Population Pharmacokinetics and Dosing Simulation of Vancomycin Administered by Continuous Injection in Critically Ill Patient
Abstract
:1. Introduction
2. Results
2.1. Patient Characteristics
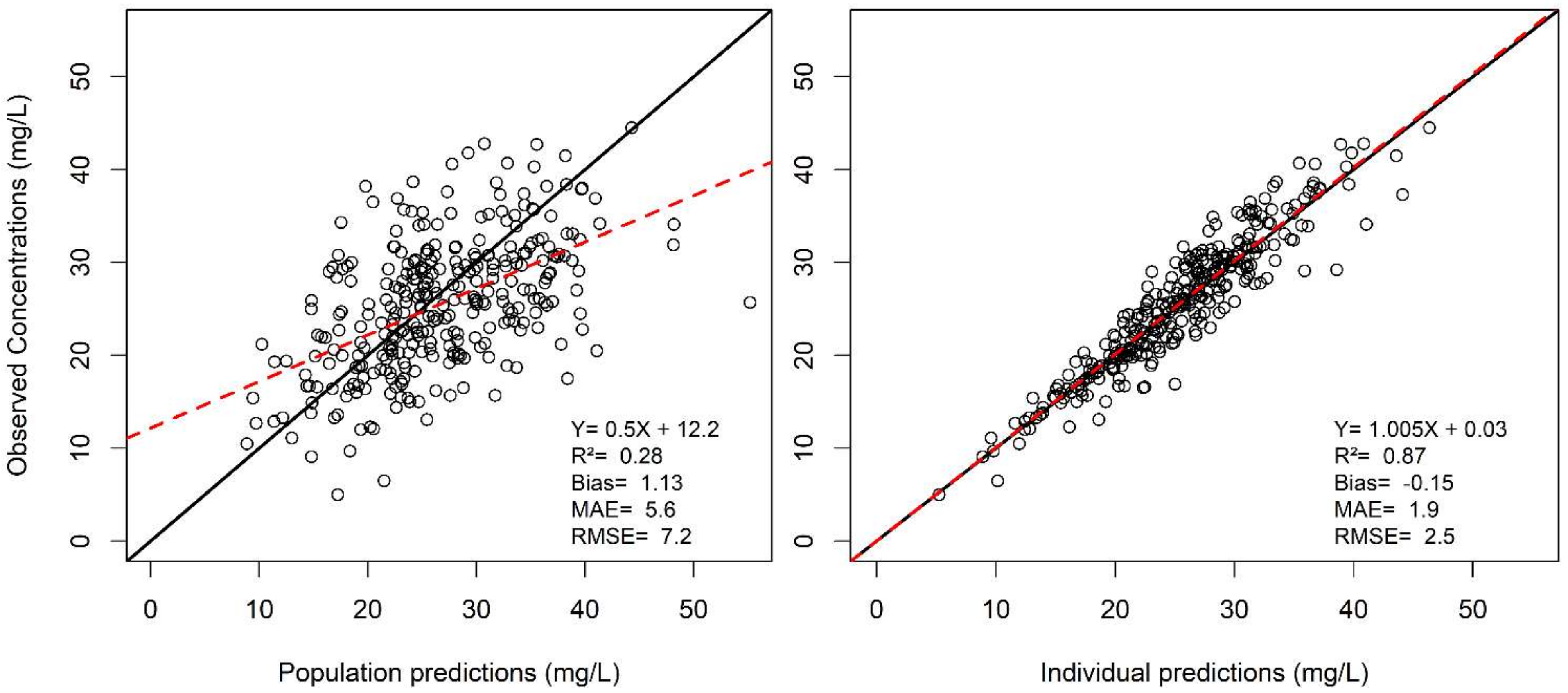
2.2. Population PK Modeling
2.3. Dosing Simulations
3. Discussion
4. Materials and Methods
4.1. Data Collection
4.2. Pharmacokinetic Modeling
4.3. Dosing Simulations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hanberger, H.; Walther, S.; Leone, M.; Barie, P.S.; Rello, J.; Lipman, J.; Marshall, J.C.; Anzueto, A.; Sakr, Y.; Pickkers, P.; et al. Increased Mortality Associated with Methicillin-Resistant Staphylococcus Aureus (MRSA) Infection in the Intensive Care Unit: Results from the EPIC II Study. Int. J. Antimicrob. Agents 2011, 38, 331–335. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cataldo, M.A.; Tacconelli, E.; Grilli, E.; Pea, F.; Petrosillo, N. Continuous versus Intermittent Infusion of Vancomycin for the Treatment of Gram-Positive Infections: Systematic Review and Meta-Analysis. J. Antimicrob. Chemother. 2012, 67, 17–24. [Google Scholar] [CrossRef] [PubMed]
- Critical Care Medicine. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Available online: https://journals.lww.com/ccmjournal/Fulltext/2017/03000/Surviving_Sepsis_Campaign___International.15.aspx (accessed on 21 June 2021).
