Survival Analysis and Contributing Factors among PCR-Confirmed Adult Inpatients during the Endemic Phase of COVID-19
Abstract
:1. Introduction
2. Materials and Methods
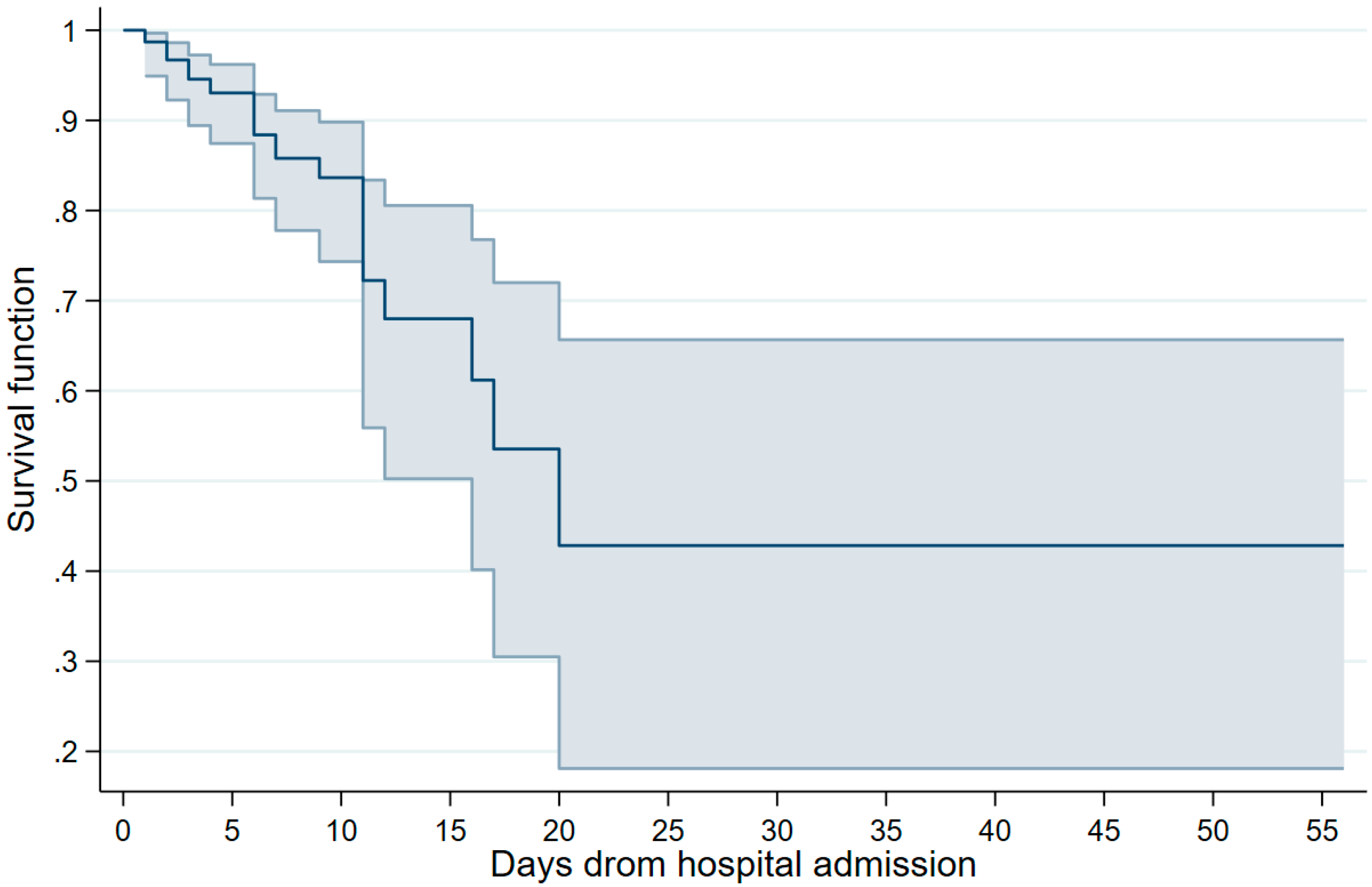
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Balqis-Ali, N.Z.; Fun, W.H.; Ismail, M.; Ng, R.J.; Jaaffar, F.S.A.; Low, L.L. Addressing Gaps for Health Systems Strengthening: A Public Perspective on Health Systems’ Response towards COVID-19. Int. J. Environ. Res. Public. Health 2021, 18, 9047. [Google Scholar] [CrossRef] [PubMed]
- Haque, A.; Pant, A.B. Mitigating COVID-19 in the face of emerging virus variants, breakthrough infections and vaccine hesitancy. J. Autoimmun. 2022, 127, 102792. [Google Scholar] [CrossRef] [PubMed]
- United Nations. UN News: WHO Chief Declares End to COVID-19 as a Global Health Emergency. Available online: https://news.un.org/en/story/2023/05/1136367#:~:text=WHO%20chief%20declares%20end%20to%20COVID%2D19%20as%20a%20global%20health%20emergency,-5%20May%202023&text=The%20head%20of%20the%20UN,no%20longer%20a%20global%20threat (accessed on 12 August 2023).
