Anacetrapib, a New CETP Inhibitor: The New Tool for the Management of Dyslipidemias?
Abstract
:1. Introduction
2. Main Results of the REVEAL Trial
2.1. Effects of Anacetrapib on Lipid and Lipoprotein Profile
2.2. Other Effects of Anacetrapib
3. Possible Future Indications of Anacetrapib
4. Conclusions
Author Contributions
Conflicts of Interest
References
- Barter, P.J.; Rye, K.A. Cholesteryl ester transfer protein inhibition as a strategy to reduce cardiovascular risk. J. Lipid. Res. 2012, 53, 1755–1766. [Google Scholar] [CrossRef] [PubMed]
- Tall, A.R. Plasma cholesteryl ester transfer protein. J. Lipid. Res. 1993, 34, 1255–1274. [Google Scholar] [PubMed]
- Barter, P.J.; Rye, K.A. Cholesteryl Ester Transfer Protein Inhibition Is Not Yet Dead-Pro. Arterioscler Thromb Vasc. Biol. 2016, 36, 439–441. [Google Scholar] [CrossRef] [PubMed]
- Barter, P.J.; Caulfield, M.; Eriksson, M.; Grundy, S.M.; Kastelein, J.J.; Komajda, M.; Lopez-Sendon, J.; Mosca, L.; Tardif, J.C.; Waters, D.D.; et al. Effects of torcetrapib in patients at high risk for coronary events. N. Engl. J. Med. 2007, 357, 2109–2122. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, G.G.; Olsson, A.G.; Abt, M.; Ballantyne, C.M.; Barter, P.J.; Brumm, J.; Chaitman, B.R.; Holme, I.M.; Kallend, D.; Leiter, L.A.; et al. Effects of dalcetrapib in patients with a recent acute coronary syndrome. N. Engl. J. Med. 2012, 367, 2089–2099. [Google Scholar] [CrossRef] [PubMed]
- Lincoff, A.M.; Nicholls, S.J.; Riesmeyer, J.S.; Barter, P.J.; Brewer, H.B.; Fox, K.A.A.; Gibson, C.M.; Granger, C.; Menon, V.; Montalescot, G.; et al. Evacetrapib and Cardiovascular Outcomes in High-Risk Vascular Disease. N. Engl. J. Med. 2017, 376, 1933–1942. [Google Scholar] [CrossRef] [PubMed]
