Investigating Association between Intraoperative Hypotension and Postoperative Neurocognitive Disorders in Non-Cardiac Surgery: A Comprehensive Review
Abstract
1. Introduction
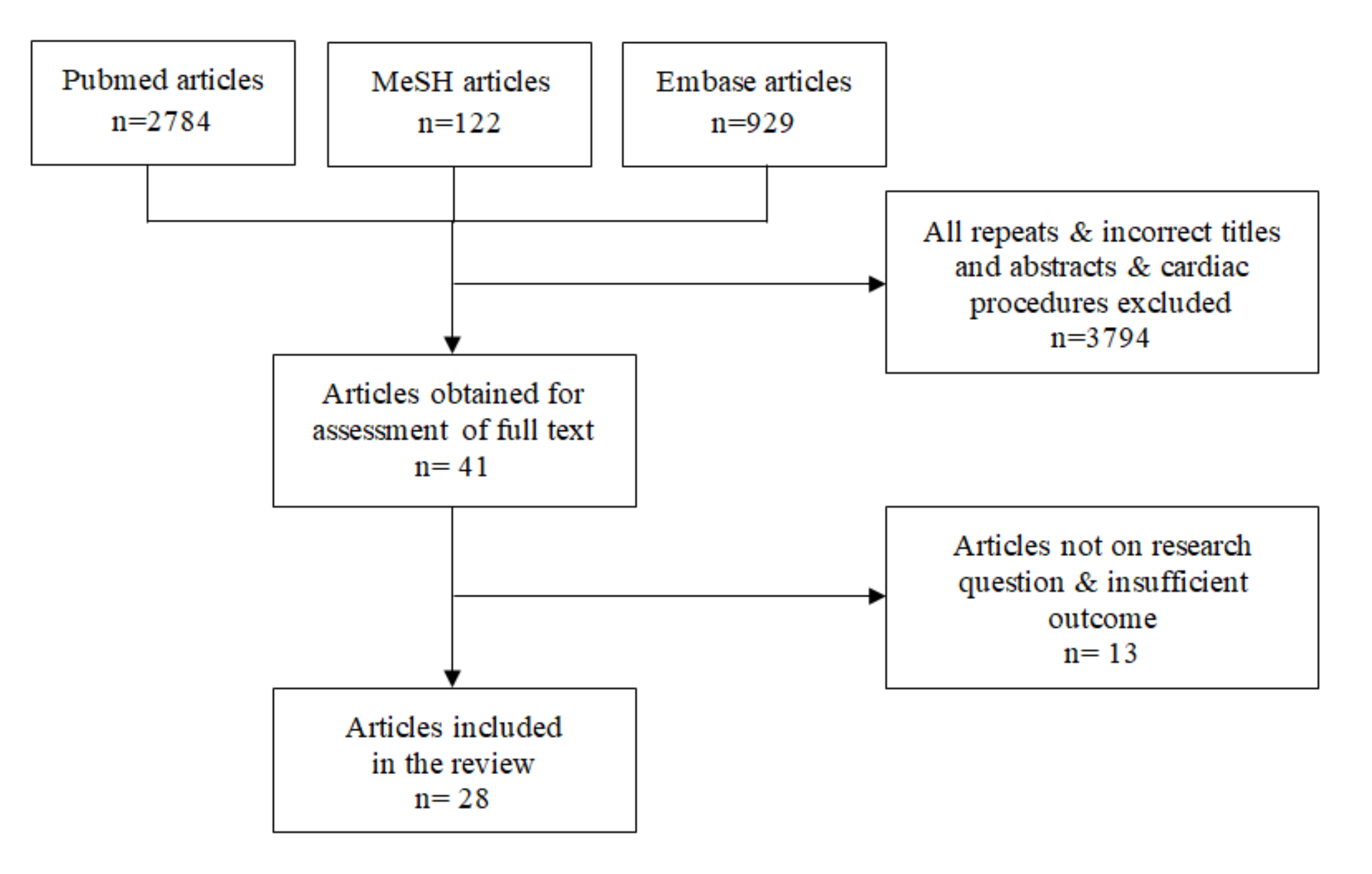
2. Methods
3. Review
3.1. Postoperative Cognitive Decline (Deficit)
3.2. Postoperative Delirium
4. Discussion
4.1. Cerebral Perfusion and Its Monitoring
4.2. POCD
4.3. POD
4.4. Major Concerns for Further Investigations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Dai, S.; Li, X.; Yang, Y.; Cao, Y.; Wang, E.; Dong, Z. A retrospective cohort analysis for the risk factors of intraoperative hypotension. Int. J. Clin. Pract. 2020, 30, 13521. [Google Scholar] [CrossRef] [PubMed]
- Kouz, K.; Hoppe, P.; Briesenick, L.; Saugel, B. Intraoperative hypotension: Pathophysiology, clinical relevance, and therapeutic approaches. Indian J. Anaesth. 2020, 64, 90–96. [Google Scholar] [PubMed]
- Cheung, C.C.; Martyn, A.; Campbell, N.; Frost, S.; Gilbert, K.; Michota, F.; Seal, D.; Ghali, W.; Khan, N.A. Predictors of intraoperative hypotension and bradycardia. Am. J. Med. 2015, 128, 532–538. [Google Scholar] [CrossRef] [PubMed]
- Sessler, D.I.; Bloomstone, J.A.; Aronson, S.; Berry, C.; Gan, T.J.; Kellum, J.A.; Plumb, J.; Mythen, M.G.; Grocott, M.P.W.; Edwards, M.R.; et al. Perioperative Quality Initiative consensus statement on intraoperative blood pressure, risk and outcomes for elective surgery. Br. J. Anaesth. 2019, 122, 563–574. [Google Scholar] [CrossRef]
- Evered, L.; Silbert, B.; Knopman, D.S.; Scott, D.A.; DeKosky, S.T.; Rasmussen, L.S.; Oh, E.S.; Crosby, G.; Berger, M.; Eckenhoff, R.G.; et al. Recommendations for the nomenclature of cognitive change associated with anaesthesia and surgery-2018. Br. J. Anaesth. 2018, 121, 1005–1012. [Google Scholar] [CrossRef]
- Evered, L.A.; Silbert, B.S. Postoperative Cognitive Dysfunction and Noncardiac Surgery. Anesth. Analg. 2018, 127, 496–505. [Google Scholar] [CrossRef]
- American Society of Psychiatrists. DSM-5 Criteria for Delirium. The Diagnostic and Statistical Manual of Mental Disorders (DSM-5); American Society of Psychiatrists: Washington, DC, USA, 2013. [Google Scholar]
- Inouye, S.K.; van Dyck, C.H.; Alessi, C.A.; Balkin, S.; Siegal, A.P.; Horwitz, R.I. Clarifying confusion: The confusion assessment method. A new method for detection of delirium. Ann. Intern. Med. 1990, 113, 941–948. [Google Scholar] [CrossRef]
- Salluh, J.I.; Wang, H.; Schneider, E.B.; Nagaraja, N.; Yenokyan, G.; Damluji, A.; Serafim, R.B.; Stevens, R.D. Outcome of delirium in critically ill patients: Systematic review and meta-analysis. BMJ 2015, 350, 2538. [Google Scholar] [CrossRef]
- Rengel, K.F.; Pandharipande, P.P.; Hughes, C.G. Postoperative delirium. Presse Med. 2018, 47, 53–64. [Google Scholar] [CrossRef]
- Kotekar, N.; Shenkar, A.; Nagaraj, R. Postoperative cognitive dysfunction—current preventive strategies. Clin. Interv. Aging. 2018, 13, 2267–2273. [Google Scholar] [CrossRef]
- Moller, J.T.; Cluitmans, P.; Rasmussen, L.S.; Houx, P.; Rasmussen, H.; Canet, J.; Rabbitt, P.; Jolles, J.; Cand Scient, K.L.; Hanning, C.D.; et al. Long-term postoperative cognitive dysfunction in the elderly ISPOCD1 study. ISPOCD investigators. International Study of Post-Operative Cognitive Dysfunction. Lancet. 1998, 351, 857–861. [Google Scholar] [CrossRef]
- Steinmetz, J.; Christensen, K.B.; Lund, T.; Lohse, N.; Rasmussen, L.S.; ISPOCD Group. Long-term consequences of postoperative cognitive dysfunction. Anesthesiology 2009, 110, 548–555. [Google Scholar] [CrossRef] [PubMed]
- Krenk, L.; Rasmussen, L.S.; Kehlet, H. New insights into the pathophysiology of postoperative cognitive dysfunction. Acta Anaesthesiol. Scand. 2010, 54, 951–956. [Google Scholar] [CrossRef] [PubMed]
- Kline, R.P.; Pirraglia, E.; Cheng, H.; De Santi, S.; Li, Y.; Haile, M.; de Leon, M.J.; Alex Bekker, M.D.; Alzheimer’s Disease Neuroimaging Initiative. Surgery and brain atrophy in cognitively normal elderly subjects and subjects diagnosed with mild cognitive impairment. Anesthesiology 2012, 116, 603–612. Anesthesiology 2012, 116, 603–612. [Google Scholar]
- Hudetz, J.A.; Patterson, K.M.; Byrne, A.J. A history of alcohol dependence increases the incidence and severity of postoperative cognitive dysfunction in cardiac surgical patients. Int. J. Environ. Res. Public Health. 2009, 6, 2725–2739. [Google Scholar] [CrossRef] [PubMed]