- Blot, S.; Koulenti, D.; Akova, M.; Bassetti, M.; De Waele, J.J.; Dimopoulos, G.; Kaukonen, K.-M.; Martin, C.; Montravers, P.; Rello, J.; et al. Does Contemporary Vancomycin Dosing Achieve Therapeutic Targets in a Heterogeneous Clinical Cohort of Critically Ill Patients? Data from the Multinational DALI Study. Crit. Care 2014, 18, R99. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pea, F.; Viale, P.; Pavan, F.; Furlanut, M. Pharmacokinetic Considerations for Antimicrobial Therapy in Patients Receiving Renal Replacement Therapy. Clin. Pharmacokinet. 2007, 46, 997–1038. [Google Scholar] [CrossRef]
- Baptista, J.P.; Sousa, E.; Martins, P.J.; Pimentel, J.M. Augmented Renal Clearance in Septic Patients and Implications for Vancomycin Optimisation. Int. J. Antimicrob. Agents 2012, 39, 420–423. [Google Scholar] [CrossRef] [PubMed]
- Ocampos-Martinez, E.; Penaccini, L.; Scolletta, S.; Abdelhadii, A.; Devigili, A.; Cianferoni, S.; de Backer, D.; Jacobs, F.; Cotton, F.; Vincent, J.-L.; et al. Determinants of Early Inadequate Vancomycin Concentrations during Continuous Infusion in Septic Patients. Int. J. Antimicrob. Agents 2012, 39, 332–337. [Google Scholar] [CrossRef]
- Yamada, C.H.; Telles, J.P.; Oliveira, D.D.S.; Cieslinski, J.; Ribeiro, V.S.T.; Gasparetto, J.; Tuon, F.F. Comparison of Intermittent versus Continuous-Infusion Vancomycin for Treating Severe Patients in Intensive Care Units. Braz. J. Infect. Dis. 2020, 24, 356–359. [Google Scholar] [CrossRef]
- Chu, Y.; Luo, Y.; Quan, X.; Jiang, M.; Zhou, B. Intermittent vs. Continuous Vancomycin Infusion for Gram-Positive Infections: A Systematic Review and Meta-Analysis. J. Infect. Public Health 2020, 13, 591–597. [Google Scholar] [CrossRef]
- Wysocki, M.; Delatour, F.; Faurisson, F.; Rauss, A.; Pean, Y.; Misset, B.; Thomas, F.; Timsit, J.-F.; Similowski, T.; Mentec, H.; et al. Continuous versus Intermittent Infusion of Vancomycin in Severe Staphylococcal Infections: Prospective Multicenter Randomized Study. Antimicrob. Agents Chemother. 2001, 45, 2460–2467. [Google Scholar] [CrossRef] [Green Version]
- Flannery, A.H.; Bissell, B.D.; Bastin, M.T.; Morris, P.E.; Neyra, J.A. Continuous Versus Intermittent Infusion of Vancomycin and the Risk of Acute Kidney Injury in Critically Ill Adults: A Systematic Review and Meta-Analysis*. Crit. Care Med. 2020, 48, 912–918. [Google Scholar] [CrossRef]
- Neely, M.N.; Kato, L.; Youn, G.; Kraler, L.; Bayard, D.; van Guilder, M.; Schumitzky, A.; Yamada, W.; Jones, B.; Minejima, E. Prospective Trial on the Use of Trough Concentration versus Area under the Curve To Determine Therapeutic Vancomycin Dosing. Antimicrob. Agents Chemother. 2018, 62, e02042-17. [Google Scholar] [CrossRef] [Green Version]
