A Review and Classification of Assisted Living Systems
Abstract
1. Introduction
AAL Evaluation Reviews
2. Classification Framework Overview
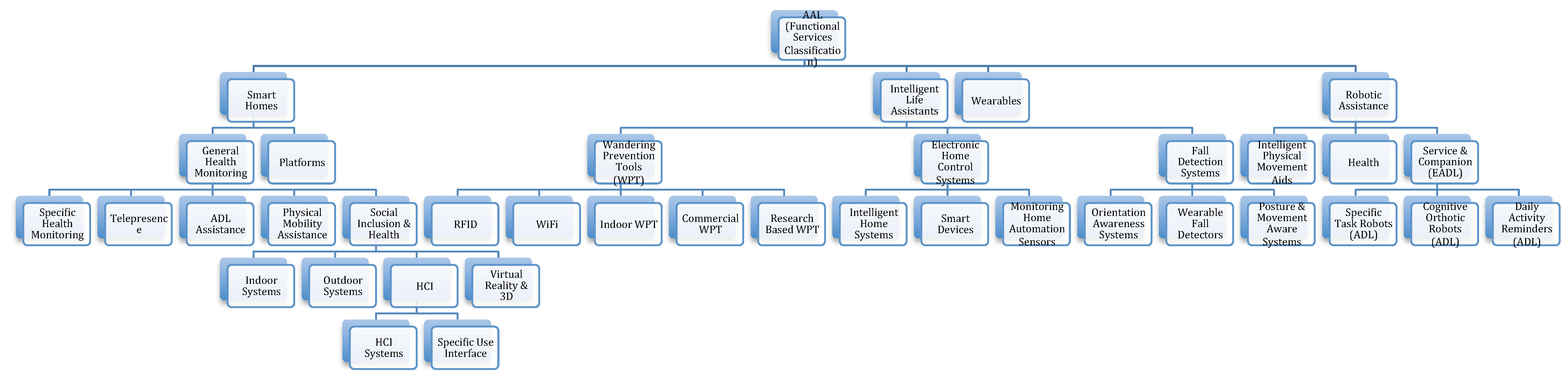
2.1. Taxonomy
2.1.1. Smart Homes
Platforms
- Home Automation
- Agent-Based AAL Systems
- Monolithic Intelligent Systems
General Health Monitoring
2.1.2. Intelligent Life Assistants
Wandering Prevention Tools
Electronic Home Control Systems
Fall Detection Systems
2.1.3. Wearables
2.1.4. Robotic Assistance
Intelligent Physical Movement Aids
Health
Service and Companion (EADL)
3. AAL System Evaluation Criteria
EvAAL: AAL Competitive Benchmarking
4. The Evolution of AAL Evaluation Criteria
5. Future Work
Author Contributions
Funding
Conflicts of Interest
References
- Rashidi, P.; Mihailidis, A. A survey on ambient-assisted living tools for older adults. IEEE J. Biomed. Health Inform. 2013, 17, 579–590. [Google Scholar] [CrossRef] [PubMed]
- Hayutin, A.M. Graying of the global population. In Public Policy and Aging Report; Hudson, R.B., Ed.; Gerontological Society of America: Washington, DC, USA, 2007; Volume 17, pp. 12–17. [Google Scholar]
- Kinsella, K.G.; Phillips, D.R. Global Aging: The Challenge of Success; Population Reference Bureau: Washington, DC, USA, 2005; Volume 60, p. 3. [Google Scholar]
- Doyle, J.; Bailey, C.; Ni Scanaill, C.; Van Der Berg, F. Lessons learned in deploying independent living technologies to older adult’s homes. In Universal Access in the Information Society; Springer: Berlin/Heidelberg, Germany, 2013. [Google Scholar]
- Sun, H.; De Florio, V.; Gui, N.; Blondia, C. Promises and Challenges of Ambient Assisted Living Systems. In Proceedings of the 2009 Sixth International Conference on Information Technology: New Generations, Las Vegas, NV, USA, 27–29 April 2009. [Google Scholar]
- Fabien, C.; Deepayan, B.; Charith, A.; Mark, S. Video based technology for ambient assisted living: A review of the literature. J. Ambient Intell. Smart Environ. 2011, 3, 253–269. [Google Scholar]
- Blackman, S.; Matlo, C.; Bobrovitskiy, C.; Waldoch, A.; Fang, M.L.; Jackson, P.; Mihailidis, A.; Nygård, L.; Astell, A.; Sixsmith, A. Ambient assisted living technologies for aging well: A scoping review. J. Intell. Syst. 2016, 25, 55–69. [Google Scholar] [CrossRef]
- Kaur, M.; Kaur, K. Review on the various services of ambient intelligent environment and internet of things. Int. J. Adv. Res. Comput. Sci. 2017, 8, 1033–1037. [Google Scholar]
- Calvaresi, D.; Cesarini, D.; Sernani, P.; Marinoni, M.; Dragoni, A.F.; Sturm, A. Exploring the ambient assisted living domain: A systematic review. J. Ambient Intell. Hum. Comput. 2017, 8, 239–257. [Google Scholar] [CrossRef]
- Memon, M.; Wagner, S.R.; Pedersen, C.F.; Beevi, F.H.A.; Hansen, F.O. Ambient Assisted Living Healthcare Frameworks, Platforms, Standards, and Quality Attributes. Sensors 2014, 14, 4312–4341. [Google Scholar] [CrossRef] [PubMed]
- Manoj, T.; Thyagaraju, G.S. Active and assisted living: A comprehensive review of enabling technologies and scenarios. Int. J. Adv. Res. Comput. Sci. 2018, 9, 461–471. [Google Scholar]
- Wolf, P.; Schmidt, A.; Otte, J.P.; Klein, M.; Rollwage, S.; König-Ries, B.; Dettborn, T.; Gabdulkhakova, A. openAAL—The open source middleware for ambient-assisted living (AAL). In Proceedings of the AALIANCE Conference, Malaga, Spain, 11–12 March 2010; pp. 1–5. [Google Scholar]
- Ambient Assisted Living Joint Programme. Available online: http://www.aaleurope.eu/aboutaal (accessed on 15 August 2017).
