Characteristics of US Medicare Beneficiaries with Chronic Cough vs. Non-Chronic Cough: 2011–2018
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Sources
2.2. Study Design and Cohort
2.3. Outcomes of Interest
2.4. Covariates
2.5. Statistical Analysis
2.6. Subgroup Analyses
3. Results
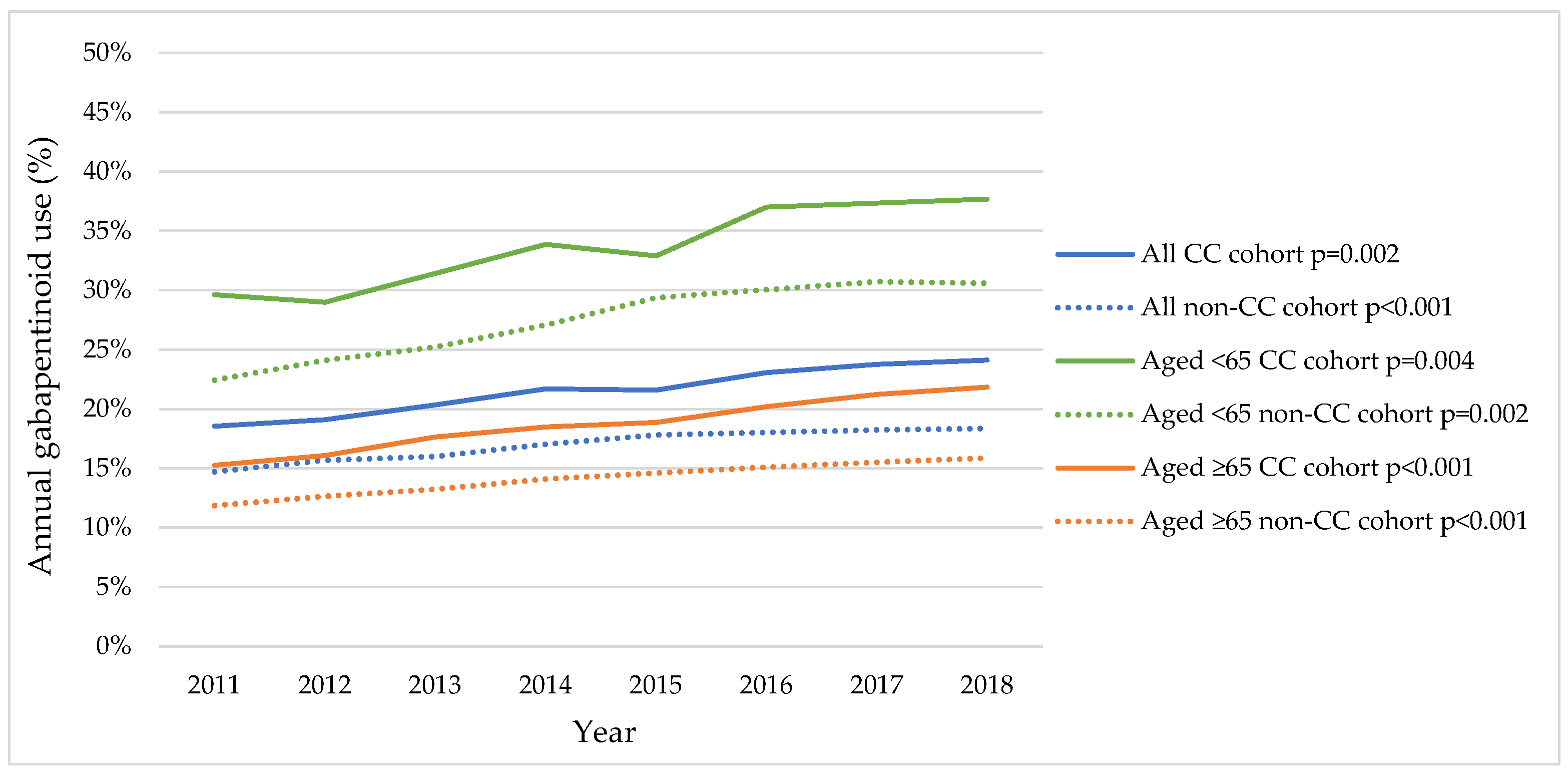
3.1. Trends in Annual Gabapentinoid Use from Repeated Cross-Sectional Analyses
3.2. GBTM Analysis: 2011–2018 Medicare Data
3.2.1. Characteristics of Patients with CC and Individuals without CC but with Any Respiratory Conditions Related to Cough
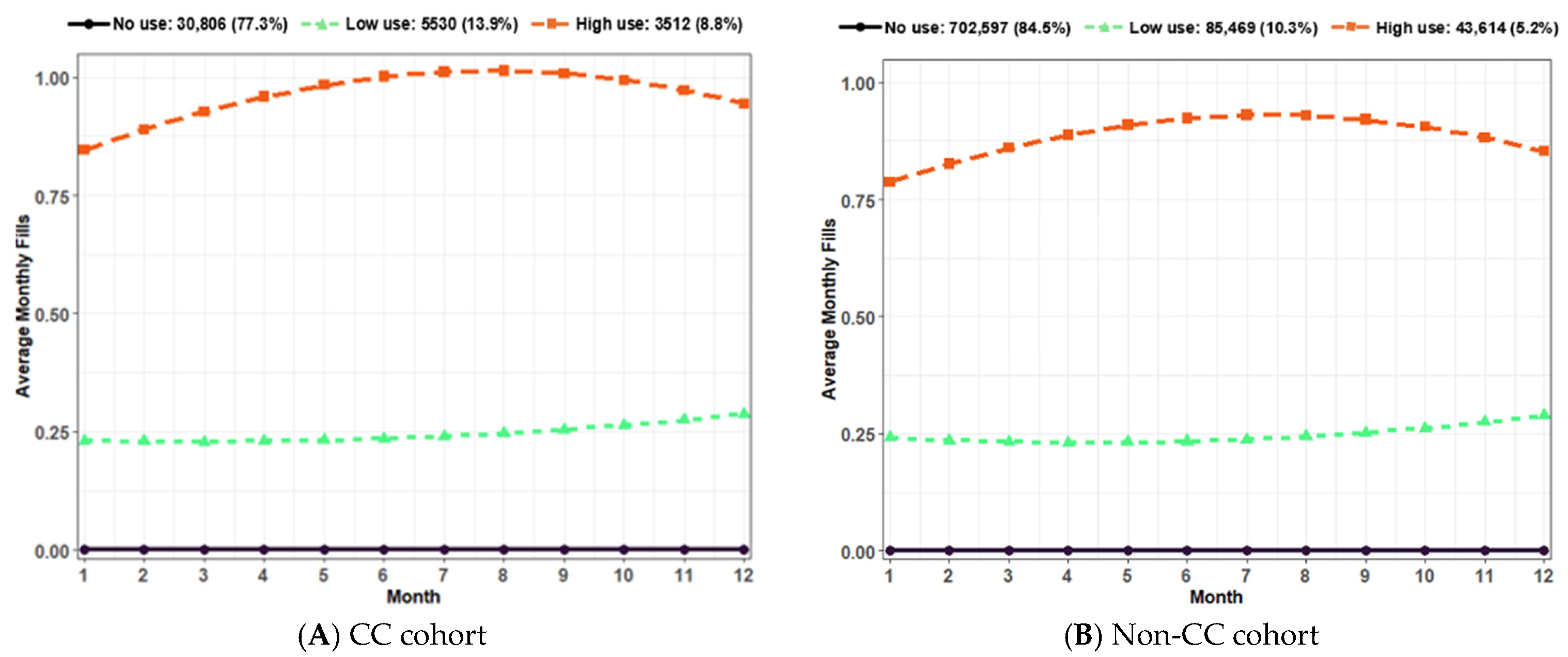
3.2.2. Gabapentinoid Utilization Trajectories
3.2.3. Characteristics of Patients with CC by Gabapentinoid Utilization Trajectories
3.2.4. Characteristics of Individuals without CC but with Any Respiratory Conditions Related to Cough by Gabapentinoid Utilization Trajectories
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Abozid, H.; Baxter, C.A.; Hartl, S.; Braun, E.; Salomonsson, S.; Breyer-Kohansal, R.; Breyer, M.K.; Wouters, E.F.M.; Agusti, A.; Burghuber, O.C. Distribution of chronic cough phenotypes in the general population: A cross-sectional analysis of the LEAD cohort in Austria. Respir. Med. 2022, 192, 106726. [Google Scholar] [CrossRef]
- Irwin, R.S.; French, C.L.; Chang, A.B.; Altman, K.W.; Panel, C.E.C. Classification of Cough as a Symptom in Adults and Management Algorithms: CHEST Guideline and Expert Panel Report. Chest 2018, 153, 196–209. [Google Scholar] [CrossRef]
- Song, W.J.; Chang, Y.S.; Faruqi, S.; Kim, J.Y.; Kang, M.G.; Kim, S.; Jo, E.J.; Kim, M.H.; Plevkova, J.; Park, H.W.; et al. The global epidemiology of chronic cough in adults: A systematic review and meta-analysis. Eur. Respir. J. 2015, 45, 1479–1481. [Google Scholar] [CrossRef]
