Mechanical Insufflation-Exsufflation: Considerations for Improving Clinical Practice
Abstract
1. Introduction
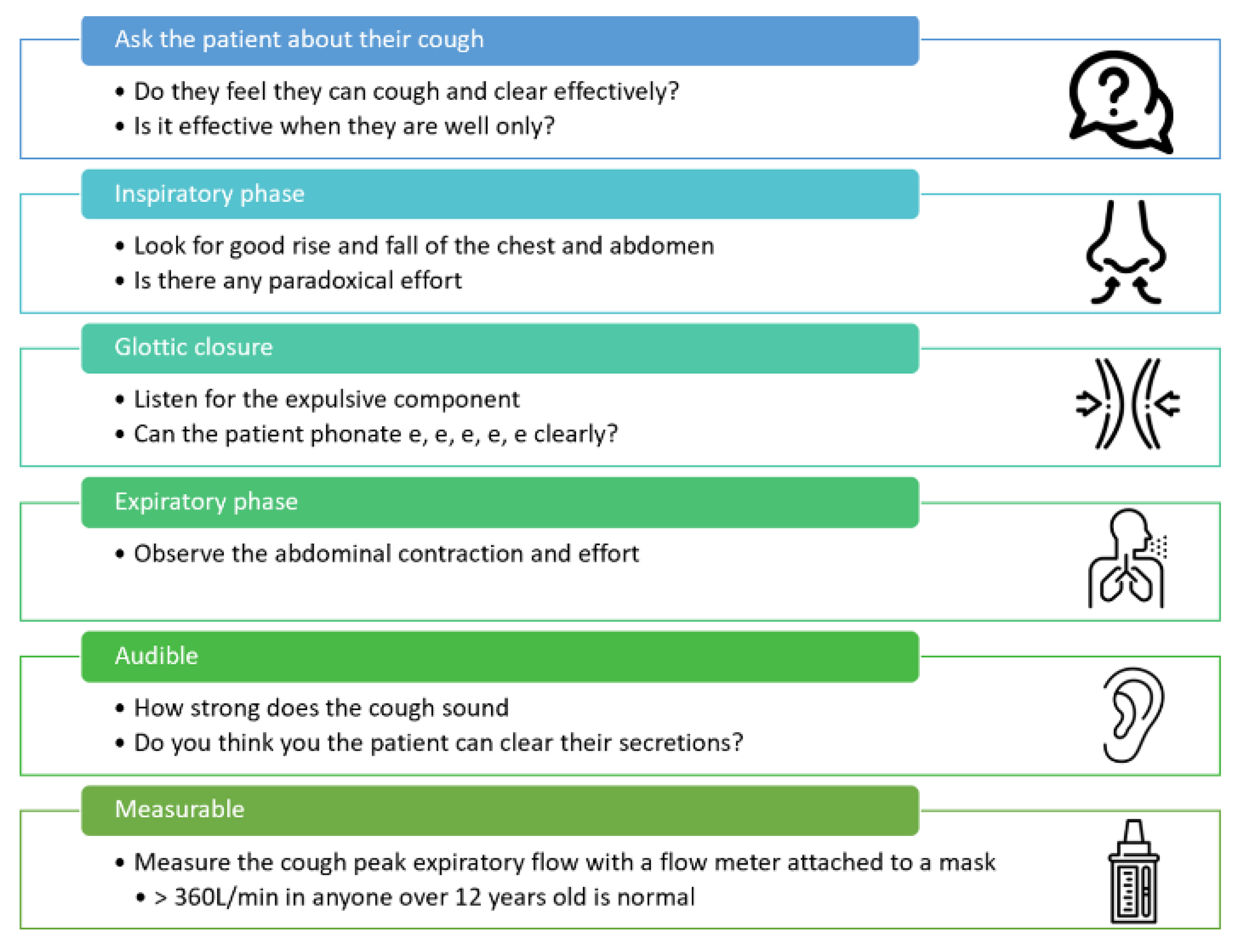
2. Cough Assessment
3. Cough Peak Flow Values
4. Proximal Airway Clearance Techniques
5. Mechanical Insufflation-Exsufflation Devices
- History of bullous emphysema, surgical emphysema, pneumothorax—undrained, known susceptibility to pneumothorax, care with patients who have had a pneumothorax, Pneumo-mediastinum, recent barotrauma, patients known to have cardiac instability should be monitored closely for pulse and oxygen saturation when using the MI-E device, tracheoesophageal fistula
- History of pneumothorax, recent lobectomy/pneumonectomy, cardiovascular insufficiency, acute abdominal distention, poor patient cooperation, pulmonary air leak
6. Patient Populations and Clinical Benefits of MI-E Devices
7. Barriers to the Use of MI-E
8. Effective MI-E Pressures
9. MI-E with the Addition of Oscillations
10. Adherence
11. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Gross, D.; Zidulka, A.; O’Brien, C.; Wight, D.; Fraser, R.; Rosenthal, L.; King, M. Peripheral mucociliary clearance with high-frequency chest wall compression. J. Appl. Physiol. 1985, 58, 1157–1163. [Google Scholar] [CrossRef]
- Warwick, W.J. Mechanisms of mucous transport. Eur. J. Respir. Dis. Suppl. 1983, 127, 162–167. [Google Scholar]
- Camner, P. Studies on the removal of inhaled particles from the lungs by voluntary coughing. Chest 1981, 80, 824–827. [Google Scholar]
- Lannefors, L.; Button, B.M.; McIlwaine, M. Physiotherapy in infants and young children with cystic fibrosis: Current practice and future developments. J. R. Soc. Med. 2004, 97 (Suppl. S44), 8–25. [Google Scholar] [PubMed]
- Chatwin, M.; Toussaint, M.; Gonçalves, M.R.; Sheers, N.; Mellies, U.; Gonzales-Bermejo, J.; Sancho, J.; Fauroux, B.; Andersen, T.; Hov, B.; et al. Airway clearance techniques in neuromuscular disorders: A state of the art review. Respir. Med. 2018, 136, 98–110. [Google Scholar] [CrossRef]
- Szeinberg, A.; Tabachnik, E.; Rashed, N.; McLaughlin, F.J.; England, S.; Bryan, C.A.; Levison, H. Cough Capacity in Patients with Muscular Dystrophy. Chest 1988, 94, 1232–1235. [Google Scholar] [CrossRef]
- Poponick, J.M.; Jacobs, I.; Supinski, G.; DiMARCO, A.F. Effect of Upper Respiratory Tract Infection in Patients with Neuromuscular Disease. Am. J. Respir. Crit. Care Med. 1997, 156, 659–664. [Google Scholar] [CrossRef]
- Toussaint, M.; Chatwin, M.; Gonzales, J.; Berlowitz, D.J. In Proceedings of the 228th ENMC International Workshop: Airway Cearance Techniques in Neuromuscular Disorders, Naarden, The Netherlands, 3–5 March 2017. Neuromuscul. Disord. 2018, 28, 289–298. [Google Scholar] [CrossRef]
