Protocol for a Cluster Randomised Controlled Trial to Compare the “Taste & See” Programme—A Church-Based Programme to Develop a Healthy Relationship with Food—With a Wait-List Control
Abstract
1. Introduction
2. Aim
3. Objectives
- To compare change in emotional eating and changes in other measures of psychological, spiritual and physical well-being, between those attending the “Taste & See” programme and those randomised to the wait list control, at the end of intervention;
- To investigate ongoing change in these variables at 6 months and 2 years;
- To assess the mediating associations between each of these variables and how well they fit the theoretical model that underpins intervention;
- To assess participant and facilitators acceptability of taking part in and facilitating the trial programme.
4. Methods
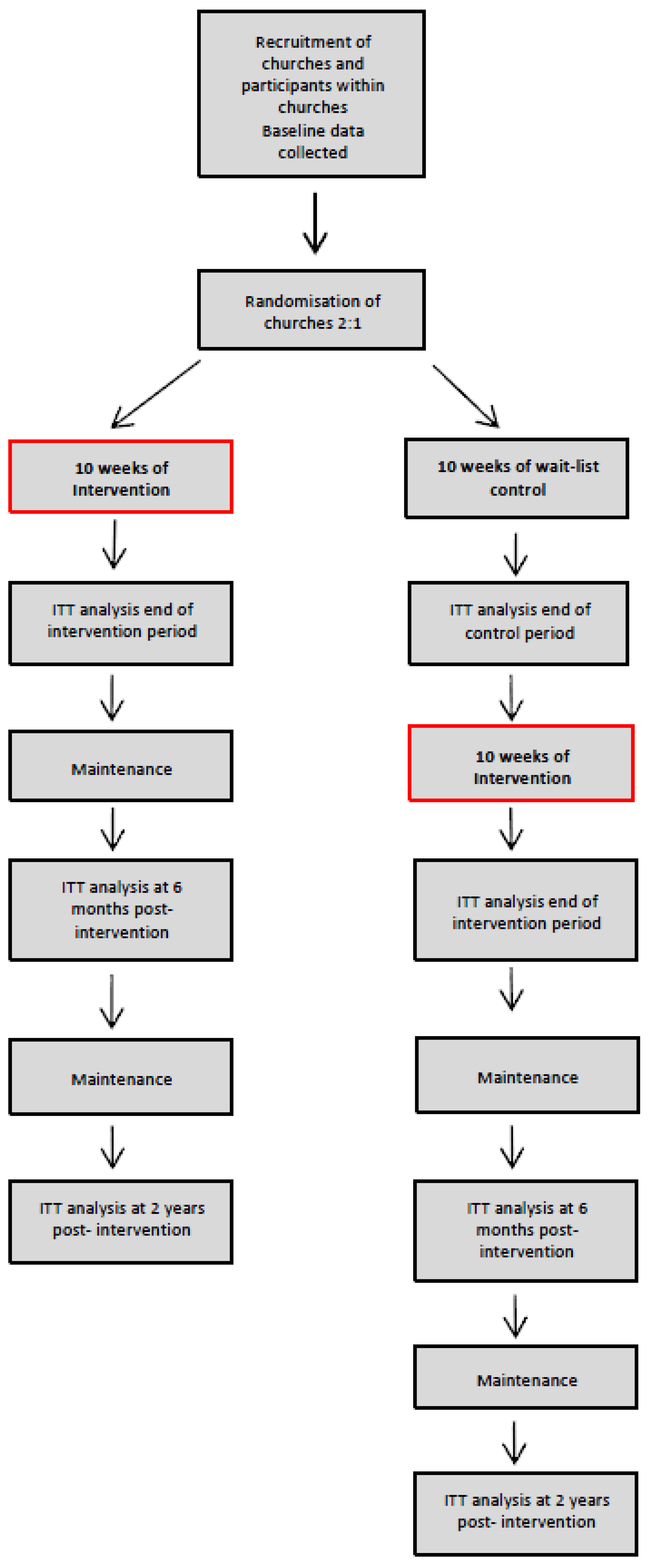
4.1. Study Design
4.2. Ethics
4.3. Participants
4.3.1. Inclusion Criteria
4.3.2. Exclusion Criteria
4.4. Study Setting and Recruitment
- Decide on a weekly time to run the course, prepare two potential start dates: one to start as soon as interested participants have registered and the other scheduled to start 10 weeks later.
