New Zealand Nurses’ Perceptions of Spirituality and Spiritual care: Qualitative Findings from a National Survey
Abstract
:1. Introduction
2. Background
2.1. The Present Study
2.2. Research Questions
- What do NZ nurses understand by the terms spirituality and spiritual care?
- Do NZ nurses consider spirituality to be a legitimate area of nursing practice?
- Do NZ nurses believe that they receive sufficient support, guidance and training in spiritual matters?
3. Methods
3.1. Participants
3.2. Measures
3.3. Procedures and Data Analysis
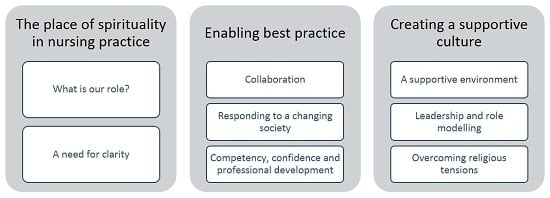
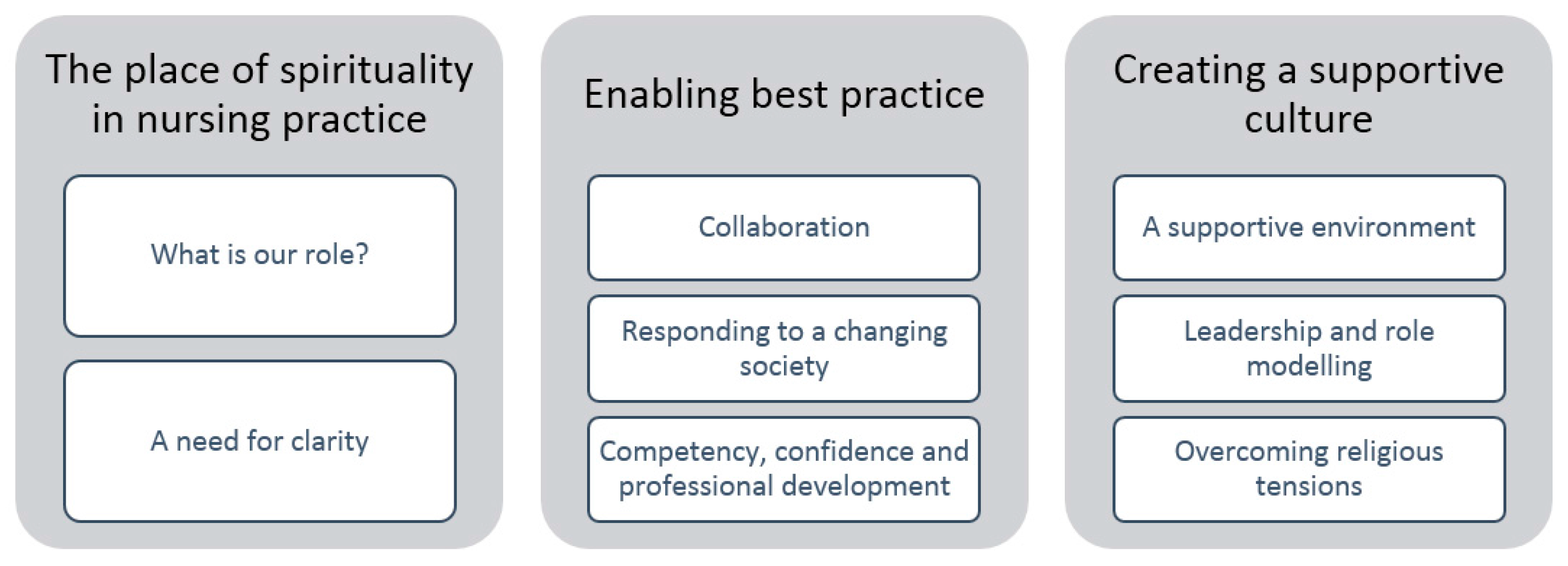
4. Results
4.1. The Place of Spirituality in Nursing Practice.
4.1.1. What is Our Role?
In this way, spiritual care formed part of an interpersonal connection that sat within professional boundaries and expectations.Identifying and addressing spiritual needs with clients/service users starts with the therapeutic relationship which in itself it a spiritual passage—the development of whakawhanaungatanga or connection between two human beings at the start of a journey of change and enlightenment. The quality of this relationship will either aid or disable the journey. Hope is another essential spiritual aspect of nursing care which again is tied to the relationship and the vision of what could be achieved together. All in all nurses are provided a beautiful opportunity to spiritually experience the many journeys of the people we are privileged to work alongside. Female, mental health (community) NZ European.
The potentially complicated connection of spirituality and spiritual care with mental health patients was frequently mentioned:Where I work there exists a paucity of guidance around spirituality as mental health consumers can experience religious delusions resulting in an avoidance of the subject of spiritual beliefs altogether…The role of nurse is also considered neutral position therefore the nurse is strongly advised not to divulge his or her own beliefs. I remain uncertain whether this is a good thing or not? Female, mental health (inpatients), NZ European.
