Tactile Myography: An Off-Line Assessment of Able-Bodied Subjects and One Upper-Limb Amputee
Abstract
1. Introduction
Related Work
2. Materials and Methods
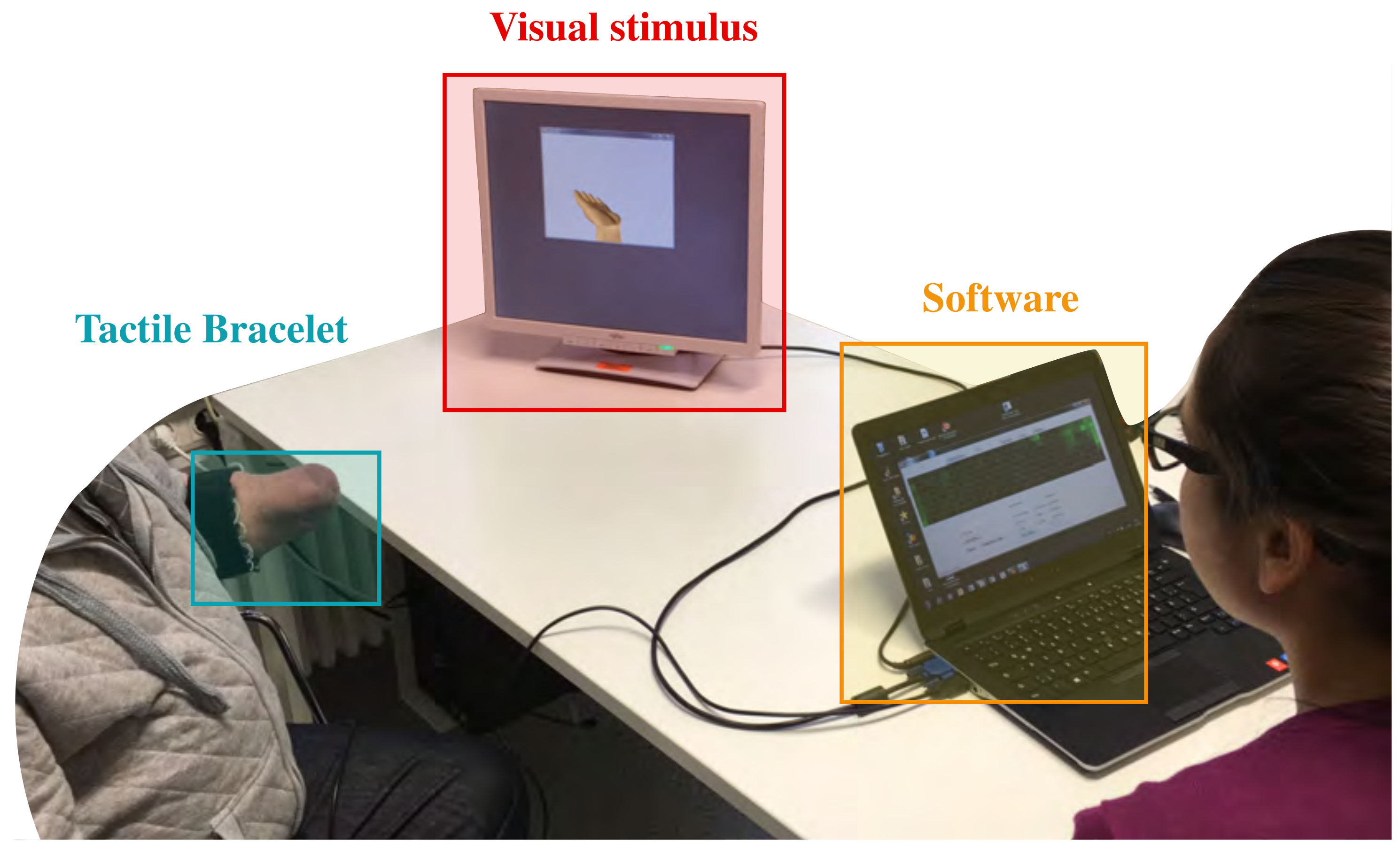
2.1. Experimental Setup
2.1.1. Tactile Bracelet
2.1.2. Visual Stimulus
2.2. Participants
2.3. Experimental Protocol
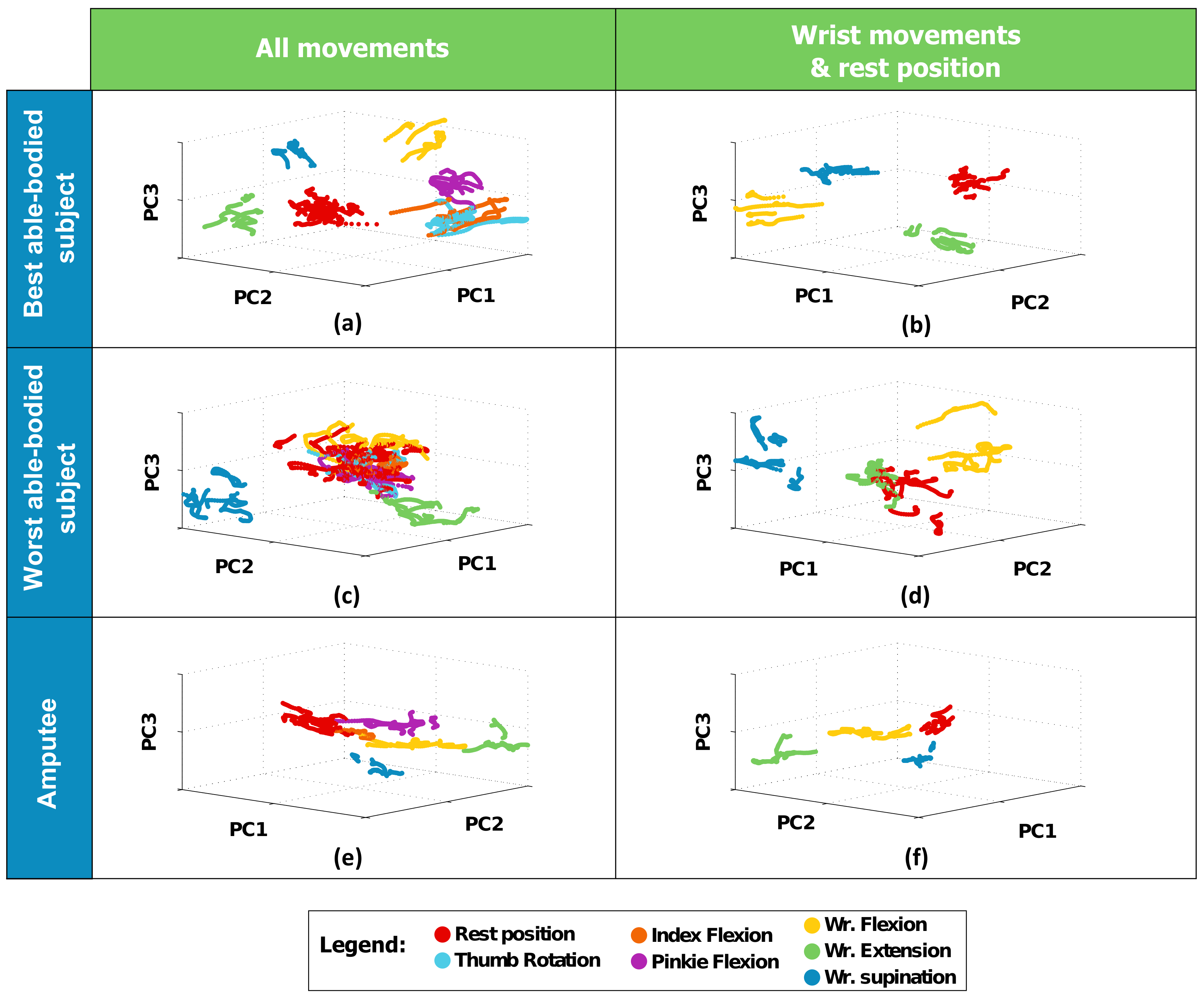
2.4. Data Analysis
3. Results
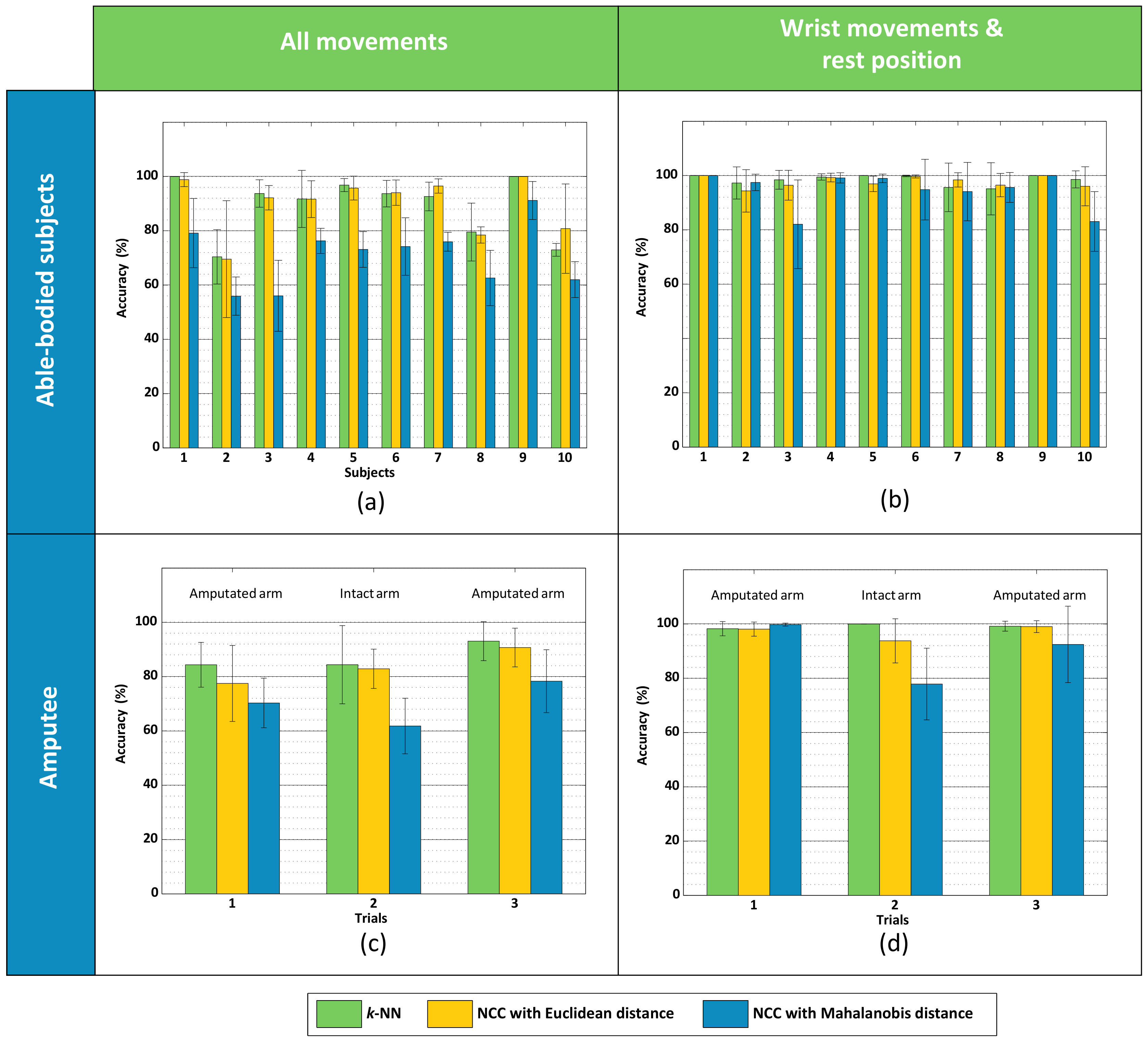
3.1. Experiment #1 (Able-Bodied Subjects)
3.2. Experiment #2 (Amputee)
4. Discussion
4.1. Tactile Myography for Myocontrol
4.2. What This Study Shows
4.3. Final Remarks and Future Work
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Biddiss, E.; Chau, T. Upper-limb prosthetics: Critical factors in device abandonment. Am. J. Phys. Med. Rehabil. 2007, 86, 977–987. [Google Scholar] [CrossRef] [PubMed]
- Peerdeman, B.; Boere, D.; Witteveen, H.; in ’t Veld, R.H.; Hermens, H.; Stramigioli, S.; Rietman, H.; Veltink, P.; Misra, S. Myoelectric forearm prostheses: State of the art from a user-centered perspective. J. Rehabil. Res. Dev. 2011, 48, 719–738. [Google Scholar] [CrossRef] [PubMed]
- Engdahl, S.M.; Christie, B.P.; Kelly, B.; Davis, A.; Chestek, C.A.; Gates, D.H. Surveying the interest of individuals with upper limb loss in novel prosthetic control techniques. J. NeuroEng. Rehabil. 2015, 12, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Micera, S.; Carpaneto, J.; Raspopovic, S. Control of hand prostheses using peripheral information. IEEE Rev. Biomed. Eng. 2010, 3, 48–68. [Google Scholar] [CrossRef] [PubMed]
- Maat, B.; Smit, G.; Plettenburg, D.; Breedveld, P. Passive prosthetic hands and tools: A literature review. Prosthet. Orthot. Int. 2018, 42, 66–74. [Google Scholar] [CrossRef] [PubMed]
