COVID-19 Vaccination Acceptance in China after It Becomes Available: A Cross-Sectional Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Sample and Data Collection
2.2. Measures
2.3. Statistical Analysis
3. Results
3.1. Sample Characteristics
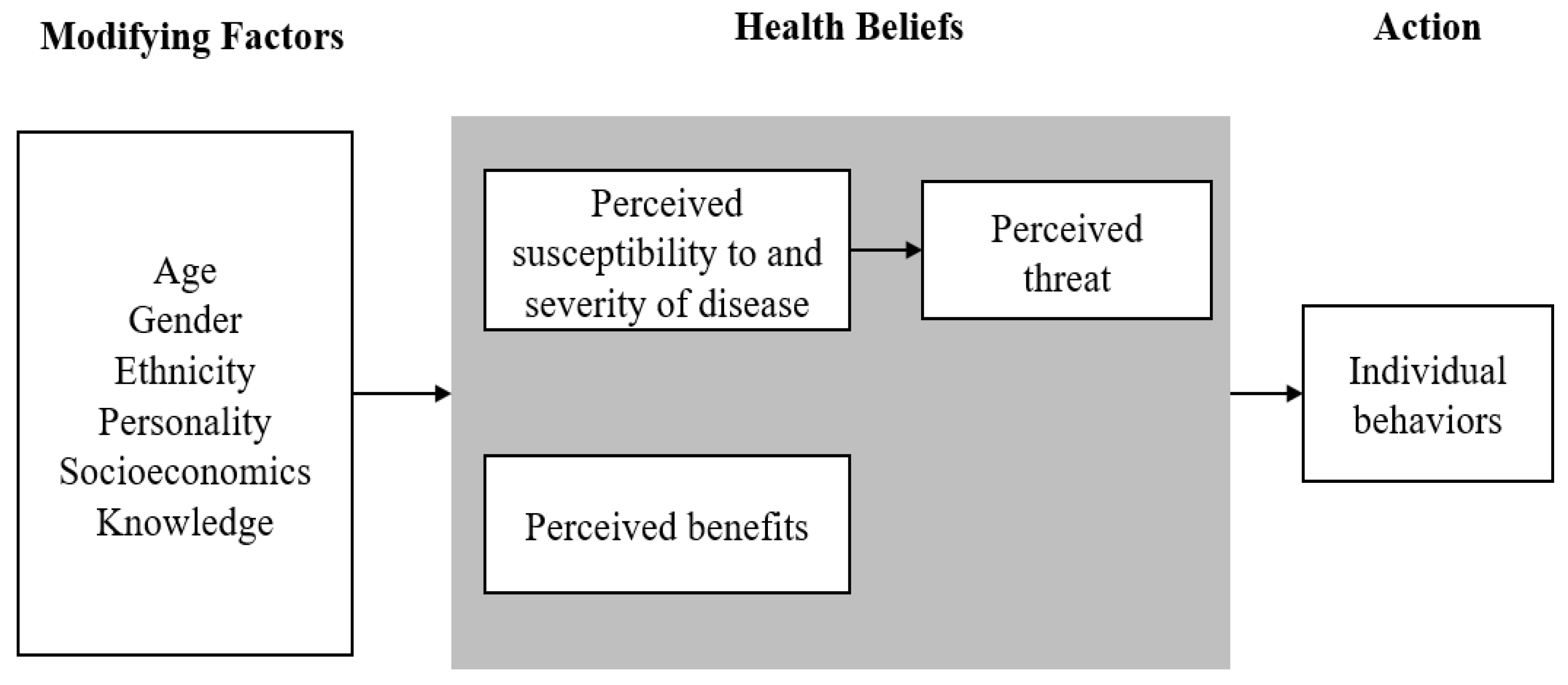
3.2. Health Beliefs of COVID-19
3.3. Acceptance of COVID-19 Vaccine
3.4. Factors Associated with Vaccination Acceptance
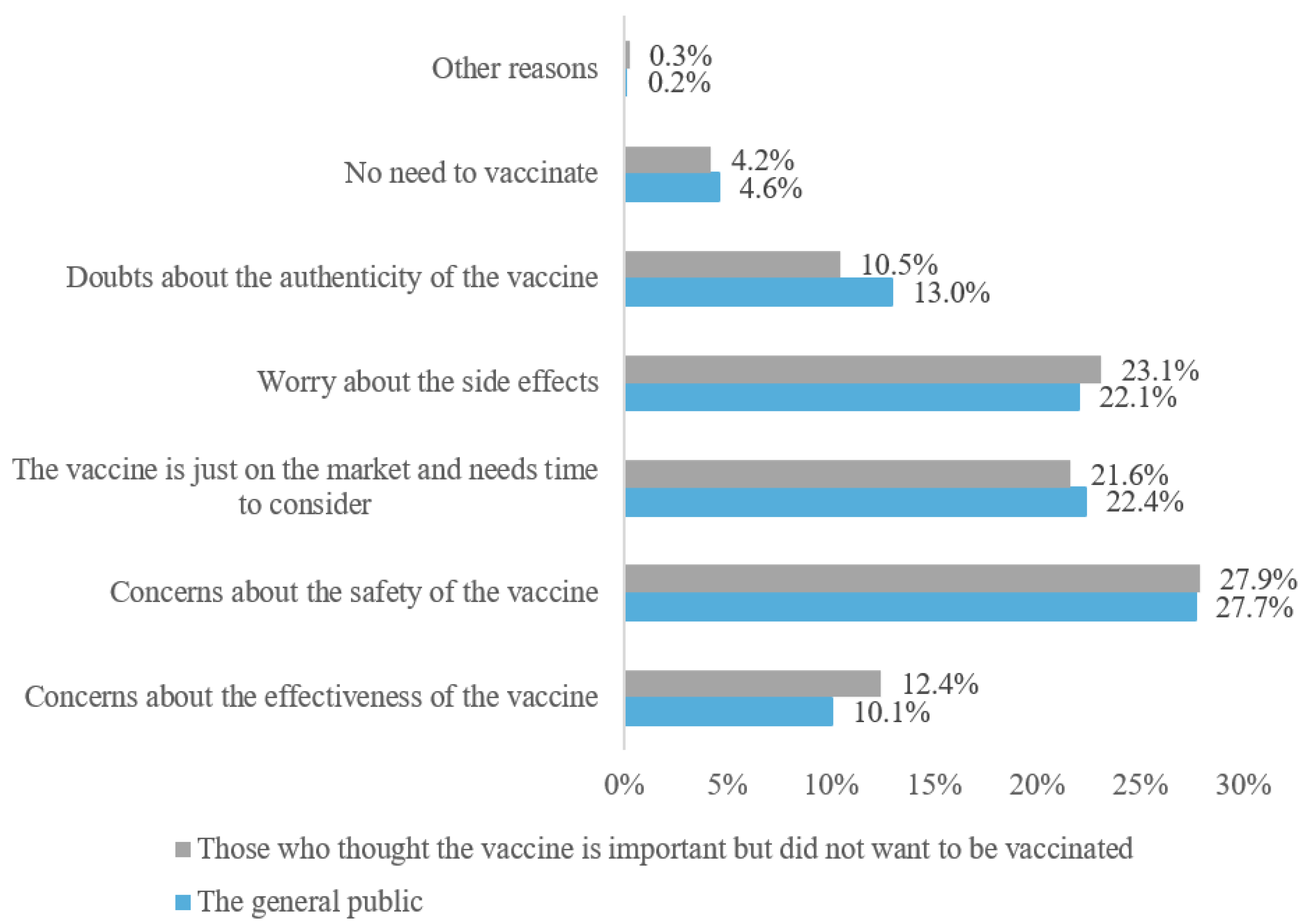
3.5. Specific Reasons for Rejecting Vaccine
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Al-Hanawi, M.K.; Mwale, M.L.; Alshareef, N.; Qattan, A.M.; Angawi, K.; Almubark, R.; Alsharqi, O. Psychological distress amongst health workers and the general public during the COVID-19 pandemic in Saudi Arabia. Risk Manag. Healthc. Policy 2020, 13, 733. [Google Scholar] [CrossRef] [PubMed]
- Lazarus, J.V.; Ratzan, S.C.; Palayew, A.; Gostin, L.O.; Larson, H.J.; Rabin, K.; Kimball, S.; EI-Mohandes, A. A global survey of potential acceptance of a COVID-19 vaccine. Nat. Med. 2021, 27, 225–228. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [Green Version]
- Wang, J.; Jing, R.; Lai, X.; Zhang, H.; Lyu, Y.; Knoll, M.D.; Fang, H. Acceptance of COVID-19 Vaccination during the COVID-19 Pandemic in China. Vaccines 2020, 8, 482. [Google Scholar] [CrossRef] [PubMed]
- Tobaiqy, M.; Qashqary, M.; Al-Dahery, S.; Mujallad, A.; Hershan, A.A.; Kamal, M.A.; Helmi, N. Therapeutic management of patients with COVID-19: A systematic review. Infect. Prev. Pract. 2020, 2, 100061. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Yu, C. The role of masks and respirator protection against SARS-CoV-2. Infect. Control. Hosp. Epidemiol. 2020, 41, 746–747. [Google Scholar] [CrossRef] [Green Version]
- Noh, J.Y.; Seong, H.; Yoon, J.G.; Song, J.Y.; Cheong, H.J.; Kim, W.J. Social distancing against COVID-19: Implication for the control of influenza. J. Korean Med. Sci. 2020, 35, e182. [Google Scholar] [CrossRef] [PubMed]
- Jang, W.M.; Jang, D.H.; Lee, J.Y. Social distancing and transmission-reducing practices during the 2019 coronavirus disease and 2015 Middle East respiratory syndrome coronavirus outbreaks in Korea. J. Korean Med. Sci. 2020, 35, e220. [Google Scholar] [CrossRef]
- Lurie, N.; Saville, M.; Hatchett, R.; Halton, J. Developing Covid-19 vaccines at pandemic speed. N. Engl. J. Med. 2020, 382, 1969–1973. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Peng, F.; Wang, R.; Guan, K.; Jiang, T.; Xu, G.; Sun, J.; Chang, C. The deadly coronaviruses: The 2003 SARS pandemic and the 2020 novel coronavirus epidemic in China. J. Autoimmun. 2020, 109, 102434. [Google Scholar] [CrossRef] [PubMed]
