COVID-19 Vaccines and Autoimmune Hematologic Disorders
Abstract
1. Introduction
2. Methods
3. Commercially Available COVID-19 Vaccines
- There are currently many different ways of producing vaccines.
- Obstacles or disadvantages may be storage, stability, or low immunogenicity.
4. International Reports of Adverse Events Associated with COVID-19 Vaccines
- AEs are generally mild or moderate.
- Albeit very infrequently, there can be SAEs that need to be paid attention to.
4.1. Autoimmune Hematologic Disorders Subsequent to COVID-19 Vaccination
4.2. Risk of Secondary ITP
4.2.1. Historical Perspective
4.2.2. COVID-19, COVID-19 Vaccination and ITP
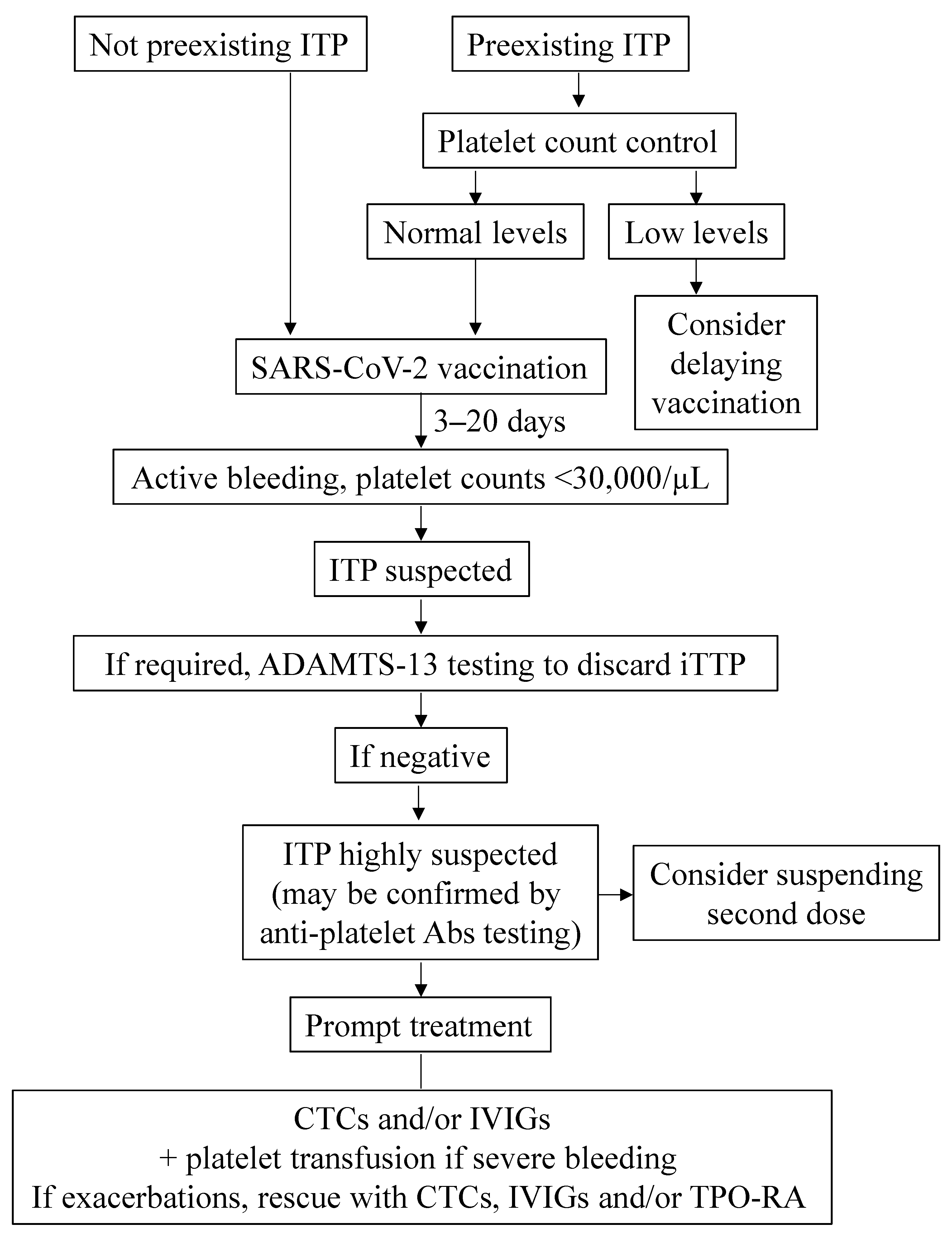
4.2.3. Management of ITP
- Cases of ITP associated with SARS-CoV-2 infection have been reported. Although infrequently, severe thrombocytopenia has been documented among these subjects.
- ITP onset subsequent to vaccination against SARS-CoV-2 has been documented. The overall incidence is extremely low. Exacerbations have been observed in a low proportion of previously diagnosed ITP patients.
- Treatment of secondary ITP or ITP exacerbations subsequent to vaccination is essentially similar to that used in patients with primary ITP. The outcome is usually favorable.
4.3. Risk of VITT
4.3.1. Newly Described Autoimmune Disorder
4.3.2. VITT and Heparin-Induced Thrombocytopenia
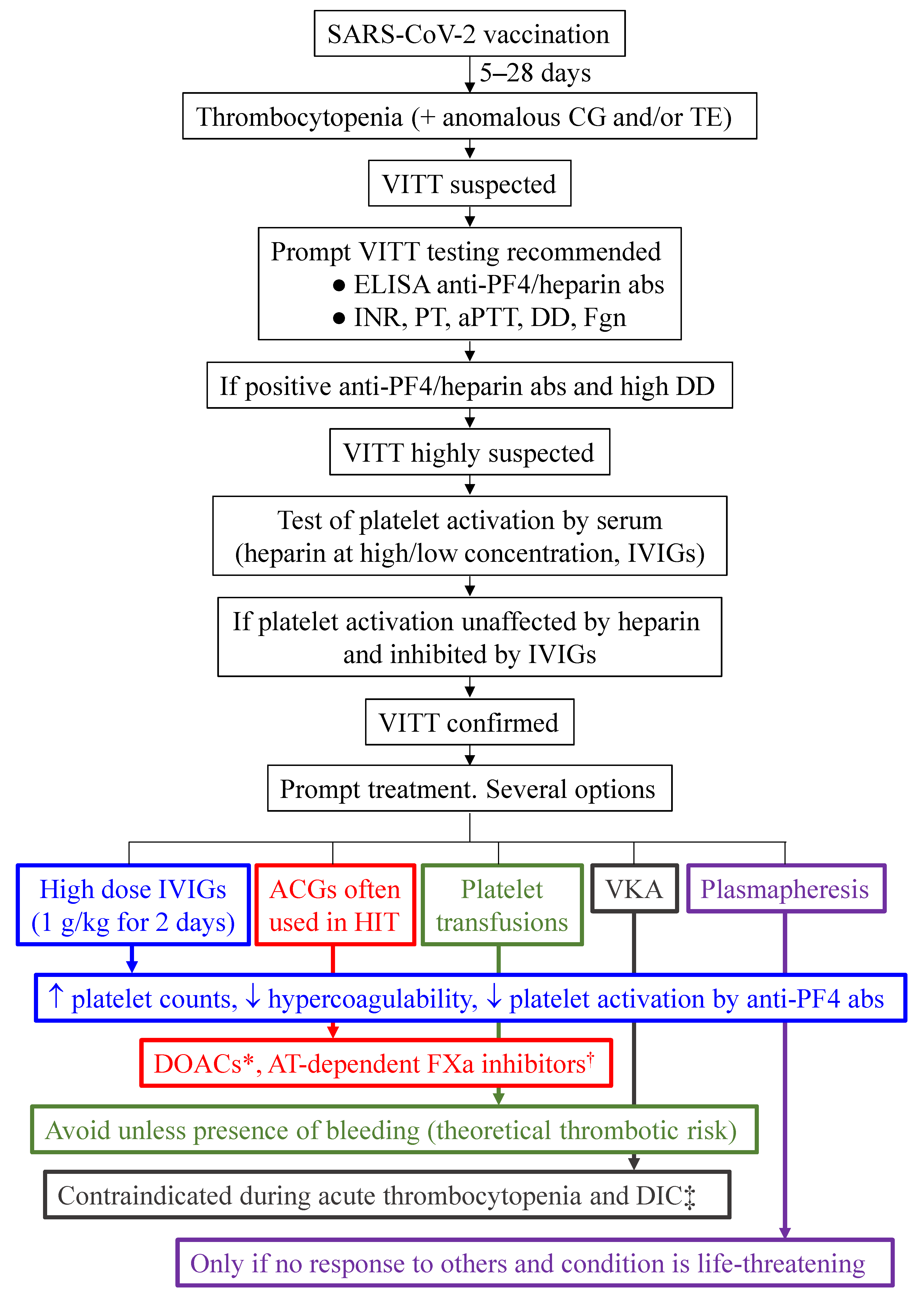
4.3.3. Management of VITT
- all samples for testing for VITT must be collected prior to administration of any treatment, especially IVIGs and danaparoid.