- Filippatos, T.D.; Elisaf, M.S. Evacetrapib and cardiovascular outcomes: Reasons for lack of efficacy. J. Thoracic Disease 2017, 9, 2308–2310. [Google Scholar] [CrossRef] [PubMed]
- Filippatos, T.D.; Klouras, E.; Barkas, F.; Elisaf, M. Cholesteryl ester transfer protein inhibitors: Challenges and perspectives. Expert. Rev. Cardiovasc. Ther. 2016, 14, 953–962. [Google Scholar] [CrossRef] [PubMed]
- HPS3/TIMI55-REVEAL Collaborative Group. Effects of Anacetrapib in Patients with Atherosclerotic Vascular Disease. N. Engl. J. Med. 2017, 377, 1217–1227. [Google Scholar]
- Cannon, C.P.; Shah, S.; Dansky, H.M.; Davidson, M.; Brinton, E.A.; Gotto, A.M.; Stepanavage, M.; Liu, S.X.; Gibbons, P.; Ashraf, T.B.; et al. Safety of anacetrapib in patients with or at high risk for coronary heart disease. N. Engl. J. Med. 2010, 363, 2406–2415. [Google Scholar] [CrossRef] [PubMed]
- Kastelein, J.J.; Besseling, J.; Shah, S.; Bergeron, J.; Langslet, G.; Hovingh, G.K.; Al-Saady, N.; Koeijvoets, M.; Hunter, J.; Johnson-Levonas, A.O.; et al. Anacetrapib as lipid-modifying therapy in patients with heterozygous familial hypercholesterolaemia (REALIZE): A randomised, double-blind, placebo-controlled, phase 3 study. Lancet 2015, 385, 2153–2161. [Google Scholar] [CrossRef]
- Millar, J.S.; Lassman, M.E.; Thomas, T.; Ramakrishnan, R.; Jumes, P.; Dunbar, R.L.; de Goma, E.M.; Baer, A.L.; Karmally, W.; Donovan, D.S.; et al. Effects of CETP inhibition with anacetrapib on metabolism of VLDL-TG and plasma apolipoproteins C-II, C-III, and E. J. Lipid Res. 2017, 58, 1214–1220. [Google Scholar] [CrossRef] [PubMed]
