Factors Associated with COVID-19 Vaccine Intentions in Eastern Zimbabwe: A Cross-Sectional Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Statistical Analysis
2.3. Ethical Considerations
3. Results
3.1. Sociodemographic Characteristics
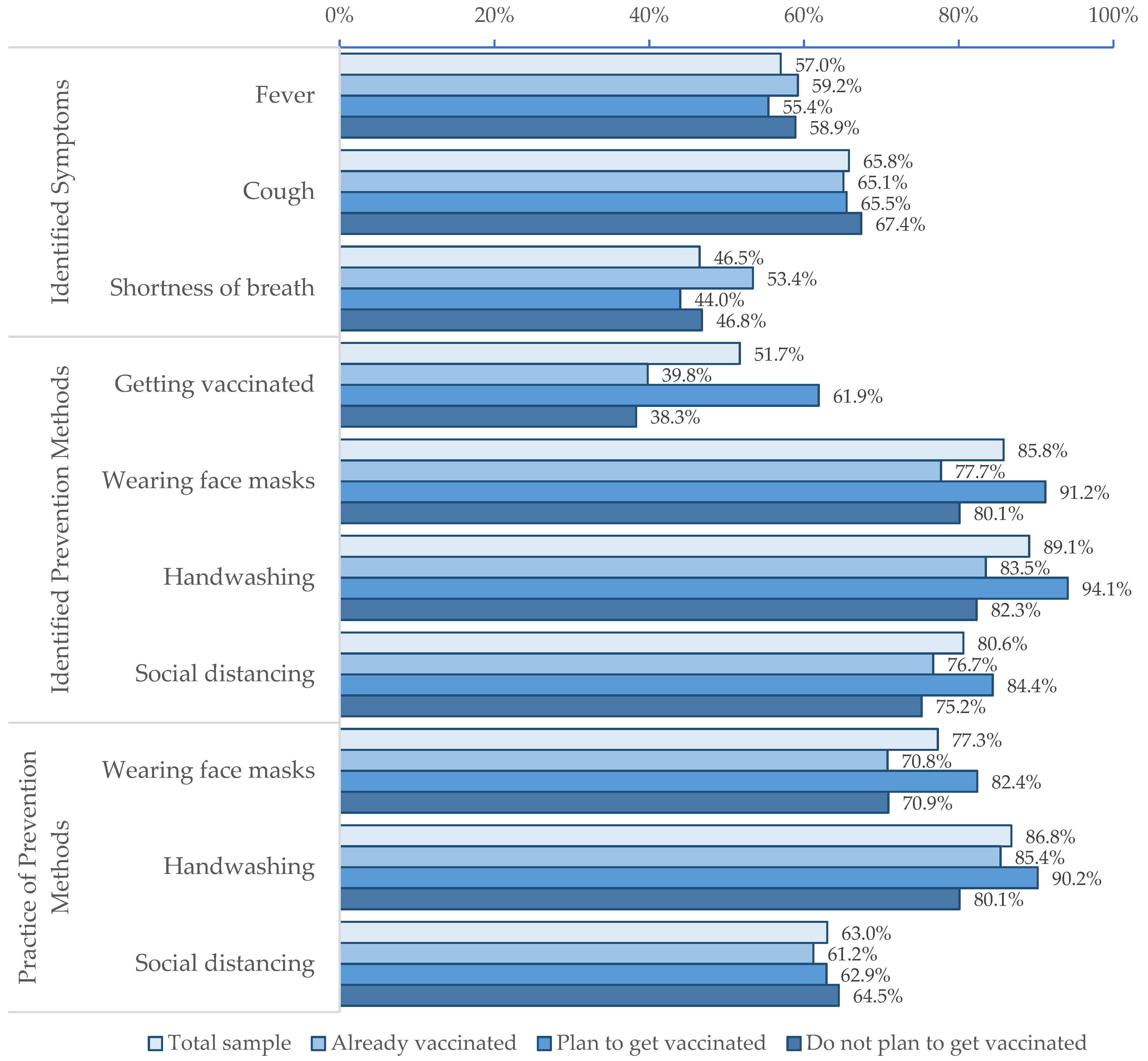
3.2. COVID-19 Knowledge, Attitudes, and Behaviors
3.3. Factors Associated with Vaccine Intentions
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- WHO Coronavirus (COVID-19) Dashboard|WHO Coronavirus (COVID-19) Dashboard with Vaccination Data. 2021. Available online: https://covid19.who.int/ (accessed on 31 August 2021).
