Hypertension Induces Pro-arrhythmic Cardiac Connexome Disorders: Protective Effects of Treatment
Abstract
1. Introduction
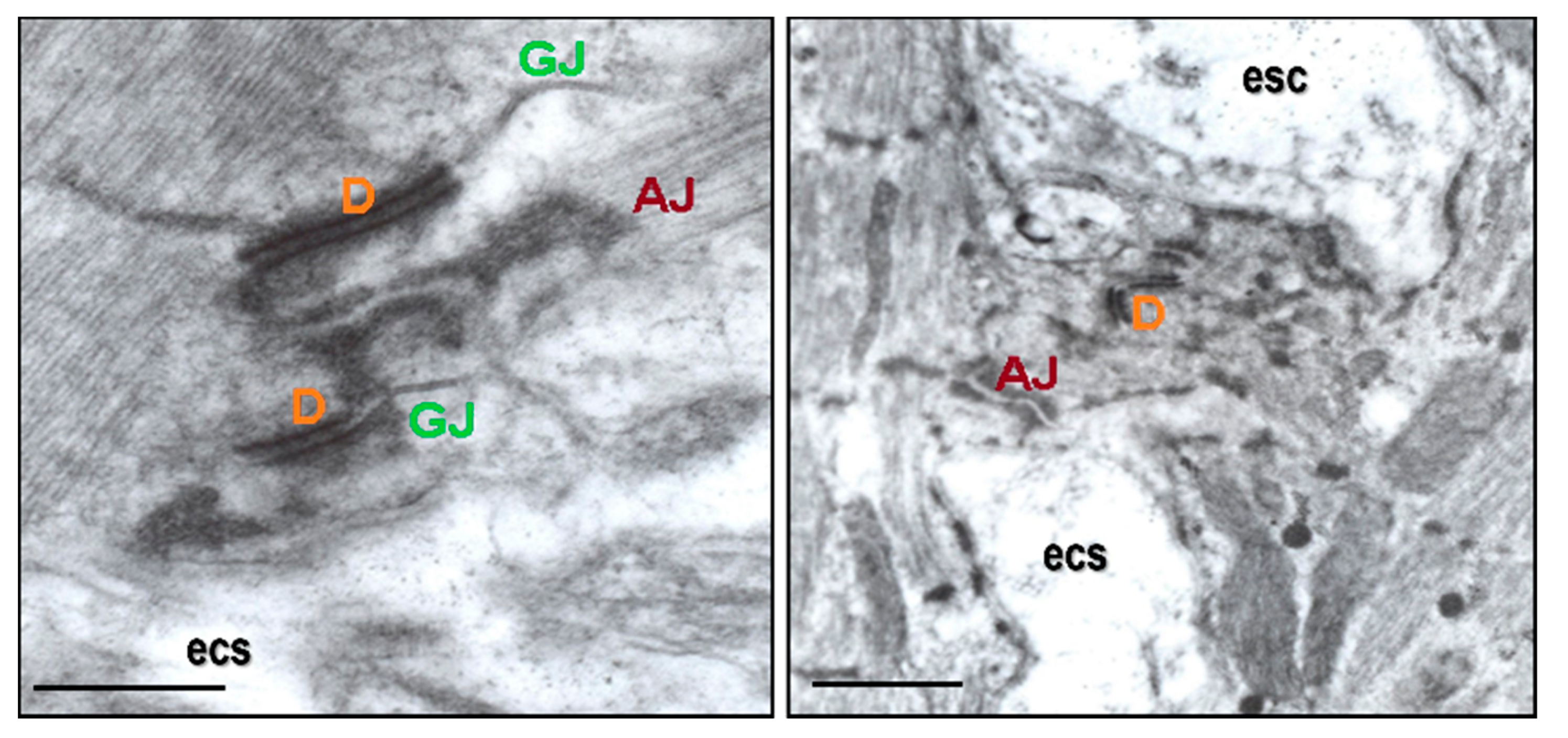
2. Factors Involved in the Development of Re-Entrant Cardiac Arrhythmias, VF, and AF
3. Connexome Impairment Promoting AF or VF Development in Primary HTN
Interventions Associated with Protecting Connexome in Primary HTN
4. Connexome Impairment Promoting VF or AF in PAH
Interventions Associated with Connexome Protection in PAH
5. Lifestyle Recommendation as Treatment for Arterial Hypertension to Protect Connexome
6. Conclusions and Perspectives
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Danik, S.B.; Liu, F.; Zhang, J.; Suk, H.J.; Morley, G.E.; Fishman, G.I.; Gutstein, D.E. Modulation of cardiac gap junction expression and arrhythmic susceptibility. Circ. Res. 2004, 95, 1035–1041. [Google Scholar] [CrossRef] [PubMed]
- Peters, N.S. New insights into myocardial arrhythmogenesis: Distribution of gap-junctional coupling in normal, ischaemic and hypertrophied human hearts. Clin. Sci. 1996, 90, 447–452. [Google Scholar] [CrossRef]
- Tribulova, N.; Okruhlicova, L.; Novakova, S.; Pancza, D.; Bernatova, I.; Pechanova, O.; Weismann, P.; Manoach, M.; Seki, S.; Mochizuki, S. Hypertension-related intermyocyte junction remodelling is associated with a higher incidence of low-K+-induced lethal arrhythmias in isolated rat heart. Exp. Physiol. 2002, 87, 195–205. [Google Scholar] [CrossRef] [PubMed]
- Tribulova, N.; Okruhlicova, L.; Imanaga, I.; Hirosawa, N.; Ogawa, K.; Weismann, P. Factors involved in the susceptibility of spontaneously hypertensive rats to low K+-induced arrhythmias. Gen. Physiol. Biophys. 2003, 22, 369–382. [Google Scholar] [PubMed]
- Tribulova, N.; Knezl, V.; Shainberg, A.; Seki, S.; Soukup, T. Thyroid hormones and cardiac arrhythmias. Vascul. Pharmacol. 2010, 52, 102–112. [Google Scholar] [CrossRef]
- Tribulova, N.; Seki, S.; Radosinska, J.; Kaplan, P.; Babusikova, E.; Knezl, V.; Mochizuki, S. Myocardial Ca2+ handling and cell-to-cell coupling, key factors in prevention of sudden cardiac death1. Can. J. Physiol. Pharmacol. 2009, 87, 1120–1129. [Google Scholar] [CrossRef]
- Andelova, K.; Benova, T.E.; Bacova, B.S.; Sykora, M.; Prado, N.J.; Diez, E.R.; Hlivak, P.; Tribulova, N. Cardiac connexin-43 hemichannels and pannexin1 channels: Provocative antiarrhythmic targets. Int. J. Mol. Sci. 2021, 22, 260. [Google Scholar] [CrossRef] [PubMed]
- Saffitz, J.E. Dependence of electrical coupling on mechanical coupling in cardiac myocytes: Insights gained from cardiomyopathies caused by defects in cell-cell connections. Ann. N. Y. Acad. Sci. 2005, 1047, 336–344. [Google Scholar] [CrossRef]
- Saffitz, J.E.; Hames, K.Y.; Kanno, S. Remodeling of Gap Junctions in Ischemic and Nonischemic Forms of Heart Disease. J. Membr. Biol. 2007, 218, 65–71. [Google Scholar] [CrossRef] [PubMed]
- Tribulova, N.; Szeiffova Bacova, B.; Benova, T.; Viczenczova, C. Can we protect from malignant arrhythmias by modulation of cardiac cell-to-cell coupling? J. Electrocardiol. 2015, 48, 434–440. [Google Scholar] [CrossRef]
- Tribulova, N.; Egan Benova, T.; Szeiffova Bacova, B.; Viczenczova, C.; Barancik, M. New aspects of pathogenesis of atrial fibrillation: Remodeling of intercalated discs. J. Physiol. Pharmacol. 2015, 66, 625–634. [Google Scholar] [PubMed]
- Sheikh, F.; Ross, R.S.; Chen, J. Cell-Cell Connection to Cardiac Disease. Trends Cardiovasc. Med. 2009, 19, 182–190. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Radice, G.L. A new perspective on intercalated disc organization: Implications for heart disease. Dermatol. Res. Pract. 2010, 2010, 207835. [Google Scholar] [CrossRef]
- Agullo-Pascual, E.; Cerrone, M.; Delmar, M. Arrhythmogenic cardiomyopathy and Brugada syndrome: Diseases of the connexome. FEBS Lett. 2014, 588, 1322–1330. [Google Scholar] [CrossRef]
- Moncayo-Arlandi, J.; Brugada, R. Unmasking the molecular link between arrhythmogenic cardiomyopathy and Brugada syndrome. Nat. Rev. Cardiol. 2017, 14, 744–756. [Google Scholar] [CrossRef]
- Ben-Haim, Y.; Asimaki, A.; Behr, E.R. Brugada syndrome and arrhythmogenic cardiomyopathy: Overlapping disorders of the connexome? Europace 2021, 23, 653–664. [Google Scholar] [CrossRef]
- Stevens, T.L.; Wallace, M.J.; El Refaey, M.; Roberts, J.D.; Koenig, S.N.; Mohler, P.J. Arrhythmogenic cardiomyopathy: Molecular insights for improved therapeutic design. J. Cardiovasc. Dev. Dis. 2020, 7, 21. [Google Scholar] [CrossRef]
- Vite, A.; Radice, G.L. N-Cadherin/Catenin Complex as a Master Regulator of Intercalated Disc Function. Cell Commun. Adhes. 2014, 21, 169–179. [Google Scholar] [CrossRef] [PubMed]