- Krauss, R.M.; Pinto, C.A.; Liu, Y.; Johnson-Levonas, A.O.; Dansky, H.M. Changes in LDL particle concentrations after treatment with the cholesteryl ester transfer protein inhibitor anacetrapib alone or in combination with atorvastatin. J. Clin. Lipidol. 2015, 9, 93–102. [Google Scholar] [CrossRef] [PubMed]
- Barter, P.J.; Tabet, F.; Rye, K.A. Reduction in PCSK9 levels induced by anacetrapib: An off-target effect? J. Lipid Res. 2015, 56, 2045–2047. [Google Scholar] [CrossRef] [PubMed]
- Millar, J.S.; Reyes-Soffer, G.; Jumes, P.; Dunbar, R.L.; deGoma, E.M.; Baer, A.L.; Karmally, W.; Donovan, D.S.; Rafeek, H.; Pollan, L.; et al. Anacetrapib lowers LDL by increasing ApoB clearance in mildly hypercholesterolemic subjects. J. Clin. Investig. 2015, 125, 2510–2522. [Google Scholar] [CrossRef] [PubMed]
- Van der Tuin, S.J.; Kuhnast, S.; Berbee, J.F.; Verschuren, L.; Pieterman, E.J.; Havekes, L.M.; van der Hoorn, J.W.; Rensen, P.C.; Jukema, J.W.; Princen, H.M.; et al. Anacetrapib reduces (V)LDL cholesterol by inhibition of CETP activity and reduction of plasma PCSK9. J. Lipid Res. 2015, 56, 2085–2093. [Google Scholar] [CrossRef] [PubMed]
- Filippatos, T.D.; Elisaf, M.S. Are lower levels of LDL-cholesterol really better? Looking at the results of IMPROVE-IT: Opinions of three experts—III. Hellenic. J. Cardiol. 2015, 56, 7–9. [Google Scholar] [PubMed]
- Catapano, A.L.; Graham, I.; De Backer, G.; Wiklund, O.; Chapman, M.J.; Drexel, H.; Hoes, A.W.; Jennings, C.S.; Landmesser, U.; Pedersen, T.R.; et al. 2016 ESC/EAS Guidelines for the Management of Dyslipidaemias. Eur. Heart J. 2016, 37, 2999–3058. [Google Scholar] [CrossRef] [PubMed]