- Bianchi, C.; Baiardi, P. Cough Peak Flows: Standard Values for Children and Adolescents. Am. J. Phys. Med. Rehabil. 2008, 87, 461–467. [Google Scholar] [CrossRef]
- Leith, D.E. The development of cough. Am. Rev. Respir. Dis. 1985, 131, S39–S42. [Google Scholar]
- Bach, J.R.; Saporito, L.R. Criteria for Extubation and Tracheostomy Tube Removal for Patients with Ventilatory Failure. A different approach to weaning. Chest 1996, 110, 1566–1571. [Google Scholar] [CrossRef]
- Bach, J.R.; Ishikawa, Y.; Kim, H. Prevention of Pulmonary Morbidity for Patients with Duchenne Muscular Dystrophy. Chest 1997, 112, 1024–1028. [Google Scholar] [CrossRef]
- Tzeng, A.C.; Bach, J.R. Prevention of Pulmonary Morbidity for Patients with Neuromuscular Disease. Chest 2000, 118, 1390–1396. [Google Scholar] [CrossRef]
- Lacombe, M.; Del Amo Castrillo, L.; Boré, A.; Chapeau, D.; Horvat, E.; Vaugier, I.; Lejaille, M.; Orlikowski, D.; Prigent, H.; Lofaso, F. Comparison of Three Cough-Augmentation Techniques in Neuromuscular Patients: Mechanical Insufflation Combined with Manually Assisted Cough, Insufflation-Exsufflation Alone and Insufflation-Exsufflation Combined with Manually Assisted Cough. Respiration 2014, 88, 215–222. [Google Scholar] [CrossRef]
- Medical, B. Clearway 2 Clinician’s Manual. In Breas Medical; Mölnlycke: Gothenburg, Sweden, 2022; Volume 009470 V9. [Google Scholar]
- Respironics, P. Cough Assist E70 User Manual; Philips Respironics: Murrysville, PA, USA, 2012. [Google Scholar]
- Swingwood, E.L.; Stilma, W.; Tume, L.N.; Cramp, F.; Voss, S.; Bewley, J.; Ntoumenopoulos, G.; Schultz, M.J.; Reimer, W.S.O.; Paulus, F.; et al. The Use of Mechanical Insufflation-Exsufflation in Invasively Ventilated Critically Ill Adults. Respir. Care 2022, 67, 1043–1057. [Google Scholar] [CrossRef] [PubMed]
- Mustfa, N.; Aiello, M.; Lyall, R.A.; Nikoletou, D.; Olivieri, D.; Leigh, P.N.; Davidson, A.C.; Polkey, M.I.; Moxham, J. Cough augmentation in amyotrophic lateral sclerosis. Neurology 2003, 61, 1285–1287. [Google Scholar] [CrossRef]
- Chatwin, M.; Ross, E.; Hart, N.; Nickol, A.H.; Polkey, M.I.; Simonds, A.K. Cough augmentation with mechanical insufflation/exsufflation in patients with neuromuscular weakness. Eur. Respir. J. 2003, 21, 502–508. [Google Scholar] [CrossRef]
- Winck, J.C.; Gonçalves, M.; Lourenço, M.C.C.; Viana, P.; Almeida, J.; Bach, J.R. Effects of Mechanical Insufflation-Exsufflation on Respiratory Parameters for Patients with Chronic Airway Secretion Encumbrance. Chest 2004, 126, 774–780. [Google Scholar] [CrossRef]
- Bach, J.R. Mechanical insufflation-exsufflation. Comparison of peak expiratory flows with manually assisted and unassisted coughing techniques. Chest 1993, 104, 1553–1562. [Google Scholar] [CrossRef]
- Chatwin, M.; Simonds, A.K. The addition of mechanical insufflation/exsufflation shortens airway-clearance sessions in neuromuscular patients with chest infection. Respir. Care 2009, 54, 1473–1479. [Google Scholar]