The relevance of spirituality and spiritual care to settings in which its provision is more challenging was doubted or challenged by some. One participant noted that “As a theatre nurse I have very limited contact with awake patients, so spirituality does not seem to be an issue in my area”. Female, perioperative care (theatre), NZ European.I remain uncertain as to what the role of the nurse is in relation to the mental health consumer and their spirituality. I have witnessed both disaster and comfort when nurses have been of the same faith as the consumer and worshipped with them. Female, mental health (inpatients), NZ European.But living well with mental illness is very possible when spiritual care is taken seriously by client and team care members...utilising a recovery approach usually involves looking at spiritual care. Female, mental health (community) NZ European.
Others were less affirmative of the spiritual care expectations placed on nurses due to the amorphous nature of spirituality and spiritual needs:Spirituality shapes, divides, draws close, separates individuals. It is part of the needs of an individual just as food is…It could be the difference in some people surviving or not surviving from illness therefore must be regarded as essential and on the spectrum of care. Female, no longer practicing, NZ European.
Some participants demonstrated hesitancy due to expectations that the presentation of spiritual needs will increasingly decline considering the current trend of waning religious identification in the NZ population. Nonetheless, various participants commented on the important distinction between the initiation of spiritual care and taking entire responsibility for a patients’ spiritual needs—only the former being the role of a nurse.There are so many levels of spiritual care and I don’t think nurses should be responsible for performing it themselves. Guidance in how to get appropriate help and the time/resources to do so should be part of our training and orientation to workplaces. Female, perioperative care (theatre), NZ European.
Participants’ comments suggest patients may not always be able to identify or articulate their own needs, however this does not mean spiritual needs are not present.Sometimes it is difficult for [patients to] identify own needs—nurses role is always to instil hope and help find meaning. Female, nursing professional advice/policy, South African.I have been a registered nurse for 40 years, and have always had an awareness of spiritual care, but it has only been in the last 10 years that I have seen the importance [of spirituality] to the person and their family/whanau as this completes them as a whole person. Often they are unaware of this need, but if they feel accepted, and treated with respect and feel listened to and understood, this is spiritual care. Female, practice nursing [recently retired], NZ European.
4.1.2. A need for Clarity
From these comments, it appears that what some nurses regard as spiritual care, others see as the provision of standard compassionate care. For the latter individuals, spiritual care appears to extend to the realm of referring to other professionals, for example religious counselling. Some nurses specifically commented on the deleterious impact of confusion between religiosity and spirituality: “Generally I don’t think [spirituality] is taken seriously by many and many mistake it with religion, which may not have anything to do with individual’s needs” (Female, primary health care, NZ European).I do not think it is the responsibility of the nurse to meet a patient’s spiritual needs outside of the kind and caring environment. I think we need to be made aware then refer to someone appropriate. Female, intensive care/cardiac care (midwife/RN), NZ European.
These comments reveal the broad spectrum of opinions concerning the term spirituality, thus highlighting the sensitive nature of the concept. Consequently, professional expectations around these terms are not well defined or articulated. As such, there is a need for common understanding of what spirituality entails to help navigate the multitude of individual perspectives on what are often highly personal issues while considering that achieving consensus or arriving at an authoritative definition may not be practical or appropriate.One of the challenges we have is the language. If we discuss religion, whatever that might mean for people, there is a common understanding, there is a religious vocab[ulary]. There is no spiritual vocab that has a shared understanding and to use religious vocab in this context can be a VERY problematic and inappropriate. It is a concept that only gets lip service on patient assessment sheets by way of tick box! Female, palliative care, NZ European.Most people in NZ are secular and non-religious and the concept of spirituality has been somewhat hijacked to cover a whole range of normal human emotions and the responses a nurse might have to them. Female, child health including neonatology, NZ European.
4.2. ‘Enabling Best Practice’
4.2.1. Collaboration
I think it would be quite nice to work more with churches and spiritual groups in the community in getting their help with some of our patients… Spiritual groups are often not connected with the healthcare system. It would be better if they were. Female, nursing administration and management, Other European.
The establishment of working relationships with community-based spiritual and religious groups would specifically assist in the continuity of care post-discharge, where there was a perceived gap in the ability of patients to access resources and services once back in the community.Make it easier for health professionals to access a list of different spiritual support systems to assist all patients with “religious and non-religious beliefs.” Female, nursing administration and management, NZ European.
To improve the efficacy of a team-based approach, some participants suggested that spiritual needs be more openly discussed during MDT meetings, and that a member of the team take on the role of ‘spiritual care champion’ and guide others in the provision of best practice spiritual care.Time is a huge challenge and probably the most important element to being able to connect with a person where we can begin to discover their spiritual needs. One person alone can never provide this. Team! Female, continuing care (elderly), NZ EuropeanSocial work is one paid service that we actually have that is quite important to us and would be beneficial to have 24/7. People don’t necessarily identify that they have a spiritual need, but they have it! They have a need and the social worker is an interdenominational multi-cultural touch-point. They are really undervalued in our health system for providing that. Female, emergency and trauma, NZ European.
