Long-Term Outcome of Bypass Surgery versus Endovascular Revascularization in Long Femoropopliteal Lesions
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Revascularization Protocol
2.3. Statistics
3. Results
3.1. Peri- and Postoperative Results
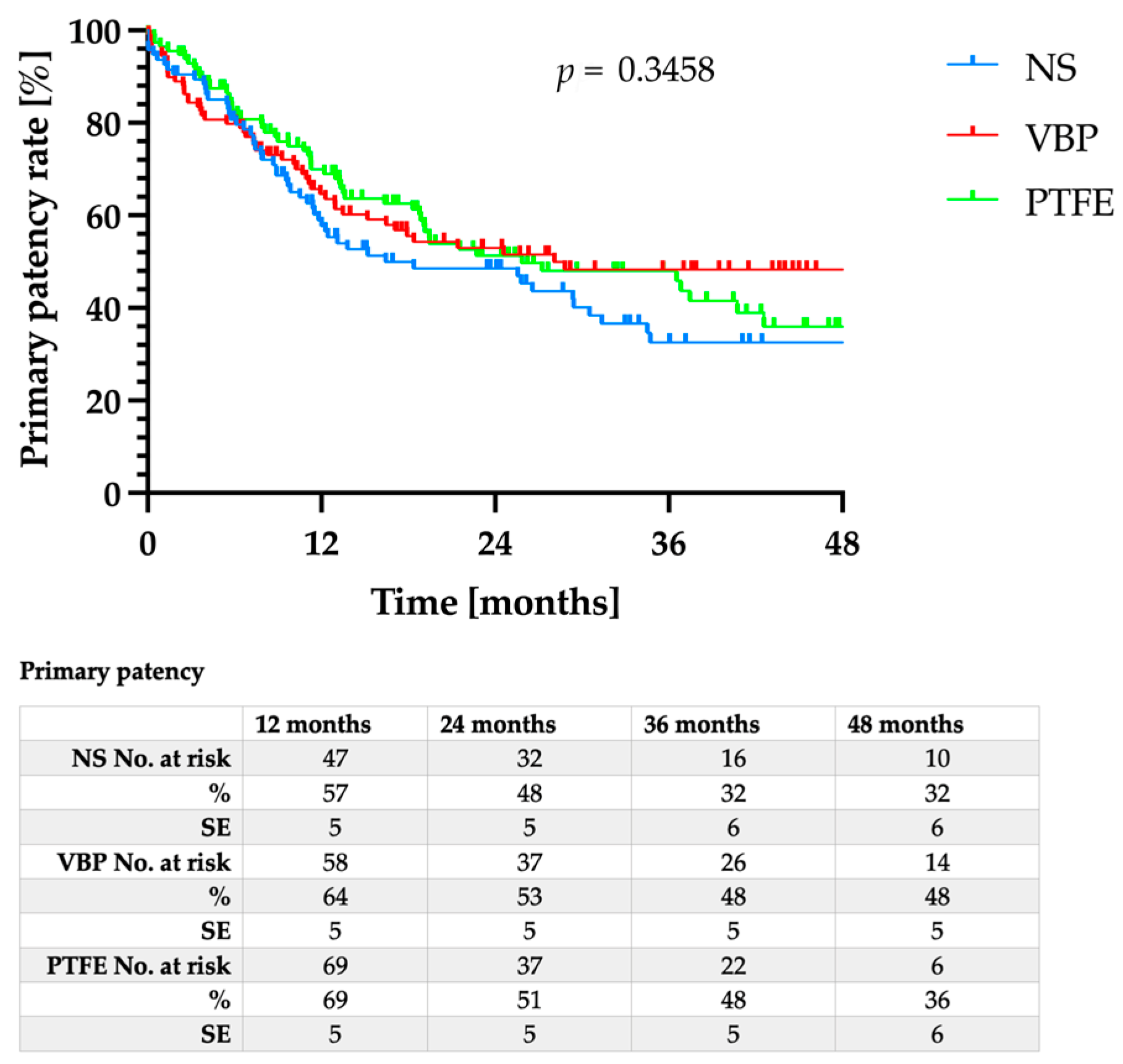
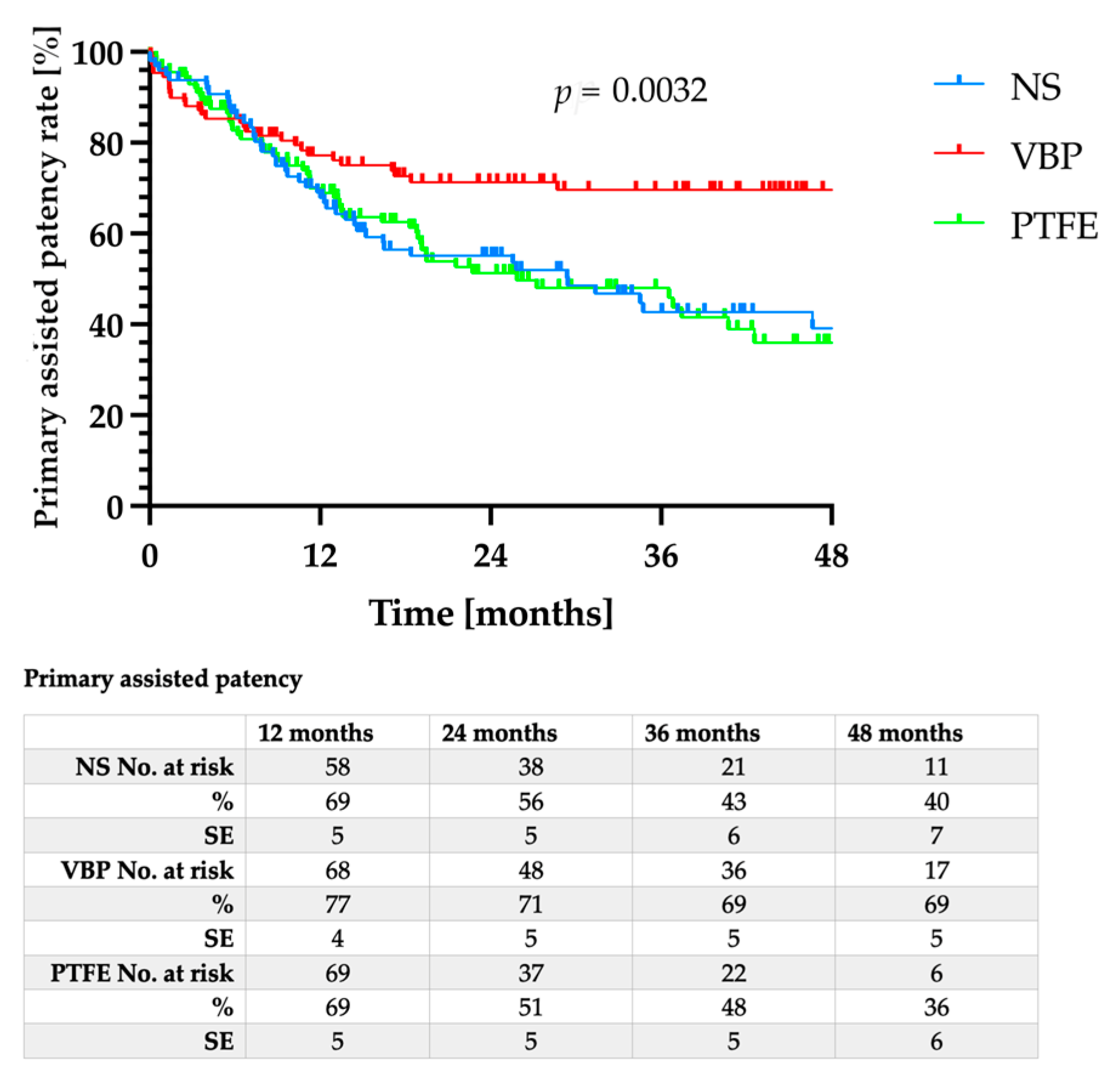
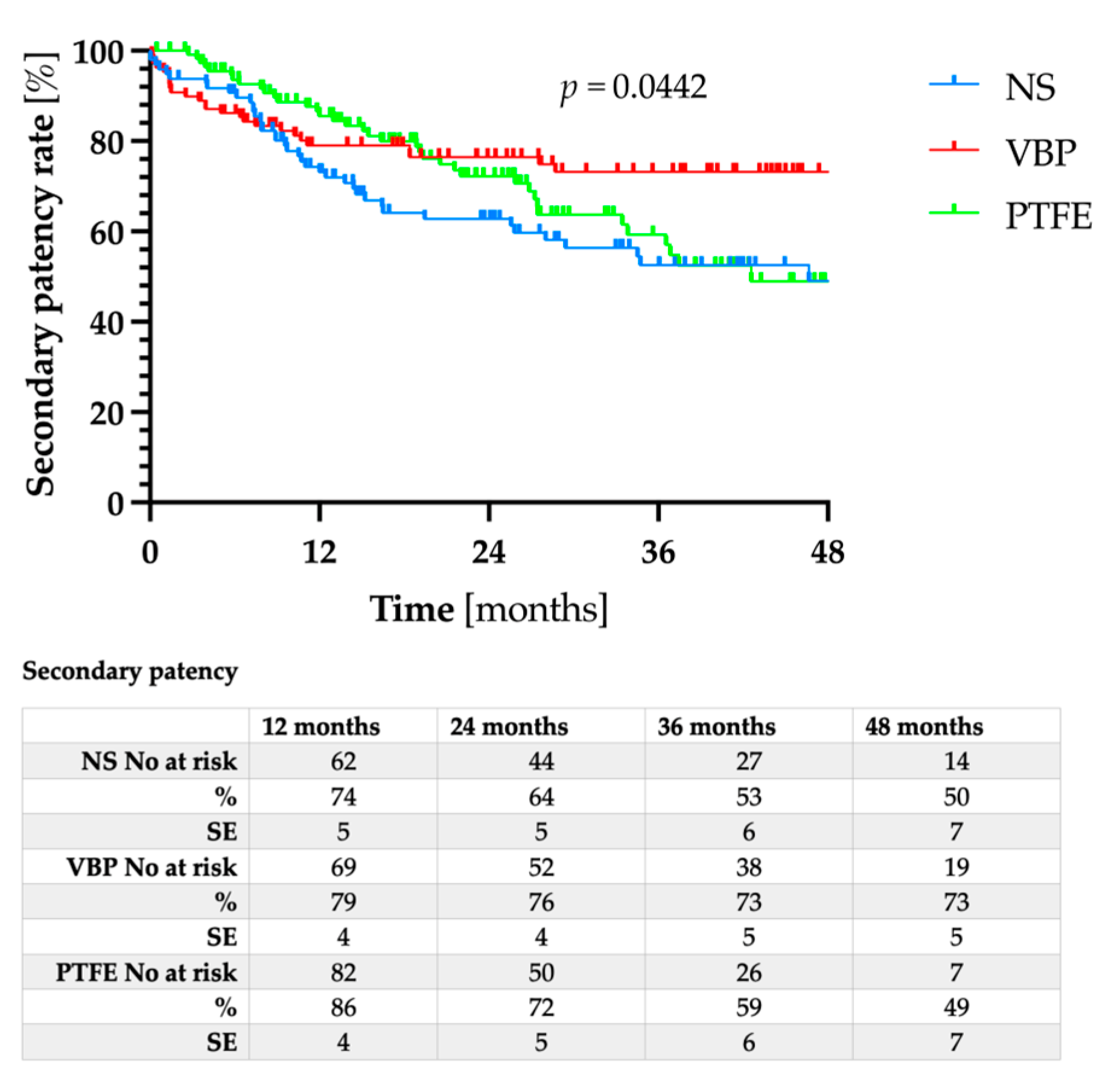
3.2. Patency Rates
3.3. Ranking
3.4. Clinical Outcome
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Frank, U.; Nikol, S.; Belch, J.; Boc, V.; Brodmann, M.; Carpentier, P.H.; Chraim, A.; Canning, C.; Dimakakos, E.; Gottsater, A.; et al. ESVM Guideline on peripheral arterial disease. Vasa 2019, 48, 1–79. [Google Scholar] [CrossRef] [PubMed]
- Farhan, S.; Enzmann, F.K.; Bjorkman, P.; Kamran, H.; Zhang, Z.; Sartori, S.; Vogel, B.; Tarricone, A.; Linni, K.; Venermo, M.; et al. Revascularization Strategies for Patients with Femoropopliteal Peripheral Artery Disease. J. Am. Coll. Cardiol. 2023, 81, 358–370. [Google Scholar] [CrossRef] [PubMed]
- Farber, A.; Menard, M.T.; Conte, M.S.; Kaufman, J.A.; Powell, R.J.; Choudhry, N.K.; Hamza, T.H.; Assmann, S.F.; Creager, M.A.; Cziraky, M.J.; et al. Surgery or Endovascular Therapy for Chronic Limb-Threatening Ischemia. N. Engl. J. Med. 2022, 387, 2305–2316. [Google Scholar] [CrossRef] [PubMed]
- Ambler, G.K.; Twine, C.P. Graft Type for Femoro-Popliteal Bypass Surgery. Cochrane Database Syst. Rev. 2018, 2, CD001487. [Google Scholar] [CrossRef] [PubMed]
- Gerhard-Herman, M.D.; Gornik, H.L.; Barrett, C.; Barshes, N.R.; Corriere, M.A.; Drachman, D.E.; Fleisher, L.A.; Fowkes, F.G.R.; Hamburg, N.M.; Kinlay, S.; et al. 2016 AHA/ACC Guideline on the Management of Patients with Lower Extremity Peripheral Artery Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J. Am. Coll. Cardiol. 2017, 135, e726–e779. [Google Scholar]