- Siriwat, R.; Deerojanawong, J.; Sritippayawan, S.; Hantragool, S.; Cheanprapai, P. Mechanical Insufflation-Exsufflation Versus Conventional Chest Physiotherapy in Children with Cerebral Palsy. Respir. Care 2017, 63, 187–193. [Google Scholar] [CrossRef]
- Vianello, A.; Corrado, A.; Arcaro, G.; Gallan, F.; Ori, C.; Minuzzo, M.; Bevilacqua, M. Mechanical Insufflation–Exsufflation Improves Outcomes for Neuromuscular Disease Patients with Respiratory Tract Infections. Am. J. Phys. Med. Rehabil. 2005, 84, 83–88; discussion 89–91. [Google Scholar] [CrossRef] [PubMed]
- Gonçalves, M.R.; Honrado, T.; Winck, J.C.; Paiva, J.A. Effects of mechanical insufflation-exsufflation in preventing respiratory failure after extubation: A randomized controlled trial. Crit. Care 2012, 16, R48. [Google Scholar] [CrossRef]
- De Camillis, M.L.F.; Savi, A.; Rosa, R.G.; Figueiredo, M.; Wickert, R.; Borges, L.G.A.; Galant, L.; Teixeira, C. Effects of Mechanical Insufflation-Exsufflation on Airway Mucus Clearance Among Mechanically Ventilated ICU Subjects. Respir. Care 2018, 63, 1471–1477. [Google Scholar] [CrossRef]
- Martínez-Alejos, R.; Martí, J.-D.; Bassi, G.L.; Gonzalez-Anton, D.; Pilar-Diaz, X.; Reginault, T.; Wibart, P.; Ntoumenopoulos, G.; Tronstad, O.; Gabarrus, A.; et al. Effects of Mechanical Insufflation-Exsufflation on Sputum Volume in Mechanically Ventilated Critically Ill Subjects. Respir. Care 2021, 66, 1371–1379. [Google Scholar] [CrossRef]
- Veldhoen, E.S.; Verweij-van den Oudenrijn, L.P.; Ros, L.A.; Hulzebos, E.H.; Papazova, D.A.; van der Ent, C.K.; van der Pol, L.W.; Nijman, J.; Wösten-van Asperen, R.M. Effect of mechanical insufflation-exsufflation in children with neuromuscular weakness. Pediatr. Pulmonol. 2020, 55, 510–513. [Google Scholar] [CrossRef]
- Khamankar, N.; Coan, G.; Weaver, B.; Mitchell, C.S. Associative Increases in Amyotrophic Lateral Sclerosis Survival Duration with Non-invasive Ventilation Initiation and Usage Protocols. Front. Neurol. 2018, 9, 578. [Google Scholar] [CrossRef]
- Legg, J.; Allen, J.-L.; Andrew, M.; Annesley, C.; Chatwin, M.; Crawford, H.; Elverson, J.; Forton, J.; Oulton, K.; Renton, K.; et al. Clinical Statement on the prevention and management of community-acquired pneumonia in people with learning disability. Thorax 2023, 78, s22–s52. [Google Scholar] [CrossRef]
- Sivasothy, P.; Brown, L.; Smith, I.E.; Shneerson, J.M. Effect of manually assisted cough and mechanical insufflation on cough flow of normal subjects, patients with chronic obstructive pulmonary disease (COPD), and patients with respiratory muscle weakness. Thorax 2001, 56, 438–444. [Google Scholar] [CrossRef]
