Galectin-3 as the Prognostic Factor of Adverse Cardiovascular Events in Long-Term Follow up in Patients after Myocardial Infarction—A Pilot Study
Abstract
1. Introduction
2. Material and Methods
2.1. Selection of the Study Population
2.2. Control Group
2.3. Biochemical Evaluation
2.4. Echocardiography
2.5. Coronary Angiography
2.6. Doppler Ultrasonography of the Carotid Arteries
2.7. Follow-Up Visit
2.8. Statistical Analysis
3. Results
3.1. Characteristics of the Study Group at Baseline and on the Follow-Up Visit
3.2. Gal-3 Concentration
3.2.1. At Baseline
3.2.2. On the Follow-up Visit
3.3. Gal-3 Concentration and Cardiovascular Risk Factors
3.4. Gal-3 Concentration and Advancement of CAD
3.5. Gal-3 Concentration and Carotid Atherosclerosis
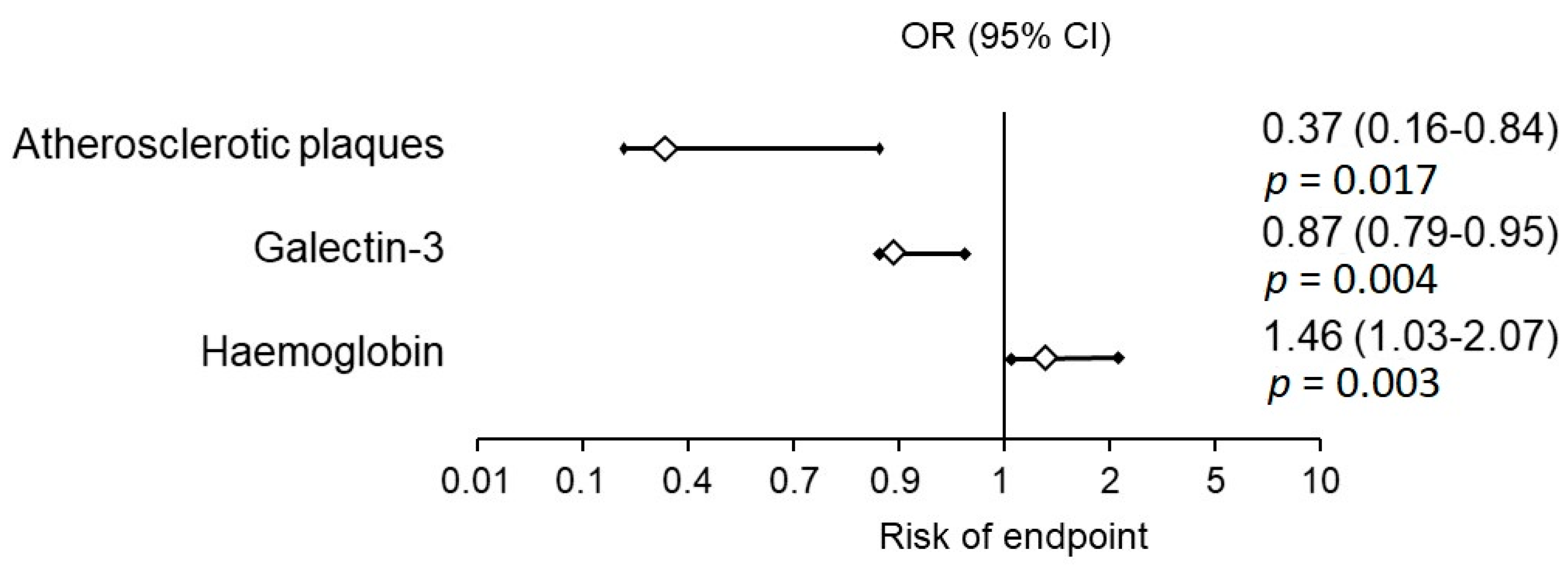
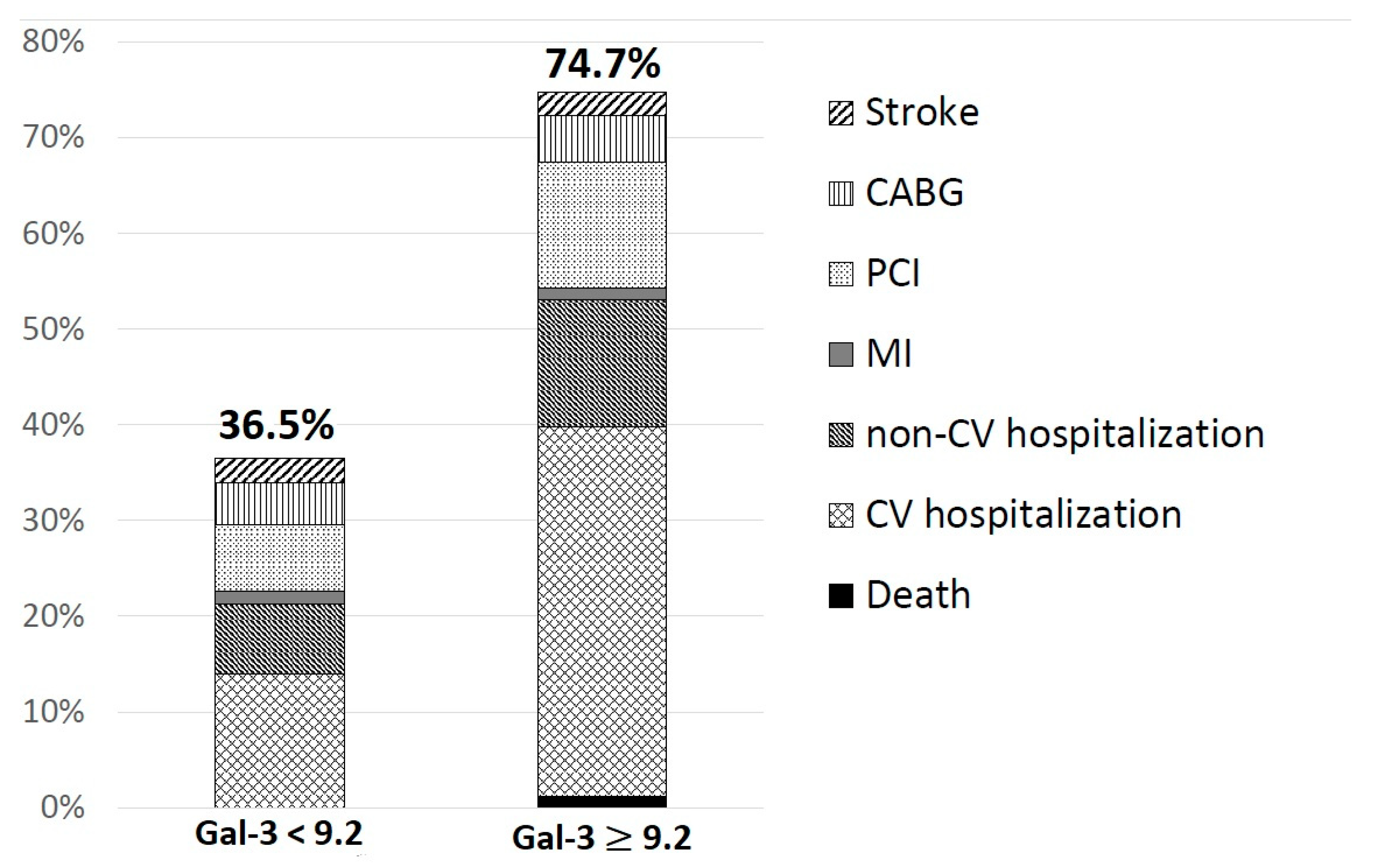
3.6. Gal-3 Concentration and Occurrence of Adverse Cardiovascular Events during Follow-up Period
3.7. Carotid Ultrasonography Parameters
3.7.1. At Baseline
3.7.2. On the Follow-Up Visit
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Pedersen, N.L.; Petersen, M.M.; Ladd, J.J.; Lampe, P.D.; Bresalier, R.S.; Davis, G.J.; Demuth, C.; Jensen, S.Ø.; Andersen, C.L.; Ferm, L.; et al. Development of blood-based biomarker tests for early detection of colorectal neoplasia: Influence of blood collection timing and handling procedures. Clin. Chim. Acta 2020, 507, 39–53. [Google Scholar] [CrossRef]
- Flaherty, M.M.; Palmer, O.R.; Diaz, J.A. Galectin-3 in venous thrombosis: A possible new target for improved patient care. Res. Pract. Thromb. Haemost. 2018, 2, 399–400. [Google Scholar] [CrossRef]
- DeRoo, E.P.; Wrobleski, S.K.; Shea, E.M.; Al-Khalil, R.K.; Hawley, A.E.; Henke, P.K.; Myers, D.D., Jr.; Wakefield, T.W.; Diaz, J.A. The role of galectin-3 and galectin-3-binding protein in venous thrombosis. Blood 2015, 125, 1813–1821. [Google Scholar] [CrossRef]
- Ho, J.E.; Liu, C.; Lyass, A.; Courchesne, P.; Pencina, M.J.; Vasan, R.S.; Larson, M.G.; Levy, D. Galectin-3, a marker of cardiac fibrosis, predicts incident heart failure in the community. J. Am. Coll. Cardiol. 2012, 60, 1249–1256. [Google Scholar] [CrossRef]