- Finch, N.A.; Zasowski, E.J.; Murray, K.P.; Mynatt, R.P.; Zhao, J.J.; Yost, R.; Pogue, J.M.; Rybak, M.J. A Quasi-Experiment To Study the Impact of Vancomycin Area under the Concentration-Time Curve-Guided Dosing on Vancomycin-Associated Nephrotoxicity. Antimicrob. Agents Chemother. 2017, 61, e01293-17. [Google Scholar] [CrossRef] [Green Version]
- Rybak, M.J.; Le, J.; Lodise, T.P.; Levine, D.P.; Bradley, J.S.; Liu, C.; Mueller, B.A.; Pai, M.P.; Wong-Beringer, A.; Rotschafer, J.C.; et al. Therapeutic Monitoring of Vancomycin for Serious Methicillin-Resistant Staphylococcus Aureus Infections: A Revised Consensus Guideline and Review by the American Society of Health-System Pharmacists, the Infectious Diseases Society of America, the Pediatric Infectious Diseases Society, and the Society of Infectious Diseases Pharmacists. Am. J. Health Syst. Pharm. 2020, 77, 835–864. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lodise, T.P.; Lomaestro, B.; Graves, J.; Drusano, G.L. Larger Vancomycin Doses (at Least Four Grams per Day) Are Associated with an Increased Incidence of Nephrotoxicity. Antimicrob. Agents Chemother. 2008, 52, 1330–1336. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- van Maarseveen, E.M.; Gipmans, S.; Vasbinder, E.; Petjak, M.; van Zanten, A.R.H. Switching From Intermittent to Continuous Infusion of Vancomycin in Critically Ill Patients: Toward a More Robust Exposure. Ther. Drug Monit. 2016, 38, 398–401. [Google Scholar] [CrossRef] [PubMed]
- Abdul-Aziz, M.H.; Alffenaar, J.-W.C.; Bassetti, M.; Bracht, H.; Dimopoulos, G.; Marriott, D.; Neely, M.N.; Paiva, J.-A.; Pea, F.; Sjovall, F.; et al. Antimicrobial Therapeutic Drug Monitoring in Critically Ill Adult Patients: A Position Paper#. Intensive Care Med. 2020, 46, 1127–1153. [Google Scholar] [CrossRef]
- Jeurissen, A.; Sluyts, I.; Rutsaert, R. A Higher Dose of Vancomycin in Continuous Infusion Is Needed in Critically Ill Patients. Int. J. Antimicrob. Agents 2011, 37, 75–77. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rybak, M.J. The Pharmacokinetic and Pharmacodynamic Properties of Vancomycin. Clin. Infect. Dis. 2006, 42, S35–S39. [Google Scholar] [CrossRef]
- Elyasi, S.; Khalili, H.; Dashti-Khavidaki, S.; Mohammadpour, A. Vancomycin-Induced Nephrotoxicity: Mechanism, Incidence, Risk Factors and Special Populations. A Literature Review. Eur. J. Clin. Pharmacol. 2012, 68, 1243–1255. [Google Scholar] [CrossRef]