4.2.2. Responding to a Changing Society
With the ever growing Indian community, and their beliefs of Hindu, Sikh, Christian, it would be helpful to be familiar with these beliefs so as to ensure their safety as well as for the nurses. Female, public health, NZ European.It would be useful to have practical values included e.g. is it considered disrespectful to look in the eye when talking to this group of people? Female, perioperative care (theatre), NZ European.
4.2.3. Competency, Confidence and Professional Development
Whilst not all participants thought spiritual care could be taught, they believed that a respect for it and awareness of how spiritual needs may manifest could be. The above comments also point to the significant contribution of institutional support to the ability of spiritually-inclined nurses to provide effective spiritual care.Nurses need to know their spiritual beliefs, before they can educate other nurses, or aid patients. Not all staff able or willing to give spiritual support. Choice of individual. Female, continuing care (elderly), NZ European.Nurses are beautifully positioned to provide practical, effective spiritual care intervention and support...It does, however, depend upon organizational support, resource allocation and a requirement for maturity and insight on the part of the practitioner which is a lifetime journey. Male, nursing education, NZ European, Māori.
That this short survey induced re-evaluations of some nurses’ scope of practice suggests a short and affordable nursing workforce intervention may be efficacious.I will discuss having a spiritual care policy within our general practice as this is something that has never been discussed. Female, practice nursing, NZ EuropeanWow, this made me reflect on my practice. This is something I don’t really address—I’ve always just thought that referring to the chaplain was all that I could do. I had never thought that by listening to the patient and providing guidance I’m providing spiritual care. Female, surgical, NZ European.
These comments indicate the need for clarification that the goals of spiritual care education, policies and competencies ought not to impose the provision of spiritual care on nurses.I would not like to see spirituality put ‘in a box’ with guidelines and policies from any of our governing bodies. If this happens we run the risk of missing out a lot of people. Female, assessment and rehabilitation, NZ European.I believe that some nurses don’t feel they want to be involved in the spiritual elements of nursing—I don’t think these nurses should be forced to do this as more damage than good could be done for both the patient and the nurse. Female, medical, NZ European.
4.3. ‘Creating a Supportive Culture’
4.3.1. A Supportive Environment
Reduce the nurse workload so we have the time to sit with our patients and can listen to their needs. Allow a private quiet place on each ward where people can sit and reflect on what is happening to them. Female, surgical, NZ European.As ward tasks like washing have been delegated to healthcare assistants, the nurses no longer gain the opportunity to have quiet, private moments in which to address spiritual needs. Female, intensive care/cardiac care, Other European.
4.3.2. Leadership and Role Modelling
4.3.3. Overcoming Religious Tensions
Others felt that particular religions were favoured more than others:People are too scared to show any religious or spiritual leaning. It is frowned upon. Religion is also unpopular, not in vogue. You are thought of as weird. You have to be very careful to express or show spirituality, which is a sad reflection on society. Female, assessment and rehabilitation, Other European.
In my work place there is a tendency to strong Christian beliefs and sometimes this is pushed a bit much onto some patients. Other religions and beliefs are not always accommodated very well by some staff. Female, palliative care, NZ European.I have always felt comfortable praying with my patients when I was in clinical practice and I saw many times that it was a help to both the patient and myself. I don’t think that Christian nurses feel they have the freedom to do this with their patients and that is such a shame. Female, nursing education, NZ European.
5. Discussion
- Whether cultivating a common understanding of spirituality can be achieved;
- Attending to the needs of a traditionally secular, but increasingly multi-faith and multi-ethnic, society; and,
- Creating the conditions for a spiritually supportive environment for staff and patients.
5.1. Cultivating a Common Understanding of Spirituality.
5.2. A Secular, but Spiritual Society with Numerous Needs
5.3. Supporting Staff and Patients
5.4. Strengths and Limitations
- Providing baseline information to inform pre/post clinical training, current nursing practice, and policy development;
- Highlighting priority areas for future research;
- Establishing a baseline of evidence regarding nurses’ views and practice of spirituality and spiritual care, enabling changes to be tracked over time.
