Examining the Effect of Context, Beliefs, and Values on UK Farm Veterinarians’ Antimicrobial Prescribing: A Randomized Experimental Vignette and Cross-Sectional Survey
Abstract
1. Introduction
1.1. Context
1.2. Beliefs
1.3. Values
1.4. Aims and Hypotheses
1.4.1. Vignette Condition (Context)
- Hypothesis 1a. Vets provided with contextual information will be more likely to prescribe antibiotics, compared to the control condition (clinical information only provided);
- Hypothesis 1b. The likelihood of prescribing antibiotics will differ between the three different contextual (experimental) conditions. The four vignette conditions were control (clinical information only), economics (farm under financial pressure), farmer (farmer under work pressure), and relationship (vet-client relationship under pressure).
1.4.2. Beliefs about Responsibility for Causing and Preventing AMR
- Hypotheses 2a, 2b. There will be a difference in the level of responsibility that vets believe different groups have for (a) causing AMR and (b) preventing AMR;
- Hypotheses 2c, 2d. Vets’ beliefs about which groups have responsibility for (c) causing AMR and (d) preventing AMR will be associated with vets’ antibiotic prescribing.
1.4.3. Values
- Hypotheses 3a, 3b. Vets who are (a) more hedonic and (b) more egoistic will be more likely to prescribe antibiotics;
- Hypotheses 3c, 3d. Vets who are (c) more altruistic and (d) more biospheric will be less likely to prescribe antibiotics.
2. Results
2.1. Distribution and Baseline Checks
2.2. Impact of Vignette Condition on Prescribing
2.3. Vets’ Beliefs about Groups’ Responsibility for Causing and Preventing AMR
2.4. Impact of Beliefs on Prescribing
2.5. Vets’ Values
2.6. Impact of Values on Prescribing
3. Discussion
Limitations
4. Materials and Methods
4.1. Design
4.2. Participants
Power Calculation
4.3. Experimental Materials and Measures
4.3.1. The Vignette
Imagine you have been called to a dairy farm to examine a sick dry cow. She is bright and alert, but has nasal discharge and a rectal temperature of 39.2 °C. You find no other clinical abnormalities. You are aware that there has been a recent laboratory confirmation of IBR (infectious bovine rhinotracheitis) in the herd, which was previously naive to IBR.[Control].
You are familiar with this farm business and know that it has been having real financial difficulties for quite some time now.[Economics].
You know this farmer is well trained and usually diligent, but he says his herdsman who usually manages the cows day-to-day has recently resigned and has yet to be replaced. It is obvious that the farmer is run off his feet and keeping an eye on this cow is likely to be a low priority for him right now.[Farmer].
You have known this farmer for a while and the last time you visited him it was quite tense, and he wasn’t happy with some of your decisions. As you are examining the cow, you hear the farmer grumbling.[Relationship].
4.3.2. Outcome Measure: Antibiotic Prescribing Behavior
Below are some common treatment options that vets might recommend in this scenario. Thinking about your own day-to-day practice, please indicate to what extent you would be likely to recommend each of the following options in the above scenario.
4.4. Cross-Sectional Measures
4.4.1. Demographics
4.4.2. Values
4.4.3. Beliefs: Responsibility for Causing AMR and Responsibility for Preventing AMR
4.4.4. Reliability
4.5. Procedure
Allocation and Randomization
4.6. Data Analysis
4.7. Ethics
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| To What Extent Do You Think Each of the Following Contributes to Causing Antimicrobial Resistance? | 1 Not at all | 2 Very little | 3 Somewhat | 4 Quite a bit | 5 Very much | |
|---|---|---|---|---|---|---|
| [Healthcare Professionals] | The number of antibiotic prescriptions that GPs write | |||||
| The amount of antibiotic use in hospitals | ||||||
| Levels of compliance with hand hygiene protocols in hospitals | ||||||
| GPs prescribing antibiotics for colds | ||||||
| [The Public] | Patients requesting antibiotics from their doctors | |||||
| Patients not completing their antibiotic courses | ||||||
| Members of the public sharing antibiotic prescriptions | ||||||
| Food hygiene practices by members of the public in their homes 1 | ||||||
| [Companion Animal Vets] | The number of antibiotic prescriptions issued by companion animal vets | |||||
| Companion animal vets prescribing single, long-acting doses of antibiotics | ||||||
| Companion animal vets prescribing antibiotics when the aetiology has not been confirmed by diagnostics | ||||||
| Levels of compliance with infection control protocols in companion animal veterinary practices | ||||||
| [Pet Owners] | Pet owners expecting antibiotics for their animals | |||||
| Pet owners disagreeing with their vet’s advice when they are not given antibiotics for their animals | ||||||
| Pet owners not giving their animals the complete course of antibiotics | ||||||
| Pets sleeping on their owners’ beds 1 | ||||||
| [Farm Animal Vets] | The level of attention paid by farm animal vets to their clients’ antibiotic use | |||||
| Farm animal vets prescribing antibiotics for infections that could be viral | ||||||