- assessment of anti-PF4 antibodies should be performed by enzyme-linked immunosorbent assay (ELISA), since rapid tests and chemiluminescence immunoassays can yield false negatives.
- the ability of a patient´s serum to activate platelets must be tested.
- the clinical picture of the individual must be taken into account:
- thrombocytopenia, bleeding, and normal coagulation parameters may indicate ITP. In this case, the bleeding risk has to be considered. High-dose IVIGs without anticoagulation is recommended, as well as testing for autoantibodies against platelet glycoproteins via monoclonal antibody immobilization of platelet antigens (MAIPA), monoclonal antigen capture ELISA (MACE), platelet antibody bead array (PABA), or flow cytometry. Platelet-associated IgGs are not often measured because of the low sensitivity of the usually available methods.
- thrombocytopenia and thrombosis may indicate VITT. An ELISA to detect anti-PF4 antibodies must be performed. If the PF4 binding assay is positive, or not available, the sample’s ability to activate platelets should be determined using serotonin release assay, platelet aggregation, P-selectin exposure, or others. A positive result in the appropriate clinical context strongly supports a diagnosis of VITT.
- thrombocytopenia without bleeding or thrombosis but abnormal coagulation parameters (at least one among PT, APTT, fibrinogen and DD) may indicate early VITT syndrome.
- VITT is a syndrome whose hallmark are anti-PF4 autoantibodies which may develop after COVID-19 vaccination, especially with adenoviral vectored vaccines, at an extremely rare frequency.
- VITT presents with thrombocytopenia and thrombosis at unusual locations, such as cerebral and splenic vascular beds.
- Early diagnosis and management according to ISTH guidelines is crucial to prevent fatalities.
4.4. Risk of iTTP
4.4.1. Historical Perspective
4.4.2. COVID-19, COVID-19 Vaccination and iTTP
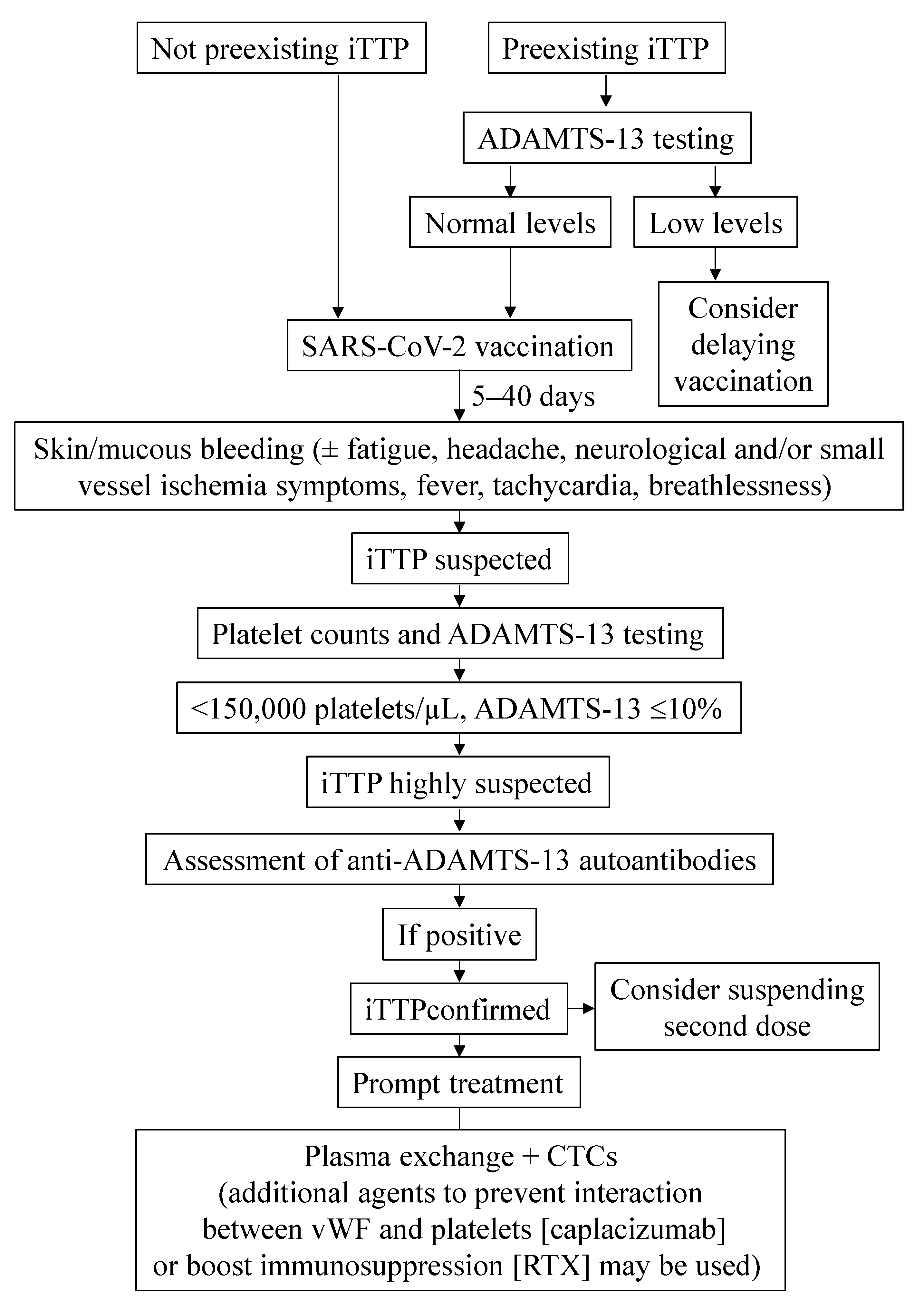
4.4.3. Management of iTTP
- Patients presenting with mucocutaneous bleeding signs and other clinical symptoms such as fatigue, headache and others, after COVID-19 vaccination, should be encouraged to seek immediate medical attention and undergo cell count analyses. Indeed, clinicians should be alert to the risk of developing iTTP.
- In patients who had already suffered an iTTP episode, the ADAMTS-13 circulating activity should be assessed before COVID-19 vaccination in order to address relapse risk.
- It may be advisable not to administer the second dose of the SARS-CoV-2 vaccine to those patients who had an iTTP episode after the first one, although evidence supporting this decision is scarce.
- Extremely infrequent cases of newly diagnosed iTTP subsequent to COVID-19 vaccination, especially with BNT162b2, have been reported. Relapses have also been documented.
- Platelet cell counts and ADAMTS-13 levels have to be assessed if vaccinated patients present with bleeding signs and fatigue and/or other clinical symptoms. A definitive diagnosis is achieved when anti-ADAMTS-13 autoantibodies are detected.
- Management does not differ greatly from that of iTTP in other scenarios, plasma exchange and corticosteroids being the gold-standard treatments. Outcomes are usually favorable.