- Mayer, P.; Rauhala, M.; Panek, P. Field test of the eHome system. In Proceedings of the 4th German AAL-Congress, Berlin, Germany, 25–26 January 2011. [Google Scholar]
- Rodner, T.; Litz, L. Data-driven generation of rule-based behavior models for an Ambient assisted living system. In Proceedings of the IEEE Third International Conference on Consumer Electronics-Berlin (ICCE-Berlin), Berlin, Germany, 9–11 September 2013; pp. 35–38. [Google Scholar]
- O’Grady, M.J.; Muldoon, C.; Dragone, M.; Tynan, R.; O’Hare, G.M.P. Towards Evolutionary Ambient Assisted Living Systems. J. Ambient Intell. Hum. Comput. 2010, 1, 15–29. [Google Scholar] [CrossRef]
- Fagerberg, G.; Kung, A.; Wichert, R.; Tazari, M.-R.; Jean-Bart, B.; Bauer, G.; Zimmermann, G.; Furfari, F.; Potorti, F.; Chessa, S.; et al. Platforms for AAL Applications. In Lecture Notes in Computer Science, Proceedings of the EuroSSC 2010, Passau, Germany, 14–16 November 2010; Lukowicz, P., Kunze, K., Kortuem, G., Eds.; Springer: Heidelberg, Germany, 2010; Volume 6446, pp. 177–201. [Google Scholar]
- Hanke, S.; Mayer, C.; Hoeftberger, O.; Boos, H.; Wichert, R.; Tazari, M.R.; Wolf, P.; Furfari, F. UniversAAL—An Open and Consolidated AAL Platform. In Ambient Assisted Living; Springer: Berlin/Heidelberg, Germany, 2011; pp. 127–140. [Google Scholar]
- Roeder, P.; Mosmonder, M.; Obermaisser, R.; Boos, H. UniversAAL Project of the Framework Programme, D6.1—A Training Plan and Training Material; Special session on Open Source in European Health Care: Valencia, Spain, 2010. [Google Scholar]
- Fernandez-Montes, A.; Alvarez, J.A.; Ortega, J.A.; Madrid, N.M.; Seepold, R. An orientation service for dependent people based on an open architecture. In HCI and Usability for Medicine and Health Care, Proceedings of the 3rd Human-Computer Interaction and Usability Engineering of the Austrian Computer Society, Graz, Austria, 22 November 2007; Springer: Berlin/Heidelberg, Germany, 2007; pp. 155–164. [Google Scholar]
- Gachet Paez, D.; de Buenaga, M.; Villalba, M.; Lara, P. An Open and Adaptable Platform for the elderly people andpersons with disability to access the Information Society. The Naviga project. In Proceedings of the 4th International Conference on Pervasive Computing Technologies for Healthcare (PervasiveHealth), Munich, Germany, 22–25 March 2010; pp. 1–5. [Google Scholar]
- Noury, N. AILISA: Experimental Platforms to Evaluate Remote Care and Assistive Technologies in Gerontology; TIMC-IMAG, Faculte de Medecine de Grenoble: La Tronche CEDEX, France, 2005. [Google Scholar]
- Antonino, P.O.; Schneider, D.; Hofmann, C.; Nakagawa, E.Y. Evaluation of AAL platforms according to architecture-based quality attributes. In Proceedings of the 2nd International Conference on Ambient Intelligence (AmI 2011), Amsterdam, The Netherlands, 16–18 November 2011; pp. 264–274. [Google Scholar]
- Fuxreiter, T.; Mayer, C.; Hanke, S.; Gira, M.; Sili, M.; Kropf, J. A Modular Platform for Event Recognition in Smart Homes. In Proceedings of the 12th IEEE International Conference on e-Health Networking, Applications and Services, Lyon, France, 1–3 July 2010. [Google Scholar]
- Wille, S.; Shcherbakov, I.; de Souza, L.; Wehn, N. TinySEP—A Tiny Platform for Ambient Assisted Living. In Ambient Assisted Living; Springer: Berlin/Heidelberg, Germany, 2012; pp. 229–243. [Google Scholar]
- Winkley, J.; Jiang, P.; Jiang, W. Verity: An ambient assisted living platform. IEEE Trans. Consum. Electron. 2012, 58, 364–373. [Google Scholar] [CrossRef]
- Soprano. Available online: http://www.soprano-ip.org/ (accessed on 22 November 2017).
- INHOME Project. An Intelligent Interactive Services Environment for Assisted Living at Home. STReP in the 6th Framework Programme of the European Union. 2007. [Google Scholar]
- EASY-LINE+ Project. Low Cost Advanced White Goods for a Longer Independent Life of Elderly People. STReP in the 6th Framework Programme of the European Union. 2007. Available online: http://www.arenque-ks.com/easynet (accessed on 20 July 2018).
- Delgado, A.R.; Blasco, R.; Marco, Á.; Cirujano, D.; Casas, R.; Yarza, A.R.; Grout, V.; Picking, R. Agent-based AmI system case study: The easy Line+ project. In Trends in Practical Applications of Agents and Multiagent Systems; Springer: Berlin/Heidelberg, Germany, 2010; pp. 157–164. [Google Scholar]
- DynAMITE Project. Dynamic Adaptive Multimodal It Ensenbles. Research Project of the German Federal Ministry of Education and Research. 2004. Available online: http://www.dynamiteproject.org (accessed on 22 November 2017).
- PERSONA Project. Perceptive Spaces Promoting Independent Aging. IP in the 6th Framework Programme of the European Union. 2007. Available online: http://www.aal-persona.org (accessed on 22 November 2017).
- AMIGO Project. Ambient Intelligence for the Networked Home Environment. STReP in the 6th Framework Programme of the European Union. 2004. Available online: http://www.amigo-project.org (accessed on 22 November 2017).
- MONAMI Project. Mainstreaming on Ambient Intelligence. IP in the 6th Framework Programme of the European Union. 2006. Available online: http://www.monami.info (accessed on 22 November 2017).
- SENSACTION-AAL Project. Sensing and Action to Support Mobility in Ambient Assisted Living. STReP in the 6th Framework Programme of the European Union. 2007. Available online: http://www.sensaction-aal.eu (accessed on 22 November 2017).
- I-Living Project. The Assisted Living Project. Research Project in NSF’s Computer Systems Research Program. 2005. Available online: http://lion.cs.uiuc.edu/assistedliving (accessed on 22 November 2017).
- EMBASSI Project. Multimodal Assistance for Infotainment and Service Infrastructures. Research Project of the German Federal Ministry of Education and Research. 2001. Available online: http://www.embassi.de (accessed on 22 November 2017).
- MAP Project. Multimedia Workplace of the Future; German Federal Ministry of Economics and Technology: Berlin, Germany, 2000. [Google Scholar]
- SmartKom Project. Dialog-Based Human-Technology Interaction by Co-Ordinated Analysis and Generation of Multiple Modalities; German Federal Ministry of Education and Research: Bonn, Germany, 2000. [Google Scholar]
- EMERGE: Emergency Monitoring and Prevention, Specific Targeted Research Project (STREP) of the EC, Project No. 045056. Available online: http://www.emergeproject.eu (accessed on 17 October 2017).
- ALADIN Project. Ambient lighting assistance for an ageing population. In STReP in the 6th Framework Programme of the European Union; European Commission: Brussels, Belgium, 2007. [Google Scholar]
- OLDES Project. Older People’S e-Services at Home. In STReP in the 6th Framework Programme of the European Union; European Commission: Brussels, Belgium, 2007. [Google Scholar]
- ENABLE Project. ABLE Project. A Wearable System Supporting Services to Enable Elderly People to Live Well, Independently and at Ease. In STReP in the 6th Framework Programme of the European Union; European Commission: Brussels, Belgium, 2007. [Google Scholar]
- SHARE-IT Project. Supported human autonomy for recovery and enhancement of cognitive and motor abilities using information technologies. In STReP in the 6th Framework Programme of the European Union; European Commission: Brussels, Belgium, 2007. [Google Scholar]
- Closs, L.; da Costa, C.A.; da Rosa Righi, R. Here I Am: Nfc-Based Indoor Location Model. In Proceedings of the 13th International Conference WWW/Internet (ICWI 2014), Porto, Portugal, 25–27 October 2014. [Google Scholar]
- Moser, C.; Kargl, T.; Tscheligi, M.; Feldbacher, B.; Collini-Nocker, B.; Harutunian, M.; Schiller, F.; Eitelberg, M.; Altaani, N.; Eisele, M.; et al. GeTVivid: A TV Platform for P2P Support Exchange. In Proceedings of the TVX2015, Brussels, Belgium, 3–5 June 2015. [Google Scholar]
- Passas, N.; Fried, M.; Manolakos, E.S. PeerAssist: A p2p platform supporting virtual communities to assist independent living of senior citizens. In Ambient Assisted Living and Home Care; Springer: Berlin/Heidelberg, Germany, 2012; pp. 25–32. 2p. [Google Scholar]
- Liu, S.; Wang, S.; Zhu, F.; Zhang, J.; Krishnan, R. Hydra: Large-scale social identity linkage via heterogeneous behavior modeling. In Proceedings of the 2014 ACM SIGMOD International Conference on Management of Data, Snowbird, UT, USA, 22–27 June 2014; pp. 51–62. [Google Scholar]