- Bayard, D.S.; Jelliffe, R.W. A Bayesian Approach to Tracking Patients Having Changing Pharmacokinetic Parameters. J. Pharm. Pharm. 2004, 31, 75–107. [Google Scholar] [CrossRef]
- van Maarseveen, E.M.; Gipmans, S.G.H.; van Zanten, A.R.H. Exposure Variability and Target Attainment of Vancomycin: A Systematic Review Comparing Intermittent and Continuous Infusion. Ther. Drug Monit. 2020, 42, 381–391. [Google Scholar] [CrossRef] [PubMed]
- Perin, N.; Roger, C.; Marin, G.; Molinari, N.; Evrard, A.; Lavigne, J.-P.; Barbar, S.; Claret, P.G.; Boutin, C.; Muller, L.; et al. Vancomycin Serum Concentration after 48 h of Administration: A 3-Years Survey in an Intensive Care Unit. Antibiotics 2020, 9, 793. [Google Scholar] [CrossRef] [PubMed]
- Marsot, A.; Boulamery, A.; Bruguerolle, B.; Simon, N. Vancomycin: A Review of Population Pharmacokinetic Analyses. Clin. Pharmacokinet. 2012, 51, 1–13. [Google Scholar] [CrossRef] [PubMed]
- del Mar Fernández de Gatta Garcia, M.; Revilla, N.; Calvo, M.V.; Domínguez-Gil, A.; Sánchez Navarro, A. Pharmacokinetic/Pharmacodynamic Analysis of Vancomycin in ICU Patients. Intensive Care Med. 2007, 33, 279–285. [Google Scholar] [CrossRef]
- Imaura, M.; Yokoyama, H.; Kohyama, T.; Nagafuchi, H.; Kohata, Y.; Takahashi, H.; Yamada, Y. Prediction of Distribution Volume of Vancomycin in Critically Ill Patients Using Extravascular Lung Water and Pulmonary Vascular Permeability Indices. Int. J. Clin. Pharmacol. Ther. 2012, 50, 814–820. [Google Scholar] [CrossRef]
- Seay, R.E.; Brundage, R.C.; Jensen, P.D.; Schilling, C.G.; Edgren, B.E. Population Pharmacokinetics of Vancomycin in Neonates. Clin. Pharmacol. Ther. 1994, 56, 169–175. [Google Scholar] [CrossRef]
- Kubiak, D.W.; Alquwaizani, M.; Sansonetti, D.; Barra, M.E.; Calderwood, M.S. An Evaluation of Systemic Vancomycin Dosing in Obese Patients. Open Forum Infect. Dis. 2015, 2, ofv176. [Google Scholar] [CrossRef] [Green Version]
- Richardson, J.; Scheetz, M.; O’Donnell, E.P. The Association of Elevated Trough Serum Vancomycin Concentrations with Obesity. J. Infect. Chemother. 2015, 21, 507–511. [Google Scholar] [CrossRef] [Green Version]
- Roberts, D.M.; Liu, X.; Roberts, J.; Nair, P.; Cole, L.; Roberts, M.S.; Lipman, J.; Bellomo, R. A Multicenter Study on the Effect of Continuous Hemodiafiltration Intensity on Antibiotic Pharmacokinetics. Available online: https://pubmed.ncbi.nlm.nih.gov/25881576/ (accessed on 8 February 2021).
- Joy, M.S.; Matzke, G.R.; Frye, R.F.; Palevsky, P.M. Determinants of Vancomycin Clearance by Continuous Venovenous Hemofiltration and Continuous Venovenous Hemodialysis. Available online: https://pubmed.ncbi.nlm.nih.gov/9631848/ (accessed on 8 February 2021).