- Qualls, N.; Levitt, A.; Kanade, N.; Wright-Jegede, N.; Dopson, S.; Biggerstaff, M.; Reed, C.; Uzicanin, A. Community mitigation guidelines to prevent pandemic influenza—United States, 2017. MMWR Recomm. Rep. 2017, 66, 1–32. [Google Scholar] [CrossRef]
- Bish, A.; Yardley, L.; Nicoll, A.; Michie, S. Factors associated with uptake of vaccination against pandemic influenza: A systematic review. Vaccine 2011, 29, 6472–6484. [Google Scholar] [CrossRef] [PubMed]
- Le, T.T.; Andreadakis, Z.; Kumar, A.; Román, R.G.; Tollefsen, S.; Saville, M.; Mayhew, S. The COVID-19 vaccine development landscape. Nat. Rev. Drug Discov. 2020, 19, 305–306. [Google Scholar] [CrossRef] [PubMed]
- Sharpe, H.R.; Gilbride, C.; Allen, E.; Belij-Rammerstorfer, S.; Bissett, C.; Ewer, K.; Lambe, T. The early landscape of coronavirus disease 2019 vaccine development in the UK and rest of the world. Immunology 2020, 160, 223–232. [Google Scholar] [CrossRef] [PubMed]
- Machida, M.; Nakamura, I.; Kojima, T.; Saito, R.; Nakaya, T.; Hanibuchi, T.; Takamiya, T.; Odagiri, Y.; Fukushima, N.; Kikuchi, H. Acceptance of a COVID-19 Vaccine in Japan during the COVID-19 Pandemic. Vaccines 2021, 9, 210. [Google Scholar] [CrossRef]
- Trogen, B.; Oshinsky, D.; Caplan, A. Adverse consequences of rushing a SARS-CoV-2 vaccine: Implications for public trust. JAMA 2020, 323, 2460–2461. [Google Scholar] [CrossRef] [PubMed]
- Hotez, P.J.; Nuzhath, T.; Colwell, B. Combating vaccine hesitancy and other 21st century social determinants in the global fight against measles. Curr. Opin. Virol. 2020, 41, 1–7. [Google Scholar] [CrossRef]
- Jarrett, C.; Wilson, R.; O’Leary, M.; Eckersberger, E.; Larson, H. SAGE Working Group on Vaccine Hesitancy. Strategies for addressing vaccine hesitancy—A systematic review. Vaccine 2015, 33, 4180–4190. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dror, A.A.; Eisenbach, N.; Taiber, S.; Morozov, N.G.; Mizrachi, M.; Zigron, A.; Srouji, A.; Sela, E. Vaccine hesitancy: The next challenge in the fight against COVID-19. Eur. J. Epidemiol. 2020, 35, 775–779. [Google Scholar] [CrossRef]
- Wong, L.P.; Alias, H.; Wong, P.F.; Lee, H.Y.; AbuBakar, S. The use of the health belief model to assess predictors of intent to receive the COVID-19 vaccine and willingness to pay. Hum. Vaccines Immunother. 2020, 16, 2204–2214. [Google Scholar] [CrossRef]
- Neumann-Böhme, S.; Varghese, N.E.; Sabat, I.; Barros, P.P.; Brouwer, W.; van Exel, J.; Schreyögg, J.; Stargardt, T. Once we have it, will we use it? A European survey on willingness to be vaccinated against COVID-19. Eur. J. Health Econ. 2020, 21, 977–982. [Google Scholar] [CrossRef] [PubMed]