6. Conclusions
7. Relevance to Clinical Practice
Acknowledgements
Author Contributions
Conflicts of Interest
References
- Abbasi, Mojgan, Marhamat Farahani-Nia, Neda Mehrdad, Azam givari, and Hamid Haghani. 2014. Nursing students’ spiritual well-being, spirituality and spiritual care. Iranian Journal of Nursing and Midwifery Research 19: 242–47. [Google Scholar] [PubMed]
- Adib-Hajbaghery, Mohsen, and Samira Zehtabchi. 2016. Developing and Validating an Instrument to Assess the Nurses’ Professional Competence in Spiritual Care. The Journal of Nursing Measurement 24: 15–27. [Google Scholar] [CrossRef] [PubMed]
- An Bord Altranais. 2009. Requirements and Standards for Nurse Registration Education Programs. Dublin: An Bord Altranais. [Google Scholar]
- Austin, Philip Daniel, Roderick Macleod, Philip John Siddall, Wilfred McSherry, and Richard Egan. 2016. The Ability of Hospital Staff to Recognise and Meet Patients’ Spiritual Needs: A Pilot Study. Journal for the Study of Spirituality 6: 20–37. [Google Scholar] [CrossRef]
- Baldacchino, Donia R. 2006. Nursing competencies for spiritual care. Journal of Clinical Nursing 15: 885–96. [Google Scholar] [CrossRef] [PubMed]
- Baldacchino, Donia R. 2008. Teaching on the spiritual dimension in care to undergraduate nursing students: The content and teaching methods. Nurse Education Today 28: 550–62. [Google Scholar] [CrossRef] [PubMed]
- Baldacchino, Donia R. 2011. Teaching on spiritual care: The perceived impact on qualified nurses. Nurse Education in Practice 11: 47–53. [Google Scholar] [CrossRef] [PubMed]
- Biro, Anne L. 2012. Creating conditions for good nursing by attending to the spiritual. Journal of Nursing Management 20: 1002–11. [Google Scholar] [CrossRef] [PubMed]
- Bradshaw, Ann. 1994. Lighting the Lamp: The Spiritual Dimension of Nursing Care. Harrow: Scutari Press. [Google Scholar]
- Braun, Virginia, and Victoria Clarke. 2006. Using thematic analysis in psychology. Qualitative Research in Psychology 3: 77–101. [Google Scholar] [CrossRef]
- Burnard, Philip. 1998. The last two taboos in community nursing. Journal of Community Nursing 12: 4–6. [Google Scholar]
- Central Cancer Network. 2015. He Anga Whakaahuru Supportive Care Framework. Palmerston North: Central Cancer Network. [Google Scholar]
- Chan, Cecilia L. W., S. M. Ng, Rainbow T. H. Ho, and Amy Y. M. Chow. 2006a. East meets West: applying Eastern spirituality in clinical practice. Journal of Clinical Nursing 15: 822–32. [Google Scholar] [CrossRef] [PubMed]
- Chan, M. F., L. Y. F. Chung, A. S. C. Lee, W. K. Wong, G. S. C. Lee, C. Y. Lau, W. Z. Lau, T. T. Hung, M. L. Liu, and J. W. S. Ng. 2006b. Investigating spiritual care perceptions and practice patterns in Hong Kong nurses: Results of a cluster analysis. Nurse Education Today 26: 139–50. [Google Scholar] [CrossRef] [PubMed]
- Clarke, Janice. 2009. A critical view of how nursing has defined spirituality. Journal of Clinical Nursing 18: 1666–73. [Google Scholar] [CrossRef] [PubMed]
- Cobb, Mark. 2007. Change and Challenge: The Dynamic of Chaplaincy. Scottish Journal of Healthcare Chaplaincy. vol. 10. Available online: http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.530.4026&rep=rep1&type=pdf (accessed on 4 February 2017).
- Cockell, Nell, and Wilfred McSherry. 2012. Spiritual care in nursing: an overview of published international research. Journal of Nursing Management 20: 958–69. [Google Scholar] [CrossRef] [PubMed]
- Cone, Pamela H., and Tove Giske. 2016. Nurses’ Comfort Level with Spiritual Assessment: A Study among Nurses Working in Diverse Healthcare Settings. Journal of Clinical Nursing. [Google Scholar] [CrossRef] [PubMed]
- Egan, Richard, Rod MacLeod, Chrystal Jaye, Rob McGee, Joanne Baxter, and Peter Herbison. 2011. What is spirituality? Evidence from a New Zealand hospice study. Mortality 16: 307–24. [Google Scholar] [CrossRef]
- Egan, Richard, Roz McKechnie, Jan Jobson, Peter Herbison, and Rose Richards. 2013. Perspectives on Psychosocial and Spiritual Cancer Support Services in New Zealand. Journal of Psychosocial Oncology 31: 659–74. [Google Scholar] [CrossRef] [PubMed]