- Schweitzer, W.; Thali, M.J.; Egger, D. Case-study of a user-driven prosthetic arm design: Bionic hand versus customized body-powered technology in a highly demanding work environment. J. NeuroEng. Rehabil. 2018, 15, 1. [Google Scholar] [CrossRef] [PubMed]
- Østlie, K.; Lesjø, I.M.; Franklin, R.J.; Garfelt, B.; Skjeldal, O.H.; Magnus, P. Prosthesis rejection in acquired major upper-limb amputees: A population-based survey. Disabil. Rehabil. Assist. Technol. 2012, 7, 294–303. [Google Scholar]
- Kyberd, P.J.; Hill, W. Survey of upper limb prosthesis users in Sweden, the United Kingdom and Canada. Prosthet. Orthot. Int. 2011, 35, 234–241. [Google Scholar] [CrossRef] [PubMed]
- i-LIMB Quantum. Available online: www.touchbionics.com/products/active-prostheses/i-limb-quantum (accessed on 22 March 2018).
- Fougner, A.; Stavdahl, Ø.; Kyberd, P.J.; Losier, Y.G.; Parker, P.A. Control of Upper Limb Prostheses: Terminology and Proportional Myoelectric Control - A Review. IEEE Trans. Neur. Syst. Rehab. Eng. 2012, 20, 663–677. [Google Scholar] [CrossRef] [PubMed]
- Jiang, N.; Dosen, S.; Müller, K.R.; Farina, D. Myoelectric control of artificial limbs: Is there the need for a change of focus? IEEE Signal Process. Mag. 2012, 29, 149–152. [Google Scholar] [CrossRef]
- Castellini, C.; Artemiadis, P.; Wininger, M.; Ajoudani, A.; Alimusaj, M.; Bicchi, A.; Caputo, B.; Craelius, W.; Dosen, S.; Englehart, K.; et al. Proceedings of the first workshop on Peripheral Machine Interfaces: Going beyond traditional surface electromyography. Front. Neurorobot. 2014, 8, 22. [Google Scholar] [CrossRef] [PubMed]