- Newman, S.; Stygall, J.; Hirani, S.; Shaefi, S.; Maze, M. Postoperative cognitive dysfunction after noncardiac surgery: A systematic review. Anesthesiology 2007, 106, 572–590. [Google Scholar] [CrossRef]
- Rundshagen, I. Postoperative cognitive dysfunction. Dtsch. Arztebl. Int. 2014, 111, 119–125. [Google Scholar] [CrossRef]
- Rossi, A.; Burkhart, C.; Dell-Kuster, S.; Pollock, B.G.; Strebel, S.P.; Monsch, A.U.; Kern, C.; Steiner, L.A. Serum Anticholinergic Activity and Postoperative Cognitive Dysfunction in Elderly Patients. Anesth Analg. 2014, 119, 947–955. [Google Scholar] [CrossRef]
- Luo, C.; Zou, W. Cerebral monitoring of anaesthesia on reducing cognitive dysfunction and postoperative delirium: A systematic review. J. Int. Med. Res. 2018, 46, 4100–4110. [Google Scholar] [CrossRef]
- Evered, L.; Scott, D.A.; Silbert, B.; Maruff, P. Postoperative cognitive dysfunction is independent of type of surgery and anesthetic. Anesth. Analg. 2011, 112, 1179–1185. [Google Scholar] [CrossRef]
- Puskas, F.; Grocott, H.P.; White, W.D.; Mathew, J.P.; Newman, M.F.; Bar-Yosef, S. Intraoperative hyperglycemia and cognitive decline after CABG. Ann. Thorac. Surg. 2007, 84, 1467–1473. [Google Scholar] [CrossRef] [PubMed]
- Bilotta, F.; Lauretta, M.P.; Borozdina, A.; Mizikov, V.M.; Rosa, G. Postoperative delirium: Risk factors, diagnosis and perioperative care. Minerva Anestesiol. 2013, 79, 1066–1076. [Google Scholar] [PubMed]
- Dasgupta, M.; Dumbrell, A.C. Preoperative risk assessment for delirium after noncardiac surgery: A systematic review. J. Am. Geriatr. Soc. 2006, 54, 1578–1589. [Google Scholar] [CrossRef] [PubMed]
- Pluta, M.P.; Dziech, M.; Czempik, P.F.; Szczepańska, A.J.; Krzych, Ł.J. Antipsychotic Drugs in Prevention of Postoperative Delirium-What Is Known in 2020? Int. J. Environ. Res. Public Health. 2020, 17, 6069. [Google Scholar] [CrossRef]
- Weiser, T.G.; Haynes, A.B.; Molina, G.; Lipsitz, S.R.; Esquivel, M.M.; Uribe-Leitz, T.; Fu, R.; Azad, T.; Chao, T.E.; Berry, W.R.; et al. Estimate of the global volume of surgery in 2012: An assessment supporting improved health outcomes. Lancet 2015, 27, 385. [Google Scholar] [CrossRef]
- Selwood, A.; Orrell, M. Long term cognitive dysfunction in older people after non-cardiac surgery. BMJ 2004, 328, 120–121. [Google Scholar] [CrossRef]
- Williams-Russo, P.; Sharrock, N.E.; Mattis, S.; Liguori, G.A.; Mancuso, C.; Peterson, M.G.; Hollenberg, J.; Ranawat, C.; Salvati, E.; Sculco, T. Randomized trial of hypotensive epidural anesthesia in older adults. Anesthesiology 1999, 91, 926–935. [Google Scholar] [CrossRef]
- Boos, G.L.; Soares, L.F.; Oliveira Filho, G.R. Disfunção cognitiva pós-operatória: Prevalência e fatores. Rev. Bras. Anestesiol. 2005, 55, 517–524. [Google Scholar] [CrossRef]
- Yocum, G.T.; Gaudet, J.G.; Teverbaugh, L.A.; Quest, D.O.; McCormick, P.C.; Connolly, E.S.; Heyer, E.J. Neurocognitive performance in hypertensive patients after spine surgery. Anesthesiology 2009, 110, 254–261. [Google Scholar] [CrossRef]
- Panda, N.B.; Mathew, P.; Narayana, Y.L.; Kohli, A.; Gandhi, K.; Kumar, P. Early Post Operative Cognitive Dysfunction (POCD) in middle aged hypertensive patients: A pilot study. J. NACC 2014, 1, 198. [Google Scholar] [CrossRef][Green Version]
- Heyer, E.J.; Mergeche, J.L.; Anastasian, Z.H.; Kim, M.; Mallon, K.A.; Connolly, E.S. Arterial blood pressure management during carotid endarterectomy and early cognitive dysfunction. Neurosurgery 2014, 74, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Neerland, B.E.; Krogseth, M.; Juliebø, V.; Hylen Ranhoff, A.; Engedal, K.; Frihagen, F.; Ræder, J.; Wyller, T.B.; Watne, L.O. Perioperative hemodynamics and risk for delirium and new onset dementia in hip fracture patients; A prospective follow-up study. PLoS ONE 2017, 12, 0180641. [Google Scholar] [CrossRef]
- Wang, H.; Gao, X.; Lv, N.; Tao, Q.; Yang, D.; Guo, J. Acute normovolemic hemodilution combined with controlled hypotension does not increase incidence of postoperative cognitive dysfunction in elderly spinal surgery patients. Int. J. Clin. Exp. Med. 2017, 10, 9526–9535. [Google Scholar]