| Levels of compliance with biosecurity protocols on farm by farm animal vets | ||||||
| The amount of antibiotics that farm animal vets prescribe | ||||||
| [Farmers] | Farmers using antibiotics to treat viral infections | |||||
| Farmers using antibiotics to compensate for issues with husbandry | ||||||
| Standards of biosecurity on farms | ||||||
| Farmers not administering antibiotics correctly |
| To What Extent Do You Think Each of the Following Contributes to Preventing Antimicrobial Resistance? | 1 Not at all | 2 Very little | 3 Somewhat | 4 Quite a bit | 5 Very much | |
|---|---|---|---|---|---|---|
| [Healthcare Professionals] | GPs explaining to patients why antibiotics are not always needed | |||||
| GPs advising patients about self-care for colds | ||||||
| Hospitals implementing antibiotic stewardship policies | ||||||
| Pharmacists being trained to challenge antibiotic prescriptions they think are unnecessary 1 | ||||||
| [The Public] | Members of the public taking antibiotics as instructed by their doctors | |||||
| Members of the public taking more care over hygienic food preparation 1 | ||||||
| The public visiting pharmacists for advice about self-care when they have a cold | ||||||
| Patients accepting their GP’s advice when they are not prescribed antibiotics | ||||||
| [Companion Animal Vets] | Companion animal vets improving their infection control practices | |||||
| Companion animal vets using more diagnostic tests | ||||||
| Companion animal veterinary practices developing antibiotic stewardship policies | ||||||
| Companion animal vets educating pet owners about why antibiotics are not always necessary | ||||||
| [Pet Owners] | Pet owners following the treatment advice of their vets | |||||
| Pet owners ensuring they give their pets complete courses of antibiotics | ||||||
| Pet owners washing their hands more thoroughly after handling their animals 1 | ||||||
| Pet owners accepting that their animals don’t always need antibiotics | ||||||
| [Farm Animal Vets] | Farm animal vets making use of diagnostic tests | |||||
| Farm animal vets adopting antibiotic stewardship policies | ||||||
| Farm animal vets refusing farmers’ requests for antibiotics that aren’t really needed | ||||||
| Farm animal vets advising farmers on measures to reduce infection rates | ||||||
| [Farmers] | Farmers reducing the level of antibiotics used in livestock | |||||
| Farmers improving nutrition and housing conditions for livestock | ||||||
| Education for farmers about antibiotic stewardship | ||||||
| Farmers complying with their vet’s treatment instructions |
References
- World Health Organization. Global Action Plan on Antimicrobial Resistance; World Health Organization: Geneva, Switzerland, 2015. [Google Scholar]
- Review on AMR. Rapid Diagnostics: Stopping Unnecessary use of Antibiotics; Review on AMR: London, UK, 2015. [Google Scholar]
- Dyar, O.J.; Beović, B.; Vlahović-Palčevski, V.; Verheij, T.J.M.; Pulcini, C. How can we improve antibiotic prescribing in primary care? Expert Rev. Anti. Infect. Ther. 2016, 14, 403–413. [Google Scholar] [CrossRef]
- Hughes, L.A.; Williams, N.J.; Clegg, P.; Callaby, R.; Nuttall, T.; Coyne, K.; Pinchbeck, G.L.; Dawson, S. Cross-sectional survey of antimicrobial prescribing patterns in UK small animal veterinary practice. Prev. Vet. Med. 2012, 104, 309–316. [Google Scholar] [CrossRef] [PubMed]
- Trauffler, M.; Griesbacher, A.; Fuchs, K.; Köfer, J. Antimicrobial drug use in Austrian pig farms: Plausibility check of electronic on-farm records and estimation of consumption. Vet. Rec. 2014, 175, 402. [Google Scholar] [CrossRef] [PubMed]
- Gibbons, J.F.; Boland, F.; Buckley, J.F.; Butler, F.; Egan, J.; Fanning, S.; Markey, B.K.; Leonard, F.C. Influences on antimicrobial prescribing behaviour of veterinary practitioners in cattle practice in Ireland. Vet. Rec. 2013, 172, 14. [Google Scholar] [CrossRef]
- Mattick, K.; Kelly, N.; Rees, C. A window into the lives of junior doctors: Narrative interviews exploring antimicrobial prescribing experiences. J. Antimicrob. Chemother. 2014, 69, 2274–2283. [Google Scholar] [CrossRef] [PubMed]
- King, C.; Smith, M.; Currie, K.; Dickson, A.; Smith, F.; Davis, M.; Flowers, P. Exploring the behavioural drivers of veterinary surgeon antibiotic prescribing: A qualitative study of companion animal veterinary surgeons in the UK. BMC Vet. Res. 2018, 14, 332. [Google Scholar] [CrossRef]
- Potthoff, S.; Rasul, O.; Sniehotta, F.F.; Marques, M.; Beyer, F.; Thomson, R.; Avery, L.; Presseau, J. The relationship between habit and healthcare professional behaviour in clinical practice: A systematic review and meta-analysis. Health Psychol. Rev. 2019, 13, 73–90. [Google Scholar] [CrossRef]
- Doidge, C.; Hudson, C.D.; Lovatt, F.; Kaler, J. To prescribe or not to prescribe? A factorial survey to explore veterinarians’ decision making when prescribing antimicrobials to sheep and beef farmers in the UK. PLoS ONE 2019, 14, e0213855. [Google Scholar] [CrossRef]
- Krockow, E.M.; Colman, A.M.; Chattoe-Brown, E.; Jenkins, D.R.; Perera, N.; Mehtar, S.; Tarrant, C. Balancing the risks to individual and society: A systematic review and synthesis of qualitative research on antibiotic prescribing behaviour in hospitals. J. Hosp. Infect. 2019, 101, 428–439. [Google Scholar] [CrossRef]