- Hyun, S.E.; Lee, S.-M.; Shin, H.-I. Peak Expiratory Flow During Mechanical Insufflation-Exsufflation: Endotracheal Tube Versus Face Mask. Respir. Care 2021, 66, 1815–1823. [Google Scholar] [CrossRef]
- Sancho, J.; Servera, E.; Díaz, J.; Marín, J. Predictors of Ineffective Cough during a Chest Infection in Patients with Stable Amyotrophic Lateral Sclerosis. Am. J. Respir. Crit. Care Med. 2007, 175, 1266–1271. [Google Scholar] [CrossRef]
- Martí, J.-D.; Martínez-Alejos, R.; Pilar-Diaz, X.; Yang, H.; Pagliara, F.; Battaglini, D.; Meli, A.; Yang, M.; Bobi, J.; Rigol, M.; et al. Effects of Mechanical Insufflation-Exsufflation with Different Pressure Settings on Respiratory Mucus Displacement During Invasive Ventilation. Respir. Care 2022, 67, 1508–1516. [Google Scholar] [CrossRef]
- Veldhoen, E.S.; Vercoelen, F.; Ros, L.; Verweij-van den Oudenrijn, L.P.; Wösten-van Asperen, R.M.; Hulzebos, E.H.; Bartels, B.; Gaytant, M.A.; van der Ent, K.; Ludo van der Pol, W. Short-term effect of air stacking and mechanical insufflation–exsufflation on lung function in patients with neuromuscular diseases. Chronic Respir. Dis. 2022, 19, 14799731221094619. [Google Scholar] [CrossRef]
- Hov, B.; Andersen, T.; Toussaint, M.; Mikalsen, I.B.; Vollsæter, M.; Markussen, H.; Indrekvam, S.; Hovland, V. User-perceived impact of long-term mechanical assisted cough in paediatric neurodisability. Dev. Med. Child Neurol. 2023. Epub ahead of print. [Google Scholar] [CrossRef]
- Chatwin, M.; Bush, A.; Simonds, A.K. Outcome of goal-directed non-invasive ventilation and mechanical insufflation/exsufflation in spinal muscular atrophy type I. Arch. Dis. Child. 2010, 96, 426–432. [Google Scholar] [CrossRef]
- Garstang, S.V.; Kirshblum, S.C.; Wood, K.E. Patient Preference for ln-Exsufflation for Secretion Management with Spinal Cord Injury. J. Spinal Cord Med. 2000, 23, 80–85. [Google Scholar] [CrossRef]
- Saitoh, Y.; Miyazaki, M.; Arai, N.; Takahashi, Y. Pneumomediastinum while using mechanical insufflation-exsufflation after recovery from riluzole-induced interstitial lung disease. eNeurologicalSci 2021, 22, 100326. [Google Scholar] [CrossRef]
- Suri, P.; Burns, S.P.; Bach, J.R. Pneumothorax Associated with Mechanical Insufflation–Exsufflation and Related Factors. Am. J. Phys. Med. Rehabil. 2008, 87, 951–955. [Google Scholar] [CrossRef]
- Bach, J.R. Update and perspective on noninvasive respiratory muscle aids. Part 2: The expiratory aids. Chest 1994, 105, 1538–1544. [Google Scholar] [CrossRef]
- Miske, L.J.; Hickey, E.M.; Kolb, S.M.; Weiner, D.; Panitch, H.B. Use of the Mechanical In-Exsufflator in Pediatric Patients with Neuromuscular Disease and Impaired Cough. Chest 2004, 125, 1406–1412. [Google Scholar] [CrossRef]
- Andersen, T.; Sandnes, A.; Brekka, A.K.; Hilland, M.; Clemm, H.; Fondenes, O.; Tysnes, O.-B.; Heimdal, J.-H.; Halvorsen, T.; Vollsæter, M.; et al. Laryngeal response patterns influence the efficacy of mechanical assisted cough in amyotrophic lateral sclerosis. Thorax 2017, 72, 221–229. [Google Scholar] [CrossRef]