- Gill, Robin, C. Kirk Hadaway, and Penny Long Marler. 1998. Is Religious Belief Declining in Britain? Journal for the Scientific Study of Religion 37: 507–16. [Google Scholar] [CrossRef]
- Health Service Executive. 2011. A Question of Faith—The Relevance of Faith and Spirituality in Health Care. Galway: Health Service Executive. [Google Scholar]
- Heelas, Paul. 2006. Nursing spirituality. Spirituality and Health International 7: 8–23. [Google Scholar] [CrossRef]
- Hubbell, Sara L., Elizabeth K. Woodard, Debra J. Barksdale-Brown, and Jill S. Parker. 2006. Spiritual care practices of nurse practitioners in federally designated nonmetropolitan areas of North Carolina. Journal of the American Academy of Nurse Practitioners 18: 379–85. [Google Scholar] [CrossRef] [PubMed]
- International Council of Nurses. 2006. The ICN Code of Ethics for Nurses. Geneva: International Council of Nurses. [Google Scholar]
- Jim, Heather S. L., James E. Pustejovsky, Crystal L. Park, Suzanne C. Danhauer, Allen C. Sherman, George Fitchett, Thomas V. Merluzzi, Alexis R. Munoz, Login George, Mallory A. Snyder, and et al. 2015. Religion, spirituality, and physical health in cancer patients: A meta-analysis. Cancer 121: 3760–68. [Google Scholar] [CrossRef] [PubMed]
- Joint Commission on Accreditation of Healthcare Associations. 2005. The Source: Evaluating Your Spiritual Assessment Process. Washington: Joint Commission on Accreditation of Healthcare Organisations. [Google Scholar]
- King, Anna. S. 1996. Spirituality: Transformation and Metamorphosis. Religion 26: 345–51. [Google Scholar] [CrossRef]
- Lopez, Violeta, Imke Fischer, Maria Cynthia Leigh, David Larkin, and Sue Webster. 2014. Spirituality, Religiosity, and Personal Beliefs of Australian Undergraduate Nursing Students. Journal of Transcultural Nursing 25: 395–402. [Google Scholar] [CrossRef] [PubMed]
- Lucchetti, Giancarlo, Alessandra Lucchetti, Daniele Espinha, Leandro Oliveira, Jose Leite, and Harold Koenig. 2012. Spirituality and health in the curricula of medical schools in Brazil. BMC Medical Education 12: 78. [Google Scholar] [CrossRef] [PubMed]
- Macrae, Janet. 1995. Nightingale’s spiritual philosophy and its significance for modern nursing. Image: The Journal of Nursing Scholarship 27: 8–10. [Google Scholar] [CrossRef]
- McSherry, Wilfred. 2010. RCN Spirituality Survey 2010: A Report by the Royal College of Nursing on Members’ Views on Spirituality and Spiritual Care in Nursing Practice. London: Royal College of Nursing. [Google Scholar]
- McSherry, Wilfred, and Steve Jamieson. 2013. The qualitative findings from an online survey investigating nurses’ perceptions of spirituality and spiritual care. Journal of Clinical Nursing 22: 3170–82. [Google Scholar] [CrossRef] [PubMed]
- McSherry, Wilfred, and Linda Ross. 2002. Dilemmas of spiritual assessment: considerations for nursing practice. Jounal of Advanced Nursing 38: 479–88. [Google Scholar] [CrossRef]
- McSherry, Wilfred, Mark Gretton, Peter Draper, and Roger Watson. 2008. The ethical basis of teaching spirituality and spiritual care: A survey of student nurses perceptions. Nurse Education Today 28: 1002–8. [Google Scholar] [CrossRef] [PubMed]
- McSherry, Wilfred, Peter Draper, and Don Kendrick. 2002. The construct validity of a rating scale designed to assess spirituality and spiritual care. International Journal of Nursing Studies 39: 723–34. [Google Scholar] [CrossRef]
- McSherry, Wilfred, and Steve Jamieson. 2011. An online survey of nurses’ perceptions of spirituality and spiritual care. Journal of Clinical Nursing 20: 1757–67. [Google Scholar] [CrossRef] [PubMed]
- Meaningful Ageing Australia. 2016. National Guidelines for Spiritual Care in Aged Care. Parkville: Meaningful Ageing Australia. [Google Scholar]
- Ministry of Health. 2010. Guidance for Improving Supportive Care for Adults with Cancer in New Zealand; Wellington: Ministry of Health.
