The Effects of Motor Imagery on Pain in Lower Limb Sports Injuries: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Eligibility Criteria
2.2. Search Strategy
2.3. Eligibility Assessment
2.4. Outcome Measures
2.5. Data Extraction and Quality Assessment
2.6. Analysis
3. Results
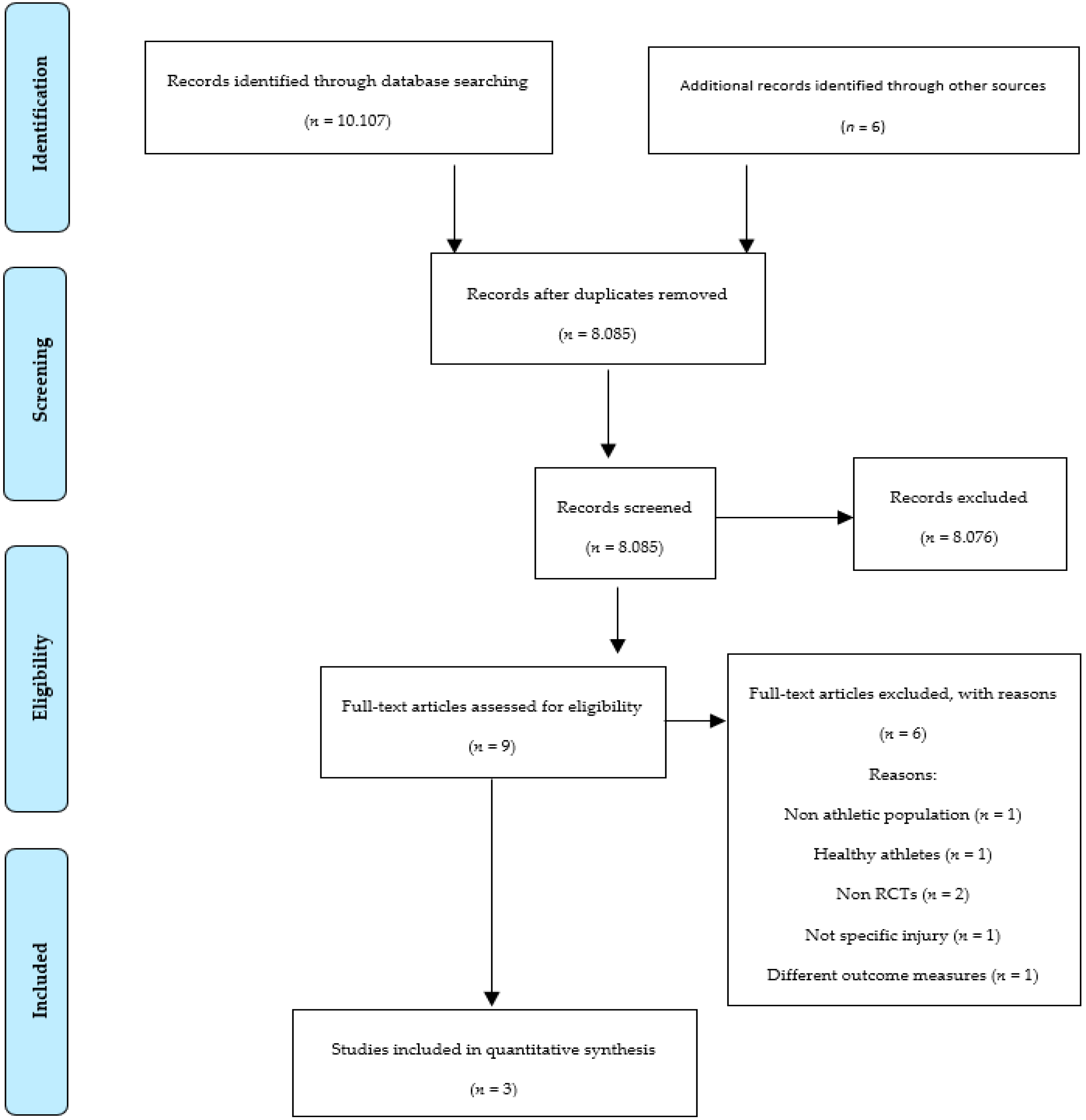
3.1. Study Selection
3.2. Study Characteristics
3.3. Methodological Quality
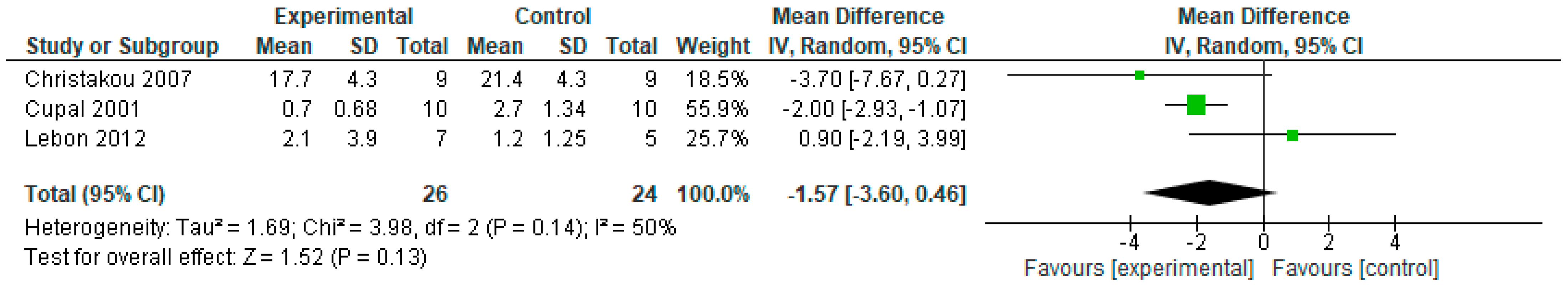
3.4. Effects of Intervention on Pain
4. Discussion
4.1. Clinical Implications
4.2. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Rodriguez, R.M.; Marroquin, A.; Cosby, N. Reducing fear of reinjury and pain perception in athletes with first-time anterior cruciate ligament reconstructions by implementing imagery training. J. Sport Rehabil. 2019, 28, 385–389. [Google Scholar] [CrossRef] [PubMed]
- Zach, S.; Dobersek, U.; Filho, E.; Inglis, V.; Tenenbaum, G. A meta-analysis of mental imagery effects on post-injury functional mobility, perceived pain, and self-efficacy. Psychol. Sport Exerc. 2018, 34, 79–87. [Google Scholar] [CrossRef]
- Wilson, B.; Bialocerkowski, A. The effects of kinesiotape applied to the lateral aspect of the ankle: Relevance to ankle sprains—A systematic review. PLoS ONE 2015, 10, e0124214. [Google Scholar] [CrossRef] [PubMed]
- Dizon, J.M.R.; Reyes, J.J.B. A systematic review on the effectiveness of external ankle supports in the prevention of inversion ankle sprains among elite and recreational players. J. Sci. Med. Sport 2010, 13, 309–317. [Google Scholar] [CrossRef] [PubMed]
- Terada, M.; Pietrosimone, B.G.; Gribble, P.A. Therapeutic interventions for increasing ankle dorsiflexion after ankle sprain: A systematic review. J. Athl. Train. 2013, 48, 696–709. [Google Scholar] [CrossRef] [PubMed]
- Dawson, M.A.; Hamson-Utley, J.J.; Hansen, R.; Olpin, M. Examining the effectiveness of psychological strategies on physiologic markers: Evidence-based suggestions for holistic care of the athlete. J. Athl. Train. 2014, 49, 331–337. [Google Scholar] [CrossRef] [PubMed]
- Hammoudi-Nassib, S.; Chtara, M.; Nassib, S.; Briki, W.; Hammoudi-Riahi, S.; Tod, D.; Chamari, K. Time interval moderates the relationship between psyching-up and actual sprint performance. J. Strength Cond. Res. 2014, 28, 3245–3254. [Google Scholar] [CrossRef]
- Treadwell, K.R.H.; Kendall, P.C. Self-talk in youth with anxiety disorders: States of mind, content specificity, and treatment outcome. J. Consult. Clin. Psychol. USA Psychol. Assoc. 1996, 64, 941–950. [Google Scholar] [CrossRef]
- Callicott, K.J.; Park, H. Effects of Self-Talk on Academic Engagement and Academic Responding. Behav. Disord. 2003, 29, 48–64. [Google Scholar] [CrossRef]
- Vella, S.A.; Swann, C.; Boydell, K.M.; Eckermann, S.; Fogarty, A.; Hurley, D.; Liddle, S.K.; Lonsdale, C.; Sanders, T.; Schweickle, M.J.; et al. Sports-based mental health promotion in Australia: Formative evaluation. Psychol. Sport Exerc. 2019, 45, 101560. [Google Scholar] [CrossRef]