- Ni, C.; Xu, T.; Li, N.; Tian, Y.; Han, Y.; Xue, Q.; Li, M.; Guo, X. Cerebral oxygen saturation after multiple perioperative influential factors predicts the occurrence of postoperative cognitive dysfunction. BMC Anesthesiol. 2015, 15, 156. [Google Scholar] [CrossRef] [PubMed]
- Sartcaoglu, F.; Celiker, V.; Basgul, E.; Yapakci, O.; Aypar, U. The effect of hypotensive anaesthesia on cognitive functions and recovery at endoscopic sinus surgery. Eur. J. Anaesthesiol. 2005, 22, 157–159. [Google Scholar] [CrossRef] [PubMed]
- Deiner, S.; Luo, X.; Silverstein, J.H.; Sano, M. Can Intraoperative Processed EEG Predict Postoperative Cognitive Dysfunction in the Elderly? Clin. Ther. 2015, 37, 2700–2705. [Google Scholar] [CrossRef] [PubMed]
- Chuan, A.; Short, T.G.; Peng, A.Z.Y.; Wen, S.Y.; Sun, A.X.; Ting, T.H.; Wan, A.S.; Pope, L.; Jaeger, M.; Aneman, A. Is cerebrovascular autoregulation associated with outcomes after major noncardiac surgery? A prospective observational pilot study. Acta Anaesthesiol. Scand. 2019, 63, 8–17. [Google Scholar] [CrossRef]
- Langer, T.; Santini, A.; Zadek, F.; Chiodi, M.; Pugni, P.; Cordolcini, V.; Bonanomi, B.; Rosini, F.; Marcucci, M.; Valenza, F.; et al. Intraoperative hypotension is not associated with postoperative cognitive dysfunction in elderly patients undergoing general anesthesia for surgery: Results of a randomized controlled pilot trial. J. Clin. Anesth. 2019, 52, 111–118. [Google Scholar] [CrossRef]
- Marcantonio, E.R.; Goldman, L.; Orav, E.J.; Cook, E.F.; Lee, T.H. The association of intraoperative factors with the development of postoperative delirium. Am. J. Med. 1998, 105, 380–384. [Google Scholar] [CrossRef]
- Tognoni, P.; Simonato, A.; Robutti, N.; Pisani, M.; Cataldi, A.; Monacelli, F.; Carmignani, G.; Odetti, P. Preoperative risk factors for postoperative delirium (POD) after urological surgery in the elderly. Arch. Gerontol. Geriatr. 2011, 52, 166–169. [Google Scholar] [CrossRef]
- Patti, R.; Saitta, M.; Cusumano, G.; Termine, G.; Di Vita, G. Risk factors for postoperative delirium after colorectal surgery for carcinoma. Eur. J. Oncol. Nurs. 2011, 15, 519–523. [Google Scholar] [CrossRef] [PubMed]
- Hirsch, J.; DePalma, G.; Tsai, T.T.; Sands, L.P.; Leung, J.M. Impact of intraoperative hypotension and blood pressure fluctuations on early postoperative delirium after non-cardiac surgery. Br. J. Anaesth. 2015, 115, 418–426. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Li, Z.; Yu, Y.; Li, B.; Shao, G.; Wang, Q. Risk factors contributing to postoperative delirium in geriatric patients postorthopedic surgery. Asia Pac. Psychiatry. 2015, 7, 375–382. [Google Scholar] [CrossRef] [PubMed]
- Wang, N.Y.; Hirao, A.; Sieber, F. Association between intraoperative blood pressure and postoperative delirium in elderly hip fracture patients. PLoS ONE 2015, 10, e0123892. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Sun, D.F.; Han, J.; Liu, R.; Wang, L.J.; Zhang, Z.Z. Effects of Intraoperative Hemodynamics on Incidence of Postoperative Delirium in Elderly Patients: A Retrospective Study. Med. Sci. Monit. 2016, 22, 1093–1100. [Google Scholar] [CrossRef]
- Van Grootven, B.; Detroyer, E.; Devriendt, E.; Sermon, A.; Deschodt, M.; Flamaing, J.; Dubois, C.; Milisen, K. Is preoperative state anxiety a risk factor for postoperative delirium among elderly hip fracture patients? Geriatr. Gerontol. Int. 2016, 16, 948–955. [Google Scholar] [CrossRef]
- Soh, S.; Shim, J.K.; Song, J.W.; Kim, K.N.; Noh, H.Y.; Kwak, Y.L. Postoperative Delirium in Elderly Patients Undergoing Major Spinal Surgery: Role of Cerebral Oximetry. J. Neurosurg. Anesthesiol. 2017, 29, 426–432. [Google Scholar] [CrossRef]
- Jiang, X.; Chen, D.; Lou, Y.; Li, Z. Risk factors for postoperative delirium after spine surgery in middle- and old-aged patients. Aging Clin. Exp. Res. 2017, 29, 1039–1044. [Google Scholar] [CrossRef]
- Guo, Z.; Liu, J.; Li, J.; Wang, X.; Guo, H.; Ma, P.; Su, X.; Li, P. Postoperative Delirium in Severely Burned Patients Undergoing Early Escharotomy: Incidence, Risk Factors, and Outcomes. J. Burn. Care Res. 2017, 38, 370–376. [Google Scholar] [CrossRef]
- Wang, Y.; Yu, H.; Qiao, H.; Li, C.; Chen, K.; Shen, X. Risk Factors and Incidence of Postoperative Delirium in Patients Undergoing Laryngectomy. Otolaryngol. Head Neck Surg. 2019, 161, 807–813. [Google Scholar] [CrossRef]
