-19 patients: The Veterans Health Administration COVID-19 (VACO) Index. PLoS ONE 2020, 15, e0241825. [Google Scholar] [CrossRef] [PubMed]
- Christensen, D.M.; Strange, J.E.; Gislason, G.; Torp-Pedersen, C.; Gerds, T.; Fosbol, E.; Phelps, M. Charlson Comorbidity Index Score and Risk of Severe Outcome and Death in Danish COVID-19 Patients. J. Gen. Intern. Med. 2020, 35, 2801–2803. [Google Scholar] [CrossRef] [PubMed]
- Iaccarino, G.; Grassi, G.; Borghi, C.; Ferri, C.; Salvetti, M.; Volpe, M. Age and Multimorbidity Predict Death Among COVID-19 Patients: Results of the SARS-RAS Study of the Italian Society of Hypertension. Hypertension 2020, 76, 366–372. [Google Scholar] [CrossRef]
- Ferroni, E.; Giorgi Rossi, P.; Spila Alegiani, S.; Trifiro, G.; Pitter, G.; Leoni, O.; Cereda, D.; Marino, M.; Pellizzari, M.; Fabiani, M.; et al. Survival of Hospitalized COVID-19 Patients in Northern Italy: A Population-Based Cohort Study by the ITA-COVID-19 Network. Clin. Epidemiol. 2020, 12, 1337–1346. [Google Scholar] [CrossRef]
- Rajgor, D.D.; Lee, M.H.; Archuleta, S.; Bagdasarian, N.; Quek, S.C. The many estimates of the COVID-19 case fatality rate. Lancet Infect. Dis. 2020, 20, 776–777. [Google Scholar] [CrossRef] [Green Version]
- Giacomelli, A.; Ridolfo, A.L.; Milazzo, L.; Oreni, L.; Bernacchia, D.; Siano, M.; Bonazzetti, C.; Covizzi, A.; Schiuma, M.; Passerini, M.; et al. 30-day mortality in patients hospitalized with COVID-19 during the first wave of the Italian epidemic: A prospective cohort study. Pharm. Res. 2020, 158, 104931. [Google Scholar] [CrossRef] [PubMed]
- Nachtigall, I.; Lenga, P.; Jozwiak, K.; Thurmann, P.; Meier-Hellmann, A.; Kuhlen, R.; Brederlau, J.; Bauer, T.; Tebbenjohanns, J.; Schwegmann, K.; et al. Clinical course and factors associated with outcomes among 1904 patients hospitalized with COVID-19 in Germany: An observational study. Clin. Microbiol. Infect. 2020, 26, 1663–1669. [Google Scholar] [CrossRef] [PubMed]
- Khalil, K.; Agbontaen, K.; McNally, D.; Love, A.; Mandalia, S.; Banya, W.; Starren, E.; Dhunnookchand, R.; Farne, H.; Morton, R.; et al. Clinical characteristics and 28-day mortality of medical patients admitted with COVID-19 to a central London teaching hospital. J. Infect. 2020, 81, e85–e89. [Google Scholar] [CrossRef]
- Zhang, Q.; Schultz, J.L.; Aldridge, G.M.; Simmering, J.E.; Narayanan, N.S. Coronavirus Disease 2019 Case Fatality and Parkinson’s Disease. Mov. Disord. 2020, 35, 1914–1915. [Google Scholar] [CrossRef] [PubMed]
- Galle, F.; Sabella, E.A.; Roma, P.; Da Molin, G.; Diella, G.; Montagna, M.T.; Ferracuti, S.; Liguori, G.; Orsi, G.B.; Napoli, C. Acceptance of COVID-19 Vaccination in the Elderly: A Cross-Sectional Study in Southern Italy. Vaccines 2021, 9, 1222. [Google Scholar] [CrossRef] [PubMed]
| Variable | Patients with COVID-19 and Obesity (n = 157) | Patients with COVID-19 without Obesity (n = 220) | Odds Ratio (95% CI) | p-Value |
|---|---|---|---|---|
| Risk factors | ||||
| Type 2 diabetes mellitus | 49 (31.2) | 49 (22.2) | 1.583 (0.996–2.517) | 0.05 |
| COPD | 10 (6.3) | 16 (10.1) | 0.867 (0.383–1.965) | 0.733 |
| Tobaccoism | 12 (7.6) | 28 (12.7) | 0.567 (0.279–1.154) | 0.114 |
| Chronic renal disease | 6 (3.8) | 3(1.3) | 2.874 (0.708–11.671) | 0.123 |
| Heart disease | 3 (1.9) | 10 (4.5) | 0.409 (0.111–1.511) | 0.167 |
| HIV/AIDS | 0 (0.0) | 1(0.4) | N.A. | - |
| Asthma | 4 (2.5) | 4 (1.8) | 1.412 (0.348–5.732) | 0.628 |
| Immunosuppression | 10 (6.3) | 12 (5.4) | 1.179 (0.496–2.802) | 0.709 |
| Hypertension | 72 (45.8) | 71 (32.2) | 1.778 (1.165–2.712) | 0.007 |
| Symptoms | ||||
| Anosmia | 62 (39.4) | 83 (37.7) | 1.077 (0.708–1.640) | 0.729 |
| Dysgeusia | 62 (39.4) | 72 (32.7) | 1.342 (0.876–2.055) | 0.176 |
| Cyanosis | 42 (26.7) | 50 (22.7) | 1.242 (0.773–1.994) | 0.370 |