- Sanders, M.R.; Shepherd, R.W.; Cleghorn, G.; Woolford, H. The Treatment of Recurrent Abdominal Pain in Children: A Controlled Comparison of Cognitive-Behavioral Family Intervention and Standard Pediatric Care. J. Consult. Clin. Psychol. 1994, 62, 306–314. [Google Scholar] [CrossRef] [PubMed]
- Kaur, J.; Ghosh, S.; Sahani, A.K.; Sinha, J.K. Mental Imagery as a Rehabilitative Therapy for Neuropathic Pain in People With Spinal Cord Injury: A Randomized Controlled Trial. Neurorehabilit. Neural Repair 2020, 34, 1038–1049. [Google Scholar] [CrossRef] [PubMed]
- Posadzki, P.; Ernst, E. Guided imagery for musculoskeletal pain: A systematic review. Clin. J. Pain 2011, 27, 648–653. [Google Scholar] [CrossRef] [PubMed]
- Kaur, J.; Ghosh, S.; Sahani, A.K.; Sinha, J.K. Mental imagery training for treatment of central neuropathic pain: A narrative review. Acta Neurol. Belg. 2019, 119, 175–186. [Google Scholar] [CrossRef]
- Thieme, H.; Morkisch, N.; Rietz, C.; Dohle, C.; Borgetto, B. The efficacy of movement representation techniques for treatment of limb pain—A systematic review and meta-analysis. J. Pain 2016, 17, 167–180. [Google Scholar] [CrossRef]
- Breckenridge, J.D.; McAuley, J.H.; Moseley, G.L.; Ginn, K.A. Is implicit motor imagery altered in people with shoulder pain? The shoulder left/right judgement task. Musculoskelet. Sci. Pract. 2020, 48, 102159. [Google Scholar] [CrossRef]
- Timpka, T.; Jacobsson, J.; Bickenbach, J.; Finch, C.F.; Ekberg, J.; Nordenfelt, L. What is a sports injury? Sport. Med. 2014, 44, 423–428. [Google Scholar] [CrossRef]
- Moseley, G.L.; Flor, H. Targeting cortical representations in the treatment of chronic pain: A review. Neurorehabilit. Neural Repair 2012, 26, 646–652. [Google Scholar] [CrossRef]
- Cuenca-Martínez, F.; Reina-Varona, Á.; Castillo-García, J.; La Touche, R.; Angulo-Díaz-Parreño, S.; Suso-Martí, L. Pain relief by movement representation strategies: An umbrella and mapping review with meta-meta-analysis of motor imagery, action observation and mirror therapy. Eur. J. Pain 2022, 26, 284–309. [Google Scholar] [CrossRef]
- Cressman, J.M.; Dawson, K.A. Evaluation of the use of healing imagery in athletic injury rehabilitation. J. Imag. Res. Sport Phys. Act. 2011, 6. [Google Scholar] [CrossRef]
- Ferrer-Peña, R.; Cuenca-Martínez, F.; Romero-Palau, M.; Flores-Román, L.M.; Arce-Vázquez, P.; Varangot-Reille, C.; Suso-Martí, L. Effects of motor imagery on strength, range of motion, physical function, and pain intensity in patients with total knee arthroplasty: A systematic review and meta-analysis. Braz. J. Phys. Ther. 2021, 25, 698–708. [Google Scholar] [CrossRef] [PubMed]
- Da Yap, B.W.; Lim, E.C.W. The Effects of Motor Imagery on Pain and Range of Motion in Musculoskeletal Disorders. Clin. J. Pain 2019, 35, 87–99. [Google Scholar] [CrossRef] [PubMed]