- World Health Organization. Rational Use of Personal Protective Equipment for Coronavirus Disease (COVID-19): Interim Guidance, 27 February 2020. 2020. Available online: https://apps.who.int/iris/bitstream/handle/10665/331498/WHO-2019-nCoV-IPCPPE_use-2020.2-eng.pdf (accessed on 31 August 2021).
- The Lancet. Access to COVID-19 vaccines: Looking beyond COVAX. Lancet 2021, 397, 941. [Google Scholar] [CrossRef]
- UNICEF. COVID-19 Vaccine Market Dashboard. 2021. Available online: https://www.unicef.org/supply/covid-19-vaccine-market-dashboard (accessed on 31 August 2021).
- Nachega, J.B.; Sam-Agudu, N.A.; Masekela, R.; van der Zalm, M.M.; Nsanzimana, S.; Condo, J.; Ntoumi, F.; Rabie, H.; Kruger, M.; Wiysonge, C.S.; et al. Addressing challenges to rolling out COVID-19 vaccines in African countries. Lancet Glob. Health 2021, 9, 746–748. [Google Scholar] [CrossRef]
- Loembé, M.M.; Nkengasong, J.N. COVID-19 vaccine access in Africa: Global distribution, vaccine platforms, and challenges ahead. Immunity 2021, 54, 1353–1362. [Google Scholar] [CrossRef] [PubMed]
- Wouters, O.J.; Shadlen, K.C.; Salcher-Konrad, M.; Pollard, A.; Larson, H.; Teerawattananon, Y.; Jit, M. Challenges in ensuring global access to COVID-19 vaccines: Production, affordability, allocation, and deployment. Lancet 2021, 397, 1023–1034. [Google Scholar] [CrossRef]
- Sallam, M. COVID-19 vaccine hesitancy worldwide: A concise systematic review of vaccine acceptance rates. Vaccines 2021, 9, 160. [Google Scholar] [CrossRef] [PubMed]
- MacDonald, N.E.; Eskola, J.; Liang, X.; Chaudhuri, M.; Dube, E.; Gellin, B.; Goldstein, S.; Larson, H.; Manzo, M.; Reingold, A.; et al. Vaccine hesitancy: Definition, scope and determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef] [PubMed]
- Ekwebelem, O.C.; Yunusa, I.; Onyeaka, H.; Ekwebelem, N.C.; Nnorom-Dike, O. COVID-19 vaccine rollout: Will it affect the rates of vaccine hesitancy in Africa? Public Health 2021, 197, e18–e19. [Google Scholar] [CrossRef] [PubMed]
- Matos, C.C.S.A.; Gonçalves, B.A.; Couto, M.T. Vaccine hesitancy in the global south: Towards a critical perspective on global health. Glob Public Health 2021, 37, 2079–2089. [Google Scholar] [CrossRef]
- Machekanyanga, Z.; Ndiaye, S.; Gerede, R.; Chindedza, K.; Chigodo, C.; Shibeshi, M.E.; Goodson, J.; Daniel, F.; Zimmerman, L.; Kaiser, R. Qualitative assessment of vaccination hesitancy among members of the apostolic church of Zimbabwe: A case study. J. Relig. Health 2017, 56, 1683–1691. [Google Scholar] [CrossRef]
- Wagner, A.L.; Masters, N.B.; Domek, G.J.; Mathew, J.L.; Sun, X.; Asturias, E.J.; Ren, J.; Huang, Z.; Contreras-Roldan, I.L.; Gebremeskel, B.; et al. Comparisons of Vaccine Hesitancy Across Five Low-And Middle-Income Countries. Vaccines. 2019, 7, 155. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dubé, E.; Laberge, C.; Guay, M.; Bramadat, P.; Roy, R.; Bettinger, J. Vaccine hesitancy: An overview. Hum Vaccin Immunother. 2013, 9, 1763–1773. [Google Scholar] [CrossRef]
- Adamu, A.A.; Essoh, T.A.; Adeyanju, G.C.; Jalo, R.I.; Saleh, Y.; Aplogan, A.; Wiysonge, C.S. Drivers of hesitancy towards recommended childhood vaccines in African settings: A scoping review of literature from Kenya, Malawi and Ethiopia. Expert Rev. Vaccines 2021, 20, 611–621. [Google Scholar] [CrossRef] [PubMed]