- Tribulova, N.; Knezl, V.; Szeiffova Bacova, B.; Egan Benova, T.; Viczenczova, C.; Gonçalvesova, E.; Slezak, J. Disordered myocardial Ca2+ homeostasis results in substructural alterations that may promote occurrence of malignant arrhythmias. Physiol. Res. 2016, 65, S139–S148. [Google Scholar] [CrossRef]
- Meens, M.J.; Pfenniger, A.; Kwak, B.R.; Delmar, M. Regulation of cardiovascular connexins by mechanical forces and junctions. Cardiovasc. Res. 2013, 99, 304–314. [Google Scholar] [CrossRef] [PubMed]
- Nagibin, V.; Egan Benova, T.; Viczenczova, C.; Szeiffova Bacova, B.; Dovinova, I.; Barancik, M.; Tribulova, N. Ageing related down-regulation of myocardial connexin-43 and up-regulation of MMP-2 may predict propensity to atrial fibrillation in experimental animals. Physiol. Res. 2016, 65, S91–S100. [Google Scholar] [CrossRef]
- Andelova, K.; Bacova, B.S.; Sykora, M.; Hlivak, P.; Barancik, M.; Tribulova, N. Mechanisms Underlying Antiarrhythmic Properties of Cardioprotective Agents Impacting Inflammation and Oxidative Stress. Int. J. Mol. Sci. 2022, 23, 1416. [Google Scholar] [CrossRef]
- Fedele, L.; Brand, T. The intrinsic cardiac nervous system and its role in cardiac pacemaking and conduction. J. Cardiovasc. Dev. Dis. 2020, 7, 54. [Google Scholar] [CrossRef] [PubMed]
- Nattel, S.; Heijman, J.; Zhou, L.; Dobrev, D. Molecular Basis of Atrial Fibrillation Pathophysiology and Therapy: A Translational Perspective. Circ. Res. 2020, 127, 51–72. [Google Scholar] [CrossRef] [PubMed]
- Tribulova, N.; Bacova, B.S.; Benova, T.E.; Knezl, V.; Barancik, M.; Slezak, J. Omega-3 index and anti-arrhythmic potential of omega-3 PUFAs. Nutrients 2017, 9, 1191. [Google Scholar] [CrossRef]
- Spach, M.S.; Heidlage, J.F.; Dolber, P.C.; Barr, R.C. Electrophysiological effects of remodeling cardiac gap junctions and cell size. Experimental and model studies of normal cardiac growth. Circ. Res. 2000, 86, 302–311. [Google Scholar] [CrossRef]
- Valderrábano, M. Influence of anisotropic conduction properties in the propagation of the cardiac action potential. Prog. Biophys. Mol. Biol. 2008, 94, 144–168. [Google Scholar] [CrossRef]
- Gutstein, D.E.; Morley, G.E.; Vaidya, D.; Liu, F.; Chen, F.L.; Stuhlmann, H.; Fishman, G.I. Heterogeneous expression of gap junction channels in the heart leads to conduction defects and ventricular dysfunction. Circulation 2001, 104, 1194–1199. [Google Scholar] [CrossRef] [PubMed]
- Gazdag, P.; Oravecz, K.; Acsai, K.; Demeter-Haludka, V.; Ördög, B.; Szlovák, J.; Kohajda, Z.; Polyák, A.; Barta, B.A.; Oláh, A.; et al. Increased Ca2+ content of the sarcoplasmic reticulum provides arrhythmogenic trigger source in swimming-induced rat athlete’s heart model. Sci. Rep. 2020, 10, 19596. [Google Scholar] [CrossRef]
- Wu, J.; Liu, T.; Shi, S.; Fan, Z.; Hiram, R.; Xiong, F.; Cui, B.; Su, X.; Chang, R.; Zhang, W.; et al. Dapagliflozin reduces the vulnerability of rats with pulmonary arterial hypertension-induced right heart failure to ventricular arrhythmia by restoring calcium handling. Cardiovasc. Diabetol. 2022, 21, 197. [Google Scholar] [CrossRef]
- Tribulova, N.; Kurahara, L.H.; Hlivak, P.; Hirano, K.; Bacova, B.S. Pro-arrhythmic signaling of thyroid hormones and its relevance in subclinical hyperthyroidism. Int. J. Mol. Sci. 2020, 21, 2844. [Google Scholar] [CrossRef]
- Patel, S.; Rauf, A.; Khan, H.; Abu-Izneid, T. Renin-angiotensin-aldosterone (RAAS): The ubiquitous system for homeostasis and pathologies. Biomed. Pharmacother. 2017, 94, 317–325. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Wang, S.; Bai, J.; Yang, X.L.; Zhang, Y.L.; Che, Y.L.; Li, H.H.; Yang, Y.Z. Novel role for the immunoproteasome subunit PSMB10 in angiotensin II-induced atrial fibrillation in Mice. Hypertension 2018, 71, 866–876. [Google Scholar] [CrossRef] [PubMed]
- Stambler, B.S.; Ryu, K.P. Atrial natriuretic peptide accelerates onset and dynamics of ventricular fibrillation during hypokalemia in isolated rabbit hearts. J. Electrocardiol. 2020, 62, 184–189. [Google Scholar] [CrossRef] [PubMed]
- Wahl, C.M.; Schmidt, C.; Hecker, M.; Ullrich, N.D. Distress-Mediated Remodeling of Cardiac Connexin-43 in a Novel Cell Model for Arrhythmogenic Heart Diseases. Int. J. Mol. Sci. 2022, 23, 10174. [Google Scholar] [CrossRef]
- Hoagland, D.T.; Santos, W.; Poelzing, S.; Gourdie, R.G. The role of the gap junction perinexus in cardiac conduction: Potential as a novel anti-arrhythmic drug target. Prog. Biophys. Mol. Biol. 2019, 144, 41–50. [Google Scholar] [CrossRef]
- Suvila, K.; Niiranen, T.J. Age of Hypertension Onset: Potential for Improving Risk Estimation and Hypertension Management? Hypertension 2021, 78, 1475–1477. [Google Scholar] [CrossRef]