- Humbarger, O.; Siracuse, J.J.; Rybin, D.; Stone, D.H.; Goodney, P.P.; Schermerhorn, M.L.; Farber, A.; Jones, D.W. Broad Variation in Prosthetic Conduit Use for Femoral-Popliteal Bypass Is Not Justified on the Basis of Contemporary Outcomes Favoring Autologous Great Saphenous Vein. J. Vasc. Surg. 2019, 70, 1514–1523.e2. [Google Scholar] [CrossRef] [PubMed]
- Dalmia, V.; Carnevale, M.; Friedmann, P.; Indes, J.; Lipsitz, E.; Futchko, J.; Koleilat, I. Impact of Tibial Bypass Conduit on Long-Term Amputation-Free Survival and Primary Patency in the Vascular Quality Initiative. J. Vasc. Surg. 2021, 75, 1351–1357. [Google Scholar] [CrossRef] [PubMed]
- Norgren, L.; Hiatt, W.R.; Dormandy, J.A.; Nehler, M.R.; Harris, K.A.; Fowkes, F.G.; Rutherford, R.B. Inter-Society Consensus for the Management of Peripheral Arterial Disease. Int. Angiol. 2007, 26, 81–157. [Google Scholar] [PubMed]
- Kluckner, M.; Gratl, A.; Wipper, S.H.; Hitzl, W.; Nierlich, P.; Aspalter, M.; Linni, K.; Enzmann, F.K. Comparison of Prosthetic and Vein Bypass with Nitinol Stents in Long Femoropopliteal Lesions. Ann. Vasc. Surg. 2021, 78, 272–280. [Google Scholar] [CrossRef] [PubMed]
- Enzmann, F.K.; Nierlich, P.; Hölzenbein, T.; Asplater, M.; Kluckner, M.; Hitzl, W.; Opperer, M.; Linni, K. Vein Bypass versus Nitinol Stent in Long Femoropopliteal Lesions: 4-Year Results of a Randomized Controlled Trial. Ann. Surg. 2022. [Google Scholar] [CrossRef] [PubMed]
- Neumayer, L.; Hosokawa, P.; Itani, K.; El-tamer, M.; Henderson, W.G.; Khuri, S.F. Multivariable Predictors of Postoperative Surgical Site Infection after General and Vascular Surgery: Results from the Patient Safety in Surgery Study. J. Am. Coll. Surg. 2007, 204, 1178–1187. [Google Scholar] [CrossRef] [PubMed]