| Conjunctivitis | 8 (5.0) | 17 (8.5) | 0.641 (0.270–1.525) | 0.311 |
| Abdominal pain | 39 (24.8) | 44 (20.0) | 1.322 (0.810–2.158) | 0.263 |
| Vomiting | 23 (14.6) | 25 (11.3) | 1.339 (0.729–2.458) | 0.345 |
| Polypnea | 101 (64.3) | 110 (50.0) | 1.804 (1.185–2.745) | 0.006 |
| Fever | 136 (86.6) | 179 (81.3) | 1.483 (0.838–2.626) | 0.174 |
| Myalgia | 113 (71.9) | 154 (70.0) | 1.101 (0.700–1.730) | 0.678 |
| Arthralgia | 102 (64.9) | 136 (61.8) | 1.145 (0.748–1.754) | 0.532 |
| Rhinorrhea | 37 (23.5) | 61 (27.7) | 0.804 (0.501–1.289) | 0.364 |
| Attack to the general state | 137 (87.2) | 176 (80.0) | 1.713 (0.965–3.040) | 0.064 |
| Headache | 126 (80.2) | 186 (84.5) | 0.743 (0.434–1.271) | 0.277 |
| Calophries | 83 (52.8) | 110 (50.0) | 1.122 (.744–1.690) | 0.583 |
| Diarrhea | 40 (25.4) | 53 (24.0) | 1.077 (0.671–1.730) | 0.758 |
| Thoracic pain | 103 (65.6) | 120 (54.4) | 1.590 (1.041–2.426) | 0.031 |
| Cough | 140 (89.1) | 189 (85.9) | 1.351 (0.719–2.538) | 0.349 |
| Odynophagia | 83 (52.8) | 115 (52.2) | 1.024 (.680–1.543) | 0.909 |
| Dyspnea | 132 (84.0) | 158 (71.8) | 2.072 (1.233–3.480) | 0.005 |
| Irritability | 11 (7.0) | 13 (5.9) | 1.200 (0.523–2.752) | 0.667 |
| Mechanical ventilation (Intubation) | 28 (17.8) | 17 (7.7) | 2.592 (1.364–4.924) | 0.003 |
| Age Group (Years) | Patients Who Died of COVID-19 (n = 132) | Charlson Comorbidity Index * | COVID-19 Survivors (n = 220) | Charlson Comorbidity Index * | p-Value |
|---|---|---|---|---|---|
| 18–30 | 4 | 2.9 ± 0.65 | 10 | 1.7 ± 0.86 | 0.013 |
| 31–40 | 4 | 3.3 ± 1.40 | 35 | 1.75 ± 0.37 | 0.008 |
| 41–50 | 21 | 7.1 ± 3.46 | 43 | 4.8 ± 0.73 | 0.003 |
| 51–60 | 34 | 30.02 ± 7.55 | 53 | 10.11 ± 1.4 | 0.005 |
| 61–70 | 30 | 42.12 ± 5.58 | 48 | 25.4 ± 4.15 | 0.007 |
| 71–80 | 22 | 63.5 ± 11.37 | 17 | 29.4 ± 11.03 | 0.001 |
| 81–90 | 15 | 61.5 ± 14.30 | 11 | 62.22 ± 11.33 | 0.661 |
| 91–100 | 2 | 88.19 ± 55.46 | 3 | 78.54 ± 10.30 | 0.020 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gutierrez-Camacho, J.R.; Avila-Carrasco, L.; Murillo-Ruíz-Esparza, A.; Garza-Veloz, I.; Araujo-Espino, R.; Martinez-Vazquez, M.C.; Trejo-Ortiz, P.M.; Rodriguez-Sanchez, I.P.; Delgado-Enciso, I.; Castañeda-López, M.E.; et al. Evaluation of the Potential Risk of Mortality from SARS-CoV-2 Infection in Hospitalized Patients According to the Charlson Comorbidity Index. Healthcare 2022, 10, 362. https://doi.org/10.3390/healthcare10020362
Gutierrez-Camacho JR, Avila-Carrasco L, Murillo-Ruíz-Esparza A, Garza-Veloz I, Araujo-Espino R, Martinez-Vazquez MC, Trejo-Ortiz PM, Rodriguez-Sanchez IP, Delgado-Enciso I, Castañeda-López ME, et al. Evaluation of the Potential Risk of Mortality from SARS-CoV-2 Infection in Hospitalized Patients According to the Charlson Comorbidity Index. Healthcare. 2022; 10(2):362. https://doi.org/10.3390/healthcare10020362
Chicago/Turabian StyleGutierrez-Camacho, Jose Roberto, Lorena Avila-Carrasco, Alberto Murillo-Ruíz-Esparza, Idalia Garza-Veloz, Roxana Araujo-Espino, Maria Calixta Martinez-Vazquez, Perla M. Trejo-Ortiz, Iram Pablo Rodriguez-Sanchez, Iván Delgado-Enciso, Maria E. Castañeda-López, and et al. 2022. "Evaluation of the Potential Risk of Mortality from SARS-CoV-2 Infection in Hospitalized Patients According to the Charlson Comorbidity Index" Healthcare 10, no. 2: 362. https://doi.org/10.3390/healthcare10020362
APA StyleGutierrez-Camacho, J. R., Avila-Carrasco, L., Murillo-Ruíz-Esparza, A., Garza-Veloz, I., Araujo-Espino, R., Martinez-Vazquez, M. C., Trejo-Ortiz, P. M., Rodriguez-Sanchez, I. P., Delgado-Enciso, I., Castañeda-López, M. E., Gamón-Madrid, A., & Martinez-Fierro, M. L. (2022). Evaluation of the Potential Risk of Mortality from SARS-CoV-2 Infection in Hospitalized Patients According to the Charlson Comorbidity Index. Healthcare, 10(2), 362. https://doi.org/10.3390/healthcare10020362