- Baigent, C.; Blackwell, L.; Emberson, J.; Holland, L.E.; Reith, C.; Bhala, N.; Peto, R.; Barnes, E.H.; Keech, A.; Simes, J.; et al. Efficacy and safety of more intensive lowering of LDL cholesterol: A meta-analysis of data from 170,000 participants in 26 randomised trials. Lancet 2010, 376, 1670–1681. [Google Scholar] [PubMed]
- Ference, B.A.; Kastelein, J.J.P.; Ginsberg, H.N.; Chapman, M.J.; Nicholls, S.J.; Ray, K.K.; Packard, C.J.; Laufs, U.; Brook, R.D.; Oliver-Williams, C.; et al. Association of Genetic Variants Related to CETP Inhibitors and Statins With Lipoprotein Levels and Cardiovascular Risk. JAMA 2017, 318, 947–956. [Google Scholar] [CrossRef] [PubMed]
- Thomas, T.; Zhou, H.; Karmally, W.; Ramakrishnan, R.; Holleran, S.; Liu, Y.; Jumes, P.; Wagner, J.A.; Hubbard, B.; Previs, S.F.; et al. CETP (Cholesteryl Ester Transfer Protein) Inhibition With Anacetrapib Decreases Production of Lipoprotein(a) in Mildly Hypercholesterolemic Subjects. Arterioscler Thromb. Vasc. Biol. 2017, 37, 1770–1775. [Google Scholar] [CrossRef] [PubMed]
- Milionis, H.J.; Filippatos, T.D.; Loukas, T.; Bairaktari, E.T.; Tselepis, A.D.; Elisaf, M.S. Serum lipoprotein(a) levels and apolipoprotein(a) isoform size and risk for first-ever acute ischaemic nonembolic stroke in elderly individuals. Atherosclerosis 2006, 187, 170–176. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.L.; Brown, J.M. Anacetrapib-driven triglyceride lowering explained: The fortuitous role of CETP in the intravascular catabolism of triglyceride-rich lipoproteins. J. Lipid Res. 2017, 58, 1031–1032. [Google Scholar] [CrossRef] [PubMed]