- Curcie, D.J.; Flint, J.A.; Craelius, W. Biomimetic finger control by filtering of distributed forelimb pressures. IEEE Trans. Neural Syst. Rehabil. Eng. 2001, 9, 69–75. [Google Scholar] [CrossRef] [PubMed]
- Schürmann, C.; Kõiva, R.; Haschke, R.; Ritter, H. A modular high-speed tactile sensor for human manipulation research. In Proceedings of the IEEE World Haptics Conference (WHC), Istanbul, Turkey, 21–24 June 2011; pp. 339–344. [Google Scholar]
- Ravindra, V.; Castellini, C. A comparative analysis of three non-invasive human-machine interfaces for the disabled. Front. Neurorobot. 2014, 8, 24. [Google Scholar] [CrossRef] [PubMed]
- Guo, J.Y.; Zheng, Y.P.; Kenney, L.P.J.; Bowen, A.; Howard, D.; Canderle, J.J. A comparative evalaution of sonomyography, electromyography, force, and wrist angle in a discrete tracking task. Ultrasound Med. Biol. 2011, 37, 884–891. [Google Scholar] [CrossRef] [PubMed]
- Lucaccini, L.F.; Kaiser, P.K.; Lyman, J. The French electric hand: Some observations and conclusions. Bull. Prosthet. Res. 1966, 10, 31–51. [Google Scholar]
- Phillips, S.L.; Craelius, W. Residual Kinetic Imaging: A Versatile Interface for Prosthetic Control. Robotica 2005, 23, 277–282. [Google Scholar] [CrossRef]
- Wininger, M.; Kim, N.; Craelius, W. Pressure signature of forearm as predictor of grip force. J. Rehabil. Res. Dev. (JRRD) 2008, 45, 883–892. [Google Scholar] [CrossRef]
- Yungher, D.A.; Wininger, M.T.; Barr, J.; Craelius, W.; Threlkeld, A.J. Surface muscle pressure as a measure of active and passive behavior of muscles during gait. Med. Eng. Phys. 2011, 33, 464–471. [Google Scholar] [CrossRef] [PubMed]
