Factors Influencing Public Attitudes towards COVID-19 Vaccination: A Scoping Review Informed by the Socio-Ecological Model
Abstract
1. Introduction
2. Materials and Methods
2.1. Information Sources
2.2. Eligibility Criteria
2.3. Data Charting Process
2.4. Synthesis of Results
2.5. Data Analysis
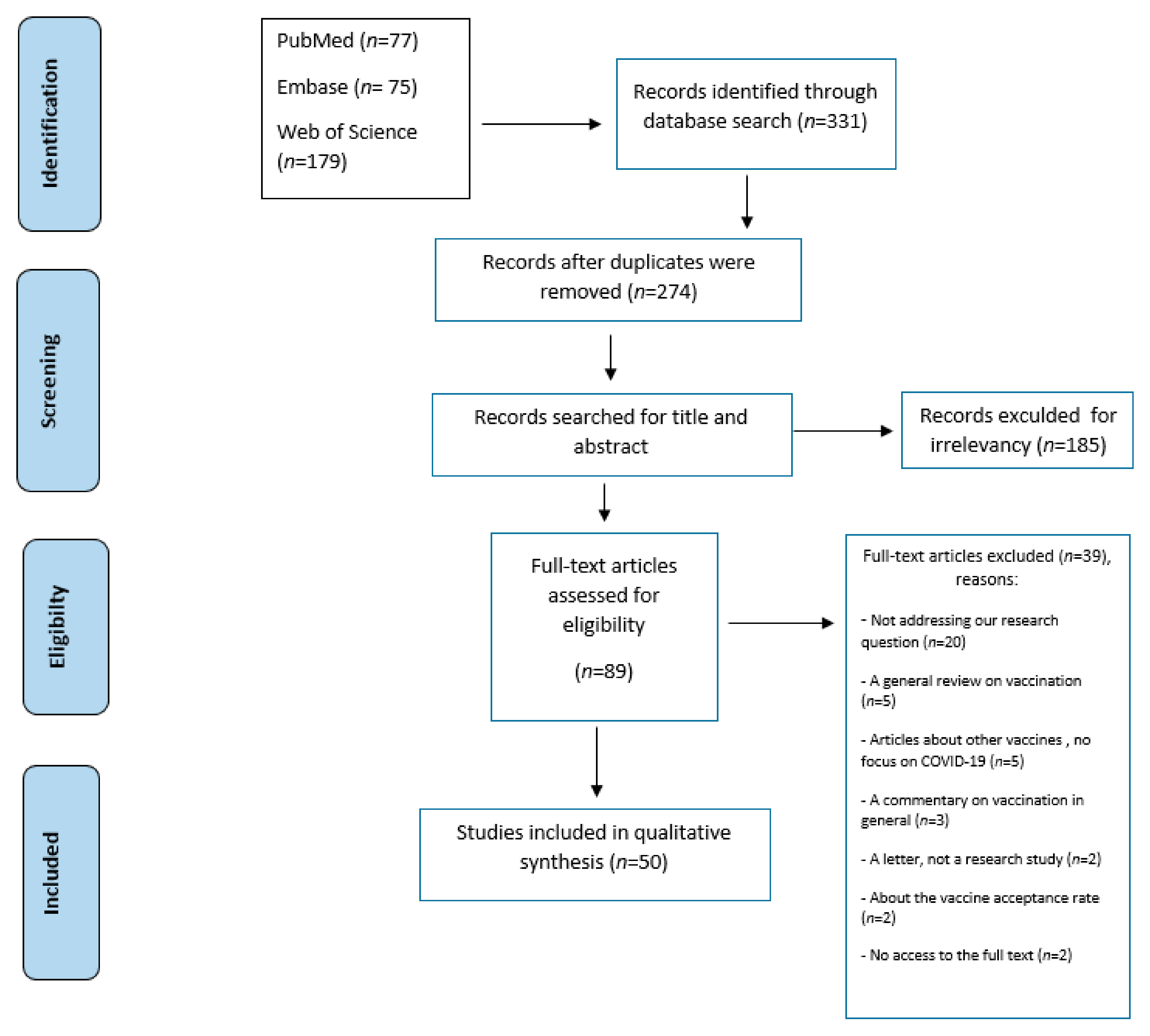
3. Results
3.1. Study Characteristics
- −
- −
- Some studies reported using specific platforms to upload surveys including crowdsourcing platform Amazon Mechanical Turk (mTurk, Amazon, Seattle, WA, USA) [32,61], computer-assisted web interviewing (CAWI) and computer-assisted telephone interviewing (CATI) [34,53], and Qualtrics (Seattle, WA, USA) [47,55];
- −
- −
- One study used an online survey with a semi-structured questionnaire following the snowball sampling technique [60];
- −
- One study used open-ended questions to ask about the factors influencing attitudes towards vaccines [47];
- −
- One study used an Internet survey and telephone interviews [35];
- −
- One study used a face-to-face-administered questionnaire [37].
3.2. Sociodemographic Characteristics Shaping Public Attitudes towards COVID-19 Vaccines
3.3. Individual Factors Shaping Public Attitudes towards COVID-19 Vaccines
3.4. Social and Organizational Factors Shaping Public Attitudes towards COVID-19 Vaccines
3.5. Characteristics of COVID-19 Vaccines and Public Concern
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Section | Item | Prisma-ScR Checklist ITEM | Reported on Page # |
|---|---|---|---|
| Title | |||
| Title | 1 | Identify the report as a scoping review. | 1 |
| Abstract | |||
| Structured summary | 2 | Provide a structured summary that includes (as applicable): background, objectives, eligibility criteria, sources of evidence, charting methods, results, and conclusions that relate to the review questions and objectives. | 1 |
| Introduction | |||
| Rationale | 3 | Describe the rationale for the review in the context of what is already known. Explain why the review questions/objectives lend themselves to a scoping review approach. | 2 |
| Objectives | 4 | Provide an explicit statement of the questions and objectives being addressed with reference to their key elements (e.g., population or participants, concepts, and context) or other relevant key elements used to conceptualize the review questions and/or objectives. | 3 |
| Methods | |||
| Protocol and registration | 5 | Indicate whether a review protocol exists; state if and where it can be accessed (e.g., a Web address); and if available, provide registration information, including the registration number. | 3 |
| Eligibility criteria | 6 | Specify characteristics of the sources of evidence used as eligibility criteria (e.g., years considered, language, and publication status), and provide a rationale. | 3 |
| Information sources * | 7 | Describe all information sources in the search (e.g., databases with dates of coverage and contact with authors to identify additional sources), as well as the date the most recent search was executed. | 3 |
| Search | 8 | Present the full electronic search strategy for at least 1 database, including any limits used, such that it could be repeated. | 3 |
| Selection of sources of evidence † | 9 | State the process for selecting sources of evidence (i.e., screening and eligibility) included in the scoping review. | 3 |
| Data charting process ‡ | 10 | Describe the methods of charting data from the included sources of evidence (e.g., calibrated forms or forms that have been tested by the team before their use, and whether data charting was done independently or in duplicate) and any processes for obtaining and confirming data from investigators. | 4 |
| Data items | 11 | List and define all variables for which data were sought and any assumptions and simplifications made. | 4 |
| Critical appraisal of individual sources of evidence § | 12 | If done, provide a rationale for conducting a critical appraisal of included sources of evidence; describe the methods used and how this information was used in any data synthesis (if appropriate). | NA |
| Synthesis of results | 13 | Describe the methods of handling and summarizing the data that were charted. | 4 |
| Results | |||
| Selection of sources of evidence | 14 | Give numbers of sources of evidence screened, assessed for eligibility, and included in the review, with reasons for exclusions at each stage, ideally using a flow diagram. | 5 |
| Characteristics of sources of evidence | 15 | For each source of evidence, present characteristics for which data were charted and provide the citations. | 6 |
| Critical appraisal within sources of evidence | 16 | If done, present data on critical appraisal of included sources of evidence (see item 12). | NA |
| Results of individual sources of evidence | 17 | For each included source of evidence, present the relevant data that were charted that relate to the review questions and objectives. | 8 |
| Synthesis of results | 18 | Summarize and/or present the charting results as they relate to the review questions and objectives. | 13 |
| Discussion | |||
| Summary of evidence | 19 | Summarize the main results (including an overview of concepts, themes, and types of evidence available), link to the review questions and objectives, and consider the relevance to key groups. | 28 |
| Limitations | 20 | Discuss the limitations of the scoping review process. | 30 |
| Conclusions | 21 | Provide a general interpretation of the results with respect to the review questions and objectives, as well as potential implications and/or next steps. | 30 |
| Funding | |||
| Funding | 22 | Describe sources of funding for the included sources of evidence, as well as sources of funding for the scoping review. Describe the role of the funders of the scoping review. | 31 |
References
- Zhu, H.; Wei, L.; Niu, P. The novel coronavirus outbreak in Wuhan, China. Glob. Health Res. Policy 2020, 5, 1–3. [Google Scholar] [CrossRef]
- Worldometer. COVID-19 Coronavirus Pandemic. Available online: https://www.worldometers.info/coronavirus/?utm_campaign=homeAdvegas1? (accessed on 21 March 2021).