- Meltzer, E.O.; Zeiger, R.S.; Dicpinigaitis, P.; Bernstein, J.A.; Oppenheimer, J.J.; Way, N.A.; Li, V.W.; Boggs, R.; Doane, M.J.; Urdaneta, E.; et al. Prevalence and Burden of Chronic Cough in the United States. J. Allergy Clin. Immunol. Pract. 2021, 9, 4037–4044.e32. [Google Scholar] [CrossRef] [PubMed]
- Arinze, J.T.; de Roos, E.W.; Karimi, L.; Verhamme, K.M.C.; Stricker, B.H.; Brusselle, G.G. Prevalence and incidence of, and risk factors for chronic cough in the adult population: The Rotterdam Study. ERJ Open Res. 2020, 6, 00300–02019. [Google Scholar] [CrossRef]
- Zeiger, R.S.; Xie, F.; Schatz, M.; Hong, B.D.; Weaver, J.P.; Bali, V.; Schelfhout, J.; Chen, W. Prevalence and Characteristics of Chronic Cough in Adults Identified by Administrative Data. Perm. J. 2020, 24, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Morice, A.H.; Jakes, A.D.; Faruqi, S.; Birring, S.S.; McGarvey, L.; Canning, B.; Smith, J.A.; Parker, S.M.; Chung, K.F.; Lai, K.; et al. A worldwide survey of chronic cough: A manifestation of enhanced somatosensory response. Eur. Respir. J. 2014, 44, 1149. [Google Scholar] [CrossRef] [PubMed]
- Chung, K.F.; Pavord, I.D. Prevalence, pathogenesis, and causes of chronic cough. Lancet 2008, 371, 1364–1374. [Google Scholar] [CrossRef]
- Gibson, P.; Wang, G.; McGarvey, L.; Vertigan, A.E.; Altman, K.W.; Birring, S.S. Treatment of Unexplained Chronic Cough: CHEST Guideline and Expert Panel Report. Chest 2016, 149, 27–44. [Google Scholar] [CrossRef]
- Morice, A.H.; Millqvist, E.; Belvisi, M.G.; Bieksiene, K.; Birring, S.S.; Chung, K.F.; Dal Negro, R.W.; Dicpinigaitis, P.; Kantar, A.; McGarvey, L.P.; et al. Expert opinion on the cough hypersensitivity syndrome in respiratory medicine. Eur. Respir. J. 2014, 44, 1132–1148. [Google Scholar] [CrossRef]