4.5. Risk of AIHA and Evans Syndrome
4.5.1. Historical Perspective
4.5.2. COVID-19, COVID-19 Vaccination and AIHA or Evans Syndrome
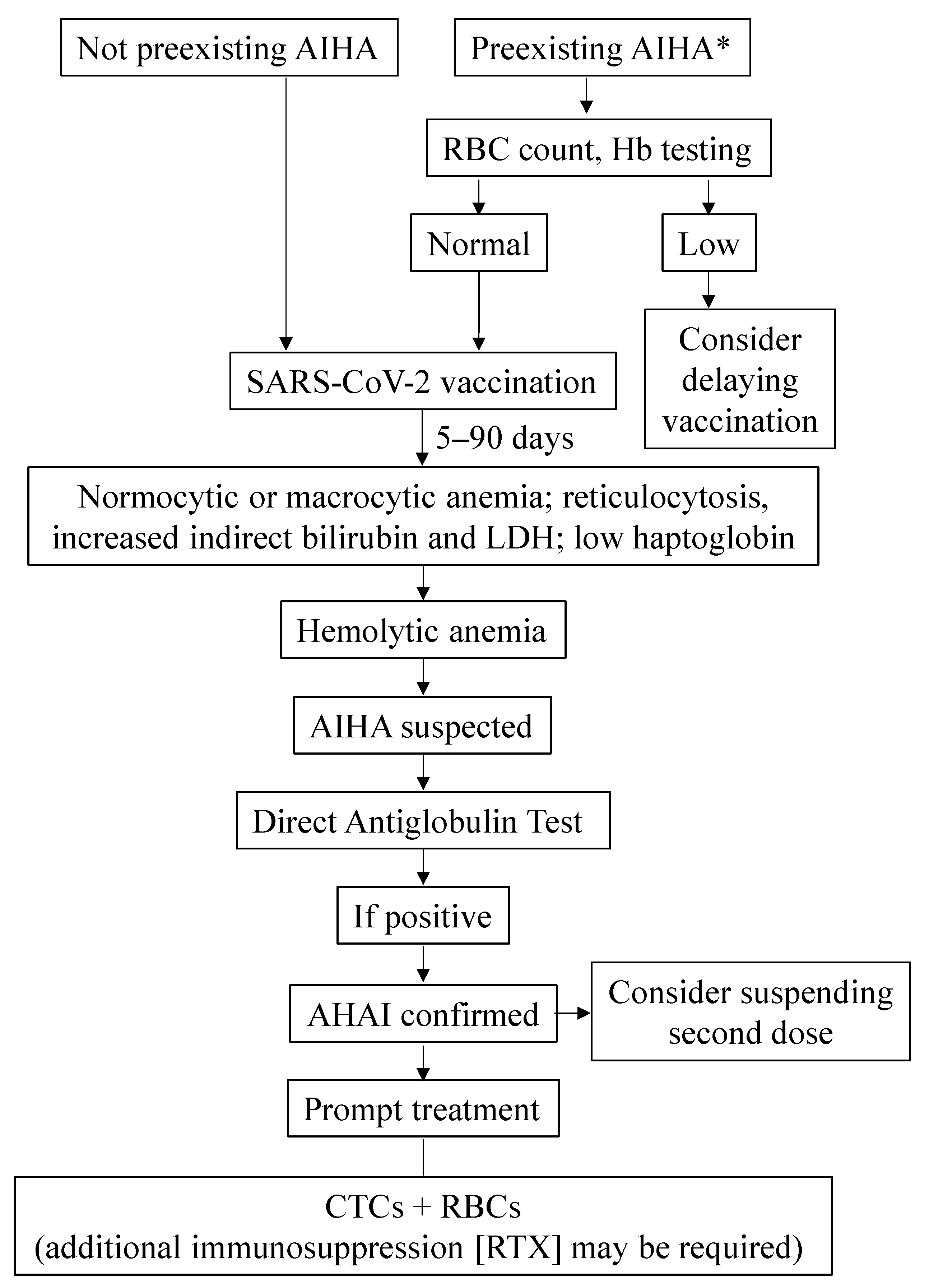
4.5.3. Management of AIHA and Evans Syndrome
- Cases of AIHA subsequent to COVID-19 infection and COVID-19 vaccination, although uncommon, may be severe and life-threatening.
- Corticosteroids and, when required, RBCs transfusion is a usually successful combination to treat patients with AIHA in the context of COVID-19 infection or vaccination. Additional boosts with agents such as rituximab may be occasionally needed.
- Evans syndrome is a rare entity, usually associated with other immune disorders or infection. Information regarding new-onset or exacerbations subsequent to COVID-19 infection or vaccination is scarce. Corticosteroids are considered as the first-line therapy.
4.5.4. Antiphospholipid Syndrome and COVID-19 Vaccines
- Adenoviral vector-based vaccines can bind platelets, activate complement and induce APLs.
- In patients suffering from APS, there has not been reported a worse evolution after COVID-19 vaccination.
- Phospholipid serologic assays seem to not be influenced by SARS-CoV-2 vaccines. Despite this, in case of results that do not fit the clinical picture following SARS-CoV-2, vaccination should be repeated.
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Fiolet, T.; Kherabi, Y.; MacDonald, C.J.; Ghosn, J.; Peiffer-Smadja, N. Comparing COVID-19 vaccines for their characteristics, efficacy and effectiveness against SARS-CoV-2 and variants of concern: A narrative review. Clin. Microbiol. Infect. 2022, 28, 202–221. [Google Scholar] [CrossRef] [PubMed]
- Ghasemiyeh, P.; Mohammadi-Samani, S.; Firouzabadi, N.; Dehshahri, A.; Vazin, A. A focused review on technologies, mechanisms, safety, and efficacy of available COVID-19 vaccines. Int. Immunopharmacol. 2021, 100, 108162. [Google Scholar] [CrossRef]
- Palatnik-De-Sousa, C.B. What Would Jenner and Pasteur Have Done About COVID-19 Coronavirus? The Urges of a Vaccinologist. Front. Immunol. 2020, 11, 2173. [Google Scholar] [CrossRef] [PubMed]
- Pushparajah, D.; Jimenez, S.; Wong, S.; Alattas, H.; Nafissi, N.; Slavcev, R.A. Advances in gene-based vaccine platforms to address the COVID-19 pandemic. Adv. Drug Deliv. Rev. 2021, 170, 113–141. [Google Scholar] [CrossRef] [PubMed]
- Wolff, J.A.; Malone, R.W.; Williams, P.; Chong, W.; Acsadi, G.; Jani, A.; Felgner, P.L. Direct gene transfer into mouse muscle in vivo. Science 1990, 247, 1465–1468. [Google Scholar] [CrossRef] [PubMed]
- Mendonça, S.A.; Lorincz, R.; Boucher, P.; Curiel, D.T. Adenoviral vector vaccine platforms in the SARS-CoV-2 pandemic. NPJ Vaccines 2021, 6, 97. [Google Scholar] [CrossRef]
- Azmi, F.; Fuaad, A.A.H.A.; Skwarczynski, M.; Toth, I. Recent progress in adjuvant discovery for peptide-based subunit vaccines. Hum. Vaccines Immunother. 2014, 10, 778–796. [Google Scholar] [CrossRef]
- European Medicines Agency. Guide on the Interpretation of Spontaneous Case Reports of Suspected Adverse Reactions to Medicines; European Medicines Agency: London, UK, 2017. [Google Scholar]
- Medicines & Healthcare Products Regulatory Agency. Coronavirus Vaccine Weekly Summary of Yellow Card Reporting. gov.uk. 2021. Available online: https://www.gov.uk/government/publications/coronavirus-covid-19-vaccine-adverse-reactions/coronavirus-vaccine-summary-of-yellow-card-reporting (accessed on 6 September 2021).
- Reported Side Effects Following COVID-19 Vaccination in Canada. Available online: https://health-infobase.canada.ca/covid-19/vaccine-safety/#a4 (accessed on 2 May 2022).
- The Vaccine Adverse Event Reporting System (VAERS). Available online: https://wonder.cdc.gov/controller/datarequest/D8;jsessionid=426D8ABB1739155E11D06093CA0D (accessed on 2 May 2022).