- Nicola, M.; Alsafi, Z.; Sohrabi, C.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, M.; Agha, R. The socio-economic implications of the coronavirus pandemic (COVID-19): A review. Int. J. Surg. 2020, 78, 185–193. [Google Scholar] [CrossRef]
- Phua, J.; Weng, L.; Ling, L.; Egi, M.; Lim, C.-M.; Divatia, J.V.; Shrestha, B.R.; Arabi, Y.M.; Ng, J.; Gomersall, C.D.; et al. Intensive care management of coronavirus disease 2019 (COVID-19): Challenges and recommendations. Lancet Respir. Med. 2020, 8, 506–517. [Google Scholar] [CrossRef]
- World Health Organization. Modes of Transmission of Virus Causing COVID-19: Implications for IPC Precaution Recommendations. Available online: https://www.who.int/news-room/commentaries/detail/modes-of-transmission-of-virus-causing-covid-19-implications-for-ipc-precaution-recommendations (accessed on 21 March 2021).
- World Health Organization. Coronavirus. Available online: https://www.who.int/health-topics/coronavirus#tab=tab_1 (accessed on 21 March 2021).
- Ferguson, N.M.; Laydon, D.; Nedjati-Gilani, G.; Imai, N.; Ainslie, K.; Baguelin, M.; Ghani, A.C. Impact of Non-Pharmaceutical Interventions (Npis) to Reduced Covid-19 Mortality and Healthcare Demand; Imperial College London: London, UK, 2020. [Google Scholar]
- Yamey, G.; Schäferhoff, M.; Hatchett, R.; Pate, M.; Zhao, F.; McDade, K.K. Ensuring global access to COVID-19 vaccines. Lancet 2020, 395, 1405–1406. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Vaccines: The Basics. Available online: https://www.cdc.gov/vaccines/vpd/vpd-vac-basics.html (accessed on 21 March 2021).
- Orenstein, W.A.; Ahmed, R. Simply put: Vaccination saves lives. Proc. Natl. Acad. Sci. USA 2017, 114, 4031–4033. [Google Scholar] [CrossRef]
- Butter, S.; McGlinchey, E.; Berry, E.; Armour, C. Psychological, social, and situational factors associated with COVID-19 vaccination intentions: A study of UK key workers and non-key workers. Br. J. Health Psychol. 2021, 1–17. [Google Scholar] [CrossRef]
- Dror, A.A.; Eisenbach, N.; Taiber, S.; Morozov, N.G.; Mizrachi, M.; Zigron, A.; Srouji, S.; Sela, E. Vaccine hesitancy: The next challenge in the fight against COVID-19. Eur. J. Epidemiol. 2020, 35, 775–779. [Google Scholar] [CrossRef]
- Geoghegan, S.; O’Callaghan, K.P.; Offit, P.A. Vaccine Safety: Myths and Misinformation. Front. Microbiol. 2020, 11, 372. [Google Scholar] [CrossRef]
- Bendau, A.; Plag, J.; Petzold, M.B.; Ströhle, A. COVID-19 vaccine hesitancy and related fears and anxiety. Int. Immunopharmacol. 2021, 97, 107724. [Google Scholar] [CrossRef]
- Wilson, K.; Nguyen, T.; Henningsen, K.H.; Brehaut, J.C.; Hoe, E. Acceptance of a pandemic influenza vaccine: A systematic review of surveys of the general public. Infect. Drug Resist. 2011, 4, 197–207. [Google Scholar] [CrossRef]
- Dubé, E.; Laberge, C.; Guay, M.; Bramadat, P.; Roy, R.; Bettinger, J.A. Vaccine hesitancy. Hum. Vaccines Immunother. 2013, 9, 1763–1773. [Google Scholar] [CrossRef]
- Paul, E.; Steptoe, A.; Fancourt, D. Attitudes towards vaccines and intention to vaccinate against COVID-19: Implications for public health communications. Lancet Reg. Health Eur. 2021, 1, 100012. [Google Scholar] [CrossRef]
- Johnson, N.F.; Velásquez, N.; Restrepo, N.J.; Leahy, R.; Gabriel, N.; El Oud, S.; Zheng, M.; Manrique, P.; Wuchty, S.; Lupu, Y. The online competition between pro- and anti-vaccination views. Nature 2020, 582, 230–233. [Google Scholar] [CrossRef]
- Bish, A.; Michie, S. Demographic and attitudinal determinants of protective behaviours during a pandemic: A review. Br. J. Health Psychol. 2010, 15, 797–824. [Google Scholar] [CrossRef]
- Habersaat, K.B.; Betsch, C.; Danchin, M.; Sunstein, C.R.; Böhm, R.; Falk, A.; Brewer, N.T.; Omer, S.B.; Scherzer, M.; Sah, S.; et al. Ten considerations for effectively managing the COVID-19 transition. Nat. Hum. Behav. 2020, 4, 677–687. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.; Horsley, T.; Weeks, L.; et al. PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef]
- Dahlgren, G.; Whitehead, M. Policies and Strategies to Promote Social Equity in Health. Background Document to WHO—Strategy Paper for Europe; Institute for Futures Studies: Stockholm, Sweden, 1991. [Google Scholar]
- Chen, T.; Dai, M.; Xia, S.; Zhou, Y. Do Messages Matter? Investigating the Combined Effects of Framing, Outcome Uncertainty, and Number Format on COVID-19 Vaccination Attitudes and Intention. Health Commun. 2021, 1–8. [Google Scholar] [CrossRef]
- Chen, M.; Li, Y.; Chen, J.; Wen, Z.; Feng, F.; Zou, H.; Fu, C.; Chen, L.; Shu, Y.; Sun, C. An online survey of the attitude and willingness of Chinese adults to receive COVID-19 vaccination. Hum. Vaccines Immunother. 2021, 1–10. [Google Scholar] [CrossRef]
- Lazarus, J.V.; Ratzan, S.C.; Palayew, A.; Gostin, L.O.; Larson, H.J.; Rabin, K.; Kimball, S.; El-Mohandes, A. A global survey of potential acceptance of a COVID-19 vaccine. Nat. Med. 2021, 27, 225–228. [Google Scholar] [CrossRef]
- Bell, S.; Clarke, R.; Mounier-Jack, S.; Walker, J.L.; Paterson, P. Parents’ and guardians’ views on the acceptability of a future COVID-19 vaccine: A multi-methods study in England. Vaccine 2020, 38, 7789–7798. [Google Scholar] [CrossRef]
- Al-Mohaithef, M.; Padhi, B.K. Determinants of COVID-19 Vaccine Acceptance in Saudi Arabia: A Web-Based National Survey. J. Multidiscip. Healthc. 2020, 13, 1657–1663. [Google Scholar] [CrossRef]
- Wang, J.; Jing, R.; Lai, X.; Zhang, H.; Lyu, Y.; Knoll, M.D.; Fang, H. Acceptance of COVID-19 Vaccination during the COVID-19 Pandemic in China. Vaccines 2020, 8, 482. [Google Scholar] [CrossRef]
- Murphy, J.; Vallières, F.; Bentall, R.P.; Shevlin, M.; McBride, O.; Hartman, T.K.; McKay, R.; Bennett, K.; Mason, L.; Gibson-Miller, J.; et al. Psychological characteristics associated with COVID-19 vaccine hesitancy and resistance in Ireland and the United Kingdom. Nat. Commun. 2021, 12, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Akarsu, B.; Özdemir, D.C.; Baser, D.A.; Aksoy, H.; Fidancı, I.; Cankurtaran, M. While studies on COVID-19 vaccine is ongoing, the public’s thoughts and attitudes to the future COVID-19 vaccine. Int. J. Clin. Pract. 2021, 75, e13891. [Google Scholar] [CrossRef]