- Pai, M.P.; Neely, M.; Rodvold, K.A.; Lodise, T.P. Innovative Approaches to Optimizing the Delivery of Vancomycin in Individual Patients. Adv. Drug Deliv. Rev. 2014, 77, 50–57. [Google Scholar] [CrossRef] [Green Version]
- Ingram, P.R.; Lye, D.C.; Tambyah, P.A.; Goh, W.P.; Tam, V.H.; Fisher, D.A. Risk Factors for Nephrotoxicity Associated with Continuous Vancomycin Infusion in Outpatient Parenteral Antibiotic Therapy. J. Antimicrob. Chemother. 2008, 62, 168–171. [Google Scholar] [CrossRef]
- Hutschala, D.; Kinstner, C.; Skhirdladze, K.; Thalhammer, F.; Müller, M.; Tschernko, E. Influence of Vancomycin on Renal Function in Critically Ill Patients after Cardiac Surgery: Continuous versus Intermittent Infusion. Anesthesiology 2009, 111, 356–365. [Google Scholar] [CrossRef] [Green Version]
- Litton, E.; Morgan, M. The PiCCO Monitor: A Review. Anaesth. Intensive Care 2012, 40, 393–409. [Google Scholar] [CrossRef] [Green Version]
- Michaud, M.; Michaud Peyrot, C. French regulation of medical research. Rev. Med. Interne 2020, 41, 98–105. [Google Scholar] [CrossRef] [PubMed]
- Rybak, M.; Lomaestro, B.; Rotschafer, J.C.; Moellering, R., Jr.; Craig, W.; Billeter, M.; Dalovisio, J.R.; Levine, D.P. Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society of America, and the Society of Infectious Diseases Pharmacists. Am. J. Health-Syst. Pharm. 2009, 66, 82–98. [Google Scholar] [CrossRef] [PubMed]
- Singer, M.; Deutschman, C.S.; Seymour, C.W.; Shankar-Hari, M.; Annane, D.; Bauer, M.; Bellomo, R.; Bernard, G.R.; Chiche, J.-D.; Coopersmith, C.M.; et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016, 315, 801. [Google Scholar] [CrossRef] [PubMed]
- Bearden, D.T.; Rodvold, K.A. Dosage Adjustments for Antibacterials in Obese Patients. Clin. Pharmacokinet. 2000, 38, 415–426. [Google Scholar] [CrossRef]
- Devine, B.J. Gentamicin therapy. Drug Intellig. Clin. Pharm. 1974, 8, 650–655. [Google Scholar]
- Mould, D.; Upton, R. Basic Concepts in Population Modeling, Simulation, and Model-Based Drug Development—Part 2: Introduction to Pharmacokinetic Modeling Methods. CPT Pharmacomet. Syst. Pharmacol. 2013, 2, 38. [Google Scholar] [CrossRef]
- Sherwin, C.M.T.; Kiang, T.K.L.; Spigarelli, M.G.; Ensom, M.H.H. Fundamentals of Population Pharmacokinetic Modelling: Validation Methods. Clin. Pharmacokinet. 2012, 51, 573–590. [Google Scholar] [CrossRef] [PubMed]


| Demographic | Learning Dataset | Validation Dataset |
|---|---|---|
| Number of Men/Women | 57/21 | 48/36 |
| Age (years) | 68.9 ± 12.3 | 58.9 ± 15.3 |
| Weight (kg) | 77.9 ± 20.4 | 81.4 ± 18.9 |