- Grguric, A.; Gil, A.M.M.; Huljenic, D.; Car, Z.; Podobnik, V. A Survey on User Interaction Mechanisms for Enhanced Living Environments. In ICT Innovations 2015; Springer International Publishing: Cham, Switzerland, 2016; pp. 131–141. [Google Scholar]
- Iverson, D.L. Inductive System Health Monitoring. In Proceedings of the IC-AI 2004, Las Vegas, NV, USA, 21–24 June 2004; pp. 605–611. [Google Scholar]
- Junnila, S.; Kailanto, H.; Merilahti, J.; Vainio, A.M.; Vehkaoja, A.; Zakrzewski, M.; Hyttinen, J. Wireless, multipurpose in-home health monitoring platform: Two case trials. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 447–455. [Google Scholar] [CrossRef] [PubMed]
- Hittle, D.F.; Shaughnessy, P.W.; Crisler, K.S.; Powell, M.C.; Richard, A.A.; Conway, K.S.; Stearns, P.M.; Engle, K. A study of reliability and burden of home health assessment using OASIS. Home Health Care Serv. Q. 2004, 22, 43–63. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, L.; Ambrosio, P. Towards an interoperable health-assistive environment: The eHealthCom platform. In Proceedings of the 2012 IEEE-EMBS International Conference onBiomedical and Health Informatics (BHI), Hong Kong, China, 5–7 January 2012; pp. 930–932. [Google Scholar]
- Jacobs, A.; Duysburgh, P.; Bleumers, L.; Ongenae, F.; Ackaert, A.; Verstichel, S. The innovation binder approach: A guide towards a social-technical balanced pervasive health system. In Pervasive Health; Springer: London, UK, 2014; pp. 69–99. [Google Scholar]
- Mikalsen, M.; Hanke, S.; Fuxreiter, T.; Walderhaug, S.; Wienhofen, L.W.; Trondheim, N. Interoperability services in the MPOWER Ambient Assisted Living platform. In Medical Informatics in a United and Healthy Europe; IOS Press: Amsterdam, The Netherlands, 2009; Volume 150, pp. 366–370. [Google Scholar]
- Jung, E.Y.; Kim, J.H.; Chung, K.Y.; Park, D.K. Home health gateway based healthcare services through U-health platform. Wirel. Pers. Commun. 2013, 73, 207–218. [Google Scholar] [CrossRef]
- Costa, R.; Novais, P.; Lima, L.; Carneiro, D.; Samico, D.; Oliveira, J.; Machado, J.; Neves, J. Virtualecare: Intelligent assisted living. In Electronic Healthcare; Springer: Berlin/Heidelberg, Germany, 2009; pp. 138–144. [Google Scholar]
- Schlögl, S.; Chollet, G.; Milhorat, P.; Deslis, J.; Feldmar, J.; Boudy, J.; Garschall, M.; Tscheligi, M. Using Wizard of Oz to Collect Interaction Data for Voice Controlled Home Care and Communication Services. In Proceedings of the International Conference on Signal Processing, Pattern Recognition and Applications, Innsbruck, Austria, 12–14 February 2013; pp. 12–14. [Google Scholar]
- Kieffer, S.; Lawson, J.-Y.; Macq, B. User-centered Design and Fast Prototyping of an Ambient Assisted Living System for Elderly People. In Proceedings of the 2009 Sixth International Conference on Information Technology: New Generations (ITNG ’09), Las Vegas, NV, USA, 27–29 April 2009; pp. 1220–1225. [Google Scholar]
- SeniorNet Members Interest Survey. 2004. Available online: http://www.seniornet.org/php/default.php?PageID=7414 (accessed on 9 June 2017).
- Kleinberger, T.; Jedlitschka, A.; Storf, H.; Steinbach-Nordmann, S.; Prueckner, S. An approach to and evaluations of Assisted Living Systems Using Ambient Intelligence for Emergency Monitoring and Prevention. In Universal Access in Human-Computer Interaction, Part II: Intelligent and Ubiquitous Interaction Environments, Proceedings of the UAHCI 2009, San Diego, CA, USA, 19–24 July 2009; Stephanidis, C., Ed.; Springer: Berlin/Heidelberg, Germany, 2009; pp. 199–208. [Google Scholar]
- University of Rochester, Center of Future Health. Available online: http://www.futurehealth.rochester.edu/news/ (accessed on 6 November 2017).
- Wang, Q.; Shin, W.; Liu, X.; Zeng, Z.; Oh, C.; AlShebli, B.K.; Sha, L. I-Living: An Open System Architecture for Assisted Living. In Proceedings of the 2006 IEEE International Conference on Systems, Man and Cybernetics, Taipei, Taiwan, 8–11 October 2006; pp. 4268–4275. [Google Scholar]
- Domenech, S.; Rivero, J.; Coll-Planas, L.; Sainz, F.J.; Reissner, A.; Miralles, F. Involving older people in the design of an innovative information and Communication technologies system promoting active aging: The saapho project. J. Access. Des. All 2013, 3, 13–27. [Google Scholar]
- Rivero-Espinosa, J.; Iglesias-Péreza, A.; Gutiérrez Dueñasa, J.A.; Rafael Paloub, X. SAAPHO: An AAL architecture to provide accessible and usable active aging services for the elderly. In Proceedings of the ACM SIGACCESS Accessibility and Computing, Bellevue, WA, USA, 21–23 October 2013; Volume 107, pp. 17–24. [Google Scholar]
- Messens, L.; Quinn, S.; Saez, I.; Squillace, P. Home Sweet Home: Health Monitoring and Social Integration Environment for Supporting Wide Extension of Independent Life at HOME; ICT PSP—Health, Ageing and Inclusion Programme; Grant Agreement No 250449; Document D7.3; Intermediate Trial Evaluation Report; ICT PSP: Brussels, Belgium, 2013. [Google Scholar]
- Huang, A.; Chen, C.; Bian, K.; Duan, X.; Chen, M.; Gao, H.; Meng, C.; Zheng, Q.; Zhang, Y.; Jiao, B.; et al. WE-CARE: An intelligent mobile telecardiology system to enable mHealth applications. IEEE J. Biomed. Health Inform. 2014, 18, 693–702. [Google Scholar] [CrossRef] [PubMed]
- Moen, A.; Brennan, P.F. Health @ Home: The work of health information management in the household (HIMH): Implications for consumer health informatics (CHI) innovations. J. Am. Med. Inform. Assoc. 2005, 12, 648–656. [Google Scholar] [CrossRef] [PubMed]
- Jara, A.J.; Zamora, M.A.; Skarmeta, A.F. An internet of things—Based personal device for diabetes therapy management in ambient assisted living (AAL). Pers. Ubiquitous Comput. 2011, 15, 431–440. [Google Scholar] [CrossRef]
- Rodriguez, M.D.; Roa, J.R.; Morán, A.L.; Nava-Muñoz, S. CAMMInA: A mobile ambient information system to motivate elders to exercise. Pers. Ubiquitous Comput. 2013, 17, 1127–1134. [Google Scholar] [CrossRef]
- Foix, L.C.; Morillo, D.S.; Crespo, M.; Gross, N.; Kunze, C.; Giokas, K.; Jiménez, J. AMICA telemedicine platform: A design for management of elderly people with COPD. In Proceedings of the 9th International Conference onInformation Technology and Applications in Biomedicine (ITAB 2009), Larnaca, Cyprus, 4–7 November 2009; pp. 1–4. [Google Scholar]
- Bleda, A.L.; Maestre, R.; Jara, A.J.; Skarmeta, A.G. Ambient Assisted Living Tools for a Sustanaible Aging Society. In Resource Management in Mobile Computing Environments; Springer: Cham, Switzerland, 2014; pp. 193–220. [Google Scholar]
- Huch, M. AAL: Ambient Assisted Living for Europe. Gerontechnology 2009, 8, 114. [Google Scholar] [CrossRef]
- Ackaert, A.; Van Hoecke, S.; Moerman, I.; Laermans, E.; Van Boxstael, K.; Demeester, P.; De Moor, G.; Buysse, H.; Spinhof, L.; De Grooff, D.; et al. Innovative Communication Platforms for Interactive eHomeCare, Methods of Information in Medicine; Thieme: Stuttgart, Germany, 2008. [Google Scholar]
- Cesta, A.; Coradeschi, S.; Cortellessa, G.; Gonzalez, J.; Tiberio, L.; Von Rump, S. Enabling social interaction through embodiment in ExCITE. In Proceedings of the Second Italian Forum on Ambient Assisted Living (ForItAAL), Trento, Italy, 5–7 October 2010; pp. 1–7. [Google Scholar]
- Katz, S.; Ford, A.B.; Moskowitz, R.W.; Jackson, B.A.; Jaffe, M.W. Studies of Illness in the Aged: The Index of ADL: A Standardized Measure of Biological and Psychosocial Function. J. Am. Med. Assoc. 1963, 185, 914–919. [Google Scholar] [CrossRef]
- Kleinberger, T.; Jedlitschka, A.; Storf, H.; Steinbach-Nordmann, S.; Pruckner, S. Evaluation of ADL detection in the EMERGE project. In Proceedings of the 3rd German AAL-congress, Berlin, Germany, 26–27 January 2010. [Google Scholar]
- Nehmer, J.; Becker, M.; Karshmer, A.; Lamm, R. Living assistance systems: an ambient intelligence approach. In Proceedings of the 28th International Conference on Software Engineering, Shanghai, China, 20–28 May 2006. [Google Scholar]
- Georgia Institute of Technology. Aware Home. Available online: http://www.cc.gatech.edu/fce/ahri/ (accessed on 26 September 2017).