- Felker, G.M.; Fiuzat, M.; Shaw, L.K.; Clare, R.; Whellan, D.J.; Bettari, L.; Shirolkar, S.C.; Donahue, M.; Kitzman, D.W.; Zannad, F.; et al. Galectin-3 in ambulatory patients with heart failure: Results from the HF-ACTION study. Circ. Heart Fail. 2012, 5, 72–78. [Google Scholar] [CrossRef]
- de Boer, R.A.; Lok, D.J.; Jaarsma, T.; van der Meer, P.; Voors, A.A.; Hillege, H.L.; van Veldhuisen, D.J. Predictive value of plasma galectin-3 levels in heart failure with reduced and preserved ejection fraction. Ann. Med. 2011, 43, 60–68. [Google Scholar] [CrossRef]
- Arar, C.; Gaudin, J.C.; Capron, L.; Legrand, A. Galectin-3 gene (LGALS3) expression in experimental atherosclerosis and cultured smooth muscle cells. FEBS Lett. 1998, 430, 307–311. [Google Scholar] [CrossRef]
- Iacobini, C.; Menini, S.; Ricci, C.; Scipioni, A.; Sansoni, V.; Cordone, S.; Taurino, M.; Serino, M.; Marano, G.; Federici, M.; et al. Accelerated lipid-induced atherogenesis in galectin-3-deficient mice: Role of lipoxidation via receptor-mediated mechanisms. Arterioscler. Thromb. Vasc. Biol. 2009, 29, 831–836. [Google Scholar] [CrossRef]
- Menini, S.; Iacobini, C.; Ricci, C.; Blasetti Fantauzzi, C.; Salvi, L.; Pesce, C.M.; Relucenti, M.; Familiari, G.; Taurino, M.; Pugliese, G. The galectin-3/RAGE dyad modulates vascular osteogenesis in atherosclerosis. Cardiovasc. Res. 2013, 100, 472–480. [Google Scholar] [CrossRef]
- MacKinnon, A.C.; Liu, X.; Hadoke, P.W.; Miller, M.R.; Newby, D.E.; Sethi, T. Inhibition of galectin-3 reduces atherosclerosis in apolipoprotein E-deficient mice. Glycobiology 2013, 23, 654–663. [Google Scholar] [CrossRef]
- Tsai, T.H.; Sung, P.H.; Chang, L.T.; Sun, C.K.; Yeh, K.H.; Chung, S.Y.; Chua, S.; Chen, Y.L.; Wu, C.J.; Chang, H.W.; et al. Value and level of galectin-3 in acute myocardial infarction patients undergoing primary percutaneous coronary intervention. J. Atheroscler. Thromb. 2012, 19, 1073–1082. [Google Scholar] [CrossRef] [PubMed]
- Lisowska, A.; Knapp, M.; Tycińska, A.; Motybel, E.; Kamiński, K.; Święcki, P.; Musiał, W.J.; Dymicka-Piekarska, V. Predictive value of Galectin-3 for the occurrence of coronary artery disease and prognosis after myocardial infarction and its association with carotid IMT values in these patients: A mid-term prospective cohort study. Atherosclerosis 2016, 246, 309–317. [Google Scholar] [CrossRef] [PubMed]