- National Autonomous University of Mexico. UNAM’s Geographic Information Platform on COVID-19 in Mexico. Available online: https://covid19.ciga.unam.mx/ (accessed on 10 August 2023). (In Spanish).
- Leach, M.; MacGregor, H.; Scoones, I.; Wilkinson, A. Post-pandemic transformations: How and why COVID-19 requires us to rethink development. World Dev. 2021, 138, 105233. [Google Scholar] [CrossRef] [PubMed]
- Michelen, M.; Manoharan, L.; Elkheir, N.; Cheng, V.; Dagens, A.; Hastie, C.; O’Hara, M.; Suett, J.; Dahmash, D.; Bugaeva, P. Characterising long COVID: A living systematic review. BMJ Glob. Health 2021, 6, e005427. [Google Scholar] [CrossRef] [PubMed]
- Murillo-Zamora, E.; Hernandez-Suarez, C.M. Survival in adult inpatients with COVID-19. Public Health 2021, 190, 1–3. [Google Scholar] [CrossRef] [PubMed]
- General Directorate of Epidemiology of Mexico. Standardized Guideline for Epidemiological and Laboratory Surveillance of Viral Respiratory Disease. 2022. Available online: https://www.gob.mx/salud/documentos/lineamiento-estandarizado-para-la-vigilancia-epidemiologica-y-por-laboratorio-de-la-enfermedad-respiratoria-viral (accessed on 11 August 2023). (In Spanish).
- Fernandes-Matano, L.; Monroy-Munoz, I.E.; Bermudez de Leon, M.; Leal-Herrera, Y.A.; Palomec-Nava, I.D.; Ruiz-Pacheco, J.A.; Escobedo-Guajardo, B.L.; Marin-Budip, C.; Santacruz-Tinoco, C.E.; Gonzalez-Ibarra, J.; et al. Analysis of influenza data generated by four epidemiological surveillance laboratories in Mexico, 2010–2016. Epidemiol. Infect. 2019, 147, e183. [Google Scholar] [CrossRef] [PubMed]
- Corman, V.M.; Landt, O.; Kaiser, M.; Molenkamp, R.; Meijer, A.; Chu, D.K.; Bleicker, T.; Brunink, S.; Schneider, J.; Schmidt, M.L.; et al. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Euro Surveill. 2020, 25, 2000045. [Google Scholar] [CrossRef] [PubMed]
- Murillo-Zamora, E.; Guzman-Esquivel, J.; Bricio-Barrios, J.A.; Mendoza-Cano, O. Comparing the survival of adult inpatients with COVID-19 during the wild-type, Delta, and Omicron emergence. Public Health 2022, 213, 124–126. [Google Scholar] [CrossRef] [PubMed]
- Mahamat-Saleh, Y.; Fiolet, T.; Rebeaud, M.E.; Mulot, M.; Guihur, A.; El Fatouhi, D.; Laouali, N.; Peiffer-Smadja, N.; Aune, D.; Severi, G. Diabetes, hypertension, body mass index, smoking and COVID-19-related mortality: A systematic review and meta-analysis of observational studies. BMJ Open 2021, 11, e052777. [Google Scholar] [CrossRef] [PubMed]
- Varikasuvu, S.R.; Dutt, N.; Thangappazham, B.; Varshney, S. Diabetes and COVID-19: A pooled analysis related to disease severity and mortality. Prim. Care Diabetes 2021, 15, 24–27. [Google Scholar] [CrossRef] [PubMed]