- Seale, H.; Heywood, A.E.; Leask, J.; Sheel, M.; Durrheim, D.N.; Bolsewicz, K.; Kaur, R. Examining Australian public perceptions and behaviors towards a future COVID-19 vaccine. BMC Infect. Dis. 2021, 21, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Hursh, S.R.; Strickland, J.C.; Schwartz, L.P.; Reed, D.D. Quantifying the Impact of Public Perceptions on Vaccine Acceptance Using Behavioral Economics. Front. Public Health 2020, 8, 608852. [Google Scholar] [CrossRef] [PubMed]
- Biasio, L.R.; Bonaccorsi, G.; Lorini, C.; Pecorelli, S. Assessing COVID-19 vaccine literacy: A preliminary online survey. Hum. Vaccines Immunother. 2021, 17, 1304–1312. [Google Scholar] [CrossRef]
- Kourlaba, G.; Kourkouni, E.; Maistreli, S.; Tsopela, C.-G.; Molocha, N.-M.; Triantafyllou, C.; Koniordou, M.; Kopsidas, I.; Chorianopoulou, E.; Maroudi-Manta, S.; et al. Willingness of Greek general population to get a COVID-19 vaccine. Glob. Health Res. Policy 2021, 6, 1–10. [Google Scholar] [CrossRef]
- Fisher, K.A.; Bloomstone, S.J.; Walder, J.; Crawford, S.; Fouayzi, H.; Mazor, K.M. Attitudes toward a potential SARS-CoV-2 vaccine: A survey of US adults. Ann. Intern. Med. 2020, 173, 964–973. [Google Scholar] [CrossRef]
- Guidry, J.P.; Laestadius, L.I.; Vraga, E.K.; Miller, C.A.; Perrin, P.B.; Burton, C.W.; Ryan, M.; Fuemmeler, B.F.; Carlyle, K.E. Willingness to get the COVID-19 vaccine with and without emergency use authorization. Am. J. Infect. Control 2021, 49, 137–142. [Google Scholar] [CrossRef]
- Popa, G.L.; Muntean, A.-A.; Muntean, M.-M.; Popa, M.I. Knowledge and Attitudes on Vaccination in Southern Romanians: A Cross-Sectional Questionnaire. Vaccines 2020, 8, 774. [Google Scholar] [CrossRef]
- Detoc, M.; Bruel, S.; Frappe, P.; Tardy, B.; Botelho-Nevers, E.; Gagneux-Brunon, A. Intention to participate in a COVID-19 vaccine clinical trial and to get vaccinated against COVID-19 in France during the pandemic. Vaccine 2020, 38, 7002–7006. [Google Scholar] [CrossRef]
- Prati, G. Intention to receive a vaccine against SARS-CoV-2 in Italy and its association with trust, worry and beliefs about the origin of the virus. Health Educ. Res. 2020, 35, 505–511. [Google Scholar] [CrossRef]
- Marco-Franco, J.E.; Pita-Barros, P.; Vivas-Orts, D.; González-De-Julián, S.; Vivas-Consuelo, D. COVID-19, Fake News, and Vaccines: Should Regulation Be Implemented? Int. J. Environ. Res. Public Health 2021, 18, 744. [Google Scholar] [CrossRef]
- Caserotti, M.; Girardi, P.; Rubaltelli, E.; Tasso, A.; Lotto, L.; Gavaruzzi, T. Associations of COVID-19 risk perception with vaccine hesitancy over time for Italian residents. Soc. Sci. Med. 2021, 272, 113688. [Google Scholar] [CrossRef]
- Alley, S.J.; Stanton, R.; Browne, M.; To, Q.G.; Khalesi, S.; Williams, S.L.; Thwaite, T.; Fenning, A.; Vandelanotte, C. As the Pandemic Progresses, How Does Willingness to Vaccinate against COVID-19 Evolve? Int. J. Environ. Res. Public Health 2021, 18, 797. [Google Scholar] [CrossRef]
- Reiter, P.L.; Pennell, M.L.; Katz, M.L. Acceptability of a COVID-19 vaccine among adults in the United States: How many people would get vaccinated? Vaccine 2020, 38, 6500–6507. [Google Scholar] [CrossRef]
- Feleszko, W.; Lewulis, P.; Czarnecki, A.; Waszkiewicz, P. Flattening the Curve of COVID-19 Vaccine Rejection—An International Overview. Vaccines 2021, 9, 44. [Google Scholar] [CrossRef]
- Harapan, H.; Wagner, A.L.; Yufika, A.; Winardi, W.; Anwar, S.; Gan, A.K.; Setiawan, A.M.; Rajamoorthy, Y.; Sofyan, H.; Mudatsir, M. Acceptance of a COVID-19 Vaccine in Southeast Asia: A Cross-Sectional Study in Indonesia. Front. Public Health 2020, 8, 381. [Google Scholar] [CrossRef]
- Lin, Y.; Hu, Z.; Zhao, Q.; Alias, H.; Danaee, M.; Wong, L.P. Understanding COVID-19 vaccine demand and hesitancy: A nationwide online survey in China. PLoS Negl. Trop. Dis. 2020, 14, e0008961. [Google Scholar] [CrossRef]
- Williams, L.; Gallant, A.J.; Rasmussen, S.; Nicholls, L.A.B.; Cogan, N.; Deakin, K.; Young, D.; Flowers, P. Towards intervention development to increase the uptake of COVID-19 vaccination among those at high risk: Outlining evidence-based and theoretically informed future intervention content. Br. J. Health Psychol. 2020, 25, 1039–1054. [Google Scholar] [CrossRef] [PubMed]
- Alqudeimat, Y.; Alenezi, D.; AlHajri, B.; Alfouzan, H.; Almokhaizeem, Z.; Altamimi, S.; Almansouri, W.; Alzalzalah, S.; Ziyab, A. Acceptance of a COVID-19 Vaccine and its Related Determinants among the General Adult Population in Kuwait. Med. Princ. Pract. 2021, 10, 2052–2061. [Google Scholar] [CrossRef]
- Sallam, M.; Dababseh, D.; Eid, H.; Al-Mahzoum, K.; Al-Haidar, A.; Taim, D.; Yaseen, A.; Ababneh, N.A.; Bakri, F.G.; Mahafzah, A. High Rates of COVID-19 Vaccine Hesitancy and Its Association with Conspiracy Beliefs: A Study in Jordan and Kuwait among Other Arab Countries. Vaccines 2021, 9, 42. [Google Scholar] [CrossRef] [PubMed]
- Wong, L.P.; Alias, H.; Wong, P.-F.; Lee, H.Y.; Abubakar, S. The use of the health belief model to assess predictors of intent to receive the COVID-19 vaccine and willingness to pay. Hum. Vaccines Immunother. 2020, 16, 1232–1238. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, K.H.; Srivastav, A.; Razzaghi, H.; Williams, W.; Lindley, M.C.; Jorgensen, C.; Abad, N.; Singleton, J.A. COVID-19 Vaccination Intent, Perceptions, and Reasons for Not Vaccinating Among Groups Prioritized for Early Vaccination—United States, September and December 2020. MMWR Morb. Mortal. Wkly. Rep. 2021, 70, 217–222. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Wong, E.L.Y.; Ho, K.-F.; Cheung, A.W.L.; Yau, P.S.Y.; Dong, D.; Wong, S.Y.S.; Yeoh, E.-K. Change of willingness to accept COVID-19 vaccine and reasons of vaccine hesitancy of working people at different waves of local epidemic in Hong Kong, China: Repeated cross-sectional surveys. Vaccines 2021, 9, 62. [Google Scholar] [CrossRef]
- La Vecchia, C.; Negri, E.; Alicandro, G.; Scarpino, V. Attitudes towards influenza vaccine and a potential COVID-19 vaccine in Italy and differences across occupational groups, September 2020. Med. Del. Lavoro 2020, 111, 445–448. [Google Scholar]