- University of Virginia. Smart In-Home Monitoring System. Available online: http://marc.med.virginia.edu/projects_smarthomemonitor.html (accessed on 9 October 2017).
- Intel Corporation. Age-In-Place. Available online: http://www.intel.com/research/prohealth/csaging_in_place.htm (accessed on 1 December 2017).
- Harjumaa, M.; Isomursu, M.; Muuraiskangas, S.; Konttila, A. HearMe: A touch-to-speech UI for medicine identification. In Proceedings of the 2011 5th International Conference on Pervasive Computing Technologies for Healthcare (PervasiveHealth), Dublin, Ireland, 23–26 May 2011; pp. 85–92. [Google Scholar]
- Mayer, C.; Morandell, M.; Gira, M.; Hackbarth, K.; Petzold, M.; Fagel, S. AALuis, a User Interface Layer That Brings Device Independence to Users of AAL Systems; Springer: Berlin/Heidelberg, Germany, 2012; pp. 650–657. [Google Scholar]
- Røssvoll, T.H. The European MobileSage project—Situated adaptive guidance for the mobile elderly: Overview, status, and preliminary results. In Proceedings of the Sixth International Conference on Advances in Computer-Human Interactions (ACHI), Nice, France, 24 February–1 March 2013. [Google Scholar]
- Peek, S.; Kristoffersson, A.; Covlescu, I. Session E8: ICT Solutions for Enabling Social Interaction. Available online: http://t.cn/RglF4hg (accessed on 20 July 2018).
- Adel, T.; Simon, M.; Lina, B.; Salomie, I.; Cioara, T.; Anghel, I.; Thomas, S.; Sanchez, V. B2. 5. DlET4ELDERS: A Service-Oriented Architecture for the Prevention and Self-Management of Malnutrition. In Proceedings of the AAL Forum 2014, Bucharest, Romania, 9–12 September 2014. [Google Scholar]
- Chiriac, S.; Saurer, B.R.; Stummer, G.; Kunze, C. Introducing a low cost ambient monitoring system for activity recognition. In Proceedings of the 2011 5th International Conference on Pervasive Computing Technologies for Healthcare (PervasiveHealth), Dublin, Ireland, 23–26 May 2011; pp. 340–345. [Google Scholar]
- Tiadjio, A.M.; Jamboti, K. Requirements and Evaluation of Safety Analysis Techniques for Ambient Assisted Living Systems. In Proceedings of the 2012 IEEE 23rd International Symposium on Software Reliability Engineering Workshops (ISSREW), Dallas, TX, USA, 27–30 November 2012; pp. 319–324. [Google Scholar]
- CONFIDENCE. Available online: http://www.confidence-eu.org (accessed on 9 June 2017).
- Gams, M.; Dovgan, E.; Cvetkovic, B.; Mircevska, V.; Kaluza, B.; Lustrek, M.; Velez, I. AAL for supporting elderly. In Proceedings of the IST-Africa Conference Proceedings, Gaborone, Botswana, 11–13 May 2011; pp. 1–8. [Google Scholar]
- Gams, M.; Dovgan, E.; Cvetković, B.; Mirćevska, V.; Kaluža, B.; Luštrek, M.; Velez, I. AAL for supporting elderly. In Proceedings of the IST-Africa Conference, Gaborone, Botswana, 11–13 May 2011. [Google Scholar]
- Gaden, U.; Löhrke, E.; Reich, M.; Schröer, W.; Stevens, T.; Vieregge, T. SAMDY-Ein sensorbasiertes adaptives Monitoringsystem für die Verhaltensanalyse von Senioren. In Ambient Assisted Living-AAL; AAL-Kongress: Berlin, Germany, 25–26 January 2011. [Google Scholar]
- Mancini, A.; Zingaretti, P. Point to point navigation for people with mobility impairments. In Proceedings of the 2014 IEEE/ASME 10th International Conference on Mechatronic and Embedded Systems and Applications (MESA), Senigallia, Italy, 10–12 September 2014; pp. 1–6. [Google Scholar]
- Wac, K.; Fiordelli, M.; Gustarini, M.; Rivas, H. Quality of Life Technologies: Experiences from the Field and Key Research Challenges. IEEE Internet Comput. 2015, 19, 28–35. [Google Scholar] [CrossRef]
- Hendeby, G.; Bleser, G.; Lamprinos, I.; Stricker, D. Healthy aging using physical activity monitoring. Germ. Res. 2010, 122, 67663. [Google Scholar]
- Krieg-Brückner, B.; Bothmer, H.; Budelmann, C.; Crombie, D.; Guerin, A.; Heindorf, A.; Lifante, J.; Martínez, A.B.; Millet, S.; Vellemann, E. Assistance for safe mobility: The ASSAM project. In Proceedings of the AAL-Forum, Eindhoven, The Netherlands, 24–27 September 2012. [Google Scholar]
- Morandell, M.; Rumsch, A.; Biallas, M.; Kindberg, S.; Züsli, R.; Lurf, R.; Fuxreiter, T. iWalkActive: An Active Walker for Active People. Assist. Technol. Res. Ser. 2013, 33, 216–221. [Google Scholar]
- Benetazzo, F.; Ferracuti, F.; Freddi, A.; Giantomassi, A.; Iarlori, S.; Longhi, S.; Monteriù, A.; Ortenzi, D. AAL Technologies for Independent Life of Elderly People. In Ambient Assisted Living; Springer International Publishing: Cham, Switzerland, 2015; pp. 329–343. [Google Scholar]
- Magnusson, C.; Östlund, B.; Rassmus-Gröhn, K.; Hedlund, A. Making navigation simple? Initial user studies within the NavMem project. In Universal Design 2014: Three Days of Creativity and Diversity, Proceedings of the International Conference on Universal Design, Lund, Sweden, 16–18 June 2014; IOS Press: Amsterdam, The Netherlands, 2014; Volume 35, p. 214. [Google Scholar]
- Tarnauca, B.; Puiu, D.; Nechifor, S.; Comnac, V. Using Complex Event Processing for implementing a geofencing service. In Proceedings of the 2013 IEEE 11th International Symposium on Intelligent Systems and Informatics (SISY), Subotica, Serbia, 26–28 September 2013; pp. 391–396. [Google Scholar]
- Sánchez-Tato, I.; del Toro, J.C.; Pérez, E.J.; Urdiales, C.; Cortés, U.; Annicchiaricco, R.; Sandoval, F.; Caltagirone, C. Collaborative control for personalized mobility assistance to persons with physical/cognitive disabilities. In Proceedings of the IROS 2007 Workshop on Assistive Technologies, San Diego, CA, USA, 29 October–2 November 2007. [Google Scholar]
- Cristancho-Lacroix, V. Seniors’ Navigation: Understanding Their Needs so as to Create an Adaptive Smartphone Application. In Proceedings of the Medicine 2.0 Conference, London, UK, 23–24 September 2013; JMIR Publications Inc.: Toronto, ON, Canada, 2013. [Google Scholar]
- ASK-IT. Ambient Intelligence System of Agents for Knowledge-Based and Integrated Services for Mobility Impaired Users. Available online: https://cordis.europa.eu/project/rcn/72134_en.html (accessed on 20 July 2018).