- De Simone, G.; Mancusi, C.; Hanssen, H.; Genovesi, S.; Lurbe, E.; Parati, G.; Sendzikaite, S.; Valerio, G.; Di Bonito, P.; Di Salvo, G.; et al. Hypertension in children and adolescents. Eur. Heart J. 2022, 43, 3290–3301. [Google Scholar] [CrossRef]
- Li, L.; Yi-Ming, W.; Li, Z.Z.; Zhao, L.; Yu, Y.S.; Li, D.J.; Xia, C.Y.; Liu, J.G.; Su, D.F. Local RAS and inflammatory factors are involved in cardiovascular hypertrophy in spontaneously hypertensive rats. Pharmacol. Res. 2008, 58, 196–201. [Google Scholar] [CrossRef]
- Bacova, B.S.; Radosinska, J.; Wallukat, G.; Barancik, M.; Wallukat, A.; Knezl, V.; Sykora, M.; Paulis, L.; Tribulova, N. Suppression of β1-adrenoceptor autoantibodies is involved in the antiarrhythmic effects of omega-3 fatty acids in male and female hypertensive rats. Int. J. Mol. Sci. 2020, 21, 526. [Google Scholar] [CrossRef]
- Bai, L.; Qu, C.; Feng, Y.; Liu, G.; Li, X.; Li, W.; Yu, S. Evidence of a casual relationship between vitamin D deficiency and hypertension: A family-based study. Hypertens. Res. 2022, 45, 1814–1822. [Google Scholar] [CrossRef]
- Bayés-Genís, A.; Díez, J. Transition to heart failure in hypertension: Going to the heart of the matter. Eur. Heart J. 2022, 43, 3332–3334. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.; Brage, S.; Sharp, S.J.; Luo, S.; Au Yeung, S.L.; Kim, Y. Associations of genetic susceptibility and healthy lifestyle with incidence of coronary heart disease and stroke in individuals with hypertension. Eur. J. Prev. Cardiol. 2022, 29, 2101–2110. [Google Scholar] [CrossRef] [PubMed]
- Vaura, F.; Kim, H.; Udler, M.S.; Salomaa, V.; Lahti, L.; Niiranen, T. Multi-Trait Genetic Analysis Reveals Clinically Interpretable Hypertension Subtypes. Circ. Genom. Precis. Med. 2022, 15, e003583. [Google Scholar] [CrossRef]
- Takahashi, H.; Yoshika, M.; Komiyama, Y.; Nishimura, M. The central mechanism underlying hypertension: A review of the roles of sodium ions, epithelial sodium channels, the renin-angiotensin-aldosterone system, oxidative stress and endogenous digitalis in the brain. Hypertens. Res. 2011, 34, 1147–1160. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.C.; Zhang, Z.S.; Zhang, L.; Wang, A.; Zhu, H.; Li, L.; Si, J.Q.; Li, X.Z.; Ma, K.T. Connexin 43 in splenic lymphocytes is involved in the regulation of CD4+CD25+ T lymphocyte proliferation and cytokine production in hypertensive inflammation. Int. J. Mol. Med. 2018, 41, 13–24. [Google Scholar] [CrossRef]
- Wang, L.J.; Zhang, W.W.; Zhang, L.; Shi, W.Y.; Wang, Y.Z.; Ma, K.T.; Liu, W.D.; Zhao, L.; Li, L.; Si, J.Q. Association of connexin gene polymorphism with essential hypertension in Kazak and Han Chinese in Xinjiang, China. J. Huazhong Univ. Sci. Technol.—Med. Sci. 2017, 37, 197–203. [Google Scholar] [CrossRef]
- Arif, M.; Sadayappan, S.; Becker, R.C.; Martin, L.J.; Urbina, E.M. Epigenetic modification: A regulatory mechanism in essential hypertension. Hypertens. Res. 2019, 42, 1099–1113. [Google Scholar] [CrossRef]
- Jusic, A.; Devaux, Y. Noncoding RNAs in Hypertension. Hypertension 2019, 74, 477–492. [Google Scholar] [CrossRef]
- Rodrigo, R.; Prat, H.; Passalacqua, W.; Araya, J.; Bächler, J.P. Decrease in oxidative stress through supplementation of vitamins C and E is associated with a reduction in blood pressure in patients with essential hypertension. Clin. Sci. 2008, 114, 625–634. [Google Scholar] [CrossRef]
- Rodrigo, R.; González, J.; Paoletto, F. The role of oxidative stress in the pathophysiology of hypertension. Hypertens. Res. 2011, 34, 431–440. [Google Scholar] [CrossRef]
- Rodriguez-Iturbe, B.; Johnson, R.J. Genetic Polymorphisms in Hypertension: Are We Missing the Immune Connection? Am. J. Hypertens. 2019, 32, 113–122. [Google Scholar] [CrossRef] [PubMed]
- Brown, J.M.; Zhou, W.; Weber, B.; Divakaran, S.; Barrett, L.; Bibbo, C.F.; Hainer, J.; Taqueti, V.R.; Dorbala, S.; Blankstein, R.; et al. Low coronary flow relative to myocardial mass predicts heart failure in symptomatic hypertensive patients with no obstructive coronary artery disease. Eur. Heart J. 2022, 43, 3323–3331. [Google Scholar] [CrossRef] [PubMed]
- Egan Benova, T.; Szeiffova Bacova, B.; Viczenczova, C.; Diez, E.; Barancik, M.; Tribulova, N. Protection of cardiac cell-to-cell coupling attenuate myocardial remodeling and proarrhythmia induced by hypertension. Physiol. Res. 2016, 65, S29–S42. [Google Scholar] [CrossRef]
- Benova, T.E.; Viczenczova, C.; Bacova, B.S.; Zurmanova, J.; Knezl, V.; Andelova, K.; Tribulova, N. Omacor protects normotensive and hypertensive rats exposed to continuous light from increased risk to malignant cardiac arrhythmias. Mar. Drugs 2021, 19, 659. [Google Scholar] [CrossRef] [PubMed]