- Higgins, H.M.; Dryden, I.L.; Green, M.J. A Bayesian elicitation of veterinary beliefs regarding systemic dry cow therapy: Variation and importance for clinical trial design. Prev. Vet. Med. 2012, 106, 87–96. [Google Scholar] [CrossRef] [PubMed]
- Smith, M.; King, C.; Davis, M.; Dickson, A.; Park, J.; Smith, F.; Currie, K.; Flowers, P. Pet owner and vet interactions: Exploring the drivers of AMR. Antimicrob. Resist. Infect. Control 2018, 7, 46. [Google Scholar] [CrossRef]
- Buller, H.J.; Hinchliffe, S.; Hockenhull, J.; Barrett, D.C.; Reyher, K.K.; Butterworth, A.; Heath, C. Systematic review and social research to further understanding of current practice in the context of using antimicrobials in livestock farming and to inform appropriate interventions to reduce antimicrobial resistance within the livestock sector. Dep. Environ. Food Rural Aff. 2015. [Google Scholar]
- Om, C.; Daily, F.; Vlieghe, E.; McLaughlin, J.C.; McLaws, M.-L. “If it’s a broad spectrum, it can shoot better”: Inappropriate antibiotic prescribing in Cambodia. Antimicrob. Resist. Infect. Control 2016, 5, 58. [Google Scholar] [CrossRef] [PubMed]
- Cattaneo, A.A.; Wilson, R.; Doohan, D.; LeJeune, J.T. Bovine veterinarians’ knowledge, beliefs, and practices regarding antibiotic resistance on Ohio dairy farms. J. Dairy Sci. 2009, 92, 3494–3502. [Google Scholar] [CrossRef] [PubMed]
- Coyne, L.A.; Pinchbeck, G.L.; Williams, N.J.; Smith, R.F.; Dawson, S.; Pearson, R.B.; Latham, S.M. Understanding antimicrobial use and prescribing behaviours by pig veterinary surgeons and farmers: A qualitative study. Vet. Rec. 2014, 175, 593. [Google Scholar] [CrossRef] [PubMed]
- Trivedi, K.K.; Dumartin, C.; Gilchrist, M.; Wade, P.; Howard, P. Identifying best practices across three countries: Hospital antimicrobial stewardship in the United Kingdom, France, and the United States. Clin. Infect. Dis. 2014, 59, S170–S178. [Google Scholar] [CrossRef]
- Hopman, N.E.M.; Hulscher, M.E.J.L.; Graveland, H.; Speksnijder, D.C.; Wagenaar, J.A.; Broens, E.M. Factors influencing antimicrobial prescribing by Dutch companion animal veterinarians: A qualitative study. Prev. Vet. Med. 2018, 158, 106–113. [Google Scholar] [CrossRef] [PubMed]
- Hardefeldt, L.Y.; Gilkerson, J.R.; Billman-Jacobe, H.; Stevenson, M.A.; Thursky, K.A.; Bailey, K.E.; Browning, G.F. Barriers to and enablers of implementing antimicrobial stewardship programs in veterinary practices. J. Vet. Intern. Med. 2018, 32, 1092–1099. [Google Scholar] [CrossRef]
- Servia-Dopazo, M.; Taracido-Trunk, M.; Figueiras, A. Non-clinical factors determining the prescription of antibiotics by veterinarians: A systematic review. Antibiotics 2021, 10, 133. [Google Scholar] [CrossRef] [PubMed]
- Tonkin-Crine, S.; Yardley, L.; Little, P. Antibiotic prescribing for acute respiratory tract infections in primary care: A systematic review and meta-ethnography. J. Antimicrob. Chemother. 2011, 66, 2215–2223. [Google Scholar] [CrossRef]
- Pinder, R.; Sallis, A.; Berry, D.; Chadborn, T. Behaviour change and antibiotic prescribing in healthcare settings: Literature review and behavioural analysis. Public Health Engl. 2015. [Google Scholar] [CrossRef]
- Papoutsi, C.; Mattick, K.; Pearson, M.; Brennan, N.; Briscoe, S.; Wong, G. Social and professional influences on antimicrobial prescribing for doctors-in-training: A realist review. J. Antimicrob. Chemother. 2017, 72, 2418–2430. [Google Scholar] [CrossRef]
- Tafa, B.; Endale, A.; Bekele, D. Paramedical staffs knowledge and attitudes towards antimicrobial resistance in Dire Dawa, Ethiopia: A cross sectional study. Ann. Clin. Microbiol. Antimicrob. 2017, 16, 64. [Google Scholar] [CrossRef] [PubMed]
- Rowbotham, S.; Chisholm, A.; Moschogianis, S.; Chew-Graham, C.; Cordingley, L.; Wearden, A.; Peters, S. Challenges to nurse prescribers of a no-antibiotic prescribing strategy for managing self-limiting respiratory tract infections. J. Adv. Nurs. 2012, 68, 2622–2632. [Google Scholar] [CrossRef] [PubMed]
- Hockenhull, J.; Turner, A.E.; Reyher, K.K.; Barrett, D.C.; Jones, L.; Hinchliffe, S.; Buller, H.J. Antimicrobial use in food-producing animals: A rapid evidence assessment of stakeholder practices and beliefs. Vet. Rec. 2017, 181, 510. [Google Scholar] [CrossRef] [PubMed]
- Redding, L.E.; Lavigne, S.; Aceto, H.; Nolen-Walston, R. Characterization of antimicrobial prescription frequency and diversity in a large animal veterinary medical teaching hospital. Prev. Vet. Med. 2019, 168, 66–74. [Google Scholar] [CrossRef] [PubMed]
- Chipangura, J.K.; Eagar, H.; Kgoete, M.; Abernethy, D.; Naidoo, V. An investigation of antimicrobial usage patterns by small animal veterinarians in South Africa. Prev. Vet. Med. 2017, 136, 29–38. [Google Scholar] [CrossRef]
- Buckland, E.L.; O’Neill, D.; Summers, J.; Mateus, A.L.P.; Church, D.; Redmond, L.; Brodbelt, D.C. Characterisation of antimicrobial usage in cats and dogs attending UK primary care companion animal veterinary practices. Vet. Rec. 2016, 179, 489. [Google Scholar] [CrossRef]