- Bekiaris, E.; Panou, M.; Mousadakou, A. Elderly and disabled travelers needs in infomobility services. In Universal Acess in Human Computer Interaction. Coping with Diversity; Springer: Berlin/Heidelberg, Germany, 2017. [Google Scholar]
- Lattanzio, F.; Abbatecola, A.M.; Bevilacqua, R.; Chiatti, C.; Corsonello, A.; Rossi, L.; Bustacchini, S.; Bernabei, R. Advanced technology care innovation for older people in Italy: Necessity and opportunity to promote health and wellbeing. J. Am. Med. Dir. Assoc. 2014, 15, 457–466. [Google Scholar] [CrossRef] [PubMed]
- Mihelj, M.; Novak, D.; Munih, M. Emotion-aware system for upper extremity rehabilitation. In Proceedings of the Virtual Rehabilitation International Conference, Haifa, Israel, 29 June–2 July 2009; pp. 160–165. [Google Scholar]
- Mowafey, S.; Gardner, S. A novel adaptive approach for home care ambient intelligent environments with an emotion-aware system. In Proceedings of the 2012 UKACC International Conference on Control, Cardiff, UK, 3–5 September 2012; pp. 771–777. [Google Scholar]
- Waterworth, J.A.; Ballesteros, S.; Peter, C.; Bieber, G.; Kreiner, A.; Wiratanaya, A.; Polymenakos, L.; Wanche-Politis, S.; Capobianco, M.; Etxeberria, I.; et al. Ageing in a networked society: Social inclusion and mental stimulation. In Proceedings of the 2nd International Conference on PErvasive Technologies Related to Assistive Environments, Corfu, Greece, 9–13 June 2009; p. 46. [Google Scholar]
- Pensas, H.; Kivimäki, T.; Vainio, A.M.; Konakas, S.; Costicoglou, S.; Kölndorfer, P.; Summanen, K.; Moisio, H.; Vanhala, J. Building a Client-Server Social Network Application for Elders and Safety Net. In Proceedings of the International Conference on Making Sense of Converging Media, Tampere, Finland, 1–4 October 2013; p. 310. [Google Scholar]
- Tantinger, D.; Braun, A. Virtual Coach Reaches Out to me: The V2me-Project. ERCIM News 2011, 87, 34–35. [Google Scholar]
- Spengler, S.; Woll, A. The more physically active, the healthier? The relationship between physical activity and health-related quality of life in adolescents: The MoMo study. J. Phys. Act. Health 2013, 10, 708–715. [Google Scholar] [CrossRef] [PubMed]
- DFA@INCLUSION. Design for All for e-Inclusion. Available online: https://cordis.europa.eu/project/rcn/80544_en.html (accessed on 20 July 2018).
- EU4ALL. European Unified Approach for Accesible Lifelong Learning. Available online: https://cordis.europa.eu/project/rcn/80191_en.html (accessed on 20 July 2018).
- Petz, A.; Miesenberger, K. Dealing with Changes in Supporting Students with Disabilities in Higher Education; Springer: Berlin/Heidelberg, Germany, 2012. [Google Scholar]
- Kamel Boulos, M.N.; Castellot Lou, R.; Anastasiou, A.; Nugent, C.D.; Alexandersson, J.; Zimmermann, G.; Cortes, U.; Casas, R. Connectivity for Healthcare and Well-Being Management: Examples from Six European Projects. Int. J. Environ. Res. Public Health 2009, 6, 1947–1971. [Google Scholar] [CrossRef] [PubMed]
- I2HOME: Intuitive Interaction for Everyone with Home Appliances Based on Industry Standards. Available online: http://www.i2home.org/ (accessed on 9 June 2017).
- Takács, B.; Hanák, D. A mobile system for assisted living with ambient facial interfaces. IADIS Int. J. Comput. Sci. Inf. Syst. 2007, 2, 33–50. [Google Scholar]
- Siciliano, P.; Leone, A.; Diraco, G.; Distante, C.; Malfatti, M.; Gonzo, L.; Grassi, M.; Lombardi, A.; Rescio, G.; Malcovati, P. A networked multisensor system for ambient assisted living application. In Proceedings of the 2009 3rd International Workshop on Advances in Sensors and Interfaces (IWASI 2009), Trani, Italy, 25–26 June 2009; pp. 139–143. [Google Scholar]
- HOMER. Available online: http://homer.aaloa.org/redmine/documents/2 (accessed on 20 January 2018).
- Boulos, M.N.; Rocha, A.; Martins, A.; Vicente, M.E.; Bolz, A.; Feld, R.; Tchoudovski, I.; Braecklein, M.; Nelson, J.; Laighin, G.Ó.; et al. CAALYX: A new generation of location-based services in healthcare. Int. J. Health Geogr. 2007, 6, 9. [Google Scholar] [CrossRef] [PubMed]
- eCAALYX: Enhanced Complete Ambient Assisted Living Experiment. Available online: http://ecaalyx.org/ (accessed on 9 June 2017).
- Hein, A.; Kirste, T. Activity Recognition for Ambient Assisted Living: Potential and Challenges. In Proceedings of the 1st German AAL-Congress, Berlin, Germany, 1 February 2008. [Google Scholar]
- Pollack, M.E. Intelligent Technology for an Aging Population-The Use of AI to Assist Elders with Cognitive Impairment. In Proceedings of the American Association for Artificial Intelligence, Pittsburgh, PA, USA, 9–13 July 2005. [Google Scholar]
- Fitzgerald, W.; Firby, R.J.; Phillips, A.; Kairys, A. Complex Event Recognition for Long-Term System Monitoring. In Proceedings of the AAAI 2004 Spring Symposium Series, California, CA, USA, 22–24 March 2004. [Google Scholar]
- Luckham, D. The Power of Events: An Introduction to Complex Event Processing in Distributed Enterprise Systems; Addison-Wesley: Reading, UK, 2002; pp. 145–174. [Google Scholar]
- Tapia, E.M.; Intille, S.S.; Larson, K. Activity Recognition in the Home Using Simple and Ubiquitous Sensors. In Lecture Notes in Computer Science, Proceedings of the PERVASIVE 2004, Linz and Vienna, Austria, 21–23 April 2004; Ferscha, A., Mattern, F., Eds.; Springer: Heidelberg, Germany, 2004; Volume 3001, pp. 158–175. [Google Scholar]
- Castro, M.D.; Ruiz-Mezcua, B.; Sánchez-Pena, J.M.; García-Crespo, Á.; Iglesias, A.; Pajares, J.L. Tablets Helping Elderly and Disabled People; Smart Homes. Dutch Expert Centre On Home Automation, Smart Living & E-Health: Holanda, The Netherlands, 2012; pp. 237–244. [Google Scholar]
- Cameirao, M.S.; Badia, S.B.; Oller, E.D.; Verschure, P.F.M.J. Neurorehabilitation using the virtual reality based Rehabilitation Gaming System: Methodology, design, psychometrics, usability and validation. J. Neuroeng. Rehabil. 2010, 7, 48. [Google Scholar] [CrossRef] [PubMed]
- Consolvo, S.; McDonald, D.W.; Toscos, T.; Chen, M.Y.; Froehlich, J.; Harrison, B.; Klasnja, P.; LaMarca, A.; LeGrand, L.; Libby, R.; et al. Activity sensing in the wild: A field trial of ubifit garden. In Proceedings of the SIGCHI Conference on Human Factors in Computing Systems, Florence, France, 5–10 April 2008; pp. 1797–1806. [Google Scholar]
- Campos-Soriano, N.; Blasco-López, C.; Laparra-Hernández, J.; Poveda-Puente, R.; Barberà-Guillem, R.; García, A.; Soriano, C.; Sancho, M. Bank4Elder: Innovative Banking Interfaces Adapted to Older People Needs and Capabilities. Assist. Technol. Res. Pract. 2013, 33, 40. [Google Scholar]
- Peterson, C.B.; Prasad, N.R. Easy Life, Intelligent Systems, and Life 2.0: European Research on ICT for Aging Adults. In Proceedings of the IASTED HCI Conference, Scottsdale, AZ, USA, 17–19 November 2003. [Google Scholar]
- Poorejbari, S.; Vahdat-Nejad, H. An Introduction to Cloud-Based Pervasive Healthcare Systems. In Proceedings of the 4th International Workshop on Pervasive and Context-Aware Middleware, Dubai, UAE, 15 October 2014. [Google Scholar]
- Tung, H.H.; Ye, K.Y.; Guo, Z.G.; Chen, M.X.; Haung, Y.Q. LED alert bracelet for patients with cognitive dysfunction. In Proceedings of the 2015 IEEE MTT-S International Microwave Workshop Series on RF and Wireless Technologies for Biomedical and Healthcare Applications (IMWS-BIO), Taipei, Taiwan, 21–23 September 2015; pp. 45–46. [Google Scholar]
- Hristova, A.; Bernardos, A.M.; Casar, J.R. Context-aware services for ambient assisted living: A case-study. In Proceedings of the First International Symposium on Applied Sciences on Biomedical and Communication Technologies (ISABEL’08), Aalborg, Denmark, 25–28 October 2008; pp. 1–5. [Google Scholar]
- Kutzik, D.M.; Glasscock, A.P.; Lundberg, L.Y.; York, J.A. Technological Tools of the Future. In The Assisted Living Residence: A Vision for the Future; The Johns Hopkins University Press: Baltimore, MD, USA, 2008. [Google Scholar]
- Biocca, L.; Dewsbury, G. Housing and Technologies in the EU for Promoting Quality of Life: Current Trends in the UK and Italy. Available online: http://www.irbnet.de/daten/iconda/CIB9775.pdf (accessed on 19 July 2018).