- Goenka, L.; George, M.; Singh, V.; Jena, A.; Seshadri, D.; Karunakaran, V.; Elumalai, D.V.; Rani, J.; Kaliappan, I. Do ANGPTL-4 and galectin-3 reflect the severity of coronary artery disease? Ther. Adv. Cardiovasc. Dis. 2017, 1753944717723311. [Google Scholar] [CrossRef] [PubMed]
- Gullestad, L.; Ueland, T.; Kjekshus, J.; Nymo, S.H.; Hulthe, J.; Muntendam, P.; McMurray, J.J.; Wikstrand, J.; Aukrust, P. The predictive value of galectin-3 for mortality and cardiovascular events in the Controlled Rosuvastatin Multinational Trial in Heart Failure (CORONA). Am. Heart J. 2012, 164, 878–883. [Google Scholar] [CrossRef]
- Touboul, P.J.; Hennerici, M.G.; Meairs, S.; Adams, H.; Amarenco, P.; Desvarieux, M.; Ebrahim, S.; Fatar, M.; Hernandez, R.H.; Kownator, S. Mannheim intima-media thickness consensus. Cerebrovasc. Dis. 2004, 18, 346–349. [Google Scholar] [CrossRef]
- Hunt, K.J.; Sharrett, A.R.; Chambless, L.E.; Folsom, A.R.; Evans, G.W.; Heiss, G. Acoustic shadowing on B-mode ultrasound of the carotid artery predicts CHD. Ultrasound Med. Biol. 2001, 27, 357–365. [Google Scholar] [CrossRef]
- González, G.E.; Cassaglia, P.; Truant, S.N.; Fernández, M.M.; Wilensky, L.; Volberg, V.; Malchiodi, E.L.; Morales, C.; Gelpi, R.J. Galectin-3 is essential for early wound healing and ventricular remodeling after myocardial infarction in mice. Int. J. Cardiol. 2014, 176, 1423–1425. [Google Scholar] [CrossRef]
- Ozturk, D.; Celik, O.; Satilmis, S.; Aslan, S.; Erturk, M.; Cakmak, H.A.; Kalkan, A.K.; Ozyilmaz, S.; Diker, V.; Gul, M. Association between serum galectin-3 levels and coronary atherosclerosis and plaque burden/structure in patients with type 2 diabetes mellitus. Coron. Artery Dis. 2015, 26, 396–401. [Google Scholar] [CrossRef]
- Kadoglou, N.P.E.; Sfyroeras, G.S.; Spathis, A.; Gkekas, C.; Gastounioti, A.; Mantas, G.; Nikita, K.S.; Karakitsos, P.; Liapis, C.D. Galectin-3, Carotid Plaque Vulnerability, and Potential Effects of Statin Therapy. Eur. J. Vasc. Endovasc. Surg. 2015, 49, 4–9. [Google Scholar] [CrossRef]
- He, X.W.; Li, W.L.; Li, C.; Liu, P.; Shen, Y.G.; Zhu, M.; Jin, X.P. Serum levels of galectin-1, galectin-3, and galectin-9 are associated with large artery atherosclerotic stroke. Sci. Rep. 2017, 7, 40994. [Google Scholar] [CrossRef]