- Carmo, L.P.; Nielsen, L.R.; Alban, L.; da Costa, P.M.; Schüpbach-Regula, G.; Magouras, I. Veterinary expert opinion on potential drivers and opportunities for changing antimicrobial usage practices in livestock in Denmark, Portugal, and Switzerland. Front. Vet. Sci. 2018, 5, 29. [Google Scholar] [CrossRef] [PubMed]
- Bourély, C.; Fortané, N.; Calavas, D.; Leblond, A.; Gay, É. Why do veterinarians ask for antimicrobial susceptibility testing? A qualitative study exploring determinants and evaluating the impact of antibiotic reduction policy. Prev. Vet. Med. 2018, 159, 123–134. [Google Scholar] [CrossRef]
- De Briyne, N.; Atkinson, J.; Pokludová, L.; Borriello, S.P.; Price, S. Factors influencing antibiotic prescribing habits and use of sensitivity testing amongst veterinarians in Europe. Vet. Rec. 2013, 173, 475. [Google Scholar] [CrossRef]
- Coyne, L.A.; Latham, S.M.; Williams, N.J.; Dawson, S.; Donald, I.J.; Pearson, R.B.; Smith, R.F.; Pinchbeck, G.L. Understanding the culture of antimicrobial prescribing in agriculture: A qualitative study of UK pig veterinary surgeons. J. Antimicrob. Chemother. 2016, 71, 3300–3312. [Google Scholar] [CrossRef]
- Coyne, L.A.; Latham, S.M.; Dawson, S.; Donald, I.J.; Pearson, R.B.; Smith, R.F.; Williams, N.J.; Pinchbeck, G.L. Antimicrobial use practices, attitudes and responsibilities in UK farm animal veterinary surgeons. Prev. Vet. Med. 2018, 161, 115–126. [Google Scholar] [CrossRef] [PubMed]
- Eriksen, E.O.; Smed, S.; Klit, K.J.; Olsen, J.E. Factors influencing Danish veterinarians’ choice of antimicrobials prescribed for intestinal diseases in weaner pigs. Vet. Rec. 2019, 184, 798. [Google Scholar] [CrossRef]
- Higgins, H.M.; Golding, S.E.; Mouncey, J.; Nanjiani, I.; Cook, A.J.C. Understanding veterinarians’ prescribing decisions on antibiotic dry cow therapy. J. Dairy Sci. 2017, 100, 2909–2916. [Google Scholar] [CrossRef]
- Espetvedt, M.N.; Rintakoski, S.; Wolff, C.; Lind, A.-K.; Lindberg, A.; Virtala, A.-M.K. Nordic veterinarians’ threshold for medical treatment of dairy cows, influence on disease recording and medicine use: Mild clinical mastitis as an example. Prev. Vet. Med. 2013, 112, 76–89. [Google Scholar] [CrossRef]
- Scherpenzeel, C.G.M.; Santman-Berends, I.M.G.A.; Lam, T.J.G.M. Veterinarians’ attitudes toward antimicrobial use and selective dry cow treatment in the Netherlands. J. Dairy Sci. 2018, 101, 6336–6345. [Google Scholar] [CrossRef] [PubMed]
- Redding, L.E.; Brooks, C.; Georgakakos, C.B.; Habing, G.; Rosenkrantz, L.; Dahlstrom, M.; Plummer, P.J. Addressing individual values to impact prudent antimicrobial prescribing in animal agriculture. Front. Vet. Sci. 2020, 7, 297. [Google Scholar] [CrossRef] [PubMed]
- Flowers, P. Antimicrobial resistance: A biopsychosocial problem requiring innovative interdisciplinary and imaginative interventions. J. Infect. Prev. 2018, 19, 195–199. [Google Scholar] [CrossRef] [PubMed]
- Aguinis, H.; Bradley, K.J. Best practice recommendations for designing and implementing experimental vignette methodology studies. Organ. Res. Methods 2014, 17, 351–371. [Google Scholar] [CrossRef]
- Evans, S.C.; Roberts, M.C.; Keeley, J.W.; Blossom, J.B.; Amaro, C.M.; Garcia, A.M.; Stough, C.O.; Canter, K.S.; Robles, R.; Reed, G.M. Vignette methodologies for studying clinicians’ decision-making: Validity, utility, and application in ICD-11 field studies. Int. J. Clin. Health Psychol. 2015, 15, 160–170. [Google Scholar] [CrossRef]
- Arnold, S.R.; To, T.; McIsaac, W.J.; Wang, E.E.L. Antibiotic prescribing for upper respiratory tract infection: The importance of diagnostic uncertainty. J. Pediatr. 2005, 146, 222–226. [Google Scholar] [CrossRef]
- Llor, C.; Vilaseca, I.; Lehrer-Coriat, E.; Boleda, X.; Cañada, J.L.; Moragas, A.; Cots, J.M. Survey of Spanish general practitioners’ attitudes toward management of sore throat: An internet-based questionnaire study. BMC Fam. Pract. 2017, 18, 21. [Google Scholar] [CrossRef] [PubMed]
- Livorsi, D.; Comer, A.R.; Matthias, M.S.; Perencevich, E.N.; Bair, M.J. Barriers to guideline-concordant antibiotic use among inpatient physicians: A case vignette qualitative study. J. Hosp. Med. 2016, 11, 174–180. [Google Scholar] [CrossRef]
- Golding, S.E.; Ogden, J.; Higgins, H.M. Shared goals, different barriers: A qualitative study of UK veterinarians’ and farmers’ beliefs about antimicrobial resistance and stewardship. Front. Vet. Sci. 2019, 6, 132. [Google Scholar] [CrossRef] [PubMed]
- Redding, L.E.; Barg, F.K.; Smith, G.; Galligan, D.T.; Levy, M.Z.; Hennessy, S. The role of veterinarians and feed-store vendors in the prescription and use of antibiotics on small dairy farms in rural Peru. J. Dairy Sci. 2013, 96, 7349–7354. [Google Scholar] [CrossRef]
- Speksnijder, D.C.; Jaarsma, A.C.D.; van der Gugten, A.C.; Verheij, T.J.M.; Wagenaar, J.A. Determinants associated with veterinary antimicrobial prescribing in farm animals in the Netherlands: A qualitative study. Zoonoses Public Health 2015, 62, 39–51. [Google Scholar] [CrossRef] [PubMed]
- Mateus, A.L.P.; Brodbelt, D.C.; Barber, N.; Stärk, K.D.C. Qualitative study of factors associated with antimicrobial usage in seven small animal veterinary practices in the UK. Prev. Vet. Med. 2014, 117, 68–78. [Google Scholar] [CrossRef] [PubMed]