- Advertise the programme in their church and local community. They will find on the website: a poster to print off insert local details and display, a 1 min advert about Taste and See and a 5 min trailer to give people more a feel for the programme.
- Facilitators refer interested people to the website to read the participant information. Interested people give the facilitator their email or postal address & permission to share these details with the researchers.
- The facilitator registers their church by completing the online registration form, confirming they have understood and agree to under-taking this role. They then insert the emails of all those who would like to do the programme.
4.5. Randomisation
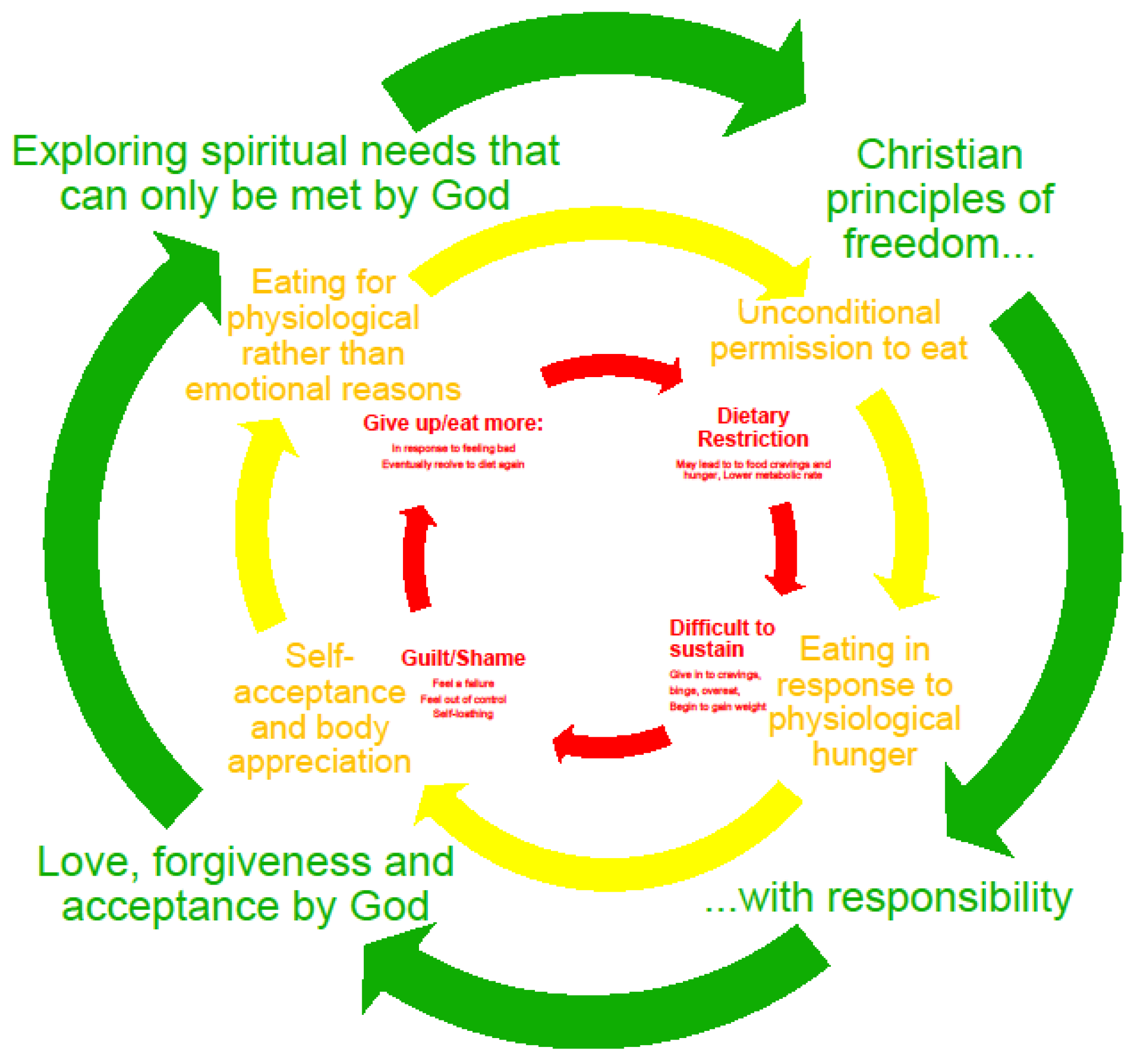
4.6. Intervention Programme
- The “Taste & See” DVD which containing a series of 10 sessions. The DVD presents both a scientific and a Christian viewpoint to the topics. The course is written by Deborah Lycett RD PhD (Reader in nutrition, dietetics and spiritual health); with Christian input from church members who have also been Taste & See facilitators (Rebekah Hodson, Elaine Davis) and this content has been checked for theological accuracy to ecumenical Christian concepts by church ministers. Healthy eating tips are presented by Nicky Walker RD. Personal stories from those who have done the programme and offered to be filmed are also included in the DVD.