- Polack, F.P.; Thomas, S.J.; Kitchin, N.; Absalon, J.; Gurtman, A.; Lockhart, S.; Perez, J.L.; Marc, G.P.; Moreira, E.D.; Zerbini, C.; et al. Safety and efficacy of the BNT162b2 mRNA COVID-19 vaccine. N. Engl. J. Med. 2020, 383, 2603–2615. [Google Scholar] [CrossRef]
- Baden, L.R.; El Sahly, H.M.; Essink, B.; Kotloff, K.; Frey, S.; Novak, R.; Diemert, M.D.; Spector, S.A.; Rouphael, N.; Creech, B.; et al. Efficacy and Safety of the mRNA-1273SARS-CoV-2 Vaccine. N. Engl. J. Med. 2021, 384, 403–416. [Google Scholar] [CrossRef]
- Folegatti, P.M.; Ewer, K.J.; Aley, P.K.; Angus, B.; Becker, S.; Belij-Rammerstorfer, S.; Bellamy, D.; Bibi, S.; Bittaye, M.; Clutterbuck, E.A.; et al. Safety and immunogenicity of the ChAdOx1 nCoV-19 vaccine against SARS-CoV-2: A preliminary report of a phase 1/2, single-blind, randomised controlled trial. Lancet 2020, 396, 467–478. [Google Scholar] [CrossRef]
- Sadoff, J.; Gray, G.; Vandebosch, A.; Cárdenas, V.; Shukarev, G.; Grinsztejn, B.; Goepfert, P.A.; Truyers, C.; Fennema, H.; Spiessens, B.; et al. Safety and Efficacy of Single-Dose Ad26.COV2.S Vaccine against Covid-19. N. Engl. J. Med. 2021, 384, 2187–2201. [Google Scholar] [CrossRef] [PubMed]
- Logunov, D.Y.; Dolzhikova, I.V.; Shcheblyakov, D.V.; Tukhvatulin, A.I.; Zubkova, O.V.; Dzharullaeva, A.S.; Kovyrshina, A.V.; Lubenets, N.L.; Grousova, D.M.; Gam-COVID-Vac Vaccine Trial Group; et al. Safety and efficacy of an rAd26 and rAd5 vector-based heterologous prime-boost COVID-19 vaccine: An interim analysis of a randomised controlled phase 3 trial in Russia. Lancet 2021, 397, 671–681. [Google Scholar] [CrossRef]
- Al-Ali, D.; Elshafeey, A.; Mushannen, M.; Kawas, H.; Shafiq, A.; Mhaimeed, N.; Mhaimeed, O.; Mhaimeed, N.; Zeghlache, R.; Salameh, M.; et al. Cardiovascular and haematological events post COVID-19 vaccination: A systematic review. J. Cell. Mol. Med. 2021, 26, 636–653. [Google Scholar] [CrossRef]
- Chen, Y.; Xu, Z.; Wang, P.; Li, X.M.; Shuai, Z.W.; Ye, D.Q.; Pan, H.F. New-onset autoimmune phenomena post-COVID-19 vaccination. Immunology 2022, 165, 386–401. [Google Scholar] [CrossRef] [PubMed]
- O’Leary, S.T.; Glanz, J.M.; McClure, D.L.; Akhtar, A.; Daley, M.F.; Nakasato, C.; Baxter, R.; Davis, R.L.; Izurieta, H.S.; Lieu, T.A.; et al. The Risk of Immune Thrombocytopenic Purpura After Vaccination in Children and Adolescents. Pediatrics 2012, 129, 248–255. [Google Scholar] [CrossRef] [PubMed]
- Perricone, C.; Ceccarelli, F.; Nesher, G.; Borella, E.; Odeh, Q.; Conti, F.; Shoenfeld, Y.; Valesini, G. Immune thrombocytopenic purpura (ITP) associated with vaccinations: A review of reported cases. Immunol. Res. 2014, 60, 226–235. [Google Scholar] [CrossRef]
- Schmidt, N.; Maitland, H. Acute Immune Thrombocytopenia following administration of Shingrix recombinant zoster vaccine. Am. J. Hematol. 2021, 96, E136–E137. [Google Scholar] [CrossRef]
- Johansen, S.; Lægreid, I.J.; Ernstsen, S.L.; Azrakhsh, N.A.; Kittang, A.O.; Lindås, R.; Gjertsen, B.T.; Vetti, N.; Mørtberg, T.V.; Sørvoll, I.H.; et al. Thrombosis and thrombocytopenia after HPV vaccination. J. Thromb. Haemost. 2021, 20, 700–704. [Google Scholar] [CrossRef] [PubMed]
- Di Pietrantonj, C.; Rivetti, A.; Marchione, P.; Debalini, M.G.; Demicheli, V. Vaccines for measles, mumps, rubella, and varicella in children. Cochrane Database Syst. Rev. 2020, 4, CD004407. [Google Scholar] [PubMed]
- Andrews, N.; Stowe, J.; Miller, E.; Svanström, H.; Johansen, K.; Bonhoeffer, J.; Hviid, A.; VAESCO consortium. A collaborative approach to investigating the risk of thrombocytopenic purpura aMer measles–mumps–rubella vaccination in England and Denmark. Vaccine 2012, 30, 3042–3046. [Google Scholar] [CrossRef]
- Perez-Vilar, S.; Weibel, D.; Sturkenboom, M.; Black, S.; Maure, C.; Castro, J.L.; Bravo-Alcántara, P.; Dodd, C.N.; Romio, S.A.; de Ridder, M.; et al. Enhancing global vaccine pharmacovigilance: Proof-of-concept study on aseptic meningitis and immune thrombocytopenic purpura following measles-mumps containing vaccination. Vaccine 2017, 36, 347–354. [Google Scholar] [CrossRef] [PubMed]
- Catani, L.; Fagioli, M.E.; Tazzari, P.L.; Ricci, F.; Curti, A.; Rovito, M.; Preda, P.; Chirumbolo, G.; Amabile, M.; Lemoli, R.M.; et al. Dendritic cells of immune thrombocytopenic purpura (ITP) show increased capacity to present apoptotic platelets to T lymphocytes. Exp. Hematol. 2006, 34, 879–887. [Google Scholar] [CrossRef] [PubMed]
- Gu, D.; Chen, Z.; Zhao, H.; Du, W.; Xue, F.; Ge, J.; Sui, T.; Wu, H.; Liu, B.; Lu, S.; et al. Th1 (CXCL10) and Th2 (CCL2) chemokine expression in patients with immune thrombocytopenia. Hum. Immunol. 2010, 71, 586–591. [Google Scholar] [CrossRef]
- Sakakura, M.; Wada, H.; Tawara, I.; Nobori, T.; Sugiyama, T.; Sagawa, N.; Shiku, H. Reduced Cd4+Cd25+ T cells in patients with idiopathic thrombocytopenic purpura. Thromb. Res. 2007, 120, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Yu, J.; Heck, S.; Patel, V.; LeVan, J.; Yu, Y.; Bussel, J.B.; Yazdanbakhsh, K. Defective circulating CD25 regulatory T cells in patients with chronic immune thrombocytopenic purpura. Blood 2008, 112, 1325–1328. [Google Scholar] [CrossRef]
- Zhang, J.; Ma, D.; Zhu, X.; Qu, X.; Ji, C.; Hou, M. Elevated profile of Th17, Th1 and Tc1 cells in patients with immune thrombocytopenic purpura. Haematologica 2009, 94, 1326–1329. [Google Scholar] [CrossRef]
- Black, C.; Kaye, J.A.; Jick, H. MMR vaccine and idiopathic thrombocytopaenic purpura. Br. J. Clin. Pharmacol. 2003, 55, 107–111. [Google Scholar] [CrossRef]
- Stowe, J.; Kafatos, G.; Andrews, N.; Miller, E. Idiopathic thrombocytopenic purpura and the second dose of MMR: Figure 1. Arch. Dis. Child. 2007, 93, 182–183. [Google Scholar] [CrossRef]