- Scott, V.; Votova, K.; Scanlan, A.; Close, J. Multifactorial and functional mobility assessment tools for fall risk among older adults in community, home-support, long-term and acute care settings. Age Ageing 2007, 36, 130–139. [Google Scholar] [CrossRef] [PubMed]
- Kumar, V. Implantable RFID Chips: Security versus Ethics. In IFIP International Federation for Information Processing; Springer: Boston, MA, USA, 2008. [Google Scholar]
- Hightower, J.; Want, R.; Borriello, G. SpotON: An Indoor 3D Location Sensing Technology Based on RF Signal Strength; UW CSE 00-02-02; University of Washington, Department of Computer Science and Engineering: Seattle, WA, USA, 2000; Volume 1. [Google Scholar]
- Ni, L.M.; Liu, Y.; Lau, Y.C.; Patil, A.P. LANDMARC: Indoor location sensing using active RFID. Wirel. Netw. 2004, 10, 701–710. [Google Scholar] [CrossRef]
- Doshi-Velez, F.; Li, W.; Battat, Y.; Charrow, B.; Curthis, D.; Park, J.G.; Hemachandra, S.; Velez, J.; Walsh, C.; Fredette, D.; et al. Improving safety and operational efficiency in residential care settings with WiFi-based localization. J. Am. Med. Dir. Assoc. 2012, 13, 558–563. [Google Scholar] [CrossRef] [PubMed]
- Timmermanns, S.; Felscher, A.; Heindorf, A.; Wallhoff, F.; Meiss, M. User Integration by the Evaluation of an Emergency Call System in the Context of the Research Project MOBECS. In Ambient Assisted Living; Springer International Publishing: Cham, Switzerland, 2015; pp. 105–110. [Google Scholar]
- Hodgkinson, B.; Koch, S.; Nay, R.; Lewis, M. Managing the wandering behaviour of people living in a residential aged care facility. Int. J. Evid.-Based Healthc. 2007, 5, 406–436. [Google Scholar] [PubMed]
- Augusto, J.C.; Zheng, H.; Mulvenna, M.; Wang, H.; Carswell, W.; Jeffers, P. Design and modelling of the nocturnal AAL care system. In Ambient Intelligence-Software and Applications; Springer: Berlin/Heidelberg, Germany, 2011; pp. 109–116. [Google Scholar]
- Iqbal, M.U.; Lim, S. Legal and ethical implications of GPS vulnerabilities. J. Int. Commer. Law Technol. 2008, 3, 178. [Google Scholar]
- Huang, G.C.; Smith, C.C.; Gordon, C.E.; Feller-Kopman, D.J.; Davis, R.B.; Phillips, R.S.; Weingart, S.N. Beyond the comfort zone: Residents assess their comfort performing inpatient medical procedures. Am. J. Med. 2006, 119, 71. [Google Scholar] [CrossRef] [PubMed]
- Hong, J.; Baker, M. From GPS Shoes to Instrumented Cities: Food for Thought. IEEE Pervasive Comput. 2013, 2, 86–88. [Google Scholar] [CrossRef]
- GTX Corp. Patrick Bertagna, GPSshoes. Available online: http://www.gtxcorp.com/investors (accessed on 14 November 2017).
- CogKnow: Helping People with Mild Dementia Navigate Their Day. Available online: http://www.cogknow.eu (accessed on 9 June 2017).
- Maeso Garcia, J.; Jorge Hernandez, F.; Garcia-Zapirain Soto, B.; Mendez Zorrilla, A.; Fernandez-Ruanova, B.; Alday Jurado, A.; Llano Hernaiz, J.X. Teleassistance outdoor system for the elderly based on android devices. In Proceedings of the 2013 IEEE International Symposium on Signal Processing and Information Technology (ISSPIT), Athens, Greece, 12–15 December 2013. [Google Scholar]
- Wan, J.; Byrne, C.; O’Hare, G.M.; O’Grady, M.J. OutCare: Support dementia patients in outdoor scenarios. In Proceedings of the International Conference on Knowledge-Based and Intelligent Information and Engineering Systems, Cardiff, UK, 8–10 September 2010. [Google Scholar]
- Wan, J.; Byrne, C.; O’Hare, G.M.; O’Grady, M.J. Orange alerts: Lessons from an outdoor case study. In Proceedings of the 2011 5th International Conference on Pervasive Computing Technologies for Healthcare (PervasiveHealth), Dublin, Ireland, 23–26 May 2011; pp. 446–451. [Google Scholar]
- Wan, J.; Byrne, C.; O’Grady, M.J.; O’Hare, G.M. Managing Wandering Risk in People With Dementia. IEEE Trans. Hum. Mach. Syst. 2015, 45, 819–823. [Google Scholar] [CrossRef]
- Fudickar, S.; Schnor, B. KopAL—A Mobile Orientation System for Dementia Patients. In Intelligent Interactive Assistance and Mobile Multimedia Computing; Springer: Berlin/Heidelberg, Germany, 2009; pp. 109–118. [Google Scholar]
- Patterson, D.J.; Liao, L.; Gajos, K.; Collier, M.; Livic, N.; Olson, K.; Wang, S.; Fox, D.; Kautz, H. Opportunity knocks: A system to provide cognitive assistance with transportation services. In UbiComp 2004: Ubiquitous Computing; Springer: Berlin/Heidelberg, Germany, 2004; pp. 433–450. [Google Scholar]
- Moore, D.H.; Algase, D.L.; Powell-Cope, G.; Applegarth, S.; Beattie, E.R. A framework for managing wandering and preventing elopement. Am. J. Alzheimer’s Dis. Other Dement. 2009, 24, 208–219. [Google Scholar] [CrossRef] [PubMed]
- Lin, Q.; Zhang, D.; Chen, L.; Ni, H.; Zhou, X. Managing Elders Wandering Behavior Using Sensors-based Solutions: A Survey. Int. J. Gerontol. 2014, 8, 49–55. [Google Scholar] [CrossRef]
- Van Megan, F.; Sugar, R.; Latour, L.; Neugebauer, M.; Gefflaut, A. Supporting Diabetes Treatment through Wearable Sensor Integration. In Proceedings of the International Workshop on Wireless Sensor Networks for Health Care, Niagara Falls, ON, Canada, 21–23 May 2007. [Google Scholar]
- Prueckner, S.; Madler, C.; Beyer, D.; Berger, M.; Kleinberger, T.; Becker, M. Emergency Monitoring and Prevention—EU Project EMERGE. Available online: https://cordis.europa.eu/project/rcn/80505_en.html (accessed on 20 July 2018).