- Wang, A.; Zhong, C.; Zhu, Z.; Xu, T.; Peng, Y.; Xu, T.; Peng, H.; Chen, C.S.; Wang, J.; Ju, Z.; et al. Serum Galectin-3 and Poor Outcomes Among Patients With Acute Ischemic Stroke. Stroke 2018, 49, 211–214. [Google Scholar] [CrossRef] [PubMed]
- Zeng, N.; Wang, A.; Zhong, C.; Zheng, X.; Zhu, Z.; Xu, T.; Peng, Y.; Peng, H.; Li, Q.; Ju, Z.; et al. Association of Serum Galectin-3 with Risks of Death and Vascular Events in Acute Ischemic Stroke Patients: The Role of Hyperglycemia. Eur. J. Neurol. 2018. [Google Scholar] [CrossRef]
- Lee, Y.J.; Koh, Y.S.; Park, H.E.; Lee, H.J.; Hwang, B.H.; Kang, M.K.; Lee, S.Y.; Kim, P.J.; Ihm, S.H.; Seung, K.B.; et al. Spatial and temporal expression, and statin responsiveness of galectin-1 and galectin-3 in murine atherosclerosis. Korean Circ. J. 2013, 43, 223–230. [Google Scholar] [CrossRef]
- Savic, J.; Zeljkovic, A.; Bogavac-Stanojevic, N.; Simic-Ogrizovic, S.; Kravljaca, M.; Stosovic, M.; Vekic, J.; Spasojevic-Kalimanovska, V.; Jelic-Ivanovic, Z.; Gojkovic, T.; et al. Association of small, dense low-density lipoprotein cholesterol and galectin-3 in patients with chronic kidney disease. Scand. J. Clin. Lab. Investig. 2014, 74, 637–643. [Google Scholar] [CrossRef]
- Laake, K.; Seljeflot, I.; Schmidt, E.B.; Myhre, P.; Tveit, A.; Norseth, J.; Arnesen, H.; Solheim, S. Galectin-3, a marker of cardiac remodeling, is inversely related to serum levels of marine omega-3 fatty acids. A cross-sectional study. JRSM Cardiovasc. Dis. 2017, 6, 2048004017729984. [Google Scholar] [CrossRef] [PubMed]
- Di Tano, G.; Caretta, G.; De Maria, R.; Bettari, L.; Parolini, M.; Testa, S.; Pirelli, S. Galectin-3 and outcomes after anterior-wall myocardial infarction treated by primary percutaneous coronary intervention. Biomark. Med. 2018, 12, 21–26. [Google Scholar] [CrossRef]
- Tan, K.C.B.; Cheung, C.L.; Lee, A.C.H.; Lam, J.K.Y.; Wong, Y.; Shiu, S.W.M. Galectin-3 and risk of cardiovascular events and all-cause mortality in type 2 diabetes. Diabetes Metab. Res. Rev. 2019, 35, e3093. [Google Scholar] [CrossRef]
- Sharma, U.C.; Mosleh, W.; Chaudhari, M.R.; Katkar, R.; Weil, B.; Evelo, C.; Cimato, T.R.; Pokharel, S.; Blankesteijn, W.M.; Suzuki, G. Myocardial and Serum Galectin-3 Expression Dynamics Marks Post-Myocardial Infarction Cardiac Remodelling. Heart Lung Circ. 2017, 26, 736–745. [Google Scholar] [CrossRef]