- Song, W.J.; Chang, Y.S.; Morice, A.H. Changing the paradigm for cough: Does ‘cough hypersensitivity’ aid our understanding? Asia Pac. Allergy 2014, 4, 3–13. [Google Scholar] [CrossRef] [PubMed]
- Arinze, J.T.; Verhamme, K.M.C.; Luik, A.I.; Stricker, B.; van Meurs, J.B.J.; Brusselle, G.G. The interrelatedness of chronic cough and chronic pain. Eur. Respir. J. 2021, 57, 2002651. [Google Scholar] [CrossRef] [PubMed]
- McGovern, A.E.; Short, K.R.; Kywe Moe, A.A.; Mazzone, S.B. Translational review: Neuroimmune mechanisms in cough and emerging therapeutic targets. J. Allergy Clin. Immunol. 2018, 142, 1392–1402. [Google Scholar] [CrossRef] [PubMed]
- Ryan, N.M.; Vertigan, A.E.; Birring, S.S. An update and systematic review on drug therapies for the treatment of refractory chronic cough. Expert. Opin. Pharmacother. 2018, 19, 687–711. [Google Scholar] [CrossRef]
- Morice, A.H.; Millqvist, E.; Bieksiene, K.; Birring, S.S.; Dicpinigaitis, P.; Domingo Ribas, C.; Hilton Boon, M.; Kantar, A.; Lai, K.; McGarvey, L.; et al. ERS guidelines on the diagnosis and treatment of chronic cough in adults and children. Eur. Respir. J. 2020, 55, 1901136. [Google Scholar] [CrossRef] [PubMed]
- U.S. Food & Drug Administration. FDA Warns about Serious Breathing Problems with Seizure and Nerve Pain Medicines Gabapentin (Neurontin, Gralise, Horizant) and Pregabalin (Lyrica, Lyrica CR). Available online: https://www.fda.gov/drugs/drug-safety-and-availability/fda-warns-about-serious-breathing-problems-seizure-and-nerve-pain-medicines-gabapentin-neurontin (accessed on 18 April 2024).