| IBW (kg) | 63.5 ± 9 | 61.4 ± 8.8 |
| Height (cm) | 168.7 ± 8.5 | 168 ± 8.3 |
| BMI (kg/m2) | 27.6 ± 7.7 | 28 ± 7.9 |
| SOFA | 11 ± 4 | NA |
| Temperature (°C) | 37.8 ± 1.1 | NA |
| Septic shock (%) | 83.3 | NA |
| IGS-II | 55.9 ± 17.3 | NA |
| CRRT (%) | 28.2 | 4.8 |
| Blood tests | ||
| Serum creatinine (µmol·L−1) | 139.3 ± 75.7 | 149 ± 123 |
| Serum protein (g·L−1) | 60 ± 11.3 | NA |
| Serum albumin (g·L−1) | 23.1 ± 5.9 | NA |
| Lactate (mmol·L−1) | 3.8 ± 3.4 | NA |
| Procalcitonin (ng·mL−1) | 2.4 [0.8–6.8] | NA |
| CRCL (mL·min−1) | 50.4 ± 29 | 55.2 ± 37.4 |
| Dialysis parameters | ||
| CRRTEFR (mL·min−1) | 35.6 ± 18.7 | 28.7 ± 6.5 |
| PiCCO variables | ||
| EVLWI (mL·kg−1) | 9.2 ± 5.5 | NA |
| PVPI | 1.9 ± 1 | NA |
| Cardiac index (µmol·L−1) | 3.0 ± 1.5 | NA |
| Vancomycin TDM | ||
| Loading dose (mg/kg) | 22.7 ± 7.5 | 22 ± 5.8 |
| Mean maintenance dose (mg/kg) | 28.6 ± 9.4 | 25.2 ± 7.6 |
| AUC24–48 h (mg·h/L−1) | 530 ± 160 | 515 ± 341 |
| AUC24–48 h > 400 (%) | 83.3 | 70.5 |
| 400 < AUC24–48 h < 600 (%) | 59 | 25.7 |
| AUC24–48 h > 600 (%) | 24.3 | 44.8 |
| Value | RSE (%) | |
|---|---|---|
| Fixed effects | ||
| CLpop (L/h) | 0.79 | 12.7 |
| V1pop (L) | 27.3 | 45.1 |
| Qpop (L/h) | 6.08 | 41.8 |
| V2pop (L) | 61.3 | 9.7 |
| α | 1.88 | 67.1 |
| Random effects (standard deviation) | ||
| ωCL | 0.76 | 11.1 |
| ωV | 0.61 | 51.1 |
| ωQ | 0.49 | 33.8 |
| ωV2 | 0.48 | 16.5 |
| Residual error model | ||
| b | 0.13 | 6.3 |
| Xpop is the population value (fixed effect) of the corresponding parameter X (clearance or volume) and ωX its corresponding random effect. The final equations of individual parameters were as follows: | ||
| Optimal Maintenance Dose (mg/kg/24 h) a | AUC24–48 (mg·h/L) b | PTA for AUC24–48 > 400 (mg·h/L) c | 400 < AUC24–48 < 600 (mg·h/L) c | PTA for AUC24–48 > 600 (mg·h/L) c | |
|---|---|---|---|---|---|
| CRCL (mL/min) | |||||
| 150 | 30 | 493 [330–644] | 0.80 | 0.64 | 0.16 |
| 140 | 30 | 506 [335–666] | 0.83 | 0.62 | 0.21 |
| 130 | 27.5 | 483 [316–643] | 0.77 | 0.63 | 0.14 |
| 120 | 27.5 | 499 [324–668] | 0.80 | 0.61 | 0.19 |
| 110 | 25 | 475 [303–646] | 0.74 | 0.60 | 0.14 |
| 100 | 25 | 492 [313–674] | 0.77 | 0.58 | 0.19 |
| 90 | 25 | 508 [320–704] | 0.80 | 0.55 | 0.25 |
| 80 | 22.5 | 484 [298–684] | 0.75 | 0.56 | 0.19 |
| 70 | 22.5 | 503 [307–720] | 0.78 | 0.55 | 0.23 |
| 60 | 20 | 486 [287–706] | 0.74 | 0.53 | 0.21 |
| 50 | 20 | 506 [295–751] | 0.77 | 0.50 | 0.27 |
| 40 | 17.5 | 472 [273–707] | 0.69 | 0.50 | 0.19 |
| 30 | 17.5 | 498 [283–761] | 0.74 | 0.47 | 0.27 |
| 20 | 15 | 480 [265–767] | 0.69 | 0.44 | 0.25 |