- Jansen, H.; Koenig, W.; Jaensch, A.; Mons, U.; Breitling, L.P.; Scharnagl, H.; Stojakovic, T.; Schunkert, H.; Brenner, H.; Rothenbacher, D. Prognostic Utility of Galectin-3 for Recurrent Cardiovascular Events During Long-term Follow-up in Patients with Stable Coronary Heart Disease: Results of the KAROLA Study. Clin. Chem. 2016, 62, 1372–1379. [Google Scholar] [CrossRef]
- Shimura, T.; Shibata, M.; Gonda, K.; Kofunato, Y.; Okada, R.; Ishigame, T.; Kimura, T.; Kenjo, A.; Kono, K.; Marubashi, S. Significance of Circulating Galectin-3 in Patients with Pancreatobiliary Cancer. Anticancer Res. 2017, 37, 4979–4986. [Google Scholar] [CrossRef]
- Stanojevic, D.; Apostolovic, S.; Stokanovic, D.; Momčilović, S.; Jevtovic-Stoimenov, T.; Salinger-Martinovic, S.; Kostic, T.; Nikolic, V.N. Galectin-3 in Acute Myocardial Infarction Patients with Atrial Fibrillation. Med. Princ. Pract. 2019, 28, 284–290. [Google Scholar] [CrossRef] [PubMed]
- Topcu, T.O.; Kavgaci, H.; Gunaldi, M.; Kocoglu, H.; Akyol, M.; Mentese, A.; Yaman, S.O.; Orem, A.; Ozdemir, F.; Aydin, F. The clinical importance of serum galectin-3 levels in breast cancer patients with and without metastasis. J. Cancer Res. Ther. 2018, 14, S583–S586. [Google Scholar] [CrossRef] [PubMed]
| STEMI Group (n = 66) | NSTEMI Group (n = 44) | Control Group (n = 100) | p-Value Control Group vs. MI Group | p-Value STEMI vs. NSTEMI Group | ||
|---|---|---|---|---|---|---|
| Age (y) | 62.4 ± 9.7 | 64.2 ± 10.1 | 61.5 ± 7.9 | NS | NS | |
| Sex | women | 6 p. (9.1%) | 16 p. (36.4%) | 34 p. (33.7%) | NS | p < 0.005 |
| men | 60 p. (90.9%) | 28 p. (63.6%) | 67 p. (66.3%) | NS | p < 0.005 | |
| BMI (kg/m2) | 27.1 ± 2.4 | 27.5 ± 3.5 | 26.9 ± 3.4 | NS | NS | |
| Smoking (n) | 40 p. (60.6%) | 26 p. (59.1%) | 28 p. (28%) | p < 0.001 | NS | |
| Hypertension (n) | 44 p. (66.7%) | 27 p. (61.4%) | 0 p. | - | NS | |
| Diabetes t.2 (n) | 12 p. (18.2%) | 5 p. (11.4%) | 0 p. | - | NS | |
| Hyperlipidemia (n) | 25 p. (37.9%) | 19 p. (43.2%) | 0 p. | - | NS | |
| Systolic BP (mmHg) | 144.1 ± 24.0 | 146.2 ± 25.0 | 132.8 ± 19.0 | p < 0.05 | NS | |
| Diastolic BP (mmHg) | 88.6 ± 15.6 | 88.8 ± 13.6 | 83.0 ± 8.0 | NS | NS | |