- Kuter, J.D. Exacerbation of immune thrombocytopenia following COVID-19 vaccination. Br. J. Haematol. 2021, 195, 365–370. [Google Scholar] [CrossRef] [PubMed]
- Dotan, A.; Muller, S.; Kanduc, D.; David, P.; Halpert, G.; Shoenfeld, Y. The SARS-CoV-2 as an instrumental trigger of autoimmunity. Autoimmun. Rev. 2021, 20, 102792. [Google Scholar] [CrossRef] [PubMed]
- Zulfiqar, A.-A.; Lorenzo-Villalba, N.; Hassler, P.; Andrès, E. Immune thrombocytopenic purpura in a patient with COVID-19. N. Engl. J. Med. 2020, 382, e43. [Google Scholar] [CrossRef] [PubMed]
- Levraut, M.; Ottavi, M.; Lechtman, S.; Mondain, V.; Jeandel, P. Immune thrombocytopenic purpura after COVID-19 infection. Int. J. Lab. Hematol. 2020, 43, e28–e30. [Google Scholar] [CrossRef]
- Murt, A.; Eskazan, A.E.; Yilmaz, U.; Ozkan, T.; Ar, M.C. COVID-19 presenting with immune thrombocytopenia: A case report and review of the literature. J. Med. Virol. 2020, 93, 43–45. [Google Scholar] [CrossRef]
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Qu, C.Q.; He, J.X.; Liu, L.; Shan, H.; Lei, C.L.; Hui, D.S.C.; et al. China medical treatment expert group for COVID-19 2020. Clinical Characteristics of coronavirus disease in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar] [CrossRef] [PubMed]
- Thomas, S.J.; Moreira, E.D., Jr.; Kitchin, N.; Absalon, J.; Gurtman, A.; Lockhart, S.; Perez, J.L.; Pérez Marc, G.; Polack, F.P.; Zerbini, C.; et al. Safety and Efficacy of the BNT162b2 mRNA COVID-19 Vaccine through 6 Months. N. Engl. J. Med. 2021, 385, 1761–1773. [Google Scholar] [CrossRef] [PubMed]
- Lee, E.J.; Cines, D.B.; Gernsheimer, T.; Kessler, C.; Michel, M.; Tarantino, M.D.; Semple, J.W.; Arnold, D.M.; Godeau, B.; Lambert, M.P.; et al. Thrombocytopenia following Pfizer and Moderna SARS-CoV-2 vaccination. Am. J. Hematol. 2021, 96, 534–537. [Google Scholar] [CrossRef] [PubMed]
- David, P.; Dotan, A.; Mahroum, N.; Shoenfeld, Y. Immune Thrombocytopenic Purpura (ITP) Triggered by COVID-19 Infection and Vaccination. Isr. Med. Assoc. J. 2021, 23, 378–380. [Google Scholar]
- Lee, E.J.; Beltrami-Moreira, M.; Al-Samkari, H.; Cuker, A.; DiRaimo, J.; Gernsheimer, T.; Kruse, A.; Kessler, C.; Kruse, C.; Leavitt, A.D.; et al. SARS-CoV-2 vaccination and ITP in patients with de novo or preexisting ITP. Blood 2022, 139, 1564–1574. [Google Scholar] [CrossRef]
- Edwards, D.K.; Jasny, E.; Yoon, H.; Horscroft, N.; Schanen, B.; Geter, T.; Fotin-Mleczek, M.; Petsch, B.; Wittman, V. Adjuvant effects of a sequence-engineered mRNA vaccine: Translational profiling demonstrates similar human and murine innate response. J. Transl. Med. 2017, 15, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Thi, T.; Suys, E.; Lee, J.; Nguyen, D.; Park, K.; Truong, N. Lipid-Based Nanoparticles in the Clinic and Clinical Trials: From Cancer Nanomedicine to COVID-19 Vaccines. Vaccines 2021, 9, 359. [Google Scholar] [CrossRef]
- Agmon-Levin, N.; Paz, Z.; Israeli, E.; Shoenfeld, Y. Vaccines and autoimmunity. Nat. Rev. Rheumatol. 2009, 5, 648–652. [Google Scholar] [CrossRef] [PubMed]
- Israeli, E.; Agmon-Levin, N.; Blank, M.; Shoenfeld, Y. Adjuvants and autoimmunity. Lupus 2009, 18, 1217–1225. [Google Scholar] [CrossRef] [PubMed]
- Shoenfeld, Y.; Agmon-Levin, N. ‘ASIA’-autoimmune/inflammatory syndrome induced by adjuvants. J. Autoimmun. 2011, 36, 4–8. [Google Scholar] [CrossRef] [PubMed]
- Welsh, K.J.; Baumblatt, J.; Chege, W.; Goud, R.; Nair, N. Thrombocytopenia including immune thrombocytopenia after receipt of mRNA COVID-19 vaccines reported to the Vaccine Adverse Event Reporting System (VAERS). Vaccine 2021, 39, 3329–3332. [Google Scholar] [CrossRef] [PubMed]
- Visser, C.; Swinkels, M.; van Werkhoven, E.D.; Croles, F.N.N.; Noordzij-Nooteboom, H.S.; Eefting, M.; Last-Koopmans, S.M.; Idink, C.; Westerweel, P.E.; Santbergen, B.; et al. COVID-19 vaccination in patients with immune thrombocytopenia. Blood Adv. 2022, 6, 1637–1644. [Google Scholar] [CrossRef]
- Bussel, J.; Cines, D.; Cooper, N.; Dunbar, C.; Michel, M.; Rodeghiero, F. COVID-19 and ITP: Frequently Asked Questions. In COVID-19 Resources of the American Society of Hematology. Available online: https://www.hematology.org/covid-19/covid-19-and-itp (accessed on 5 May 2022).
- Greinacher, A.; Thiele, T.; Warkentin, T.E.; Weisser, K.; Kyrle, P.A.; Eichinger, S. Thrombotic Thrombocytopenia after ChAdOx1 nCov-19 Vaccination. N. Engl. J. Med. 2021, 384, 2092–2101. [Google Scholar] [CrossRef]
- See, I.; Su, J.R.; Lale, A.; Woo, E.J.; Guh, A.Y.; Shimabukuro, T.T.; Streiff, M.B.; Rao, A.K.; Wheeler, A.P.; Beavers, S.F.; et al. US Case Reports of Cerebral Venous Sinus Thrombosis With Thrombocytopenia After Ad26.COV2.S Vaccination, March 2 to April 21, 2021. JAMA 2021, 325, 2448–2456. [Google Scholar] [CrossRef]
- Cines, D.B.; Bussel, J.B. SARS-CoV-2 Vaccine-Induced Immune Thrombotic Thrombocytopenia. N. Engl. J. Med. 2021, 384, 2254–2256. [Google Scholar] [CrossRef]
- Smadja, D.M.; Yue, Q.-Y.; Chocron, R.; Sanchez, O.; Louet, A.L.-L. Vaccination against COVID-19: Insight from arterial and venous thrombosis occurrence using data from VigiBase. Eur. Respir. J. 2021, 58, 2100956. [Google Scholar] [CrossRef]
- Afshar, Z.M.; Babazadeh, A.; Janbakhsh, A.; Afsharian, M.; Saleki, K.; Barary, M.; Ebrahimpour, S. Vaccine-induced immune thrombotic thrombocytopenia after vaccination against COVID-19: A clinical dilemma for clinicians and patients. Rev. Med. Virol. 2022, 32, e2273. [Google Scholar]
- Warkentin, T.E.; Cuker, A. COVID-19: Vaccine-Induced Immune Thrombotic Thrombocytopenia (VITT), UpToDate. 2022. Available online: https://www.uptodate.com/contents/covid-19-vaccine-induced-immune-thrombotic-thrombocytopenia-vitt (accessed on 8 May 2022).