- Rutherford, R.B.; Baker, J.D.; Ernst, C.; Johnston, K.W.; Porter, J.M.; Ahn, S.; Jones, D.N. Recommended Standards for Reports Dealing with Lower Extremity Ischemia: Revised Version. J. Vasc. Surg. 1997, 26, 517–538. [Google Scholar] [CrossRef] [PubMed]
- Frank, E.; Hall, M.A.; Witten, I.H.; Weka, T. The WEKA Workbench. Online Appendix for “Data Mining: Practical Machine Learning Tools and Techniques”, 4th ed.; Morgan Kaufmann: Burlington, MA, USA, 2016. [Google Scholar]
- Moreira, C.C.; Leung, A.D.; Farber, A.; Rybin, D.; Doros, G.; Siracuse, J.J.; Kalish, J.; Eslami, M.H. Alternative Conduit for Infrageniculate Bypass in Patients with Critical Limb Ischemia. J. Vasc. Surg. 2016, 64, 131–139.e1. [Google Scholar] [CrossRef] [PubMed]
- Bosiers, M.; Setacci, C.; De Donato, G.; Torsello, G.; Silveira, P.G.; Deloose, K.; Scheinert, D.; Veroux, P.; Hendriks, J.; Maene, L.; et al. ZILVERPASS Study: ZILVER PTX Stent vs Bypass Surgery in Femoropopliteal Lesions. J. Endovasc. Ther. 2020, 27, 287–295. [Google Scholar] [CrossRef] [PubMed]
- Reijnen, M.M.P.J.; van Walraven, L.A.; Fritschy, W.M.; Lensvelt, M.M.A.; Zeebregts, C.J.; Lemson, M.S.; Wikkeling, O.R.M.; Smeets, L.; Holewijn, S. 1-Year Results of a Multicenter Randomized Controlled Trial Comparing Heparin-Bonded Endoluminal to Femoropopliteal Bypass. JACC Cardiovasc. Interv. 2017, 10, 2320–2331. [Google Scholar] [CrossRef] [PubMed]
- Conte, M.S.; Bradbury, A.W.; Kolh, P.; White, J.V.; Dick, F.; Fitridge, R.; Mills, J.L.; Ricco, J.B.; Suresh, K.R.; Murad, M.H.; et al. Global Vascular Guidelines on the Management of Chronic Limb-Threatening Ischemia. Eur. J. Vasc. Endovasc. Surg. 2019, 58, S1–S109.e33. [Google Scholar] [CrossRef] [PubMed]