- Morgan, Anne, Rod MacLeod, Mary Schumacher, and Richard Egan. 2015. Delivering spiritual care: A resource to train hospice staff in New Zealand. European Journal of Palliative Care 22: 130–32. [Google Scholar]
- Nascimento, C. Lucila, A. Willyane Alvarenga, Sílvia Caldeira, M. Tâmisa Mica, C. Fabiane Oliveira, Raquel Pan, F. Tabatha Santos, C. Emília Carvalho, and Margarida Vieira. 2016. Spiritual Care: The Nurses’ Experiences in the Pediatric Intensive Care Unit. Religions 7: article 27. [Google Scholar] [CrossRef]
- National Institute for Clinical Excellence. 2004. Guidance on Cancer Services. Improving Supportive and Palliative Care for Adults with Cancer: Executive Summary. London: National Institute for Clinical Excellence. [Google Scholar]
- NHS Education Scotland. 2009. Spiritual Care Matters: An Introductory Resource for all NHS Scotland Staff. Edinburgh: NHS Education for Scotland. [Google Scholar]
- Nightingale, Florence. 1996. Notes on Nursing. New York: Dover. [Google Scholar]
- Nursing and Midwifery Council. 2012. Standards of Proficiency for Pre-registration Nursing Education. London: Nursing and Midwifery Council. [Google Scholar]
- Paley, John. 2008a. Spirituality and nursing: a reductionist approach. Nursing Philosophy 9: 3–18. [Google Scholar] [CrossRef] [PubMed]
- Paley, John. 2008b. Spirituality and secularization: nursing and the sociology of religion. Journal of Clinical Nursing 17: 175–86. [Google Scholar] [CrossRef] [PubMed]
- Paley, John. 2009. Keep the NHS secular. Nursing Standard 23: 26–27. [Google Scholar] [CrossRef] [PubMed]
- Puchalski, Christina M. 2006. A Time for Listening and Caring: Spirituality and the Care of the Chronically Ill and Dying. New York: Oxford University Press. [Google Scholar]
- Puchalski, Christina, Betty Ferrell, Rose Virani, Shirley Otis-Green, Pamela Baird, Janet Bull, Harvey Chochinov, George Handzo, Holly Nelson-Becker, and Maryjo Prince-Paul. 2009. Improving the quality of spiritual care as a dimension of palliative care: the report of the consensus conference. Journal of palliative medicine 12: 885–904. [Google Scholar] [CrossRef] [PubMed]
- Puchalski, Christina, Robert Vitillo, Sharon K. Hull, and Nancy Reller. 2014. Improving the spiritual dimension of whole person care: reaching national and international consensus. Journal of Palliative Medicine 17: 642–56. [Google Scholar] [CrossRef] [PubMed]
- Ramezani, M., F. Ahmadi, E. Mohammadi, and A. Kazemnejad. 2014. Spiritual care in nursing: A concept analysis. International Nursing Review 61: 211–19. [Google Scholar] [CrossRef] [PubMed]
- Reimer-Kirkham, Sheryl, Barbara Pesut, Richard Sawatzky, Marie Cochrane, and Anne Redmond. 2012. Discourses of spirituality and leadership in nursing: A mixed methods analysis. Journal of nursing management 20: 1029–38. [Google Scholar] [CrossRef] [PubMed]
- Reinert, K. G., and H. G. Koenig. 2013. Re-examining definitions of spirituality in nursing research. Jounal Advanced Nursing 69: 2622–34. [Google Scholar] [CrossRef] [PubMed]
- Ross, Linda, Tove Giske, René van Leeuwen, Donia Baldacchino, Wilfred McSherry, Aru Narayanasamy, Paul Jarvis, and Annemiek Schep-Akkerman. 2016. Factors contributing to student nurses’/midwives’ perceived competency in spiritual care. Nurse Educ Today 36: 445–51. [Google Scholar] [CrossRef] [PubMed]
- Ross, Linda. 2006. Spiritual care in nursing: An overview of the research to date. Journal of Clinical Nursing 15: 852–62. [Google Scholar] [CrossRef] [PubMed]
- Ross, Linda, René van Leeuwen, Donia Baldacchino, Tove Giske, Wilfred McSherry, Aru Narayanasamy, Carmel Downes, Paul Jarvis, and Annemiek Schep-Akkerman. 2014. Student nurses perceptions of spirituality and competence in delivering spiritual care: A European pilot study. Nurse Education Today 34: 697–702. [Google Scholar] [CrossRef] [PubMed]
- Royal College of Nursing. 2011. RCN Spirituality Survey 2010. London: Royal College of Nursing. [Google Scholar]
- Salsman, John M., James E. Pustejovsky, Heather S. L. Jim, Alexis R. Munoz, Thomas V. Merluzzi, Login George, Crystal L. Park, Suzanne C. Danhauer, Allen C. Sherman, Mallory A. Snyder, and et al. 2015. A meta-analytic approach to examining the correlation between religion/spirituality and mental health in cancer. Cancer 121: 3769–78. [Google Scholar] [CrossRef] [PubMed]
- Sherman, Allen C., Thomas V. Merluzzi, James E. Pustejovsky, Crystal L. Park, Login George, George Fitchett, Heather S. L. Jim, Alexis R. Munoz, Suzanne C. Danhauer, Mallory A. Snyder, and et al. 2015. A meta-analytic review of religious or spiritual involvement and social health among cancer patients. Cancer 121: 3779–88. [Google Scholar] [CrossRef] [PubMed]
- Sloan, Richard P., Emilia Bagiella, and Tia Powell. 1999. Religion, spirituality, and medicine. The Lancet 353: 664–67. [Google Scholar] [CrossRef]
- Spadoni, Michelle, and Patricia Sevean. 2016. Relational Inquiry—Attending to the Spirit of Nursing Students. Religions 7: article 34. [Google Scholar] [CrossRef]
- Statistics New Zealand Tatauranga Aotearoa. 2013. Census QuickStats about culture and identity. Available online: http://www.stats.govt.nz/Census/2013-census/profile-and-summary-reports/quickstats-culture-identity.aspx (accessed on 24 April 2017).