- Greinacher, A.; Selleng, K.; Mayerle, J.; Palankar, R.; Wesche, J.; Reiche, S.; Aebischer, A.; Warkentin, T.E.; Muenchhoff, M.; Immune-Response in COVID-19 Vaccination Study Group; et al. Anti-platelet factor 4 antibodies causing VITT do not cross-react with SARS-CoV-2 spike protein. Blood 2021, 138, 1269–1277. [Google Scholar] [CrossRef]
- Schultz, N.H.; Sørvoll, I.H.; Michelsen, A.E.; Munthe, L.A.; Lund-Johansen, F.; Ahlen, M.T.; Wiedmann, M.; Aamodt, A.-H.; Skattør, T.H.; Tjønnfjord, G.E.; et al. Thrombosis and Thrombocytopenia after ChAdOx1 nCoV-19 Vaccination. N. Engl. J. Med. 2021, 384, 2124–2130. [Google Scholar] [CrossRef] [PubMed]
- Greinacher, A.; Selleng, K.; Warkentin, T.E. Autoimmune heparin-induced thrombocytopenia. J. Thromb. Haemost. 2017, 15, 2099–2114. [Google Scholar] [CrossRef] [PubMed]
- Rizk, J.G.; Gupta, A.; Sardar, P.; Henry, B.M.; Lewin, J.C.; Lippi, G.; Lavie, C.J. Clinical Characteristics and Pharmacological Management of COVID-19 Vaccine-Induced Immune Thrombotic Thrombocytopenia With Cerebral Venous Sinus Thrombosis: A Review. JAMA Cardiol. 2021, 6, 1451–1460. [Google Scholar] [CrossRef] [PubMed]
- Jaax, M.E.; Krauel, K.; Marschall, T.; Brandt, S.; Gansler, J.; Fürll, B.; Appel, B.; Fischer, S.; Block, S.; Helm, C.A.; et al. Complex formation with nucleic acids and aptamers alters the antigenic properties of platelet factor 4. Blood 2013, 122, 272–281. [Google Scholar] [CrossRef] [PubMed]
- Klok, F.A.; Pai, M.; Huisman, M.V.; Makris, M. Vaccine-induced immune thrombotic thrombocytopenia. Lancet Haematol. 2022, 9, e73–e80. [Google Scholar] [CrossRef]
- Nazy, I.; Sachs, U.J.; Arnold, D.M.; McKenzie, S.E.; Choi, P.; Althaus, K.; Ahlen, M.T.; Sharma, R.; Grace, R.F.; Bakchoul, T. Recommendations for the clinical and laboratory diagnosis of VITT against COVID-19: Communication from the ISTH SSC Subcommittee on Platelet Immunology. J. Thromb. Haemost. 2021, 19, 1585–1588. [Google Scholar] [CrossRef]
- Van de Munckhof, A.; Krzywicka, K.; de Sousa, D.A.; van Kammen, M.S.; Heldner, M.R.; Jood, K.; Lindgren, K.; Tatlisumak, T.; Putaala, J.; Hovinga, J.A.K.; et al. Declining mortality of cerebral venous sinus thrombosis with thrombocytopenia after SARS-CoV-2 vaccination. Eur. J. Neurol. 2022, 29, 339–344. [Google Scholar] [CrossRef]
- Sadler, J.E. What’s new in the diagnosis and pathophysiology of thrombotic thrombocytopenic purpura. Hematol. Am. Soc. Hematol. Educ. Program 2015, 2015, 631–636. [Google Scholar] [CrossRef]
- Yavaşoğlu, I. Vaccination and Thrombotic Thrombocytopenic Purpura. Turk. J. Hematol. 2020, 37, 218–219. [Google Scholar] [CrossRef]
- Kadikoylu, G.; Yavasoglu, I.; Bolaman, Z. Rabies vaccine-associated thrombotic thrombocytopenic purpura. Transfus. Med. 2014, 24, 428–429. [Google Scholar] [CrossRef] [PubMed]
- Kojima, Y.; Ohashi, H.; Nakamura, T.; Nakamura, H.; Yamamoto, H.; Miyata, Y.; Iida, H.; Nagai, H. Acute thrombotic thrombocytopenic purpura after pneumococcal vaccination. Blood Coagul. Fibrinolysis 2014, 25, 512–514. [Google Scholar] [CrossRef] [PubMed]
- Ramakrishnan, N.; Parker, L.P. Thrombotic thrombocytopenic purpura following influenza vaccination—A brief case report. Connect. Med. 1998, 62, 587–588. [Google Scholar]
- Dias, P.J.; Gopal, S. Refractory thrombotic thrombocytopenic purpura following influenza vaccination. Anaesthesia 2009, 64, 444–446. [Google Scholar] [CrossRef] [PubMed]
- Hermann, R.; Pfeil, A.; Busch, M.; Kettner, C.; Kretzschmar, D.; Hansch, A.; La Rosée, P.; Wolf, G. Very severe thrombotic thrombocytopenic purpura (TTP) after H1N1 vaccination. Med. Klin. 2010, 105, 663–668. [Google Scholar] [CrossRef]
- Brown, R.C.; Blecher, T.E.; French, E.A.; Toghill, P.J. Thrombotic thrombocytopenic purpura after influenza vaccination. BMJ 1973, 2, 303. [Google Scholar] [CrossRef]
- Tehrani, H.A.; Darnahal, M.; Vaezi, M.; Haghighi, S. COVID-19 associated thrombotic thrombocytopenic purpura (TTP); A case series and mini-review. Int. Immunopharmacol. 2021, 93, 107397. [Google Scholar] [CrossRef]
- Hindilerden, F.; Yonal-Hindilerden, I.; Akar, E.; Kart-Yasar, K. Covid-19 associated autoimmune thrombotic thrombocytopenic purpura: Report of a case. Thromb. Res. 2020, 195, 136–138. [Google Scholar] [CrossRef]
- Capecchi, M.; Mocellin, C.; Abbruzzese, C.; Mancini, I.; Prati, D.; Peyvandi, F. Dramatic presentation of acquired thombotic thrombocytopenic purpura associated with COVID-19. Haematologica 2020, 105, e540. [Google Scholar] [CrossRef]
- Albiol, N.; Awol, R.; Martino, R. Autoimmune thrombotic thrombocytopenic purpura (TTP) associated with COVID-19. Ann. Hematol. 2020, 99, 1673–1674. [Google Scholar] [CrossRef]
- Giuffrida, G.; Condorelli, A.; Di Giorgio, M.A.; Markovic, U.; Sciortino, R.; Nicolosi, D.; Di Raimondo, F. Immune-mediated thrombotic thrombocytopenic purpura following administration of Pfizer-BioNTech COVID-19 vaccine. Haematologica 2022, 107, 1008–1010. [Google Scholar] [PubMed]
- De Bruijn, S.; Maes, M.B.; De Waele, L.; Vanhoorelbeke, K.; Gadisseur, A. First report of a de novo iTTP episode associated with an mRNA-based anti-COVID-19 vaccination. J. Thromb. Haemost. 2021, 19, 2014–2018. [Google Scholar] [CrossRef] [PubMed]
- Maayan, H.; Kirgner, I.; Gutwein, O.; Herzog-Tzarfati, K.; Rahimi-Levene, N.; Koren-Michowitz, M.; Blickstein, D. Acquired thrombotic thrombocytopenic purpura: A rare disease associated with BNT162b2 vaccine. J. Thromb. Haemost. 2021, 19, 2314–2317. [Google Scholar] [CrossRef] [PubMed]
- Ruhe, J.; Schnetzke, U.; Kentouche, K.; Prims, F.; Baier, M.; Herfurth, K.; Schlosser, M.; Busch, M.; Hochhaus, A.; Wolf, G. Acquired thrombotic thrombocytopenic purpura after first vaccination dose of BNT162b2 mRNA COVID-19 vaccine. Ann. Hematol. 2021, 101, 717–719. [Google Scholar] [CrossRef]
- Yoshida, K.; Sakaki, A.; Matsuyama, Y.; Mushino, T.; Matsumoto, M.; Sonoki, T.; Tamura, S. Acquired Thrombotic Thrombocytopenic Purpura Following BNT162b2 mRNA Coronavirus Disease Vaccination in a Japanese Patient. Intern. Med. 2022, 61, 407–412. [Google Scholar] [CrossRef]
- Alislambouli, M.; Victoria, A.V.; Matta, J.; Yin, F. Acquired thrombotic thrombocytopenic purpura following Pfizer COVID-19 vaccination. eJHaem 2021, 3, 207–210. [Google Scholar] [CrossRef]
- Yocum, A.; Simon, E.L. Thrombotic Thrombocytopenic Purpura after Ad26.COV2-S Vaccination. Am. J. Emerg. Med. 2021, 49, 441.e3–441.e4. [Google Scholar] [CrossRef]
- Waqar, S.H.B.; Khan, A.A.; Memon, S. Thrombotic thrombocytopenic purpura: A new menace after COVID bnt162b2 vaccine. Int. J. Hematol. 2021, 114, 626–629. [Google Scholar] [CrossRef]