- Hernandez-Suarez, C.; Murillo-Zamora, E. Waning immunity to SARS-CoV-2 following vaccination or infection. Front. Med. 2022, 9, 972083. [Google Scholar] [CrossRef] [PubMed]
- Pecly, I.M.D.; Azevedo, R.B.; Muxfeldt, E.S.; Botelho, B.G.; Albuquerque, G.G.; Diniz, P.H.P.; Silva, R.; Rodrigues, C.I.S. COVID-19 and chronic kidney disease: A comprehensive review. J. Bras. Nefrol. 2021, 43, 383–399. [Google Scholar] [CrossRef] [PubMed]
- Mahalingasivam, V.; Su, G.; Iwagami, M.; Davids, M.R.; Wetmore, J.B.; Nitsch, D. COVID-19 and kidney disease: Insights from epidemiology to inform clinical practice. Nat. Rev. Nephrol. 2022, 18, 485–498. [Google Scholar] [CrossRef] [PubMed]
- Galmiche, S.; Luong Nguyen, L.B.; Tartour, E.; de Lamballerie, X.; Wittkop, L.; Loubet, P.; Launay, O. Immunological and clinical efficacy of COVID-19 vaccines in immunocompromised populations: A systematic review. Clin. Microbiol. Infect. 2022, 28, 163–177. [Google Scholar] [CrossRef] [PubMed]
- Goldman, J.D.; Robinson, P.C.; Uldrick, T.S.; Ljungman, P. COVID-19 in immunocompromised populations: Implications for prognosis and repurposing of immunotherapies. J. Immunother. Cancer 2021, 9, e002630. [Google Scholar] [CrossRef] [PubMed]
- Culqui, D.R.; Ortega Segura, J.; Da Costa-Venancio, E.; Renom-Guiteras, A.; Roquer, E.; Muñoz Tejada, S.M.; Rodriguez, P.; Alba Travieso, A.L.; Medrano, I.; Canchucaja-Gutarra, L. Risk factors associated with the mortality of COVID-19 patients aged ≥60 years neither Intubated nor treated with mechanical ventilation: A multicentre retrospective cohort study during the first wave in Spain. BioMed 2022, 2, 341–358. [Google Scholar] [CrossRef]
| Characteristic | In-Hospital Outcome | p | Follow-Up (Days) | |
|---|---|---|---|---|
| Recovery | Death | |||
| Gender | ||||
| Female | 75 (59.1) | 10 (40.0) | 0.079 | 651 |
| Male | 52 (40.9) | 15 (60.0) | 492 | |
| Age (years, median and IQR) | 62 (42–76) | 68 (59–81) | 0.156 | 1143 |
| COVID-19 vaccination status | ||||
| Not vaccinated | 101 (79.5) | 20 (80.0) | 0.973 | 910 |
| One dose | 1 (0.8) | 0 (0) | 7 | |
| Two doses | 16 (12.6) | 3 (12.0) | 129 | |
| Three doses | 9 (7.1) | 2 (8.0) | 97 | |
| Pneumonia at hospital admission | ||||
| No | 109 (85.8) | 15 (60.0) | 0.002 | 923 |
| Yes | 18 (14.2) | 10 (40.0) | 220 | |
| Personal history of: | ||||
| Tobacco use, yes | 5 (3.9) | 3 (12.0) | 0.099 | 71 |
| Obesity (BMI ≥ 30), yes | 15 (11.8) | 5 (20.0) | 0.268 | 150 |
| Asthma, yes | 4 (3.2) | 0 (0) | 0.369 | 22 |
| COPD, yes | 11 (8.7) | 2 (8.0) | 0.914 | 119 |
| Type 2 diabetes mellitus, yes | 26 (20.5) | 12 (52.0) | 0.001 | 261 |
| Arterial hypertension, yes | 38 (29.9) | 11 (44.0) | 0.169 | 317 |
| CKD, yes | 8 (6.3) | 7 (28.0) | 0.001 | 74 |
| Immunosuppression (any cause), yes | 2 (1.6) | 5 (20.0) | < 0.001 | 53 |