- Ward, J.K.; Alleaume, C.; Peretti-Watel, P.; Seror, V.; Cortaredona, S.; Launay, O.; Raude, J.; Verger, P.; Beck, F.; Legleye, S.; et al. The French public’s attitudes to a future COVID-19 vaccine: The politicization of a public health issue. Soc. Sci. Med. 2020, 265, 113414. [Google Scholar] [CrossRef]
- Romer, D.; Jamieson, K.H. Conspiracy theories as barriers to controlling the spread of COVID-19 in the U.S. Soc. Sci. Med. 2020, 263, 113356. [Google Scholar] [CrossRef]
- Sherman, S.M.; Smith, L.E.; Sim, J.; Amlôt, R.; Cutts, M.; Dasch, H.; Rubin, G.J.; Sevdalis, N. COVID-19 vaccination intention in the UK: Results from the COVID-19 vaccination acceptability study (CoVAccS), a nationally representative cross-sectional survey. Hum. Vaccines Immunother. 2021, 17, 1612–1621. [Google Scholar] [CrossRef]
- McCaffery, K.J.; Dodd, R.H.; Cvejic, E.; Ayrek, J.; Isautier, J.M.; Copp, T.; Bonner, C.; Pickles, K.; Nickel, B.; Dakin, T.; et al. Health literacy and disparities in COVID-19–related knowledge, attitudes, beliefs and behaviours in Australia. Public Health Res. Pr. 2020, 30. [Google Scholar] [CrossRef]
- Pogue, K.; Jensen, J.L.; Stancil, C.K.; Ferguson, D.G.; Hughes, S.J.; Mello, E.J.; Burgess, R.; Berges, B.K.; Quaye, A.; Poole, B.D. Influences on Attitudes Regarding Potential COVID-19 Vaccination in the United States. Vaccines 2020, 8, 582. [Google Scholar] [CrossRef] [PubMed]
- Taylor, S.; Landry, C.A.; Paluszek, M.M.; Groenewoud, R.; Rachor, G.S.; Asmundson, G.J.G. A Proactive Approach for Managing COVID-19: The Importance of Understanding the Motivational Roots of Vaccination Hesitancy for SARS-CoV2. Front. Psychol. 2020, 11, 575950. [Google Scholar] [CrossRef]
- Reuben, R.C.; Danladi, M.M.A.; Saleh, D.A.; Ejembi, P.E. Knowledge, Attitudes and Practices towards COVID-19: An Epidemiological Survey in North-Central Nigeria. J. Community Health 2021, 46, 457–470. [Google Scholar] [CrossRef]
- Corpuz, R.; D’Alessandro, S.; Adeyemo, J.; Jankowski, N.; Kandalaft, K. Life History Orientation Predicts COVID-19 Precautions and Projected Behaviors. Front. Psychol. 2020, 11, 1857. [Google Scholar] [CrossRef] [PubMed]
- Bertin, P.; Nera, K.; Delouvée, S. Conspiracy Beliefs, Rejection of Vaccination, and Support for hydroxychloroquine: A Conceptual Replication-Extension in the COVID-19 Pandemic Context. Front. Psychol. 2020, 11, 11. [Google Scholar] [CrossRef]
- Coustasse, A.; Kimble, C.; Maxik, K. COVID-19 and Vaccine Hesitancy. J. Ambul. Care Manag. 2021, 44, 71–75. [Google Scholar] [CrossRef] [PubMed]
- Puri, N.; Coomes, E.A.; Haghbayan, H.; Gunaratne, K. Social media and vaccine hesitancy: New updates for the era of COVID-19 and globalized infectious diseases. Hum. Vaccines Immunother. 2020, 16, 2586–2593. [Google Scholar] [CrossRef]
- Danchin, M.; Biezen, R.; Manski-Nankervis, J.-A.; Kaufman, J.; Leask, J. Preparing the public for COVID-19 vaccines: How can general practitioners build vaccine confidence and optimise uptake for themselves and their patients? Aust. J. Gen. Pract. 2020, 49, 625–629. [Google Scholar] [CrossRef]
- Ling, R. Confirmation Bias in the Era of Mobile News Consumption: The Social and Psychological Dimensions. Digit. J. 2020, 8, 596–604. [Google Scholar] [CrossRef]
- Dubé, E.; MacDonald, N.E. How can a global pandemic affect vaccine hesitancy? Expert Rev. Vaccines 2020, 19, 899–901. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.; Tu, P.; Beitsch, L.M. Confidence and Receptivity for COVID-19 Vaccines: A Rapid Systematic Review. Vaccines 2021, 9, 16. [Google Scholar] [CrossRef] [PubMed]
- Bogart, L.M.; Ojikutu, B.O.; Tyagi, K.; Klein, D.J.; Mutchler, M.G.; Dong, L.; Lawrence, S.J.; Thomas, D.R.; Kellman, S. COVID-19 Related Medical Mistrust, Health Impacts, and Potential Vaccine Hesitancy Among Black Americans Living with HIV. JAIDS J. Acquir. Immune Defic. Syndr. 2021, 86, 200–207. [Google Scholar] [CrossRef] [PubMed]
- Jung, H.; Albarracín, D. Concerns for others increases the likelihood of vaccination against influenza and COVID-19 more in sparsely rather than densely populated areas. Proc. Natl. Acad. Sci. USA 2021, 118, e2007538118. [Google Scholar] [CrossRef]
- Largent, E.A.; Persad, G.; Sangenito, S.; Glickman, A.; Boyle, C.; Emanuel, E.J. US Public Attitudes Toward COVID-19 Vaccine Mandates. JAMA Netw. Open 2020, 3, e2033324. [Google Scholar] [CrossRef]
- Yin, F.; Wu, Z.; Xia, X.; Ji, M.; Wang, Y.; Hu, Z. Unfolding the Determinants of COVID-19 Vaccine Acceptance in China. J. Med. Internet Res. 2021, 23, e26089. [Google Scholar] [CrossRef]
- Robles, A.S.; Gallahue, A.; Bennett, S.; Nerida, T.; Larson, T.; Parker, H.; Riddle, M. Determinants of Covid-19 Vaccine Acceptance among Health Care Providers and Citizens in Nevada. J. Investig. Med. 2021, 69, 235. [Google Scholar] [CrossRef]
- Gangarosa, E.; Galazka, A.; Wolfe, C.; Phillips, L.; Miller, E.; Chen, R. Impact of anti-vaccine movements on pertussis control: The untold story. Lancet 1998, 351, 356–361. [Google Scholar] [CrossRef]
- Benecke, O.; Deyoung, S.E. Anti-Vaccine Decision-Making and Measles Resurgence in the United States. Glob. Pediatr. Health 2019, 6. [Google Scholar] [CrossRef]
- Phadke, V.K.; Bednarczyk, R.A.; Salmon, D.A.; Omer, S.B. Association Between Vaccine Refusal and Vaccine-Preventable Diseases in the United States. JAMA 2016, 315, 1149–1158. [Google Scholar] [CrossRef]
- Sallam, M. COVID-19 Vaccine Hesitancy Worldwide: A Concise Systematic Review of Vaccine Acceptance Rates. Vaccines 2021, 9, 160. [Google Scholar] [CrossRef] [PubMed]
- Roller-Wirnsberger, R.; Lindner, S.; Kolosovski, L.; Platzer, E.; Dovjak, P.; Flick, H.; Tziraki, C.; Illario, M. The role of health determinants in the influenza vaccination uptake among older adults (65+): A scope review. Aging Clin. Exp. Res. 2021, 15, 1–10. [Google Scholar] [CrossRef]
- UK Government Scientific Advisory Group for Emergencies. Factors Influencing Covid-19 Vaccine Uptake among Minority Ethnic Groups, 17 December 2020. Available online: https://www.gov.uk/government/publications/factors-influencing-covid-19-vaccine-uptake-among-minority-ethnic-groups-17-december-2020 (accessed on 21 March 2021).