- Al-Ahmad, M.; Al-Rasheed, M.; Shalaby, N.A.B. Acquired thrombotic thrombocytopenic purpura with possible association with AstraZeneca-Oxford COVID-19 vaccine. EJHaem 2021, 2, 534–536. [Google Scholar] [CrossRef]
- Lee, H.P.; Selvaratnam, V.; Rajasuriar, J.S. Thrombotic thrombocytopenic purpura after ChAdOx1 nCoV-19 vaccine. BMJ Case Rep. 2021, 14, e246049. [Google Scholar] [CrossRef]
- Kirpalani, A.; Garabon, J.; Amos, K.; Patel, S.; Sharma, A.P.; Ganesan, S.L.; Barton, M.; Cacciotti, C.; Leppington, S.; Bakovic, L.; et al. Thrombotic thrombocytopenic purpura temporally associated with BNT162b2 vaccination in an adolescent successfully treated with caplacizumab. Br. J. Haematol. 2021, 196, e11–e14. [Google Scholar] [CrossRef] [PubMed]
- Sissa, C.; Al-Khaffaf, A.; Frattini, F.; Gaiardoni, R.; Mimiola, E.; Montorsi, P.; Melara, B.; Amato, M.; Peyvandi, F.; Franchini, M. Relapse of thrombotic thrombocytopenic purpura after COVID-19 vaccine. Transfus. Apher. Sci. 2021, 60, 103145. [Google Scholar] [CrossRef] [PubMed]
- Deucher, W.; Sukumar, S.; Cataland, S.R. Clinical relapse of immune-mediated thrombotic thrombocytopenic purpura following COVID-19 vaccination. Res. Pr. Thromb. Haemost. 2022, 6, e12658. [Google Scholar] [CrossRef] [PubMed]
- Saluja, P.; Gautam, N.; Yadala, S.; Venkata, A.N. Thrombotic thrombocytopenic purpura (TTP) after COVID-19 vaccination: A systematic review of reported cases. Thromb. Res. 2022, 214, 115–121. [Google Scholar] [CrossRef] [PubMed]
- Barcellini, W.; Fattizzo, B. The Changing Landscape of Autoimmune Hemolytic Anemia. Front. Immunol. 2020, 11, 946. [Google Scholar] [CrossRef] [PubMed]
- Audia, S.; Grienay, N.; Mounier, M.; Michel, M.; Bonnotte, B. Evans’ Syndrome: From Diagnosis to Treatment. J. Clin. Med. 2020, 9, 3851. [Google Scholar] [CrossRef]
- Seltsam, A.; Shukry-Schulz, S.; Salama, A. Vaccination-associated immune hemolytic anemia in two children. Transfusion 2000, 40, 907–909. [Google Scholar] [CrossRef]
- Downes, K.A.; Domen, R.E.; McCarron, K.F.; Bringelsen, K.A. Acute Autoimmune Hemolytic Anemia Following DTP Vaccination: Report of a Fatal Case and Review of the Literature. Clin. Pediatr. 2001, 40, 355–358. [Google Scholar] [CrossRef]
- Johnson, S.T.; McFarland, J.G.; Kelly, K.J.; Casper, J.T.; Gottschall, J.L. Transfusion support with RBCs from an Mk homozygote in a case of autoimmune hemolytic anemia following diphtheria-pertussis-tetanus vaccination. Transfusion 2002, 42, 567–571. [Google Scholar] [CrossRef]
- Montagnani, S.; Tuccori, M.; Lombardo, G.; Testi, A.; Mantarro, S.; Ruggiero, E.; Blandizzi, C. Autoimmune Hemolytic Anemia Following MF59-Adjuvanted Influenza Vaccine Administration: A Report of Two Cases. Ann. Pharmacother. 2010, 45, 128. [Google Scholar] [CrossRef]
- Gani, I.; Hinnant, G.; Kapoor, R.; Savage, N. Autoimmune Hemolytic Anemia in a Renal Transplant Patient Following Seasonal Influenza Vaccination. Case Rep. Hematol. 2019, 2019, 1–4. [Google Scholar] [CrossRef] [PubMed]
- Bowen, L.; LePage, N.; Lewandowska, M.; Waxman, D.A. Anti-Pr antibody induced cold autoimmune hemolytic anemia following pneumococcal vaccination. Clin. Case Rep. 2019, 7, 1763–1765. [Google Scholar] [CrossRef] [PubMed]
- Shlamovitz, G.Z.; Johar, S. A Case of Evans’ Syndrome Following Influenza Vaccine. J. Emerg. Med. 2013, 44, e149–e151. [Google Scholar] [CrossRef]
- Hsieh, Y.-L.; Lin, L.-H. Thrombocytopenic Purpura Following Vaccination in Early Childhood: Experience of a Medical Center in the Past 2 Decades. J. Chin. Med Assoc. 2010, 73, 634–637. [Google Scholar] [CrossRef]
- Lazarian, G.; Quinquenel, A.; Bellal, M.; Siavellis, J.; Jacquy, C.; Re, D.; Merabet, F.; Mekinian, A.; Braun, T.; Damaj, G.; et al. Autoimmune haemolytic anaemia associated with COVID-19 infection. Br. J. Haematol. 2020, 190, 29–31. [Google Scholar] [CrossRef] [PubMed]
- Finkenthal, T.A.; Aldaher, Z.; Ahmed, S.; DiValentin, L. Autoimmune Hemolytic Anemia Exacerbation Associated With COVID-19 Infection and Markedly Elevated Inflammatory Markers. Cureus 2021, 13, e20416. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, J.W.; Booth, G.S. COVID-19 and Immune-Mediated RBC Destruction. Am. J. Clin. Pathol. 2021, 157, 844–851. [Google Scholar] [CrossRef] [PubMed]
- Taherifard, E.; Taherifard, E.; Movahed, H.; Mousavi, M.R. Hematologic autoimmune disorders in the course of COVID-19: A systematic review of reported cases. Hematology 2021, 26, 225–239. [Google Scholar] [CrossRef]
- Turgutkaya, A.; Bolaman, A.Z.; Yavaşoğlu, İ. COVID-19-associated Evans syndrome: A case report and review of the literature. Transfus. Apher. Sci. 2021, 61, 103339. [Google Scholar] [CrossRef]
- Jaydev, F.; Kumar, V.; Khatri, J.; Shahani, S.; Beganovic, S. A Case of Autoimmune Hemolytic Anemia after the First Dose of COVID-19 mRNA-1273 Vaccine with Undetected Pernicious Anemia. Case Rep. Hematol. 2022, 2022, 2036460. [Google Scholar] [CrossRef]
- Fatima, Z.; Reece, B.R.A.; Moore, J.S.; Means, R.T., Jr. Autoimmune Hemolytic Anemia After mRNA COVID Vaccine. J. Investig. Med. High Impact Case Rep. 2022, 10, 23247096211073258. [Google Scholar] [CrossRef] [PubMed]
- De Bruyne, S.; Van Landeghem, S.; Schauwvlieghe, A.; Noens, L. Life-threatening autoimmune hemolytic anemia following mRNA COVID-19 vaccination: Don’t be too prudent with the red gold. Clin. Chem. Lab. Med. 2022, 60, 118. [Google Scholar] [CrossRef] [PubMed]
- Angileri, F.; Légaré, S.; Gammazza, A.M.; de Macario, E.C.; Macario, A.J.L.; Cappello, F. Is molecular mimicry the culprit in the autoimmune haemolytic anaemia affecting patients with COVID-19? Br. J. Haematol. 2020, 190, e92–e93. [Google Scholar] [CrossRef]
- Hidaka, D.; Ogasawara, R.; Sugimura, S.; Fujii, F.; Kojima, K.; Nagai, J.; Ebata, K.; Okada, K.; Kobayashi, N.; Ogasawara, M.; et al. New-onset Evans syndrome associated with systemic lupus erythematosus after BNT162b2 mRNA COVID-19 vaccination. Int. J. Hematol. 2021, 115, 424–427. [Google Scholar] [CrossRef] [PubMed]
- Fattizzo, B.; Giannotta, J.A.; Cecchi, N.; Barcellini, W. SARS-CoV-2 vaccination in patients with autoimmune cytopenias: The experience of a reference center. Am. J. Hematol. 2021, 96, E413–E416. [Google Scholar] [CrossRef]
- Yu, J.; Yuan, X.; Chen, H.; Chaturvedi, S.; Braunstein, E.M.; Brodsky, R.A. Direct activation of the alternative complement pathway by SARS-CoV-2 spike proteins is blocked by factor D inhibition. Blood 2020, 136, 2080–2089. [Google Scholar] [CrossRef] [PubMed]