- Hildebrand, A.; Sá, V. Embassi: Electronic multimedia and service assistance. In Proceedings of the IMC 2000, London, UK, 26–31 July 2000; pp. 50–59. [Google Scholar]
- Maniatopoulos, G.; McLoughlin, I.; Wilson, R.; Martin, M. Developing virtual healthcare systems in complex multi-agency service settings: The OLDES Project. Electron. J. e-Gov. 2009, 7, 163–170. [Google Scholar]
- Holmes, A.; Duman, H.; Pounds-Cornish, A. The iDorm: Gateway to heterogeneous networking environments. In Proceedings of the International ITEA Workshop on Virtual Home Environments, Paderborn, Germany, 20–21 February 2002; Volume 1, pp. 20–21. [Google Scholar]
- Rialle, V.; Duchene, F.; Noury, N.; Bajolle, L.; Demongeot, J. Health smart home: Information technology for patients at home. Telemed. J. E-Health 2002, 8, 395–409. [Google Scholar] [CrossRef] [PubMed]
- Adlam, T.; Orpwood, R.D. Taking the Gloucester Smart House from the laboratory to the living room. In Proceedings of the 3rd International Workshop on Ubiquitous Computing for Pervasive Healthcare Applications, Nottingham, UK, 4 September 2004. [Google Scholar]
- Uhr, M.B.; Redel, B.; Biallas, M.; Andrushevich, A.; Morandell, M.; Dittenberger, S.; Koscher, A. RelaxedCare-Connecting people in care situations: User involvement to collect informal caregivers needs. Stud. Health Technol. Inform. 2014, 217, 865–872. [Google Scholar]
- Park, S.H.; Won, S.H.; Lee, J.B.; Kim, S.W. Smart home—Digitally engineered domestic life. Pers. Ubiquitous Comput. 2003, 7, 189–196. [Google Scholar] [CrossRef]
- Jiang, L.; Liu, D.Y.; Yang, B. Smart home research. In Proceedings of the Third Conference on Machine Learning and Cybernetics, Shanghai, China, 26–29 August 2004; pp. 659–664. [Google Scholar]
- Munstermann, M. SAMDY–TECHNOLOGIES TO SUPPORT “CARE ON DEMAND”; Fraunhofer: Munich, Germany, 2012; p. 81. [Google Scholar]
- Werner, F.; Diermaier, J.; Schmid, S.; Panek, P. Fall detection with distributed floor-mounted accelerometers: An overview of the development and evaluation of a fall detection system within the project eHome. In Proceedings of the 2011 5th International Conference on Pervasive Computing Technologies for Healthcare (PervasiveHealth), Dublin, Ireland, 23–26 May 2011; pp. 354–361. [Google Scholar]
- Degen, T.; Jaeckel, H.; Rufer, M.; Wyss, S. SPEEDY: A Fall Detector in a Wrist Watch. In Proceedings of the Seventh IEEE International Symposium on Wearable Computers (ISWC), White Plains, NY, USA, 21–23 October 2003; pp. 184–189. [Google Scholar]
- Bektemirova, A. Ambient Assisted living systems and platforms. Comput. Model. New Technol. 2015, 19, 7–10. [Google Scholar]
- Planinc, R.; Kampel, M. Introducing the use of depth data for fall detection. Person. Ubiquitous Comput. 2013, 17, 1063–1072. [Google Scholar] [CrossRef]
- Sixsmith, A.; Johnson, N. A smart sensor to detect the falls of the elderly. IEEE Pervasive Comput. 2004, 3, 42–47. [Google Scholar] [CrossRef]
- Cucchiara, R.; Prati, A.; Vezzani, R. A multi-camera vision system for fall detection and alarm generation. Exp. Syst. 2007, 24, 334–345. [Google Scholar] [CrossRef]
- Chan, H.K.; Zheng, H.; Wang, H.; Gawley, R.; Yang, M.; Sterritt, R. Feasibility study on iPhone accelerometer for gait detection. In Proceedings of the 2011 5th International Conference on Pervasive Computing Technologies for Healthcare (PervasiveHealth), Dublin, Ireland, 23–26 May 2011; pp. 184–187. [Google Scholar]
- Bao, L.; Intille, S.S. Activity recognition from user-annotated acceleration data. In Pervasive Computing; Springer: Berlin/Heidelberg, Germany, 2014; pp. 1–17. [Google Scholar]
- Picard, R.W.; Healey, J. Affective wearables. Pers. Technol. 1997, 1, 231–240. [Google Scholar] [CrossRef]
- Lukowicz, P.; Junker, H.; Stäger, M.; von Bueren, T.; Tröster, G. WearNET: A distributed multi-sensor system for context aware wearables. In UbiComp 2002: Ubiquitous Computing; Springer: Berlin/Heidelberg, Germany, 2002; pp. 361–370. [Google Scholar]
- Lymberis, A. Smart wearables for remote health monitoring, from prevention to rehabilitation: Current R/D, future challenges. In Proceedings of the 4th International IEEE EMBS Special Topic Conference on Information Technology Applications in Biomedicine, Cancun, Mexico, 17–21 September 2003; pp. 272–275. [Google Scholar]
- Patel, S.; Park, H.; Bonato, P.; Chan, L.; Rodgers, M. A review of wearable sensors and systems with application in rehabilitation. J. Neuroeng. Rehabil. 2012, 9, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Bodine, K.; Gemperle, F. Effects of functionality on perceived comfort of wearables. In Proceedings of the Seventh IEEE International Symposium on Wearable Computers, White Plains, NY, USA, 21–23 October 2003; p. 57. [Google Scholar]
- Mayol, W.W.; Davison, A.J.; Tordoff, B.J.; Murray, D.W. Applying active vision and slam to wearables. In Robotics Research. The Eleventh International Symposium; Springer: Berlin/Heidelberg, Germany, 2005; pp. 325–334. [Google Scholar]
- Meng, Y.; Zhao, Y.; Hu, C.; Cheng, H.; Hu, Y.; Zhang, Z.; Shi, G.; Qu, L. All-Graphene Core-Sheath Microfibers for All-Solid-State, Stretchable Fibriform Supercapacitors and Wearable Electronic Textiles. Adv. Mater. 2013, 25, 2326–2331. [Google Scholar] [CrossRef] [PubMed]
- Rekimoto, J. Gesturewrist and gesturepad: Unobtrusive wearable interaction devices. In Proceedings of the Fifth International Symposium on Wearable Computers, Zurich, Switzerland, 8–9 October 2001; pp. 21–27. [Google Scholar]
- Ashbrook, D.; Baudisch, P.; White, S. Nenya: Subtle and eyes-free mobile input with a magnetically-tracked finger ring. In Proceedings of the SIGCHI Conference on Human Factors in Computing Systems, Vancouver, BC, Canada, 7–12 May 2011; pp. 2043–2046. [Google Scholar]
- Pantelopoulos, A.; Bourbakis, N. A survey on wearable biosensor systems for health monitoring. In Proceedings of the 30th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBS 2008), Vancouver, BC, Canada, 20–25 August 2008; pp. 4887–4890. [Google Scholar]
- Halín, N.; Junnila, M.; Loula, P.; Aarnio, P. The LifeShirt system for wireless patient monitoring in the operating room. J. Telemed. Telecare 2005, 11 (Suppl. 2), 41–43. [Google Scholar] [CrossRef] [PubMed]
- Ranck, J. The Wearable Computing Market: A Global Analysis; Gigaom Pro.: Austin, TX, USA, 2012. [Google Scholar]
- Zheng, J.; Shen, Y.; Zhang, Z.; Wu, T.; Zhang, G.; Lu, H. Emerging wearable medical devices towards personalized healthcare. In Proceedings of the 8th International Conference on Body Area Networks, Boston, MA, USA, 30 September–2 October 2013; ICST (Institute for Computer Sciences, Social-Informatics and Telecommunications Engineering): Brussels, Belgium, 2003; pp. 427–431. [Google Scholar]
- Anliker, U.; Ward, J.; Lukowicz, P.; Tröster, G.; Dolveck, F.; Baer, M.; Keita, F.; Schenker, E.B.; Catarsi, F.; Coluccini, L.; et al. AMON: A wearable multiparameter medical monitoring and alert system. IEEE Trans. Inf. Technol. Biomed. 2004, 8, 415–427. [Google Scholar] [CrossRef] [PubMed]
- Coyle, S.; Lau, K.T.; Moyna, N.; Gorman, D.O.; Diamond, D.; Di Francesco, F.; Costanzo, D.; Salvo, P.; Trivella, M.G.; De Rossi, D.E.; et al. BIOTEX—Biosensing textiles for personalised healthcare management. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 364–370. [Google Scholar] [CrossRef] [PubMed]
- Lymberis, A. Wearable Ehealth Systems for Personalised Health Management: State of the Art and Future Challenges; IOS Press: Amsterdam, The Netherlands, 2004. [Google Scholar]
- Noorzaie, I. Survey Paper: Medical Applications of Wireless Networks. Available online: http://t.cn/RgjStFP (accessed on 19 July 2018).