- Malik, A.A.; McFadden, S.M.; Elharake, J.; Omer, S.B. Determinants of COVID-19 vaccine acceptance in the US. EClinicalMedicine 2020, 26, 100495. [Google Scholar] [CrossRef]
- Dodd, R.H.; Cvejic, E.; Bonner, C.; Pickles, K.; McCaffery, K.J.; Ayre, J.; Batcup, C.; Copp, T.; Cornell, S.; Dakin, T. Willingness to vaccinate against COVID-19 in Australia. Lancet Infect. Dis. 2021, 21, 318–319. [Google Scholar] [CrossRef]
- Rosenstock, I.M. The health belief model and preventive health behavior. Health Educ. Monogr. 1974, 2, 354–386. [Google Scholar] [CrossRef]
- Barakat, A.M.; Kasemy, Z.A. Preventive health behaviours during coronavirus disease 2019 pandemic based on health belief model among Egyptians. Middle East Curr. Psychiatry 2020, 27, 1–9. [Google Scholar] [CrossRef]
- Champion, V.L.; Skinner, C.S. The health belief model. In Health Behavior and Health Education: Theory, Research, and Practice; Jossey-Bass: San Francisco, CA, USA, 2008; Volume 4, pp. 45–65. [Google Scholar]
- Slovic, P. Perception of risk. Science 1987, 236, 280–285. [Google Scholar] [CrossRef] [PubMed]
- Fougeroux, C.; Holst, P.J. Future prospects for the development of cost-effective adenovirus vaccines. Int. J. Mol. Sci. 2017, 18, 686. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mello, M.M.; Silverman, R.D.; Omer, S.B. Ensuring uptake of vaccines against SARS-CoV-2. N. Engl. J. Med. 2020, 383, 1296–1299. [Google Scholar] [CrossRef] [PubMed]
- Opel, D.J.; Diekema, D.S.; Ross, L.F. Should we mandate a COVID-19 vaccine for children? JAMA Pediatr. 2021, 175, 125–126. [Google Scholar] [CrossRef] [PubMed]
- Kreps, S.; Prasad, S.; Brownstein, J.S.; Hswen, Y.; Garibaldi, B.T.; Zhang, B.; Kriner, D.L. Factors associated with US adults’ likelihood of accepting COVID-19 vaccination. JAMA Netw. Open 2020, 3, e2025594. [Google Scholar] [CrossRef]
- Lin, Y.; Hu, Z.; Zhao, Q.; Alias, H.; Danaee, M.; Wong, L.P. Understanding COVID-19 vaccine demand and hesitancy: A nationwide online survey in China. PLoS Negl. Trop. Dis. 2020, 14, e0008961. [Google Scholar] [CrossRef]
- Yin, F.; Wu, Z.; Xia, X.; Ji, M.; Wang, Y.; Hu, Z. Unfolding the determinants of COVID-19 vaccine acceptance in China. J. Med Internet Res. 2021, 23, e26089. [Google Scholar] [CrossRef]
- Li, Y.; Tenchov, R.; Smoot, J.; Liu, C.; Watkins, S.; Zhou, Q. A comprehensive review of the global efforts on COVID-19 vaccine development. ACS Cent. Sci. 2021, 7, 512–533. [Google Scholar] [CrossRef]