- Ferreira Dias Kanthack, T.; Guillot, A.; Saboul, D.; Debarnot, U.; Di Rienzo, F. Breathing with the mind: Effects of motor imagery on breath-hold performance. Physiol. Behav. 2019, 208, 27–29. [Google Scholar]
- Williams, S.E. Comparing movement imagery and action observation as techniques to increase imagery ability. Psychol. Sport Exerc. 2019, 44, 99–106. [Google Scholar] [CrossRef]
- Jones, L.; Stuth, G. The uses of mental imagery in athletics: An overview. Appl. Prev. Psychol. 1997, 6, 101–115. [Google Scholar] [CrossRef]
- Slimani, M.; Tod, D.; Chaabene, H.; Miarka, B.; Chamari, K. Effects of mental imagery on muscular strength in healthy and patient participants: A systematic review. J. Sport. Sci. Med. 2016, 15, 434–450. [Google Scholar]
- Mouthon, A.; Ruffieux, J.; Wälchli, M.; Keller, M.; Taube, W. Task-dependent changes of corticospinal excitability during observation and motor imagery of balance tasks. Neuroscience 2015, 303, 535–543. [Google Scholar] [CrossRef]
- MacIntyre, T.E.; Madan, C.R.; Moran, A.P.; Collet, C.; Guillot, A. Motor imagery, performance and motor rehabilitation. Prog. Brain Res. 2018, 240, 141–159. [Google Scholar]
- Robin, N.; Toussaint, L.; Charles-Charlery, C.; Coudevylle, G.R. Free throw performance in non-expert basketball players: The effect of dynamic motor imagery combined with action observation. Learn. Motiv. 2019, 68, 101595. [Google Scholar] [CrossRef]
- Javdaneh, N.; Molayei, F.; Kamranifraz, N. Effect of adding motor imagery training to neck stabilization exercises on pain, disability and kinesiophobia in patients with chronic neck pain. Complement. Ther. Clin. Pract. 2021, 42, 101263. [Google Scholar] [CrossRef]
- Salik Sengul, Y.; Kaya, N.; Yalcinkaya, G.; Kirmizi, M.; Kalemci, O. The effects of the addition of motor imagery to home exercises on pain, disability and psychosocial parameters in patients undergoing lumbar spinal surgery: A randomized controlled trial. Explore 2021, 17, 334–339. [Google Scholar] [CrossRef] [PubMed]
- Opsommer, E.; Chevalley, O.; Korogod, N. Motor imagery for pain and motor function after spinal cord injury: A systematic review. Spinal Cord 2020, 58, 262–274. [Google Scholar] [CrossRef]
- Méndez-Rebolledo, G.; Gatica-Rojas, V.; Torres-Cueco, R.; Albornoz-Verdugo, M.; Guzmán-Muñoz, E. Update on the effects of graded motor imagery and mirror therapy on complex regional pain syndrome type 1: A systematic review. J. Back Musculoskelet. Rehabil. 2017, 30, 441–449. [Google Scholar] [CrossRef] [PubMed]
- Multhaupt, G.; Beuth, J. The use of imagery in athletic injury rehabilitation. A systematic review. Dtsch. Z. Sportmed. 2018, 69, 57–64. [Google Scholar] [CrossRef]