- Reyes-Soffer, G.; Millar, J.S.; Ngai, C.; Jumes, P.; Coromilas, E.; Asztalos, B.; Johnson-Levonas, A.O.; Wagner, J.A.; Donovan, D.S.; Karmally, W.; et al. Cholesteryl Ester Transfer Protein Inhibition With Anacetrapib Decreases Fractional Clearance Rates of High-Density Lipoprotein Apolipoprotein A-I and Plasma Cholesteryl Ester Transfer Protein. Arterioscler Thromb. Vasc. Biol. 2016, 36, 994–1002. [Google Scholar] [CrossRef] [PubMed]
- Raal, F.J.; Blom, D.J. Anacetrapib in familial hypercholesterolaemia: Pros and cons. Lancet 2015, 385, 2124–2126. [Google Scholar] [CrossRef]
- Filippatos, T.D.; Filippas-Ntekouan, S.; Pappa, E.; Panagiotopoulou, T.; Tsimihodimos, V.; Elisaf, M.S. PCSK9 and carbohydrate metabolism: A double-edged sword. World J. Diabetes 2017, 8, 311–316. [Google Scholar] [CrossRef] [PubMed]
- Lotta, L.A.; Sharp, S.J.; Burgess, S.; Perry, J.R.B.; Stewart, I.D.; Willems, S.M.; Luan, J.; Ardanaz, E.; Arriola, L.; Balkau, B.; et al. Association Between Low-Density Lipoprotein Cholesterol-Lowering Genetic Variants and Risk of Type 2 Diabetes: A Meta-analysis. JAMA 2016, 316, 1383–1391. [Google Scholar] [CrossRef] [PubMed]
- Filippatos, T.D.; Elisaf, M.S. Effects of ezetimibe/simvastatin combination on metabolic parameters. Int. J. Cardiol. 2016, 202, 273–274. [Google Scholar] [CrossRef] [PubMed]
- Filippatos, T.D.; Elisaf, M.S. Pitavastatin and carbohydrate metabolism: What is the evidence? Expert Rev. Clin. Pharmacol 2016, 9, 955–960. [Google Scholar] [CrossRef] [PubMed]