- Zheng, W.; Yan, X.; Zhao, Z.; Yang, J.; Yu, H. COVID-19 Vaccination Program in China: A Subnational Descriptive Analysis on Target Population Size and Current Progress. Infect. Dis. Poverty 2021, 10, 124. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Yue, X.-G.; Tchounwou, P.B. Response to the COVID-19 epidemic: The Chinese experience and implications for other countries. Nt. J. Environ. Res. Public Health 2020, 17, 2304. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- William, F.; Vásquez, J.M.T. Will Americans Get Vaccinated? Predicting COVID-19 Vaccine Uptake Rates Under Contingent Scenarios. Value Health 2021, 24, 1543–1550. [Google Scholar]
- Bell, S.; Clarke, R.; Mounier-Jack, S.; Walker, J.L.; Paterson, P. Parents’ and guardians’ views on the acceptability of a future COVID-19 vaccine: A multi-methods study in England. Vaccine 2020, 38, 7789–7798. [Google Scholar] [CrossRef]
- Graffigna, G.; Palamenghi, L.; Boccia, S.; Barello, S. Relationship between citizens’ health engagement and intention to take the COVID-19 vaccine in Italy: A mediation analysis. Vaccines 2020, 8, 576. [Google Scholar] [CrossRef] [PubMed]
- Barello, S.; Nania, T.; Dellafiore, F.; Graffigna, G.; Caruso, R. ‘Vaccine hesitancy’among university students in Italy during the COVID-19 pandemic. Eur. J. Epidemiol. 2020, 35, 781–783. [Google Scholar] [CrossRef]
- Detoc, M.; Bruel, S.; Frappe, P.; Tardy, B.; Botelho-Nevers, E.; Gagneux-Brunon, A. Intention to participate in a COVID-19 vaccine clinical trial and to get vaccinated against COVID-19 in France during the pandemic. Vaccine 2020, 38, 7002–7006. [Google Scholar] [CrossRef]
- Gagneux-Brunon, A.; Detoc, M.; Bruel, S.; Tardy, B.; Rozaire, O.; Frappe, P.; Botelho-Nevers, E. Intention to get vaccinations against COVID-19 in French healthcare workers during the first pandemic wave: A cross-sectional survey. J. Hosp. Infect. 2021, 108, 168–173. [Google Scholar] [CrossRef] [PubMed]
- Murphy, J.; Vallières, F.; Bentall, R.P.; Shevlin, M.; McBride, O.; Hartman, T.K.; McKay, R.; Bennett, K.; Mason, L.; Gibson-Miller, J. Psychological characteristics associated with COVID-19 vaccine hesitancy and resistance in Ireland and the United Kingdom. Nat. Commun. 2021, 12, 1–15. [Google Scholar] [CrossRef]
- Ditekemena, J.D.; Nkamba, D.M.; Mavoko, A.M.; Hypolite, M.; Siewe Fodjo, J.N.; Luhata, C.; Obimpeh, M.; Van Hees, S.; Nachega, J.B.; Colebunders, R. COVID-19 vaccine acceptance in the Democratic Republic of Congo: A cross-sectional survey. Vaccines 2021, 9, 153. [Google Scholar] [CrossRef]