- Maheshwari, K.; Ahuja, S.; Khanna, A.K.; Mao, G.; Perez-Protto, S.; Farag, E.; Turan, A.; Kurz, A.; Sessler, D. Association Between Perioperative Hypotension and Delirium in Postoperative Critically Ill Patients: A Retrospective Cohort Analysis. Anesth. Analg. 2020, 130, 636–643. [Google Scholar] [CrossRef]
- Wang, X.; Feng, K.; Liu, H.; Liu, Y.; Ye, M.; Zhao, G.; Wang, T. Regional cerebral oxygen saturation and postoperative delirium in endovascular surgery: A prospective cohort study. Trials 2019, 20, 504. [Google Scholar] [CrossRef] [PubMed]
- Radinovic, K.; Markovic Denic, L.; Milan, Z.; Cirkovic, A.; Baralic, M.; Bumbasirevic, V. Impact of intraoperative blood pressure, blood pressure fluctuation, and pulse pressure on postoperative delirium in elderly patients with hip fracture: A prospective cohort study. Injury 2019, 50, 1558–1564. [Google Scholar] [CrossRef] [PubMed]
- Paulson, O.B.; Strandgaard, S.; Edvinsson, L. Cerebral autoregulation. Cerebrovasc. Brain Metab. Rev. 1990, 2, 161–192. [Google Scholar] [PubMed]
- Cipolla, M.J. The Cerebral Circulation; Morgan & Claypool Life Sciences: San Rafael, CA, USA, 2009. [Google Scholar]
- Bor-Seng-Shu Edson Kita William, S.; Figueiredo Eberval, G.; Paiva Wellingson, S.; Fonoff Erich, T.; Teixeira Manoel, J.; Panerai Ronney, B. Cerebral hemodynamics: Concepts of clinical importance. Arq. Neuro Psiquiatr. 2012, 70, 352–356. [Google Scholar]
- Kucewicz-Czech, E.; Krzych, Ł.J.; Ligowski, M. Perioperative haemodynamic optimisation in patients undergoing non-cardiac surgery—A position statement from the Cardiac and Thoracic Anaesthesia Section of the Polish Society of Anaesthesiology and Intensive Therapy. Part 2. Anaesthesiol. Intensive Ther. 2017, 49, 16–27. [Google Scholar] [CrossRef]
- Pang, Q.; Hendrickx, J.; Liu, H.L.; Poelaert, J. Contemporary perioperative haemodynamic monitoring. Anaesthesiol. Intensive Ther. 2019, 51, 147–158. [Google Scholar] [CrossRef]
- Kucewicz-Czech, E.; Krzych, Ł.J.; Ligowski, M. Perioperative haemodynamic optimisation in patients undergoing non-cardiac surgery—A position statement from the Cardiac and Thoracic Anaesthesia Section of the Polish Society of Anaesthesiology and Intensive Therapy. Part 1. Anaesthesiol. Intensive Ther. 2017, 49, 6–15. [Google Scholar] [CrossRef]
- Chan, M.T.V.; Hedrick, T.L.; Egan, T.D.; García, P.S.; Koch, S.; Purdon, P.L.; Ramsay, M.A.; Miller, T.E.; McEvoy, M.D.; Gan, T.J.; et al. American Society for Enhanced Recovery and Perioperative Quality Initiative Joint Consensus Statement on the Role of Neuromonitoring in Perioperative Outcomes: Electroencephalography. Anesth. Analg. 2020, 130, 1278–1291. [Google Scholar] [CrossRef]
- Pérez-Calatayud, Á.A.; Esper, R.C.; Gasca-Aldama, J.C.; Linarte-Basilio, M.E.; Anica-Malagon, E.D.; Briones-Garduño, J.C. Perioperative ultrasound neuromonitoring: Transcraneal Doppler and optic nerve. Cir. Cir. 2019, 87, 580–586. [Google Scholar]
- Yu, Y.; Zhang, K.; Zhang, L.; Zong, H.; Meng, L.; Han, R. Cerebral near-infrared spectroscopy (NIRS) for perioperative monitoring of brain oxygenation in children and adults. Cochrane Database Syst Rev. 2018, 1, 10947. [Google Scholar] [CrossRef] [PubMed]
- Krenk, L.; Rasmussen, L.S. Postoperative delirium and postoperative cognitive dysfunction in the elderly—What are the differences? Minerva Anestesiol. 2011, 77, 742–749. [Google Scholar] [PubMed]
- Gajniak, D.; Mendrala, K.; Gierek, D.; Krzych, Ł.J. Inter-arm differences in blood pressure among subjects with disseminated atherosclerosis scheduled for vascular surgery. Anaesthesiol Intensive Ther. 2018, 50, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Baron, R.; Binder, A.; Biniek, R.; Braune, S.; Buerkle, H.; Dall, P.; Demirakca, S.; Eckardt, R.; Eggers, V.; Eichler, I.; et al. Evidence and consensus based guideline for the management of delirium, analgesia, and sedation in intensive care medicine. Revision 2015 (DAS-Guideline 2015)—short version. Ger. Med. Sci. 2015, 13, 19. [Google Scholar]
- van Waes, J.A.; Van Klei, W.A.; Wijeysundera, D.N.; Van Wolfswinkel, L.; Lindsay, T.F.; Beattie, W.S. Association between Intraoperative Hypotension and Myocardial Injury after Vascular Surgery. Anesthesiology 2016, 124, 35–44. [Google Scholar] [CrossRef]