- Dzau, V.J.; Balatbat, C.A. Future of hypertension: The need for transformation. Hypertension 2019, 74, 450–457. [Google Scholar] [CrossRef]
- Marazzato, J.; Blasi, F.; Golino, M.; Verdecchia, P.; Angeli, F.; De Ponti, R. Hypertension and Arrhythmias: A Clinical Overview of the Pathophysiology-Driven Management of Cardiac Arrhythmias in Hypertensive Patients. J. Cardiovasc. Dev. Dis. 2022, 9, 110. [Google Scholar] [CrossRef] [PubMed]
- Crea, F. Hypertension in children, adolescents, and pregnant women: Challenges and opportunities. Eur. Heart J. 2022, 43, 3275–3278. [Google Scholar] [CrossRef]
- Bacharova, L.; Plandorova, J.; Klimas, J.; Krenek, P.; Kyselovic, J. Discrepancy between increased left ventricular mass and “normal” QRS voltage is associated with decreased connexin 43 expression in early stage of left ventricular hypertrophy in spontaneously hypertensive rats. J. Electrocardiol. 2008, 41, 730–734. [Google Scholar] [CrossRef] [PubMed]
- Hussain, W.; Patel, P.M.; Chowdhury, R.A.; Cabo, C.; Ciaccio, E.J.; Lab, M.J.; Duffy, H.S.; Wit, A.L.; Peters, N.S. The Renin-Angiotensin System Mediates the Effects of Stretch on Conduction Velocity, Connexin43 Expression, and Redistribution in Intact Ventricle. J. Cardiovasc. Electrophysiol. 2010, 21, 1276–1283. [Google Scholar] [CrossRef]
- Teunissen, B.E.J.; Jongsma, H.J.; Bierhuizen, M.F.A. Regulation of myocardial connexins during hypertrophic remodelling. Eur. Heart J. 2004, 25, 1979–1989. [Google Scholar] [CrossRef] [PubMed]
- Bačová, B.; Radošinská, J.; Viczenczová, C.; Knezl, V.; Dosenko, V.; Beňova, T.; Navarová, J.; Gonçalvesová, E.; van Rooyen, J.; Weismann, P.; et al. Up-regulation of myocardial connexin-43 in spontaneously hypertensive rats fed red palm oil is most likely implicated in its anti-arrhythmic effects. Can. J. Physiol. Pharmacol. 2012, 90, 1235–1245. [Google Scholar] [CrossRef] [PubMed]
- Strauss, B.; Sassi, Y.; Bueno-Beti, C.; Ilkan, Z.; Raad, N.; Cacheux, M.; Bisserier, M.; Turnbull, I.C.; Kohlbrenner, E.; Hajjar, R.J.; et al. Intra-tracheal gene delivery of aerosolized SERCA2a to the lung suppresses ventricular arrhythmias in a model of pulmonary arterial hypertension. J. Mol. Cell. Cardiol. 2019, 127, 20–30. [Google Scholar] [CrossRef]
- Bacova, B.S.; Viczenczova, C.; Andelova, K.; Sykora, M.; Chaudagar, K.; Barancik, M.; Adamcova, M.; Knezl, V.; Benova, T.E.; Weismann, P.; et al. Antiarrhythmic effects of melatonin and omega-3 are linked with protection of myocardial cx43 topology and suppression of fibrosis in catecholamine stressed normotensive and hypertensive rats. Antioxidants 2020, 9, 546. [Google Scholar] [CrossRef]
- Hein, S.; Elsässer, A.; Kostin, S.; Zimmermann, R.; Schaper, J. Functional disturbances due to structural remodeling in the failing human heart. Arch. Mal. Coeur Vaiss. 2002, 95, 815–820. [Google Scholar]
- Hein, S.; Arnon, E.; Kostin, S.; Schönburg, M.; Elsässer, A.; Polyakova, V.; Bauer, E.P.; Klövekorn, W.P.; Schaper, J. Progression from compensated hypertrophy to failure in the pressure-overloaded human: Heart structural deterioration and compensatory mechanisms. Circulation 2003, 107, 984–991. [Google Scholar] [CrossRef] [PubMed]
- Kostin, S.; Dammer, S.; Hein, S.; Klovekorn, W.P.; Bauer, E.P.; Schaper, J. Connexin 43 expression and distribution in compensated and decompensated cardiac hypertrophy in patients with aortic stenosis. Cardiovasc. Res. 2004, 62, 426–436. [Google Scholar] [CrossRef]
- Fischer, R.; Dechend, R.; Gapelyuk, A.; Shagdarsuren, E.; Gruner, K.; Gruner, A.; Gratze, P.; Qadri, F.; Wellner, M.; Fiebeler, A.; et al. Angiotensin II-induced sudden arrhythmic death and electrical remodeling. Am. J. Physiol.—Heart Circ. Physiol. 2007, 293, 1242–1253. [Google Scholar] [CrossRef] [PubMed]
- Fischer, R.; Dechend, R.; Qadri, F.; Markovic, M.; Feldt, S.; Herse, F.; Park, J.K.; Gapelyuk, A.; Schwarz, I.; Zacharzowsky, U.B.; et al. Dietary n-3 polyunsaturated fatty acids and direct renin inhibition improve electrical remodeling in a model of high human renin hypertension. Hypertension 2008, 51, 540–546. [Google Scholar] [CrossRef] [PubMed]
- Kasi, V.S.; Xiao, H.D.; Shang, L.L.; Iravanian, S.; Langberg, J.; Witham, E.A.; Jiao, Z.; Gallego, C.J.; Bernstein, K.E.; Dudley, S.C. Cardiac-restricted angiotensin-converting enzyme overexpression causes conduction defects and connexin dysregulation. Am. J. Physiol.—Heart Circ. Physiol. 2007, 293, H182–H192. [Google Scholar] [CrossRef]
- Monitillo, F.; Di Terlizzi, V.; Gioia, M.I.; Barone, R.; Grande, D.; Parisi, G.; Brunetti, N.D.; Iacoviello, M. Right ventricular function in chronic heart failure: From the diagnosis to the therapeutic approach. J. Cardiovasc. Dev. Dis. 2020, 7, 12. [Google Scholar] [CrossRef] [PubMed]