- van Cleven, A.; Sarrazin, S.; de Rooster, H.; Paepe, D.; van der Meeren, S.; Dewulf, J. Antimicrobial prescribing behaviour in dogs and cats by Belgian veterinarians. Vet. Rec. 2018, 182, 324. [Google Scholar] [CrossRef]
- Schneider, S.; Salm, F.; Vincze, S.; Moeser, A.; Petruschke, I.; Schmücker, K.; Ludwig, N.; Hanke, R.; Schröder, C.; Gropmann, A.; et al. Perceptions and attitudes regarding antibiotic resistance in Germany: A cross-sectoral survey amongst physicians, veterinarians, farmers and the general public. J. Antimicrob. Chemother. 2018, 73, 1984–1988. [Google Scholar] [CrossRef] [PubMed]
- Hardin, G. The tragedy of the commons. Science 1968, 162, 1243–1248. [Google Scholar] [CrossRef]
- Tonkin-Crine, S.; Walker, A.S.; Butler, C.C. Contribution of behavioural science to antibiotic stewardship. BMJ 2015, 350, h3413. [Google Scholar] [CrossRef] [PubMed]
- American Psychological Association. Psychology and Global Climate Change. A Report by the American Psychological Association Task Force on the Interface between Psychology and Global Climate Change; American Psychological Association: Washington, DC, USA, 2009. [Google Scholar]
- McCullough, A.R.; Rathbone, J.; Parekh, S.; Hoffmann, T.C.; Del Mar, C.B. Not in my backyard: A systematic review of clinicians’ knowledge and beliefs about antibiotic resistance. J. Antimicrob. Chemother. 2015, 70, 2465–2473. [Google Scholar] [CrossRef]
- Broom, A.; Kenny, K.; Prainsack, B.; Broom, J. Antimicrobial resistance as a problem of values? Views from three continents. Crit. Public Health 2020. [Google Scholar] [CrossRef]
- Steg, L.; Vlek, C.A.J. Encouraging pro-environmental behaviour: An integrative review and research agenda. J. Environ. Psychol. 2009, 29, 309–317. [Google Scholar] [CrossRef]
- Wallinga, D.; Rayner, G.; Lang, T. Antimicrobial resistance and biological governance: Explanations for policy failure. Public Health 2015, 129, 1314–1325. [Google Scholar] [CrossRef] [PubMed]
- Laxminarayan, R.; Duse, A.; Wattal, C.; Zaidi, A.K.M.; Wertheim, H.F.L.; Sumpradit, N.; Vlieghe, E.; Levy Hara, G.; Gould, I.M.; Goossens, H.; et al. Antibiotic resistance: The need for global solutions. Lancet Infect. Dis. 2013, 13, 1057–1098. [Google Scholar] [CrossRef]
- Lübbert, C.; Baars, C.; Dayakar, A.; Lippmann, N.; Rodloff, A.C.; Kinzig, M.; Sörgel, F. Environmental pollution with antimicrobial agents from bulk drug manufacturing industries in Hyderabad, South India, is associated with dissemination of extended-spectrum beta-lactamase and carbapenemase-producing pathogens. Infection 2017, 45, 479–491. [Google Scholar] [CrossRef] [PubMed]
- Steg, L.; de Groot, J.I.M. Environmental values. In The Oxford Handbook of Environmental and Conservation Psychology; Clayton, S.D., Ed.; Oxford University Press: Oxford, UK, 2012; pp. 1–21. [Google Scholar]
- Steg, L.; Perlaviciute, G.; van der Werff, E.; Lurvink, J. The significance of hedonic values for environmentally relevant attitudes, preferences, and actions. Environ. Behav. 2014, 46, 163–192. [Google Scholar] [CrossRef]
- de Groot, J.I.M.; Steg, L. Value orientations to explain beliefs related to environmental significant behavior: How to measure egoistic, altruistic and biospheric value orientations. Environ. Behav. 2008, 40, 330–354. [Google Scholar] [CrossRef]
- de Groot, J.I.M.; Steg, L. Value orientations and environmental beliefs in five countries: Validity of an instrument to measure egoistic, altruistic and biospheric value orientations. J. Cross. Cult. Psychol. 2007, 38, 318–332. [Google Scholar] [CrossRef]
- Gatersleben, B.; Murtagh, N.; Abrahamse, W. Values, identity and pro-environmental behaviour. Contemp. Soc. Sci. 2014, 9, 374–392. [Google Scholar] [CrossRef]
- Thøgersen, J.; Ölander, F. Human values and the emergence of a sustainable consumption pattern: A panel study. J. Econ. Psychol. 2002, 23, 605–630. [Google Scholar] [CrossRef]
- Schwartz, S.H. Universals in the content and structure of values: Theoretical advances and empirical tests in 20 countries. Adv. Exp. Soc. Psychol. 1992, 25, 1–65. [Google Scholar] [CrossRef]
- Feather, N.T. Values, valences, and choice: The influences of values on the perceived attractiveness and choice of alternatives. J. Pers. Soc. Psychol. 1995, 68, 1135–1151. [Google Scholar] [CrossRef]
- Steg, L.; Bolderdijk, J.W.; Keizer, K.; Perlaviciute, G. An integrated framework for encouraging pro-environmental behaviour: The role of values, situational factors and goals. J. Environ. Psychol. 2014, 38, 104–115. [Google Scholar] [CrossRef]
- Speksnijder, D.C.; Jaarsma, A.C.D.; Verheij, T.J.M.; Wagenaar, J.A. Attitudes and perceptions of Dutch veterinarians on their role in the reduction of antimicrobial use in farm animals. Prev. Vet. Med. 2015, 121, 365–373. [Google Scholar] [CrossRef]
- Currie, K.; King, C.; Nuttall, T.; Smith, M.; Flowers, P. Expert consensus regarding drivers of antimicrobial stewardship in companion animal veterinary practice: A Delphi study. Vet. Rec. 2018, 182, 691. [Google Scholar] [CrossRef]
- Postma, M.; Vanderhaeghen, W.; Sarrazin, S.; Maes, D.; Dewulf, J. Reducing antimicrobial usage in pig production without jeopardizing production parameters. Zoonoses Public Health 2017, 64, 63–74. [Google Scholar] [CrossRef] [PubMed]