- Santhanes, D.; Wong, C.P.; Yap, Y.Y.; San, S.P.; Chaiyakunapruk, N.; Khan, T.M. Factors involved in human papillomavirus (HPV) vaccine hesitancy among women in the South-East Asian Region (SEAR) and Western Pacific Region (WPR): A scoping review. Hum. Vaccines Immunother. 2018, 14, 124–133. [Google Scholar] [CrossRef] [PubMed]
- Ashfield, S.; Donelle, L. Parental Online Information Access and Childhood Vaccination Decisions in North America: A Scoping Review (Preprint). J. Med. Internet Res. 2020, 22, e20002. [Google Scholar] [CrossRef]
| Search | Search Term |
|---|---|
| #1 | “Corona” OR “SARS-CoV-2” OR “COVID 19” |
| #2 | “Vaccine” OR “Vaccination” |
| #3 | “Acceptance” OR “Agreement” OR “Willingness” OR “Refusal” OR “Resistance” OR “Confidence” OR “Hesitancy” OR “Antivaxx” OR “Antivaxxers” OR “Antivaccine” OR “Anti-vaccine” |
| #4 | #1, #2, and #3 |
| First Author/Year of Publication | Study Design | Study Setting | Population | Sample Size | Mean Age (in Years) | Attitudes towards COVID-19 Vaccines |
|---|---|---|---|---|---|---|
| Chen, T.E. 2021 [23] | Experimental design | Online experiment | Chinese adults | 413 | Aged between 18 and 60 (M = 24.70, SD = 9.55) | Attitudes towards COVID-19 vaccination scores were highly favorable and the intention to get vaccinated was high |
| Chen, M.S. 2020 [24] | Cross-sectional | Online questionnaire | Chinese adults | 3195 | Majority aged 18–44 | 83.8% were willing to receive a COVID-19 vaccine, 13.6% were unsure |
| Lazarus, J.V. 2020 [25] | Cross-sectional | 19 countries (global) | 13,426 | Majority aged 25–54 | 46.8% completely agreed to accept a COVID-19 vaccine | |
| Bell, S. 2020 [26] | Cross-sectional survey | Online social media strategy | Parents and guardians (aged 16+ years) who reported living in England with a child aged 18 months or under | 1190 | 33 | Acceptability of a future COVID-19 vaccine |
| Coustasse, A. 2020 [63] | Review | US population | 50% willing to get a vaccine in study 1 65% willing to get a vaccine in study 2 | |||
| Al-Mohaithef, M. 2020 [27] | Web-based cross-sectional study | Public | General public in Saudi Arabia | 992 | Most of the respondents aged 26–35 | Willingness to accept a vaccine |
| Robles, A.S. 2020 [73] | Conference paper | Nevada | Vaccine acceptance | |||
| Wang, J. 2020 [28] | Online cross-sectional survey | Public | China | 2058 | Adults | Willingness to accept a vaccine |
| Lin, C. 2021 [68] | Systematic review | 126 surveys | Vaccine intention and acceptance | |||
| Murphy, J. 2021 [29] | Cross-sectional survey | Online survey | General adult populations of Ireland and the United Kingdom | 3066 | Mostly 55–64 (Ireland) and 45–54 (UK) | COVID-19 vaccine hesitancy and resistance, including psychological indicators |
| Akarsu, B. 2020 [30] | Cross-sectional web-based survey | Public | General public in Turkey | 759 | 32.41 ± 9.92 | Vaccination acceptance |
| Seale, H. 2021 [31] | National cross-sectional survey | Online survey | Australian adults (18 years and older) | 1420 | Mostly 30–49 | Perceptions and behaviors towards a future COVID-19 vaccine |
| Hursh, S.R. 2020 [32] | Cross-sectional survey | Online using crowdsourcing platform Amazon Mechanical Turk (mTurk) | Participants from the United States | 534 | 41.9 | Evaluation of COVID-19 vaccine demand |
| Biasio, L.R. 2020 [33] | Online survey | Online study | Italian adults | 885 | Majority aged 31–50 | Perceptions about getting a vaccine |
| Kourlaba, G. 2021 [34] | Cross-sectional survey | Computer-assisted telephone interviewing (CATI) and computer-assisted web interviewing (CAWI) | Adult Greeks | 1004 | 41.7 (17.7) | Willingness to receive a COVID-19 vaccine |
| Fisher, K. 2020 [35] | Cross-sectional survey | Internet survey and telephone interviews | US general public | 1000 | Adults | Vaccine hesitancy |
| Guidry, J.P.D. 2021 [36] | Cross-sectional survey | Online survey | US adults | 788 | 45.9 | Willingness to get a COVID-19 vaccine |
| Jung, H. 2020 [70] | Longitudinal survey, two experiments | United states | Survey: 2490 Experiment: 800 | Vaccination intention | ||
| Popa, G.L. 2020 [37] | Face-to-face cross-sectional survey | Public | Romanian respondents | 1647 | Median age, 37 | Vaccination acceptance |
| Detoc, M. 2020 [38] | Cross-sectional survey | Online via social networks | General population in France | 3250 | Mostly 30–49 | Intention to get vaccinated against COVID-19 |
| Prati, G. 2021 [39] | Online survey | Online study | General public in Italy | 624 | Between 18 and 72 years | Willingness to accept a vaccine |
| Marco-Franco, J.L. 2021 [40] | Cross-sectional, legal analysis | Several countries | Vaccine hesitancy | |||
| Caserotti, M. 2021 [41] | Cross-sectional online questionnaire (pre-lockdown, during lockdown, and post-lockdown) Note: “different participants every phase” | Various institutional and personal social channels related to the research team | Italian residents | 2267 | 25–65 | The percentage of people who accepted a vaccine was high during the lockdown |
| Bogart, L.M. 2021 [69] | RCT | Community-based | Black Americans | 101 | 50.3 (11.5) | COVID-19 mistrust beliefs, COVID-19 vaccine or treatment hesitancy |
| Alley, S.J. 2021 [42] | Repeated cross-sectional survey | Online | Australian adults | 575 | Mostly over 55 years | Willingness to get vaccinated against COVID-19 |
| Puri, N. 2020 [64] | Review | Social media | Vaccine hesitancy | |||
| Reiter, P.L. 2020 [43] | Online survey | Online study | US general public | 2006 | >18 | Willingness to accept a vaccine |
| Feleszko, W. 2021 [44] | Poland, an online omnibus survey tool | Public | Poland public | 1066 | 18–65 | 37% supported COVID-19 vaccination |
| Danchin, M. 2020 [65] | Review | Vaccine refusal | ||||
| Harapan, H. 2020 [45] | Cross-sectional online survey | Online study | General population in Indonesia | 1359 | More than half of the respondents were aged 21–30 years | 50 or 95% effective COVID-19 vaccine |
| Lin, Y. 2020 [46] | Nationwide cross-sectional self-administered online survey | Public | China | 3541 | Adults | 83.5% said yes to the intent to get a vaccine |
| Williams, L. 2020 [47] | Cross-sectional study with open-ended questions about the factors | Online | Older adults and people with respiratory chronic diseases | 527 | Older sample with adults aged 65 | 86% of respondents wanted to receive a COVID-19 vaccine |