- Andersen, T.M.; Hov, B.; Halvorsen, T.; Røksund, O.D.; Vollsæter, M. Upper Airway Assessment and Responses During Mechanically Assisted Cough. Respir. Care 2021, 66, 1196–1213. [Google Scholar] [CrossRef]
- Sancho, J.; Servera, E.; Díaz, J.; Marín, J. Efficacy of Mechanical Insufflation-Exsufflation in Medically Stable Patients with Amyotrophic Lateral Sclerosis. Chest 2004, 125, 1400–1405. [Google Scholar] [CrossRef] [PubMed]
- Mahede, T.; Davis, G.; Rutkay, A.; Baxendale, S.; Sun, W.; Dawkins, H.J.; Molster, C.; Graham, C.E. Use of mechanical airway clearance devices in the home by people with neuromuscular disorders: Effects on health service use and lifestyle benefits. Orphanet J. Rare Dis. 2015, 10, 54. [Google Scholar] [CrossRef]
- Rose, L.; McKim, D.; Leasa, D.; Nonoyama, M.; Tandon, A.; Kaminska, M.; O’Connell, C.; Loewen, A.; Connolly, B.; Murphy, P.; et al. Monitoring Cough Effectiveness and Use of Airway Clearance Strategies: A Canadian and UK Survey. Respir. Care 2018, 63, 1506–1513. [Google Scholar] [CrossRef] [PubMed]
- Khamiees, M.; Raju, P.; DeGirolamo, A.; Amoateng-Adjepong, Y.; Manthous, C.A. Predictors of Extubation Outcome in Patients Who Have Successfully Completed a Spontaneous Breathing Trial. Chest 2001, 120, 1262–1270. [Google Scholar] [CrossRef]
- Stilma, W.; van der Hoeven, S.; Reimer, W.S.O.; Schultz, M.; Rose, L.; Paulus, F. Airway Care Interventions for Invasively Ventilated Critically Ill Adults—A Dutch National Survey. J. Clin. Med. 2021, 10, 3381. [Google Scholar] [CrossRef]
- Swingwood, E.; Tume, L.; Cramp, F. A survey examining the use of mechanical insufflation-exsufflation on adult intensive care units across the UK. J. Intensiv. Care Soc. 2020, 21, 283–289. [Google Scholar] [CrossRef]
- Bach, J.R. Amyotrophic lateral sclerosis: Predictors for prolongation of life by noninvasive respiratory aids. Chest 2002, 122, 92–98. [Google Scholar] [CrossRef]
- Gómez-Merino, E.; Sancho, J.; Marín, J.; Servera, E.; Blasco, M.L.; Belda, F.J.; Castro, C.; Bach, J.R. Mechanical insufflation-exsufflation: Pressure, volume, and flow relationships and the adequacy of the manufacturer’s guidelines. Am. J. Phys. Med. Rehabil. 2002, 81, 579–583. [Google Scholar] [CrossRef]
- Crew, J.D.; Svircev, J.N.; Burns, S.P. Mechanical Insufflation-Exsufflation Device Prescription for Outpatients with Tetraplegia. J. Spinal Cord Med. 2010, 33, 128–134. [Google Scholar] [CrossRef] [PubMed]
- Fauroux, B.; Guillemot, N.; Aubertin, G.; Nathan, N.; Labit, A.; Clément, A.; Lofaso, F. Physiologic Benefits of Mechanical Insufflation-Exsufflation in Children with Neuromuscular Diseases. Chest 2008, 133, 161–168. [Google Scholar] [CrossRef]