- Turner, A.E.; Tisdall, D.A.; Barrett, D.C.; Wood, S.; Dowsey, A.; Reyher, K.K. Ceasing the use of the highest priority critically important antimicrobials does not adversely affect production, health or welfare parameters in dairy cows. Vet. Rec. 2018, 183, 67. [Google Scholar] [CrossRef] [PubMed]
- van Dijk, L.; Hayton, A.; Main, D.C.J.; Booth, A.; King, A.; Barrett, D.C.; Buller, H.J.; Reyher, K.K. Participatory policy making by dairy producers to reduce antimicrobial use on farms. Zoonoses Public Health 2017, 64, 476–484. [Google Scholar] [CrossRef]
- Speksnijder, D.C.; Graveland, H.; Eijck, I.A.J.M.; Schepers, R.W.M.; Heederik, D.J.J.; Verheij, T.J.M.; Wagenaar, J.A. Effect of structural animal health planning on antimicrobial use and animal health variables in conventional dairy farming in the Netherlands. J. Dairy Sci. 2017, 100, 4903–4913. [Google Scholar] [CrossRef]
- Doidge, C.; Ruston, A.; Lovatt, F.; Hudson, C.; King, L.; Kaler, J. Farmers’ perceptions of preventing antibiotic resistance on sheep and beef farms: Risk, responsibility, and action. Front. Vet. Sci. 2020, 7, 524. [Google Scholar] [CrossRef]
- Zhuo, A.; Labbate, M.; Norris, J.M.; Gilbert, G.L.; Ward, M.P.; Bajorek, B.V.; Degeling, C.; Rowbotham, S.J.; Dawson, A.; Nguyen, K.-A.; et al. Opportunities and challenges to improving antibiotic prescribing practices through a One Health approach: Results of a comparative survey of doctors, dentists and veterinarians in Australia. BMJ Open 2018, 8, e020439. [Google Scholar] [CrossRef] [PubMed]
- Norris, J.M.; Zhuo, A.; Govendir, M.; Rowbotham, S.J.; Labbate, M.; Degeling, C.; Gilbert, G.L.; Dominey-Howes, D.; Ward, M.P. Factors influencing the behaviour and perceptions of Australian veterinarians towards antibiotic use and antimicrobial resistance. PLoS ONE 2019, 14, e0223534. [Google Scholar] [CrossRef]
- Biezen, R.; Grando, D.; Mazza, D.; Brijnath, B. Dissonant views: GPs’ and parents’ perspectives on antibiotic prescribing for young children with respiratory tract infections. BMC Fam. Pract. 2019, 20, 46. [Google Scholar] [CrossRef]
- Cho, H.-J.; Soo-Jong, H.; Park, S. Knowledge and beliefs of primary care physicians, pharmacists, and parents on antibiotic use for the pediatric common cold. Soc. Sci. Med. 2004, 58, 623–629. [Google Scholar] [CrossRef]
- Keizer, J.; Braakman-Jansen, L.M.A.; Kampmeier, S.; Köck, R.; Al Naiemi, N.; Te Riet-Warning, R.; Beerlage-De Jong, N.; Becker, K.; van Gemert-Pijnen, J.E.W.C. Cross-border comparison of antimicrobial resistance (AMR) and AMR prevention measures: The healthcare workers’ perspective. Antimicrob. Resist. Infect. Control 2019, 8, 123. [Google Scholar] [CrossRef] [PubMed]
- Visschers, V.H.M.; Iten, D.M.; Riklin, A.; Hartmann, S.; Sidler, X.; Siegrist, M. Swiss pig farmers׳ perception and usage of antibiotics during the fattening period. Livest. Sci. 2014, 162, 223–232. [Google Scholar] [CrossRef]
- Visschers, V.H.M.; Backhans, A.; Collineau, L.; Iten, D.M.; Loesken, S.; Postma, M.; Belloc, C.; Dewulf, J.; Emanuelson, U.; Grosse Beilage, E.; et al. Perceptions of antimicrobial usage, antimicrobial resistance and policy measures to reduce antimicrobial usage in convenient samples of Belgian, French, German, Swedish and Swiss pig farmers. Prev. Vet. Med. 2015, 119, 10–20. [Google Scholar] [CrossRef]
- Fynbo, L.; Jensen, C.S. Antimicrobial stigmatization: Public health concerns about conventional pig farming and pig farmers’ experiences with stigmatization. Soc. Sci. Med. 2018, 201, 1–8. [Google Scholar] [CrossRef]
- Johnson, I.; Hansen, A.; Bi, P. The challenges of implementing an integrated One Health surveillance system in Australia. Zoonoses Public Health 2018, 65, e229–e236. [Google Scholar] [CrossRef]
- Kesten, J.M.; Bhattacharya, A.; Ashiru-Oredope, D.; Gobin, M.; Audrey, S. The Antibiotic Guardian campaign: A qualitative evaluation of an online pledge-based system focused on making better use of antibiotics. BMC Public Health 2018, 17, 5. [Google Scholar] [CrossRef]
- Powell, N.; Davidson, I.; Yelling, P.; Collinson, A.; Pollard, A.; Johnson, L.; Gibson, N.; Taylor, J.; Wisner, K.; Gaze, W.H.; et al. Developing a local antimicrobial resistance action plan: The Cornwall One Health Antimicrobial Resistance Group. J. Antimicrob. Chemother. 2017, 72, 2661–2665. [Google Scholar] [CrossRef]
- Mölstad, S.; Erntell, M.; Hanberger, H.; Melander, E.; Norman, C.; Skoog, G.; Stålsby Lundborg, C.; Söderström, A.; Torell, E.; Cars, O. Sustained reduction of antibiotic use and low bacterial resistance: 10-year follow-up of the Swedish Strama programme. Lancet Infect. Dis. 2008, 8, 125–132. [Google Scholar] [CrossRef]
- Coelho, F.; Pereira, M.C.; Cruz, L.; Simões, P.; Barata, E. Affect and the adoption of pro-environmental behaviour: A structural model. J. Environ. Psychol. 2017, 54, 127–138. [Google Scholar] [CrossRef]
- Dono, J.; Webb, J.; Richardson, B. The relationship between environmental activism, pro-environmental behaviour, and social identity. J. Environ. Psychol. 2010, 30, 178–186. [Google Scholar] [CrossRef]