- Mues, K.E.; Liede, A.; Liu, J.; Wetmore, J.B.; Zaha, R.; Bradbury, B.D.; Collins, A.J.; Gilbertson, D.T. Use of the Medicare database in epidemiologic and health services research: A valuable source of real-world evidence on the older and disabled populations in the US. Clin. Epidemiol. 2017, 9, 267–277. [Google Scholar] [CrossRef]
- Katherine, K.S.; Lisa, N.B.; Rachel, A.L. U.S. Census Bureau, Current Population Reports, P60-281, Health Insurance Coverage in the United States: 2022; U.S. Government Publishing Office: Washington, DC, USA, 2023.
- U.S. Department of Health & Human Services. Area Health Resources Files. Available online: https://data.hrsa.gov/topics/health-workforce/ahrf (accessed on 12 April 2024).
- Yang, S.; Huang, S.; Hincapie-Castillo, J.M.; Ke, X.; Ding, H.; Schelfhout, J.; Sher, M.R.; Jones, B.; Wilson, D.L.; Lo-Ciganic, W.H. Patterns of Cough Medication Prescribing among Patients with Chronic Cough in Florida: 2012–2021. J. Clin. Med. 2023, 12, 6286. [Google Scholar] [CrossRef] [PubMed]
- CMS. Medicare Prescription Drug Benefit Manual Chapter 6—Part D Drugs and Formulary (Rev. 18, 01-15-16). Available online: https://www.cms.gov/medicare/prescription-drug-coverage/prescriptiondrugcovcontra/downloads/part-d-benefits-manual-chapter-6.pdf (accessed on 12 April 2024).
- Bali, V.; Weaver, J.; Turzhitsky, V.; Schelfhout, J.; Paudel, M.; Hulbert, E.; Peterson-Brandt, J.; Hertzberg, J.; Kelly, N.R.; Patel, R.H. Development of a Claims-Based Algorithm to Identify Patients with Chronic Cough. In TP65. TP065 Environmental Exposures and Lung Disease; American Thoracic Society International Conference Abstracts; American Thoracic Society: New York, NY, USA, 2021; p. A3146. [Google Scholar]
- Zhou, L.; Bhattacharjee, S.; Kwoh, C.K.; Tighe, P.J.; Malone, D.C.; Slack, M.; Wilson, D.L.; Brown, J.D.; Lo-Ciganic, W.H. Trends, Patient and Prescriber Characteristics in Gabapentinoid Use in a Sample of United States Ambulatory Care Visits from 2003 to 2016. J. Clin. Med. 2019, 9, 83. [Google Scholar] [CrossRef]
- Elixhauser, A.; Steiner, C.; Harris, D.R.; Coffey, R.M. Comorbidity measures for use with administrative data. Med. Care 1998, 36, 8–27. [Google Scholar] [CrossRef]
- Meals, D.W.; Spooner, J.; Dressing, S.A.; Harcum, J.B.; Statistical analysis for monotonic trends, Tech Notes 6, November 2011. Statistical analysis for monotonic trends, Tech Notes 6, November 2011. Developed for U.S. Environmental Protection Agency by Tetra Tech, Inc., Fairfax, VA, 23 p. Available online: https://www.epa.gov/sites/default/files/2016-05/documents/tech_notes_6_dec2013_trend.pdf (accessed on 1 August 2024).