| Total cholesterol (mmol/L) | 4.96 ± 1.0 | 4.91 ± 0.95 | 4.40 ± 0.9 | p < 0.05 | NS | |
| LDL cholesterol (mmol/L) | 3.19 ± 0.95 | 3.11 ± 0.89 | 2.74 ± 0.8 | p < 0.05 | NS | |
| HDL cholesterol (mmol/L) | 1.15 ± 0.3 | 1.2 ± 0.24 | 1.6 ± 0.35 | p < 0.05 | NS | |
| TG (mmol/L) | 1.59 ± 0.95 | 1.53 ± 0.87 | 1.42 ± 0.54 | NS | NS | |
| Glucose (mmol/L) | 6.35 ± 1.4 | 5.8 ± 1.3 | 5.65 ± 1.1 | p < 0.05 | p < 0.05 | |
| Creatinine (µmol/L) | 91.05 ± 28.0 | 79.6 ± 19.5 | 89.2 ± 14.8 | NS | p < 0.05 | |
| GFR (mL/min) | 82.7 ± 25.6 | 87.1 ± 23.7 | 109.5 ± 30.0 | p < 0.01 | NS | |
| Haemoglobin (mmol/L) | 8.7 ± 0.8 | 8.5 ± 0.7 | 8.9 ± 1.0 | NS | NS | |
| EF (%) | 45.9 ± 9.5 | 49.7 ± 10.1 | 55.0 ± 12.5 | p < 0.01 | NS (p = 0.05) | |
| 1-vessel disease (n) | 25 p. (37.9%) | 15 p. (34.1%) | - | - | NS | |
| 2-vessel disease (n) | 15 p. (22.7%) | 7 p. (15.9%) | - | - | NS | |
| 3-vessel disease (n) | 25 p. (37.9%) | 17 p. (38.6%) | - | - | NS | |
| Clinical Characteristics of the Study Group | STEMI Patients (n = 66) | NSTEMI Patients (n = 44) | p-Value |
|---|---|---|---|
| CCS class | 0.5 ± 0.8 | 0.6 ± 0.9 | p = 0.5 |
| NYHA class | 1.5 ± 0.95 | 1.6 ± 1.0 | p = 0.3 |
| EF (%) | 45.6 ± 9.9 | 49.5 ± 9.8 | p = 0.04 |
| Rehospitalization from cardiac causes | 41 p. (60.3%) | 27 p. (61.4%) | p = 0.9 |
| Rehospitalization from non-cardiac causes | 17 p. (25.0%) | 12 p. (27.3%) | p = 0.8 |
| Subsequent MI | 0 p. (0%) | 4 p. (9.1%) | p = 0.005 |
| Re-PCI | 18 p. (26.5%) | 10 p. (22.7%) | p = 0.6 |
| CABG | 10 p. (14.7%) | 5 p. (11.4%) | p = 0.6 |
| Stroke | 4 p. (5.9%) | 5 p. (11.4%) | p = 0.3 |
| Peripheral artery disease | 10 p. (14.7%) | 4 p. (9.1%) | p = 0.4 |
| Carotid artery disease | 2 p. (2.9%) | 2 p. (4.5%) | p = 0.6 |
| Smoking | 23 p. (33.8%) | 8 p. (18.2%) | p = 0.04 |
| Treatment | |||
| Aspirin | 58 p. (85.3%) | 38 p. (86.4%) | p = 0.9 |
| Clopidogrel | 8 p. (17.7%) | 8 p. (18.2%) | p = 0.3 |
| ACEIs | 47 p. (69.1%) | 23 p. (52.3%) | p = 0.04 |
| ARBs | 8 p. (11.8%) | 6 p. (13.6%) | p = 0.8 |
| Beta blockers | 63 p. (92.6%) | 39 p. (88.6%) | p = 0.5 |
| MRAs | 17 p. (25.0%) | 9 p. (20.5%) | p = 0.6 |
| Statins | 62 p. (91.2%) | 38 p. (86.4%) | p = 0.4 |
| Diuretics | 24 p. (35.3%) | 19 p. (43.2%) | p = 0.4 |
| Oral antidiabetic | 15 p. (22.1%) | 8 p. (18.2%) | p = 0.6 |