- Robinson, D.; Edwards, M.; Mason, B.; Cockett, J.; Graham, K.A.; Martin, A. The 2019 Survey of the Veterinary Profession. A report for the Royal College of Veterinary Surgeons; Institute for Employment Studies: Brighton, UK, 2019. [Google Scholar]
- Wasserstein, R.L.; Lazar, N.A. The ASA’s Statement on p-values: Context, process, and purpose. Am. Stat. 2016, 70, 129–133. [Google Scholar] [CrossRef]
- Wasserstein, R.L.; Schirm, A.L.; Lazar, N.A. Moving to a world beyond “p < 0.05.”. Am. Stat. 2019, 73, 1–19. [Google Scholar] [CrossRef]
- Hoenig, J.M.; Heisey, D.M. The abuse of power: The pervasive fallacy of power calculations for data analysis. Am. Stat. 2001, 55, 19–24. [Google Scholar] [CrossRef]
- Lenth, R.V. Some practical guidelines for effective sample size determination. Am. Stat. 2001, 55, 187–193. [Google Scholar] [CrossRef]
- Perneger, T.V. What’s wrong with Bonferroni adjustments. BMJ 1998, 316, 1236–1238. [Google Scholar] [CrossRef]
- Rothman, K.J. No adjustments are needed for multiple comparisons. Epidemiology 1990, 1, 43–46. [Google Scholar] [CrossRef] [PubMed]
- Peabody, J.W.; Luck, J.; Glassman, P.; Dresselhaus, T.R.; Lee, M. Comparison of vignettes, standardized patients, and chart abstraction: A prospective validation study of 3 methods for measuring quality. JAMA 2000, 283, 1715. [Google Scholar] [CrossRef]
- Veloski, J.; Tai, S.; Evans, A.S.; Nash, D.B. Clinical vignette-based surveys: A tool for assessing physician practice variation. Am. J. Med. Qual. 2005, 20, 151–157. [Google Scholar] [CrossRef] [PubMed]
- Golding, S.E.; Ogden, J.; Higgins, H.M. ‘Ideal’ versus ‘real-world’: Application of vignettes to investigate antibiotic prescribing decisions by farm vets. Cattle Pract. in press.
- Faul, F.; Erdfelder, E.; Lang, A.G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav. Res. Methods 2007, 39, 175–191. [Google Scholar] [CrossRef] [PubMed]
- van Voorhis, C.R.W.; Morgan, B.L. Understanding power and rules of thumb for determining sample sizes. Tutor. Quant. Methods Psychol. 2007, 3, 43–50. [Google Scholar] [CrossRef]
- Streiner, D.L. Starting at the beginning: An introduction to coefficient alpha and internal consistency. J. Pers. Assess. 2003, 80, 99–103. [Google Scholar] [CrossRef] [PubMed]
- Greenland, S. Valid P-values behave exactly as they should: Some misleading criticisms of P-values and their resolution with S-values. Am. Stat. 2019, 73, 106–114. [Google Scholar] [CrossRef]
- Rafi, Z.; Greenland, S. Semantic and cognitive tools to aid statistical inference: Replace confidence and significance by compatibility and surprise. BMC Med. Res. Methodol. 2020, 20, 244. [Google Scholar] [CrossRef]
- Cole, S.R.; Edwards, J.K.; Greenland, S. Surprise! Am. J. Epidemiol. 2021, 190, 191–193. [Google Scholar] [CrossRef] [PubMed]
- Schulz, K.F.; Altman, D.G.; Moher, D. CONSORT 2010 Statement: Updated guidelines for reporting parallel group randomised trials. BMC Med. 2010, 8, 18. [Google Scholar] [CrossRef] [PubMed]
- von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. Strengthening the reporting of observational studies in epidemiology (STROBE) statement: Guidelines for reporting observational studies. BMJ 2007, 335, 806–808. [Google Scholar] [CrossRef] [PubMed]
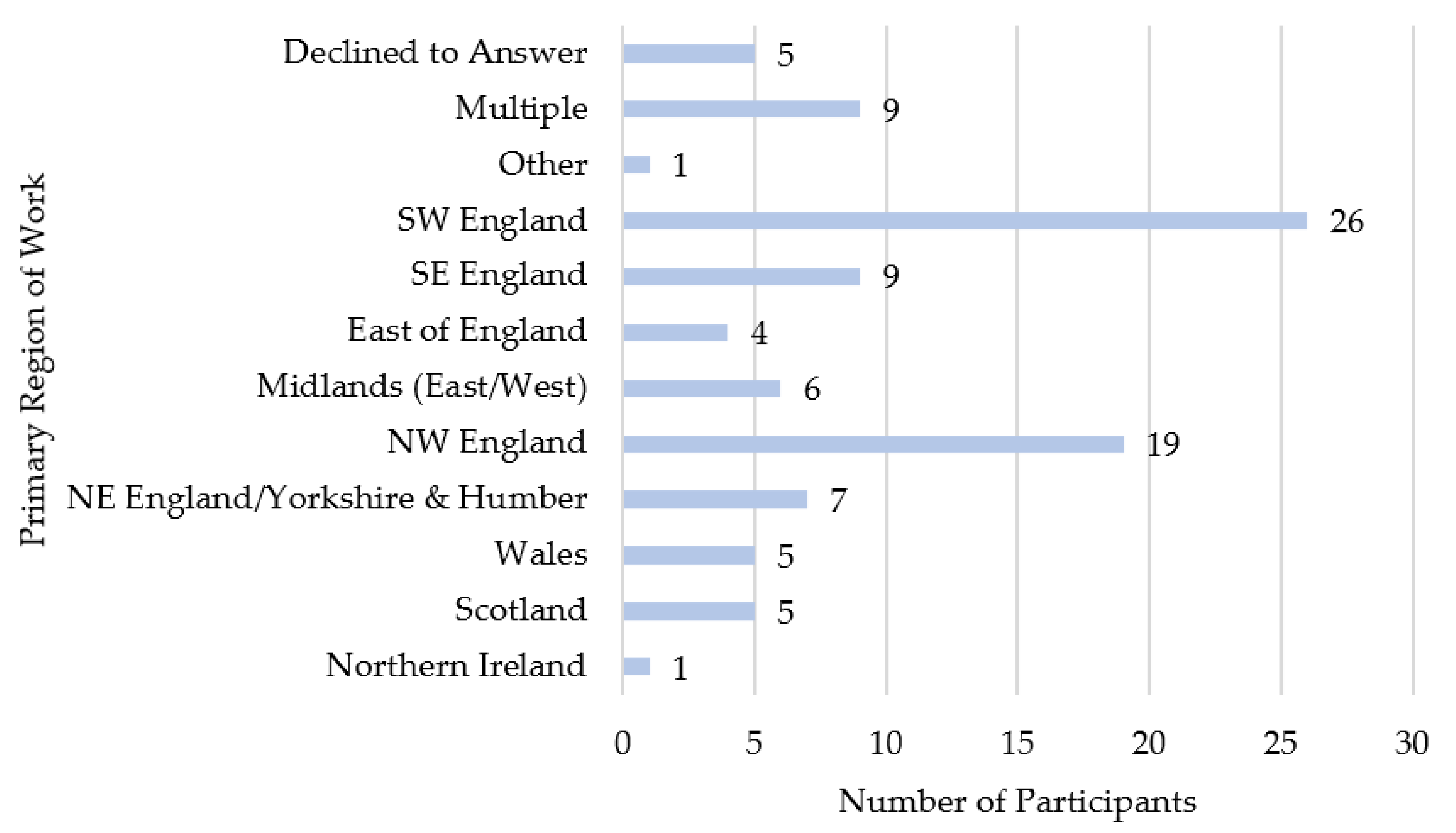



| Characteristic | Response Option | Individuals in Sample (n = 97) | Percentage of Sample |
|---|---|---|---|
| Gender 1 | Female | 46 | 46.39 |
| Male | 45 | 47.42 | |
| Other | 0 | 0.00 | |
| Prefer Not to Say | 1 | 1.03 | |
| Declined to Answer | 5 | 5.15 | |
| Ethnicity 1 | White | 91 | 93.81 |
| Black | 0 | 0.00 | |
| Asian | 0 | 0.00 | |
| Mixed | 0 | 0.00 | |
| Other | 0 | 0.00 | |
| Prefer Not to Say | 1 | 1.03 | |
| Declined to Answer | 5 | 5.15 | |
| Holds Postgraduate Veterinary Qualifications | Yes | 26 | 26.80 |
| No | 65 | 67.01 | |
| Declined to Answer | 6 | 6.19 |
| Condition | Mean | Lower BCa 95% CI 1 | Upper BCa 95% CI 1 | Standard Deviation |
|---|---|---|---|---|
| Control | 3.27 | 2.73 | 3.85 | 1.39 |
| Economics | 3.35 | 2.88 | 3.76 | 1.23 |
| Farmer | 3.75 | 3.18 | 4.29 | 1.36 |
| Relationship | 3.96 | 3.56 | 4.36 | 1.06 |
| Beliefs | Subscale | Mean 1 | Lower BCa 95% CI 2 | Upper BCa 95% CI 2 | Standard Deviation | p | S |
|---|---|---|---|---|---|---|---|
| Responsibility for Causing AMR (n = 89) | Human Medics | 3.77 | 3.63 | 3.92 | 0.68 | <0.001 | 9.97 |
| Public/Patients | 3.72 | 3.56 | 3.88 | 0.75 | <0.001 | 9.97 | |
| Farmers | 3.62 | 3.46 | 3.77 | 0.72 | <0.001 | 9.97 | |
| Farm Animal Vets 3 | 3.19 | 3.05 | 3.34 | 0.70 | - | - | |
| Pet Owners | 3.18 | 3.01 | 3.35 | 0.82 | 0.95 | 0.07 | |
| Companion Animal Vets | 3.05 | 2.90 | 3.21 | 0.73 | 1.00 | 0.00 | |
| Responsibility for Preventing AMR (n = 88) | Human Medics | 4.28 | 4.14 | 4.41 | 0.62 | 0.031 | 1.69 |
| Farmers | 4.21 | 4.07 | 4.35 | 0.65 | 0.072 | 3.80 | |
| Public/Patients | 4.08 | 3.94 | 4.22 | 0.64 | 1.00 | 0.00 | |
| Farm Animal Vets 3 | 4.06 | 3.94 | 4.19 | 0.60 | - | - | |
| Pet Owners | 3.93 | 3.78 | 4.09 | 0.72 | 1.00 | 0.00 | |
| Companion Animal Vets | 3.63 | 3.48 | 3.79 | 0.74 | <0.001 | 9.97 |
| Variable | B [BCa 95% CI] 2 | SE B | Β | t | p | |
|---|---|---|---|---|---|---|
| Block 1 | Constant | 3.21 [2.51, 3.83] | 0.30 | 10.87 | <0.001 | |