- Cunha, J.P.S.; Cunha, B.; Pereira, A.S.; Xavier, W.; Ferreira, N.; Meireles, L. Vital-Jacket®: A wearable wireless vital signs monitor for patients’ mobility in cardiology and sports. In Proceedings of the 2010 4th International Conference on Pervasive Computing Technologies for Healthcare (PervasiveHealth), Munich, Germany, 22–25 March 2010; pp. 1–2. [Google Scholar]
- Blobel, B.; Sauermann, S.; Mense, A. PHealth 2014: Proceedings of the 11th International Conference on Wearable Micro and Nano Technologies for Personalized Health, Vienna, Austria, 11–13 June 2014; IOS Press: Amsterdam, The Netherlands, 2014; Volume 200. [Google Scholar]
- Nijholt, A.; Tan, D.F. Brain-computer interfacing for intelligent systems. IEEE Intell. Syst. 2008, 23, 72–79. [Google Scholar] [CrossRef]
- Annicchiarico, R.; Cortés, U. To share or not to share share-it: Lessons learnt. In Electronic Healthcare; Springer: Berlin/Heidelberg, Germany, 2012; pp. 295–302. [Google Scholar]
- Annicchiarico, R.; Barrué, C.; Benedico, T.; Campana, F.; Cortés, U.; Martínez-Velasco, A. The i-Walker: An intelligent pedestrian mobility aid. In Proceedings of the 18th European Conference on Artificial Intelligence (ECAI 2008), Patras, Greece, 21–25 August 2008; pp. 708–712. [Google Scholar]
- Virk, G.S. CLAWAR to service robots. In Proceedings of the 17th International Conference on Climbing and Walking Robots (CLAWAR), Poznan, Poland, 21–23 July 2014; pp. 40–41. [Google Scholar]
- Matthews, J.T. The Nursebot Project: Developing a personal robotic assistant for frail older adults in the community. Home Health Care Manag. Pract. 2002, 14, 403–405. [Google Scholar] [CrossRef]
- Díaz, U.; Laskibar, I.; Badiyani, S.; Raja, H.; Buiza, C.; Raja, V. Preferences of Healthcare Staff in the Way of Interacting with Robots Depending on Their Prior Knowledge of ICTs: Findings from Iward Project. In Ambient Assistive Health and Wellness Management in the Heart of the City; Springer: Berlin/Heidelberg, Germany, 2009; pp. 282–285. [Google Scholar]
- Wada, K.; Shibata, T.; Saito, T.; Sakamoto, K.; Tanie, K. Psychological and social effects of one year robot assisted activity on elderly people at a health service facility for the aged. In Proceedings of the 2005 IEEE International Conference on Robotics and Automation (ICRA 2005), Barcelona, Spain, 18–22 April 2005; pp. 2785–2790. [Google Scholar]
- Dautenhahn, K.; Woods, S.; Kaouri, C.; Walters, M.L.; Koay, K.L.; Werry, I. What is a robot companion-friend, assistant or butler? In Proceedings of the 2005 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS 2005), Edmonton, AL, Canada, 2–6 August 2005; pp. 1192–1197. [Google Scholar]
- Broekens, J.; Heerink, M.; Rosendal, H. Assistive social robots in elderly care: A review. Gerontechnology 2009, 8, 94–103. [Google Scholar] [CrossRef]
- Simmons, R.; Apfelbaum, D. A task description language for robot control. In Proceedings of the 1998 IEEE/RSJ International Conference on Intelligent Robots and Systems, Victoria, BC, Canada, 17 October 1998; Volume 3, pp. 1931–1937. [Google Scholar]
- Sugano, S.; Shirai, Y.; Chae, S. Environment Design for Human-Robot Symbiosis-Introduction of WABOT-HOUSE Project. In Proceedings of the 23rd International Symposium on Automation and Robotics in Construction, Tokyo, Japan, 3–5 October 2006; pp. 152–157. [Google Scholar]
- Fan, Z.; King, C.H.; Darb, H.; Kemp, C.C. Dusty: A Teleoperated Assistive Mobile Manipulator That Retrieves Objects From the Floor; Georgia Institute of Technology: Atlanta, GA, USA, 2010. [Google Scholar]
- Pollack, M.E.; Brown, L.; Colbry, D.; McCarthy, C.E.; Orosz, C.; Peintner, B.; Ramakrishnan, S.; Tsamardinos, I. Autominder: An intelligent cognitive orthotic system for people with memory impairment. Robot. Auton. Syst. 2003, 44, 273–282. [Google Scholar] [CrossRef]
- Mayer, P.; Beck, C.; Panek, P. Examples of multimodal user interfaces for socially assistive robots in Ambient Assisted Living environments. In Proceedings of the 2012 IEEE 3rd International Conference on Cognitive Infocommunications (CogInfoCom), Kosice, Slovakia, 2–5 December 2012; pp. 401–406. [Google Scholar]
- Modayil, J.; Levinson, R.; Harman, C.; Halper, D.; Kautz, H.A. Integrating Sensing and Cueing for More Effective Activity Reminders. In Proceedings of the AAAI Fall Symposium: AI in Eldercare: New Solutions to Old Problems, Arlington, VA, USA, 7–9 November 2008; pp. 60–66. [Google Scholar]
- Liao, L.; Chen, M.; Rodrigues, J.J.; Lai, X.; Vuong, S. A novel web-enabled healthcare solution on healthvault system. J. Med. Syst. 2012, 36, 1095–1105. [Google Scholar] [CrossRef] [PubMed]
- Sunyaev, A.; Chornyi, D.; Mauro, C.; Krcmar, H. Evaluation framework for personal health records: Microsoft HealthVault vs. Google Health. In Proceedings of the 2010 43rd Hawaii International Conference on System Sciences (HICSS), Honolulu, HI, USA, 5–8 January 2010; pp. 1–10. [Google Scholar]
- Morrison, K.; Szymkowiak, A.; Gregor, P. Memojog—An interactive memory aid incorporating mobile based technologies. In Proceedings of the Mobile Human-Computer Interaction-MobileHCI 2004, Glasgow, UK, 13–16 September 2004; Springer: Berlin/Heidelberg, Germany, 2004; pp. 481–485. [Google Scholar]
- Man Bok, H.; Sin Jung, K.; Um, T.; Keehoon, K. KULEX: An ADL power-assistance demonstration. In Proceedings of the 10th International Conference on Ubiquitous Robots and Ambient Intelligence (URAI), Jeju, Korea, 30 October–2 November 2013; pp. 542–544. [Google Scholar]
- Kumata, A.; Tsuda, Y.; Suzuki, H.; Ra, E.; Morishita, T. Advanced community model using daily life information transmitter for supporting welfare workers and senior citizens living alone in a welfare society. In Proceedings of the 2011 8th International Conference on Ubiquitous Robots and Ambient Intelligence (URAI 2011), Incheon, Korea, 23–26 November 2011; pp. 414–417. [Google Scholar]
- Granata, C.; Chetouani, M.; Tapus, A.; Bidaud, P.; Dupourqué, V. Voice and graphical based interfaces for interaction with a robot dedicated to elderly and people with cognitive disorders. In Proceedings of the 19th International Symposium in Robot and Human Interactive Communication, Viareggio, Italy, 13–15 September 2010. [Google Scholar]
- Álvarez-García, J.A.; Barsocchi, P.; Chessa, S.; Salvi, D. Evaluation of localization and activity recognition systems for ambient assisted living: The experience of the 2012 EvAAL competition. J. Ambient Intell. Smart Environ. 2013, 5, 119–132. [Google Scholar]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Byrne, C.A.; Collier, R.; O’Hare, G.M.P. A Review and Classification of Assisted Living Systems. Information 2018, 9, 182. https://doi.org/10.3390/info9070182
Byrne CA, Collier R, O’Hare GMP. A Review and Classification of Assisted Living Systems. Information. 2018; 9(7):182. https://doi.org/10.3390/info9070182
Chicago/Turabian StyleByrne, Caroline A., Rem Collier, and Gregory M. P. O’Hare. 2018. "A Review and Classification of Assisted Living Systems" Information 9, no. 7: 182. https://doi.org/10.3390/info9070182
APA StyleByrne, C. A., Collier, R., & O’Hare, G. M. P. (2018). A Review and Classification of Assisted Living Systems. Information, 9(7), 182. https://doi.org/10.3390/info9070182