- Stewart, Moira, Judith Belle Brown, Wayne Weston, Ian R. McWhinney, Carol L. McWilliam, and Thomas Freeman. 1995. Patient-Centred Medicine: Transforming the Clinical Method. Thousand Oaks: Sage Publications. [Google Scholar]
- Swinton, John, and Stephen Pattison. 2010. Moving beyond clarity: towards a thin, vague, and useful understanding of spirituality in nursing care. Nursing Philosophy 11: 226–37. [Google Scholar] [CrossRef] [PubMed]
- Tacey, D. 2003. The Spiritual Revolution: The Emergence of Contemporary Spirituality. Sydney: HarperCollins Publishers. [Google Scholar]
- Tanyi, R. A. 2002. Towards clarification of the meaning of spirituality. Journal of Advanced Nursing 39: 500–9. [Google Scholar] [CrossRef] [PubMed]
- Taylor, Bridget. 2014. Experiences of sexuality and intimacy in terminal illness: A phenomenological study. Palliative Medicine 28: 438–47. [Google Scholar] [CrossRef] [PubMed]
- Taylor, Elizabeth J. 2011. Spiritual care: Evangelism at the bedside. Journal of Christian Nursing 28: 194–202. [Google Scholar] [CrossRef] [PubMed]
- Timmins, Fiona, and Sílvia Caldeira. 2017. Understanding spirituality and spiritual care in nursing. Nursing Standard 31: 50–57. [Google Scholar] [CrossRef] [PubMed]
- Timmins, Fiona, and Wilf McSherry. 2012. Spirituality: The Holy Grail of contemporary nursing practice. Journal of nursing management 20: 951–57. [Google Scholar] [CrossRef] [PubMed]
- Timmins, Fiona, Maryanne Murphy, Freda Neill, Thelma Begley, and Greg Sheaf. 2015. An exploration of the extent of inclusion of spirituality and spiritual care concepts in core nursing textbooks. Nurse Education Today 35: 277–82. [Google Scholar] [CrossRef] [PubMed]
- Vaccarino, F., H. Kavan, and P. Gendall. 2011. Spirituality and Religion in the Lives of New Zealanders. International Journal of Religion and Spirituality in Society 1: 88–96. [Google Scholar]
- van Leeuwen, R., L. J. Tiesinga, B. Middel, D. Post, and H. Jochemsen. 2008. The effectiveness of an educational programme for nursing students on developing competence in the provision of spiritual care. Journal of Clinical Nursing 17: 2768–81. [Google Scholar] [CrossRef] [PubMed]
- van Leeuwen, René, and Annemiek Schep-Akkerman. 2015. Nurses’ Perceptions of Spirituality and Spiritual Care in Different Health Care Settings in the Netherlands. Religions 6: 1346–57. [Google Scholar] [CrossRef]
- Weathers, Elizabeth, Geraldine McCarthy, and Alice Coffey. 2015. Concept Analysis of Spirituality: An Evolutionary Approach. Nursing Forum 51: 79–92. [Google Scholar] [CrossRef] [PubMed]
- Weaver, Andrew J., Harold G. Koenig, and Laura T. Flannelly. 2008. Nurses and Healthcare Chaplains: Natural Allies. Journal of Health Care Chaplaincy 14: 91–98. [Google Scholar] [CrossRef] [PubMed]
- Wittenberg, Elaine, Sandra L. Ragan, and Betty Ferrell. 2016. Exploring Nurse Communication About Spirituality. American Journal of Hospice and Palliative Medicine. [Google Scholar] [CrossRef] [PubMed]
- Wu, Li-Fen, Hui-Chen Tseng, and Yu Chen. Liao. 2016. Nurse education and willingness to provide spiritual care. Nurse Education Today 38: 36–41. [Google Scholar] [CrossRef] [PubMed]
| Age Group | NZ Council-Registered Rurses | Electoral Roll |
|---|---|---|
| < 25 | 1499 | 681 |
| 25–29 | 4060 | 2465 |
| 30–34 | 3861 | 3255 |
| 35–39 | 4173 | 3805 |
| 40–44 | 5890 | 5829 |
| 45–49 | 6242 | 6068 |
| 50–54 | 7671 | 7704 |
| 55–59 | 6948 | 7427 |
| 60–64 | 4504 | 5250 |
| 65+ | 2913 | 5599 |
| Total | 47,751 | 48,083 |
| CHARACTERISTICS | Electoral roll * (%) | Selection ** (%) | Participants † (%) |
|---|---|---|---|
| Female | 92.1 | 93.2 | 95.4 |
| Age (years) | |||
| 30–39 | 18.7 | 20.1 | 16.5 |
| 40–49 | 29.5 | 28.7 | 28.1 |
| 50–59 | 38.0 | 37.0 | 40.9 |
| 60–64 | 13.6 | 14.2 | 14.4 |
| District Health Board Region | |||
| Auckland | 8.4 | 9.1 | 16.7 |
| Waikato | 8.5 | 8.4 | 7.7 |
| Canterbury | 12.8 | 13.6 | 17.7 |
| Southern | 7.9 | 7.3 | 10.7 |
| Other | 62.4 | 61.6 | 47.2 |
| Institution | |||
| Public Hospital | 48.8 | ||
| Private Hospital | 8.8 | ||
| Public Health Organisation | 7.2 | ||
| Aged Care Facility | 9.1 | ||
| Other | 26.1 | ||
| Scope of Practice | |||
| Registered Nurse | 92.0 | 91.1 | 92.5 |