| Control v. Economics | 0.05 [−0.75, 0.86] | 0.40 | 0.02 | 0.13 | 0.90 | |
| Control v. Farmer | 0.52 [−0.45, 1.53] | 0.40 | 0.17 | 1.28 | 0.20 | |
| Control v. Relationship | 0.75 [−0.01, 1.57] | 0.39 | 0.26 | 1.91 | 0.059 | |
| Block 2 1 | Constant | 5.11 [3.03, 7.15] | 0.96 | 5.34 | <0.001 | |
| Control v. Economics | −0.006 [−0.77, 0.80] | 0.40 | −0.002 | 0.02 | 0.99 | |
| Control v. Farmer | 0.32 [−0.64, 1.27] | 0.40 | 0.11 | 0.79 | 0.43 | |
| Control v. Relationship | 0.79 [−0.24, 1.55] | 0.39 | 0.27 | 2.01 | 0.048 | |
| Medics Causing AMR | −0.06 [−0.50, 0.44] | 0.23 | −0.0 | 0.24 | 0.81 | |
| Public/Patients Causing AMR | −0.56 [−0.95, −0.13] | 0.24 | −0.32 | 2.33 | 0.022 | |
| Comp. Animal Vets Causing AMR | −0.32 [−0.87, 0.37] | 0.27 | −0.18 | 1.18 | 0.24 | |
| Pet Owners Causing AMR | 0.22 [−0.23, 0.70] | 0.24 | 0.14 | 0.92 | 0.36 | |
| Farm Vets Causing AMR | 0.43 [−0.27, 0.94] | 0.35 | 0.23 | 1.24 | 0.22 | |
| Farmers Causing AMR | −0.18 [−0.81, 0.60] | 0.33 | −0.10 | 0.53 | 0.60 |
| Variable | B [BCa 95% CI] 2 | SE B | Β | t | p | |
|---|---|---|---|---|---|---|
| Block 1 | Constant | 3.20 [2.54, 3.81] | 0.29 | 11.16 | <0.001 | |
| Control v. Economics | 0.12 [−0.71, 1.01] | 0.40 | 0.04 | 0.30 | 0.77 | |
| Control v. Farmer | 0.53 [−0.28, 1.37] | 0.40 | 0.18 | 1.33 | 0.19 | |
| Control v. Relationship | 0.71 [−0.006, 1.53] | 0.39 | 0.25 | 1.85 | 0.068 | |
| Block 2 1 | Constant | 6.15 [4.35, 7.90] | 1.08 | 5.70 | <0.001 | |
| Control v. Economics | 0.34 [−0.55, 1.33] | 0.41 | 0.12 | 0.84 | 0.41 | |
| Control v. Farmer | 0.53 [−0.26, 1.33] | 0.39 | 0.18 | 1.36 | 0.18 | |
| Control v. Relationship | 0.86 [0.05, 1.78] | 0.38 | 0.30 | 2.24 | 0.028 | |
| Medics Preventing AMR | 0.14 [−0.52, 0.86] | 0.35 | 0.07 | 0.40 | 0.69 | |
| Public/Patients Preventing AMR | −0.69 [−1.47, 0.15] | 0.37 | −0.34 | 1.87 | 0.065 | |
| Comp. Animal Vets Preventing AMR | −0.40 [−1.00, 0.15] | 0.27 | −0.23 | 1.51 | 0.14 | |
| Pet Owners Preventing AMR | 0.15 [−0.54, 0.87] | 0.33 | 0.08 | 0.43 | 0.67 | |
| Farm Vets Preventing AMR | 0.10 [−0.81, 0.98] | 0.41 | 0.05 | 0.26 | 0.80 | |
| Farmers Preventing AMR | −0.09 [−0.87, 0.51] | 0.34 | −0.04 | 0.25 | 0.81 |
| Values | Mean | Lower BCa 95% CI 1 | Upper BCa 95% CI 1 | Standard Deviation |
|---|---|---|---|---|
| Hedonic | 6.38 | 6.10 | 6.65 | 1.34 |
| Egoistic | 4.61 | 4.37 | 4.85 | 1.17 |
| Altruistic | 6.76 | 6.48 | 7.04 | 1.35 |
| Biospheric | 6.33 | 6.05 | 6.62 | 1.38 |
| Variable | B [BCa 95% CI] 2 | SE B | Β | t | p | |
|---|---|---|---|---|---|---|
| Block 1 | Constant | 3.20 [2.59, 3.79] | 0.29 | 11.23 | <0.001 | |
| Control v. Economics | 0.09 [−0.71, 1.01] | 0.39 | 0.03 | 0.24 | 0.81 | |
| Control v. Farmer | 0.58 [−0.20, 1.43] | 0.39 | 0.20 | 1.50 | 0.14 | |
| Control v. Relationship | 0.76 [−0.02, 1.56] | 0.38 | 0.26 | 1.99 | 0.050 | |
| Block 2 1 | Constant | 2.97 [0.33, 5.54] | 1.20 | 2.48 | 0.015 | |
| Control v. Economics | 0.08 [−0.80, 1.12] | 0.41 | 0.03 | 0.19 | 0.85 | |
| Control v. Farmer | 0.56 [−0.32, 1.44] | 0.40 | 0.19 | 1.39 | 0.17 | |
| Control v. Relationship | 0.75 [−0.05, 1.60] | 0.40 | 0.26 | 1.87 | 0.065 | |
| Hedonic | −0.03 [−0.25, 0.19] | 0.16 | −0.03 | 0.23 | 0.82 | |
| Egoistic | −0.01 [−0.33, 0.31] | 0.14 | −0.01 | 0.08 | 0.94 | |
| Altruistic | 0.02 [−0.26, 0.28] | 0.12 | 0.02 | 0.18 | 0.86 | |
| Biospheric | 0.05 [−0.23, 0.31] | 0.12 | 0.05 | 0.43 | 0.67 |
| Measure | Subscale | Cronbach’s α |
|---|---|---|
| Values | Hedonic | 0.79 |
| Egoistic | 0.66 | |
| Altruistic | 0.75 | |
| Biospheric | 0.88 | |
| Responsibility for causing AMR | Human medics | 0.70 |
| Public/patients | 0.56 1 | |
| Companion animal vets | 0.83 | |
| Pet owners | 0.68 1 | |
| Farm animal vets | 0.73 | |
| Farmers | 0.78 | |
| Responsibility for preventing AMR | Human medics | 0.65 1 |
| Public/patients | 0.57 1 | |
| Companion animal vets | 0.82 | |
| Pet owners | 0.74 1 | |
| Farm animal vets | 0.73 | |
| Farmers | 0.81 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Golding, S.E.; Ogden, J.; Higgins, H.M. Examining the Effect of Context, Beliefs, and Values on UK Farm Veterinarians’ Antimicrobial Prescribing: A Randomized Experimental Vignette and Cross-Sectional Survey. Antibiotics 2021, 10, 445. https://doi.org/10.3390/antibiotics10040445
Golding SE, Ogden J, Higgins HM. Examining the Effect of Context, Beliefs, and Values on UK Farm Veterinarians’ Antimicrobial Prescribing: A Randomized Experimental Vignette and Cross-Sectional Survey. Antibiotics. 2021; 10(4):445. https://doi.org/10.3390/antibiotics10040445
Chicago/Turabian StyleGolding, Sarah E., Jane Ogden, and Helen M. Higgins. 2021. "Examining the Effect of Context, Beliefs, and Values on UK Farm Veterinarians’ Antimicrobial Prescribing: A Randomized Experimental Vignette and Cross-Sectional Survey" Antibiotics 10, no. 4: 445. https://doi.org/10.3390/antibiotics10040445
APA StyleGolding, S. E., Ogden, J., & Higgins, H. M. (2021). Examining the Effect of Context, Beliefs, and Values on UK Farm Veterinarians’ Antimicrobial Prescribing: A Randomized Experimental Vignette and Cross-Sectional Survey. Antibiotics, 10(4), 445. https://doi.org/10.3390/antibiotics10040445