- Li, R.Q.; Li, Z.M.; Tan, J.Y.; Chen, G.L.; Lin, W.Y. Effects of motor imagery on walking function and balance in patients after stroke: A quantitative synthesis of randomized controlled trials. Complement. Ther. Clin. Pract. 2017, 28, 75–84. [Google Scholar] [CrossRef]
- Iskandar, I.; Patak, A.A. The significance of Mendeley usage on the accuracy of citation and references. Int. J. Humanit. Innov. 2019, 2, 108–114. [Google Scholar] [CrossRef]
- Hølen, J.C.; Hjermstad, M.J.; Loge, J.H.; Fayers, P.M.; Caraceni, A.; De Conno, F.; Forbes, K.; Fürst, C.J.; Radbruch, L.; Kaasa, S. Pain Assessment Tools: Is the Content Appropriate for Use in Palliative Care? J. Pain Symptom Manag. 2006, 32, 567–580. [Google Scholar] [CrossRef]
- Maher, C.G.; Sherrington, C.; Herbert, R.D.; Moseley, A.M.; Elkins, M. Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys. Ther. 2003, 83, 713–721. [Google Scholar] [CrossRef]
- Maddison, R.; Prapavessis, H.; Clatworthy, M.; Hall, C.; Foley, L.; Harper, T.; Cupal, D.; Brewer, B. Guided imagery to improve functional outcomes post-anterior cruciate ligament repair: Randomized-controlled pilot trial. Scand. J. Med. Sci. Sport. 2012, 22, 816–821. [Google Scholar] [CrossRef]
- Law, B.; Ma, M.; Driediger, M. Imagery use, perceived pain, limb functioning and satisfaction in athletic injury rehabilitation Children’s imagery use in PE View project Self-Control of Learning View project. N. Z. J. Physiother. 2006, 34, 10–16. [Google Scholar]
- Ismail, S.A.; Simic, M.; Stanton, T.R.; Pappas, E. Motor imagery in high-functioning individuals with chronic anterior cruciate ligament deficiency: A cross-sectional study. Knee 2019, 26, 545–554. [Google Scholar] [CrossRef]
- Wesch, N.; Callow, N.; Hall, C.; Pope, J.P. Imagery and self-efficacy in the injury context. Psychol. Sport Exerc. 2016, 24, 72–81. [Google Scholar] [CrossRef]
- Christakou, A.; Zervas, Y.; Lavallee, D. The adjunctive role of imagery on the functional rehabilitation of a grade II ankle sprain. Hum. Mov. Sci. 2007, 26, 141–154. [Google Scholar] [CrossRef] [PubMed]
- Christakou, A.; Zervas, Y. The effectiveness of imagery on pain, edema, and range of motion in athletes with a grade II ankle sprain. Phys. Ther. Sport 2007, 8, 130–140. [Google Scholar] [CrossRef]
- Cupal, D.; Brewer, B. Relaxation and Imagery on Knee Strength and Re-Injury. Rehabil. Phychol. 2001, 46, 28–43. [Google Scholar] [CrossRef]
- Lebon, F.; Guillot, A.; Collet, C. Increased muscle activation following motor imagery during the rehabilitation of the anterior cruciate ligament. Appl. Psychophysiol. Biofeedback 2012, 37, 45–51. [Google Scholar] [CrossRef]
- Kwekkeboom, K.L.; Kneip, J.; Pearson, L. A pilot study to predict success with guided imagery for cancer pain. Pain Manag. Nurs. 2003, 4, 112–123. [Google Scholar] [CrossRef]
- Barbin, J.; Seetha, V.; Casillas, J.M.; Paysant, J.; Pérennou, D. The effects of mirror therapy on pain and motor control of phantom limb in amputees: A systematic review. Ann. Phys. Rehabil. Med. 2016, 59, 270–275. [Google Scholar] [CrossRef]