- Szczepańska, A.; Pluta, M.; Krzych, Ł. Clinical practice in intraoperative haemodynamic monitoring in Poland: A point prevalence study in 31 Polish hospitals. Anaesthesiol Intensive Ther. 2020, 52, 97–104. [Google Scholar] [CrossRef]
- Bocskai, T.; Kovács, M.; Szakács, Z.; Gede, N.; Hegyi, P.; Varga, G.; Pap, I.; Tóth, I.; Révész, P.; Szanyi, I.; et al. Is the bispectral index monitoring protective against postoperative cognitive decline? A systematic review with meta-analysis. PLoS ONE 2020, 15, e0229018. [Google Scholar] [CrossRef]
- Franklin, S.S.; Thijs, L.; Hansen, T.W.; O’Brien, E.; Staessen, J.A. White-coat hypertension: New insights from recent studies. Hypertension 2013, 62, 982–987. [Google Scholar] [CrossRef]
- Yokoyama, M.; Ueda, W.; Hirakawa, M.; Yamamoto, H. Hemodynamic effect of the prone position during anesthesia. Acta Anaesthesiol. Scand. 1991, 35, 741–744. [Google Scholar] [CrossRef]
- Critchley, L.A. Hypotension, subarachnoid block and the elderly patient. Anaesthesia 1996, 51, 1139–1143. [Google Scholar] [CrossRef]
| Patient Related | Procedure Related |
|---|---|
| Older age | Anesthesia induction with propofol |
| Male sex | Combined regional and general anesthesia |
| Low pre-induction systolic arterial blood pressure | Longer procedure |
| High American Society of Anesthesiologists (ASA) physical status (PS) class | Emergency procedure |
| Use of antihypertensive medications | Major procedure |
| Hypertension | Procedure in prone position |
| Preoperative Factors | Intraoperative Factors |
|---|---|
| Older age (>60 years old) | Excessive depth of anesthesia |
| Pre-existing cognitive impairment | Extensive surgery |
| History of alcohol abuse | Type of surgery |
| Low educational level | Re-operation |
| APOE4 genotype | Hyperglycemia |
| Cardiovascular diseases | Pulmonary complications |
| Use of anticholinergic agents |
| Risk Factors | Triggering Factors | |||
|---|---|---|---|---|
| Demography-Related | Comorbidities-Related | Surgery-Related | Anesthesia-Related | Postoperative Period-Related |
| Age > 70 | Cognitive status | Aortic aneurysm surgery | Premedication with benzodiazepines | Inadequate pain control/inadequate opioid analgesia/drug toxicity |
| Male gender | Anemia | Thoracic surgery | American Society of Anesthesiology Physical Class ≥ 3 | Sepsis |
| Education level | History of smoking | Abdominal surgery | Transfusions > 800 mL | Prolonged mechanical ventilation |
| Alcohol abuse | Hypertension | Hip replacement surgery | Fluid fasting time > 6 h | Hypoperfusion/Hypoxia |
| Malnutrition | Diabetes melitus | Medication (anticholinergic drugs, dezocine, meperidine) | ||
| Peripheral vascular disease | ||||
| Heart failure | ||||
| Polymorphism apoE | ||||
| Obstructive sleep apnea | ||||
| Prior postoperative delirium | ||||
| Visual/hearing impairment | ||||
| Functional impairment | ||||
| #1. PubMed search on 04/10/2020 using ‘MeSH terms’ and ‘best match’ strategy: |
| ((“Neurocognitive Disorders”[Mesh]) AND “Hypotension”[Mesh]) AND “Surgical Procedures, Operative”[Mesh]) (n = 47) OR ((“Intraoperative Period”[Mesh]) AND “Hypotension”[Mesh]) AND “Treatment Outcome”[Mesh]) (n = 15) OR ((“Perioperative Period”[Mesh]) AND “Hypotension”[Mesh]) AND “Outcome Assessment, Health Care”[Mesh]) (n = 38) OR ((“Treatment Outcome”[Mesh]) AND “Intraoperative Period”[Mesh]) AND “Hypotension”[Mesh]) (n = 15) OR ((“Intraoperative Period”[Mesh]) AND “Blood Pressure”[Mesh]) AND “Neurobehavioral Manifestations”[Mesh] (n = 7) |
| #2. PubMed search on 04/11/2020 using ‘key words’ and ‘best match’ strategy: |
| ((intraoperative hypotension) AND (postoperative period)) AND (delirium) (n = 13) OR (intraoperative hypotension) AND (cognitive defect) (n = 3) OR ((perioperative) AND (hypotension)) AND (cognitive function) (n = 20) OR ((intraoperative) AND (hypotension)) AND (cognitive impairment) (n = 23) OR (intraoperative blood pressure) AND (delirium) (n = 78) OR (intraoperative hypotension) AND (outcome) (n = 1486) OR ((surgery) AND (blood pressure)) AND (cognition) (n = 952) OR (postoperative cognitive dysfunction) AND (blood pressure) (n = 134) OR (hypotension) AND (postoperative cognitive dysfunction) (n = 75) |
| #3. Embase search on 04/15/2020 using ‘all fields’ algorithm: |