| Stent (n = 103, 109 Lesions) | VBP (n = 106, 109 Lesions) | PTFE (n = 107, 114 Lesions) | p Value $ | |
|---|---|---|---|---|
| Age (years) | 69.3 ± 7 | 68.5 ± 7.8 | 68.7 ± 9.4 | 0.990 ◊ |
| Male | 69 (67) | 78 (74) | 70 (65) | 0.269 § |
| Cardiovascular risk factors | ||||
| Atrial fibrillation | 15 (15) | 15 (14) | 11 (10) | 0.527 § |
| Coronary artery bypass | 15 (14) | 3 (3) | 11 (10) | 0.014 § |
| Coronary artery disease | 48 (47) | 31 (29) | 36 (34) | 0.033 § |
| Diabetes mellitus | 36 (35) | 40 (38) | 34 (32) | 0.691 § |
| Dyslipidemia | 63 (61) | 69 (65) | 38 (36) | <0.001 § |
| Hemodialysis | 3 (3) | 3 (3) | - | 0.138 § |
| Hypertension | 89 (86) | 88 (83) | 77 (72) | 0.033 § |
| Prior stroke | 12 (12) | 10 (9) | 9 (8) | 0.667 § |
| Rutherford category | 0.361 § | |||
| 3 | 51 (47) | 51 (47) | 60 (56) | |
| 4 | 17 (16) | 14 (13) | 14 (13) | |
| 5 | 39 (36) | 43 (40) | 29 (27) | |
| 6 | 2 (2) | 1 (1) | 3 (3) | |
| CLTI | 58 (53) | 58 (53) | 46 (43) | 0.116 § |
| ASA classification | 0.787 § | |||
| I | 1 (1) | 1 (1) | 1 (1) | |
| II | 25 (24) | 29 (27) | 31 (29) | |
| III | 77 (75) | 76 (72) | 74 (69) | |
| Stent (n = 109) | VBP (n = 109) | PTFE (n = 114) | p Value | |
|---|---|---|---|---|
| Lesion length (mm) | 264 ± 59 | 272 ± 70 | 274 ± 58 | 0.427 ◊ |
| TASC II type | ||||
| C | 48 (44) | 48 (44) | 51 (45) | 0.993 § |
| D | 61 (56) | 61 (56) | 63 (55) | 0.993 § |
| Previous intervention ipsilateral | 31 (28) | 49 (45) | 29 (25) | 0.004 § |
| Chronic total occlusion | 87 (80) | 96 (88) | 107 (94) | 0.007 § |
| Reference vessel diameter (mm) | 5 ± 0.7 | 5 ± 1 | 5.1 ± 1.1 | 0.783 ◊ |