- Nagin, D.S.; Odgers, C.L. Group-based trajectory modeling in clinical research. Annu. Rev. Clin. Psychol. 2010, 6, 109–138. [Google Scholar] [CrossRef]
- Bobby, L.J.; Daniel, S.N. Advances in Group-Based Trajectory Modeling and an SAS Procedure for Estimating Them. Sociol. Methods Res. 2007, 35, 542–571. [Google Scholar] [CrossRef]
- Daniel, S.N.; Bobby, L.J.; Valéria Lima, P.; Richard, E.T. Group-based multi-trajectory modeling. Stat. Methods Med. Res. 2016, 0962280216673085. [Google Scholar] [CrossRef]
- Song, W.-J.; Won, H.-K.; An, J.; Kang, S.-Y.; Jo, E.-J.; Chang, Y.-S.; Lee, B.-J.; Cho, S.-H. Chronic cough in the elderly. Pulm. Pharmacol. Ther. 2019, 56, 63–68. [Google Scholar] [CrossRef] [PubMed]
- By the American Geriatrics Society Beers Criteria Update Expert, P. American Geriatrics Society 2019 Updated AGS Beers Criteria(R) for Potentially Inappropriate Medication Use in Older Adults. J. Am. Geriatr. Soc. 2019, 67, 674–694. [Google Scholar] [CrossRef] [PubMed]
- Ryan, N.M.; Birring, S.S.; Gibson, P.G. Gabapentin for refractory chronic cough: A randomised, double-blind, placebo-controlled trial. Lancet 2012, 380, 1583–1589. [Google Scholar] [CrossRef] [PubMed]
- Vertigan, A.E.; Kapela, S.L.; Ryan, N.M.; Birring, S.S.; McElduff, P.; Gibson, P.G. Pregabalin and Speech Pathology Combination Therapy for Refractory Chronic Cough: A Randomized Controlled Trial. Chest 2016, 149, 639–648. [Google Scholar] [CrossRef] [PubMed]
- Gorfinkel, L.R.; Hasin, D.; Saxon, A.J.; Wall, M.; Martins, S.S.; Cerda, M.; Keyes, K.; Fink, D.S.; Keyhani, S.; Maynard, C.C.; et al. Trends in Prescriptions for Non-opioid Pain Medications Among U.S. Adults with Moderate or Severe Pain, 2014–2018. J. Pain. 2022, 23, 1187–1195. [Google Scholar] [CrossRef] [PubMed]
- Johansen, M.E.; Maust, D.T. Update to Gabapentinoid Use in the United States, 2002–2021. Ann. Fam. Med. 2024, 22, 45–49. [Google Scholar] [CrossRef]
- Johansen, M.E. Gabapentinoid Use in the United States 2002 Through 2015. JAMA Intern. Med. 2018, 178, 292–294. [Google Scholar] [CrossRef]
- Gabapentin, P.; Micromedex® 2.0, (Electronic Version). Greenwood Village (CO): Truven Health Analytics 2019. Available online: http://www.micromedexsolutions.com/ (accessed on 16 May 2024).
- Smith, R.V.; Lofwall, M.R.; Havens, J.R. Abuse and diversion of gabapentin among nonmedical prescription opioid users in Appalachian Kentucky. Am. J. Psychiatry 2015, 172, 487–488. [Google Scholar] [CrossRef]
- Smith, R.V.; Havens, J.R.; Walsh, S.L. Gabapentin misuse, abuse and diversion: A systematic review. Addiction 2016, 111, 1160–1174. [Google Scholar] [CrossRef] [PubMed]
- Radley, D.C.; Finkelstein, S.N.; Stafford, R.S. Off-label prescribing among office-based physicians. Arch. Intern. Med. 2006, 166, 1021–1026. [Google Scholar] [CrossRef]
- Buttram, M.E.; Kurtz, S.P.; Dart, R.C.; Margolin, Z.R. Law enforcement-derived data on gabapentin diversion and misuse, 2002–2015: Diversion rates and qualitative research findings. Pharmacoepidemiol. Drug Saf. 2017, 26, 1083–1086. [Google Scholar] [CrossRef]