| (‘perioperative period’/exp OR ‘perioperative period’) AND (‘cognition’/exp OR cognition) AND (‘blood pressure’/exp OR ‘blood pressure’) (n = 187) OR ‘cognitive defect’ AND ‘intraoperative hypotension’ (n = 12) OR ‘hypotension’ AND ‘intraoperative period’ AND ‘cognition’ (n = 232) OR ‘hypotension’ AND ‘intraoperative period’ AND ‘disorders of higher cerebral function’ (n = 258) OR ‘treatment outcome’ AND ‘intraoperative hypotension’ (n = 157) OR ‘postoperative cognitive dysfunction’ AND ‘hypotension’ (n = 83) |
| Author | Design of the Study | Study Population | Other Factors Associated with POCD Established by the Study (Only with p < 0.05) | IOH Definition | POCD Screening Method | Effects |
|---|---|---|---|---|---|---|
| Moller et al.,1998 [12] | Observational, prospective | 1218 patients undergoing major abdominal, thoracic and orthopedic procedures with general anesthesia | Older age (OR 1.3) Second operation (OR 2.7) Respiratory Complications (OR 1.6) Longer duration of anesthesia (OR 1.1, p = 0.01) Infectious complication (OR 1.7, p = 0.04) | MAP drop for at least 60% from baseline for at least 30 min | Battery of neuropsychological tests 1 week and 3 months post-procedure | No effect |
| Wiliams-Russo et al., 1999 [28] | Randomized controlled | 235 patients undergoing orthopedic procedures with epidural anesthesia | Older age | Two arms of controlled IOH, with a MAP of 45–55 mmHg or 55–75 mmHg | 10 neuropsychologic tests after e.g., 1 week and after e.g., 4-months postoperatively | No effect |
| Boos et al., 2005 [29] | Observational, prospective | 55 patients undergoing orthopedic, vascular, urologic and general procedures with general anesthesia (51%) and epidural anesthesia (49%) | Pre-existing cognitive impairment, defined as preoperative MMSE score (for each point of MMSE) (OR 0.41, p = 0.0038) | Systolic BP decrease above 30% of a baseline value, lasting more than 5 min or needing vasopressor or inotropic support | MMSE before, 24 h after surgery and on postoperative days 3 and 7 | No effect |
| Yocum et al., 2009 [30] | Post-hoc cohort analysis | 48 patients undergoing spine surgery with general anesthesia | Duration of anesthesia | Not defined, BP was recorded as a fraction of baseline MAP | A battery of 5 neuro-psychometric tests on postoperative day 1 and 1 month after surgery | Hypertensive subjects with a significant drop of MAP had cognitive decline |
| Panda et al., 2016 [31] | Observational, prospective | 60 patients undergoing various non-cardiac procedures with general anesthesia | - | Not defined | Neuropsychological Test Battery on postoperative day 7 | Postoperative cognitive decline pattern differed in patients with lower minimal MAP |
| Heyer et al., 2014 [32] | Observational | 183 patients undergoing cross-clamp endarterectomy with general anesthesia | Low educational level (per year) (OR 1.16, p = 0.003) Diabetes mellitus (OR 2.73, p = 0.03) MAP kept ≥20% of baseline MAP (OR 0.18, p = 0.001) | Not defined | Self-developed battery of neuropsychometric tests applied preoperatively and 24 h postoperatively | Patients who had intraoperative MAP maintained ≥ 20% of baseline values exhibited a 82% lower risk of POCD |
| Neerland et al., 2017 [33] | Observational, prospective | 696 patients undergoing orthopedic procedures with general anesthesia (8%) and epidural anesthesia (92%) | Older age (OR 8.8, p = 0.006) ASA group ≥ III (OR 3.5, p = 0.038) Vasopressor used during surgery (OR 3.5, p = 0.027) Postoperative MAP >100 mmHg (OR 10.6, p = 0.027) Delirium during hospitalization (OR 6.7, p = 0.001) | Not defined | ICD-10 research criteria for dementia applied within 6 or 12 months after surgery | Patients with MAP >100 mmHg had over 10-times higher risk of dementia compared to individuals with MAP <80 mmHg |
| Wang H et al., 2017 [34] | Randomized controlled | 80 patients undergoing spine surgery with general anesthesia | - | Controlled hypotension was defined as a MAP not less than 55 mmHg, but there was no upper BP limit | MMSE preoperatively and on postoperative days 1 and 7 | The crude score in MMSE was significantly lower on a postoperative day ‘1’ and POCD occurred in 20% of subjects |