- Sancho, J.; Servera, E.; Marín, J.; Vergara, P.; Belda, F.J.; Bach, J.R. Effect of Lung Mechanics on Mechanically Assisted Flows and Volumes. Am. J. Phys. Med. Rehabil. 2004, 83, 698–703. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.M.; Choi, W.A.; Won, Y.H.; Kang, S.-W. A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness. Yonsei Med. J. 2016, 57, 1488–1493. [Google Scholar] [CrossRef]
- Chatwin, M.; Simonds, A.K. Long-Term Mechanical Insufflation-Exsufflation Cough Assistance in Neuromuscular Disease: Patterns of Use and Lessons for Application. Respir. Care 2020, 65, 135–143. [Google Scholar] [CrossRef]
- Lalmolda, C.; Prados, H.; Mateu, G.; Noray, M.; Pomares, X.; Luján, M. Titration of Mechanical Insufflation-Exsufflation Optimal Pressure Combinations in Neuromuscular Diseases by Flow/Pressure Waveform Analysis. Arch. Bronconeumol. 2019, 55, 246–251. [Google Scholar] [CrossRef]
- Hov, B.; Andersen, T.; Hovland, V.; Toussaint, M. The clinical use of mechanical insufflation-exsufflation in children with neuromuscular disorders in Europe. Paediatr. Respir. Rev. 2018, 27, 69–73. [Google Scholar] [CrossRef]
- Hov, B.; Andersen, T.; Toussaint, M.; Fondenes, O.; Carlsen, K.C.L.; Hovland, V. Optimizing expiratory flows during mechanical cough in a pediatric neuromuscular lung model. Pediatr. Pulmonol. 2020, 55, 433–440. [Google Scholar] [CrossRef]
- Mellies, U.; Goebel, C. Optimum Insufflation Capacity and Peak Cough Flow in Neuromuscular Disorders. Ann. Am. Thorac. Soc. 2014, 11, 1560–1568. [Google Scholar] [CrossRef]
- Sancho, J.; Ferrer, S.; Bures, E.; Fernandez-Presa, L.; Bañuls, P.; Gonzalez, M.C.; Signes-Costa, J. Waveforms Analysis in Patients with Amyotrophic Lateral Sclerosis for Enhanced Efficacy of Mechanically Assisted Coughing. Respir. Care 2022, 67, 1226–1235. [Google Scholar] [CrossRef]
- Volpe, M.S.; Naves, J.M.; Ribeiro, G.G.; Ruas, G.; Amato, M.B.P. Airway Clearance with an Optimized Mechanical Insufflation-Exsufflation Maneuver. Respir. Care 2018, 63, 1214–1222. [Google Scholar] [CrossRef] [PubMed]
- Lacombe, M.; Boré, A.; Castrillo, L.D.A.; Boussaïd, G.; Falaize, L.; Vlachos, E.; Orlikowski, D.; Prigent, H.; Lofaso, F. Peak Cough Flow Fails to Detect Upper Airway Collapse During Negative Pressure Titration for Cough-Assist. Arch. Phys. Med. Rehabil. 2019, 100, 2346–2353. [Google Scholar] [CrossRef]
- King, M.; Phillips, D.M.; Gross, D.; Vartian, V.; Chang, H.K.; Zidulka, A. Enhanced Tracheal Mucus Clearance with High Frequency Chest Wall Compression. Am. Rev. Respir. Dis. 1983, 128, 511–515. [Google Scholar] [CrossRef]
- Sancho, J.; Burés, E.; Ferrer, S.; Bondía, E.; Servera, E. Usefulness of Oscillations Added to Mechanical In-Exsufflation in Amyotrophic Lateral Sclerosis. Respir. Care 2019, 65, 596–602. [Google Scholar] [CrossRef]