- Bonnet, U.; Scherbaum, N. How addictive are gabapentin and pregabalin? A systematic review. Eur. Neuropsychopharmacol. 2017, 27, 1185–1215. [Google Scholar] [CrossRef] [PubMed]
- Goodman, C.W.; Brett, A.S. A Clinical Overview of Off-label Use of Gabapentinoid Drugs. JAMA Intern. Med. 2019, 179, 695–701. [Google Scholar] [CrossRef] [PubMed]
- Grauer, J.S.; Cramer, J.D. Association of State-Imposed Restrictions on Gabapentin with Changes in Prescribing in Medicare. J. Gen. Intern. Med. 2022, 37, 3630–3637. [Google Scholar] [CrossRef]
| Characteristic a | Pre-Index Period b | Post-index Period c | ||||
|---|---|---|---|---|---|---|
| CC Cohort | Non-CC Cohort | p-Value | CC Cohort | Non-CC Cohort | p-Value | |
| N | 39,848 | 831,680 | 39,848 | 831,680 | ||
| Demographics, % | ||||||
| Age in years, mean (SD) | 71.9 (12.5) | 70.1 (12.7) | <0.001 | 71.9 (12.5) | 70.1 (12.7) | <0.001 |
| Age ≥ 65 years | 82.5 | 81.7 | <0.001 | 82.5 | 81.7 | <0.001 |
| Female | 69.0 | 62.4 | <0.001 | 69.0 | 62.4 | <0.001 |
| Race/ethnicity | <0.001 | <0.001 | ||||
| Hispanic | 8.0 | 6.7 | 8.0 | 6.7 | ||
| Non-Hispanic White | 78.4 | 80.5 | 78.4 | 80.5 | ||
| Non-Hispanic Black | 8.6 | 8.0 | 8.6 | 8.0 | ||
| Others/multiple/unknown | 5.1 | 4.9 | 5.1 | 4.9 | ||
| Disability | 28.1 | 25.9 | <0.001 | 28.1 | 25.9 | <0.001 |
| LIS and dual Medicaid eligibility | <0.001 | <0.001 | ||||
| No LIS or dual eligibility | 61.9 | 68.4 | 61.9 | 68.4 | ||
| Only LIS or dual eligibility | 3.7 | 5.2 | 3.7 | 5.2 | ||
| Both LIS and dual eligibility | 34.4 | 26.4 | 34.4 | 26.4 | ||
| Residency in a metropolitan area | 84.2 | 81.3 | <0.001 | 84.2 | 81.3 | <0.001 |
| Healthcare utilization factors, % | ||||||
| Any hospitalization | 19.0 | 9.7 | <0.001 | 35.8 | 23.3 | <0.001 |
| Emergency department visits | <0.001 | <0.001 | ||||
| 0 | 66.9 | 79.6 | 43.7 | 57.6 | ||
| 1 | 6.4 | 3.7 | 4.1 | 4.0 | ||
| ≥2 | 26.7 | 16.7 | 52.2 | 39.4 | ||
| Outpatient visits | <0.001 | <0.001 | ||||
| 0 | 0.7 | 3.7 | 0.0 | 0.0 | ||
| 1 | 0.4 | 1.4 | 0.0 | 0.2 | ||
| 2–4 | 2.1 | 5.7 | 0.0 | 0.7 | ||
| ≥5 | 96.8 | 89.2 | 100.0 | 99.1 | ||
| Comorbidity index, mean (SD) | ||||||
| Elixhauser index d | 2.0 (1.9) | 1.4 (1.6) | <0.001 | 3.1 (2.4) | 2.1 (2.1) | <0.001 |
| No. of encounters with respiratory conditions related to cough, mean (SD) | ||||||
| No. visits with acute URTI | n/m | n/m | 2.3 (4.7) | 1.8 (3.4) | <0.001 | |
| No. visits with bronchitis | n/m | n/m | 4.1 (8.6) | 1.6 (4.5) | <0.001 | |
| No. visits with chronic URTD | n/m | n/m | 1.8 (5.7) | 0.7 (2.9) | <0.001 | |
| No. visits with cough | n/m | n/m | 0.6 (3.1) | 0.1 (1.0) | <0.001 | |
| No. visits with influenza | n/m | n/m | 0.6 (3.5) | 0.3 (2.6) | <0.001 | |
| No. visits with pneumonia | n/m | n/m | 5.5 (14.0) | 2.1 (8.1) | <0.001 | |
| No. visits with any respiratory conditions related to cough | n/m | n/m | 13.7 (18.7) | 6.2 (10.2) | <0.001 | |
| Respiratory comorbidities, % | ||||||
| Acute URTI | 22.2 | 0.0 | <0.001 | 45.0 | 52.6 | <0.001 |
| Allergic rhinitis | 17.6 | 6.4 | <0.001 | 37.8 | 16.2 | <0.001 |
| Asthma | 20.0 | 6.0 | <0.001 | 36.8 | 12.2 | <0.001 |
| Bronchiectasis | 2.8 | 0.4 | <0.001 | 8.2 | 1.0 | <0.001 |