- Dula, J.; Mulhanga, A.; Nhanombe, A.; Cumbi, L.; Júnior, A.; Gwatsvaira, J.; Fodjo, J.N.S.; Faria de Moura Villela, E.; Chicumbe, S.; Colebunders, R. COVID-19 Vaccine Acceptability and Its Determinants in Mozambique: An Online Survey. Vaccines 2021, 9, 828. [Google Scholar] [CrossRef]
- Roozenbeek, J.; Schneider, C.R.; Dryhurst, S.; Kerr, J.; Freeman, A.L.; Recchia, G.; Van Der Bles, A.M.; Van Der Linden, S. Susceptibility to misinformation about COVID-19 around the world. R. Soc. Open Sci. 2020, 7, 201199. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.; Tu, P.; Beitsch, L.M. Confidence and Receptivity for COVID-19 Vaccines: A Rapid Systematic Review. Vaccines 2021, 9, 16. [Google Scholar] [CrossRef] [PubMed]
- Acheampong, T.; Akorsikumah, E.A.; Osae-Kwapong, J.; Khalid, M.; Appiah, A.; Amuasi, J.H. Examining Vaccine Hesitancy in Sub-Saharan Africa: A Survey of the Knowledge and Attitudes among Adults to Receive COVID-19 Vaccines in Ghana. Vaccines 2021, 9, 814. [Google Scholar] [CrossRef]
- Tozivepi, S.N.; Mundagowa, P.; Tirivavi, M.; Maponga, B.; Mugwagwa, N.; Magande, P.; Mutseyekwa, F.; Makurumidze, R. Covid-19 Vaccine Hesitancy Survey Preliminary Report; Zimbabwe College of Public Health Physicians: Harare, Zimbabwe, 2020. [Google Scholar]
- Africa CDC-COVID 19 Vaccine Perceptions: A 15 Country Study. Available online: https://africacdc.org/download/covid-19-vaccine-perceptions-a-15-country-study/ (accessed on 31 August 2021).
- Heidari, S.; Goodman, T. Critical Sex and Gender Considerations for Equitable Research, Development and Delivery of COVID-19 Vaccines. 2021. Available online: https://www.who.int/publications/m/item/critical-sex-and-gender-considerations-for-equitable-research-development-and-delivery-of-covid-19-vaccines (accessed on 31 August 2021).
- Garcia, L.L.; Yap, J.F.C. The role of religiosity in COVID-19 vaccine hesitancy. J. Public Health 2021, 43, e529–e530. [Google Scholar] [CrossRef]
- Seydou, A. Who Wants COVID-19 Vaccination? In 5 West African Countries, Hesitancy Is High, Trust Low. Available online: https://afrobarometer.org/publications/ad432-who-wants-covid-19-vaccination-5-west-african-countries-hesitancy-high-trust-low (accessed on 29 August 2021).
- Dzinamarira, T.; Nachipo, B.; Phiri, B.; Musuka, G. COVID-19 Vaccine Roll-Out in South Africa and Zimbabwe: Urgent Need to Address Community Preparedness, Fears and Hesitancy. Vaccines 2021, 9, 250. [Google Scholar] [CrossRef]
- Our World In Data. COVID-19 Data Explorer. Available online: https://ourworldindata.org/coronavirus-data-explorer (accessed on 31 August 2021).
- Mundagowa, P.T.; Tozivepi, S.N.; Chiyaka, E.T.; Mukora-Mutseyekwa, F.; Makurumidze, R. Assessment of COVID-19 vaccine hesitancy among Zimbabweans: A rapid national survey. medRxiv 2021. [Google Scholar] [CrossRef]
- UN 2019 Revision of World Population Prospects; United Nations, Department of Economic and Social Affairs, Population Division: New York, NY, USA, 2019.
- Voice of America. Zimbabwe, China Allay Sinopharm COVID-19 Vaccine Fears. Available online: https://www.voanews.com/covid-19-pandemic/zimbabwe-china-allay-sinopharm-covid-19-vaccine-fears (accessed on 21 August 2021).
- Mavhunga, C. Government Urges Zimbabweans to Accept COVID-19 Vaccine. 2021. Available online: https://www.voanews.com/covid-19-pandemic/government-urges-zimbabweans-accept-covid-19-vaccine (accessed on 31 August 2021).