| Characteristic | HR (95% CI), p | |
|---|---|---|
| Bivariate Analysis | Multivariate Analysis | |
| Gender | ||
| Female | 1.00 | 1.00 |
| Male | 2.10 (0.94–4.69), 0.071 | 2.79 (0.92–8.49), 0.067 |
| Age (per each additional year) | 1.01 (0.99–1.03), 0.276 | 1.02 (0.99–1.04), 0.236 |
| COVID-19 vaccination status | ||
| Not vaccinated | 1.00 | 1.00 |
| One dose | 0.73 (0.16–3.70), 0.685 | 0.50 (0.11–2.63), 0.482 |
| Two doses | 1.11 (0.33–3.81), 0.861 | 0.59 (0.13–2.66), 0.497 |
| Three doses | 0.76 (0.17–3.27), 0.707 | 0.70 (0.13–3.66), 0.668 |
| Pneumonia at hospital admission | ||
| No | 1.00 | 1.00 |
| Yes | 2.38 (1.06–5.37), 0.036 | 1.97 (0.78–4.99), 0.151 |
| Personal history of: | ||
| Type 2 diabetes mellitus | ||
| No | 1.00 | 1.00 |
| Yes | 3.35 (1.52–7.35), 0.003 | 2.33 (0.93–5.88), 0.056 |
| CKD | ||
| No | 1.00 | 1.00 |
| Yes | 5.41 (2.22–13.17), <0.001 | 3.43 (1.07–11.0), 0.038 |
| Immunosuppression (any cause) | ||
| No | 1.00 | 1.00 |
| Yes | 4.39 (1.61–11.96), 0.004 | 6.44 (1.49–17.8), 0.013 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Benites-Godínez, V.; Mendoza-Cano, O.; Trujillo, X.; Ríos-Silva, M.; Lugo-Radillo, A.; Bricio-Barrios, J.A.; Cuevas-Arellano, H.B.; Ríos-Bracamontes, E.F.; Serrano-Moreno, W.; Cárdenas, Y.; et al. Survival Analysis and Contributing Factors among PCR-Confirmed Adult Inpatients during the Endemic Phase of COVID-19. Diseases 2023, 11, 119. https://doi.org/10.3390/diseases11030119
Benites-Godínez V, Mendoza-Cano O, Trujillo X, Ríos-Silva M, Lugo-Radillo A, Bricio-Barrios JA, Cuevas-Arellano HB, Ríos-Bracamontes EF, Serrano-Moreno W, Cárdenas Y, et al. Survival Analysis and Contributing Factors among PCR-Confirmed Adult Inpatients during the Endemic Phase of COVID-19. Diseases. 2023; 11(3):119. https://doi.org/10.3390/diseases11030119
Chicago/Turabian StyleBenites-Godínez, Verónica, Oliver Mendoza-Cano, Xóchitl Trujillo, Mónica Ríos-Silva, Agustin Lugo-Radillo, Jaime Alberto Bricio-Barrios, Herguin Benjamin Cuevas-Arellano, Eder Fernando Ríos-Bracamontes, Walter Serrano-Moreno, Yolitzy Cárdenas, and et al. 2023. "Survival Analysis and Contributing Factors among PCR-Confirmed Adult Inpatients during the Endemic Phase of COVID-19" Diseases 11, no. 3: 119. https://doi.org/10.3390/diseases11030119
APA StyleBenites-Godínez, V., Mendoza-Cano, O., Trujillo, X., Ríos-Silva, M., Lugo-Radillo, A., Bricio-Barrios, J. A., Cuevas-Arellano, H. B., Ríos-Bracamontes, E. F., Serrano-Moreno, W., Cárdenas, Y., Baltazar-Rodríguez, G. M., Ortega-Ramírez, A. D., & Murillo-Zamora, E. (2023). Survival Analysis and Contributing Factors among PCR-Confirmed Adult Inpatients during the Endemic Phase of COVID-19. Diseases, 11(3), 119. https://doi.org/10.3390/diseases11030119