- Barter, P.J.; Rye, K.A.; Tardif, J.C.; Waters, D.D.; Boekholdt, S.M.; Breazna, A.; Kastelein, J.J. Effect of torcetrapib on glucose, insulin, and hemoglobin A1c in subjects in the Investigation of Lipid Level Management to Understand its Impact in Atherosclerotic Events (ILLUMINATE) trial. Circulation 2011, 124, 555–562. [Google Scholar] [CrossRef] [PubMed]
- Borghi, C.; Cicero, A.F. Pharmacokinetic drug evaluation of anacetrapib for the treatment of dyslipidemia. Expert Opin. Drug Metab. Toxicol. 2017, 13, 205–209. [Google Scholar] [CrossRef] [PubMed]
- Sabatine, M.S.; Giugliano, R.P.; Keech, A.C.; Honarpour, N.; Wiviott, S.D.; Murphy, S.A.; Kuder, J.F.; Wang, H.; Liu, T.; Wasserman, S.M.; et al. Evolocumab and Clinical Outcomes in Patients with Cardiovascular Disease. N. Engl. J. Med. 2017, 376, 1713–1722. [Google Scholar] [CrossRef] [PubMed]
- Filippatos, T.D.; Kei, A.; Rizos, C.V.; Elisaf, M.S. Effects of PCSK9 Inhibitors on Other than Low-Density Lipoprotein Cholesterol Lipid Variables. J. Cardiovasc. Pharmacol Ther. 2017. [Google Scholar] [CrossRef] [PubMed]
- Hovingh, G.K.; Kastelein, J.J.; Van Deventer, S.J.; Round, P.; Ford, J.; Saleheen, D.; Rader, D.J.; Brewer, H.B.; Barter, P.J. Cholesterol ester transfer protein inhibition by TA-8995 in patients with mild dyslipidaemia (TULIP): A randomised, double-blind, placebo-controlled phase 2 trial. Lancet 2015, 386, 452–460. [Google Scholar] [CrossRef]
- Miyosawa, K.; Watanabe, Y.; Murakami, K.; Murakami, T.; Shibata, H.; Iwashita, M.; Yamazaki, H.; Yamazaki, K.; Ohgiya, T.; Shibuya, K.; et al. New CETP inhibitor K-312 reduces PCSK9 expression: A potential effect on LDL cholesterol metabolism. Am. J. Physiol. Endocrinol. Metab. 2015, 309, E177–190. [Google Scholar] [CrossRef] [PubMed]