| 10 | 12.5 | 470 [245–776] | 0.66 | 0.42 | 0.24 |
| CRRT Effluent Flow Rate (mL/min) | |||||
| 30 | 20 | 494 [295–723] | 0.74 | 0.5 | 0.24 |
| 20 | 17.5 | 480 [277–728] | 0.71 | 0.49 | 0.22 |
| Optimal Maintenance Dose (mg/kg/24 h) a | AUC24–48 (mg·h/L) b | PTA forAUC24–48 > 400 (mg·h/L) c | PTA for AUC24–48 > 600 (mg·h/L) c | |
|---|---|---|---|---|
| CRCL (mL/min) | ||||
| 150 | 35 | 557 [370–728] | 0.91 | 0.39 |
| 140 | 32.5 | 538 [355–708] | 0.89 | 0.32 |
| 130 | 32.5 | 552 [362–735] | 0.90 | 0.37 |
| 120 | 32.5 | 566 [368–758] | 0.91 | 0.43 |
| 110 | 30 | 547 [351–742] | 0.88 | 0.36 |
| 100 | 30 | 563 [358–771] | 0.89 | 0.42 |
| 90 | 30 | 580 [365–802] | 0.91 | 0.48 |
| 80 | 27.5 | 562 [349–788] | 0.89 | 0.42 |
| 70 | 27.5 | 582 [358–828] | 0.90 | 0.48 |
| 60 | 27.5 | 604 [365–874] | 0.91 | 0.54 |
| 50 | 25 | 588 [352–869] | 0.89 | 0.50 |
| 40 | 25 | 598 [355–899] | 0.89 | 0.52 |
| 30 | 25 | 626 [368–968] | 0.91 | 0.59 |
| 20 | 22.5 | 614 [348–976] | 0.89 | 0.56 |
| 10 | 20 | 615 [331–1013] | 0.89 | 0.55 |
| CRRT Effluent Flow Rate (mL/min) | ||||
| 30 | 27.5 | 613 [371–899] | 0.91 | 0.56 |
| 20 | 25 | 610 [359–911] | 0.90 | 0.54 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Garreau, R.; Falquet, B.; Mioux, L.; Bourguignon, L.; Ferry, T.; Tod, M.; Wallet, F.; Friggeri, A.; Richard, J.-C.; Goutelle, S. Population Pharmacokinetics and Dosing Simulation of Vancomycin Administered by Continuous Injection in Critically Ill Patient. Antibiotics 2021, 10, 1228. https://doi.org/10.3390/antibiotics10101228
Garreau R, Falquet B, Mioux L, Bourguignon L, Ferry T, Tod M, Wallet F, Friggeri A, Richard J-C, Goutelle S. Population Pharmacokinetics and Dosing Simulation of Vancomycin Administered by Continuous Injection in Critically Ill Patient. Antibiotics. 2021; 10(10):1228. https://doi.org/10.3390/antibiotics10101228
Chicago/Turabian StyleGarreau, Romain, Benoît Falquet, Lisa Mioux, Laurent Bourguignon, Tristan Ferry, Michel Tod, Florent Wallet, Arnaud Friggeri, Jean-Christophe Richard, and Sylvain Goutelle. 2021. "Population Pharmacokinetics and Dosing Simulation of Vancomycin Administered by Continuous Injection in Critically Ill Patient" Antibiotics 10, no. 10: 1228. https://doi.org/10.3390/antibiotics10101228
APA StyleGarreau, R., Falquet, B., Mioux, L., Bourguignon, L., Ferry, T., Tod, M., Wallet, F., Friggeri, A., Richard, J.-C., & Goutelle, S. (2021). Population Pharmacokinetics and Dosing Simulation of Vancomycin Administered by Continuous Injection in Critically Ill Patient. Antibiotics, 10(10), 1228. https://doi.org/10.3390/antibiotics10101228