- The “Taste & See” Participant’s Manual, this is a workbook which accompanies the “Taste & See” DVD so participants can document their reflections, their goals and the group discussions that take place each week. There are discussion prompts on the DVD so that issues raised can be discussed in small groups.
- The “Taste & See” Bible Meditations, this is a booklet of readings for daily inspiration throughout the programme.
- The “Taste & See” Facilitator’s Manual, this is an instruction booklet for facilitators with a step by step guide on how to run the programme locally. It describes the course ethos and contains instructions on facilitating groups effectively, creating an emotionally safe and confidential group environment and when to refer people on to health professionals.
4.7. Control Programme
4.8. Primary Outcome
4.9. Secondary Outcomes
4.10. Process Outcomes
4.11. Outcome Measures
4.12. Sample Size
4.13. Data Analysis
5. Implication of Results
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ashfield-Watt, P. A. L., A. A. Welch, S. Godward, and S. A. Bingham. 2007. Effect of a pilot community intervention on fruit and vegetable intakes: Use of FACET (Five-a-day Community Evaluation Tool). Public Health Nutrition 10: 671–80. [Google Scholar] [CrossRef] [PubMed]
- Beck, R., and A. McDonald. 2004. Attachment to God: The attachment to God inventory, tests of working model. Journal of Psychology and Theology 32: 92–103. [Google Scholar] [CrossRef]
- Butler, G. S., T. M. Vallis, B. Perey, S. J. O. Veldhuyzen van Zanten, S. MacDonald, and G. Konok. 1999. The Obesity Adjustment Survey: Development of a scale to assess psychological adjustment to morbid obesity. International Journal of Obesity and Related Metabolic Disorders 23: 505–11. [Google Scholar] [CrossRef] [PubMed]
- Campbell, M. K., D. R. Elbourne, and D. G. Altman. 2004. CONSORT statement: Extension to cluster randomised trials. British Medical Journal 328: 702–8. [Google Scholar] [CrossRef] [PubMed]
- Conradt, M., J. M. Dierk, P. Schlumberger, E. Rauh, J. Hebebrand, and W. Rief. 2007. Development of the Weight-and Body-Related Shame and Guilt Scale (WEB–SG) in a nonclinical sample of obese individuals. Journal of Personality Assessment 88: 317–27. [Google Scholar] [CrossRef] [PubMed]
- Fiala, W. E., J. P. Bjorck, and R. Gorsuch. 2002. The religious social support scale: Construction, validation, and cross-validation. American Journal of Community Psychology 30: 761–86. [Google Scholar] [CrossRef] [PubMed]
- Frühbeck, G., and V. Yumuk. 2014. Obesity: A Gateway Disease with a Rising Prevalence. Obesity Facts 7: 33–36. [Google Scholar] [CrossRef] [PubMed]
- Hawks, S. R., M. B. Goudy, and J. A. Gast. 2003. Emotional Eating and Spiritual Well-being: A Possible Connection? American Journal of Health Education 34: 30–33. [Google Scholar] [CrossRef]
- Heinberg, L. J., and J. K. Thompson. 1995. Body image and televised images of thinness and attractiveness: A controlled laboratory investigation. Journal of Social and Clinical Psychology 14: 325–88. [Google Scholar] [CrossRef]
- Herdman, M., C. Gudex, A. Lloyd, B. Janssen, P. Kind, D. Parkin, G. Bonsel, and X. Badia. 2011. Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Quality of Life Research 20: 1727–36. [Google Scholar] [CrossRef] [PubMed]