| Yin, F. 2021 [72] | Media analysis through a proposed novel behavioral dynamics model, SRS/I (susceptible–reading–susceptible/immune) | Microblogging platform Weibo (social media) | Chinese citizens (living in China and abroad) | 1.75 million Weibo messages | COVID-19 vaccine acceptance | |
| Alqudeimat, Y.2021 [48] | Web-based cross-sectional study | Public (adults living in Kuwait) | Kuwait | 2368 | >21 | Participants were willing to accept a COVID-19 vaccine once available (53.1%) |
| Sallam, M. 2021 [49] | Cross-sectional online survey | Online study | Jordan, Kuwait, and Saudi Arabia | 3414 | Vaccine acceptance (29.4%) | |
| Wong, L.P. 2020 [50] | Cross-sectional online survey | Online survey | Malaysian general public | 1159 | Adults | Willingness to accept a vaccine |
| Nguyen, K.H. 2020 [51] | CDC-conducted household panel surveys | Internet survey | US general public | Adults | Willingness to accept a vaccine | |
| Wang, K.L. 2021 [52] | Cross-sectional | Online questionnaire | Working population in Hong Kong (HK), China | 1196 | Majority aged 40–49 | Standardized rate of vaccine acceptance in the first survey was 44.2% and 34.8% in the second survey |
| Largent, E.A. 2020 [71] | Gallup panel | Online study | US adults | 2730 | Not available | Acceptability of COVID-19 vaccines |
| LaVecchia, K. 2020 [53] | National cross-sectional survey | Online using computer- assisted web interviews (CAWI) | Italians aged 15–85 years | 1055 | 33.2 | Attitudes towards a potential COVID-19 vaccine |
| Ward, J.K. 2020 [54] | Cross-sectional survey | Online | French population of 18 years of age | 5018 | Mostly less than 35 | Attitudes to a future COVID-19 vaccine |
| Romer, D. 2020 [55] | Two-wave follow-up surveys | Online using Qualtrics | US general population | 1050 | Mostly 60+ | Intention to get vaccinated against COVID-19 |
| Sherman, S.M. 2020 [56] | Cross-sectional online survey | Online study | UK adults | 1500 | 46 ± 15.8 | Vaccination intention |
| McCaffery, K.J. 2020 [57] | National cross-sectional community online survey | Australian general public, adults aged over 18 years | 4362 | 42.6 ± 17.4 | Vaccine hesitancy | |
| Pogue, K. 2020 [58] | Cross-sectional survey | Public online survey | US respondents | 316 | COVID-19 vaccine intention | |
| Taylor, S. 2020 [59] | Cross-sectional survey | Public Internet-based study | American and Canadian adults | 3674 | 53 ± 15 | Vaccination hesitancy |
| Reuben, R.C. 2020 [60] | Cross-sectional online survey with a semi-structured questionnaire using a snowball sampling technique | Public | North-central Nigeria | 589 | 80.6% were 18–39 years | 29% accepted to take a vaccine |
| Corpuz, R. 2020 [61] | Cross-sectional Amazon’s Mechanical Turk (MTurk), an online survey tool | Online study | US general public | 209 | Mean age M = 33.4 years (SD = 11.4) | Endorsement of the vaccines |
| Bertin, P. 2020 [62] | Two cross-sectional studies. An online questionnaire was disseminated by the authors on Facebook, Twitter, and Linkedin | Online studies | General public in France | 396 | Mage = 26.1, SD = 10.3, min = 18, max = 70 | Negatively predicted participants intention to get the vaccine |
| Ling, R. 2020 [66] | Review | Social media | Anti-vaccination | |||
| Dube, E. 2020 [67] | Review | Vaccine hesitancy |
| First Author | Hesitancy (−) or Acceptance (+) of COVID-19 Vaccines | Sociodemographics Shaping Public Attitudes towards COVID-19 Vaccines |
|---|---|---|
| Chen, T.E. 2021 [23] | + | - High education level - Increasing age |
| Chen, M.S. 2020 [24] | + | - Male gender - High income - Education level - Han nationality |
| Lazarus, J.V. 2020 [25] | + | - Age older than 25 - Male gender - High income - High education level |
| − | - Sick people or sick family members | |
| Bell, S. 2020 [26] | − | - Black, Asian, Chinese, mixed, or other ethnicity - Low income |
| Coustasse, A. 2020 [63] | + | - 60 years and older - Non-Hispanic Whites - High education level - High income |
| Al-Mohaithef, M. 2020 [27] | − | - Older age - Being married - High education level - Non-Saudi - Employed in the government sector |
| Robles, A.S. 2020 [73] | + | - Age - Ethnicity - Chronic disease - Education level - Employment status - Country |
| Wang, J. 2020 [28] | + | - Male gender - Being married |
| Lin, C. 2021 [68] | + | - College degrees - Income, - Insurance - Living in rural or larger areas - Gender - Race |
| Murphy, J. 2021 [29] | − | Irish sample, vaccine-hesitant - Female gender - Aged between 35 and 44 years - No mental health problem Irish sample, vaccine-resistant - Aged 35–44 years - Residing in a city - Non-Irish ethnicity - Lower income - Underlying health condition UK sample, vaccine-hesitant - Female gender - Younger than 65 UK sample, vaccine-resistant - Younger age - More likely to reside in a suburb - In the three lowest income brackets - Being pregnant |
| Akarsu, B. 2020 [30] | − | - Female gender - Unemployed |
| + | - Have SSI or private health insurance - Have children - Those who were thinking about getting their child a COVID-19 vaccine were more willing to get vaccinated - High level of education | |
| Seale, H. 2021 [31] | + | - Female gender - Aged 70 years and above - Reporting chronic disease - Holding private health insurance |
| Hursh, S.R. 2020 [32] | − | - Male gender |
| Kourlaba, G. 2021 [34] | + | - Aged > 65 years old - Those belonging to vulnerable groups or members of their household belonging to vulnerable groups |
| Fisher, K. 2020 [35] | - | - Young age - Black race - Low educational attainment |
| Guidry, J.P.D. 2021 [36] | + | - Education - Having insurance - Age - Race/ethnicity |
| Detoc, M. 2020 [38] | + | - Older age, - Male gender |
| Alley, S.J. 2021 [42] | − | - Low education - Female gender |
| Danchin, M. 2020 [65] | − | - Low education - Low income - Potentially more prone to infectious diseases - Women aged < 35 years - People aged > 75 years who are at a higher risk of disease from COVID-19 |
| Lin, Y. 2020 [46] | + | - Self-employed and service sector workers |