- Eguia, H.; Vinciarelli, F.; Bosque-Prous, M.; Kristensen, T.; Saigí-Rubió, F. Spain’s Hesitation at the Gates of a COVID-19 Vaccine. Vaccines 2021, 9, 170. [Google Scholar] [CrossRef]
- Dryhurst, S.; Schneider, C.R.; Kerr, J.; Freeman, A.L.; Recchia, G.; Van Der Bles, A.M.; Spiegelhalter, D.; Van Der Linden, S. Risk perceptions of COVID-19 around the world. J. Risk Res. 2020, 23, 994–1006. [Google Scholar] [CrossRef]
- Ding, Z.; Xie, L.; Guan, A.; Huang, D.; Mao, Z.; Liang, X. Global COVID-19: Warnings and suggestions based on experience of China. J. Glob. Health 2020, 10, 11005. [Google Scholar] [CrossRef]
- Guo, Y.; Li, Y.; Monroe-Wise, A.; Yeung, S.-C.J.; Huang, Y. A dynamic residential community-based quarantine strategy: China’s experience in fighting COVID-19. Infect. Control. Hosp. Epidemiol. 2020, 41, 1363–1364. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tian, W. How China managed the COVID-19 pandemic. Asian Econ. Pap. 2021, 20, 75–101. [Google Scholar] [CrossRef]
- Jin, H.; Lu, L.; Liu, J.; Cui, M. COVID-19 emergencies around the globe: China’s experience in controlling COVID-19 and lessons learned. Int. J. Qual. Health Care 2021, 33, mzaa143. [Google Scholar] [CrossRef] [PubMed]
- Dimaschko, J.; Shlyakhover, V.; Iabluchanskyi, M. Why did the COVID-19 Epidemic Stop in China and does not Stop in the Rest of the World? (Application of the Two-Component Model). SciMed. J. 2021, 3, 88–99. [Google Scholar] [CrossRef]
- Reno, C.; Maietti, E.; Fantini, M.P.; Savoia, E.; Manzoli, L.; Montalti, M.; Gori, D. Enhancing COVID-19 Vaccines Acceptance: Results from a Survey on Vaccine Hesitancy in Northern Italy. Vaccines 2021, 9, 378. [Google Scholar] [CrossRef]
- Wang, K.; Wong, E.L.-Y.; Ho, K.-F.; Cheung, A.W.-L.; Yau, P.S.-Y.; Dong, D.; Wong, S.S.-Y.; Yeoh, E.-K. Change of willingness to accept COVID-19 vaccine and reasons of vaccine hesitancy of working people at different waves of local epidemic in Hong Kong, China: Repeated cross-sectional surveys. Vaccines 2021, 9, 62. [Google Scholar] [CrossRef]
- Hotez, P. America and Europe’s new normal: The return of vaccine-preventable diseases. Pediatr. Res. 2019, 85, 912–914. [Google Scholar] [CrossRef] [PubMed]
- Burki, T. The online anti-vaccine movement in the age of COVID-19. Lancet Digit. Health 2020, 2, e504–e505. [Google Scholar] [CrossRef]
- Johnson, N.F.; Velásquez, N.; Restrepo, N.J.; Leahy, R.; Gabriel, N.; El Oud, S.; Zheng, M.; Manrique, P.; Wuchty, S.; Lupu, Y. The online competition between pro-and anti-vaccination views. Nature 2020, 582, 230–233. [Google Scholar] [CrossRef] [PubMed]