| Enrolled Nurse | 2.3 | 2.7 | 4 |
| Nurse Practitioner | 0.1 | 0.2 | 1.2 |
| Other | 5.6 | 6 | 2.3 |
| Years Worked | |||
| < 1 year | 4.9 | ||
| 1–2 years | 7.9 | ||
| 3+ years | 87.2 | ||
| Ethnicity | |||
| New Zealand European | 82.1 | ||
| Maori | 8.3 | 8.2 | 7.2 |
| Indian | 2.3 | ||
| African | 1.4 | ||
| Other European | 2.6 | ||
| Other Asian | 1.2 | ||
| Religion | |||
| None | 35.3 | ||
| Christian | 57.9 | ||
| Hindu | 1.4 | ||
| Other | 2.1 | ||
| Practicing their religion | 61.5 |
| Theme | Subtheme | Quote | Implication |
|---|---|---|---|
| The place of spirituality in nursing practice | An integral component | “When spiritual needs are addressed healing time, anxiety and prognosis all improve the patient’s journey.” “Identifying and addressing spiritual needs with clients/service users starts with the therapeutic relationship which in itself it a spiritual passage—the development of whakawhanaungatanga or connection between two human beings at the start of a journey of change… All in all nurses are provided a beautiful opportunity to spiritually experience the many journeys of the people we are privileged to work alongside.” “Nursing is a spiritual job. If you don’t believe in meaning and purpose, love and hope you shouldn’t be doing it.” “Spirituality shapes, divides, draws close, separates individuals. It is part of the needs of an individual just as food is. If is clearly connected to the mental health and wellbeing of many people therefore must be given equal and considered care in its approach. It could be the difference in some people surviving or not surviving from illness therefore must be regarded as essential and on the spectrum of care.” “One of the distinguishing features of nursing is its focus on things unspoken—and that includes spirituality.” | Many participants expressed a common idea that “spiritual healing will help the healing of sickness.” The idea of the ‘therapeutic relationship’ signals the role of nurses in spiritual care—a connection of some sort that does not have to cross professional boundaries. Would framing spiritual care in terms of a ‘journey’ and ‘therapeutic relationship’ overcome some resistance? |
| Not our role | “Whilst I understand that there are people who require spiritual care, I feel this will lessen as the population further identifies as not having a religion.” “There are so many levels of spiritual care and I don’t think nurses should be responsible for performing it themselves. Guidance in how to get appropriate help and the time/resources to do so should be part of our training and orientation to workplaces.” | The idea that spiritual needs will decline contradicts some research on the rise of spirituality—and dual decline of religious affiliation—and highlights the need for education. Is there a need to transform the idea of an ‘amorphous’ spirituality from a scary prospect to a necessary state to accommodate all needs? In this way, a nurse is not expected to be able to cater for all, but recognise, potentially help, but also have the capacity to refer on as required. |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Egan, R.; Llewellyn, R.; Cox, B.; MacLeod, R.; McSherry, W.; Austin, P. New Zealand Nurses’ Perceptions of Spirituality and Spiritual care: Qualitative Findings from a National Survey. Religions 2017, 8, 79. https://doi.org/10.3390/rel8050079
Egan R, Llewellyn R, Cox B, MacLeod R, McSherry W, Austin P. New Zealand Nurses’ Perceptions of Spirituality and Spiritual care: Qualitative Findings from a National Survey. Religions. 2017; 8(5):79. https://doi.org/10.3390/rel8050079
Chicago/Turabian StyleEgan, Richard, Rebecca Llewellyn, Brian Cox, Rod MacLeod, Wilfred McSherry, and Philip Austin. 2017. "New Zealand Nurses’ Perceptions of Spirituality and Spiritual care: Qualitative Findings from a National Survey" Religions 8, no. 5: 79. https://doi.org/10.3390/rel8050079
APA StyleEgan, R., Llewellyn, R., Cox, B., MacLeod, R., McSherry, W., & Austin, P. (2017). New Zealand Nurses’ Perceptions of Spirituality and Spiritual care: Qualitative Findings from a National Survey. Religions, 8(5), 79. https://doi.org/10.3390/rel8050079