| Williams, L. 2020 [47] | + | - White ethnicity - High education level - High income - High-risk/shielding |
| Alqudeimat, Y. 2021 [48] | + | - Male gender |
| Sallam, M. 2021 [49] | + | - Male gender - High education levels - History of chronic disease |
| Wong, L.P. 2020 [50] | + | - Higher education levels - Professional and managerial occupations - High income |
| Nguyen, K.H. 2020 [51] | − | - Young adults - Female gender - Non-Hispanic Black (Black) persons - Adults living in nonmetropolitan areas - Adults with lower educational attainment - Low income - No health insurance |
| Wang, K.L. 2021 [52] | + | - Young age - Male gender - Being married |
| Largent, E.A. 2020 [71] | + | - Non-Black respondents more likely to get vaccinated - Respondents with a bachelor’s degree or higher |
| LaVecchia, K. 2020 [53] | + | - Age above 55 - Professionals, managers, teachers, and manual workers |
| First Author | Hesitancy (−) or Acceptance (+) of COVID-19 Vaccines | Individual Factors Shaping Public Attitudes towards COVID-19 Vaccines |
|---|---|---|
| Chen, M.S. 2020 [24] | + | - Confidence, satisfaction, and worries about risks - Attention to relevant COVID-19 information - Perceived views of the severity of COVID-19 disease - Degree of concern regarding the COVID-19 pandemic |
| Lazarus, J.V. 2020 [25] | + | - Trust in the government |
| Wang, J. 2020 [28] | + | - Perceiving a high risk of infection - Being vaccinated against influenza in the previous season |
| Lin, C. 2021 [68] | − | - Belief that vaccines are unnecessary - Inadequate information - General anti-vaccine stand - Willingness to pay |
| Murphy, J. 2021 [29] | − | - Irish sample: more likely to have voted for the political party Sinn Féin or an independent politician in the previous general election |
| Akarsu, B. 2020 [30] | + | - Got a seasonal flu vaccine - High level of anxiety |
| − | - “Afraid of the side effects of the vaccines” - “Do not think it can be reliable as it will be a new vaccine” - “COVID-19 infection is a biological weapon” - “The vaccine will serve those who produce this virus” | |
| Hursh, S.R. 2020 [32] | − | - Greater conspiracy beliefs and political conservatism |
| Biasio, L.R. 2020 [33] | Attitudes to a COVID-19 vaccine | - Health literacy |
| Kourlaba, G. 2021 [34] | + | - Those believing that the COVID-19 virus was not developed in laboratories by humans - Those believing that coronavirus is far more contagious and lethal compared to the H1N1 virus - Those believing that next waves are coming - Higher knowledge score regarding symptoms, transmission routes, and prevention and control measures against COVID-19 |
| Fisher, K.A. 2020 [35] | − | - Vaccine-specific concerns - Need for more information - General anti-vaccine beliefs - Lack of trust |
| Guidry, J.P.D. 2021 [36] | + | - Positive subjective norms - A positive attitude toward vaccines in general - Perceived susceptibility to COVID-19 - High perceived benefits of the vaccines - Scoring low on barriers to the vaccines - Scoring high on self-efficacy - High perceived behavioral control |
| Jung, H. 2020 [70] | + | - Prosocial concern for vaccination motivates vaccination in more and less populated regions |
| Popa, G.L. 2020 [37] | − | - Lack of information - Fear of adverse reactions - Fears of toxicity and poor quality related to vaccine components - Doubts about the technology used to produce the vaccines - Personal reasons to refuse vaccines (which included religious conviction) - Lack of trust in the healthcare system |
| Detoc, M. 2020 [38] | + | - Fear about COVID-19 and individual perceived risk |
| Prati, G. 2021 [39] | Attitudes to a COVID-19 vaccine | - Being worried about the non-natural origin of the virus and the role of the institutional trust |
| Caserotti, M. 2021 [41] | + | - Likelihood of getting the infection - Perceived severity of the disease |
| Reiter, P.L. 2020 [43] | + | - Likelihood of getting the COVID-19 infection in the future - Perceived severity of the COVID-19 infection |
| Danchin, M. 2020 [65] | + | - Adequate health literacy |
| Harapan, H. 2020 [45] | + | - Perceived risk of the COVID-19 infection |
| Lin, Y. 2020 [46] | + | - Perceiving overall health as very good - Perceiving the benefit of feeling less worried of contracting coronavirus after getting a vaccine - Perceiving the benefit of a COVID-19 vaccine in reducing the risk of infection and resultant complications - If given adequate information and if taken by many in the general public |
| Williams, L. 2020 [47] | Attitudes to a COVID-19 vaccine | - The perception that COVID-19 will persist over time - Perceiving the media to have overexaggerated the risk - The “beliefs about consequences” TDF domain, with themes relating to personal health, health consequences to others, and severity of COVID-19 |
| Alqudeimat, Y. 2021 [48] | − | - Likelihood of infection - Viewed vaccines in general to have health-related risks |
| Sallam, M. 2021 [49] | − | - Beliefs that COVID-19 vaccines are intended to inject microchips into recipients and that the vaccines are related to infertility |
| Wang, K.L. 2021 [52] | + | - Influenza vaccine uptake during the previous year |
| Largent, E.A. 2020 [71] | − | - Republicans and Independents were less likely to get vaccinated than Democrats |
| Ward, J.K. 2020 [54] | Attitudes to a COVID-19 vaccine | - Political partisanship and engagement with the political system |
| Romer, D. 2020 [55] | − | - Belief in three COVID-19-related conspiracy theories |
| Sherman, S.M. 2020 [56] | + | - Having been vaccinated for influenza the previous winter - Perceiving a great risk of COVID-19 - Positive general COVID-19 vaccination beliefs and attitudes - Weak beliefs that the vaccination would cause side effects - Greater perceived information sufficiency to make an informed decision about COVID-19 vaccination - Lower endorsement of the notion that only people who are at risk of serious illness should be vaccinated for COVID-19 |
| McCaffery, K.J. 2020 [57] | − | - Beliefs and misinformation about COVID-19/vaccines - Inadequate health literacy |