| Ni C et al., 2015 [35] | Observational prospective | 78 patients undergoing orthopedic procedures with epidural anesthesia | Older age (OR 1.2, p < 0.05) Lower average ScO2 after tourniquet deflation (OR 0.84, p < 0.05) | Not defined | Battery of neuropsychometric ISPOCD tests and MMSE, 1 day before surgery and on postoperative day 6 | In subjects who developed POCD, a statistically significant decrease in MAP was observed after anesthesia induction |
| Sartacaoglu et al., 2005 [36] | Randomized controlled | 46 patients undergoing endoscopic sinus surgery with general anesthesia | - | MAP 60–70 mmHg | MMSE and VADST after 2 and 24 h postoperatively | No effect |
| Deiner et al., 2015 [37] | Observational, retrospective | 77 patients undergoing major non-cardiac procedures with TIVA or volatile anesthesia | MMSE in no-POCD vs. POCD patients (median) = 29 vs. 27.5 (p = 0.02) | MAP <55 mmHg lasting for at least 5 min | Battery of neuro-psychometric tests, MMSE and CAM within 30 days before and 3 months after surgery | No effect |
| Chuan et al., 2019 [38] | Observational, prospective | 140 patients undergoing various non-cardiac procedures with | Older age Higher TOx | Not defined, MAP was maintained within a range of 75–90 mmHg | Cognitive domain of the Postoperative Quality of Recovery Scale preoperatively and on postoperative day 3 | Defective cerebrovascular autoregulation was associated with the failure of cognitive recovery |
| Langer et al., 2019 [39] | Randomized controlled | 101 patients undergoing various non-cardiac procedures with general anesthesia | - | Personalized treatment, study group (MAP within 90% of baseline) vs. control group | Neurocognitive evaluation performed by neuropsychiatrist with a battery of 7 tests preoperatively and 3 months after surgery | No effect |
| Author | Design | Study Population | Other Factors Associated with POD Established by the Study (Only with p < 0.05) | IOH Definition | POD Screening Method | Effect |
|---|---|---|---|---|---|---|
| Marcantonio et al., 1998 [40] | Observational, retrospective | 1341 patients; mixed major non-cardiac surgery | Age ≥ 70 year (OR 2.8) Cognitively impaired (OR 4.1) History of alcohol abuse (OR 2.8) Intrathoracic surgery (OR 3.0) Abdominal aneurysm surgery (OR = 9.1) Limited physical function (OR = 3.1) Lowest postoperative hematocrit ≤30% (OR = 1.7) | BP decline to 66% of preoperative baseline or <90 mm Hg requiring vasopressors or fluid resuscitation | CAM on postoperative days 2–5 or until the day before hospital discharge | No effect |
| Tognoni et al., 2010 [41] | Observational | 90 patients; urology | Drop in systolic BP <90 mmHg, requiring implementation of fluid therapy or infusion of catecholamines | CAM daily for the first postoperative week | IOH occurred more frequently in patients with POD | |
| Patti et al., 2011 [42] | Observational, prospective | 100 patients; colorectal surgery | Preoperative albumin concentration (OR = 0.26) Alcohol abuse (OR = 5.76) | Decrease in MAP <60 mmHg or the need for catecholamines | CAM twice a day from the first postoperative day to hospital discharge or death | IOH was an independent risk factor for POD |
| Hirsch et al., 2015 [43] | Observational, prospective | 540 patients; mixed major non-cardiac surgery | Age (OR 1.04) Gender (OR 1.71) Surgery duration (OR 1.24) | Absolute MAP drop <50 mmHg or relative decrease in MAP or systolic BP by more than 20, 30 or 40% from the baseline value | CAM preoperatively and on postoperative days 1–2 | No effect, however higher intraoperative BP variability was a risk factor of POD (OR 1.04) |
| Van Grootven et al., 2016 [47] | Observational, prospective | 86 patients; 15 orthopedic surgery (hip fracture) | Osteosynthesis surgery (OR 3.66) | Not defined | CAM, Delirium Index measured pre- and postoperatively (days 1, 3, 5, 8) | The lowest intraoperative diastolic BP was the protective factor for POD (OR = 0.92) |
| Wang J et al., 2015 [44] | Observational | 200 patients; orthopedic surgery | Age (R = 0.04) Anesthesia type (R = 0.15) Surgical type (R = −0.04) Intraoperative hypercapnia (R = 0.12) Preoperative affective dysfunction (R= −0.13) Postoperative sleep disorders (R = 0.12) Hyperlipidemia (R= −0.09) | Not defined | CAM once a day for 7 post-operative days | IOH was associated with POD (R = −0.11) |