| Bronchitis | 21.8 | 0.0 | <0.001 | 47.6 | 32.8 | <0.001 |
| Chronic URTD | 9.8 | 0.0 | <0.001 | 26.2 | 15.0 | <0.001 |
| COPD | 33.8 | 10.6 | <0.001 | 58.4 | 28.4 | <0.001 |
| Cough | 28.8 | 0.0 | <0.001 | 100.0 | 47.2 | <0.001 |
| Influenza | 1.0 | 0.0 | <0.001 | 6.4 | 4.6 | <0.001 |
| Obstructive sleep apnea | 12.8 | 7.8 | <0.001 | 20.2 | 11.6 | <0.001 |
| Pneumonia | 11.6 | 0.0 | <0.001 | 31.2 | 14.8 | <0.001 |
| Pulmonary fibrosis | 3.6 | 0.8 | <0.001 | 10.0 | 2.4 | <0.001 |
| UACS | 2.6 | 0.4 | <0.001 | 11.6 | 2.8 | <0.001 |
| Non-respiratory comorbidities, % | ||||||
| Anxiety disorders | 23.4 | 14.8 | <0.001 | 36.0 | 24.0 | <0.001 |
| Atrial fibrillation | 15.0 | 10.2 | <0.001 | 20.8 | 14.6 | <0.001 |
| Coronary artery disease | 29.4 | 21.0 | <0.001 | 40.0 | 29.8 | <0.001 |
| GERD | 34.0 | 18.4 | <0.001 | 59.2 | 31.8 | <0.001 |
| Heart failure | 16.0 | 7.6 | <0.001 | 26.4 | 14.2 | <0.001 |
| Hypertension | 71.8 | 61.4 | <0.001 | 83.2 | 75.0 | <0.001 |
| Mood disorders | 25.2 | 16.2 | <0.001 | 35.6 | 24.2 | <0.001 |
| Musculoskeletal conditions | 70.6 | 57.0 | <0.001 | 84.8 | 74.0 | <0.001 |
| Non-opioid substance use disorders | 5.8 | 4.6 | <0.001 | 12.2 | 10.6 | <0.001 |
| Obesity | 18.8 | 13.8 | <0.001 | 30.0 | 23.2 | <0.001 |
| Opioid use disorders | 2.2 | 1.4 | <0.001 | 3.6 | 2.4 | <0.001 |
| Other immune disorders | 6.6 | 4.0 | <0.001 | 9.8 | 6.0 | <0.001 |
| Peripheral vascular disease | 10.6 | 6.6 | <0.001 | 16.2 | 10.8 | <0.001 |
| Sleep disturbance | 9.6 | 5.4 | <0.001 | 16.8 | 10.0 | <0.001 |
| Stress incontinence | 4.4 | 2.6 | <0.001 | 7.2 | 4.4 | <0.001 |
| Vomiting | 2.4 | 1.0 | <0.001 | 6.0 | 2.8 | <0.001 |
| Procedures, % | ||||||
| Allergy radioallergosorbent testing | 16.0 | 10.4 | <0.001 | 36.6 | 20.8 | <0.001 |
| Barium swallow or upper GI imaging | 3.2 | 1.0 | <0.001 | 12.2 | 3.4 | <0.001 |
| Chest CT/MRI/ultrasound | 18.6 | 9.0 | <0.001 | 50.8 | 23.0 | <0.001 |
| Chest X-ray | 35.6 | 15.4 | <0.001 | 82.8 | 52.0 | <0.001 |
| Complete blood count | 53.2 | 44.8 | <0.001 | 88.2 | 78.6 | <0.001 |
| Esophageal endoscopy | 5.6 | 3.4 | <0.001 | 15.2 | 7.4 | <0.001 |
| Laryngoscopy | 2.8 | 0.6 | <0.001 | 14.0 | 3.4 | <0.001 |
| Nasal/sinus endoscopy | 10.0 | 4.6 | <0.001 | 23.4 | 12.0 | <0.001 |
| Sinus X-ray/CT | 18.6 | 12.6 | <0.001 | 39.0 | 26.4 | <0.001 |
| Spirometry | 18.6 | 5.2 | <0.001 | 58.8 | 19.8 | <0.001 |
| Potential cough medication | ||||||
| Gabapentinoids, % | 17.6 | 12.2 | <0.001 | 22.6 | 15.6 | <0.001 |
| Cardiovascular medications (oral), % | ||||||
| ACE inhibitors | 23.4 | 25.8 | <0.001 | 22.8 | 27.2 | <0.001 |
| Respiratory medications (oral or inhaled), % | ||||||
| H1 antihistamines | 6.6 | 3.4 | <0.001 | 10.6 | 5.8 | <0.001 |
| ICS monotherapy | 3.6 | 1.0 | <0.001 | 8.8 | 2.0 | <0.001 |
| ICS/LABA combination | 15.0 | 4.8 | <0.001 | 28.0 | 7.8 | <0.001 |
| LAMA monotherapy | 5.8 | 1.8 | <0.001 | 9.6 | 2.6 | <0.001 |
| Leukotriene modifiers | 13.8 | 4.0 | <0.001 | 25.6 | 6.8 | <0.001 |
| Nasal antihistamines | 3.0 | 0.8 | <0.001 | 8.2 | 2.2 | <0.001 |
| Nasal corticosteroids | 17.0 | 6.8 | <0.001 | 31.8 | 17.0 | <0.001 |