- Machado, D.C.D.; Lima, G.C.; Souza Dos Santos, R.S.; Bezerra Ramos, A.J.; De Sousa, C.C.M.; Moreira Dos Santos, R.P.; Coelho, K.K.; Cagy, M.; Orsini, M.; Bastos, V.H. Comparative analysis electroencephalographic of alpha, beta and gamma bands of a healthy individual and one with hemiparesis. J. Phys. Ther. Sci. 2014, 26, 801–804. [Google Scholar] [CrossRef][Green Version]
- Moseley, G.L. Graded motor imagery for pathologic pain: A randomized controlled trial. Neurology 2006, 67, 2129–2134. [Google Scholar] [CrossRef]
- Kho, A.Y.; Liu, K.P.Y.; Chung, R.C.K. Meta-analysis on the effect of mental imagery on motor recovery of the hemiplegic upper extremity function. Aust. Occup. Ther. J. 2014, 61, 38–48. [Google Scholar] [CrossRef] [PubMed]
- Morioka, S.; Osumi, M.; Nishi, Y.; Ishigaki, T.; Ishibashi, R.; Sakauchi, T.; Takamura, Y.; Nobusako, S. Motor-imagery ability and function of hemiplegic upper limb in stroke patients. Ann. Clin. Transl. Neurol. 2019, 6, 596–604. [Google Scholar] [CrossRef] [PubMed]
- Dickstein, R.; Deutsch, J.E. Physical Therapist Practice. Phys. Ther. 2007, 87, 942–953. [Google Scholar] [CrossRef] [PubMed]
- McArdle, S. Psychological rehabilitation from anterior cruciate ligament-medial collateral ligament reconstructive surgery: A case study. Sport. Health 2010, 2, 73–77. [Google Scholar] [CrossRef] [PubMed]
- Gignac, M.A.M.; Cao, X.; Ramanathan, S.; White, L.M.; Hurtig, M.; Kunz, M.; Marks, P.H. Perceived personal importance of exercise and fears of re-injury: A longitudinal study of psychological factors related to activity after anterior cruciate ligament reconstruction. BMC Sport. Sci. Med. Rehabil. 2015, 7, 4. [Google Scholar] [CrossRef]
- Coslett, H.B.; Medina, J.; Kliot, D.; Burkey, A. Mental motor imagery and chronic pain: The foot laterality task. J. Int. Neuropsychol. Soc. 2010, 16, 603–612. [Google Scholar] [CrossRef] [PubMed]
- Di Rienzo, F.; Joassy, P.; Ferreira Dias Kanthack, T.; Moncel, F.; Mercier, Q.; Collet, C.; Guillot, A. Stabilometric Correlates of Motor and Motor Imagery Expertise. Front. Hum. Neurosci. 2022, 15, 741709. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. Syst. Rev. 2021, 10, 89. [Google Scholar] [CrossRef]
| Study | Age; n; Sex; Athletic Level; | Injury | Methods | Intervention | Results | PEDro Scale |
|---|---|---|---|---|---|---|
| 18–30 yrs; n = 18; M; at least 2 years of athletic experience | Ankle sprain grade II | Randomly allocated into 2 groups: 1. RI (n = 9), 2. CNTL, (n = 9), (Physical Therapy Program) | RI protocol 12 sessions/ 4 weeks 45 min each session | VAS: No significant statistical difference in the RI condition compared with the CNTL condition | 7/11 |