- Homan, K. 2012. Attachment to God mitigates negative effect of media exposure on women’s body image. Psychology of Religion and Spirituality 4: 324–31. [Google Scholar] [CrossRef]
- Homan, K. J., and C. J. Boyatzis. 2010. The Protective Role of Attachment to God against Eating Disorder Risk Factors: Concurrent and Prospective Evidence. Eating Disorders 18: 239–58. [Google Scholar] [CrossRef] [PubMed]
- Huber, S., and O.W. Huber. 2012. The Centrality of Religiosity Scale (CRS). Religions 3: 710–24. [Google Scholar] [CrossRef]
- Karlsson, J., L. O. Persson, L. Sjostrom, and M. Sullivan. 2000. Psychometric properties and factor structure of the Three-Factor Eating Questionnaire (TFEQ) in obese men and women. Results from the Swedish Obese Subjects. International Journal of Obesity Related Metabolic Disorder 24: 1715–25. [Google Scholar] [CrossRef]
- Koenig, H. G. 2009. Research on religion, spirituality, and mental health: A review. Canadian Journal of Psychiatry 54: 283–91. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K., and R. L. Spitzer. 2002. The PHQ-9: A new depression diagnostic and severity measure. Psychiatric Annals 32: 509–21. [Google Scholar] [CrossRef]
- Luppino, F. S., L. M. de Wit, P. F. Bouvy, T. Stijnen, P. Cuijpers, B. W. J. H. Penninx, and F. G. Zitman. 2010. Overweight, obesity, and depression: A systematic review and meta-analysis of longitudinal studies. Archives of General Psychiatry 67: 220–29. [Google Scholar] [CrossRef] [PubMed]
- Lycett, D., R. Patel, A. Coufopoulos, and A. Turner. 2016. Protocol of Taste and See: A Feasibility Study of a Church-Based, Healthy, Intuitive Eating Programme. Religions 7: 41. [Google Scholar] [CrossRef]
- Michie, S., M. Richardson, M. Johnston, C. Abraham, J. Francis, W. Hardeman, M. P. Eccles, J. Cane, and C. E. Wood. 2013. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: Building an international consensus for the reporting of behavior change interventions. Annals of Behavioral Medicine 46: 81–95. [Google Scholar] [CrossRef] [PubMed]
- Pargament, K., M. Feuille, and D. Burdzy. 2011. The brief RCOPE: Current psychometric status of a short measure of religious coping. Religions 2: 51–76. [Google Scholar] [CrossRef]
- Patel, R., D. Lycett, A. Coufopoulos, and A. Turner. 2017a. A Feasibility Study of Taste & See: A Church Based Programme to Develop a Healthy Relationship with Food. Religions 8: 29. [Google Scholar] [CrossRef]
- Patel, R., D. Lycett, A. Coufopoulos, and A. Turner. 2017b. Moving Forward in Their Journey: Participants’ Experience of Taste & See, A Church-Based Programme to Develop a Healthy Relationship with Food. Religions 8: 14. [Google Scholar] [CrossRef]
- Preacher, K. J., M. J. Zyphur, and Z. Zhang. 2010. A general multilevel SEM framework for assessing multilevel mediation. Psychological Methods 15: 209–33. [Google Scholar] [CrossRef] [PubMed]
- Puhl, R. M., and C. A. Heuer. 2009. The stigma of obesity: A review and update. Obesity 17: 941–64. [Google Scholar] [CrossRef] [PubMed]
- Rowatt, W. C., and L. A. Kirkpatrick. 2002. Two Dimensions of Attachment to God and Their Relation to Affect, Religiosity, and Personality Constructs. Journal for the Scientific Study of Religion 41: 637–51. [Google Scholar] [CrossRef]