| Wang NY et al., 2015 [45] | Randomized controlled | 103 patients; orthopedic surgery (hip fracture) | Age (OR = 1.09) Trial intervention (OR = 0.22) RBC transfusion (OR = 1.51) | Not defined | CAM on day ‘2’ post-surgery | Very high and very low MAP values were associated with significantly increased risk of POD (OR = 2.28) |
| Yang et al., 2016 [46] | Observational, retrospective | 480 patients, mixed non-cardiac elective surgery | Hypertension (OR = 2.83) Tachycardia (OR = 2.74) | Decrease in baseline MAP >30% | Clinical observation within one week post-surgery, POD confirmed by a neurologist using CAM | No effect |
| Soh et al., 2016 [48] | Observational, prospective | 109 patients; neurosurgery (major spinal surgery) | Decrease in MAP <80% of preoperative value or systolic BP <90 mmHg or absolute MAP <60 mmHg | CAM-ICU, ICDSC for 48 h after surgery | IOH episodes were more frequent in patients with POD | |
| Jiang et al., 2017 [49] | Observational, retrospective | 451 patients; neurosurgery (spine surgery) | Dezocine (OR = 6.68) | Drop in systolic BP <80 mmHg | Clinical assessment on preoperative day 1 and postoperative days 1, 2 and 3 | No effect |
| Neerland et al., 2017 [33] | Observational, prospective | 696 patients; orthopedic surgery (hip fracture) | NEADL <45 points (OR = 2.9) BMI <20 kg m−2 (OR = 4.5) ASA ≥ 3 (OR = 3.5) Blood transfusion ≥2 (OR = 3.4) | Not defined | CAM once a day preoperatively and until the fifth postoperative day (all) or until discharge (delirious patients), except for the weekends | No effect |
| Guo et al., 2017 [50] | Observational | 385 patients; escharotomy | Age >50 years (OR = 7.68) Drinking >3 per week (OR = 19.34) ASA >II (OR = 302.48) Preoperative time >2 days (OR = 14.66) Number of previous escharotomy >2 (OR = 24.69) Operation time >180 min (OR = 81.86) | MAP <55 mmHg | CAM once a day for 5 postoperative days | Patients with POD had more incidents of IOH (OR = 27.07) |
| Langer et al., 2019 [48] | Randomized controlled | 101 patients; mixed non-cardiac surgery | Not defined | CAM-ICU once a day for the first week post-operatively | No effect | |
| Wang Y et al., 2019 [51] | Observational, prospective | 323 patients; laryngectomy | Cancer stage (OR = 1.98) | BP lower than 70% of the baseline value lasting for >30 min | CAM once a day for 6 days post-operatively | IOH was more frequent in patients with POD |
| Maheshwari et al., 2019 [52] | Observational, retrospective | 1083 patients; non-cardiac surgery | MAP <65 mmHg | CAM-ICU twice a day while patient remained in the ICU | IOH was associated with POD (HR = 1.11) | |
| Wang X et al., 2019 [53] | Observational, prospective | 39 patients; neurosurgery (intracranial aneurysm) | rSO2 desaturation score (OR = 1.002) | Not defined | CAM (frequency not specified) | The maximal intraoperative decrease of SBP was significantly higher in patients with POD |
| Radinovic et al., 2019 [54] | Observational, prospective | 277 patients; orthopedic surgery | Not defined | CAM preoperatively and once a day for 7 post-operative days | Lower BP was observed in patients with POD |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Krzych, Ł.J.; Pluta, M.P.; Putowski, Z.; Czok, M. Investigating Association between Intraoperative Hypotension and Postoperative Neurocognitive Disorders in Non-Cardiac Surgery: A Comprehensive Review. J. Clin. Med. 2020, 9, 3183. https://doi.org/10.3390/jcm9103183
Krzych ŁJ, Pluta MP, Putowski Z, Czok M. Investigating Association between Intraoperative Hypotension and Postoperative Neurocognitive Disorders in Non-Cardiac Surgery: A Comprehensive Review. Journal of Clinical Medicine. 2020; 9(10):3183. https://doi.org/10.3390/jcm9103183
Chicago/Turabian StyleKrzych, Łukasz J., Michał P. Pluta, Zbigniew Putowski, and Marcelina Czok. 2020. "Investigating Association between Intraoperative Hypotension and Postoperative Neurocognitive Disorders in Non-Cardiac Surgery: A Comprehensive Review" Journal of Clinical Medicine 9, no. 10: 3183. https://doi.org/10.3390/jcm9103183
APA StyleKrzych, Ł. J., Pluta, M. P., Putowski, Z., & Czok, M. (2020). Investigating Association between Intraoperative Hypotension and Postoperative Neurocognitive Disorders in Non-Cardiac Surgery: A Comprehensive Review. Journal of Clinical Medicine, 9(10), 3183. https://doi.org/10.3390/jcm9103183