- Talotta, R.; Robertson, E.S. Antiphospholipid antibodies and risk of post-COVID-19 vaccination thrombophilia: The straw that breaks the camel’s back? Cytokine Growth Factor Rev. 2021, 60, 52–60. [Google Scholar] [CrossRef]
- Moreno-Torres, V.; Gutiérrez, Á.; Valdenebro, M.; Ortega, A.; Cítores, M.J.; Montero, E. Catastrophic antiphospholipid syndrome triggered by mRNA COVID-19 vaccine. Clin. Exp. Rheumatol. 2022, 40, 1054–1055. [Google Scholar] [CrossRef]
- Molina Rios, S.; Rojas Martinez, R.; Estévez Ramirez, G.M.; Medina, Y.F. Systemic Lupus Erythematosus and Antiphospholipid Syndrome After COVID-19 Vaccination. A Case Report. Mod. Rheumatol. Case Rep. 2022, 4, rxac018. [Google Scholar] [CrossRef] [PubMed]
- Jinno, S.; Naka, I.; Nakazawa, T. Catastrophic antiphospholipid syndrome complicated with essential thrombocythaemia after COVID-19 vaccination: In search of the underlying mechanism. Rheumatol. Adv. Pract. 2021, 5, rkab096. [Google Scholar] [CrossRef] [PubMed]
- Pengo, V.; Del Ross, T.; Tonello, M.; Andreoli, L.; Tincani, A.; Gresele, P.; Silvestri, E.; Simioni, P.; Campello, E.; Hoxha, A.; et al. Impact of COVID-19 and COVID-19 vaccination on high-risk patients with Antiphospholipid Syndrome: A nationwide survey. Rheumatology 2022, 12, keac224. [Google Scholar] [CrossRef] [PubMed]
- Korentzelos, D.; Baloda, V.; Jung, Y.; Wheeler, B.; Shurin, M.R.; Wheeler, S.E. COVID-19 mRNA Vaccines May Cause False Reactivity in Some Serologic Laboratory Tests, Including Rapid Plasma Reagin Tests. Am. J. Clin. Pathol. 2022, 30, aqac025. [Google Scholar] [CrossRef] [PubMed]
- Signorelli, F.; Balbi, G.G.M.; Aikawa, N.E.; Silva, C.A.; Kupa, L.V.K.; Medeiros-Ribeiro, A.C.; Yuki, E.F.; Pasoto, S.G.; Saad, C.G.; Borba, E.F.; et al. Immunogenicity, safety, and antiphospholipid antibodies after SARS-CoV-2 vaccine in patients with primary antiphospholipid syndrome. Lupus 2022, 20, 9612033221102073. [Google Scholar] [CrossRef] [PubMed]
- Thurm, C.; Reinhold, A.; Borucki, K.; Kahlfuss, S.; Feist, E.; Schreiber, J.; Reinhold, D.; Schraven, B. Homologous and Heterologous Anti-COVID-19 Vaccination Does Not Induce New-Onset Formation of Autoantibodies Typically Accompanying Lupus Erythematodes, Rheumatoid Arthritis, Celiac Disease and Antiphospholipid Syndrome. Vaccines 2022, 10, 333. [Google Scholar] [CrossRef] [PubMed]
| Compound (Trade Name) | Manufacturer | Mechanism | Doses Needed | Interval | Storage (°C) | Efficacy (%) |
|---|---|---|---|---|---|---|
| BNT162b2 (Comirnaty) | Pfizer/BioNTech | mRNA | 2 | 21 d | −70 | 95 |
| mRNA-1273 (Spikevax) | Moderna | mRNA | 2 | 28 d | −20 | 94.5 |
| ChAdOx1 nCoV-19 (Vaxzevria) | AstraZeneca/Oxford | AdV-vectored | 2 | 4–12 wk | 2–8 | 70 |
| Ad26.CoV2.S | Johnson & Johnson | AdV-vectored | 1 | - | 2–8 | 66.3 |
| Gam-COVID-Vac (Sputnik V) | Gamaleya Research Institute | AdV-vectored | 2 | 21 d | −18 | 92 |
| Ad5-nCoV (Convidecia) | CanSino | AdV-vectored | 1 | - | −20 | 65.7 |
| NVX-CoV2373 (Covovax) | Novavax | Protein subunit | 2 | 21 d | −20 | 89.3 |
| EpiVacCorona (Aurora-CoV) | Vector Institute | Protein subunit | 2 | 21 d | 2–8 | n.a. |
| BBIBP-CorV (Covilo) | Sinopharm (Beijing) | Inactivated virus | 2 | 21–28 d | 2–8 | 79 |
| WIBP-CorV | Sinopharm (Wuhan) | Inactivated virus | 2 | 14–21 d | 2–8 | 72.5 |
| Vero cell (CoronaVac) | Sinovac Biotech | Inactivated virus | 2 | 28 d | 2–8 | 50–83.5 |
| BBV152 (Covaxin) | Bharat Biotech | Inactivated virus | 2 | 28 d | 2–8 | 81 |
| Vaccine | Number of Administered Doses * | Incidence of SAEs (%) *,† | Common AEs ‡ | SAEs § |
|---|---|---|---|---|
| BNT162b2 | 770,897,374 | 0.13 (0.05–0.21) | Local pain (>80%) fever (>10%) headache (>50%) fatigue (>60%) myalgia (>40%) arthralgia (>20%), lymphadenopathy (3%) chills (>30%) | ATE/VTE, ITP, TTS, allergic reactions including anaphylaxis, paroxysmal ventricular arrhythmia, syncope, MIS, myocarditis, pericarditis |
| mRNA-1273 | 203,315,870 | 0.18 (0.06–0.29) | Local pain (92%) fever (16%) headache (65%) fatigue (70%) myalgia (61%) arthralgia (46%), lymphadenopathy (20%) chills (45%) nausea/vomiting (23%) | ATE/VTE, ITP, TTS, allergic reactions including anaphylaxis, facial swelling, Bell’s palsy, myocarditis, pericarditis |
| ChAdOx1 nCoV-19 | 120,953,207 | 0.42 (0.13–0.68) | Local pain (58%) fever (8%) headache (53%) fatigue (53%) myalgia (44%) arthralgia (27%) chills (32%) nausea/vomiting (22%) | ATE/VTE, TTS, ITP, Guillain-Barré syndrome, CLS, CVST without thrombocytopenia, capillary leak syndrome |
| Ad26.CoV2.S | 19,219,676 | 0.26 (0.23–0.29) | Local pain (49%) fever (9%) headache (39%) fatigue (38%) myalgia (33%) nausea/vomiting (14%) | ATE/VTE, TTS, ITP, Guillain-Barré syndrome, capillary leak syndrome |
| Vaccine | Doses, n | ITP, n (inc) | TTP, n (inc) | ES, n (inc) | AIHA, n (inc) |
|---|---|---|---|---|---|
| BNT162b2 | 770,897,374 | 424 (0.55) | 89 (0.11) | 10 (0.01) | 124 (0.16) |
| mRNA-1273 | 203,315,870 | 24 (0.12) | 38 (0.19) | 7 (0.03) | 46 (0.23) |
| ChAdOx1 nCoV-19 | 120,953,207 | 254 (2.10) | 51 (0.42) | 5 (0.04) | 123 (1.02) |
| Ad26.CoV2.S | 19,219,676 | 13 (0.68) | 14 (0.73) | 0 (0) | 4 (0.21) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mingot-Castellano, M.E.; Butta, N.; Canaro, M.; Gómez del Castillo Solano, M.d.C.; Sánchez-González, B.; Jiménez-Bárcenas, R.; Pascual-Izquierdo, C.; Caballero-Navarro, G.; Entrena Ureña, L.; José González-López, T.; et al. COVID-19 Vaccines and Autoimmune Hematologic Disorders. Vaccines 2022, 10, 961. https://doi.org/10.3390/vaccines10060961
Mingot-Castellano ME, Butta N, Canaro M, Gómez del Castillo Solano MdC, Sánchez-González B, Jiménez-Bárcenas R, Pascual-Izquierdo C, Caballero-Navarro G, Entrena Ureña L, José González-López T, et al. COVID-19 Vaccines and Autoimmune Hematologic Disorders. Vaccines. 2022; 10(6):961. https://doi.org/10.3390/vaccines10060961
Chicago/Turabian StyleMingot-Castellano, María Eva, Nora Butta, Mariana Canaro, María del Carmen Gómez del Castillo Solano, Blanca Sánchez-González, Reyes Jiménez-Bárcenas, Cristina Pascual-Izquierdo, Gonzalo Caballero-Navarro, Laura Entrena Ureña, Tomás José González-López, and et al. 2022. "COVID-19 Vaccines and Autoimmune Hematologic Disorders" Vaccines 10, no. 6: 961. https://doi.org/10.3390/vaccines10060961
APA StyleMingot-Castellano, M. E., Butta, N., Canaro, M., Gómez del Castillo Solano, M. d. C., Sánchez-González, B., Jiménez-Bárcenas, R., Pascual-Izquierdo, C., Caballero-Navarro, G., Entrena Ureña, L., José González-López, T., & on behalf of the GEPTI. (2022). COVID-19 Vaccines and Autoimmune Hematologic Disorders. Vaccines, 10(6), 961. https://doi.org/10.3390/vaccines10060961