- Chigevenga, R. Commentary on the Zimbabwean People’s Response towards the Anticipated COVID-19 Vaccine. J. Biomed. Res. Environ. Sci. 2021, 2, 174–177. [Google Scholar] [CrossRef]
- Kreps, S.; Prasad, S.; Brownstein, J.S.; Hswen, Y.; Garibaldi, B.T.; Zhang, B.; Kriner, D.L. Factors Associated with US Adults’ Likelihood of Accepting COVID-19 Vaccination. JAMA Netw. Open 2020, 3, e2025594. [Google Scholar] [CrossRef]
- World Health Organization. WHO Validates Sinovac COVID-19 Vaccine for Emergency Use and Issues Interim Policy Recommendations. Available online: https://www.who.int/news/item/01-06-2021-who-validates-sinovac-covid-19-vaccine-for-emergency-use-and-issues-interim-policy-recommendations (accessed on 31 August 2021).
- Kriss, J.L.; Goodson, J.; Machekanyanga, Z.; Shibeshi, M.E.; Daniel, F.; Masresha, B.; Kaiser, R. Vaccine receipt and vaccine card availability among children of the apostolic faith: Analysis from the 2010–2011 Zimbabwe demographic and health survey. Pan Afr. Med. J. 2016, 24, 47. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Total | Vaccinated | Intend to Vaccinate | Do Not Intend to Vaccinate | p-Value |
|---|---|---|---|---|---|
| N | 551 | 103 | 307 | 141 | |
| Household head age | 0.4 | ||||
| 18–29 years | 137 (24.9%) | 24 (23.3%) | 81 (26.4%) | 32 (22.7%) | |
| 30–39 years | 136 (24.7%) | 23 (22.3%) | 84 (27.4%) | 29 (20.6%) | |
| 40–54 years | 142 (25.8%) | 24 (23.3%) | 84 (27.4%) | 34 (24.1%) | |
| ≥55 years | 136 (24.7%) | 32 (31.1%) | 58 (18.9%) | 46 (32.6%) | |
| Household head is male | 152 (27.6%) | 28 (27.2%) | 98 (31.9%) | 115 (81.6%) | 0.9 |
| Household head is married/co-habiting | 372 (67.5%) | 62 (60.2%) | 213 (69.4%) | 97 (68.8%) | 0.08 |
| Household head attended secondary school or higher | 379 (68.8%) | 81 (78.6%) | 220 (71.7%) | 78 (55.3%) | 0.02 |
| Household head is employed | 322 (58.4%) | 74 (71.8%) | 168 (54.7%) | 80 (56.7%) | 0.002 |
| Household has more than 4 members | 298 (54.1%) | 50 (48.5%) | 170 (55.4%) | 78 (55.3%) | 0.2 |
| District of residence | 0.008 | ||||
| Buhera | 211 (38.3%) | 27 (26.2%) | 123 (40.1%) | 61 (43.3%) | |
| Makoni | 119 (21.6%) | 22 (21.4%) | 64 (20.9%) | 33 (23.4%) | |
| Mutare rural | 221 (40.1%) | 54 (52.4%) | 120 (39.1%) | 47 (33.3%) | |
| Has health insurance | 26 (4.7%) | 13 (12.6%) | 6 (2.0%) | 7 (5.0%) | <0.001 |
| Transportation time to get to health facility | 0.002 | ||||
| 0–45 min | 363 (55.9%) | 77 (74.7%) | 189 (61.6%) | 97 (68.8%) | |
| 46–90 min | 115 (20.9%) | 18 (17.5%) | 73 (23.8%) | 24 (17.0%) | |
| ≥90 min | 73 (13.3%) | 8 (7.8%) | 45 (14.7%) | 20 (14.2%) | |
| Drivers of decision to get vaccinated | |||||
| Recommendation from Ministry of Health | 356 (64.6%) | 68 (66.0%) | 222 (72.3%) | 66 (46.8%) | 0.7 |
| Recommendation from doctor | 285 (51.7%) | 66 (64.1%) | 152 (49.5%) | 67 (47.5%) | 0.005 |
| Vaccine available free of charge | 210 (38.1%) | 41 (39.8%) | 142 (46.3%) | 27 (19.2%) | 0.7 |
| Ease of getting the vaccine | 195 (35.4%) | 42 (40.8%) | 126 (41.0%) | 27 (19.2%) | 0.2 |