| Number of stenosis free outflow vessels | ||||
| 1 | 26 (24) | 21 (19) | 20 (18) | 0.482 |
| 2 | 53 (49) | 54 (50) | 44 (39) | 0.188 |
| 3 | 30 (30) | 34 (31) | 50 (44) | 0.026 |
| CFA endarterectomy | - | 39 (36) | 33 (29) | <0.001 § |
| Infragenicular bypass | - | 60 (55) | 12 (11) | <0.001 § |
| ePTFE graft | - | - | 12 (11) | |
| Ipsilateral GSV | - | 100 (92) | - | |
| Alternative vein graft | - | 9 (8) | - | |
| Reversed vein graft | - | 15 (14) | - | |
| Stent diameter (mm) * | 6 ± 0.5 | - | - | |
| Stented lesion length (mm) * | 248 ± 98 | - | - | |
| Number of stents * | 4 ± 2 | - | - | |
| CFA angioplasty | 4 (4) | - | - | |
| Popliteal stenting * | 30 (28) | - | - | |
| Procedural length | 72 ± 31 | 181 ± 63 | 142 ± 54 | p < 0.001 |
| Stent (n = 103; 109 Lesions) | VBP (n = 106; 109 Lesions) | PTFE (n = 107; 114 Lesions) | p Value | |
|---|---|---|---|---|
| Patients with ≥ 1 complication | 7 (6) | 12 (11) | 1 (1) | 0.007 § |
| Local complications | ||||
| Superficial SSI | - | 14 (13) | 8 (7) | 0.001 § |
| Deep SSI | - | 9 (8) | 3 (3) | 0.004 § |
| Bleeding/pseudoaneurysm | 6 (6) | 6 (6) | 3 (3) | 0.543 § |
| Distal embolization | 7 (7) | - | - | |
| Vessel perforation | 10 (9) | - | - | |
| Unplanned minor amputation | 4 (4) | 1 (1) | 1 (1) | 0.080 § |
| Systemic complications | ||||
| Anemia/blood transfusion | 5 (5) | 20 (18) | 4 (4) | <0.001 § |
| Myocardial Infarction | 1 (1) | 1 (1) | 2 (2) | 0.797 § |
| Renal function deterioration | 3 (3) | 4 (4) | - | 0.140 § |
| Predictor | Rank | Gain Ratio Merit | OR [95% CI] | p-Value |
|---|---|---|---|---|
| Surgery type Stent (vs. VBP) PFTE (vs. VBP) | 1.7 ± 0.6 | 0.02 ± 0.003 | 0.532 [0.302 to 0.938] 0.324 [0.176 to 0.595] | 0.001 0.029 0.000 |