| 18–50 yrs; n = 30; M = 16, F = 14; recreational and competitive athletes | ACL reconstructive surgery | Randomly allocated into 3 groups: 1. RGI (n = 10), 2. PL (attention, encouragement and support), (n = 10), 3. CNTL Group (Physical Therapy Program) | RGI protocol 10 sessions every 2 weeks apart over 6 months/10–15 min (visual, kinesthetic, motivational and healing imagery) | NRS: Significant statistical difference in RGI condition compared with the PL and the CNTL condition | 7/11 |
| 18–40 yrs; n = 12; M = 10, F = 2; recreational and competitive athletes | ACL reconstructive surgery | Randomly allocated into 2 groups: 1. KI (n = 7), 2. CNTL, (n = 5), (Physical Therapy Program) | KI protocol 12 sessions/5 weeks every second day/15 min each session | VAS: No significant statistical difference in the KI condition compared with the control condition | 9/11 |
| Study | Eligibility Criteria | Randomization | Allocation Concealed | Baseline Criteria | Participants Blinded | Therapist Blinded | Assessor Blinded | Minimum of 85% at Follow-Up | Statistical Analysis | Analysis between Groups | Point and Variance Data | Total |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Christakou and Zervas [44] | Y | Y | Y | U | N | N | Y | U | Y | Y | Y | 7/11 |
| Cupal and Brewer [45] | Y | Y | N | Y | N | N | N | Y | Y | Y | Y | 7/11 |
| Lebon et al. [46] | Y | Y | Y | Y | N | N | Y | Y | Y | Y | Y | 9/11 |
| Certainty Assessment | No. of Patients | Effect | Certainty | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| No. of Studies | Study Design | Risk of Bias | Inconsistency | Indirectness | Imprecision | Other Considerations | Motor Imagery | Control | Absolute (95% CI) | |
| Christakou and Zervas [44] Cupal and Brewer [45] Lebon, Guillot and Collet [46] | randomized trials | not serious | serious b | not serious | serious a | none | 26 | 24 | MD −1.57 (−3.60 to 0.46) | ⨁⨁◯◯ LOW |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Plakoutsis, G.; Paraskevopoulos, E.; Zavvos, A.; Papandreou, M. The Effects of Motor Imagery on Pain in Lower Limb Sports Injuries: A Systematic Review and Meta-Analysis. Healthcare 2022, 10, 2545. https://doi.org/10.3390/healthcare10122545
Plakoutsis G, Paraskevopoulos E, Zavvos A, Papandreou M. The Effects of Motor Imagery on Pain in Lower Limb Sports Injuries: A Systematic Review and Meta-Analysis. Healthcare. 2022; 10(12):2545. https://doi.org/10.3390/healthcare10122545
Chicago/Turabian StylePlakoutsis, George, Eleftherios Paraskevopoulos, Athanasios Zavvos, and Maria Papandreou. 2022. "The Effects of Motor Imagery on Pain in Lower Limb Sports Injuries: A Systematic Review and Meta-Analysis" Healthcare 10, no. 12: 2545. https://doi.org/10.3390/healthcare10122545
APA StylePlakoutsis, G., Paraskevopoulos, E., Zavvos, A., & Papandreou, M. (2022). The Effects of Motor Imagery on Pain in Lower Limb Sports Injuries: A Systematic Review and Meta-Analysis. Healthcare, 10(12), 2545. https://doi.org/10.3390/healthcare10122545