| Recommendation from World Health Organization | 117 (21.2%) | 29 (28.2%) | 74 (24.1%) | 14 (9.9%) | 0.06 |
| Country where vaccine is produced | 102 (18.5%) | 24 (23.3%) | 39 (12.7%) | 39 (27.7%) | 0.2 |
| Univariate | Multivariate | |||||
|---|---|---|---|---|---|---|
| OR | 95% CI | p-Value | aOR | 95% CI | p-Value | |
| Household head age | ||||||
| 18–29 years | Ref | Ref | ||||
| 30–39 years | 1.14 | 0.64–2.06 | 0.7 | 1.49 | 0.69–3.19 | 0.3 |
| 40–54 years | 0.98 | 0.55–1.73 | 0.9 | 1.67 | 0.79–3.53 | 0.2 |
| ≥55 years | 0.50 | 0.28–0.88 | 0.02 | 1.35 | 0.58–3.13 | 0.5 |
| Household head is male | 2.08 | 1.27–3.33 | 0.003 | 2.63 | 1.41–4.76 | 0.002 |
| Household head attended secondary school or higher | 2.04 | 1.35–3.09 | 0.001 | 1.73 | 0.93–3.22 | 0.08 |
| Identification of COVID-19 prevention measures | ||||||
| Getting vaccinated | 2.62 | 1.74–3.94 | <0.001 | 1.75 | 1.02–2.98 | 0.04 |
| Handwashing | 3.46 | 1.82–6.58 | <0.001 | 3.51 | 1.42–8.67 | 0.007 |
| Wearing face masks | 2.57 | 1.45–4.55 | 0.001 | |||
| Social distancing | 1.78 | 1.09–2.91 | 0.02 | |||
| Reported practice of COVID-19 prevention measures | ||||||
| Wearing face masks | 1.92 | 1.20–3.07 | 0.006 | |||
| Handwashing | 2.29 | 1.31–4.00 | 0.004 | |||
| Social distancing | 0.93 | 0.61–1.41 | 0.7 | |||
| Concerned about community spread | 1.05 | 0.70–1.56 | 0.8 | |||
| Concerned about getting infected | 1.00 | 0.64–1.53 | 1.0 | |||
| Confident that vaccines are safe | 23.63 | 12.47–44.76 | <0.001 | 28.14 | 13.89–57.01 | <0.001 |
| Drivers of decision to get vaccinated | ||||||
| Recommendation from Ministry of Health | 2.97 | 1.96–4.49 | <0.001 | |||
| Recommendation from doctor | 1.08 | 0.73–1.61 | 0.7 | |||
| Vaccine available free of charge | 3.63 | 2.26–5.85 | <0.001 | 3.83 | 2.05–7.15 | <0.001 |
| Ease of getting the vaccine | 2.94 | 1.82–4.74 | <0.001 | |||
| Recommendation from World Health Organization | 2.88 | 1.56–5.31 | 0.001 | 3.12 | 1.41–6.92 | 0.005 |
| Country where vaccine is produced | 0.38 | 0.23–0.63 | <0.001 | 0.47 | 0.24–0.95 | 0.04 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
McAbee, L.; Tapera, O.; Kanyangarara, M. Factors Associated with COVID-19 Vaccine Intentions in Eastern Zimbabwe: A Cross-Sectional Study. Vaccines 2021, 9, 1109. https://doi.org/10.3390/vaccines9101109
McAbee L, Tapera O, Kanyangarara M. Factors Associated with COVID-19 Vaccine Intentions in Eastern Zimbabwe: A Cross-Sectional Study. Vaccines. 2021; 9(10):1109. https://doi.org/10.3390/vaccines9101109
Chicago/Turabian StyleMcAbee, Lauren, Oscar Tapera, and Mufaro Kanyangarara. 2021. "Factors Associated with COVID-19 Vaccine Intentions in Eastern Zimbabwe: A Cross-Sectional Study" Vaccines 9, no. 10: 1109. https://doi.org/10.3390/vaccines9101109
APA StyleMcAbee, L., Tapera, O., & Kanyangarara, M. (2021). Factors Associated with COVID-19 Vaccine Intentions in Eastern Zimbabwe: A Cross-Sectional Study. Vaccines, 9(10), 1109. https://doi.org/10.3390/vaccines9101109