| Rutherford classification 5/6 | 2.8 ± 0.92 | 0.016 ± 0.002 | 0.742 [0.344 to 1.604] | 0.448 |
| CLTI | 3.9 ± 0.94 | 0.014 ± 0.002 | 0.726 [0.356 to 1.480] | 0.378 |
| Superficial surgical site infection | 5.4 ± 1.64 | 0.011 ± 0.003 | 0.739 [0.252 to 2.170] | 0.582 |
| Atrial fibrillation | 5.8 ± 1.83 | 0.01 ± 0.003 | 0.620 [0.289 to 1.331] | 0.220 |
| Diabetes mellitus | 6.9 ± 1.44 | 0.009 ± 0.002 | 0.719 [0.425 to 1.216] | 0.219 |
| Hypertension | 7.5 ± 1.87 | 0.008 ± 0.002 | 1.559 [0.824 to 2.950] | 0.172 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kluckner, M.; Gruber, L.; Wippel, D.; Lobenwein, D.; Westreicher, W.; Pilz, M.; Enzmann, F.K. Long-Term Outcome of Bypass Surgery versus Endovascular Revascularization in Long Femoropopliteal Lesions. J. Clin. Med. 2023, 12, 3507. https://doi.org/10.3390/jcm12103507
Kluckner M, Gruber L, Wippel D, Lobenwein D, Westreicher W, Pilz M, Enzmann FK. Long-Term Outcome of Bypass Surgery versus Endovascular Revascularization in Long Femoropopliteal Lesions. Journal of Clinical Medicine. 2023; 12(10):3507. https://doi.org/10.3390/jcm12103507
Chicago/Turabian StyleKluckner, Michaela, Leonhard Gruber, David Wippel, Daniela Lobenwein, Werner Westreicher, Manuela Pilz, and Florian K. Enzmann. 2023. "Long-Term Outcome of Bypass Surgery versus Endovascular Revascularization in Long Femoropopliteal Lesions" Journal of Clinical Medicine 12, no. 10: 3507. https://doi.org/10.3390/jcm12103507
APA StyleKluckner, M., Gruber, L., Wippel, D., Lobenwein, D., Westreicher, W., Pilz, M., & Enzmann, F. K. (2023). Long-Term Outcome of Bypass Surgery versus Endovascular Revascularization in Long Femoropopliteal Lesions. Journal of Clinical Medicine, 12(10), 3507. https://doi.org/10.3390/jcm12103507