- Yungher, D.; Craelius, W. Improving fine motor function after brain injury using gesture recognition biofeedback. Disabil. Rehabil. Assist. Technol. 2012, 7, 464–468. [Google Scholar] [CrossRef] [PubMed]
- Lukowicz, P.; Hanser, F.; Szubski, C.; Schobersberger, W. Detecting and Interpreting Muscle Activity with Wearable Force Sensors. In Pervasive Computing; Fishkin, K.P., Schiele, B., Nixon, P., Quigley, A., Eds.; Springer: Berlin/Heidelberg, Germany, 2006; Volume 3968, pp. 101–116. [Google Scholar]
- Connan, M.; Ruiz Ramírez, E.; Vodermayer, B.; Castellini, C. Assessment of a wearable force- and electromyography device and comparison of the related signals for myocontrol. Front. Neurorobot. 2016, 10. [Google Scholar] [CrossRef] [PubMed]
- Cho, E.; Chen, R.; Merhi, L.K.; Xiao, Z.; Pousett, B.; Menon, C. Force Myography to Control Robotic Upper Extremity Prostheses: A Feasibility Study. Front. Bioeng. Biotechnol. 2016, 4, 18. [Google Scholar] [CrossRef] [PubMed]
- Kõiva, R.; Riedenklau, E.; Viegas, C.; Castellini, C. Shape conformable high spatial resolution tactile bracelet for detecting hand and wrist activity. In Proceedings of the ICORR—International Conference on Rehabilitation Robotics, Singapore, 11–14 August 2015; pp. 157–162. [Google Scholar]
- Radmand, A.; Scheme, E.; Englehart, K. High-density force myography: A possible alternative for upper-limb prosthetic control. J. Rehabil. Res. Dev. 2016, 53, 443–456. [Google Scholar] [CrossRef] [PubMed]
- Lowe, D.G. Object Recognition from Local Scale-Invariant Features. In Proceedings of the International Conference on Computer Vision, Corfu, Greece, 20–25 September 1999. [Google Scholar]