- Hofgaard, J.P.; Banach, K.; Mollerup, S.; Jørgensen, H.K.; Olesen, S.P.; Holstein-Rathlou, N.-H.; Nielsen, M.S. Phosphatidylinositol-bisphosphate regulates intercellular coupling in cardiac myocytes. Pflügers Arch.—Eur. J. Physiol. 2008, 457, 303–313. [Google Scholar] [CrossRef]
- Radosinska, J.; Bacova, B.; Knezl, V.; Benova, T.; Zurmanova, J.; Soukup, T.; Arnostova, P.; Slezak, J.; Goncalvesova, E.; Tribulova, N. Dietary omega-3 fatty acids attenuate myocardial arrhythmogenic factors and propensity of the heart to lethal arrhythmias in a rodent model of human essential hypertension. J. Hypertens. 2013, 31, 1876–1885. [Google Scholar] [CrossRef]
- Kvakan, H.; Kleinewietfeld, M.; Qadri, F.; Park, J.K.; Fischer, R.; Schwarz, I.; Rahn, H.P.; Plehm, R.; Wellner, M.; Elitok, S.; et al. Regulatory T cells ameliorate angiotensin II-induced cardiac damage. Circulation 2009, 119, 2904–2912. [Google Scholar] [CrossRef] [PubMed]
- Hesketh, G.G.; Shah, M.H.; Halperin, V.L.; Cooke, C.A.; Akar, F.G.; Yen, T.E.; Kass, D.A.; MacHamer, C.E.; Van Eyk, J.E.; Tomaselli, G.F. Ultrastructure and regulation of lateralized connexin43 in the failing heart. Circ. Res. 2010, 106, 1153–1163. [Google Scholar] [CrossRef] [PubMed]
- Benova, T.; Viczenczova, C.; Radosinska, J.; Bacova, B.; Knezl, V.; Dosenko, V.; Weismann, P.; Zeman, M.; Navarova, J.; Tribulova, N. Melatonin attenuates hypertension-related proarrhythmic myocardial maladaptation of connexin-43 and propensity of the heart to lethal arrhythmias. Can. J. Physiol. Pharmacol. 2013, 91, 633–639. [Google Scholar] [CrossRef]
- Andelova, K.; Szeiffova Bacova, B.; Sykora, M.; Pavelka, S.; Rauchova, H.; Tribulova, N. Cardiac Cx43 Signaling Is Enhanced and TGF-β1/SMAD2/3 Suppressed in Response to Cold Acclimation and Modulated by Thyroid Status in Hairless SHRM. Biomedicines 2022, 10, 1707. [Google Scholar] [CrossRef]
- Seidel, T.; Salameh, A.; Dhein, S. A simulation study of cellular hypertrophy and connexin lateralization in cardiac tissue. Biophys. J. 2010, 99, 2821–2830. [Google Scholar] [CrossRef]
- Chkourko, H.S.; Guerrero-Serna, G.; Lin, X.; Darwish, N.; Pohlmann, J.R.; Cook, K.E.; Martens, J.R.; Rothenberg, E.; Musa, H.; Delmar, M. Remodeling of mechanical junctions and of microtubule-associated proteins accompany cardiac connexin43 lateralization. Heart Rhythm 2012, 9, 1133–1140.e6. [Google Scholar] [CrossRef]
- Craig, M.A.; McBride, M.W.; Smith, G.; George, S.J.; Baker, A. Dysregulation of cadherins in the intercalated disc of the spontaneously hypertensive stroke-prone rat. J. Mol. Cell. Cardiol. 2010, 48, 1121–1128. [Google Scholar] [CrossRef]
- Jansen, J.A.; Van Veen, T.A.B.; De Jong, S.; Van Der Nagel, R.; Van Stuijvenberg, L.; Driessen, H.; Labzowski, R.; Oefner, C.M.; Bosch, A.A.; Nguyen, T.Q.; et al. Reduced Cx43 expression triggers increased fibrosis due to enhanced fibroblast activity. Circ. Arrhythmia Electrophysiol. 2012, 5, 380–390. [Google Scholar] [CrossRef]
- Rohr, S. Arrhythmogenic implications of fibroblast-myocyte interactions. Circ. Arrhythmia Electrophysiol. 2012, 5, 442–452. [Google Scholar] [CrossRef] [PubMed]
- Cooklin, M.; Wallis, W.R.J.; Sheridan, D.J.; Fry, C.H. Changes in Cell-to-Cell Electrical Coupling Associated With Left Ventricular Hypertrophy. Circ. Res. 1997, 80, 765–771. [Google Scholar] [CrossRef] [PubMed]
- Wehbe, N.; Nasser, S.A.; Pintus, G.; Badran, A.; Eid, A.H.; Baydoun, E. MicroRNAs in Cardiac Hypertrophy. Int. J. Mol. Sci. 2019, 20, 4714. [Google Scholar] [CrossRef] [PubMed]
- Yang, B.; Lin, H.; Xiao, J.; Lu, Y.; Luo, X.; Li, B.; Zhang, Y.; Xu, C.; Bai, Y.; Wang, H.; et al. The muscle-specific microRNA miR-1 regulates cardiac arrhythmogenic potential by targeting GJA1 and KCNJ2. Nat. Med. 2007, 13, 486–491. [Google Scholar] [CrossRef] [PubMed]
- Stauffer, B.L.; Sobus, R.D.; Sucharov, C.C. Sex differences in cardiomyocyte connexin43 expression. J. Cardiovasc. Pharmacol. 2011, 58, 32–39. [Google Scholar] [CrossRef]
- Tribulová, N.; Dupont, E.; Soukup, T.; Okruhlicová, L.; Severs, N.J. Sex differences in connexin-43 expression in left ventricles of aging rats. Physiol. Res. 2005, 54, 705–708. [Google Scholar] [CrossRef]
- Curcio, A.; Torella, D.; Iaconetti, C.; Pasceri, E.; Sabatino, J.; Sorrentino, S.; Giampà, S.; Micieli, M.; Polimeni, A.; Henning, B.J.; et al. MicroRNA-1 Downregulation Increases Connexin 43 Displacement and Induces Ventricular Tachyarrhythmias in Rodent Hypertrophic Hearts. PLoS ONE 2013, 8, e0070158. [Google Scholar] [CrossRef]