| Pogue, K. 2020 [58] | + | - Respondents who routinely got vaccines were more likely to be receptive to receiving a COVID-19 vaccine - The greater the perceived impact of COVID-19 in America, the more receptive the respondent was to receive a potential COVID-19 vaccine |
| Taylor, S. 2020 [59] | − | - Mistrust of vaccine benefits - Worries about unforeseen future negative effects - Concerns about commercial profiteering - Preference for natural immunity |
| Reuben, R.C. 2020 [60] | − | - No confidence in the present intervention by Chinese doctors |
| Corpuz, R. 2020 [61] | + | - Those exhibiting a slow life history orientation were more likely to endorse mandatory vaccination for COVID-19 |
| − | - Social and political conservatism | |
| Bertin, P. 2020 [62] | − | - COVID-19 conspiracy beliefs |
| Ling, R. 2020 [66] | − | - Confirmation bias, consumption of only those news that confirm the pre-existing attitudes and beliefs |
| First Author | Hesitancy (−) or Acceptance (+) of COVID-19 Vaccines | Social Networks and Organizational Factors (Family, Friends, HC Providers, Employers) and Media Shaping Public Attitudes towards COVID-19 Vaccines |
|---|---|---|
| Chen, T.E. 2021 [23] | + | - Type of messages received and message frames - Outcome uncertainty - Number format - Numeracy skills |
| Lazarus, J.V. 2020 [25] | + | - Accepting their employer’s recommendation to do so |
| Wang, J. 2020 [28] | + | - Valuing their doctor’s recommendations |
| Seale, H. 2021 [31] | +/− | - Decision to get vaccinated would be supported by family and friends |
| Popa, G.L. 2020 [37] | − | - Disinformation (through classic media, social media, and the Internet) |
| Bogart, L.M. 2021 [69] | + | - Social service and healthcare providers |
| Alley, S.J. 2021 [42] | − | - Infrequent users of traditional media |
| Puri, N. 2020 [64] | − | - Anti-vaccination messages on social platforms |
| Reiter, P.L. 2020 [43] | + | - Healthcare providers recommending vaccination |
| Feleszko, W. 2021 [44] | + | - Recommended by a family doctor - Someone of family members/friends was vaccinated - Need a vaccination certificate to enter some countries |
| First Author | Hesitancy (−) or Acceptance (+) of COVID-19 Vaccines | Characteristics of COVID-19 Vaccines Shaping Public Attitudes towards COVID-19 Vaccines |
|---|---|---|
| Chen, M.2020 [24] | + | - If the vaccine is domestic, not imported |
| Lazarus, J.V. 2020 [25] | + | - Vaccine proved safe and effective by the government |
| Coustasse, A. 2020 [63] | +/− | - Effectiveness estimate of the vaccine - Safety based on newness and adverse effects - Lack of testing - Vaccination timeframe - Who will have access to it - Cost to consumers - How states and the federal government will determine vaccination methods - Getting COVID-19 from the shot - Fear of side effects from an untested vaccine |
| Robles, A.S. 2020 [73] | +/− | - Perception of efficacy, safety, and adverse effects of the vaccines - Source of information - Conspiracy theories - Reactance and outrage regarding new information |
| Wang, J. 2020 [28] | +/− | - Efficacy of COVID-19 vaccination - Concerns about vaccine safety |
| Lin, C. 2021 [68] | +/− | - Newness of COVID-19 vaccines - Inadequate information - Unknown/short duration of immunity - Cost - Country of vaccine origin - Fear of side effects, safety, and effectiveness |
| Fisher, K.A. 2020 [35] | − | - Vaccine-specific concerns - Need for more information |
| Popa, G.L.P. 2020 [37] | − | - Fear of adverse reactions - Fear of toxicity and poor quality related to vaccine components - Doubts about the technology used to produce the vaccines - Price |
| Marco-Franco, J.E. 2021 [40] | − | - Worries about the side effects, safety and effectiveness of the vaccines |
| Reiter, P.L. 2020 [43] | + | - Effectiveness of a COVID-19 vaccine |
| Danchin, M. 2020 [65] | + | - Vaccine safety and effectiveness |
| Harapan, H. 2020 [45] | + | - The baseline effectiveness of the vaccines |
| Lin, Y. 2020 [46] | +/− | - Concerns about faulty/fake vaccines - Affordability and high price - Safety and efficacy - Confidence and preference of domestically made vaccines |
| Williams, L. 2020 [47] | +/− | - Personal concerns regarding vaccine safety |
| Yin, F. 2021 [72] | + | - The majority thought the price was low - Positive views on side effects - Information about inactivated vaccines (inactivated vaccines are more accepted) |
| Wang, K.L. 2021 [52] | − | - Doubts of effectiveness - Thought of the vaccines as unnecessary - More accepted in the first wave compared to the third wave |
| Dube, E. 2020 [67] | − | - Vaccine development is being pushed - COVID-19 vaccine antigen-carrying platforms have never been used - The production of new COVID-19 vaccines will not meet demand - Conspiracy theories - More than one type of COVID-19 vaccines is likely to be used within a country. Thus, the safety and efficacy profiles may vary |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Al-Jayyousi, G.F.; Sherbash, M.A.M.; Ali, L.A.M.; El-Heneidy, A.; Alhussaini, N.W.Z.; Elhassan, M.E.A.; Nazzal, M.A. Factors Influencing Public Attitudes towards COVID-19 Vaccination: A Scoping Review Informed by the Socio-Ecological Model. Vaccines 2021, 9, 548. https://doi.org/10.3390/vaccines9060548
Al-Jayyousi GF, Sherbash MAM, Ali LAM, El-Heneidy A, Alhussaini NWZ, Elhassan MEA, Nazzal MA. Factors Influencing Public Attitudes towards COVID-19 Vaccination: A Scoping Review Informed by the Socio-Ecological Model. Vaccines. 2021; 9(6):548. https://doi.org/10.3390/vaccines9060548
Chicago/Turabian StyleAl-Jayyousi, Ghadir Fakhri, Mohamed Abdelhady Mabrouk Sherbash, Lamees Abdullah Mohammed Ali, Asmaa El-Heneidy, Nour Waleed Zuhair Alhussaini, Manar Elsheikh Abdelrahman Elhassan, and Maisa Ayman Nazzal. 2021. "Factors Influencing Public Attitudes towards COVID-19 Vaccination: A Scoping Review Informed by the Socio-Ecological Model" Vaccines 9, no. 6: 548. https://doi.org/10.3390/vaccines9060548
APA StyleAl-Jayyousi, G. F., Sherbash, M. A. M., Ali, L. A. M., El-Heneidy, A., Alhussaini, N. W. Z., Elhassan, M. E. A., & Nazzal, M. A. (2021). Factors Influencing Public Attitudes towards COVID-19 Vaccination: A Scoping Review Informed by the Socio-Ecological Model. Vaccines, 9(6), 548. https://doi.org/10.3390/vaccines9060548