- Luo, S.; Mou, W.; Althoefer, K.; Liu, H. Novel Tactile-SIFT Descriptor for Object Shape Recognition. IEEE Sens. 2015, 15, 5001–5009. [Google Scholar] [CrossRef]
- Castellini, C.; Passig, G.; Zarka, E. Using ultrasound images of the forearm to predict finger positions. IEEE Trans. Neural Syst. Rehabil. Eng. 2012, 20, 788–797. [Google Scholar] [CrossRef] [PubMed]
- Sierra González, D.; Castellini, C. A realistic implementation of ultrasound imaging as a human-machine interface for upper-limb amputees. Front. Neurorobot. 2013, 7, 17. [Google Scholar] [CrossRef] [PubMed]
- Ortenzi, V.; Tarantino, S.; Castellini, C.; Cipriani, C. Ultrasound Imaging for Hand Prosthesis Control: A Comparative Study of Features and Classification Methods. In Proceedings of the ICORR—International Conference on Rehabilitation Robotics, Singapore, 11–14 August 2015; pp. 1–6. [Google Scholar]
- Krizhevsky, A.; Sutskever, I.; Hinton, G.E. ImageNet Classification with Deep Convolutional Neural Networks. In Proceedings of the 25th International Conference on Neural Information Processing Systems, Lake Tahoe, NV, USA, 3–6 December 2012; Pereira, F., Burges, C.J.C., Bottou, L., Weinberger, K.Q., Eds.; pp. 1097–1105. [Google Scholar]
- Jones, N. The learning machines. Nature 2014, 505, 146–148. [Google Scholar] [CrossRef] [PubMed]
- Weiss, K.; Wörn, H. The working principle of resistive tactile sensor cells. In Proceedings of the IEEE International Conference Mechatronics and Automation (ICMA), Niagara Falls, ON, Canada, 29 July–1 August 2005; Volume 1, pp. 471–476. [Google Scholar]
- Wolfgang Warmbier GmbH & Co. KG. Available online: www.warmbier.com (accessed on 22 March 2018).