- Lapikova-Bryhinska, T.; Zhukovska, A.; Nagibin, V.; Tumanovska, L.; Portnichenko, G.; Goncharov, S.; Portnychenko, A.; Dosenko, V. Altered biogenesis of microRNA-1 is associated with cardiac dysfunction in aging of spontaneously hypertensive rats. Mol. Cell. Biochem. 2019, 459, 73–82. [Google Scholar] [CrossRef]
- Luo, X.; Yang, B.; Nattel, S. MicroRNAs and atrial fibrillation: Mechanisms and translational potential. Nat. Rev. Cardiol. 2015, 12, 80–90. [Google Scholar] [CrossRef]
- Bruce, A.F.; Rothery, S.; Dupont, E.; Severs, N.J. Gap junction remodelling in human heart failure is associated with increased interaction of connexin43 with ZO-1. Cardiovasc. Res. 2008, 77, 757–765. [Google Scholar] [CrossRef] [PubMed]
- Kostin, S. Zonula occludens-1 and connexin 43 expression in the failing human heart. J. Cell. Mol. Med. 2007, 11, 892–895. [Google Scholar] [CrossRef] [PubMed]
- Palatinus, J.A.; Rhett, J.M.; Gourdie, R.G. Enhanced PKCε mediated phosphorylation of connexin43 at serine 368 by a carboxyl-terminal mimetic peptide is dependent on injury. Channels 2011, 5, 236–240. [Google Scholar] [CrossRef] [PubMed]
- Bupha-Intr, T.; Haizlip, K.M.; Janssen, P.M.L. Temporal changes in expression of connexin 43 after load-induced hypertrophy in vitro. Am. J. Physiol.—Heart Circ. Physiol. 2009, 296, 806–814. [Google Scholar] [CrossRef]
- Cone, A.C.; Cavin, G.; Ambrosi, C.; Hakozaki, H.; Wu-Zhang, A.X.; Kunkel, M.T.; Newton, A.C.; Sosinsky, G.E. Protein kinase Cδ-mediated phosphorylation of connexin43 gap junction channels causes movement within gap junctions followed by vesicle internalization and protein degradation. J. Biol. Chem. 2014, 289, 8781–8798. [Google Scholar] [CrossRef]
- Kells-Andrews, R.M.; Margraf, R.A.; Fisher, C.G.; Falk, M.M. Connexin 43 K63-polyubiquitylation on lysines 264 and 303 regulates gap junction internalization. J. Cell Sci. 2018, 131, jcs204321. [Google Scholar] [CrossRef] [PubMed]
- Panagopoulou, P.; Davos, C.H.; Milner, D.J.; Varela, E.; Cameron, J.A.; Mann, D.L.; Capetanaki, Y. Desmin mediates TNF-α-induced aggregate formation and intercalated disk reorganization in heart failure. J. Cell Biol. 2008, 181, 761–775. [Google Scholar] [CrossRef]
- Brooks, W.W.; Shen, S.; Conrad, C.H.; Goldstein, R.H.; Deng, L.L.; Bing, O.H.L. Transcriptional changes associated with recovery from heart failure in the SHR. J. Mol. Cell. Cardiol. 2010, 49, 390–401. [Google Scholar] [CrossRef]
- Chen, H.J.; Yao, L.; Chen, T.G.; Yu, M.; Wang, L.H.; Chen, J.Z. Atorvastatin prevents connexin43 remodeling in hypertrophied left ventricular myocardium of spontaneously hypertensive rats. Chin. Med. J. 2007, 120, 1902–1907. [Google Scholar] [CrossRef]
- De Mello, W.C.; Specht, P. Chronic blockade of angiotensin II AT1-receptors increased cell-to-cell communication, reduced fibrosis and improved impulse propagation in the failing heart. JRAAS—J. Renin-Angiotensin-Aldosterone Syst. 2006, 7, 201–205. [Google Scholar] [CrossRef]
- Choisy, S.C.; Kim, S.J.; Hancox, J.C.; Jones, S.A.; James, A.F. Effects of candesartan, an angiotensin II receptor type I blocker, on atrial remodeling in spontaneously hypertensive rats. Physiol. Rep. 2015, 3, e12274. [Google Scholar] [CrossRef] [PubMed]
- De Mello, W.C. Opposite effects of angiotensin II and angiotensin (1-7) on impulse propagation, excitability and cardiac arrhythmias. Is the overexpression of ACE2 arrhythmogenic? Regul. Pept. 2009, 153, 7–10. [Google Scholar] [CrossRef] [PubMed]
- Fu, Y.L.; Tao, L.; Peng, F.H.; Zheng, N.Z.; Lin, Q.; Cai, S.Y.; Wang, Q. GJA1-20k attenuates Ang II-induced pathological cardiac hypertrophy by regulating gap junction formation and mitochondrial function. Acta Pharmacol. Sin. 2021, 42, 536–549. [Google Scholar] [CrossRef] [PubMed]
- Díaz del Campo, L.S.; García-Redondo, A.B.; Rodriguez, C.; Zaragoza, C.; Duro-Sánchez, S.; Palmas, F.; de Benito-Bueno, A.; Socuéllamos, P.G.; Peraza, D.A.; Rodrigues-Diez, R.; et al. Resolvin D2 Attenuates Cardiovascular Damage in Angiotensin Ii-Induced Hypertension. Hypertension 2023, 80, 84–96. [Google Scholar] [CrossRef] [PubMed]
- Ni, X.; Zhang, L.; Peng, M.; Shen, T.W.; Yu, X.S.; Shan, L.Y.; Li, L.; Si, J.Q.; Li, X.Z.; Ma, K.T. Hydrogen sulfide attenuates hypertensive inflammation via regulating connexin expression in spontaneously hypertensive rats. Med. Sci. Monit. 2018, 24, 1205–1218. [Google Scholar] [CrossRef] [PubMed]
- Szeiffova Bacova, B.; Andelova, K.; Sykora, M.; Egan Benova, T.; Barancik, M.; Kurahara, L.H.; Tribulova, N. Does myocardial atrophy represent anti-arrhythmic phenotype? Biomedicines 2022, 10, 2819. [Google Scholar] [CrossRef]