- Sekhon, M., M. Cartwright, and J. Francis. 2017. Acceptability of healthcare interventions: An overview of reviews and development of a theoretical framework. BMC Health Services Research 17: 88. [Google Scholar] [CrossRef] [PubMed]
- Spitzer, R. L., K. Kroenke, J. B. W. Williams, and B. Löwe. 2006. A brief measure for assessing generalized anxiety disorder: The GAD-7. Archives of Internal Medicine 166: 1092–97. [Google Scholar] [CrossRef] [PubMed]
- Stroebe, W., G. M. van Koningsbruggen, E. K. Papies, and H. Aarts. 2013. Why most Dieters Fail but some Succeed: A Goal Conflict Model of Eating Behavior. Psychological Review 120: 110–38. [Google Scholar] [CrossRef] [PubMed]
- Tennant, R., L. Hiller, R. Fishwick, S. Platt, S. Joseph, S. Weich, and S. Stewart-Brown. 2007. The Warwick-Edinburgh mental well-being scale (WEMWBS): Development and UK validation. Health and Quality of Life Outcomes 5: 63–73. [Google Scholar] [CrossRef] [PubMed]
- Thompson, D. M., D. H. Fernald, and J. W. Mold. 2012. Intraclass correlation coefficients typical of cluster-randomized studies: Estimates from the Robert Wood Johnson Prescription for Health projects. The Annals of Family Medicine 10: 235–40. [Google Scholar] [CrossRef] [PubMed]
- Tylka, T. L., and A. M. Kroon van Diest. 2013. The Intuitive Eating Scale—2: Item Refinement and Psychometric Evaluation with College Women and Men. Journal of Counseling Psychology 60: 137–53. [Google Scholar] [CrossRef] [PubMed]
- Underwood, L. 2011. The Daily Spiritual Experience Scale: Overview and Results. Religions 2: 29–50. [Google Scholar] [CrossRef]
- Wareham, N. J., R. W. Jakes, K. L. Rennie, J. Schuit, and J. Mitchell. 2003. Validity and repeatability of a simple index derived from the short physical activity questionnaire used in the European Prospective Investigation into Cancer and Nutrition (EPIC) study. Public Health Nutrition 6: 407–13. [Google Scholar] [CrossRef] [PubMed]
- Wood, B., E. Worthington, Jr., J. Exline, A. Yali, J. Aten, and M. McMinn. 2010. Development, refinement, and psychometric properties of the Attitudes toward God Scale (ATGS-9). Psychology of Religion and Spirituality 2: 1–29. [Google Scholar] [CrossRef]
© 2018 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lycett, D. Protocol for a Cluster Randomised Controlled Trial to Compare the “Taste & See” Programme—A Church-Based Programme to Develop a Healthy Relationship with Food—With a Wait-List Control. Religions 2018, 9, 88. https://doi.org/10.3390/rel9030088
Lycett D. Protocol for a Cluster Randomised Controlled Trial to Compare the “Taste & See” Programme—A Church-Based Programme to Develop a Healthy Relationship with Food—With a Wait-List Control. Religions. 2018; 9(3):88. https://doi.org/10.3390/rel9030088
Chicago/Turabian StyleLycett, Deborah. 2018. "Protocol for a Cluster Randomised Controlled Trial to Compare the “Taste & See” Programme—A Church-Based Programme to Develop a Healthy Relationship with Food—With a Wait-List Control" Religions 9, no. 3: 88. https://doi.org/10.3390/rel9030088
APA StyleLycett, D. (2018). Protocol for a Cluster Randomised Controlled Trial to Compare the “Taste & See” Programme—A Church-Based Programme to Develop a Healthy Relationship with Food—With a Wait-List Control. Religions, 9(3), 88. https://doi.org/10.3390/rel9030088