- Polyform Kunststofftechnik GmbH & Co. Betriebs KG. Available online: www.polyform.de (accessed on 22 March 2018).
- Strazzulla, I.; Nowak, M.; Controzzi, M.; Cipriani, C.; Castellini, C. Online Bimanual Manipulation Using Surface Electromyography and Incremental Learning. IEEE Trans. Neural Syst. Rehabil. Eng. 2016, in press. [Google Scholar] [CrossRef] [PubMed]
- Harris, C.; Stephens, M. A combined corner and edge detector. In Proceedings of the 4th Alvey Vision Conference, Manchester, UK, 31 August–2 September 1988; Volume 15, p. 50. [Google Scholar]
- Boschmann, A.; Platzner, M. A Computer Vision-Based Approach to High Density EMG Pattern Recognition Using Structural Similarity; University of New Brunswick’s Myoelectric Controls/Powered Prosthetics Symposium (MEC): Fredericton, NB, Canada, 2014. [Google Scholar]
- Castellini, C.; Passig, G. Ultrasound image features of the wrist are linearly related to finger positions. In Proceedings of the IROS—International Conference on Intelligent Robots and Systems, San Francisco, CA, USA, 25–30 September 2011; pp. 2108–2114. [Google Scholar]
- De Oliveira Viegas, C.L. Tactile-Based Control of a Dexterous Hand Prosthesis. Master’s thesis, Friedrich-Alexander-Universität Erlangen-Nürnberg, Erlangen, Germany, 2016. [Google Scholar]
- Powell, M.A.; Thakor, N.V. A Training Strategy for Learning Pattern Recognition Control for Myoelectric Prostheses. J. Prosthet. Orthot. 2013, 25, 30–41. [Google Scholar] [CrossRef] [PubMed]
- Jaquier, N.; Connan, M.; Castellini, C.; Calinon, S. Combining electro- and tactile myography to improve hand and wrist activity detection in prostheses. MDPI Technol. 2017, 5, 64. [Google Scholar]
- Fang, Y.; Hettiarachchi, N.; Zhou, D.; Liu, H. Multi-Modal Sensing Techniques for Interfacing Hand Prostheses: A Review. IEEE Sen. J. 2015, 15, 6065–6076. [Google Scholar] [CrossRef]
- Jiang, N.; Vujaklija, I.; Rehbaum, H.; Graimann, B.; Farina, D. Is Accurate Mapping of EMG Signals on Kinematics Needed for Precise Online Myoelectric Control? IEEE Trans. Neural Syst. Rehabil. Eng. 2014, 22, 549–558. [Google Scholar] [CrossRef] [PubMed]
- Castellini, C.; Bongers, R.M.; Nowak, M.; van der Sluis, C.K. Upper-limb prosthetic myocontrol: Two recommendations. Front. Neurosci. 2015, 9, 496. [Google Scholar] [CrossRef] [PubMed]



© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Castellini, C.; Kõiva, R.; Pasluosta, C.; Viegas, C.; Eskofier, B.M. Tactile Myography: An Off-Line Assessment of Able-Bodied Subjects and One Upper-Limb Amputee. Technologies 2018, 6, 38. https://doi.org/10.3390/technologies6020038
Castellini C, Kõiva R, Pasluosta C, Viegas C, Eskofier BM. Tactile Myography: An Off-Line Assessment of Able-Bodied Subjects and One Upper-Limb Amputee. Technologies. 2018; 6(2):38. https://doi.org/10.3390/technologies6020038
Chicago/Turabian StyleCastellini, Claudio, Risto Kõiva, Cristian Pasluosta, Carla Viegas, and Björn M. Eskofier. 2018. "Tactile Myography: An Off-Line Assessment of Able-Bodied Subjects and One Upper-Limb Amputee" Technologies 6, no. 2: 38. https://doi.org/10.3390/technologies6020038
APA StyleCastellini, C., Kõiva, R., Pasluosta, C., Viegas, C., & Eskofier, B. M. (2018). Tactile Myography: An Off-Line Assessment of Able-Bodied Subjects and One Upper-Limb Amputee. Technologies, 6(2), 38. https://doi.org/10.3390/technologies6020038