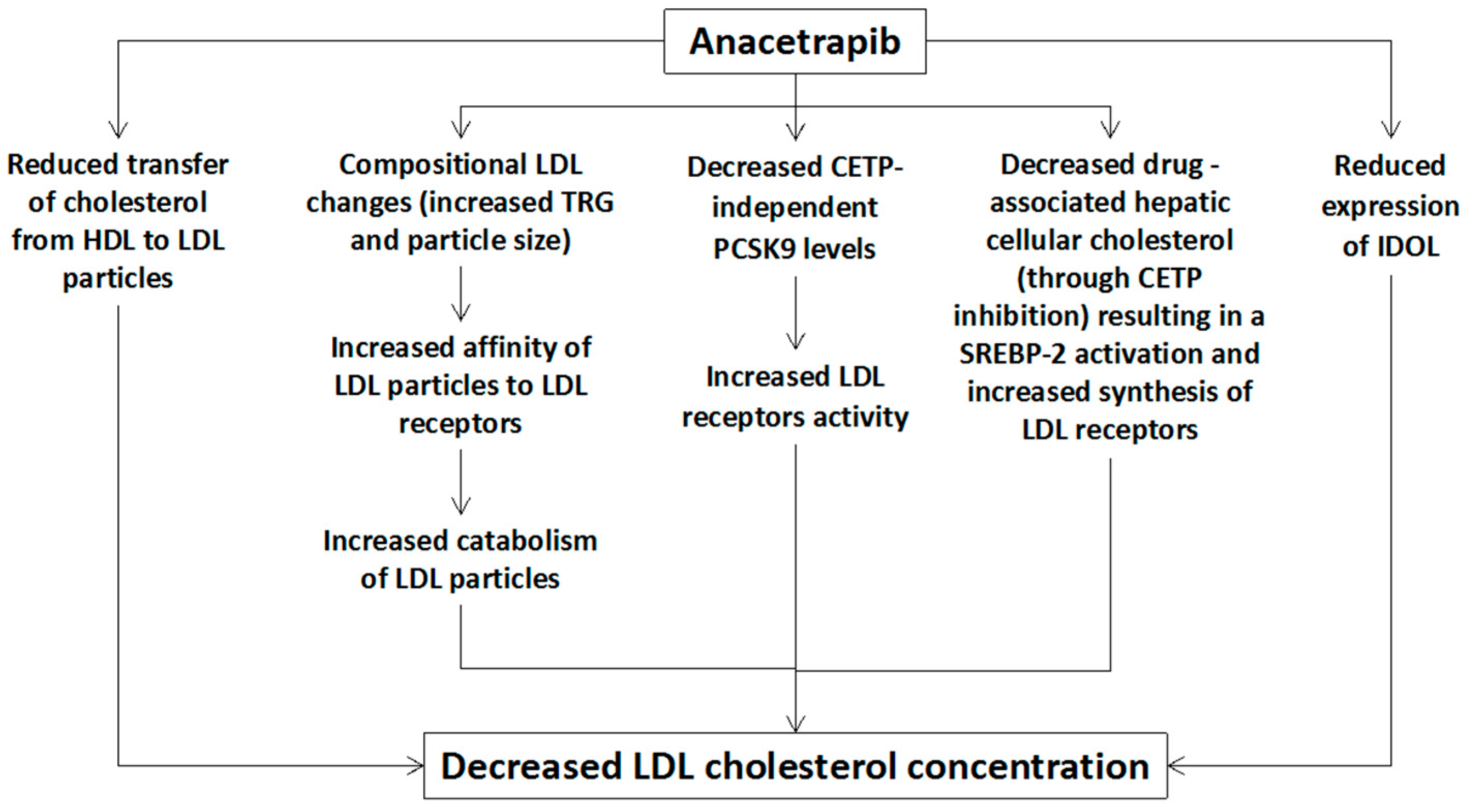
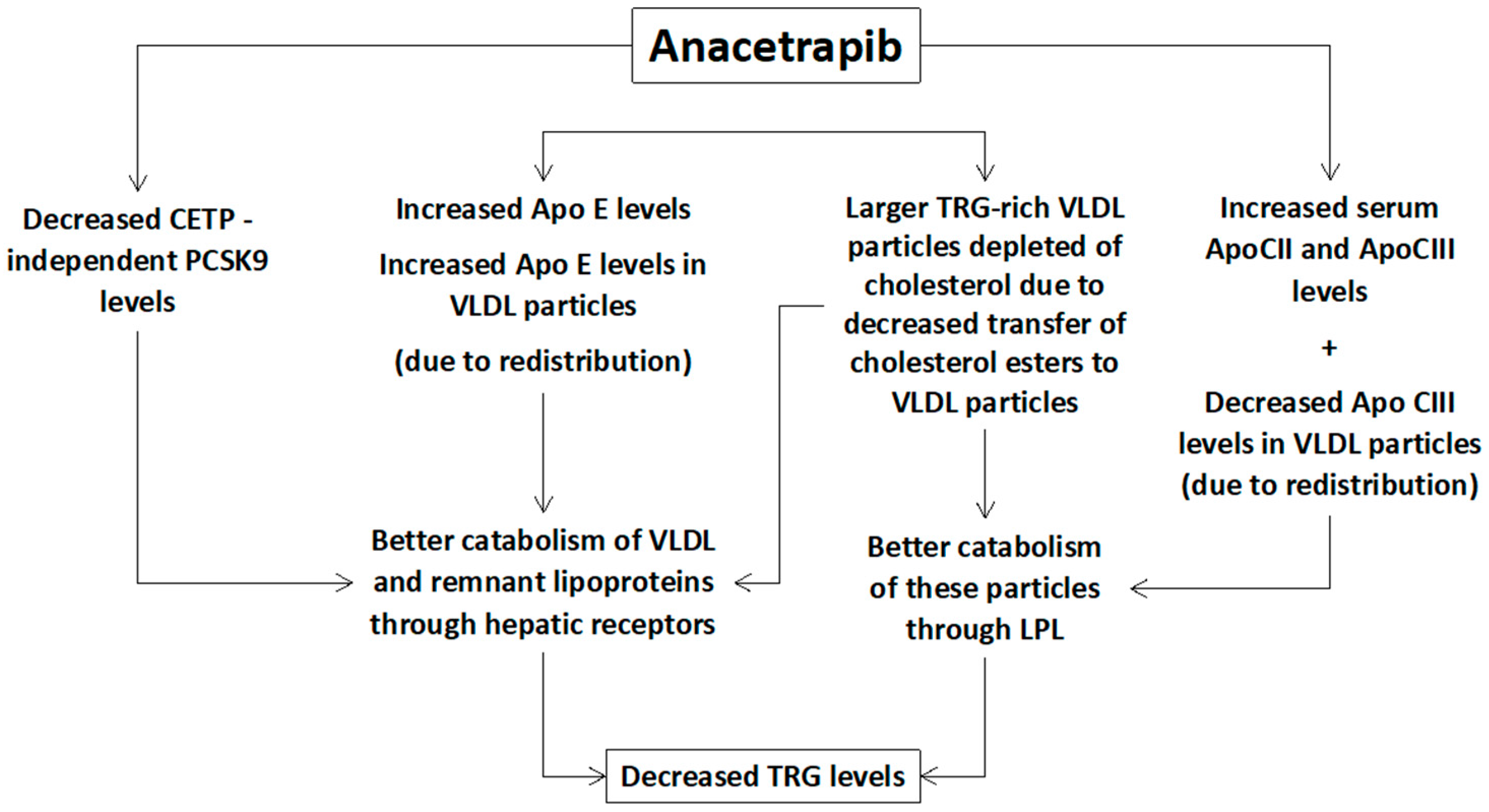
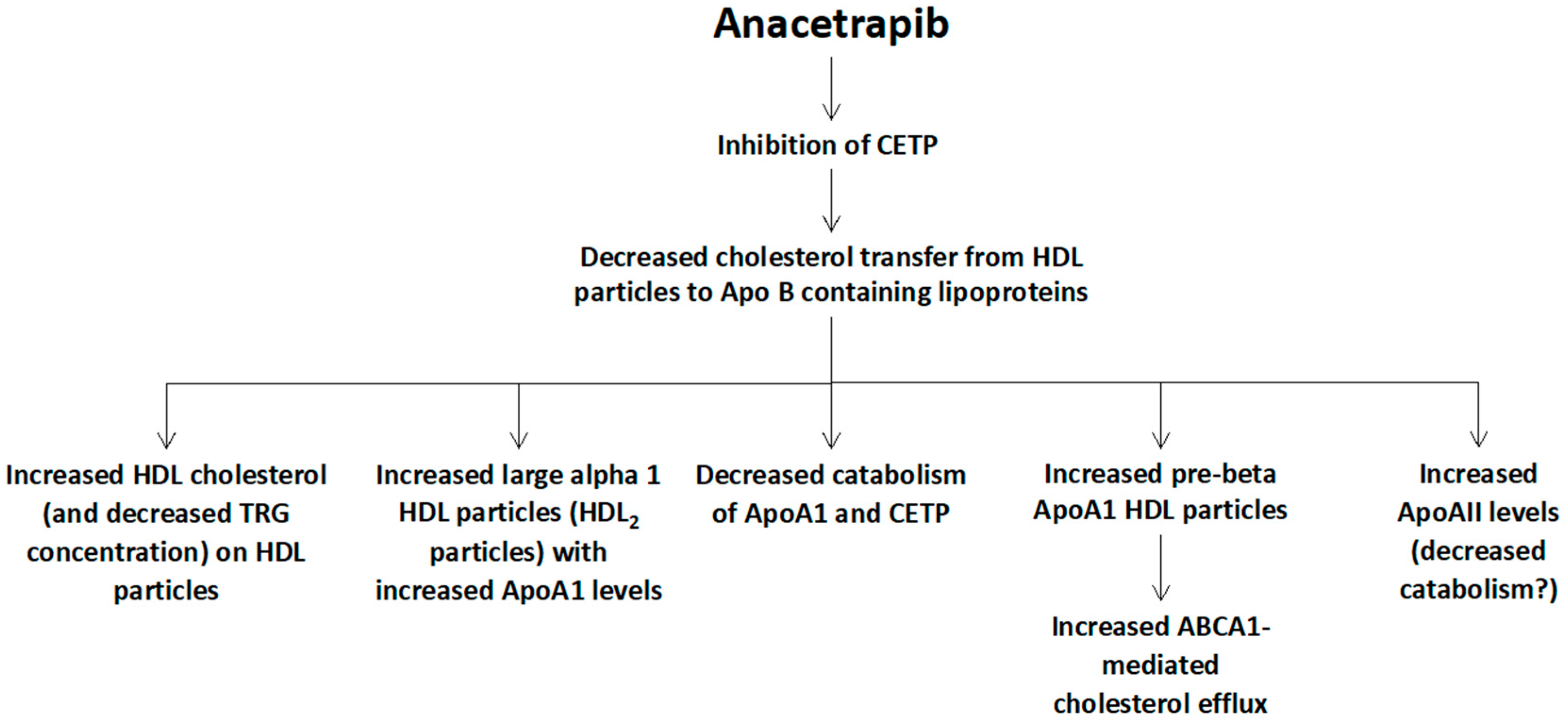
| Lipid Parameters | REALIZE Trial [11] (Patients with Familial Hypercholesterolemia) | DEFINE Trial [10] (Patients with Coronary Heart Disease or at Risk for Coronary Heart Disease) | REVEAL Trial [9] (Patients with Atherosclerotic Vascular Disease) * |
|---|---|---|---|
| LDL cholesterol | −39.7% ** | −39.8% *** | −41% (direct method) −17% ** (in a subgroup of 2000 patients) |
| HDL cholesterol | +102.1% | +138.1% | +104% |
| Non-HDL cholesterol | −36.4% | −31.7% | −18% |
| Apo B | −24.8% | −21% | −18% |
| Apo AI | +32.9% | +44.7% | +36% |
| Lp(a) | −27.9% | −36.4% | −25% |
| TRG | −5.5% | −6.8% | −7% |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Filippatos, T.D.; Kei, A.; Elisaf, M.S. Anacetrapib, a New CETP Inhibitor: The New Tool for the Management of Dyslipidemias? Diseases 2017, 5, 21. https://doi.org/10.3390/diseases5040021
Filippatos TD, Kei A, Elisaf MS. Anacetrapib, a New CETP Inhibitor: The New Tool for the Management of Dyslipidemias? Diseases. 2017; 5(4):21. https://doi.org/10.3390/diseases5040021
Chicago/Turabian StyleFilippatos, Theodosios D., Anastazia Kei, and Moses S. Elisaf. 2017. "Anacetrapib, a New CETP Inhibitor: The New Tool for the Management of Dyslipidemias?" Diseases 5, no. 4: 21. https://doi.org/10.3390/diseases5040021
APA StyleFilippatos, T. D., Kei, A., & Elisaf, M. S. (2017). Anacetrapib, a New CETP Inhibitor: The New Tool for the Management of Dyslipidemias? Diseases, 5(4), 21. https://doi.org/10.3390/diseases5040021