- Frank, K.; Arim, R. Canadians’ Willingness to Get a COVID-19 Vaccine When One Becomes Available: What Role Does Trust Play? Available online: https://www150.statcan.gc.ca/n1/pub/45-28-0001/2020001/article/00043-eng.htm (accessed on 31 May 2021).
- Shekhar, R.; Sheikh, A.B.; Upadhyay, S.; Singh, M.; Kottewar, S.; Mir, H.; Barrett, E.; Pal, S. COVID-19 vaccine acceptance among health care workers in the United States. Vaccines 2021, 9, 119. [Google Scholar] [CrossRef]
- Frederiksen, L.S.F.; Zhang, Y.; Foged, C.; Thakur, A. The long road toward COVID-19 herd immunity: Vaccine platform technologies and mass immunization strategies. Front. Immunol. 2020, 11, 1817. [Google Scholar] [CrossRef]
| Dimension | Item | ||
|---|---|---|---|
| Risk perception of COVID-19 | Dread risk | There is a high risk of death when infected with COVID-19 | 2.93 ± 1.28 |
| COVID-19 has had a big impact on my life | 3.04 ± 1.25 | ||
| Uncontrollable | COVID-19 will become increasingly dangerous | 2.71 ± 1.20 | |
| If contracted COVID-19, it can affect the next generation | 2.80 ± 1.22 | ||
| Unknown risk | Scientists do not yet fully understand the COVID-19 | 2.79 ± 1.24 | |
| Uncertainty | There is no telling how long COVID-19 will continue to prevail | 3.00 ± 1.25 | |
| Cognition of COVID-19 vaccine | Vaccination is important to against COVID-19 | 3.98 ± 1.13 | |
| Variables | Willingness to Accept a COVID-19 Vaccine | ||||
|---|---|---|---|---|---|
| Yes (N = 3568) N (%) | No (N = 372) N (%) | Total N (%) | Chi-Square | p-Value | |
| Region of residence | |||||
| Rural | 492 (88.8) | 62 (11.2) | 554(14.1) | 2.31 | 0.129 |
| Urban | 3076 (90.8) | 310 (9.2) | 3386 (85.9) | ||
| Sex | |||||
| Male | 2072 (90.4) | 221 (9.6) | 2293 (58.2) | 0.25 | 0.619 |
| Female | 1496 (90.8) | 151 (9.2) | 1647 (41.8) | ||
| Age | |||||
| 18–25 | 872 (92.4) | 72 (7.6) | 944 (24.0) | 17.48 | 0.002 |
| 26–30 | 1276 (91.8) | 114 (8.2) | 1390 (35.3) | ||
| 31–40 | 982 (87.8) | 136 (12.2) | 1118 (28.4) | ||
| 41–50 | 319 (88.9) | 40 (11.1) | 359 (9.1) | ||
| >50 | 119 (92.3) | 10 (7.7) | 129 (3.2) | ||
| Marital status | |||||
| Single | 415 (91.0) | 41 (9.0) | 456 (11.6) | 34.82 | <0.001 |
| Married | 2988 (91.2) | 287 (8.8) | 3275 (83.1) | ||
| Divorced/widowed | 165 (79.0) | 44 (21.0) | 209 (5.3) | ||
| Ethnicity | |||||
| Non-minority | 3321 (90.9) | 333 (9.1) | 3654 (92.7) | 6.35 | 0.012 |
| Minority | 247 (86.4) | 39 (13.6) | 286 (7.3) | ||
| Graduate | |||||
| Middle school and below | 521 (85.4) | 89 (14.6) | 610 (15.5) | 45.81 | <0.001 |
| High school | 987 (90.6) | 102 (9.4) | 1089 (27.6) | ||
| Associate or bachelor | 1960 (92.6) | 156 (7.4) | 2116 (53.7) | ||