- Hajri, T.; Ibrahimi, A.; Coburn, C.T.; Knapp, F.F.; Kurtz, T.; Pravenec, M.; Abumrad, N.A. Defective Fatty Acid Uptake in the Spontaneously Hypertensive Rat Is a Primary Determinant of Altered Glucose Metabolism, Hyperinsulinemia, and Myocardial Hypertrophy. J. Biol. Chem. 2001, 276, 23661–23666. [Google Scholar] [CrossRef]
- STEINBERG, S.F. Distinctive activation mechanisms and functions for protein kinase Cδ. Biochem. J. 2004, 384, 449–459. [Google Scholar] [CrossRef]
- Kohutova, J.; Elsnicova, B.; Holzerova, K.; Neckar, J.; Sebesta, O.; Jezkova, J.; Vecka, M.; Vebr, P.; Hornikova, D.; Bacova, B.S.; et al. Anti-arrhythmic cardiac phenotype elicited by chronic intermittent hypoxia is associated with alterations in connexin-43 expression, phosphorylation, and distribution. Front. Endocrinol. 2019, 10, 1–10. [Google Scholar] [CrossRef]
- Zhang, W.; Zhao, G.; Hu, X.; Wang, M.; Li, H.; Ye, Y.; Du, Q.; Yao, J.; Bao, Z.; Hong, W.; et al. Aliskiren-attenuated myocardium apoptosis via regulation of autophagy and connexin-43 in aged spontaneously hypertensive rats. J. Cell. Mol. Med. 2014, 18, 1247–1256. [Google Scholar] [CrossRef]
- Rassler, B.; Hawlitschek, C.; Brendel, J.; Zimmer, H.-G. How Do Young and Old Spontaneously Hypertensive Rats Respond to Antihypertensive Therapy? Comparative Studies on the Effects of Combined Captopril and Nifedipine Treatment. Biomedicines 2022, 10, 3059. [Google Scholar] [CrossRef]
- Parikh, A.; Patel, D.; McTiernan, C.F.; Xiang, W.; Haney, J.; Yang, L.; Lin, B.; Kaplan, A.D.; Bett, G.C.L.; Rasmusson, R.L.; et al. Relaxin suppresses atrial fibrillation by reversing fibrosis and myocyte hypertrophy and increasing conduction velocity and sodium current in spontaneously hypertensive rat hearts. Circ. Res. 2013, 113, 313–321. [Google Scholar] [CrossRef] [PubMed]
- Mavrogeni, S.; Piaditis, G.; Bacopoulou, F.; Chrousos, G.P. Cardiac Remodeling in Hypertension: Clinical Impact on Brain, Heart, and Kidney Function. Horm. Metab. Res. 2022, 54, 273–279. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Schreier, D.A.; Hacker, T.A.; Chesler, N.C. Progressive right ventricular functional and structural changes in a mouse model of pulmonary arterial hypertension. Physiol. Rep. 2013, 1, e00184. [Google Scholar] [CrossRef] [PubMed]
- Omura, J.; Habbout, K.; Shimauchi, T.; Wu, W.H.; Breuils-Bonnet, S.; Tremblay, E.; Martineau, S.; Nadeau, V.; Gagnon, K.; Mazoyer, F.; et al. Identification of Long Noncoding RNA H19 as a New Biomarker and Therapeutic Target in Right Ventricular Failure in Pulmonary Arterial Hypertension. Circulation 2020, 142, 1464–1484. [Google Scholar] [CrossRef] [PubMed]
- Sasano, C.; Honjo, H.; Takagishi, Y.; Uzzaman, M.; Emdad, L.; Shimizu, A.; Murata, Y.; Kamiya, K.; Kodama, I. Internalization and dephosphorylation of Connexin43 in hypertrophied right ventricles of rats with pulmonary hypertension. Circ. J. 2007, 71, 382–389. [Google Scholar] [CrossRef]
- Bouvard, C.; Genet, N.; Phan, C.; Rode, B.; Thuillet, R.; Tu, L.; Robillard, P.; Campagnac, M.; Soleti, R.; de la Roque, E.D.; et al. Connexin-43 is a promising target for pulmonary hypertension due to hypoxaemic lung disease. Eur. Respir. J. 2020, 55, 1900169. [Google Scholar] [CrossRef]
- Boengler, K.; Rohrbach, S.; Weissmann, N.; Schulz, R. Importance of CX43 for right ventricular function. Int. J. Mol. Sci. 2021, 22, 987. [Google Scholar] [CrossRef]
- Htet, M.; Nally, J.E.; Martin, P.E.; Dempsie, Y. New insights into pulmonary hypertension: A role for connexin-mediated signalling. Int. J. Mol. Sci. 2022, 23, 379. [Google Scholar] [CrossRef]
- Ou, B.; Nakagawa, M.; Kajimoto, M.; Nobe, S.; Ooie, T.; Ichinose, M.; Yonemochi, H.; Ono, N.; Shimada, T.; Saikawa, T. Heterogeneous expression of connexin 43 in the myocardium of rabbit right ventricular outflow tract. Life Sci. 2005, 77, 52–59. [Google Scholar] [CrossRef]
- Strauss, B.; Bisserier, M.; Obus, E.; Katz, M.G.; Fargnoli, A.; Cacheux, M.; Akar, J.G.; Hummel, J.P.; Hadri, L.; Sassi, Y.; et al. Right predominant electrical remodeling in a pure model of pulmonary hypertension promotes reentrant arrhythmias. Heart Rhythm 2022, 19, 113–124. [Google Scholar] [CrossRef] [PubMed]
- Uzzaman, M.; Honjo, H.; Takagishi, Y.; Emdad, L.; Magee, A.I.; Severs, N.J.; Kodama, I. Remodeling of gap junctional coupling in hypertrophied right ventricles of rats with monocrotaline-induced pulmonary hypertension. Circ. Res. 2000, 86, 871–878. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.Y.; Lin, F.J.; Chen, Y.C.; Kao, Y.H.; Higa, S.; Chen, S.A.; Chen, Y.J. Role of Endothelin-1 in Right Atrial Arrhythmogenesis in Rabbits with Monocrotaline-Induced Pulmonary Arterial Hypertension. Int. J. Mol. Sci. 2022, 23, 10993. [Google Scholar] [CrossRef]