| Nasal SAMA | 2.2 | 0.6 | <0.001 | 6.2 | 1.8 | <0.001 |
| SABA singly inhaled | 20.6 | 6.4 | <0.001 | 40.8 | 18.6 | <0.001 |
| SABA/SAMA combination | 3.4 | 0.8 | <0.001 | 7.6 | 1.8 | <0.001 |
| Gastrointestinal (oral), % | ||||||
| H2 blockers | 10.2 | 5.8 | <0.001 | 17.6 | 8.6 | <0.001 |
| PPIs | 38.4 | 24.2 | <0.001 | 52.0 | 29.8 | <0.001 |
| Miscellaneous (oral), % | ||||||
| Corticosteroids | 28.4 | 10.2 | <0.001 | 55.0 | 30.8 | <0.001 |
| Potential respiratory antibiotics | 62.0 | 32.6 | <0.001 | 87.0 | 78.0 | <0.001 |
| Pain medications, psychotherapeutics, others (oral), % | ||||||
| Antidepressants | 40.0 | 29.4 | <0.001 | 45.6 | 34.0 | <0.001 |
| Antipsychotics | 9.6 | 7.0 | <0.001 | 11.4 | 8.4 | <0.001 |
| Benzodiazepines | 23.2 | 16.4 | <0.001 | 28.0 | 20.2 | <0.001 |
| Muscle relaxants | 10.2 | 7.4 | <0.001 | 15.0 | 11.2 | <0.001 |
| Non-benzodiazepine hypnotics | 6.2 | 4.8 | <0.001 | 7.6 | 5.8 | <0.001 |
| Opioid analgesics | 33.8 | 26.6 | <0.001 | 44.4 | 36.2 | <0.001 |
| Other anxiolytics | 2.4 | 1.6 | <0.001 | 3.4 | 2.2 | <0.001 |
| Other neuromodulators | 18.6 | 12.8 | <0.001 | 21.8 | 15.4 | <0.001 |
| Specialist visits, % | ||||||
| ≥1 visit to allergist | n/m | n/m | 6.2 | 1.2 | <0.001 | |
| ≥1 visit to gastroenterologist | n/m | n/m | 1.3 | 0.8 | <0.001 | |
| ≥1 visit to otolaryngologist/head and neck surgeon | n/m | n/m | 15.5 | 5.9 | <0.001 | |
| ≥1 visit to pulmonologist | n/m | n/m | 15.4 | 2.7 | <0.001 | |
| ≥1 visit to urologist | n/m | n/m | 8.7 | 6.9 | <0.001 | |
| Visited any specialists specified above | n/m | n/m | 37.1 | 15.9 | <0.001 | |
| Visited ≥ 2 different specialists specified above | n/m | n/m | 30.5 | 11.8 | <0.001 | |
| Visited ≥ 3 different specialists specified above | n/m | n/m | 25.8 | 9.2 | <0.001 | |
| All missing specialty information | n/m | n/m | 0.1 | 0.2 | <0.001 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yang, S.; Huang, S.; Hincapie-Castillo, J.M.; Ke, X.; Ding, H.; Sher, M.R.; Jones, B.; Wilson, D.L.; Lo-Ciganic, W.-H. Characteristics of US Medicare Beneficiaries with Chronic Cough vs. Non-Chronic Cough: 2011–2018. J. Clin. Med. 2024, 13, 4549. https://doi.org/10.3390/jcm13154549
Yang S, Huang S, Hincapie-Castillo JM, Ke X, Ding H, Sher MR, Jones B, Wilson DL, Lo-Ciganic W-H. Characteristics of US Medicare Beneficiaries with Chronic Cough vs. Non-Chronic Cough: 2011–2018. Journal of Clinical Medicine. 2024; 13(15):4549. https://doi.org/10.3390/jcm13154549
Chicago/Turabian StyleYang, Seonkyeong, Shu Huang, Juan M. Hincapie-Castillo, Xuehua Ke, Helen Ding, Mandel R. Sher, Bobby Jones, Debbie L. Wilson, and Wei-Hsuan Lo-Ciganic. 2024. "Characteristics of US Medicare Beneficiaries with Chronic Cough vs. Non-Chronic Cough: 2011–2018" Journal of Clinical Medicine 13, no. 15: 4549. https://doi.org/10.3390/jcm13154549
APA StyleYang, S., Huang, S., Hincapie-Castillo, J. M., Ke, X., Ding, H., Sher, M. R., Jones, B., Wilson, D. L., & Lo-Ciganic, W.-H. (2024). Characteristics of US Medicare Beneficiaries with Chronic Cough vs. Non-Chronic Cough: 2011–2018. Journal of Clinical Medicine, 13(15), 4549. https://doi.org/10.3390/jcm13154549