| Master and above | 100 (80.0) | 25 (20.0) | 125 (3.2) | ||
| Number of family members | |||||
| 1 | 47 (87.0) | 7 (13.0) | 54 (1.4) | 16.29 | <0.001 |
| 2 | 257 (89.2) | 31 (10.8) | 288 (7.2) | ||
| 3–5 | 2824 (91.5) | 263 (8.5) | 3087 (78.4) | ||
| ≥6 | 440 (86.1) | 71 (13.9) | 511 (13.0) | ||
| Occupation | |||||
| Government employee | 241 (87.0) | 36 (13.0) | 277 (7.0) | 10.29 | 0.113 |
| Non-government employee | 990 (90.7) | 102 (9.3) | 1092 (27.7) | ||
| Flexible-job worker | 1402 (91.7) | 126 (8.3) | 1528 (38.8) | ||
| Self-employed | 503 (88.6) | 65 (11.4) | 568 (14.4) | ||
| Farmer | 87 (88.8) | 11 (11.2) | 98 (2.5) | ||
| Student | 271 (91.9) | 24 (8.1) | 295 (7.5) | ||
| Retired/unemployed | 74 (90.2) | 8 (9.8) | 82 (2.1) | ||
| Annual income | |||||
| CNY24,000 | 417 (92.1) | 36 (7.9) | 453 (11.5) | 70.41 | <0.001 |
| CNY24,000–60,000 | 1406 (93.7) | 95 (6.3) | 1501 (38.1) | ||
| CNY60,000–120,000 | 1127 (90.2) | 122 (9.8) | 1249 (31.7) | ||
| CNY120,000–240,000 | 441 (86.1) | 71 (13.9) | 512 (13.0) | ||
| CNY240,000–360,000 | 134 (80.7) | 32 (19.3) | 166 (4.2) | ||
| Above CNY360,000 | 43 (72.9) | 16 (27.1) | 59 (1.5) | ||
| Experienced major infectious events | |||||
| No | 1206 (89.3) | 144 (10.7) | 1350 (34.3) | 3.60 | 0.058 |
| Yes | 2362 (91.2) | 228 (8.8) | 2590 (65.7) | ||
| Perceived risk of COVID-19 | |||||
| High (21–30) | 514 (96.6) | 18 (3.4) | 532 (13.5) | 34.50 | <0.001 |
| Middle (11–20) | 2188 (90.5) | 229 (9.5) | 2417 (61.4) | ||
| Low (6–10) | 866 (87.4) | 125 (12.6) | 991 (25.1) | ||
| Do you think vaccination is important to against COVID-19 | |||||
| Not important | 330 (71.4) | 132 (28.6) | 462 (11.7) | 224.01 | <0.001 |
| important | 3238 (93.1) | 240 (6.9) | 3478 (88.3) | ||
| Characteristics | OR | SE | p-Value | 95%CI |
|---|---|---|---|---|
| Region of residence | ||||
| Rural | Ref | |||
| Urban | 1.59 | 0.28 | 0.009 | 1.12–2.24 |
| Sex | ||||
| Male | Ref | |||
| Female | 1.19 | 0.15 | 0.156 | 0.93–1.53 |
| Age | ||||
| 18–25 | Ref | |||
| 26–30 | 1.13 | 0.24 | 0.566 | 0.75–1.71 |
| 31–40 | 0.86 | 0.19 | 0.475 | 0.56–1.31 |
| 41–50 | 0.72 | 0.20 | 0.229 | 0.43–1.23 |
| >50 | 1.15 | 0.51 | 0.750 | 0.49–2.73 |
| Marital status | ||||
| Single | Ref | |||
| Married | 1.28 | 0.35 | 0.372 | 0.75–2.19 |
| Divorced/widowed | 0.58 | 0.19 | 0.103 | 0.29–1.12 |
| Ethnicity | ||||
| Non-minority | Ref | |||
| Minority | 0.63 | 0.14 | 0.038 | 0.41–0.98 |
| Graduate | ||||
| Middle school and below | Ref | |||
| High school | 1.35 | 0.24 | 0.101 | 0.94–1.92 |
| Associated or bachelor | 1.40 | 0.24 | 0.050 | 0.99–1.96 |