| Insulin | 6 p. (8.8%) | 4 p. (9.1%) | p = 0.9 |
| Oral anticoagulant | 6 p. (8.8%) | 3 p. (6.8%) | p = 0.5 |
| No Endpoints during Follow Up | Gal-3 Concentration (ng/mL) at Baseline | Gal-3 Concentration (ng/mL) on the Follow-Up Visit | p-Value |
|---|---|---|---|
| Subsequent MI | 10.8 ± 6.1 | 8.8 ± 2.4 | p = 0.03 |
| Re-PCI | 10.6 ± 5.8 | 8.6 ± 2.4 | p = 0.04 |
| CABG | 11.1 ± 7.5 | 8.7 ± 2.5 | p = 0.016 |
| Stroke | 10.7 ± 5.9 | 8.7 ± 2.3 | p = 0.03 |
| MI Group at Baseline (n = 110) | MI Group on the Follow-Up Visit | p-Value | Control Group (n = 100) | p-Value (MI Patients vs. Control) | |
|---|---|---|---|---|---|
| Plaque occurrence in CCA | 12 p. (10.9%) | 10 p. (9.1%) | NS | 0 | p = 0.000001 |
| Plaque occurrence in CB | 87 p. (79.1%) | 69 p. (62.7%) | p = 0.003 | 0 | p = 0.000001 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Święcki, P.; Sawicki, R.; Knapp, M.; Kamiński, K.A.; Ptaszyńska-Kopczyńska, K.; Sobkowicz, B.; Lisowska, A. Galectin-3 as the Prognostic Factor of Adverse Cardiovascular Events in Long-Term Follow up in Patients after Myocardial Infarction—A Pilot Study. J. Clin. Med. 2020, 9, 1640. https://doi.org/10.3390/jcm9061640
Święcki P, Sawicki R, Knapp M, Kamiński KA, Ptaszyńska-Kopczyńska K, Sobkowicz B, Lisowska A. Galectin-3 as the Prognostic Factor of Adverse Cardiovascular Events in Long-Term Follow up in Patients after Myocardial Infarction—A Pilot Study. Journal of Clinical Medicine. 2020; 9(6):1640. https://doi.org/10.3390/jcm9061640
Chicago/Turabian StyleŚwięcki, Przemysław, Robert Sawicki, Małgorzata Knapp, Karol Adam Kamiński, Katarzyna Ptaszyńska-Kopczyńska, Bożena Sobkowicz, and Anna Lisowska. 2020. "Galectin-3 as the Prognostic Factor of Adverse Cardiovascular Events in Long-Term Follow up in Patients after Myocardial Infarction—A Pilot Study" Journal of Clinical Medicine 9, no. 6: 1640. https://doi.org/10.3390/jcm9061640
APA StyleŚwięcki, P., Sawicki, R., Knapp, M., Kamiński, K. A., Ptaszyńska-Kopczyńska, K., Sobkowicz, B., & Lisowska, A. (2020). Galectin-3 as the Prognostic Factor of Adverse Cardiovascular Events in Long-Term Follow up in Patients after Myocardial Infarction—A Pilot Study. Journal of Clinical Medicine, 9(6), 1640. https://doi.org/10.3390/jcm9061640