- García-Álvarez, A.; Blanco, I.; García-Lunar, I.; Jordà, P.; Rodriguez-Arias, J.J.; Fernández-Friera, L.; Zegri, I.; Nuche, J.; Gomez-Bueno, M.; Prat, S.; et al. β3 adrenergic agonist treatment in chronic pulmonary hypertension associated with heart failure (SPHERE-HF): A double blind, placebo-controlled, randomized clinical trial. Eur. J. Heart Fail. 2022, 279400. [Google Scholar] [CrossRef]
- Hardziyenka, M.; Campian, M.E.; Verkerk, A.O.; Surie, S.; Van Ginneken, A.C.G.; Hakim, S.; Linnenbank, A.C.; De Bruin-Bon, H.A.C.M.R.; Beekman, L.; Van Der Plas, M.N.; et al. Electrophysiologic remodeling of the left ventricle in pressure overload-induced right ventricular failure. J. Am. Coll. Cardiol. 2012, 59, 2193–2202. [Google Scholar] [CrossRef] [PubMed]
- Hiram, R.; Naud, P.; Xiong, F.; Al-u’datt, D.; Algalarrondo, V.; Sirois, M.G.; Tanguay, J.F.; Tardif, J.C.; Nattel, S. Right Atrial Mechanisms of Atrial Fibrillation in a Rat Model of Right Heart Disease. J. Am. Coll. Cardiol. 2019, 74, 1332–1347. [Google Scholar] [CrossRef]
- Hemnes, A.R.; Rathinasabapathy, A.; Austin, E.A.; Brittain, E.L.; Carrier, E.J.; Chen, X.; Fessel, J.P.; Fike, C.D.; Fong, P.; Fortune, N.; et al. A potential therapeutic role for angiotensin-converting enzyme 2 in human pulmonary arterial hypertension. Eur. Respir. J. 2018, 51, 1702638. [Google Scholar] [CrossRef]
- Lee, F.Y.; Lu, H.I.; Zhen, Y.Y.; Leu, S.; Chen, Y.L.; Tsai, T.H.; Chung, S.Y.; Chua, S.; Sheu, J.J.; Hsu, S.Y.; et al. Benefit of combined therapy with nicorandil and colchicine in preventing monocrotaline-induced rat pulmonary arterial hypertension. Eur. J. Pharm. Sci. 2013, 50, 372–384. [Google Scholar] [CrossRef]
- Sun, C.K.; Yuen, C.M.; Kao, Y.H.; Chang, L.T.; Chua, S.; Sheu, J.J.; Yen, C.H.; Ko, S.F.; Yip, H.K. Propylthiouracil attenuates monocrotaline-induced pulmonary arterial hypertension in rats. Circ. J. 2009, 73, 1722–1730. [Google Scholar] [CrossRef]
- Tan, X.Y.; He, J.G. The remodeling of connexin in the hypertrophied right ventricular in pulmonary arterial hypertension and the effect of a dual ET receptor antagonist (bosentan). Pathol. Res. Pract. 2009, 205, 473–482. [Google Scholar] [CrossRef]
- Tanaka, Y.; Takase, B.; Yao, T.; Ishihara, M. Right Ventricular Electrical Remodeling and Arrhythmogenic Substrate in Rat Pulmonary Hypertension. Am. J. Respir. Cell Mol. Biol. 2013, 49, 426–436. [Google Scholar] [CrossRef] [PubMed]
- Yen, C.-H.; Tsai, T.-H.; Leu, S.; Chen, Y.-L.; Chang, L.-T.; Chai, H.-T.; Chung, S.-Y.; Chua, S.; Tsai, C.-Y.; Chang, H.-W.; et al. Sildenafil improves long-term effect of endothelial progenitor cell-based treatment for monocrotaline-induced rat pulmonary arterial hypertension. Cytotherapy 2013, 15, 209–223. [Google Scholar] [CrossRef] [PubMed]
- Parati, G.; Goncalves, A.; Soergel, D.; Bruno, R.M.; Caiani, E.G.; Gerdts, E.; Mahfoud, F.; Mantovani, L.; McManus, R.J.; Santalucia, P.; et al. New Perspectives for Hypertension Management: Progress in Methodological and Technological Developments. Eur. J. Prev. Cardiol. 2022, 30, 48–60. [Google Scholar] [CrossRef]
- Maniero, C.; Lopuszko, A.; Papalois, K.B.; Gupta, A.; Kapil, V.; Khanji, M.Y. Non-pharmacological factors for hypertension management: A systematic review of international guidelines. Eur. J. Prev. Cardiol. 2022, 30, 17–33. [Google Scholar] [CrossRef]
- Pagonasa, N.; Saskoa, B.; Rittera, O. Managing hypertension in the future: A multifactorial approach. Eur. J. Prev. Cardiol. 2022, 30, 46–47. [Google Scholar] [CrossRef] [PubMed]




Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sykora, M.; Andelova, K.; Szeiffova Bacova, B.; Egan Benova, T.; Martiskova, A.; Knezl, V.; Tribulova, N. Hypertension Induces Pro-arrhythmic Cardiac Connexome Disorders: Protective Effects of Treatment. Biomolecules 2023, 13, 330. https://doi.org/10.3390/biom13020330
Sykora M, Andelova K, Szeiffova Bacova B, Egan Benova T, Martiskova A, Knezl V, Tribulova N. Hypertension Induces Pro-arrhythmic Cardiac Connexome Disorders: Protective Effects of Treatment. Biomolecules. 2023; 13(2):330. https://doi.org/10.3390/biom13020330
Chicago/Turabian StyleSykora, Matus, Katarina Andelova, Barbara Szeiffova Bacova, Tamara Egan Benova, Adriana Martiskova, Vladimir Knezl, and Narcis Tribulova. 2023. "Hypertension Induces Pro-arrhythmic Cardiac Connexome Disorders: Protective Effects of Treatment" Biomolecules 13, no. 2: 330. https://doi.org/10.3390/biom13020330
APA StyleSykora, M., Andelova, K., Szeiffova Bacova, B., Egan Benova, T., Martiskova, A., Knezl, V., & Tribulova, N. (2023). Hypertension Induces Pro-arrhythmic Cardiac Connexome Disorders: Protective Effects of Treatment. Biomolecules, 13(2), 330. https://doi.org/10.3390/biom13020330