| Master and above | 0.72 | 0.23 | 0.300 | 0.39–1.34 |
| Number of family members | ||||
| 1 | Ref | |||
| 2 | 1.50 | 0.77 | 0.428 | 0.55–4.11 |
| 3–5 | 1.69 | 0.80 | 0.268 | 0.67–4.29 |
| ≥6 | 1.21 | 0.59 | 0.693 | 0.46–3.18 |
| Occupation | ||||
| Government employee | Ref | |||
| Nongovernment employee | 1.06 | 0.28 | 0.782 | 0.66–1.71 |
| Flexible-job worker | 1.14 | 0.27 | 0.564 | 0.72–1.85 |
| Self-employed | 0.94 | 0.25 | 0.802 | 0.56–1.57 |
| Farmer | 1.08 | 0.47 | 0.856 | 0.46–2.54 |
| Student | 1.23 | 0.59 | 0.666 | 0.48–3.16 |
| Retired/unemployed | 0.68 | 0.34 | 0.440 | 0.25–1.83 |
| Annual income | ||||
| CNY24,000 | Ref | |||
| CNY24,000–60,000 | 0.77 | 0.24 | 0.405 | 0.41–1.43 |
| CNY60,000–120,000 | 0.59 | 0.19 | 0.105 | 0.31–1.12 |
| CNY24,000–60,000 | 0.63 | 0.21 | 0.169 | 0.32–1.21 |
| CNY240,000–36,000 | 0.59 | 0.23 | 0.185 | 0.28–1.28 |
| Above CNY360,000 | 0.38 | 0.18 | 0.040 | 0.15–0.96 |
| Experienced major infectious events | ||||
| No | Ref | |||
| Yes | 2.37 | 0.35 | <0.001 | 1.77–3.17 |
| Perceived risk of COVID-19 | ||||
| High (21–30) | Ref | |||
| Middle (11–20) | 0.37 | 0.11 | <0.001 | 0.17–0.65 |
| Low (6–10) | 0.32 | 0.09 | <0.001 | 0.18–0.58 |
| Do you think vaccination is important to against COVID-19 | ||||
| Not important | Ref | |||
| Important | 3.76 | 0.59 | <0.001 | 2.76–5.11 |
| Number of confirmed or suspected cases in the county | 0.99 | 0.03 | 0.657 | 0.93–1.05 |
| Population density | 1.00 | 0.01 | 0.940 | 0.99–1.01 |
| Urbanization rate | 1.01 | 0.013 | 0.481 | 0.98–1.03 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhou, Q.; Tian, T.; Ni, J.; Zhao, X.; Li, H.; Yang, Y.; Zhang, Y.; Pan, J. COVID-19 Vaccination Acceptance in China after It Becomes Available: A Cross-Sectional Study. Vaccines 2021, 9, 1398. https://doi.org/10.3390/vaccines9121398
Zhou Q, Tian T, Ni J, Zhao X, Li H, Yang Y, Zhang Y, Pan J. COVID-19 Vaccination Acceptance in China after It Becomes Available: A Cross-Sectional Study. Vaccines. 2021; 9(12):1398. https://doi.org/10.3390/vaccines9121398
Chicago/Turabian StyleZhou, Qian, Tian Tian, Jie Ni, Xiaoheng Zhao, Hong Li, Yili Yang, Yumeng Zhang, and Jay Pan. 2021. "COVID-19 Vaccination Acceptance in China after It Becomes Available: A Cross-Sectional Study" Vaccines 9, no. 12: 1398. https://doi.org/10.3390/vaccines9121398
APA StyleZhou, Q., Tian, T., Ni, J., Zhao, X., Li, H., Yang, Y., Zhang, Y., & Pan, J. (2021). COVID-19 Vaccination Acceptance in China after It Becomes Available: A Cross-Sectional Study. Vaccines, 9(12), 1398. https://doi.org/10.3390/vaccines9121398