- Sancho, J.; Burés, E.; Ferrer, S.; Lahosa, C.; Signes-Costa, J.; Servera, E. Mechanical Insufflation-Exsufflation with Oscillations in Amyotrophic Lateral Sclerosis with Home Ventilation via Tracheostomy. Respir. Care 2020, 66, 378–383. [Google Scholar] [CrossRef]
- Sancho, J.; Bures, E.; de La Asunción, S.; Servera, E. Effect of High-Frequency Oscillations on Cough Peak Flows Generated by Mechanical In-Exsufflation in Medically Stable Subjects with Amyotrophic Lateral Sclerosis. Respir. Care 2016, 61, 1051–1058. [Google Scholar] [CrossRef]
- Bach, J.R.; Niranjan, V.; Weaver, B. Spinal muscular atrophy type 1: A noninvasive respiratory management approach. Chest 2000, 117, 1100–1105. [Google Scholar] [CrossRef]
- Mitropoulou, G.; Heinzer, R.; Janssens, J.-P.; von Garnier, C.; Prella, M. Home Use of Mechanical Insufflation/Exsufflation in Adult Patients in Western Switzerland. Respiration 2023, 1–10. [Google Scholar] [CrossRef]


| Physiological Benefits of MI-E | Reference |
|---|---|
| Increased cough peak flow | [18,19,20,21,31,32,33] |
| Increased secretion clearance | [26,34] |
| Improvements in lung compliance | [26,34] |
| Short term improvements in forced vital capacity | [35] |
| Clinical benefits | |
| Decreased hospital admissions, time in hospital or Physicians visits | [36] |
| Decrease treatment failure | [24,25] |
| Decreased treatment time | [22,23] |
| Increased survival (in conjunction with ventilatory support) | [29,37] |
| Patient preference for MI-E over suction | [38] |
| Complications to MI-E | |
| Pneumothorax, pneumomediastinum | [39] |
| Abdominal distention, nausea, bloating | [40] |
| Bradycardia, tachycardia | [41] |
| Thoracic wall discomfort | [42] |
| Upper airway collapse | [43,44,45] |
| Quality of life benefits | |
| Perceived improvement in overall respiratory health | [46] |
| Disadvantage was the size of the devices | [46] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chatwin, M.; Wakeman, R.H. Mechanical Insufflation-Exsufflation: Considerations for Improving Clinical Practice. J. Clin. Med. 2023, 12, 2626. https://doi.org/10.3390/jcm12072626
Chatwin M, Wakeman RH. Mechanical Insufflation-Exsufflation: Considerations for Improving Clinical Practice. Journal of Clinical Medicine. 2023; 12(7):2626. https://doi.org/10.3390/jcm12072626
Chicago/Turabian StyleChatwin, Michelle, and Ruth Helen Wakeman. 2023. "Mechanical Insufflation-Exsufflation: Considerations for Improving Clinical Practice" Journal of Clinical Medicine 12, no. 7: 2626. https://doi.org/10.3390/jcm12072626
APA StyleChatwin, M., & Wakeman, R. H. (2023). Mechanical Insufflation-Exsufflation: Considerations for Improving Clinical Practice. Journal of Clinical Medicine, 12(7), 2626. https://doi.org/10.3390/jcm12072626






